Spondylolysis
| Spondylolysis | |
|---|---|
| Specialty | Orthopedic surgery |
Spondylolysis (spon-dee-low-lye-sis) is defined as a defect or stress fracture in the pars interarticularis of the vertebral arch.[1] The vast majority of cases occur in the lower lumbar vertebrae (L5), but spondylolysis may also occur in the cervical vertebrae.[2]
Pathophysiology
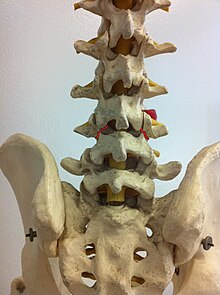
Spondylolysis is a bony defect or fracture within the pars interarticularis of the vertebral arch in the spinal column. The vast majority of spondylolysis occur in the lumbar vertebrae, however it can also be seen in cervical vertebrae.[2] The lumbar vertebra consist of a body, pedicle, lamina, pars interarticularis, transverse process, spinous process and superior and inferior articular facets, which form joints that link the vertebrae together. When examining the vertebra, the pars interarticularis is the bony segment between the superior and inferior articular facet joints located anterior to the lamina and posterior to the pedicle. Separation of the pars interarticularis occurs when spondylolysis is present in the spinal column.[3]
Spondylolysis is typically caused by a stress fracture of the bone, and is especially common in adolescents who over-train in activities. The pars interarticularis is vulnerable to fracture during spinal hyperextension, especially when combined with rotation, or when experiencing a force during a landing. This stress fracture most commonly occurs where the concave lumbar spine transitions to the convex sacrum (L5-S1). A significant amount of individuals with spondylolysis will develop spondylolisthesis, which is true for 50-81% of this population.[4][5]
Epidemiology/Etiology
The cause of spondylolysis remains unknown, however many factors are thought to contribute to its development. The condition is present in up to 6% of the population, majority of which usually present asymptomatically.[6] Research supports that there are hereditary and acquired risk factors that can make one more susceptible to the defect. The disorder is generally more prevalent in males compared to females, and tends to occur earlier in males due to their involvement in more strenuous activities at a younger age.[7] In a young athlete, the spine is still growing which means there are many ossification centers, leaving points of weakness in the spine. This leaves young athletes at increased risk, particularly when involved in repetitive hyperextension and rotation across the lumbar spine.[8] Spondylolysis is a common cause of low back in preadolescents and adolescent athletes, as it accounts for about 50% of all low back pain.[6] It is believed that both repetitive trauma and an inherent genetic weakness can make an individual more susceptible to spondylolysis.[9]
Signs and Symptoms
In majority of cases, spondylolysis presents asymptomatically which can make diagnosis both difficult and incidental.[5] When a patient does present with symptoms, there are general signs and symptoms a clinician will look for:
- Clinical Signs:[9][10]
- Pain on completion of the stork test (placed in hyperextension and rotation)
- Excessive lordotic posture
- Unilateral tenderness on palpation
- Visible on diagnostic imaging (Scottie dog fracture)
- Symptoms:[9][10]
- Unilateral low back pain
- Pain that radiates into the buttocks or legs
- Onset of pain can be acute or gradual
- Pain that can restricts daily activities
- Pain that worsens after strenuous activity
- Pain aggravated with lumbar hyperextension
Risk Factors
Sports involving repetitive or forceful hyperextension of the spine, especially when combined with rotation are the main mechanism of injury for spondylolysis. The stress fracture of the pars interarticularis occurs on the side opposite to activity. For instance, for a right handed player, the fracture occurs on the left side of the vertebrae.[10]
Spondylolysis has a higher occurrence in the following activities:[10]
- Tennis
- Diving
- Cheerleading
- Gymnastics
- Football
- Soccer
- Wrestling
- Weightlifting
- Cricket
- Rugby
- Volleyball
Although this condition can be caused by repetitive trauma to the lumbar spine in strenuous sports, however other risk factors can predispose individuals to spondylolsis. Males are more commonly affected by spondylolysis than females.[5] In one study looking at youth athletes, it was found that the mean age of individuals with spondylolisthesis was 20 years of age.[11] Spondylolysis also runs in families suggesting a hereditary component such as a predisposition to weaker vertebrae.[5]
Diagnosis
There are several imaging techniques used to diagnose spondylolysis. Common imaging techniques include X-ray, MRI, Bone Scintigraphy (Bone Scan), and Computed Tomography (CT Scan). Qualified health care practitioners are also able to conduct clinical tests such as the one-legged hyperextension test to diagnose active spondylolysis.[12]
One-legged Hyperextension Test
