Pernicious anemia
| Pernicious anemia | |
|---|---|
| Specialty | Hematology |
Pernicious anaemia (also known as vitamin B12 deficiency anaemia,[1] Biermer's anemia, Addison's anemia, or Addison–Biermer anemia) is one of many types of the larger family of megaloblastic anemias. One way pernicious anemia can develop is by loss of gastric parietal cells, which are responsible, in part, for the secretion of intrinsic factor, a protein essential for subsequent absorption of vitamin B12 in the ileum.
The loss of ability to absorb vitamin B12 is the most common cause of adult B12 deficiency.[2] A common underlying cause is atrophic gastritis with autoimmune destruction of gastric parietal cells (and autoantibody inactivation of intrinsic factor) leading to a lack of intrinsic factor.[3] Absorption of vitamin B12[4] in the gut is normally dependent on intrinsic factor, the loss of which leads to vitamin B12 deficiency. While the term pernicious anemia is sometimes also incorrectly used to indicate megaloblastic anemia due to any cause of B12 deficiency, its proper usage refers to that caused by atrophic gastritis, parietal cell loss, and lack of intrinsic factor only.
Historically, pernicious anemia (PA) was detected only after causing symptoms and with well established anemia, i.e., liver stores of B12 had been depleted. The "pernicious" aspect of the disease – prior to the discovery of treatment – was an invariably fatal prognosis. Modern tests which specifically target B12 absorption can diagnose the disease before it gives symptoms. Replacement of vitamin stores does not correct the defect in absorption from loss of intrinsic factor. Since the defect defines the disease, people without the ability to absorb B12 in this way will have pernicious anemia for the remainder of their lives. However, unless the patient has sustained permanent peripheral nerve damage before treatment, regular B12 replacement will keep PA in check, with no anemia and no further symptoms.
Although initial treatment of the disease usually involves injections of B12 to rapidly replace body stores, a number of studies have shown long-term vitamin replacement treatment may be maintained with high-dose oral B12 supplements, since sufficient B12 is absorbed from these by a normal intestine, even without any intrinsic factor. In this regard, nasal and sublingual forms of B12 have not been found to have any special value over simple swallowed tablets.[5]
Signs and symptoms
Pernicious anemia presents insidiously, meaning that it slowly and subtly causes harm. Many of the signs and symptoms are due to anemia itself, where anemia is present. Untreated pernicious anemia can lead to neurological complications, and in serious cases, death. However, in 20% of cases of cobalamin deficiency, anemia is not observed.[6] While it may consist of the triad of paresthesias, sore tongue, and weakness, this is not the chief symptom complex.[7] Common symptoms include anemia,[8] fatigue,[8] depression,[9] low-grade fevers, diarrhea,[9] dyspepsia,[9] weight loss,[7] neuropathic pain, jaundice, glossitis (swollen, red and smooth appearance of the tongue),[10] angular cheilitis (sores at the corner of the mouth),[9] dehydrated/cracked and pale lips and dark circles around the eyes (look of exhaustion),[9] brittle nails,[10] and thinning and early greying of the hair.[10] Because PA may affect the nervous system, symptoms may also include difficulty in proprioception,[11] memory changes,[9] mild cognitive impairment (including difficulty concentrating and sluggish responses, colloquially referred to as brain fog), psychosis, impaired urination,[7] loss of sensation in the feet, unsteady gait,[11] difficulty in walking,[10] muscle weakness[8] and clumsiness.[7] Anemia may cause tachycardia (rapid heartbeat)[7] and cardiac murmurs, along with a yellow waxy pallor,[10] low blood pressure, high blood pressure, and shortness of breath[8] (known as 'the sighs'). The deficiency also may present with thyroid disorders.[8] In severe cases, the anemia may cause evidence of congestive heart failure.[9] A complication of severe chronic PA is subacute combined degeneration of spinal cord, which leads to distal sensory loss (posterior column), absent ankle reflex, increased knee reflex response, and extensor plantar response.[12] Other than anemia, hematological symptoms may include cytopenias, intramedullary hemolysis and pseudothrombotic microangiopathy.[13] Pernicious anemia can contribute to a delay in physical growth in children, and may also be a cause for delay in puberty for adolescents.
