Bone marrow
| Bone marrow | |
|---|---|
 A section of bone marrow tissue (Prussian blue-stained) | |
| Details | |
| System | Hematopoietic system, immune system,[1] lymphatic system |
| Identifiers | |
| Latin | medulla ossium |
| MeSH | D001853 |
| TA98 | A13.1.01.001 |
| TA2 | 388 |
| FMA | 9608 |
| Anatomical terminology | |
Bone marrow is a semi-solid tissue found within the spongy (also known as cancellous) portions of bones.[2] In birds and mammals, bone marrow is the primary site of new blood cell production (or haematopoiesis).[3] It is composed of hematopoietic cells, marrow adipose tissue, and supportive stromal cells. In adult humans, bone marrow is primarily located in the ribs, vertebrae, sternum, and bones of the pelvis.[4] Bone marrow comprises approximately 5% of total body mass in healthy adult humans, such that a man weighing 73 kg (161 lbs) will have around 3.7 kg (8 lbs) of bone marrow.[5]
Human marrow produces approximately 500 billion blood cells per day, which join the systemic circulation via permeable vasculature sinusoids within the medullary cavity.[6] All types of hematopoietic cells, including both myeloid and lymphoid lineages, are created in bone marrow; however, lymphoid cells must migrate to other lymphoid organs (e.g. thymus) in order to complete maturation.
Bone marrow transplants can be conducted to treat severe diseases of the bone marrow, including certain forms of cancer such as leukemia. Several types of stem cells are related to bone marrow. Hematopoietic stem cells in the bone marrow can give rise to hematopoietic lineage cells, and mesenchymal stem cells, which can be isolated from the primary culture of bone marrow stroma, can give rise to bone, adipose, and cartilage tissue.[7]
Structure
[edit]The composition of marrow is dynamic, as the mixture of cellular and non-cellular components (connective tissue) shifts with age and in response to systemic factors. In humans, marrow is colloquially characterized as "red" or "yellow" marrow (Latin: medulla ossium rubra, Latin: medulla ossium flava, respectively) depending on the prevalence of hematopoietic cells vs fat cells. While the precise mechanisms underlying marrow regulation are not understood,[6] compositional changes occur according to stereotypical patterns.[8] For example, a newborn baby's bones exclusively contain hematopoietically active "red" marrow, and there is a progressive conversion towards "yellow" marrow with age. In adults, red marrow is found mainly in the central skeleton, such as the pelvis, sternum, cranium, ribs, vertebrae and scapulae, and variably found in the proximal epiphyseal ends of long bones such as the femur and humerus. In circumstances of chronic hypoxia, the body can convert yellow marrow back to red marrow to increase blood cell production.[9]
Hematopoietic components
[edit]
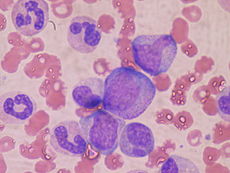
At the cellular level, the main functional component of bone marrow includes the progenitor cells which are destined to mature into blood and lymphoid cells. Human marrow produces approximately 500 billion blood cells per day.[10] Marrow contains hematopoietic stem cells which give rise to the three classes of blood cells that are found in circulation: white blood cells (leukocytes), red blood cells (erythrocytes), and platelets (thrombocytes).[11]
| Group | Cell type | Average fraction |
Reference range |
|---|---|---|---|
| Myelopoietic cells |
Myeloblasts | 0.9 | 0.2–1.5 |
| Promyelocytes | 3.3% | 2.1–4.1 | |
| Neutrophilic myelocytes | 12.7% | 8.2–15.7 | |
| Eosinophilic myelocytes | 0.8% | 0.2–1.3 | |
| Neutrophilic metamyelocytes | 15.9% | 9.6–24.6 | |
| Eosinophilic metamyelocytes | 1.2% | 0.4–2.2 | |
| Neutrophilic band cells | 12.4% | 9.5–15.3 | |
| Eosinophilic band cells | 0.9% | 0.2–2.4 | |
| Segmented neutrophils | 7.4% | 6.0–12.0 | |
| Segmented eosinophils | 0.5% | 0.0–1.3 | |
| Segmented basophils and mast cells | 0.1% | 0.0–0.2 | |
| Erythropoietic cells |
Pronormoblasts | 0.6% | 0.2–1.3 |
| Basophilic normoblasts | 1.4% | 0.5–2.4 | |
| Polychromatic normoblasts | 21.6% | 17.9–29.2 | |
| Orthochromatic normoblast | 2.0% | 0.4–4.6 | |
| Other cell types |
Megakaryocytes | < 0.1% | 0.0-0.4 |
| Plasma cells | 1.3% | 0.4-3.9 | |
| Reticular cells | 0.3% | 0.0-0.9 | |
| Lymphocytes | 16.2% | 11.1-23.2 | |
| Monocytes | 0.3% | 0.0-0.8 |
Stroma
[edit]The stroma of the bone marrow includes all tissue not directly involved in the marrow's primary function of hematopoiesis.[6] Stromal cells may be indirectly involved in hematopoiesis, providing a microenvironment that influences the function and differentiation of hematopoietic cells. For instance, they generate colony stimulating factors, which have a significant effect on hematopoiesis. Cell types that constitute the bone marrow stroma include:
- fibroblasts (reticular connective tissue)
- macrophages, which contribute especially to red blood cell production, as they deliver iron for hemoglobin production.
