Glucagon-like peptide-1 receptor
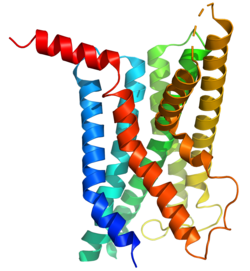
The glucagon-like peptide-1 receptor (GLP1R) is a G protein-coupled receptor (GPCR) found on beta cells of the pancreas and on neurons of the brain. It is involved in the control of blood sugar level by enhancing insulin secretion. In humans it is synthesised by the gene GLP1R, which is present on chromosome 6.[5][6] It is a member of the glucagon receptor family of GPCRs.[7] GLP1R is composed of two domains, one extracellular (ECD) that binds the C-terminal helix of GLP-1,[8] and one transmembrane (TMD) domain[9] that binds the N-terminal region of GLP-1.[10][11][12] In the TMD domain there is a fulcrum of polar residues that regulates the biased signaling of the receptor [10] while the transmembrane helical boundaries[13] and extracellular surface are a trigger for biased agonism.[11]
Ligands
[edit]GLP1R binds glucagon-like peptide-1 (GLP1) and glucagon as its natural endogenous agonists.[14]
- GLP-1 – endogenous in humans[14]
- glucagon – endogenous in humans[14]
- oxyntomodulin
- exendin-4,[14][15]
- exenatide
- lixisenatide[14]
- albiglutide
- beinaglutide
- dulaglutide
- efpeglenatide
- langlenatide
- liraglutide[14]
- PEG- Loxenatide
- semaglutide
- taspoglutide
- Ecnoglutide
- Utreglutide
- Glepaglutide
- Apraglutide
- Maridebart Cafraglutide/AMG133
- Tirzepatide
- pegapamodutide
- Mazdutide
- Survodutide
- Bamadutide
- Pemvidutide
- Cotadutide
- Retatrutide
- lithium chloride
- Grutalumab
- DA1726
- GX-G6
- GZR18
- HRS9531
- BGMO504
- PB718
- RAY1225
- VCT220
- VK2735
- BLX7006
- Supaglutide
- ASC30
- Positive:
Structure
[edit]The GLP-1 receptor is a transmembrane protein composed of seven alpha-helical transmembrane domains (TM1-TM7), an extracellular N-terminus, and an intracellular C-terminus. It belongs to the class B family of G protein-coupled receptors, also known as secretin-like receptors. The N-terminus of the receptor is responsible for binding glucagon-like peptide-1 (GLP-1) ligands, while the intracellular C-terminus interacts with intracellular signaling proteins to initiate downstream signaling pathways.
The extracellular N-terminus contains key regions involved in ligand recognition and binding. It undergoes conformational changes upon ligand binding, leading to activation of intracellular signaling cascades. The intracellular C-terminus interacts with G proteins and other signaling molecules to initiate cellular responses.

Function
[edit]Glucagon-like peptide-1 (GLP-1) is a hormone consisting of 30 amino acids. It is released by intestinal L cells when nutrients are consumed. GLP-1 has multiple effects, including enhancing insulin secretion from pancreatic beta cells in response to glucose, increasing insulin expression, preventing beta-cell apoptosis, promoting the formation of new beta cells, reducing glucagon secretion, slowing down stomach emptying, promoting satiety, and improving glucose disposal in peripheral tissues. Due to these diverse effects, there has been significant interest in developing long-lasting agonists of the GLP-1 receptor (GLP-1R) for the treatment of type 2 diabetes (T2D).
