Cysteamine
 | |
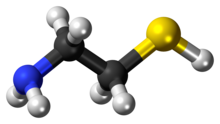 Skeletal formula (top) Ball-and-stick model of the cysteamine | |
| Clinical data | |
|---|---|
| Trade names | Cystagon, Procysbi, Cystaran, others |
| Other names | 2-Aminoethanethiol, β-Mercaptoethylamine, 2-Mercaptoethylamine, decarboxycysteine, thioethanolamine, mercaptamine bitartrate, cysteamine (USAN US) |
| AHFS/Drugs.com | Micromedex Detailed Consumer Information |
| License data |
|
| Pregnancy category |
|
| Routes of administration | By mouth, eye drops |
| ATC code | |
| Legal status | |
| Legal status | |
| Identifiers | |
| |
| CAS Number | |
| PubChem CID | |
| IUPHAR/BPS | |
| DrugBank | |
| ChemSpider | |
| UNII | |
| KEGG | |
| ChEBI | |
| ChEMBL | |
| PDB ligand | |
| CompTox Dashboard (EPA) | |
| ECHA InfoCard | 100.000.421 |
| Chemical and physical data | |
| Formula | C2H7NS |
| Molar mass | 77.15 g·mol−1 |
| 3D model (JSmol) | |
| Melting point | 95 to 97 °C (203 to 207 °F) |
| |
| |
Cysteamine is an organosulfur compound with the formula HSCH2CH2NH2. A white, water-soluble solid, it contains both an amine and a thiol functional groups. It is often used as salts of the ammonium derivative [HSCH2CH2NH3]+[12] including the hydrochloride, phosphocysteamine, and the bitartrate.[13]The intermediate pantetheine is broken down into cysteamine and pantothenic acid.[13]
It is biosynthesized in mammals, including humans, by the degradation of coenzyme A. It is the biosynthetic precursor to the neurotransmitter hypotaurine.[14][13]
Medical uses[edit]
As a medication, cysteamine, sold under the brand name Cystagon among others, is indicated to treat cystinosis, a lysosomal storage disease characterized by the abnormal accumulation of cystine, the oxidized dimer of the amino acid cysteine.[15][6][7][8] It removes the excessive cystine that builds up in cells of people with the disease.[13] It is available by mouth (capsule and extended release capsule) and in eye drops.[16][8][9][6][10][7][11][17]
When applied topically it can lighten skin that's been darkened as a result of post-inflammatory hyperpigmentation, sun exposure and Melasma.[18][19][20][21] Tentative evidence suggests that it may be a more effective depigmentation agent than hydroquinone, retinoids and topical corticosteroids in individuals with chronic skin discoloration.[22][23][24] Topical application of cysteamine cream has also demonstrated similar efficacy to intradermal tranexamic acid injections for the treatment of Melasma but with much fewer adverse effects.[25]
Adverse effects[edit]
Topical use[edit]
The most important adverse effect related to topical use might be skin irritation.[medical citation needed] However it's significantly better tolerated than alternative skin lightening treatments with similar efficacy.[24][25]
Oral use[edit]
The label for oral formulations of cysteamine carry warnings about symptoms similar to Ehlers-Danlos syndrome, severe skin rashes, ulcers or bleeding in the stomach and intestines, central nervous symptoms including seizures, lethargy, somnolence, depression, and encephalopathy, low white blood cell levels, elevated alkaline phosphatase, and idiopathic intracranial hypertension that can cause headache, tinnitus, dizziness, nausea, double or blurry vision, loss of vision, and pain behind the eye or pain with eye movement.[8]
Additional adverse effects of oral cysteamine include bad breath, skin odor, vomiting, nausea, stomach pain, diarrhea, and loss of appetite.[8]
The risks of cysteamine to a fetus are not known but it harms babies in animal models at doses less than those given to people.[6][7]
For eye drops, the most common adverse effects are sensitivity to light, redness, and eye pain, headache, and visual field defects.[7]
Interactions[edit]
There are no drug interactions for normal capsules or eye drops,[6][7] but the extended release capsules should not be taken with drugs that affect stomach acid like proton pump inhibitors or with alcohol, as they can cause the drug to be released too quickly.[8] It doesn't inhibit any cytochrome P450 enzymes.[8]
Pharmacology[edit]
