Pheochromocytoma
| Pheochromocytoma | |
|---|---|
| Other names | Phaeochromocytoma |
 | |
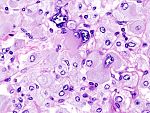
| High magnification micrograph of a pheochromocytoma, showing the nested arrangement of cells (Zellballen) and stippled chromatin. H&E stain. | |
| Specialty | Oncology |
Pheochromocytomas (PH or PCC) are rare tumors arising from chromaffin cells of the adrenal medulla.[1] They make, store, metabolize and usually but not always release catecholamines. Extra-adrenal paragangliomas (often described as extra-adrenal pheochromocytomas) are closely related, though less common, tumors that originate in the ganglia of the sympathetic nervous system and are named based upon the primary anatomical site of origin. The term is from the Greek phaios (dark), chroma (color), kytos (cell), and -oma (tumor).
Signs and symptoms
The signs and symptoms of a pheochromocytoma are those of sympathetic nervous system hyperactivity,[2] with three classic signs: diaphoresis (excessive sweating), headaches and elevated heart rate, including:
- Skin sensations
- Flank pain
- Elevated blood pressure, including paroxysmal (sporadic, episodic) high blood pressure, which sometimes can be more difficult to detect; another clue to the presence of pheochromocytoma is orthostatic hypotension (a fall in systolic blood pressure greater than 20 mmHg or a fall in diastolic blood pressure greater than 10 mmHg upon standing)
- Anxiety often resembling that of a panic attack
- Pallor
- Weight loss
- Localized amyloid deposits found microscopically
- Elevated blood glucose level (due primarily to catecholamine stimulation of lipolysis (breakdown of stored fat) leading to high levels of free fatty acids and the subsequent inhibition of glucose uptake by muscle cells. Further, stimulation of beta-adrenergic receptors leads to glycogenolysis and gluconeogenesis and thus elevation of blood glucose levels).
A pheochromocytoma can also cause resistant arterial hypertension. A pheochromocytoma can be fatal if it causes a hypertensive emergency, that is, severely high blood pressure that impairs one or more organ systems (formerly called "malignant hypertension"). This hypertension is not well controlled with standard blood pressure medications.
Tumors may grow large, but most are smaller than 10 centimetres (4 in).
Pheochromocytoma crisis is a rare and potentially lifethreatening emergency. It can occur spontaneously or be precipitated by administration of pharmacological agents, tumor manipulation, micturition (urinary bladder pheochromocytoma), or foods that aggravate release of catecholamines by the tumor.[3]
Complications
The massive release of catecholamines in pheochromocytoma can cause damage to heart cells.[4] This damage may be due to either compromising the coronary microcirculation or by direct toxic effects on the heart cells.[4]
A common clinical presentation of pheochromocytoma includes hypertension, due to increased total peripheral resistance. Most pheochromocytomas secrete norepinephrine, which is a vasoconstrictor via α-adrenergic receptor stimulation, however research has yet to significantly correlate the increase in peripheral resistance with increased circulating norepinephrine. Theories behind the inability to correlate the two variables include simultaneous dopamine release, which has the opposing effect of norepinephrine in terms of vasodilation. Other mechanisms propose the down-regulation of α-adrenergic receptors or the release of other hormones that have opposing effects to norepinephrine. Due to increased catecholamine production, cardiovascular complications upon presentation and throughout the course of the disease are common. Complications that arise from these cardiovascular disturbances include blood pressure changes as well as possible sudden death, heart attack despite no prior history, noncardiogenic pulmonary shock/edema, and arrhythmias.
Pheochromocytoma is also capable of causing, at presentation, pseudo-obstruction of bowels, diabetic ketoacidosis, or multisystem crisis involving lactic acidosis. These symptoms may be in part due to the co-secretion of other hormones associated with norepinephrine, such as corticotropin-releasing hormone, adrenocorticotropin, and interleukin six.