Causes
Vitamin B12 cannot be produced by the human body, and must be obtained from the diet. When foods containing B12 are eaten, the vitamin is usually bound to protein and is released by stomach acid. Following its release, most B12 is absorbed by the body in the small bowel (ileum) after binding to a protein known as intrinsic factor. Intrinsic factor is produced by parietal cells of the gastric mucosa (stomach lining) and the intrinsic factor-B12 complex is absorbed by cubilin receptors on the ileum epithelial cells.[14][15] PA is characterised by B12 deficiency caused by the absence of intrinsic factor.[16]
PA may be considered as an end stage of immune gastritis, a disease characterised by stomach atrophy and the presence of antibodies to parietal cells and intrinsic factor.[17] A specific form of chronic gastritis, type A gastritis or atrophic body gastritis, is highly associated with PA. This autoimmune disorder is localised to the body of the stomach, where parietal cells are located.[16] Antibodies to intrinsic factor and parietal cells cause the destruction of the oxyntic gastric mucosa, in which the parietal cells are located, leading to the subsequent loss of intrinsic factor synthesis. Without intrinsic factor, the ileum can no longer absorb the B12.[18]
Although the exact role of Helicobacter pylori infection in PA remains controversial, evidence indicates H. pylori is involved in the pathogenesis of the disease. A long-standing H. pylori infection may cause gastric autoimmunity by a mechanism known as molecular mimicry. Antibodies produced by the immune system can be cross-reactive and may bind to both H. pylori antigens and those found in the gastric mucosa. The antibodies are produced by activated B cells that recognise both pathogen and self-derived peptides. The autoantigens believed to cause the autoreactivity are the alpha and beta subunits of the H+/K+-ATPase.[18][19]
Less commonly, H. pylori and Zollinger-Ellison syndrome may also cause a form of nonautoimmune gastritis that can lead to pernicious anemia.[20]
Impaired B12 absorption can also occur following gastric removal (gastrectomy) or gastric bypass surgery. In these surgeries, either the parts of the stomach that produce gastric secretions are removed or they are bypassed. This means intrinsic factor, as well as other factors required for B12 absorption, are not available. However, B12 deficiency after gastric surgery does not usually become a clinical issue. This is probably because the body stores many years' worth of B12 in the liver and gastric surgery patients are adequately supplemented with the vitamin.[21][22]
Although no specific PA susceptibility genes have been identified, a genetic factor likely is involved in the disease. Pernicious anemia is often found in conjunction with other autoimmune disorders, suggesting common autoimmune susceptibility genes may be a causative factor.[16] In spite of that, previous family studies and case reports focusing on PA have suggested that there is a tendency of genetic heritance of PA in particular, and close relatives of the PA patients seem to have higher incidence of PA and associated PA conditions.[23][24][25] Moreover, it was further indicated that the formation of antibodies to gastric cells was autosomal dominant gene determined, and the presence of antibodies to the gastric cells might not be necessarily related to the occurrence of atrophic gastritis related to PA.[23][25]
Pathophysiology
Although the healthy body stores three to five years' worth of B12 in the liver, the usually undetected autoimmune activity in one's gut over a prolonged period of time leads to B12 depletion and the resulting anemia. B12 is required by enzymes for two reactions: the conversion of methylmalonyl CoA to succinyl CoA, and the conversion of homocysteine to methionine. In the latter reaction, the methyl group of 5-methyltetrahydrofolate is transferred to homocysteine to produce tetrahydrofolate and methionine. This reaction is catalyzed by the enzyme methionine synthase with B12 as an essential cofactor. During B12 deficiency, this reaction cannot proceed, which leads to the accumulation of 5-methyltetrahydrofolate. This accumulation depletes the other types of folate required for purine and thymidylate synthesis, which are required for the synthesis of DNA. Inhibition of DNA replication in red blood cells results in the formation of large, fragile megaloblastic erythrocytes. The neurological aspects of the disease are thought to arise from the accumulation of methylmalonyl CoA due to the requirement of B12 as a cofactor to the enzyme methylmalonyl CoA mutase.[14][26][27][28]
Diagnosis

