Urushiol-induced contact dermatitis
| Urushiol-induced contact dermatitis | |
|---|---|
 | |
| Specialty | Dermatology |
| Symptoms | rashes, itching, inflammation, oozing, and, in severe cases, a burning sensation. |
| Causes | urushiol contact |
Urushiol-induced contact dermatitis (also called Toxicodendron dermatitis or Rhus dermatitis) is a type of allergic contact dermatitis caused by the oil urushiol found in various plants, most notably sumac family species of the genus Toxicodendron: poison ivy, poison oak, poison sumac, and the Chinese lacquer tree.[1] The name is derived from the Japanese word for the sap of the Chinese lacquer tree, urushi. Other plants in the sumac family (including mango, pistachio, the Burmese lacquer tree, the India marking nut tree, and the cashew) also contain urushiol,[2] as do unrelated plants such as Ginkgo biloba.[3]
As is the case with all contact dermatitis, urushiol-induced allergic rashes are a Type IV hypersensitivity reaction, also known as delayed-type hypersensitivity. Symptoms include itching, inflammation, oozing, and, in severe cases, a burning sensation.
The American Academy of Dermatology estimates that there are up to 50 million cases of urushiol-induced dermatitis annually in the United States alone, accounting for 10% of all lost-time injuries in the United States Forest Service. Poison oak is a significant problem in the rural Western and Southern United States, while poison ivy is most rampant in the Eastern United States. Dermatitis from poison sumac is less common.
Signs and symptoms
[edit]Urushiol causes an eczematous contact dermatitis characterized by redness, swelling, papules, vesicles, blisters, and streaking.[4][5] People vary greatly in their sensitivity to urushiol. In approximately 15%[6] to 30%[7] of people, urushiol does not trigger an immune system response, while at least 25% of people have a very strong immune response resulting in severe symptoms.[citation needed]
The rash takes one to two weeks to run its course and may cause scars, depending on the severity of the exposure.[4] Severe cases involve small (1–2 mm), clear, fluid-filled blisters on the skin. Pus-filled vesicles containing a whitish fluid may indicate an infection. Most poison ivy rashes, without infections, will resolve within 14 days without treatment. Excessive scratching may result in infection, commonly by staphylococcal and streptococcal species; these may require antibiotics.
-
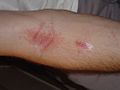
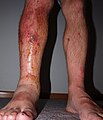
Severe allergic reaction to urushiol (poison oak) 4 days after exposure.
-
Blistering 48 hours after urushiol contact.
-
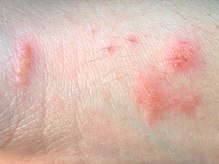
Poison ivy rash after 2 days.
-
Poison ivy rash with swelling about 3 days after direct contact.
Cause
[edit]
Urushiol-induced contact dermatitis is caused by contact with a plant or any other object containing urushiol oil.[1] The oil adheres to almost anything with which it comes in contact, such as towels, blankets, clothing, and landscaping tools.[4] Clothing or other materials that touch the plant and then, before being washed, touch the skin are common causes of exposure.[4]
For people who have never been exposed or are not yet allergic to urushiol, it may take 10 to 21 days for a reaction to occur the first time. Once allergic to urushiol, however, most people break out 48 to 72 hours after contact with the oil. Typically, individuals have been exposed at least once, if not several times, before they develop a rash.[8] The rash typically persists one to two weeks, but in some cases may last up to five weeks.
Urushiol is primarily found in the spaces between cells beneath the outer skin of the plant, so the effects are less severe if the plant tissue remains undamaged on contact. Once the oil and resin are thoroughly washed from the skin, the rash is not contagious. Urushiol does not always spread once it has bonded with the skin, and cannot be transferred once the urushiol has been washed away.
Although simple skin exposure is most common, ingestion of urushiol can lead to serious, systemic reactions. Burning plant material is commonly said to create urushiol-laden smoke that causes a systemic reaction, as well as a rash in the throat and eyes. Firefighters often get rashes and eye inflammation from smoke-related contact.[9] A high-temperature bonfire may incinerate urushiol before it can cause harm, while a smoldering fire may vaporize the volatile oil and spread it as white smoke. However, some sources dispute the danger of burning urushiol-containing plant material.[10]
Mechanism
[edit]Urushiol is fat-soluble, penetrating the stratum corneum of the skin, then binding to Langerhans cells in the epidermis.[1] The affected cells then migrate to lymph nodes, where T cells become activated, then return to the skin where they stimulate an urushiol-activated dermatitis.[1] The toxic effect is indirect, mediated by an induced immune response.[1] The oxidized urushiols act as haptens, chemically reacting with, binding to, and changing the shape of integral membrane proteins on exposed skin cells.[1] Urushiols are oxidized in vivo, generating a quinone form of the molecules.[11]
Affected proteins interfere with immune system ability to recognize these cells as normal parts of the body, causing a T-cell-mediated immune response.[12] This response is directed at the complex of urushiol derivatives (namely, pentadecacatechol) bound in the skin proteins, attacking the cells as if they were foreign bodies.