People with cystinosis lack a functioning transporter (cystinosin) which transports cystine from the lysosome to the cytosol. This ultimately leads to buildup of cystine in lysosomes, where it crystallizes and damages cells.[16] Cysteamine enters lysosomes and converts cystine into cysteine and cysteine-cysteamine mixed disulfide, both of which can exit the lysosome.[8]
Cysteamine also promotes the transport of L-cysteine into cells.[13]
Society and culture[edit]
It is approved by the U.S. Food and Drug Administration (FDA) and the European Medicines Agency (EMA).[16][8][9][10][11][26][27]
In 2013, the regular capsule of cysteamine cost about $8,000 per year; the extended release form that was introduced that year was priced at $250,000 per year.[28]
History[edit]
The therapeutic effect of cysteamine on cystinosis was reported in the 1950s. Cysteamine was approved as a drug for cystinosis in the US in 1994.[8] An extended release form was approved in 2013.[28]
Research[edit]
It was studied in in vitro and animal models for radiation protection in the 1950s, and in similar models from the 1970s onwards for sickle cell anemia, effects on growth, its ability to modulate the immune system, and as a possible inhibitor of HIV.[13]
In the 1970s it was tested in clinical trials for Paracetamol toxicity which it failed, and in clinical trials for systemic lupus erythematosus in the 1990s and early 2000s, which it also failed.[13]
Clinical trials in Huntington's disease were begun in the 1990s and were ongoing as of 2015.[13][29]
As of 2013[update], it was in clinical trials for Parkinson's disease, malaria, radiation sickness, neurodegenerative disorders, neuropsychiatric disorders, and cancer treatment.[13][needs update]
It has been studied in clinical trials for pediatric nonalcoholic fatty liver disease.[30]
References[edit]
- ^ "CYSTADROPS : Cysteamine Ophthalmic Solution" (PDF). Pdf.hres.ca. Archived (PDF) from the original on 10 June 2022. Retrieved 8 June 2022.
- ^ "Genetic disorders". Health Canada. 9 May 2018. Retrieved 13 April 2024.
- ^ "Cystagon 150 mg hard capsules - Summary of Product Characteristics (SmPC)". Medicines.org.uk. 19 June 2019. Archived from the original on 9 June 2021. Retrieved 28 April 2020.
- ^ "Cystadrops 3.8 mg/mL eye drops solution - Summary of Product Characteristics (SmPC)". (emc). 19 June 2019. Archived from the original on 9 June 2020. Retrieved 9 June 2020.
- ^ "Procysbi 25 mg gastro-resistant hard capsules - Summary of Product Characteristics (SmPC)". Medicines.org.uk. 17 September 2019. Archived from the original on 22 January 2021. Retrieved 9 June 2020.
- ^ a b c d e "Cystagon- cysteamine bitartrate capsule". DailyMed. 29 January 2019. Archived from the original on 25 March 2021. Retrieved 27 April 2020.
- ^ a b c d e f "Cystaran- cysteamine hydrochloride solution". DailyMed. 22 November 2019. Archived from the original on 24 March 2021. Retrieved 27 April 2020.
- ^ a b c d e f g h i j "Procysbi- cysteamine bitartrate capsule, delayed release pellets Procysbi- cysteamine bitartrate granule, delayed release". DailyMed. U.S. National Library of Medicine. 23 March 2020. Archived from the original on 25 March 2021. Retrieved 27 April 2020.
- ^ a b c "Procysbi EPAR". European Medicines Agency (EMA). Archived from the original on 4 August 2020. Retrieved 27 April 2020.
- ^ a b c "Cystagon EPAR". European Medicines Agency (EMA). Archived from the original on 11 November 2020. Retrieved 27 April 2020.
- ^ a b c "Cystadrops EPAR". European Medicines Agency (EMA). Archived from the original on 4 August 2020. Retrieved 27 April 2020.
- ^ Reid EE (1958). Organic Chemistry of Bivalent Sulfur. Vol. 1. New York: Chemical Publishing Company, Inc. pp. 398–399.
- ^ a b c d e f g h i Besouw M, Masereeuw R, van den Heuvel L, Levtchenko E (August 2013). "Cysteamine: an old drug with new potential". Drug Discovery Today. 18 (15–16): 785–792. doi:10.1016/j.drudis.2013.02.003. PMID 23416144.
- ^ Singer TP (1975). "Oxidative Metabolism of Cysteine and Cystine". In Greenberg DM (ed.). Metabolic pathways: Metabolism of sulfur compounds. Vol. 7 (3rd ed.). New York: Academic Press. p. 545. ISBN 9780323162081. Archived from the original on 7 June 2021. Retrieved 11 January 2017.