This is a test conducted by a qualified healthcare practitioner within a clinical setting. It involves having the patient stand upon one leg and then lean backwards. The test should produce pain on the same side of the spine as the leg that you are standing on. If it produces pain this indicates spondylolysis on that side. The test is then performed on the other side assessing for pain again. The test can be positive on one side, both sides or neither.[12]
X-Ray
X-ray imaging uses electromagnetic radiation and projects it into the body. The radiation is blocked by the dense tissues of the body (i.e. bone) and appear white on the image that is produced. Tissues that contain air and are less dense appear as black on the x-ray image. A vertebra with a fracture will have a black mark in it. The black mark will appear on the pars interarticularis if someone has spondylolysis. This area is difficult to image as the pars interarticularis is blocked by multiple structures. A CT scan is able to circumvent this difficulty because of its ability to produce 3-dimensional images.[12][13]

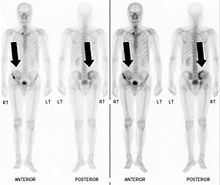
Bone Scintigraphy
Also known as a bone scan, bone scintigraphy involves the injection of a small amount of radioactive tracer into the bloodstream. This tracer decays and emits radioactive energy which can be detected by a special camera. The camera produces a black and white image where areas shown as dark black indicate bone damage of some kind. If there is a black spot in the lumbar vertebrae (e.g. L5) this indicates damage and potentially spondylolysis. If this test is positive, a CT scan is usually ordered to confirm spondylolysis.[12]
Computed Tomography
Commonly known as a CT Scan or CAT scan, this form of imaging is very similar to x-ray technology but produces many more images than an x-ray does. The multiple images produce cross-sectional views not possible with an x-ray. This allows a physician or radiologist to examine the images from many more angles than an x-ray allows. For this reason the CT scan is much more accurate in detecting spondylolysis than an x-ray. Bone scintigraphy combined with CT scan is considered the gold standard which means that it is best at detecting spondylolysis.[12][14]
MRI
MRI is a newer technique used to diagnose spondylolysis and is favorable for a few reasons. The MRI is much more accurate than the x-ray and also does not use radiation. The MRI uses powerful magnets and radio frequencies to produce very detailed images of many different densities of tissue including bone and soft tissues.[12][15]
Treatment
Conservative Management
Treatment for spondylosis ranges from bracing, activity restriction, extension exercises, flexion exercises and deep abdominal strengthening, that is administered through physical therapy. The duration of physical therapy a patient receives varies upon the severity of spondylolysis, however typically ranges from three to six months. The goal of physical therapy is to minimize movement at the unstable defect of the pars interarticularis. Once a patient completes physical therapy, and displays no symptoms or inflammation in the lower back, they are cleared to continue with daily or athletic activities. However, a patient may need to maintain a variety of rehabilitation techniques after physical therapy to prevent the recurrence of spondylolysis.[16]
Deep Abdominal Co-contraction Exercises
The aim of deep abdominal co-contraction exercises is to train muscles surrounding the lumbar spine which provide stability of the spine. Spondylolysis results in a spinal instability and disrupts patterns of co-recruitment between muscle synergies. Specifically, local muscles that attach directly to the spine are affected. The lumbar multifidis and transversus abdominis play a direct role in stabilizing the lumbar spine. Instead the local muscles in individuals with spondylolysis are vulnerable to dysfunction, which results in abnormal spinal stability causing chronic low back pain. To compensate, the large torque producing global muscles are used to stabilize the spine.[17]
In one study, patients are taught to train the co-contraction of deep abdominal muscles and lumbar multifidus in static postures, functional tasks and aerobic activities. This technique was shown to reduce pain and functional disability when compared to other conservative treatments. These results also had a long- term effect in reducing levels of pain and functional disability. This is because motor programming eventually became automatic, and conscious control was no longer needed to contract the deep abdominal muscles during activities.[17]
Activity Restriction
Activity restriction of spondylolysis is advised for a short period of time once the patient becomes symptomatic, followed by a guided physical therapy program. Once spondylolysis has been diagnosed, treatment often consists of a short rest period of two to three days, followed by a physical therapy program. There should be restriction of heavy lifting, excessive bending, twisting and avoidance of any work, recreational activities or participation in sport that causes stress to the lumbar spine.[18] Activity restriction can help eliminate and control a patient's symptoms so they are able to resume their normal activities.[19] Activity restriction is most commonly used in conjunction with other rehabilitation techniques including bracing.
