Photorejuvenation
Photorejuvenation is a skin treatment that uses lasers, intense pulsed light, or photodynamic therapy to treat skin conditions and remove effects of photoaging such as wrinkles, spots, and textures. The process induces controlled wounds to the skin. This prompts the skin to heal itself, by creating new cells. This process—to a certain extent—removes the signs of photoaging.[1] The technique was invented by Thomas L Roberts, III using CO2 lasers in the 1990s.[2][3] Observed complications have included scarring, hyperpigmentation, acne, and herpes.
Skin rejuvenation[edit]
Skin rejuvenation can be effected through various modalities, including thermal, chemical, mechanical, injection, and light.[4]
Laser resurfacing[edit]
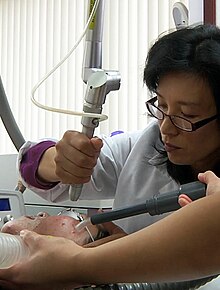
Laser resurfacing is a laser surgery technique that disassociates molecular bonds. It is used for the treatment of wrinkles, solar lentigenes, sun damage, scarring (acne scars and surgical scars), stretch marks, actinic keratosis, and telangiectasias. It can be combined with liposuction to help tighten and smooth over the new contours after removal of excess fat. Resurfacing can be ablative, which vaporizes tissue and creates wounds, or non-ablative which keeps the skin intact.
Laser resurfacing is usually done with a 2940 nm Er:YAG laser or a 10,600 nm CO2 laser. Complete resurfacing was first done with a CO2 laser. Both Erbium and CO2 are used to treat deep rhytides, sun damage and age spots. Through the heating of the deep dermis, fibroblasts are stimulated to form new collagen and elastin helping to bring increased turgor and thickness to the skin. A variety of modes have been developed including Nd:Yag lasers and a plasma device.[5]
CO2 resurfacing has been shown to have an increased risk of hypopigmentation and scarring than erbium lasers. This is due to the high degree of coagulation and thus heat production that occurs as a nature of the CO2 wavelength.
Fractional laser[edit]
Fractional laser photothermolysis (FP) is a form of laser-based skin resurfacing, with several devices on the market, such as Fraxel. A fractional laser delivers laser light to the skin. Hundreds or thousands of laser pinpoints may be used per square inch, leaving healthy skin between the ablated areas.
Complications observed in a study of 961 treatments included acne and herpes outbreaks.[6] There have been anecdotal negative accounts of bad scarring and hyperpigmentation.[7]
Erbium and CO2 fractional systems have a better safety profile than lasers of the past.[8]
Intense pulsed light[edit]
Intense Pulsed Light (IPL) uses flashlamps (and not lasers) to produce high intensity light over broad visible and infrared wavelengths with filters that select the desired range. IPL is used to treat dyschromia, rosacea, melasma, acne, photodamage, vascular and pigmented lesions, and rhytides.[9]
One study conducted by a group of four researchers from the Weill Cornell Medical College of Cornell University in 2004 found IPL to be a "non-invasive, non-ablative method for rejuvenating photoaged skin with minimal adverse events".[10]
Other studies, however, have noted that exposing cells to direct heat can cause DNA damage — not only in those cells, but also in surrounding tissue that was not directly exposed, and concluded treatments can cause microscopic thermal injuries, and that further research is warranted.[11]
IPL is effective for pigmentation and telangiectasias, but has lesser results for wrinkles.[12]
Photodynamic therapy[edit]
Photodynamic therapy (PDT) uses photosensitive compounds that are activated by light. It is used to treat actinic keratoses, acne, photoaging, and skin cancer.
See also[edit]
References[edit]
- ^ Lim, Henry W.; Herbert Honigsmann; John L. M. Hawk (2007). Photodermatology. CRC Press. pp. 402, 403. ISBN 978-0-8493-7496-8.
- ^ Roberts, Thomas L III. The emerging role of the CO2 lasers in aesthetic plastic surgery. Presented at the XIII Congress of the International Society for Aesthetic Plastic Surgery, New York, NY, Sept. 28-Oct. 1, 1995.
- ^ Roberts, Thomas L III; Lettieri, John T; Ellis, Laura B. (1996). "CO2 Laser Resurfacing: Recognizing and Minimizing Complications". Aesthetic Surgery Journal. 16 (2). American Society for Aesthetic Plastic Surgery: 142–148. doi:10.1016/S1090-820X(96)70038-9.
- ^ "Photo Rejuvenation for Better-Looking Skin: What Doctors Are Saying". Retrieved 2009-07-02.
- ^ "Portrait(R) Plasma Skin Regeneration". medicalnewstoday.com. MediLexicon International Ltd. September 2006. Retrieved 17 February 2014.
- ^ Graber, Emmy M.; Tanzi, Elizabeth L.; Alster, Tina S. (March 2008). "Side Effects and Complications of Fractional Laser Photothermolysis: Experience with 961 Treatments". Dermatologic Surgery. 34 (3): 301–307. doi:10.1111/j.1524-4725.2007.34062.x. PMID 18190541. S2CID 23942929.
- ^ Hoene, Christine. "Adverse Effects Fraxel Repair". realself.com. RealSelf, Inc. Retrieved 17 February 2014.
- ^ Ortiz, A. E.; Goldman, M. P.; Fitzpatrick, R. E. (December 2014). "Ablative CO2 Lasers for Skin Tightening: Traditional Versus Fractional". Dermatologic Surgery. 40 (Suppl 12): S147–51. doi:10.1097/DSS.0000000000000230. PMID 25417566. S2CID 8266926.
- ^ Babilas, P; Schreml, S; Szeimies, R. M.; Landthaler, M (Feb 2010). "Intense pulsed light (IPL): a review". Lasers Surg. Med. 42 (2): 93–104. doi:10.1002/lsm.20877. PMID 20166155.
- ^ Sadick NS, Weiss R, Kilmer S, Bitter P, NS; Weiss, R; Kilmer, S; Bitter, P (January 2004). "Photorejuvenation with intense pulsed light: results of a multi-center study". Journal of Drugs in Dermatology. 3 (1): 41–49. PMID 14964745.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Purschke, M; Laubach, HJ; Anderson, RR; Manstein, D (2010). "Thermal injury causes DNA damage and lethality in unheated surrounding cells: active thermal bystander effect". The Journal of Investigative Dermatology. 130 (1): 86–92. doi:10.1038/jid.2009.205. PMID 19587691.
- ^ Kohl, E. A.; Babilas, P; Landthaler, M (2010). "Skin rejuvenation with intense pulsed light". Acta Dermatovenerol Croat. 18 (3): 181–4. PMID 20887700.
