Bladder exstrophy
| Bladder exstrophy | |
|---|---|
| Other names | Ectopia vesicae |
 | |
| Female baby with classical bladder exstrophy | |
| Specialty | Medical genetics |
Bladder exstrophy is a congenital anomaly that exists along the spectrum of the exstrophy-epispadias complex, and most notably involves protrusion of the urinary bladder through a defect in the abdominal wall. Its presentation is variable, often including abnormalities of the bony pelvis, pelvic floor, and genitalia. The underlying embryologic mechanism leading to bladder exstrophy is unknown, though it is thought to be in part due to failed reinforcement of the cloacal membrane by underlying mesoderm.[1] Exstrophy means the inversion of a hollow organ.[2]
Signs and symptoms
[edit]The classic manifestation of bladder exstrophy presents with:[citation needed]
- A defect in the abdominal wall occupied by both the exstrophied bladder as well as a portion of the urethra
- A flattened puborectal sling
- Separation of the pubic symphysis
- Shortening of a pubic rami
- External rotation of the pelvis.
Females frequently have a displaced and narrowed vaginal orifice, a bifid clitoris, and divergent labia.[3]
Cause
[edit]The cause is not yet clinically established but is thought to be in part due to failed reinforcement of the cloacal membrane by underlying mesoderm.[4]
Diagnosis
[edit]In a small retrospective study of 25 pregnancies, five factors were found to be strongly associated with a prenatal diagnosis of bladder exstrophy:[4]
- Inability to visualize the bladder on ultrasound
- A lower abdominal bulge
- A small penis with anteriorly displaced scrotum
- A low set umbilical insertion
- Abnormal widening of the iliac crests
While a diagnosis of bladder exstrophy was made retrospectively in a majority of pregnancies, in only three cases was a prenatal diagnosis made.[5]
Management
[edit]The extreme rarity of the disease limits the surgical opportunities to practice the complex closure required in these patients. For this reason, patients have the best outcomes when the bladder closures are performed at high volume centers where surgical and nursing teams have extensive experience in caring for the disease.[6] The highest volume center in the United States, and the world, is the Johns Hopkins Hospital in Baltimore, Maryland; they have seen over 1300 exstrophy patients in the past 50 years.[7]
Upon delivery, the exposed bladder is irrigated and a non-adherent film is placed to prevent as much contact with the external environment as possible. In the event the child was not born at a medical center with an appropriate exstrophy support team then transfer will likely follow. Upon transfer, or for those infants born at a medical center able to care for bladder exstrophy, imaging may take place in the first few hours of life prior to the child undergoing surgery.[3]
Primary (immediate) closure is indicated only in those patients with a bladder of appropriate size, elasticity, and contractility as those patients are most likely to develop a bladder of adequate capacity after early surgical intervention.[8]
Conditions that are absolute contraindications despite bladder adequacy include duplication of the penis or scrotum and significant bilateral hydronephrosis.[9]
Surgery
[edit]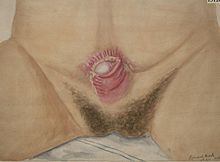
Modern therapy is aimed at surgical reconstruction of the bladder and genitalia. Both males and females are born with this anomaly. Treatment is similar.
In males treatments have been: In the modern staged repair of exstrophy (MSRE) the initial step is closure of the abdominal wall, often requiring a pelvic osteotomy. This leaves the patient with penile epispadias and urinary incontinence. At approximately 2–3 years of age, the patient then undergoes repair of the epispadias after testosterone stimulation. Finally, bladder neck repair usually occurs around the age of 4–5 years, though this is dependent upon a bladder with adequate capacity and, most importantly, an indication that the child is interested in becoming continent. In some of the bladder reconstructions, the bladder is augmented with the addition of a segment of the large intestines to increase the volume capacity of the reconstructed bladder.[citation needed] In the complete primary repair of exstrophy (CPRE) the bladder closure is combined with an epispadias repair, in an effort to decrease costs and morbidity.[10] This technique has, however, led to significant loss of penile and corporal tissue, particularly in younger patients.[11]
In females treatment has included: Surgical reconstruction of the clitoris, which is separated into two distinct bodies. Surgical reconstruction to correct the split of the mons, redefine the structure of the bladder neck and urethra. Vaginoplasty will correct the anteriorly displaced vagina. If the anus is involved, it is also repaired. Fertility remains and women who were born with bladder exstrophy usually develop prolapse due to the weaker muscles of the pelvic floor.[12]
Bladder exstrophy males reassigned and raised as females
[edit]Between 1960 and 2000,[13] doctors believed XY males with cloacal exstrophy (the most extreme form of bladder exstrophy) would be happier socially as females, and surgically reassigned them. This occurred under the belief that humans were born psychosexually neutral. The practice proved controversial, after follow-ups by William Reiner[14] found that many struggled to adhere to a female gender identity, had masculine interests, were attracted to females, or reverted to the male sex spontaneously or upon learning they were genetic males.[15]
According to J. Michael Bailey:[15]
Reiner thinks that all the cloacal cases born as boys would be happier as boys rather than girls, because their brains have been biologically prepared for the male role. He thinks that those who remain girls are at best missing out, and at worst are experiencing great inner torment. He thinks their parents should tell them and, essentially, let them choose their sex.