GLP1R is also expressed in the brain[18] where it is involved in the control of appetite.[19] Furthermore, mice that over express GLP1R display improved memory and learning.[20]
Stretch responsive vagal neurons in the stomach and intestines also express GLP1R.[21] GLP1R neurons particularly and densely innervate stomach muscle and can communicate with additional organ systems changing breathing and heart rate due to activation.[21]
Mechanism of action
[edit]Upon binding to its ligand GLP-1, the GLP-1 receptor activates intracellular signaling pathways that regulate insulin secretion, glucose metabolism, and satiety. In pancreatic beta cells, GLP-1 receptor activation enhances glucose-stimulated insulin secretion. This occurs through the activation of adenylyl cyclase, leading to increased intracellular levels of cyclic AMP (cAMP). The rise in cAMP activates protein kinase A (PKA), which promotes insulin exocytosis and enhances beta cell survival and proliferation. GLP-1 receptor signaling in pancreatic alpha cells reduces glucagon secretion, further contributing to glucose lowering. By inhibiting glucagon release, GLP-1 receptor activation helps to maintain glucose homeostasis. Another important function of the GLP-1 receptor is the regulation of gastric emptying. Activation of the receptor delays the rate at which the stomach empties, leading to increased satiety and reduced food intake. This effect contributes to weight management and appetite control.
'Appetite regulation and satiety': GLP-1 receptor signaling influences the central nervous system, particularly regions involved in appetite regulation. Activation of the GLP-1 receptor promotes feelings of satiety, leading to a reduction in food intake and improved weight management.
Gastric emptying': GLP-1 receptor activation slows down the rate at which the stomach empties its contents into the small intestine. This delay in gastric emptying contributes to the feeling of fullness and aids in controlling postprandial blood glucose levels.
Clinical significance
[edit]This article needs more reliable medical references for verification or relies too heavily on primary sources. (January 2024) |  |
Glucose Control: GLP-1 and its agonists enhance glucose control by promoting insulin secretion from pancreatic beta cells in a glucose-dependent manner. This means that they stimulate insulin release when blood glucose levels are elevated, helping to maintain normal blood sugar levels. By mimicking the physiological actions of GLP-1, GLP-1 receptor agonists effectively lower blood glucose levels, particularly after meals.
Weight Management: GLP-1 and its agonists have demonstrated the ability to promote weight loss or weight stabilization. These agents help reduce appetite, delay gastric emptying, and enhance satiety, leading to reduced food intake. The weight loss effect is particularly beneficial for individuals with type 2 diabetes who often struggle with obesity or overweight conditions.
Cardiovascular Protection: GLP-1 receptor agonists have shown potential cardiovascular benefits beyond glucose control. Some studies suggest that these agents may reduce the risk of cardiovascular events, such as heart attacks, strokes, and cardiovascular-related mortality. The cardiovascular protective effects may be related to their favorable effects on blood pressure, lipid profiles, inflammation, and endothelial function.
Beta Cell Preservation: GLP-1 and its agonists have been found to exert protective effects on pancreatic beta cells, which are responsible for producing insulin. They can enhance beta cell survival, promote beta cell proliferation, and inhibit beta cell apoptosis, thus preserving beta cell function over time.
Combination Therapy: GLP-1 receptor agonists are often used as part of combination therapy in the treatment of type 2 diabetes. They can be prescribed alongside other oral antidiabetic medications, such as metformin or sulfonylureas, to provide additional glycemic control and improve overall treatment outcomes.
Different GLP-1 receptor agonists go through inactivation by dipeptidyl peptidase-4 (DPP-4) enzymes (The clinical use of GLP-1 is hampered by its short-half life in the circulation (1-2 min), because of its proteolytic degradation by the enzymes dipeptidyl peptidase-4 (DPP-4) and neutral endopeptidase). One strategy used for overcoming this problem is by synthesising new GLP-1 receptor agonists with a prolonged circulating half-life that will display a reduced degradation by DPP-4 enzymes. Another strategy is to inihibit DPP-4 enzymes.
The debate about which treatment in combatting T2D still wages. Some studies suggest GLP1 Receptor Agonists (GLP1RAs) which have shown significant results compared to treatment with DPP-4 inhibitors. Some studies provided an insight into the reduction in limb incidents when treated with GLP1RAs. Other studies showed that GLP1RAs provide superior glycaemic control and weight loss when compared with DPP-4 inhibitors in patients with T2D.
Semaglutide
[edit]Commercially known as Ozempic (semaglutide), is a medication that belongs to a class of drugs called glucagon-like peptide-1 receptor agonists (GLP-1 RAs). It is primarily used for the treatment of type 2 diabetes and has shown potential benefits in addressing obesity as well. Semaglutide has an experimented half-life of 183 hours compared with Liraglutide (15 hours).