The insidious nature of PA may mean that diagnosis is delayed. The Schilling test, the classic test for PA, is no longer widely used, as safer and more efficient methods are available. Part one of the Schilling test consists of taking an oral dose of radiolabelled B12 and having the radioactivity of the urine measured over a 24-hour period. The second part of the test is a repeat of the first, with the addition of oral intrinsic factor. With lower than normal amounts of intrinsic factor produced in PA, the addition of intrinsic factor in the second test allows the body to absorb more B12, producing a higher urine radioactivity. This test can distinguish PA from other forms of B12 deficiency.[14] Specifically, the Schilling test can be used to differentiate PA from Imerslund-Grasbeck Syndrome (IGS), from which IGS is also a vitamin B12-deficiency disease but caused by genetic mutations in cobalamin receptor [29]). PA may be suspected when a patient's blood smear shows large, fragile, immature erythrocytes, known as megaloblasts. A diagnosis of PA first requires demonstration of megaloblastic anemia by conducting a full blood count and blood smear, which evaluates the mean corpuscular volume (MCV), as well the mean corpuscular hemoglobin concentration (MCHC). PA is identified with a high MCV (macrocytic anemia) and a normal MCHC (normochromic anemia).[30] Ovalocytes are also typically seen on the blood smear, and a pathognomonic feature of megaloblastic anemias (which include PA and others) is hypersegmented neutrophils.[10]
Serum B12 levels are used to detect B12 deficiency, but they do not distinguish its causes. B12 levels can be falsely high or low and data for sensitivity and specificity vary widely. Normal serum levels may be found in cases of deficiency where myeloproliferative disorders, liver disease, transcobalamin II deficiency, or intestinal bacterial overgrowth are present. Low levels of serum B12 may be caused by other factors than B12 deficiency, such as folate deficiency, pregnancy, oral contraceptive use, haptocorrin deficiency, and myeloma.[31][32]
The presence of antibodies to gastric parietal cells and intrinsic factor is common in PA. Parietal cell antibodies are found in other autoimmune disorders and also in up to 10% of healthy individuals, making the test nonspecific. However, around 85% of PA patients have parietal cell antibodies, which means they are a sensitive marker for the disease. Intrinsic factor antibodies are much less sensitive than parietal cell antibodies, but they are much more specific. They are found in about half of PA patients and are very rarely found in other disorders. These antibody tests can distinguish between PA and food-B12 malabsorption.[32] It has been suggested that the combination of both tests of intrinsic factor antibodies and parietal cell antibodies could improve overall sensitivity and specificity of the diagnostic results.[33]
A buildup of certain metabolites occurs in B12 deficiency due to its role in cellular physiology. Methylmalonic acid can be measured in both the blood and urine, whereas homocysteine is only measured in the blood. An increase in both MMA and homocysteine can distinguish between B12 deficiency and folate deficiency because only homocysteine increases in the latter.[32][34]
Elevated gastrin levels can be found in around 80-90% of PA cases, but they may also be found in other forms of gastritis. Decreased pepsinogen I levels or a decreased pepsinogen I to pepsinogen II ratio may also be found, although these findings are less specific to PA and can be found in food-B12 malabsorption and other forms of gastritis.[34]
The diagnosis of atrophic gastritis type A should be confirmed by gastroscopy and stepwise biopsy.[35] About 90% of individuals with PA have antibodies for parietal cells; however, only 50% of all individuals in the general population with these antibodies have pernicious anemia.[36]
Forms of B12 deficiency other than PA must be considered in the differential diagnosis of megaloblastic anemia. For example, a B12-deficient state which causes megaloblastic anemia and which may be mistaken for classical PA may be caused by infection with the tapeworm Diphyllobothrium latum, possibly due to the parasite's competition for B12.[37]
Treatment
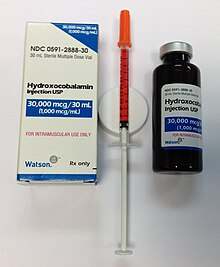
The treatment of PA varies from country to country and from area to area. Opinions vary over the efficacy of administration (parenteral/oral), the amount and time interval of the doses, or the forms of vitamin B12 (e.g. cyanocobalamin/hydrocobalamin). More comprehensive studies are still needed in order to validate the feasibility of a particular therapeutic method for PA in clinical practices. A permanent cure for PA is lacking, although repletion of B12 should be expected to result in cessation of anemia-related symptoms, a halt in neurological deterioration, and in cases where neurological problems are not advanced, neurological recovery and a complete and permanent remission of all symptoms, so long as B12 is supplemented. Repletion of B12 can be accomplished in a variety of ways.