In terms of their sexual orientations, a 2016 academic review by J. Michael Bailey found 7 published cases of boys reassigned female at birth and raised as girls, of which 5 were cloacal exstrophy cases. All were strongly attracted to females.[13] According a 2015 article in The Boston Globe, Wiliam Reiner has followed up on the sexual orientations of approximately 70 genetic males who were raised as females. Only one reported having sexual attractions to males, "I’m more convinced than ever that sexual orientation is built in... certainly for males" he said.[16] A 2023 review by Swift-Gallant et al. also cited two additional cases from media reports, both of whom were gynephilic.[17]
Reiner's results have caused some doctors to reconsider the practice of sex reassigning genetic males.[15] A 2011 study found that 79% of paediatric urologists surveyed favoured male assignment for genetic males with cloacal exstrophy.[18]
Cases in the media
[edit]- Joe Holliday. British cloacal exstrophy male who was raised female. Masculine interests and attracted to females. Found out born male at age 25, and reverted to male sex.[19][17]
- Sophie Ottaway. British cloacal exstrophy male raised as a female. Found out about birth sex at age 22. Retained female identity, although believes the reassignment was incorrect. Attracted to women.[20][17]
Prognosis
[edit]The most important criterion for improving long-term prognosis is success of the initial closure.[21][22] If a patient requires more than one closure their chance of continence drops off precipitously with each additional closure - at just two closures the chance of voiding continence is just 17%.[23]
Even with successful surgery, people may have long-term complications.[24] Some of the most common include:
Epidemiology
[edit]Occurring at a rate between 1 in 10,000 to 1 in 50,000 [25] with a male-to-female ratio of 2.3–6:1,[26][27][28] bladder exstrophy is relatively rare. For those individuals with bladder exstrophy who maintain their ability to reproduce, the risk of bladder exstrophy in their children is approximately 500-fold greater than the general population.[26]
References
[edit]- ^ Muecke EC: The role of the cloacal membrane in exstrophy: the first successful experimental study. J Urol 1964; 92:659.
- ^ Larsen WJ (2001). Human embryology (3rd ed.). Philadelphia, Pa.: Churchill Livingstone. p. 275. ISBN 0-443-06583-7.
- ^ a b Gearhart JP, Mathews R (2011). "Chapter 124: Exstrophy-epispadias complex". In Wein AJ (ed.). Campbell-Walsh Urology (10th ed.). Philadelphia, Pa: Saunders Elsevier.
- ^ a b Anand S, Lotfollahzadeh S (2022). "Bladder Exstrophy". National Center for Biotechnology Information, U.S. National Library of Medicine. PMID 33085303. Archived from the original on 25 October 2023. Retrieved 25 July 2021.
- ^ Gearhart JP, Ben-Chaim J, Jeffs RD, Sanders RC (June 1995). "Criteria for the prenatal diagnosis of classic bladder exstrophy". Obstetrics and Gynecology. 85 (6): 961–4. doi:10.1016/0029-7844(95)00069-4. PMID 7770267. S2CID 2096064.
- ^ Nelson CP, Dunn RL, Wei JT, Gearhart JP (September 2005). "Surgical repair of bladder exstrophy in the modern era: contemporary practice patterns and the role of hospital case volume". The Journal of Urology. 174 (3): 1099–102. doi:10.1097/01.ju.0000169132.14799.33. PMID 16094068.
- ^ Kasprenski M, Benz K, Maruf M, Jayman J, Di Carlo H, Gearhart J (March 2020). "Modern Management of the Failed Bladder Exstrophy Closure: A 50-yr Experience". European Urology Focus. 6 (2): 383–389. doi:10.1016/j.euf.2018.09.008. PMID 30292419. S2CID 52926501.
- ^ Gearhart JP, Jeffs RD (1998). "The bladder exstrophy-epispadias complex". In Walsh PC (ed.). Campbell's urology (7th ed.). Philadelphia: WB Saunders. p. 1939.
- ^ "Hydronephrosis". The Lecturio Medical Concept Library. Archived from the original on 25 July 2021. Retrieved 25 July 2021.
- ^ Grady RW, Mitchell ME (October 1999). "Complete primary repair of exstrophy". The Journal of Urology. 162 (4): 1415–20. doi:10.1016/S0022-5347(05)68327-9. PMID 10492227.