Treatments
[edit]Treatment consists of two phases: stopping the urushiol contact that is causing the reaction (this must be done within minutes)[13] and, later, reducing the pain and itching.[4]
Primary treatment involves washing exposed skin thoroughly with soap, cool water, and friction as soon as possible after exposure is discovered.[4] Soap or detergent is necessary because urushiol is an oil; friction, with a washcloth or something similar, is necessary because urushiol adheres strongly to the skin.[4]Commercial removal preparations, which are available in areas where poison ivy grows, usually contain surfactants, such as the nonionic detergent Triton X-100, to solubilize urushiol; some products also contain abrasives.
The U.S. Food and Drug Administration recommends applying a wet compress or soaking the affected area in cool water; topical corticosteroids (available over-the-counter) or oral corticosteroids (available by prescription); and topical skin protectants, such as zinc acetate, zinc carbonate, zinc oxide, and calamine. Baking soda or colloidal oatmeal can relieve minor irritation and itching. Aluminium triacetate, sometimes known as Burow's solution, can also ease the rash.[14]
Showers or compresses using hot (but not scalding) water can relieve itching for up to several hours, though this "also taxes the skin's integrity, opening pores and generally making it more vulnerable", and is only useful for secondary treatment (not for cleaning urushiol from the skin, which should be done with cold water).[15] People who have had a prior systemic reaction may be able to prevent subsequent exposure from turning systemic by avoiding heat and excitation of the circulatory system and applying moderate cold to any infected skin with biting pain.
In cases of extreme symptoms, steroids such as prednisone, triamcinolone, or dexamethasone are sometimes administered to attenuate the immune response and prevent long-term skin damage, especially if the eyes are involved. Prednisone is the most commonly prescribed systemic treatment but can cause serious adrenal suppression, so it must be taken carefully and tapered off slowly.[16] If bacterial secondary infection of affected areas occurs, antibiotics may also be necessary.
Scrubbing with plain soap and cold water will remove urushiol from skin if it is done within a few minutes of exposure.[4][13]
Further observations
[edit]- Ordinary laundering with laundry detergent will remove urushiol from most clothing.[4]
- Urushiol may adhere to pet fur.[4]
- Urushiol oil left on clothing and surfaces can be deactivated using bleach.[17]
- The fluid from the resulting blisters does not spread urushiol to others.[18][14]
- Blisters should be left unbroken during healing.[19]
- Poison ivy and poison oak are still harmful when the leaves have fallen off, as the toxic residue is persistent, and exposure to any parts of plants containing urushiol can cause a rash at any time of the year.[13]
- Ice, cold water, cooling lotions, and cold air do not help cure poison ivy rashes, but cooling can reduce inflammation and soothe the itch.
- Results for jewelweed as a natural agent for treatment are conflicting. Some studies indicate that it "failed to decrease symptoms of poison ivy dermatitis" [1980] and had "no prophylactic effect" [1997].[20] The juice of the leaves and stems of Impatiens capensis is a traditional Native American remedy for skin rashes, including poison ivy.[21]
Prevention
[edit]A rarely cited double-blind study in 1982 reported that a course of oral urushiol usually hyposensitized subjects, with the principal side effect, pruritus ani, being reported by 85% of the participants who ingested the urushiol.[22]
Research conducted on urushiol by Mahmoud ElSohly led to the development of PDC-APB, a candidate for a vaccine against skin irritation from poison ivy.[23]
See also
[edit]References
[edit]- ^ a b c d e f "Urushiol". PubChem. US National Library of Medicine. 1 January 2022. Retrieved 4 January 2022.
- ^ Gross M, Baer H, Fales HM (1975). "Urushiols of poisonous anacardiaceae". Phytochemistry. 14 (10): 2263–2266. doi:10.1016/S0031-9422(00)91113-0.
- ^ Lepoittevin JP, Benezra C, Asakawa Y (1989). "Allergic contact dermatitis to Ginkgo biloba L.: relationship with urushiol". Archives of Dermatological Research. 281 (4): 227–30. doi:10.1007/BF00431055. PMID 2774654. S2CID 24855206.