Intramuscular injections
The standard treatment for PA has been parenteral (intramuscular) administration of cobalamin in the form of cyanocobalamin (CN-Cbl) and hydroxocobalamin (OH-Cbl). Andrès et al. recommend a general method to administer CN-Cbl in three stages; 1000 μg/day for 1 week, then 1000 μg/week for 1 month, followed by 1000 μg/month for life.[38]
Oral doses
Oral treatment [39] with high dose vitamin B12 also appears effective.[38][40]
Prognosis
A patient with well-treated PA can live a healthy life. Failure to diagnosis and treat in time, however, may result in permanent neurological damage, excessive fatigue, depression, memory loss, and other complications. In severe cases, the neurological complications of pernicious anemia can lead to death - hence the name, "pernicious", meaning deadly.
An association has been observed between pernicious anemia and certain types of gastric cancer, but a causal link has not been established.[18]
Epidemiology
PA is estimated to affect 0.1% of the general population and 1.9% of those over 60, accounting for 20-50% of B12 deficiency in adults.[13] It has been shown from a literature review that the prevalence of PA was higher in North European, especially for Scandinavian countries and African descent, in which high/increased awareness towards the disease and better diagnostic tools might partly play a role in it [41]
History
The symptoms are first described in 1822 by Dr James Scarth Combe in the Transactions of the Medico-Chirurgical Society of Edinburgh, under the title of History of a Case of Anaemia.[42]
However, not until 1849 was this investigated in more depth, by the British physician Thomas Addison, from which it acquired the common name of Addison's anemia. In 1871, German physician Michael Anton Biermer (1827–1892) noticed the particular characteristic of the anemia in one of his patients; he later coined the term "progressive pernicious anemia".[43] In 1907, Richard Clarke Cabot reported on a series of 1200 patients with PA. Their average survival was between one and three years. Dr. William Bosworth Castle performed an experiment whereby he ingested raw hamburger meat and regurgitated it after an hour, and subsequently fed it to a group of ten patients.[44] Untreated raw hamburger meat was fed to the control group. The former group showed a disease response, whereas the latter group did not. This was not a sustainable practice, but it demonstrated the existence of an 'intrinsic factor' from gastric juice.
Pernicious anemia was a fatal disease before about the year 1920, when George Whipple suggested raw liver as a treatment. The first workable treatment for pernicious anemia began when Whipple made a discovery in the course of experiments in which he bled dogs to make them anemic, then fed them various foods to see which would make them recover most rapidly (he was looking for treatments for anemia from bleeding, not pernicious anemia). Whipple discovered ingesting large amounts of liver seemed to cure anemia from blood loss, and tried liver ingestion as a treatment for pernicious anemia, reporting improvement there, also, in a paper in 1920. George Minot and William Murphy then set about to partly isolate the curative property in liver, and in 1926 showed it was contained in raw liver juice (in the process also showing it was the iron in liver tissue, not the soluble factor in liver juice, which cured the anemia from bleeding in dogs; thus, the discovery of the liver juice factor as a treatment for pernicious anemia had been by coincidence). Frieda Robscheit-Robbins worked closely with Whipple, co-authoring 21 papers from 1925-30. For the discovery of the cure of a previously fatal disease of unknown etiology, Whipple, Minot, and Murphy shared the 1934 Nobel Prize in Medicine.[45]
After Minot and Murphy's verification of Whipple's results in 1926, pernicious anemia victims ate or drank at least one-half pound of raw liver, or drank raw liver juice, every day. This continued for several years, until a concentrate of liver juice became available. In 1928, chemist Edwin Cohn prepared a liver extract that was 50 to 100 times more potent than the natural food (liver). The extract could even be injected into muscle, which meant patients no longer needed to eat large amounts of liver or juice. This also reduced the cost of treatment considerably.