Concerning obesity, semaglutide has also shown effectiveness in treating obesity. In higher doses than those used for diabetes management, it can help reduce body weight. The precise mechanism by which semaglutide induces weight loss is not fully understood, but it is believed to involve various factors. Semaglutide decreases appetite by acting on the brain's centers responsible for appetite regulation, leading to a feeling of fullness and reduced food intake. It also slows down the emptying of the stomach, which can contribute to a decreased caloric intake. These combined effects on appetite and digestion help individuals lose weight.
The medication is administered as a once-weekly subcutaneous injection. The starting dose is usually low and gradually increased over several weeks to help minimize potential gastrointestinal side effects, such as nausea. The optimal dose for an individual is determined by their healthcare provider based on factors such as blood sugar levels, response to treatment, and tolerability.
Clinical trials have demonstrated the efficacy of Ozempic in improving glycemic control. The medication has shown significant reductions in HbA1c (a measure of long-term blood sugar control) as well as fasting and postprandial (after-meal) glucose levels.
possible Side effects of semaglutide:
Like any medication, Ozempic may cause side effects. Common side effects include nausea, vomiting, diarrhea, and constipation. These side effects are usually temporary and tend to diminish over time. Rare but more serious side effects may include pancreatitis, gallbladder disease, and allergic reactions. It is essential to discuss potential side effects and risks with a healthcare provider before starting Ozempic.
Huntington's disease
[edit]The diabetic, pancreatic, and neuroprotection implications of GLP1R are also thought to be potential therapies for treating the diabetes and energy metabolism abnormalities associated with Huntington's disease affecting the brain and periphery. Exendin-4, an FDA-approved antidiabetic glucagon-like peptide 1 (GLP-1) receptor agonist, has been tested in mice with the mutated human huntingtin protein showing neurodegenerative changes, motor dysfunction, poor energy metabolism, and high blood glucose levels. Exendin-4 (Ex-4) treatment reduced the accumulation of mutated human huntingtin protein aggregates, improved motor function, extended the survival time, improved glucose regulation, and decreased brain and pancreas pathology.[22]
Exendin-4 increases beta cell mass in the pancreatic islets to improve the release of insulin to ultimately increase glucose uptake. The mechanism regarding this insulin increase involves Ex-4 and GLP-1. When the islets in the pancreas are exposed to GLP-1, there is an increased expression of the anti-apoptotic gene bcl-2 and decreased expression of pro-apoptotic genes bax and caspase-3, which leads to greater cell survival. GLP-1 binding to its G protein-coupled receptor activates various different pathways including the growth factor receptor and is coupled to pathways stimulating mitogenesis. Some of these pathways include Rap, Erk1/2, MAPK, B-RAF, PI3-K, cAMP, PKA, and TORC2 that are activated to initiate exocytosis, proinsulin gene expression and translation, increase insulin biosynthesis, and genetically increase beta cell proliferation and neogenesis. The GLP-1R is a G protein-coupled receptor that is dependent on glucose and GLP-1 is a peptide hormone that acts directly on the beta cell to stimulate insulin secretion by activating signal transduction when glucose is present. When glucose is not present, this receptor no longer couples to stimulate insulin secretion in order to prevent hypoglycemia.[23]
Relating glucose metabolism and insulin sensitivity back to Huntington's disease, increased insulin release and beta cell proliferation by a GLP-1 agonist, Ex-4, helps combat the damage done by mutant htt in peripheral tissues. Htt aggregation decreases beta cell mass and thus impairs insulin release and increases blood glucose levels. Disruption of glycemic homeostasis then affects nutrient availability to neurons and alters neuron function contributing to neurodegeneration and motor problems seen in Huntington's disease. The health of the nervous system is related to metabolic health, thus a diabetes medication as a Huntington's disease treatment is a potential treatment. Ex-4 easily crosses the blood-brain barrier and GLP-1 and Ex-4 have been shown to act on neurons in the brain by exerting neuroprotective actions.[22]
In studies with Huntington's disease mice, daily treatments of Ex-4 significantly reduced glucose levels compared to those mice treated with saline. It also increased insulin sensitivity by about 50%, improved insulin-stimulated glucose uptake, and protect pancreatic beta cell function. Huntington's disease has also been linked to imbalances in leptin and ghrelin levels. Ex-4 restored ghrelin levels and also lowered leptin levels allowing Huntington's disease mice to eat more and counteract symptomatic weight loss. This treatment restored beta cell cells and islet structure, reduce mutated human huntingtin aggregates in the brain and pancreas, and also improve motor function seen by the increased activity level of the mice. Improvements were found in the areas of the body that expressed GLP-1R. In addition to its other effects on the Huntington's disease mouse model, daily treatment of Ex-4, the GLP-1R agonist, significantly delayed the onset of mortality and extended the lifespan by approximately one month.[22]
See also
[edit]References
[edit]- ^ a b c GRCh38: Ensembl release 89: ENSG00000112164 – Ensembl, May 2017
- ^ a b c GRCm38: Ensembl release 89: ENSMUSG00000024027 – Ensembl, May 2017
- ^ "Human PubMed Reference:". National Center for Biotechnology Information, U.S. National Library of Medicine.