Pheochromocytoma may go undiagnosed or undetected for multiple reasons. The main reason is the fact that the tumors are rare. Hypertension may not clinically present itself right away due to the fact that catecholamines can convert into their biologically inactive forms in the tumor, suppressing symptoms. Lastly, the symptoms of the disease are non-specific and common to stress neuronal release of catecholamines. Lag in diagnosis averages about three years. Presymptomatic diagnosis is most possible in patients with germ-line inheritance.
Cause
The hereditary implications of pheochromocytoma are still being investigated, however, genes have been identified as genomic biomarkers to aid in the identification of inherited disease. Of these genes studied, the most well-known include VHL, RET, and NF1 of neurofibromatosis type I. Aberrations of these genes are associated with bilateral disease.
The RET protein is a tyrosine kinase receptor that plays an integral role in development of sympathetic neurons [2]. Mutations in the gene via germ-line (MEN-2) or somatic acquisition activate multiple signaling pathways involved in PCC, as well as other neuroendocrine tumors in humans. MEN-2 generally results from a gain-of-function variant of this RET gene, and MEN-2 is commonly associated with pheochromocytoma and amyloid producing medullary thyroid carcinoma.
Mutations in two subunits of the succinate dehydrogenase gene, SDHB and SDHD, have been strongly associated with cancer presenting at a younger age as well as extra-adrenal location, multiple tumors/metastasis, and poor prognosis.
Pheochromocytoma linked to MEN II can be caused by RET oncogene mutations. Both syndromes are characterized by pheochromocytoma as well as thyroid cancer (thyroid medullary carcinoma). MEN IIA also presents with hyperparathyroidism, while MEN IIB also presents with mucosal neuroma.
Diagnosis


The diagnosis can be established by measuring catecholamines and metanephrines in plasma (blood) or through a 24-hour urine collection. Care should be taken to rule out other causes of adrenergic (adrenaline-like) excess like hypoglycemia, stress, exercise, and drugs affecting the catecholamines like stimulants, methyldopa, dopamine agonists, or ganglion blocking antihypertensives. Various foodstuffs (e.g. coffee, tea, bananas, chocolate, cocoa, citrus fruits, and vanilla) can also affect the levels of urinary metanephrine and VMA (vanillylmandelic acid).[5]
Imaging by computed tomography or a T2 weighted MRI of the head, neck, and chest, and abdomen can help localize the tumor. Tumors can also be located using an MIBG scan, which is scintigraphy using iodine-123-marked metaiodobenzylguanidine. Even finer localization can be obtained in certain PET scan centers using PET-CT or PET-MRI with [18F] fluorodopamine[6] or FDOPA.[7]
Pheochromocytomas occur most often during young-adult to mid-adult life.
These tumors can form a pattern with other endocrine gland cancers which is labeled multiple endocrine neoplasia (MEN). Pheochromocytoma may occur in patients with MEN 2 and MEN 3 (MEN 2B). Von Hippel Lindau patients may also develop these tumors.[8]
Patients experiencing symptoms associated with pheochromocytoma should be aware that it is rare. However, it often goes undiagnosed until autopsy; therefore patients might wisely choose to take steps to provide a physician with important clues, such as recording whether blood pressure changes significantly during episodes of apparent anxiety.
Testing
Testing prior to tumor excision helps ascertain whether the tumor is a singular tumor or if there are multiple, if it is ectopic or adrenal originating, malignant or benign, and isolated or present with other tumors in context of inherited disease. CT is the most commonly used imaging technique, however MRI is preferred. MIBG scanning should be used when possible, as it is the most accurate way to locate cancer in catecholamine producing cancers, as catecholamine plasma membrane and vesicular transport systems are especially abundant in pheochromocytoma cells. Imaging using MIBG would yield specific and sensitive results compared to CT and MRI, as the latter two are non-specific generalized imaging techniques


- Blood tests: Buters and others have suggested that analysis of free metanephrines (metadrenalines) (normetanephrine and metanephrine) in blood plasma is the most accurate test for detecting pheochromocytoma.