The active ingredient in liver remained unknown until 1948, when it was isolated by two chemists, Karl A. Folkers of the United States and Alexander R. Todd of Great Britain. The substance was a cobalamin, which the discoverers named vitamin B12. The new vitamin in liver juice was eventually completely purified and characterized in the 1950s, and other methods of producing it from bacteria were developed. It could be injected into muscle with even less irritation, making it possible to treat PA with even more ease. Pernicious anemia was eventually treated with either injections or large oral doses of B12, typically between 1 and 4 mg daily.[citation needed]
Research
SNAC complex
Although oral megadoses and intramuscular injections are the most common methods of treatment currently available, several novel methods are being tested, with high promise for future incorporation into mainstream treatment methods. As injections are unfavourable vehicles for drug delivery, current research involves improving the passive diffusion across the ileum upon oral ingestion of cobalamin derivatives. Researchers have recently taken advantage of the novel compound sodium N-[8-(2-hydroxybenzoyl)amino]caprylate (SNAC), which greatly enhances both bioavailability and metabolic stability.[46] SNAC is able to form a noncovalent complex with cobalamin while preserving its chemical integrity.[47] This complex is much more lipophilic than the water-soluble B12, so is able to pass through cellular membranes with greater ease.
Recombinant intrinsic factor
Another method for increasing absorption through the ileum is to ingest a Cbl complex to which IF is already bound. The lack of intrinsic factor produced by the patient's body can be supplemented by using synthetic human IF produced from pea plant recombinants.[48] However, in cases where IF-antibodies are the reason for malabsorption across the ileum, this treatment would be ineffective.
Sublingual/intranasal delivery
Sublingual treatments have also been postulated to be more effective than oral treatments alone. A 2003 study[49] found, while this method is effective, a dose of 500 μg of cyanocobalamin given either orally or sublingually, is equally efficacious in restoring normal physiological concentrations of cobalamin. Intranasal methods have also been studied as a vehicle for the delivery of cobalamin. A 1997 study[50] monitored the plasma cobalamin concentration of six patients with pernicious anemia over a period of 35 days while being treated with 1500 μg of intranasal hydroxocobalamin. One hour after administration, all patients showed on average an immediate eight-fold increase in plasma cobalamin concentration and a two-fold increase after 35 days with three 1500 μg treatments. However, further studies are needed to investigate the long-term effectiveness of this delivery method.
Transdermal patches
An alternative method for the treatment of pernicious anemia includes the use of transdermal patches. These patches are composed of CN-Cbl complexed with B12 stabilizers, and epidermal penetration enhancers.[51] Vitamin-loaded electrospun nanofibers are able to deliver the vitamin effectively through the stratum corneum. The transdermal route allows CN-Cbl to passively diffuse through the stratum corneum, viable epidermis, and dermis layer, and ultimately entering the bloodstream. A 20-mg 5% drug-loaded polycaprolactone fiber can release 340 μg of cobabalmin per day.[52] Since the drug is absorbed directly from the epidermis to the bloodstream, it avoids the hepatic first pass effect, improving bioavailability and therapeutic efficacy of the drug. The slow release of the drug from the patch to the bloodstream also increases its half-life, maintaining a constant cyanocobalamin level in blood for longer periods of time. This decreases the dosage required in comparison to oral delivery methods.
References
- ^ "ICD-10 Version:2015". apps.who.int. Retrieved 2015-11-13.
- ^ Masnou H; Domènech E; Navarro-Llavat M; et al. (December 2007). "Pernicious anaemia in triplets. A case report and literature review". Gastroenterología y Hepatología. 30 (10): 580–2. doi:10.1157/13112591. PMID 18028852.