- ^ "Mouse PubMed Reference:". National Center for Biotechnology Information, U.S. National Library of Medicine.
- ^ Thorens B (September 1992). "Expression cloning of the pancreatic beta cell receptor for the gluco-incretin hormone glucagon-like peptide 1". Proceedings of the National Academy of Sciences of the United States of America. 89 (18): 8641–5. Bibcode:1992PNAS...89.8641T. doi:10.1073/pnas.89.18.8641. PMC 49976. PMID 1326760.
- ^ Dillon JS, Tanizawa Y, Wheeler MB, Leng XH, Ligon BB, Rabin DU, et al. (October 1993). "Cloning and functional expression of the human glucagon-like peptide-1 (GLP-1) receptor". Endocrinology. 133 (4): 1907–10. doi:10.1210/endo.133.4.8404634. PMID 8404634.
- ^ Brubaker PL, Drucker DJ (2002). "Structure-function of the glucagon receptor family of G protein-coupled receptors, coupled to: the glucagon, GIP, GLP-1, and GLP-2 receptors" (PDF). Receptors & Channels. 8 (3–4): 179–88. doi:10.1080/10606820213687. PMID 12529935.
- ^ Underwood CR, Garibay P, Knudsen LB, Hastrup S, Peters GH, Rudolph R, Reedtz-Runge S (January 2010). "Crystal structure of glucagon-like peptide-1 in complex with the extracellular domain of the glucagon-like peptide-1 receptor". The Journal of Biological Chemistry. 285 (1): 723–30. doi:10.1074/jbc.M109.033829. PMC 2804221. PMID 19861722.
- ^ Song G, Yang D, Wang Y, de Graaf C, Zhou Q, Jiang S, et al. (June 2017). "Human GLP-1 receptor transmembrane domain structure in complex with allosteric modulators". Nature. 546 (7657): 312–315. Bibcode:2017Natur.546..312S. doi:10.1038/nature22378. PMID 28514449. S2CID 2141649.
- ^ a b Wootten D, Reynolds CA, Koole C, Smith KJ, Mobarec JC, Simms J, et al. (March 2016). "A Hydrogen-Bonded Polar Network in the Core of the Glucagon-Like Peptide-1 Receptor Is a Fulcrum for Biased Agonism: Lessons from Class B Crystal Structures". Molecular Pharmacology. 89 (3): 335–47. doi:10.1124/mol.115.101246. PMC 4767408. PMID 26700562.
- ^ a b Wootten D, Reynolds CA, Smith KJ, Mobarec JC, Koole C, Savage EE, et al. (June 2016). "The Extracellular Surface of the GLP-1 Receptor Is a Molecular Trigger for Biased Agonism". Cell. 165 (7): 1632–1643. doi:10.1016/j.cell.2016.05.023. PMC 4912689. PMID 27315480.