- Urine tests: Although this test is slightly less effective than plasma testing it is still considered highly effective in diagnosis. Usually the metabolites of norepinephrine and epinephrine, normetanephrine (NMN) and metanephrine (MN), are found in relatively small amounts in normal humans. The increased excretion of these metabolites is indicative of the disease, but does not completely rule out other diseases which may cause the same excretion values.
- Other Tests:
- One diagnostic test used in the past for a pheochromocytoma is to administer clonidine, a centrally-acting alpha-2 agonist used to treat high blood pressure. Clonidine mimics catecholamines in the brain, causing it to reduce the activity of the sympathetic nerves controlling the adrenal medulla. A healthy adrenal medulla will respond to the clonidine suppression test by reducing catecholamine production; the lack of a response is evidence of pheochromocytoma.
- Chromogranin A is elevated in case of pheochromocytoma.[9]
-
Micrograph of pheochromocytoma.
-
Micrograph of pheochromocytoma.
-
Micrograph of pheochromocytoma.
-
Bilateral pheochromocytoma in MEN2.
-
Pheochromocytoma. CT abdomen.
-
Pheochromocytoma. CT abdomen.
Tumor location
In adults, approximately 80% of pheochromocytomas are unilateral and solitary, 10% are bilateral, and 10% are extra-adrenal. In children, a quarter of tumors are bilateral, and an additional quarter are extra-adrenal. Solitary lesions inexplicably favor the right side. Although pheochromocytomas may grow to large size (>3 kg), most weigh <100 g and are <10 cm in diameter. Pheochromocytomas are highly vascular.
The tumors are made up of large, polyhedral, pleomorphic chromaffin cells. Fewer than 10% of these tumors are malignant. As with several other endocrine tumors, malignancy cannot be determined from the histologic appearance; tumors that contain large number of aneuploid or tetraploid cells, as determined by flow cytometry, are more likely to recur. Local invasion of surrounding tissues or distant metastases indicate malignancy.
Extra-adrenal pheochromocytomas: Extra-adrenal pheochromocytomas usually weigh 20 to 40 g and are <5 cm in diameter. Most are located within the abdomen in association with the celiac, superior mesenteric, and inferior mesenteric ganglia and the organ of Zuckerkandl. Approximately 10% are in the thorax, 1% are within the urinary bladder, and less than 3% are in the neck, usually in association with the sympathetic ganglia or the extracranial branches of the ninth cranial nerves.
Pheochromocytomatosis: Pheochromocytomatosis is defined as a multifocal cell dissemination limited to the operatively opened space with no signs of distant metastasis. After primary adrenalectomy due to a pheochromocytoma this is a rare and underrecognized manifestation of a tumor recurrence[10]. Its treament is complete surgical cytoreduction[11].
Differential diagnosis
The differential diagnoses of pheochromocytoma include:
- Anxiety disorders, including Benzodiazepine withdrawal syndrome
- Paragangliomas
- Von Hippel–Lindau Disease
- Essential hypertension
- Hyperthyroidism
- Insulinoma
- Mercury poisoning
- Paroxysmal supraventricular tachycardia
- Renovascular hypertension
- Carcinoid[12]
Treatment
Surgical resection of the tumor is the treatment of first choice, either by open laparotomy or laparoscopy.[13] Given the complexity of perioperative management, and the potential for catastrophic intra and postoperative complications, such surgery should be performed only at centers experienced in the management of this disorder. In addition to the surgical expertise that such centers can provide, they will also have the necessary endocrine and anesthesia resources. It may also be necessary to carry out adrenalectomy, a complete surgical removal of the affected adrenal gland(s).
Either surgical option requires prior treatment with the non-specific and irreversible alpha adrenoceptor blocker phenoxybenzamine or a short-acting alpha antagonist (e.g. prazosin, terazosin, or doxazosin).[14] Doing so permits the surgery to proceed while minimizing the likelihood of severe intraoperative hypertension (as might occur when the tumor is manipulated). Some authorities would recommend that a combined alpha/beta blocker such as labetalol also be given in order to slow the heart rate. Regardless, a nonselective beta-adrenergic receptor blocker such as propranolol must never be used, without adequate alpha blockade, in the presence of a pheochromocytoma. The mechanism for β-adrenoceptor blocker-associated adverse events is generally ascribed to inhibition of β2-adrenoceptor-mediated vasodilatation, leaving α1-adrenoceptor-mediated vasoconstrictor responses to catecholamines unopposed and, thus, severe and potentially refractory hypertension. However some clinical guidelines permit beta-1 blockade use together with alpha blockers during surgery for control of tachycardia.