{{cite journal}}: Unknown parameter|name-list-format=ignored (|name-list-style=suggested) (help)[dead link] - ^ "University of Chicago Med Ctr: Megaloblastic (Pernicious) Anemia". Archived from the original on September 3, 2006. Retrieved 2008-01-27.
{{cite web}}: Unknown parameter|deadurl=ignored (|url-status=suggested) (help) - ^ Kumar V (February 2007). "Pernicious anemia". MLO. 39 (2): 28, 30–1. PMID 17375844.
- ^ "Office of Dietary Supplements". National Institutes of Health. Retrieved 11 January 2013.
- ^ Fred F. Ferri, M.D. "Ferri: Ferri's Clinical Advisor 2012, 1st ed". Retrieved 2015-12-26.
- ^ a b c d e emedicine, Medscape. "Pernicious anemia Clinical Presentation". Retrieved 21 January 2013.
- ^ a b c d e Ramani, James Carton, Richard Daly, Pramila (2007). Clinical pathology. Oxford: Oxford University Press. ISBN 0198569467.
{{cite book}}: CS1 maint: multiple names: authors list (link) - ^ a b c d e f g Turgeon, Mary L. (2005). Clinical hematology : theory and procedures (4th ed.). Philadelphia: Lippincott Williams & Wilkins. ISBN 0781750075.
- ^ a b c d e f al.], editors John P. Greer... [et (2009). Wintrobe's clinical hematology (12th ed.). Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins. ISBN 0781765072.
{{cite book}}:|first=has generic name (help) - ^ a b Hvas AM, Nexo E (November 2006). "Diagnosis and treatment of vitamin B12 deficiency--an update". Haematologica. 91 (11): 1506–12. PMID 17043022.
- ^ "Pernicious anemia: MedlinePlus Medical Encyclopedia". Nlm.nih.gov. Retrieved 2010-03-18.
- ^ a b Andres E, Serraj K (2012). "Optimal management of pernicious anemia". Journal of Blood Medicine. 3: 97–103. doi:10.2147/JBM.S25620. PMC 3441227. PMID 23028239.
{{cite journal}}: CS1 maint: unflagged free DOI (link) - ^ a b c Wickramasinghe, SN (November 2006). "Diagnosis of megaloblastic anaemias". Blood reviews. 20 (6): 299–318. doi:10.1016/j.blre.2006.02.002. PMID 16716475.
- ^ Christensen EI, Birn H (April 2002). "Megalin and cubilin: multifunctional endocytic receptors". Nat. Rev. Mol. Cell Biol. 3 (4): 256–66. doi:10.1038/nrm778. PMID 11994745.
- ^ a b c Banka S, Ryan K, Thomson W, Newman WG (June 2011). "Pernicious anemia – genetic insights". Autoimmunity reviews. 10 (8): 455–9. doi:10.1016/j.autrev.2011.01.009. PMID 21296191.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ De Block CE, De Leeuw IH, Van Gaal LF (February 2008). "Autoimmune gastritis in type 1 diabetes: a clinically oriented review". The Journal of Clinical Endocrinology and Metabolism. 93 (2): 363–71. doi:10.1210/jc.2007-2134. PMID 18029461.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ a b c Lahner E, Annibale B (November 2009). "Pernicious anemia: New insights from a gastroenterological point of view". World J. Gastroenterol. 15 (41): 5121–8. doi:10.3748/wjg.15.5121. PMC 2773890. PMID 19891010.
{{cite journal}}: CS1 maint: unflagged free DOI (link) - ^ Desai HG, Gupte PA (December 2007). "Helicobacter pylori link to pernicious anaemia". The Journal of the Association of Physicians of India. 55: 857–9. PMID 18405134.
- ^ Kaferle J, Strzoda CE (Feb 1, 2009). "Evaluation of macrocytosis". American family physician. 79 (3): 203–8. PMID 19202968.