- ^ Gahl WA, Thoene JG, Schneider JA (July 2002). "Cystinosis". The New England Journal of Medicine. 347 (2): 111–121. doi:10.1056/NEJMra020552. PMID 12110740.
- ^ a b c Nesterova G, Gahl WA (6 October 2016). "Cystinosis". In Adam MP, Ardinger HH, Pagon RA, Wallace SE, Bean LJ, Stephens K, Amemiya A (eds.). GeneReviews. Seattle WA: University of Washington. PMID 20301574. Archived from the original on 5 April 2011. Retrieved 11 January 2017.
- ^ Shams F, Livingstone I, Oladiwura D, Ramaesh K (10 October 2014). "Treatment of corneal cystine crystal accumulation in patients with cystinosis". Clinical Ophthalmology. 8: 2077–2084. doi:10.2147/OPTH.S36626. PMC 4199850. PMID 25336909.
- ^ Hsu C, Mahdi H, Pourahmadi M, Ahmadi S (April 2013). "Cysteamine cream as a new skin depigmenting product". Journal of the American Academy of Dermatology. 68 (4): AB189. doi:10.1016/j.jaad.2012.12.781. Retrieved 10 October 2021.
- ^ "Cysteamine cream". DermNet NZ. Archived from the original on 29 June 2021. Retrieved 29 June 2021.
- ^ Grimes PE, Ijaz S, Nashawati R, Kwak D (February 2019). "New oral and topical approaches for the treatment of melasma". International Journal of Women's Dermatology. 5 (1): 30–36. doi:10.1016/j.ijwd.2018.09.004. PMC 6374710. PMID 30809577.
- ^ Mansouri P, Farshi S, Hashemi Z, Kasraee B (July 2015). "Evaluation of the efficacy of cysteamine 5% cream in the treatment of epidermal melasma: a randomized double-blind placebo-controlled trial". The British Journal of Dermatology. 173 (1): 209–217. doi:10.1111/bjd.13424. PMID 25251767. S2CID 21618233.
- ^ Mathe N, Balogun M, Yoo J (January 2021). "A case report on the use of topical cysteamine 5% cream in the management of refractory postinflammatory hyperpigmentation (PIH) resistant to triple combination cream (hydroquinone, topical corticosteroids, and retinoids)". Journal of Cosmetic Dermatology. 20 (1): 204–206. doi:10.1111/jocd.13755. PMID 32997864. S2CID 222163129.
- ^ Kasraee B, Mansouri P, Farshi S (February 2019). "Significant therapeutic response to cysteamine cream in a melasma patient resistant to Kligman's formula". Journal of Cosmetic Dermatology. 18 (1): 293–295. doi:10.1111/jocd.12837. PMID 30537063. S2CID 54481706.
- ^ a b Karrabi M, David J, Sahebkar M (January 2021). "Clinical evaluation of efficacy, safety and tolerability of cysteamine 5% cream in comparison with modified Kligman's formula in subjects with epidermal melasma: A randomized, double-blind clinical trial study". Skin Research and Technology. 27 (1): 24–31. doi:10.1111/srt.12901. PMID 32585079. S2CID 220078010.
- ^ a b Hilton L (14 October 2020). "Cysteamine cream, tranexamic acid mesotherapy reveal similar efficacy, different safety". Dermatology Times. Archived from the original on 29 June 2021. Retrieved 29 June 2021.
- ^ "Drug Approval Package: Cystaran (cysteamine) NDA #200740". U.S. Food and Drug Administration (FDA). 26 August 2013. Archived from the original on 9 June 2020. Retrieved 9 June 2020.
- ^ "Drug Approval Package: PROCYSBI (cysteamine bitartrate) Delayed-Release Capsules NDA #203389". U.S. Food and Drug Administration (FDA). 24 December 1999. Archived from the original on 9 June 2020. Retrieved 9 June 2020.
- ^ a b Pollack A (30 April 2013). "F.D.A. Approves Raptor Drug for Form of Cystinosis". The New York Times. Archived from the original on 10 September 2021. Retrieved 26 February 2017.
- ^ Shannon KM, Fraint A (September 2015). "Therapeutic advances in Huntington's Disease". Movement Disorders. 30 (11): 1539–1546. doi:10.1002/mds.26331. PMID 26226924. S2CID 31037666.
- ^ Mitchel EB, Lavine JE (November 2014). "Review article: the management of paediatric nonalcoholic fatty liver disease". Alimentary Pharmacology & Therapeutics. 40 (10): 1155–1170. doi:10.1111/apt.12972. PMID 25267322. S2CID 21263419.