- ^ Yang D, de Graaf C, Yang L, Song G, Dai A, Cai X, et al. (June 2016). "Structural Determinants of Binding the Seven-transmembrane Domain of the Glucagon-like Peptide-1 Receptor (GLP-1R)". The Journal of Biological Chemistry. 291 (25): 12991–3004. doi:10.1074/jbc.M116.721977. PMC 4933217. PMID 27059958.
- ^ Wootten D, Reynolds CA, Smith KJ, Mobarec JC, Furness SG, Miller LJ, et al. (October 2016). "Key interactions by conserved polar amino acids located at the transmembrane helical boundaries in Class B GPCRs modulate activation, effector specificity and biased signalling in the glucagon-like peptide-1 receptor". Biochemical Pharmacology. 118: 68–87. doi:10.1016/j.bcp.2016.08.015. PMC 5063953. PMID 27569426.
- ^ a b c d e f g Maguire JJ, Davenport AP. "GLP-1 receptor". IUPHAR/BPS Guide to PHARMACOLOGY. International Union of Basic and Clinical Pharmacology. Retrieved 13 September 2015.
- ^ Koole C, Reynolds CA, Mobarec JC, Hick C, Sexton PM, Sakmar TP (April 2017). "Genetically encoded photocross-linkers determine the biological binding site of exendin-4 peptide in the N-terminal domain of the intact human glucagon-like peptide-1 receptor (GLP-1R)". The Journal of Biological Chemistry. 292 (17): 7131–7144. doi:10.1074/jbc.M117.779496. PMC 5409479. PMID 28283573.
- ^ Biggs EK, Liang L, Naylor J, Madalli S, Collier R, Coghlan MP, et al. (March 2018). "Development and characterisation of a novel glucagon like peptide-1 receptor antibody". Diabetologia. 61 (3): 711–721. doi:10.1007/s00125-017-4491-0. PMC 5890879. PMID 29119245.
- ^ O'Brien A, Andrews S, Baig AH, Bortolato A, Brown JH, Brown GA, et al. (2019-08-09). "Identification of a novel allosteric GLP–1R antagonist HTL26119 using structure-based drug design". Bioorganic & Medicinal Chemistry Letters. 29 (20): 126611. doi:10.1016/j.bmcl.2019.08.015. PMID 31447084. S2CID 201749908.
- ^ Cork SC, Richards JE, Holt MK, Gribble FM, Reimann F, Trapp S (October 2015). "Distribution and characterisation of Glucagon-like peptide-1 receptor expressing cells in the mouse brain". Molecular Metabolism. 4 (10): 718–31. doi:10.1016/j.molmet.2015.07.008. PMC 4588458. PMID 26500843.
- ^ Kinzig KP, D'Alessio DA, Seeley RJ (December 2002). "The diverse roles of specific GLP-1 receptors in the control of food intake and the response to visceral illness". The Journal of Neuroscience. 22 (23): 10470–6. doi:10.1523/JNEUROSCI.22-23-10470.2002. PMC 6758755. PMID 12451146.
- ^ During MJ, Cao L, Zuzga DS, Francis JS, Fitzsimons HL, Jiao X, et al. (September 2003). "Glucagon-like peptide-1 receptor is involved in learning and neuroprotection". Nature Medicine. 9 (9): 1173–9. doi:10.1038/nm919. PMID 12925848. S2CID 10370218.
- ^ a b Williams EK, Chang RB, Strochlic DE, Umans BD, Lowell BB, Liberles SD (June 2016). "Sensory Neurons that Detect Stretch and Nutrients in the Digestive System". Cell. 166 (1): 209–21. doi:10.1016/j.cell.2016.05.011. PMC 4930427. PMID 27238020.
- ^ a b c Martin B, Golden E, Carlson OD, Pistell P, Zhou J, Kim W, et al. (February 2009). "Exendin-4 improves glycemic control, ameliorates brain and pancreatic pathologies, and extends survival in a mouse model of Huntington's disease". Diabetes. 58 (2): 318–28. doi:10.2337/db08-0799. PMC 2628604. PMID 18984744.
- ^ Drucker DJ. "Resurrecting the Beta Cell in Type 2 Diabetes: Beta-cell Function, Preservation, and Neogenesis". PowerPoint slides. Medscape.