- ^ von Drygalski A, Andris DA (Apr–May 2009). "Anemia after bariatric surgery: more than just iron deficiency". Nutrition in clinical practice : official publication of the American Society for Parenteral and Enteral Nutrition. 24 (2): 217–26. doi:10.1177/0884533609332174. PMID 19321896.
- ^ John S, Hoegerl C (November 2009). "Nutritional deficiencies after gastric bypass surgery". The Journal of the American Osteopathic Association. 109 (11): 601–4. PMID 19948694.
- ^ a b Whttingham, S., Ungar, B., Mackay, I. R., & Mathews, J. D. (1969). The Genetic Factor in Pernicious Anemia. A Family Study in Patients with Gastritis. The Lancet, 1(7602), 951-954.
- ^ McIntyre, O. R., Sullivan, L. W., Jeffries, G. H., & Silver, R. H. (1965). Pernicious Anemia in Childhood. The New England Journal of Medicine, 272, 981-986.
- ^ a b Wangel, A. G., Callender, S. T., Spray, G. H., & Wright, R. (1968). A Family Study of Pernicious Anemia II. Intrinsic Factor Secretion, Vitamin B12 Absorption and Genetic Aspects of Gastric Autoimmunity. British Journal of Haematology, 14(2), 183-204.
- ^ Oh R, Brown DL (Mar 1, 2003). "Vitamin B12 deficiency". American family physician. 67 (5): 979–86. PMID 12643357.
- ^ O'Leary F, Samman S (March 2010). "Vitamin B12 in health and disease". Nutrients. 2 (3): 299–316. doi:10.3390/nu2030299. PMC 3257642. PMID 22254022.
{{cite journal}}: CS1 maint: unflagged free DOI (link) - ^ Stover, PJ (June 2004). "Physiology of folate and vitamin B12 in health and disease". Nutrition Reviews. 62 (6 Pt 2): S3-12, discussion S13. doi:10.1111/j.1753-4887.2004.tb00070.x. PMID 15298442.
- ^ Andres, E., & Serra, K. (2012). Optimal management of pernicious anemia. Journal of Blood Medicine, 3, 97-103.
- ^ Pagana, Timothy James; Pagana, Kathleen Deska (2006). Mosby's manual of diagnostic and laboratory tests. Mosby Elsevier. ISBN 0-323-03903-0.
{{cite book}}: CS1 maint: multiple names: authors list (link)[page needed] - ^ Devalia V (August 2006). "Diagnosing vitamin B-12 deficiency on the basis of serum B-12 assay". BMJ. 333 (7564): 385–6. doi:10.1136/bmj.333.7564.385. PMC 1550477. PMID 16916826.
- ^ a b c Snow, CF (Jun 28, 1999). "Laboratory diagnosis of vitamin B12 and folate deficiency: a guide for the primary care physician". Archives of Internal Medicine. 159 (12): 1289–98. doi:10.1001/archinte.159.12.1289. PMID 10386505.
- ^ Grasbeck, R. (2006). Imerslund-Grasbeck syndrome (selective vitamin B12 malabsorption with proteinuria). Orphanet Journal of Rare diseases, 1(1), 17.
- ^ a b Moridani, Majid; Shana Ben-Poorat (March 2006). "Laboratory Investigation of Vitamin B12 Deficiency". LabMedicine. 37 (3): 166–74. doi:10.1309/cvhkle2r4w68k2nq.
- ^ Miederer, S.E. (1977). The Histotopography of the Gastric Mucosa. Thieme, ISBN 3-13-508601-1
- ^ Butler CC; Vidal-Alaball J; Cannings-John R; et al. (June 2006). "Oral vitamin B12 versus intramuscular vitamin B12 for vitamin B12 deficiency: a systematic review of randomized controlled trials". Family Practice. 23 (3): 279–85. doi:10.1093/fampra/cml008. PMID 16585128.
{{cite journal}}: Unknown parameter|name-list-format=ignored (|name-list-style=suggested) (help) - ^ Ramakrishnan, edited by Usha (2000). Nutritional anemias. Boca Raton: CRC Press. ISBN 0849385695.