- ^ Husmann DA, Gearhart JP (October 2004). "Loss of the penile glans and/or corpora following primary repair of bladder exstrophy using the complete penile disassembly technique". The Journal of Urology. 172 (4 Pt 2): 1696–700, discussion 1700–1. doi:10.1097/01.ju.0000138675.16931.cb. PMID 15371793.
- ^ Moliterno D (2013). Therapeutic advances in thrombosis. Chichester, West Sussex: Wiley-Blackwell. pp. 779–798. ISBN 9781405196253.
- ^ a b Bailey JM, Vasey PL, Diamond LM, Breedlove SM, Vilain E, Epprecht M (September 2016). "Sexual Orientation, Controversy, and Science". Psychological Science in the Public Interest. 17 (2): 45–101. doi:10.1177/1529100616637616. PMID 27113562.
- ^ Reiner WG, Gearhart JP (January 2004). "Discordant sexual identity in some genetic males with cloacal exstrophy assigned to female sex at birth". The New England Journal of Medicine. 350 (4): 333–341. doi:10.1056/NEJMoa022236. PMC 1421517. PMID 14736925.
- ^ a b c Bailey JM (2003). The Man Who Would Be Queen (PDF). Joseph Henry Press. pp. 48–52. ISBN 978-0309084185.
- ^ Swidey N (23 August 2015). "What makes people gay? (An update)". The Boston Globe.
- ^ a b c Swift-Gallant A, Aung T, Rosenfield K, Dawood K, Puts D (2023-09-20). "Organizational Effects of Gonadal Hormones on Human Sexual Orientation". Adaptive Human Behavior and Physiology. 9 (4): 347. doi:10.1007/s40750-023-00226-x. ISSN 2198-7335 – via Springer.
- ^ Diamond DA, Burns JP, Huang L, Rosoklija I, Retik AB (October 2011). "Gender assignment for newborns with 46XY cloacal exstrophy: a 6-year followup survey of pediatric urologists". The Journal of Urology. 186 (4 Suppl): 1642–1648. doi:10.1016/j.juro.2011.03.101. PMID 21862059.
- ^ Chapman N (10 August 2015). "Joe (27) was raised a female on medical advice. He feels his identity was stolen as a baby and wants it back". The Voice of Spalding and South Holland.
- ^ Calkin J (2023-08-25). "'The doctors changed my gender at two days old – 22 years later, I discovered the truth'". The Telegraph. ISSN 0307-1235. Retrieved 2024-06-03.
- ^ Oesterling JE, Jeffs RD (February 1987). "The importance of a successful initial bladder closure in the surgical management of classical bladder exstrophy: analysis of 144 patients treated at the Johns Hopkins Hospital between 1975 and 1985". The Journal of Urology. 137 (2): 258–62. doi:10.1016/s0022-5347(17)43972-3. PMID 3806816.
- ^ Husmann DA, McLorie GA, Churchill BM (August 1989). "Closure of the exstrophic bladder: an evaluation of the factors leading to its success and its importance on urinary continence". The Journal of Urology. 142 (2 Pt 2): 522–4, discussion 542–3. doi:10.1016/s0022-5347(17)38803-1. PMID 2746771.
- ^ Novak TE, Costello JP, Orosco R, Sponseller PD, Mack E, Gearhart JP (August 2010). "Failed exstrophy closure: management and outcome". Journal of Pediatric Urology. 6 (4): 381–4. doi:10.1016/j.jpurol.2009.10.009. PMID 19906564.
- ^ Gargollo PC, Borer JG (2007). "Contemporary outcomes in bladder exstrophy". Current Opinion in Urology. 17 (4): 272–80. doi:10.1097/MOU.0b013e3281ddb32f. PMID 17558272. S2CID 6290323.
- ^ Lattimer JK, Smith MJK: Exstrophy closure: a follow up on 70 cases. J Urol 1966; 95:356.
- ^ a b Shapiro E, Jeffs RD, Gearhart JP, Lepor H (August 1985). "Muscarinic cholinergic receptors in bladder exstrophy: insights into surgical management". The Journal of Urology. 134 (2): 308–10. doi:10.1016/s0022-5347(17)47139-4. PMID 4020984.
- ^ Ives E, Coffey R, Carter CO (April 1980). "A family study of bladder exstrophy". Journal of Medical Genetics. 17 (2): 139–41. doi:10.1136/jmg.17.2.139. PMC 1048521. PMID 7381870.
- ^ Lancaster PA (1987). "Epidemiology of bladder exstrophy: a communication from the International Clearinghouse for Birth Defects monitoring systems". Teratology. 36 (2): 221–227. doi:10.1002/tera.1420360210. PMID 3424208.