- adipocytes (fat cells)
- osteoblasts (synthesize bone)
- osteoclasts (resorb bone)
- endothelial cells, which form the sinusoids. These derive from endothelial stem cells, which are also present in the bone marrow.[11]
Function
[edit]Central hematopoietic and antigen-responsive organ
[edit]That bone marrow is a priming site for T-cell responses to blood-borne antigens was first described in 2003.[13] Mature circulating naïve T cells home to bone marrow sinuses after they have passed through arteries and arterioles.[14] They transmigrate sinus endothelium and enter the parenchyma which contains dendritic cells (DCs). These have a capacity of antigen uptake, processing, and presentation.[13] Cognate interactions between antigen-specific T cells and antigen-presenting DCs (APCs) in parenchyma lead to rapid T-APC cluster formation followed by T cell activation, T cell proliferation and T cell re-circulation to blood.[13] These findings were corroborated and extended in 2013 by in situ two-photon dynamic imaging of mice skulls.[15]
Importance for storage and long-term survival of memory B and memory T cells
[edit]Bone marrow is a nest for migratory memory T cells[16] and a sanctuary for plasma cells.[17] This has implications for adaptive immunity and vaccinology.[17] Memory B and T cells persist in the parenchyma in dedicated survival niches organized by stromal cells.[18] This memory can be maintained over long time periods in the form of quiescent cells[18] or by repeated antigenic restimulation.[19] Bone marrow protects and optimizes immunological memory during dietary restriction.[20] In cancer patients, cancer-reactive memory T cells can arise in bone marrow spontaneously or after specific vaccination.[21] Bone marrow is a center of a variety of immune activities: i) hematopoiesis, ii) osteogenesis, iii) immune responses, iv) distinction between self and non-self antigens, v) central immune regulatory function, vi) storage of memory cells, vii) immune surveillance of the central nervous system, viii) adaptation to energy crisis, ix) provision of mesenchymal stem cells for tissue repair.[22]
Mesenchymal stem cells
[edit]The bone marrow stroma contains mesenchymal stem cells (MSCs),[11] which are also known as marrow stromal cells. These are multipotent stem cells that can differentiate into a variety of cell types. MSCs have been shown to differentiate, in vitro or in vivo, into osteoblasts, chondrocytes, myocytes, marrow adipocytes and beta-pancreatic islets cells.[citation needed]
Bone marrow barrier
[edit]The blood vessels of the bone marrow constitute a barrier, inhibiting immature blood cells from leaving the marrow. Only mature blood cells contain the membrane proteins, such as aquaporin and glycophorin, that are required to attach to and pass the blood vessel endothelium.[23] Hematopoietic stem cells may also cross the bone marrow barrier, and may thus be harvested from blood.[citation needed]
Lymphatic role
[edit]The red bone marrow is a key element of the lymphatic system, being one of the primary lymphoid organs that generate lymphocytes from immature hematopoietic progenitor cells.[24] The bone marrow and thymus constitute the primary lymphoid tissues involved in the production and early selection of lymphocytes. Furthermore, bone marrow performs a valve-like function to prevent the backflow of lymphatic fluid in the lymphatic system.[citation needed]
Compartmentalization
[edit]Biological compartmentalization is evident within the bone marrow, in that certain cell types tend to aggregate in specific areas. For instance, erythrocytes, macrophages, and their precursors tend to gather around blood vessels, while granulocytes gather at the borders of the bone marrow.[11]
As food
[edit]People have used animal bone-marrow in cuisine worldwide for millennia, as in the famed Milanese Ossobuco.[25]
Clinical significance
[edit]Disease
[edit]The normal bone marrow architecture can be damaged or displaced by aplastic anemia, malignancies such as multiple myeloma, or infections such as tuberculosis, leading to a decrease in the production of blood cells and blood platelets. The bone marrow can also be affected by various forms of leukemia, which attacks its hematologic progenitor cells.[26] Furthermore, exposure to radiation or chemotherapy will kill many of the rapidly dividing cells of the bone marrow, and will therefore result in a depressed immune system. Many of the symptoms of radiation poisoning are due to damage sustained by the bone marrow cells.[citation needed]