The patient with pheochromocytoma is invariably volume depleted. In other words, the chronically elevated adrenergic state characteristic of an untreated pheochromocytoma leads to near-total inhibition of renin-angiotensin activity, resulting in excessive fluid loss in the urine and thus reduced blood volume. Hence, once the pheochromocytoma has been resected, thereby removing the major source of circulating catecholamines, a situation arises where there is both very low sympathetic activity and volume depletion. This can result in profound hypotension. Therefore, it is usually advised to "salt load" pheochromocytoma patients before their surgery. This may consist of simple interventions such as consumption of high salt food pre-operatively, direct salt replacement or through the administration of intravenous saline solution.
Prognosis
There is increased life-time risk of secondary cancers (relative risk 3.63), with a slightly increased mortality risk (1.21) according to a 2004 Swedish study of 481 patients.[15]
Epidemiology
Pheochromocytoma is seen in between two and eight in 1,000,000, with approximately 1000 cases diagnosed in United States yearly. It mostly occurs in young or middle age adults, though it presents earlier in hereditary cases.
- About 10% of adrenal cases are bilateral (suggesting hereditary disease)
- About 10% of adrenal cases occur in children (also suggesting hereditary disease)
- About 15% are extra-adrenal (located in any orthosympathetic tissue): Of these 9% are in the abdomen, and 1% are located elsewhere. Some extra-adrenal pheochromocytomas are probably actually paragangliomas, but the distinction can only be drawn after surgical resection.
- About 11.1% of adrenal cases are malignant, but this rises to 30% for extra-adrenal cases
- About 15–20% are hereditary[16]
- About 5% are caused by VHL disease
- About 3% recur after being resected
- About 14% of affected individuals do not have arterial hypertension (Campbell's Urology)
History
Charles Surgue of Cork (1775-1816). In 1886, Felix Fränkel made the first description of a patient with pheochromocytoma. The term "pheochromocytoma" was first coined by Ludwig Pick, a pathologist, in 1912. In 1926, César Roux (in Switzerland) and Charles Horace Mayo (in the US) were the first surgeons to successfully remove pheochromocytomas.
In the 1970s, Greene and Tischler derived a line of cells, called the PC12 cell line, from a rat pheochromocytoma.[17]
References
- ^ "Pheochromocytoma: An approach to diagnosis". Best Pract Res Clin Endocrinol Metab.: 101346. 2019. doi:10.1016/j.beem.2019.101346. PMID 31708376.
{{cite journal}}: Unknown parameter|authors=ignored (help) - ^ "Pheochromocytoma: Symptoms, Treatment, Diagnosis, Test". medicinenet.com. Archived from the original on 16 July 2017. Retrieved 4 May 2018.
- ^ Hosseinnezhad A, Black RM, Aeddula NR, Adhikari D, Trivedi N (2011). "Glucagon-induced pheochromocytoma crisis". Endocr Pract. 17: e51–54. doi:10.4158/EP10388.CR. PMID 21324811.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ a b Goldman 2011, p. 327
- ^ "Catecholamines – urine – Penn State Hershey Medical Center". Pennstatehershey.adam.com. 2011-01-06. Archived from the original on 2013-12-03. Retrieved 2013-02-23.
- ^ Pacak, K.; Eisenhofer, G.; Carrasquillo, J. A.; Chen, C. C.; Li, S. T.; Goldstein, D. S. (July 2001). "6-[18F]Fluorodopamine Positron Emission Tomographic (PET) Scanning for Diagnostic Localization of Pheochromocytoma". Hypertension. 38 (1). Hyper.ahajournals.org: 6–8. doi:10.1161/01.HYP.38.1.6. PMID 11463751.