Further reading
[edit]- van Eyll B, Lankat-Buttgereit B, Bode HP, Göke R, Göke B (July 1994). "Signal transduction of the GLP-1-receptor cloned from a human insulinoma". FEBS Letters. 348 (1): 7–13. doi:10.1016/0014-5793(94)00553-2. PMID 7517895. S2CID 9085188.
- Liu C, Sun S, Xie J, Li H, Li T, Wu Q, Zhang Y, Bai X, Wang J, Wang X, Li Z, Wang W (2022). "GLP-1R Agonist Exendin-4 Protects Against Hemorrhagic Transformation Induced by rtPA After Ischemic Stroke via the Wnt/β-Catenin Signaling Pathway". Mol Neurobiol. 59 (6): 3649–3664. doi:10.1007/s12035-022-02811-9. PMC 9148281. PMID 35359227.
- Gromada J, Rorsman P, Dissing S, Wulff BS (October 1995). "Stimulation of cloned human glucagon-like peptide 1 receptor expressed in HEK 293 cells induces cAMP-dependent activation of calcium-induced calcium release". FEBS Letters. 373 (2): 182–6. doi:10.1016/0014-5793(95)01070-U. PMID 7589461. S2CID 28488846.
- Wei Y, Mojsov S (January 1995). "Tissue-specific expression of the human receptor for glucagon-like peptide-I: brain, heart and pancreatic forms have the same deduced amino acid sequences". FEBS Letters. 358 (3): 219–24. doi:10.1016/0014-5793(94)01430-9. PMID 7843404. S2CID 44371465.
- Lankat-Buttgereit B, Göke R, Stöckmann F, Jiang J, Fehmann HC, Göke B (1994). "Detection of the human glucagon-like peptide 1(7-36) amide receptor on insulinoma-derived cell membranes". Digestion. 55 (1): 29–33. doi:10.1159/000201119. PMID 8112494.
- Graziano MP, Hey PJ, Borkowski D, Chicchi GG, Strader CD (October 1993). "Cloning and functional expression of a human glucagon-like peptide-1 receptor". Biochemical and Biophysical Research Communications. 196 (1): 141–6. doi:10.1006/bbrc.1993.2226. PMID 8216285.
- Stoffel M, Espinosa R, Le Beau MM, Bell GI (August 1993). "Human glucagon-like peptide-1 receptor gene. Localization to chromosome band 6p21 by fluorescence in situ hybridization and linkage of a highly polymorphic simple tandem repeat DNA polymorphism to other markers on chromosome 6". Diabetes. 42 (8): 1215–8. doi:10.2337/diabetes.42.8.1215. PMID 8392011.
- Dillon JS, Tanizawa Y, Wheeler MB, Leng XH, Ligon BB, Rabin DU, et al. (October 1993). "Cloning and functional expression of the human glucagon-like peptide-1 (GLP-1) receptor". Endocrinology. 133 (4): 1907–10. doi:10.1210/endo.133.4.8404634. PMID 8404634.
- Thorens B, Porret A, Bühler L, Deng SP, Morel P, Widmann C (November 1993). "Cloning and functional expression of the human islet GLP-1 receptor. Demonstration that exendin-4 is an agonist and exendin-(9-39) an antagonist of the receptor". Diabetes. 42 (11): 1678–82. doi:10.2337/diabetes.42.11.1678. PMID 8405712.
- Lankat-Buttgereit B, Göke B (1997). "Cloning and characterization of the 5' flanking sequences (promoter region) of the human GLP-1 receptor gene". Peptides. 18 (5): 617–24. doi:10.1016/S0196-9781(97)00001-6. PMID 9213353. S2CID 29733898.
- Frimurer TM, Bywater RP (June 1999). "Structure of the integral membrane domain of the GLP1 receptor". Proteins. 35 (4): 375–86. doi:10.1002/(SICI)1097-0134(19990601)35:4<375::AID-PROT1>3.0.CO;2-2. PMID 10382665.
- Huypens P, Ling Z, Pipeleers D, Schuit F (August 2000). "Glucagon receptors on human islet cells contribute to glucose competence of insulin release". Diabetologia. 43 (8): 1012–9. doi:10.1007/s001250051484. PMID 10990079.