To diagnose diseases involving the bone marrow, a bone marrow aspiration is sometimes performed. This typically involves using a hollow needle to acquire a sample of red bone marrow from the crest of the ilium under general or local anesthesia.[27]
Imaging
[edit]Medical imaging may provide a limited amount of information regarding bone marrow. Plain film x-rays pass through soft tissues such as marrow and do not provide visualization, although any changes in the structure of the associated bone may be detected.[28] CT imaging has somewhat better capacity for assessing the marrow cavity of bones, although with low sensitivity and specificity. For example, normal fatty "yellow" marrow in adult long bones is of low density (-30 to -100 Hounsfield units), between subcutaneous fat and soft tissue. Tissue with increased cellular composition, such as normal "red" marrow or cancer cells within the medullary cavity will measure variably higher in density.[29]
MRI is more sensitive and specific for assessing bone composition. MRI enables assessment of the average molecular composition of soft tissues and thus provides information regarding the relative fat content of marrow. In adult humans, "yellow" fatty marrow is the dominant tissue in bones, particularly in the (peripheral) appendicular skeleton. Because fat molecules have a high T1-relaxivity, T1-weighted imaging sequences show "yellow" fatty marrow as bright (hyperintense). Furthermore, normal fatty marrow loses signal on fat-saturation sequences, in a similar pattern to subcutaneous fat.[citation needed]
When "yellow" fatty marrow becomes replaced by tissue with more cellular composition, this change is apparent as decreased brightness on T1-weighted sequences. Both normal "red" marrow and pathologic marrow lesions (such as cancer) are darker than "yellow" marrow on T1-weight sequences, although can often be distinguished by comparison with the MR signal intensity of adjacent soft tissues. Normal "red" marrow is typically equivalent or brighter than skeletal muscle or intervertebral disc on T1-weighted sequences.[8][30]
Fatty marrow change, the inverse of red marrow hyperplasia, can occur with normal aging,[31] though it can also be seen with certain treatments such as radiation therapy. Diffuse marrow T1 hypointensity without contrast enhancement or cortical discontinuity suggests red marrow conversion or myelofibrosis. Falsely normal marrow on T1 can be seen with diffuse multiple myeloma or leukemic infiltration when the water to fat ratio is not sufficiently altered, as may be seen with lower grade tumors or earlier in the disease process.[32]
Histology
[edit]
Bone marrow examination is the pathologic analysis of samples of bone marrow obtained via biopsy and bone marrow aspiration. Bone marrow examination is used in the diagnosis of a number of conditions, including leukemia, multiple myeloma, anemia, and pancytopenia. The bone marrow produces the cellular elements of the blood, including platelets, red blood cells and white blood cells. While much information can be gleaned by testing the blood itself (drawn from a vein by phlebotomy), it is sometimes necessary to examine the source of the blood cells in the bone marrow to obtain more information on hematopoiesis; this is the role of bone marrow aspiration and biopsy.[citation needed]
The ratio between myeloid series and erythroid cells is relevant to bone marrow function, and also to diseases of the bone marrow and peripheral blood, such as leukemia and anemia. The normal myeloid-to-erythroid ratio is around 3:1; this ratio may increase in myelogenous leukemias, decrease in polycythemias, and reverse in cases of thalassemia.[33]
Donation and transplantation
[edit]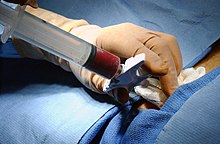
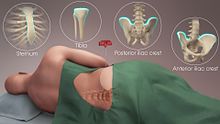
In a bone marrow transplant, hematopoietic stem cells are removed from a person and infused into another person (allogenic) or into the same person at a later time (autologous). If the donor and recipient are compatible, these infused cells will then travel to the bone marrow and initiate blood cell production. Transplantation from one person to another is conducted for the treatment of severe bone marrow diseases, such as congenital defects, autoimmune diseases or malignancies. The patient's own marrow is first killed off with drugs or radiation, and then the new stem cells are introduced. Before radiation therapy or chemotherapy in cases of cancer, some of the patient's hematopoietic stem cells are sometimes harvested and later infused back when the therapy is finished to restore the immune system.[34]