- ^ Jager P. L., Chirakal R., Marriott C. J., Brouwers A. H., Koopmans K. P., Gulenchyn K. Y. (2008). "6-L-18F-fluorodihydroxyphenylalanine PET in neuroendocrine tumors: basic aspects and emerging clinical applications". Journal of Nuclear Medicine. 49: 573–586. doi:10.2967/jnumed.107.045708.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Goldman 2011, pp. 185
- ^ Cotesta, D; Caliumi, C; Alò, P; Petramala, L; Reale, MG; Masciangelo, R; Signore, A; Cianci, R; et al. (2005). "High plasma levels of human chromogranin A and adrenomedullin in patients with pheochromocytoma". Tumori. 91 (1): 53–8. doi:10.1177/030089160509100110. PMID 15850005.
- ^ Weber, F; Belker, J; Unger, N; Lahner, H; Theurer, S; Schmid, KW; Führer, D; Dralle, H (April 2020). "[Pheochromocytomatosis after adrenalectomy: metastasis or cell seeding?]". Der Chirurg; Zeitschrift fur alle Gebiete der operativen Medizen. 91 (4): 345–353. doi:10.1007/s00104-019-01070-0. PMID 31781805.
- ^ Ferrer-Inaebnit, E; Segura-Sampedro, JJ; Alfonso-García, M; González-Argente, X; Morales-Soriano, R (10 May 2020). "Cytoreductive surgery in functioning peritoneal pheochromocytomatosis". Cirugia espanola. doi:10.1016/j.ciresp.2020.03.010. PMID 32402418.
- ^ Giannini, A. James; Black, Henry R.; Goettsche, Roger L. (1978). Psychiatric, Psychogenic and Somatopsychic Disorders Handbook. Garden City, NY: Medical Examination. pp. 213–4. ISBN 978-0-87488-596-5.
- ^ Jaroszewski, D. E.; Tessier, D. J.; Schlinkert, R. T.; Grant, C. S.; Thompson, G. B.; Van Heerden, J. A.; Farley, D. R.; Smith, S. L.; Hinder, R. A. (2003). "Laparoscopic Adrenalectomy for Pheochromocytoma". Mayo Clinic Proceedings. 78 (12): 1501–04. doi:10.4065/78.12.1501. PMID 14661679.
- ^ Pacack, K. (2007). "Preoperative management of the pheochromocytoma patient". J Clin Endocrinol Metab. 92 (11): 4069–79. doi:10.1210/jc.2007-1720. PMID 17989126.
- ^ Khorram-Manesh, A.; Ahlman, H.; Nilsson, O.; Odén, A.; Jansson, S. (2004). "Mortality associated with pheochromocytoma in a large Swedish cohort". European Journal of Surgical Oncology. 30 (5): 556–59. doi:10.1016/j.ejso.2004.03.006. PMID 15135486.
- ^ Goldman 2011, pp. 1470
- ^ Greene LA, Tischler AS; Tischler (1976). "Establishment of a noradrenergic clonal line of rat adrenal pheochromocytoma cells which respond to nerve growth factor". Proc. Natl. Acad. Sci. U.S.A. 73 (7): 2424–28. Bibcode:1976PNAS...73.2424G. doi:10.1073/pnas.73.7.2424. PMC 430592. PMID 1065897.
Notes
- Goldman, Lee (2011). Goldman's Cecil Medicine (24th ed.). Philadelphia: Elsevier Saunders. pp. 1362. ISBN 978-1437727883.
{{cite book}}: Invalid|ref=harv(help)
External links
- MedlinePlus Overview pheochromocytoma
- GeneReviews entry on "Hereditary Paraganglioma-Pheochromocytoma Syndromes"
- "General Information About Pheochromocytoma and Paraganglioma" from the National Cancer Institute
Template:Gonadal tumors, paraganglioma, glomus, nevi and melanomas