- Hartley JL, Temple GF, Brasch MA (November 2000). "DNA cloning using in vitro site-specific recombination". Genome Research. 10 (11): 1788–95. doi:10.1101/gr.143000. PMC 310948. PMID 11076863.
- Xiao Q, Jeng W, Wheeler MB (December 2000). "Characterization of glucagon-like peptide-1 receptor-binding determinants". Journal of Molecular Endocrinology. 25 (3): 321–35. doi:10.1677/jme.0.0250321. PMID 11116211.
- Bazarsuren A, Grauschopf U, Wozny M, Reusch D, Hoffmann E, Schaefer W, et al. (May 2002). "In vitro folding, functional characterization, and disulfide pattern of the extracellular domain of human GLP-1 receptor". Biophysical Chemistry. 96 (2–3): 305–18. doi:10.1016/S0301-4622(02)00023-6. PMID 12034449.
- Tokuyama Y, Matsui K, Egashira T, Nozaki O, Ishizuka T, Kanatsuka A (October 2004). "Five missense mutations in glucagon-like peptide 1 receptor gene in Japanese population". Diabetes Research and Clinical Practice. 66 (1): 63–9. doi:10.1016/j.diabres.2004.02.004. PMID 15364163.
- Jorgensen R, Martini L, Schwartz TW, Elling CE (March 2005). "Characterization of glucagon-like peptide-1 receptor beta-arrestin 2 interaction: a high-affinity receptor phenotype". Molecular Endocrinology. 19 (3): 812–23. doi:10.1210/me.2004-0312. PMID 15528268.
- Mahon MJ, Shimada M (January 2005). "Calmodulin interacts with the cytoplasmic tails of the parathyroid hormone 1 receptor and a sub-set of class b G-protein coupled receptors". FEBS Letters. 579 (3): 803–7. doi:10.1016/j.febslet.2004.12.056. PMID 15670850. S2CID 6471940.
- Graaf C, Donnelly D, Wootten D, Lau J, Sexton PM, Miller LJ, et al. (October 2016). "Glucagon-Like Peptide-1 and Its Class B G Protein-Coupled Receptors: A Long March to Therapeutic Successes". Pharmacological Reviews. 68 (4): 954–1013. doi:10.1124/pr.115.011395. PMC 5050443. PMID 27630114.
- Song G, Yang D, Wang Y, de Graaf C, Zhou Q, Jiang S, et al. (June 2017). "Human GLP-1 receptor transmembrane domain structure in complex with allosteric modulators". Nature. 546 (7657): 312–315. Bibcode:2017Natur.546..312S. doi:10.1038/nature22378. PMID 28514449. S2CID 2141649.
- Brunton S (May 2014). "GLP-1 receptor agonists vs. DPP-4 inhibitors for type 2 diabetes: is one approach more successful or preferable than the other?". International Journal of Clinical Practice. 68 (5): 557–567. doi:10.1111/ijcp.12361. PMC 4238422. PMID 24499291.
- Donnelly D (May 2012). "The structure and function of the glucagon-like peptide-1 receptor and its ligands". British Journal of Pharmacology. 166 (1): 27–41. doi:10.1111/j.1476-5381.2011.01687.x. PMC 3415635. PMID 21950636.
- Christou GA, Katsiki N, Blundell J, Fruhbeck G, Kiortsis DN (June 2019). "Semaglutide as a promising antiobesity drug". Obesity Reviews. 20 (6): 805–815. doi:10.1111/obr.12839. PMID 30768766. S2CID 73422503.
External links
[edit]- "Glucagon Receptor Family: GLP-1". IUPHAR Database of Receptors and Ion Channels. International Union of Basic and Clinical Pharmacology. Archived from the original on 2016-03-03. Retrieved 2007-10-25.
- glucagon-like+peptide+receptor at the U.S. National Library of Medicine Medical Subject Headings (MeSH)
- Overview of all the structural information available in the PDB for UniProt: P43220 (Glucagon-like peptide 1 receptor) at the PDBe-KB.