Bone marrow stem cells can be induced to become neural cells to treat neurological illnesses,[35] and can also potentially be used for the treatment of other illnesses, such as inflammatory bowel disease.[36] In 2013, following a clinical trial, scientists proposed that bone marrow transplantation could be used to treat HIV in conjunction with antiretroviral drugs;[37][38] however, it was later found that HIV remained in the bodies of the test subjects.[39]
Harvesting
[edit]The stem cells are typically harvested directly from the red marrow in the iliac crest, often under general anesthesia. The procedure is minimally invasive and does not require stitches afterwards. Depending on the donor's health and reaction to the procedure, the actual harvesting can be an outpatient procedure, or can require 1–2 days of recovery in the hospital.[40]
Another option is to administer certain drugs that stimulate the release of stem cells from the bone marrow into circulating blood.[41] An intravenous catheter is inserted into the donor's arm, and the stem cells are then filtered out of the blood. This procedure is similar to that used in blood or platelet donation. In adults, bone marrow may also be taken from the sternum, while the tibia is often used when taking samples from infants.[27] In newborns, stem cells may be retrieved from the umbilical cord.[42]
Fertility Aid
[edit]One of the most damaged areas of the body following chemotherapy is typically the uterus. Following uterine damage due to cancer treatment, follicle damage makes it difficult for individuals to get pregnant even if viable ova are present. With bone marrow stem cell transplants, chemotherapy patients have been able to increase their fertility as follicle damage is repaired.[43] As follicles are necessary for ovum attachment to the endometrium, it is important for these areas to be repaired in order to increase fertility. For individuals who have sustained egg and follicle damage, IVF has been found to be more effective following bone marrow stem cell transplantation.[44]
One human clinical case has shown improvements of uterine lining thickness and overall endometrium repair following bone marrow stem cell transplantation.[45] This repair allowed for the patient to successfully become pregnant and carry to term.
Additional repairs following bone marrow stem cell transplant to the endometrium include increased vascularity and iron levels, with egg implantation clustering around areas with high blood flow.[44][46]
Persistent viruses
[edit]Using quantitative polymerase chain reaction (qPCR) and next-generation sequencing (NGS) a maximum of five DNA viruses per individual have been identified. Included were several herpesviruses, hepatitis B virus, Merkel cell polyomavirus, and human papillomavirus 31. Given the reactivation and/or oncogenic potential of these viruses, their repercussion on hematopoietic and malignant disorders calls for further studies.[47]
Fossil record
[edit]
The earliest fossilised evidence of bone marrow was discovered in 2014 in Eusthenopteron, a lobe-finned fish which lived during the Devonian period approximately 370 million years ago.[48] Scientists from Uppsala University and the European Synchrotron Radiation Facility used X-ray synchrotron microtomography to study the fossilised interior of the skeleton's humerus, finding organised tubular structures akin to modern vertebrate bone marrow.[48] Eusthenopteron is closely related to the early tetrapods, which ultimately evolved into the land-dwelling mammals and lizards of the present day.[48]
See also
[edit]- LOC100272216 protein
- Myelonecrosis
- National Marrow Donor Program
- Gift of Life Marrow Registry
- List of distinct cell types in the adult human body
References
[edit]- ^ Schmidt, Richard F.; Lang, Florian; Heckmann, Manfred (30 November 2010). What are the organs of the immune system?. Institute for Quality and Efficiency in Health Care. pp. 3/7.
- ^ C., Farhi, Diane (2009). Pathology of bone marrow and blood cells (2nd ed.). Philadelphia: Wolters Kluwer Health/Lippincott William & Wilkins. ISBN 9780781770934. OCLC 191807944.
{{cite book}}: CS1 maint: multiple names: authors list (link) - ^ Arikan, Hüseyin; Çiçek, Kerim (2014). "Haematology of amphibians and reptiles: a review" (PDF). North-Western Journal of Zoology. 10: 190–209.