{{cite book}}:|first=has generic name (help) - ^ a b Andrès, E.; Fothergill, H.; Mecili, M. (2010). "Efficacy of oral cobalamin (vitamin B12) therapy". Expert Opinion on Pharmacotherapy. 11 (2): 249–256. doi:10.1517/14656560903456053. PMID 20088746.
- ^ R. Carmel (9 August 2008). "How I treat cobalamin (vitamin B12) deficiency". Blood. 112 (6): 2214–2221. doi:10.1182/blood-2008-03-040253.
- ^ Andrès, E.; Dali-Youcef, N.; Vogel, T.; Serraj, K.; Zimmer, J. (2009). "Oral cobalamin (vitamin B12) treatment. An update". International Journal of Laboratory Hematology. 31: 1. doi:10.1111/j.1751-553X.2008.01115.x.
- ^ Stabler, S. P., & Allen, R. H. (2004). Vitamin B12 deficiency as a worldwide problem. Annual Review of Nutrition, 24(1), 299-326.
- ^ History of Leith, Edinburgh » James Scarth Combe
- ^ Whonamedit - dictionary of medical eponyms
- ^ William B. Castle 1897–1990 A Biographical Memoir by James H. Jandl Copyright 1995 National Academies Press Washington D.C.
- ^ Nobel Prize archive. "The Nobel Prize in Physiology or Medicine 1934" (Nobelprize.org). Retrieved 2012-08-05.
- ^ Castelli, M. C.; Wong, D. F.; Friedman, K.; Riley, M. G. I. (2011). "Pharmacokinetics of Oral Cyanocobalamin Formulated with Sodium N-\8-(2-hydroxybenzoyl)amino]caprylate (SNAC): An Open-Label, Randomized, Single-Dose, Parallel-Group Study in Healthy Male Subjects". Clinical Therapeutics. 33 (7): 934–945. doi:10.1016/j.clinthera.2011.05.088. PMID 21722960.
- ^ [1] Archived 2014-10-06 at the Wayback Machine
- ^ Fedosov, S. N.; Laursen, N. B.; Nexo, E.; Moestrup, S. K.; Petersen, T. E.; Jensen, E. O.; Berglund, L. (2003). "Human intrinsic factor expressed in the plant Arabidopsis thaliana". European Journal of Biochemistry. 270 (16): 3362–3367. doi:10.1046/j.1432-1033.2003.03716.x. PMID 12899693.
- ^ Sharabi, A.; Cohen, E.; Sulkes, J.; Garty, M. (2003). "Replacement therapy for vitamin B12 deficiency: Comparison between the sublingual and oral route". British Journal of Clinical Pharmacology. 56 (6): 635–638. doi:10.1046/j.1365-2125.2003.01907.x. PMC 1884303. PMID 14616423.
- ^ Slot WB, Merkus FW, Van Deventer SJ, Tytgat GN (August 1997). "Normalization of plasma vitamin B12 concentration by intranasal hydroxocobalamin in vitamin B12-deficient patients". Gastroenterology. 113 (2): 430–3. doi:10.1053/gast.1997.v113.pm9247460. PMID 9247460.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Patent US20080233180 - Transdermal Patch and Method For Delivery Of Vitamin B12 - Google Patents
- ^ Madhaiyan, K.; Sridhar, R.; Sundarrajan, S.; Venugopal, J. R.; Ramakrishna, S. (2013). "Vitamin B12 loaded polycaprolactone nanofibers: A novel transdermal route for the water soluble energy supplement delivery". International Journal of Pharmaceutics. 444 (1–2): 70–76. doi:10.1016/j.ijpharm.2013.01.040. PMID 23370432.
External links
- The Pernicious Anaemia Society, a UK-based charitable organization
- Parietal cell antibody
- Antibody to GPC
- [2]
- Rare Anemias Foundation
{{Diseases of RBCs and megakaryocytes}} may refer to:
- {{Diseases of RBCs}}, a navigational template for diseases of red blood cells
- {{Diseases of megakaryocytes}}, a navigational template for diseases of clotting
{{Template disambiguation}} should never be transcluded in the main namespace.