Bracing

Acute spondylolysis is most commonly treated through the use of an anti-lordotic brace (Boston brace) to control and limit spinal movement, and reduce stress on the injured spinal segment.[18][20] Bracing immobilizes the spine in a flexed position for a short period to allow healing of the bony defect in the pars interarticularis.[20][21] An antilordotic brace commonly utilizes a plastic component that is contoured to closely fit the body.[20] Antilordotic bracing subsequently reduces the athlete’s symptoms by decreasing the amount of stress on the low back, and allows a prompt return to sport for athletes.[18] Typically, bracing is utilized for 6–12 weeks.[21]
In order for a brace to be effective, it must be worn every day for the required amount of time. Patients are given a brace schedule determined by their physical therapist that explains the amount of time the brace must be worn daily. A brace's effectiveness increases with adherence to the bracing schedule. Patients that do not follow their bracing schedule are more likely to have their symptoms progress.[21] Research has demonstrated that when braces are used as prescribed with full compliance, they are successful at preventing spondylolysis progression.[18]
Surgery
Most patients with spondylolysis do not require surgery but, if the symptoms are not relieved with non-surgical treatments, or when the condition progresses to high grade spondylolisthesis, then patients may require surgery. There are two main types of surgery for this condition:[22]
- Posterior Lumbar Spinal Fusion: This procedure is recommended when a set of vertebrae becomes loose or unstable. The surgeon joins two or more bones (vertebrae) together through the use of metal rods, screws, and bone grafts. The bone grafts complete their fusion in 4–8 months following the surgery, securing the spine in the correct position. The procedure is also used to treat spinal instability, fractures in the lumbar spine and, severe degenerative disc disease. The process is relatively non-invasive, performed through small incisions and has a high success rate.[22]
- Laminectomy: Often performed when spinal stenosis occurs in conjunction with spondylolysis. The procedure surgically removes part or all of the lamina from the bony ring of the vertebra to reduce the pressure on the spinal cord. The laminectomy is commonly performed on the vertebrae in the lower back and in the neck.[22]
Implications for Rehabilitation
Those who suffer from Spondylolysis are typically otherwise healthy individuals who are still able to contribute to their team and society as a whole.
References
- ^ Iwamoto, J., Takeda, T., Wakano, K. Returning athletes with severe low back pain and spondylolysis to original sporting activities with conservative treatment. Sports Scandinavian Journal of Medicine and Science in Sports. 2004;14(6):346–351.
- ^ a b Dubousset, J. Treatment of Spondylolysis and Spondylolisthesis in Children and Adolescents. Clinical Orthopaedics and Related Research. 1997;337:77–85.
- ^ Standaert, C.J., Herring, S.A., Cole, A.J., Stratton, S.A. The Lumbar Spine and Sports. Low Back Pain Handbook. 2003:385–404.
- ^ Cianfoni A, Cerase A, Magarelli N, Bonomo L. Lumbar spondylolysis: a review. Skeletal Radiology. 2011;40:683-700.
- ^ a b c d Syrmou, E., Tsitsopoulos, P. P., Marinopoulos, D., Tsonidis, C., Anagnostopoulos, I., & Tsitsopoulos, P. D.Spondylolysis: A Review and Reappraisal. H Quarterly Medical Journal. 2010;14(1): 17–21
- ^ a b McTimoney, M. & Micheli, L. J. Current Evaluation and Management of Spondylolysis and Spondylolisthesis. Current Sports Medicine Reports. 2003, 2:41–46
- ^ Canzonieri, C., & Pilloud, M. A. The Occurrence and Possible and Aetiology of spondylolysis in a Pre-Contact California Population. International Journal of Osteoarchaeology. 2012, 24:602-613
- ^ McCleary, M. D. and Congeni, J. A. Current concepts in the diagnosis and treatment of spondylolysis in young athletes. Current sports medicine reports. 2007;6(1):62-66.