- ^ Katherine, Abel (2013). Official CPC Certification Study Guide. American Medical Association.
- ^ Hindorf, C.; Glatting, G.; Chiesa, C.; Lindén, O.; Flux, G. (2010). "EANM Dosimetry Committee guidelines for bone marrow and whole-body dosimetry". Eur J Nucl Med Mol Imaging. 37 (6): 1238–1250. doi:10.1007/s00259-010-1422-4. PMID 20411259. S2CID 9755621.
- ^ a b c Birbrair, Alexander; Frenette, Paul S. (1 March 2016). "Niche heterogeneity in the bone marrow". Annals of the New York Academy of Sciences. 1370 (1): 82–96. Bibcode:2016NYASA1370...82B. doi:10.1111/nyas.13016. ISSN 1749-6632. PMC 4938003. PMID 27015419.
- ^ Lindberg, Matthew R.; Lamps, Laura W. (2018). "Bone Marrow". Diagnostic Pathology: Normal Histology. pp. 130–137. doi:10.1016/B978-0-323-54803-8.50035-8. ISBN 9780323548038.
- ^ a b Chan, Brian Y.; Gill, Kara G.; Rebsamen, Susan L.; Nguyen, Jie C. (1 October 2016). "MR Imaging of Pediatric Bone Marrow". RadioGraphics. 36 (6): 1911–1930. doi:10.1148/rg.2016160056. ISSN 0271-5333. PMID 27726743.
- ^ Poulton, T B; Murphy, W D; Duerk, J L; Chapek, C C; Feiglin, D H (1 December 1993). "Bone marrow reconversion in adults who are smokers: MR Imaging findings". American Journal of Roentgenology. 161 (6): 1217–1221. doi:10.2214/ajr.161.6.8249729. ISSN 0361-803X. PMID 8249729.
- ^ Nombela-Arrieta, Cesar; G. Manz, Markus (2017). "Quantification and three-dimensional microanatomical organization of the bone marrow". Blood Advances. 1 (6): 407–416. doi:10.1182/bloodadvances.2016003194. PMC 5738992. PMID 29296956.
- ^ a b c d Raphael Rubin & David S. Strayer (2007). Rubin's Pathology: Clinicopathologic Foundations of Medicine. Lippincott Williams & Wilkins. p. 90. ISBN 978-0-7817-9516-6.
- ^ Appendix A:IV in Wintrobe's clinical hematology (9th edition). Philadelphia: Lea & Febiger (1993).
- ^ a b c Feuerer, Markus; Beckhove, Philipp; Garbi, Natalio (10 August 2003). "Bone marrow as a priming site for T-cell responses to blood-borne antigen". Nature Medicine. 9 (9): 1151–1157. doi:10.1038/nm914. PMID 12910264.
- ^ Mazo, I.B.; von Adrian, U.H. (1999). "Adhesion and homing of blood-borne cells in bone marrow microvessels". Journal of Leukocyte Biology. 66 (1): 25–32. doi:10.1002/jlb.66.1.25. PMID 10410986.
- ^ Milo, Idan; Sapoznikov, Anita; Kalchenko, Vyacheslav (2013). "Dynamic imaging reveals promiscuous crosspresentation of blood-borne antigens to naïve CD8+ T cells in the bone marrow". Blood. 122 (2): 193–208. doi:10.1182/blood-2012-01-401265. PMID 23637125.
- ^ Di Rosa, Francesca; Pabst, Reinhard (2005). "The bone marrow: A nest for migratory memory T cells". Trends in Immunology. 26 (7): 360–366. doi:10.1016/j.it.2005.04.011. PMID 15978522.
- ^ a b Salaming, Stephan A.; Nolte, Martijn A. (2021). "The bone marrow as sanctuary for plasma cells and memory T-cells: Implications for adaptive immunity and vaccinology". Cells. 10 (6): 1508. doi:10.3390/cells10061508. PMC 8232593. PMID 34203839.
- ^ a b Chang, Hyun-Dong; Radbruch, Andreas (19 May 2021). "Maintenance of quiescent immune memory in the bone marrow". European Journal of Immunology. 51 (7): 1592–1601. doi:10.1002/eji.202049012. PMID 34010475.
- ^ Mahnke, Yolanda; Schwendemann, Jochen; Beckhove, Philipp; Schirrmacher, Volker (9 June 2005). "Maintenance of long-term tumour-specific T-cell memory by residual dormant tumour cells". Immunology. 115 (3): 325–336. doi:10.1111/j.1365-2567.2005.02163.x. PMC 1782166. PMID 15946250.