- ^ a b c d e f g h i j "Poison ivy rash". Mayo Clinic. 17 October 2020. Retrieved 4 January 2022.
- ^ DermAtlas -1892628434
- ^ Wilson S (2005-09-23). "Howstuffworks "How Poison Ivy Works"". Science.howstuffworks.com. Retrieved 2010-06-04.
- ^ Rohde M. "Contact-Poisonous Plants of the World". Mic-ro.com. Archived from the original on 2010-07-02. Retrieved 2010-06-04.
- ^ Ray T. "Poison Ivy: The Most Common of Allergens". University of Iowa Health Care. Archived from the original on 12 January 2016. Retrieved 30 October 2015.
- ^ "Firefighters Battle Hidden Dangers This Wildfire Season: Poison Oak, Ivy And Sumac Plants Top Cause Of Disability, Sick Time". FireEngineering. Fireengineering.com. 26 July 2005. Archived from the original on 2021-10-20. Retrieved 2015-10-06.
- ^ Frohne D, Pfander HJ (1984). A Colour Atlas of Poisonous Plants: A Handbook for Pharmacists, Doctors, Toxicologists, and Biologists. Wolfe Publishing Ltd. p. 291 pp. ISBN 978-0-7234-0839-0.
- ^ Kalergis AM, López CB, Becker MI, Díaz MI, Sein J, Garbarino JA, De Ioannes AE (January 1997). "Modulation of fatty acid oxidation alters contact hypersensitivity to urushiols: role of aliphatic chain beta-oxidation in processing and activation of urushiols". The Journal of Investigative Dermatology. 108 (1): 57–61. doi:10.1111/1523-1747.ep12285632. PMID 8980288.
- ^ Hogan CM (2008). "Western poison-oak: Toxicodendron diversilobum". GlobalTwitcher. Archived from the original on 2009-07-21. Retrieved 2010-04-21.
- ^ a b c Einsig B (May 2002). "Poison Ivy Myth: Science, Environment and Ecology Flash for Educators". Keystone Outdoors Magazine (341). Penn State Integrated Pest Management. Archived from the original on 25 July 2017. Retrieved 7 October 2015.
- ^ a b "Outsmarting Poison Ivy and Other Poisonous Plants". Food and Drug Administration. Archived from the original on July 16, 2010. Retrieved December 16, 2019.
- ^ Hauser SC, Epstein WL (2008). A Field Guide to Poison Ivy, Poison Oak, and Poison Sumac. Globe Pequot. p. 60. ISBN 978-0-7627-4741-2. Retrieved 2010-11-21.[permanent dead link]
- ^ "Poison Ivy, Oak, and Sumac". Surviveoutdoors.com. Archived from the original on 2010-06-12. Retrieved 2010-06-04.
- ^ Chastant LR, Davis T, Libow L (March 2018). "Black-spot poison ivy, a report of 3 cases with clinicopathologic correlation". JAAD Case Reports. 4 (2): 140–142. doi:10.1016/j.jdcr.2017.09.035. PMC 5789763. PMID 29387766.
- ^ "Poison ivy, oak, and sumac". American Academy of Dermatology. Archived from the original on 9 March 2012.
- ^ "Poison Ivy, Oak and Sumac". OutDoorPlaces.com. Archived from the original on 18 October 2010. Retrieved 22 September 2010.
- ^ Shenefelt PD (2011). "Herbal Treatment for Dermatologic Disorders". Herbal Medicine. Oxidative Stress and Disease. Vol. 20115386 (2nd ed.). Boca Raton, Florida, USA: CRC Press. pp. 383–403. doi:10.1201/b10787-19 (inactive 2024-11-12). ISBN 978-1-4398-0713-2. PMID 22593930. Retrieved October 5, 2015.
{{cite book}}:|journal=ignored (help)CS1 maint: DOI inactive as of November 2024 (link) - ^ Smith HH (1933). "Ethnobotany of the Forest Potawatomi Indians". Bulletin of the Public Museum of the City of Milwaukee. 7: 1-230 (42).
- ^ Epstein WL, Byers VS, Frankart W (September 1982). "Induction of antigen specific hyposensitization to poison oak in sensitized adults". Archives of Dermatology. 118 (9): 630–633. doi:10.1001/archderm.1982.01650210010008. PMID 06180687.
- ^ Niemeyer, Kenneth (10 July 2019). "Poison ivy vaccine making progress, still years away". The Daily Mississippian. Retrieved 27 July 2022.
External links
[edit] Media related to Urushiol-induced contact dermatitis at Wikimedia Commons
Media related to Urushiol-induced contact dermatitis at Wikimedia Commons