- ^ a b c Spondylolysis and Spondylolisthesis of the Lumbar Spine. , Children's Orthopaedics, Mass General. Available at: http://www.massgeneral.org/ortho-childrens/conditions-treatments/spondylolysis.aspx. Accessed March 28, 2016
- ^ a b c d Humphreys, D. Lecture on Spondylolysis and Spondylolisthesis. [OWL]. Western University Kinesiology Program; 2015.
- ^ Debnath, U. K., Freeman, B. J. C., Gregory, P., de la Harpe, D., Kerslake, R. W. and Webb, J.K. Clinical outcome and return to sport after the surgical treatment of spondylolysis in young athletes. Journal of Bone & Joint Surgery, British Volume. 2003, 85(2): 244-249.
- ^ a b c d e f Masci L, Pike J, Malara F, Phillips B, Bennell K, Brukner P. Use of the one-legged hyperextension test and magnetic resonance imaging in the diagnosis of active spondylolysis.British Journal of Sports Medicine. 2006;40:940-946.
- ^ X-ray: MedlinePlus Medical Encyclopedia. US National Library of Medicine. 2014. Available at: https://www.nlm.nih.gov/medlineplus/ency/article/003337.htm. Accessed March 30, 2016.
- ^ Body CT (CAT Scan). Body CT (CAT Scan). 2016. Available at: http://www.radiologyinfo.org/en/info.cfm?pg=bodyct. Accessed March 30, 2016.
- ^ Body MRI - magnetic resonance imaging of the chest, abdomen and pelvis. Body MRI - magnetic resonance imaging of the chest, abdomen and pelvis. 2014. Available at: http://www.radiologyinfo.org/en/info.cfm?pg=bodymr. Accessed March 30, 2016.
- ^ Pizzutillo, PD, Hummer, CD. Nonoperative Treatment for Painful Adolescent Spondylolysis or Spondylolisthesis. Journal of Pediatric Orthopaedics. 1989;9(5):538–540.
- ^ a b O'Sullivan, P. B., Phyty, D. M., Twomey, L. T., & Allison, G. T.Evaluation of Specific Stabilizing Exercise in the Treatment of Chronic Low Back Pain with Radiologic Diagnosis of Spondylolysis or Spondylolisthesis. Spine. 1997, 22(24):2959-2967.
- ^ a b c d Iwamoto, J. Return to sports activity by athletes after treatment of spondylolysis. World Journal of Orthopedics. 2010;1(1):26.
- ^ Bergmann TF, Hyde TE, Yochum TR. Active or Inactive Spondylolysis and/or Spondylolisthesis: What's the Real Cause of Back Pain? Journal of the Neuromusculoskeletal System. 2002:10:70-78.
- ^ a b c Boston Brace: The Orthotics and Prosthetics Leaders. Boston Overlap Brace. Boston Overlap Brace. Available at: http://www.bostonbrace.com/content/boston_overlap_brace.asp. Accessed March 27, 2016.
- ^ a b c Parkview Spine Institute. Treatment Options for Pediatric/Adolescent Spondylolysis and Spondylolisthesis - Parkview Orthopedics. Parkview Orthopedics. Available at: http://parkviewspine.com/patient-education/treatment-options-for-pediatricadolescent-spondylolysis-and-spondylolisthesis/. Accessed March 27, 2016.
- ^ a b c Deguchi M, Rapoff AJ, Zdeblick TA. Posterolateral fusion for isthmic spondylolisthesis in adults: Analysis of fusion rate and clinical results. Journal of Spinal Disorders. 1998;11:459-464.
External links
- http://www.physio-pedia.com/Spondylolysis_in_Young_Athletes#cite_ref-Debnath_35-0
- A Patient's Guide to Lumbar Spondylolysis
- Spondylosis Treatement
- http://www.orthoseek.com/articles/spondyl.html
- http://www.orthogate.org/patient-education/lumbar-spine/lumbar-spondylolysis.html
- http://www.emedicinehealth.com/spondylosis/page14_em.htm