- ^ Collins, Nicolas; Han, Seong-Ji; Enamorado, Michel (22 August 2019). "The bone marrow protects and optimizes immunological memory during dietary restriction". Cell. 178 (5): 1088–1101. doi:10.1016/j.cell.2019.07.049. PMC 6818271. PMID 31442402.
- ^ Schirrmacher, Volker (12 October 2015). "Cancer-reactive memory T cells from bone marrow: Spontaneous induction and therapeutic potential (Review)". International Journal of Oncology. 47 (6): 2005–2016. doi:10.3892/ijo.2015.3197. PMID 26459860.
- ^ Schirrmacher, Volker (2023). "Bone marrow: The central immune system". Immuno. 3 (3): 289–329. doi:10.3390/immuno3030019.
- ^ "The Red Cell Membrane: structure and pathologies" (PDF). Australian Centre for Blood Diseases/Monash University. Retrieved 24 January 2015.
- ^ The Lymphatic System. Allonhealth.com. Retrieved 5 December 2011.
- ^ Fabricant, Florence. "Begging for Bones: A New Craving for Marrow". The New York Times. 16 September 1998.
- ^ Bonnet, D; Dick, JE (1997). "Human acute myeloid leukemia is organized as a hierarchy that originates from a primitive hematopoietic cell". Nature Medicine. 3 (7): 730–737. doi:10.1038/nm0797-730. PMID 9212098. S2CID 205381050.
- ^ a b "Bone Marrow Aspiration and Biopsy". Lab Tests Online UK. Retrieved 16 February 2013.
- ^ Ellmann, Stephan; Beck, Michael; Kuwert, Torsten; Uder, Michael; Bäuerle, Tobias (2015). "Multimodal imaging of bone metastases: From preclinical to clinical applications". Journal of Orthopaedic Translation. 3 (4): 166–177. doi:10.1016/j.jot.2015.07.004. PMC 5986987. PMID 30035055.
- ^ Nishida, Y; Matsue, Y; Suehara, Y; Fukumoto, K; Fujisawa, M; Takeuchi, M; Ouchi, E; Matsue, K (August 2015). "Clinical and prognostic significance of bone marrow abnormalities in the appendicular skeleton detected by low-doe whole-body multidetector computed tomography in patients with multiple myeloma". Blood Cancer Journal. 5 (7): e329. doi:10.1038/bcj.2015.57. ISSN 2044-5385. PMC 4526783. PMID 26230953.
- ^ Poulton, TB; Murphy, WD; Duerk, JL; Chapek, CC; Feiglin, DH (December 1993). "Bone marrow reconversion in adults who are smokers: MR Imaging findings". AJR. American Journal of Roentgenology. 161 (6): 1217–21. doi:10.2214/ajr.161.6.8249729. PMID 8249729.
- ^ Shah, LM; Hanrahan, CJ (December 2011). "MRI of spinal bone marrow: part I, techniques and normal age-related appearances". AJR. American Journal of Roentgenology. 197 (6): 1298–308. doi:10.2214/ajr.11.7005. PMID 22109283. S2CID 20115888.
- ^ Vande Berg, BC; Lecouvet, FE; Galant, C; Maldague, BE; Malghem, J (July 2005). "Normal variants and frequent marrow alterations that simulate bone marrow lesions at MR imaging". Radiologic Clinics of North America. 43 (4): 761–70, ix. doi:10.1016/j.rcl.2005.01.007. PMID 15893536.
- ^ "Definition: 'M:E Ratio'". Stedman's Medical Dictionary via MediLexicon.com. 2006. Archived from the original on 10 May 2013. Retrieved 20 December 2012.
- ^ "Bone marrow transplantation". UpToDate.com. Retrieved 12 April 2014.
- ^ "Antibody Transforms Stem Cells Directly into Brain Cells". Science Daily. 22 April 2013. Retrieved 24 April 2013.
- ^ "Research Supports Promise of Cell Therapy for Bowel Disease". Wake Forest Baptist Medical Center. 28 February 2013. Archived from the original on 8 August 2017. Retrieved 5 March 2013.
- ^ "Bone marrow 'frees men of HIV drugs'". BBC. 3 July 2013. Retrieved 3 July 2013.
- ^ "Stem-Cell Transplants Erase HIV in Two Men". PopSci. 3 July 2013. Retrieved 3 July 2013.
- ^ "HIV Returns in Two Men Thought 'Cured' by Bone Marrow Transplants". RH Reality Check. 10 December 2013. Retrieved 10 December 2013.
- ^ National Marrow Donor Program Donor Guide Archived 8 September 2008 at the Wayback Machine. Marrow.org. Retrieved 5 November 2012.
- ^ Bone marrow donation: What to expect when you donate. Mayo Clinic. Retrieved 16 February 2013.
- ^ McGuckin, C. P.; Forraz, N.; Baradez, M. -O.; Navran, S.; Zhao, J.; Urban, R.; Tilton, R.; Denner, L. (2005). "Production of stem cells with embryonic characteristics from human umbilical cord blood". Cell Proliferation. 38 (4): 245–255. doi:10.1111/j.1365-2184.2005.00346.x. PMC 6496335. PMID 16098183.
- ^ Herraiz, Sonia; Buigues, Anna; Díaz-García, César; Romeu, Mónica; Martínez, Susana; Gómez-Seguí, Inés; Simón, Carlos; Hsueh, Aaron J.; Pellicer, Antonio (May 2018). "Fertility rescue and ovarian follicle growth promotion by bone marrow stem cell infusion". Fertility and Sterility. 109 (5): 908–918.e2. doi:10.1016/j.fertnstert.2018.01.004.
- ^ a b Herraiz, Sonia; Buigues, Anna; Díaz-García, César; Romeu, Mónica; Martínez, Susana; Gómez-Seguí, Inés; Simón, Carlos; Hsueh, Aaron J.; Pellicer, Antonio (1 May 2018). "Fertility rescue and ovarian follicle growth promotion by bone marrow stem cell infusion". Fertility and Sterility. 109 (5): 908–918.e2. doi:10.1016/j.fertnstert.2018.01.004. PMID 29576341.
- ^ Patel, Nayana H.; Jadeja, Yuvraj D.; Patel, Niket H.; Patel, Molina N.; Bhadarka, Harsha K.; Chudasama, Piyush N.; Thakkar, Harmi R. (26 August 2021). "Birth of a healthy infant after bone marrow-derived cell therapy". Clinical and Experimental Reproductive Medicine. 48 (3): 268–272. doi:10.5653/cerm.2020.04252. PMC 8421658. PMID 34488290.
- ^ Badawy, Ahmed; Sobh, Mohamed A.; Ahdy, Mohamed; Abdelhafez, Mohamed Sayed (15 June 2017). "Bone marrow mesenchymal stem cell repair of cyclophosphamide-induced ovarian insufficiency in a mouse model". International Journal of Women's Health. 9: 441–447. doi:10.2147/IJWH.S134074. PMID 28670143.
- ^ Toppinen, Mari; Sajantila, Antti; Pratas, Diogo; Hedman, Klaus; Perdomo, Maria F. (2021). "The Human Bone Marrow Is Host to the DNAs of Several Viruses". Front. Cell. Infect. Microbiol. 11: 657245. doi:10.3389/fcimb.2021.657245. PMC 8100435. PMID 33968803.
- ^ a b c Sanchez, S.; Tafforeau, P.; Ahlberg, P. E. (2014). "The humerus of Eusthenopteron: a puzzling organization presaging the establishment of tetrapod limb bone marrow". Proceedings of the Royal Society B: Biological Sciences. 281 (1782): 20140299. doi:10.1098/rspb.2014.0299. PMC 3973280. PMID 24648231.
Further reading
[edit]- Nature Bone Marrow Transplantation (Nature Publishing Group) – specialist scientific journal with articles on bone marrow biology and clinical uses.
- Cooper, B (2011). "The origins of bone marrow as the seedbed of our blood: from antiquity to the time of Osler". Baylor University Medical Center Proceedings. 24 (2): 115–8. doi:10.1080/08998280.2011.11928697. PMC 3069519. PMID 21566758.
- Wang J, Liu X, Lu H, Jiang C, Cui X, Yu L, Fu X, Li Q, Wang J (2015). "CXCR4(+)CD45(-) BMMNC subpopulation is superior to unfractionated BMMNCs for protection after ischemic stroke in mice". Brain Behav. Immun. 45: 98–108. doi:10.1016/j.bbi.2014.12.015. PMC 4342301. PMID 25526817.
