Lung cancer: Difference between revisions
No edit summary |
Biosthmors (talk | contribs) Undid revision 476676757 by 151.188.213.173 (talk) |
||
| Line 15: | Line 15: | ||
}} |
}} |
||
'''Lung cancer''' is |
'''Lung cancer''' is a disease characterized by uncontrolled [[cell growth]] in [[tissue (biology)|tissues]] of the [[lung]]. If left untreated, this growth can spread beyond the lung in a process called [[metastasis]] into nearby tissue and, eventually, into other parts of the body. Most cancers that start in lung, known as primary lung cancers, are [[carcinomas]] that derive from [[epithelium|epithelial]] cells. Worldwide, lung [[cancer]] is the most common cause of cancer-related death in men and women, and is responsible for [[:Category:Deaths from lung cancer|1.3 million deaths]] |
||
annually, as of 2004.<ref name="WHO" /> The most common [[symptom]]s are shortness of breath, coughing (including [[Hemoptysis|coughing up blood]]), and weight loss.<ref name="Harrison" /> |
annually, as of 2004.<ref name="WHO" /> The most common [[symptom]]s are shortness of breath, coughing (including [[Hemoptysis|coughing up blood]]), and weight loss.<ref name="Harrison" /> |
||
Revision as of 17:49, 13 February 2012
| Lung cancer | |
|---|---|
| Specialty | Oncology, pulmonology |
Lung cancer is a disease characterized by uncontrolled cell growth in tissues of the lung. If left untreated, this growth can spread beyond the lung in a process called metastasis into nearby tissue and, eventually, into other parts of the body. Most cancers that start in lung, known as primary lung cancers, are carcinomas that derive from epithelial cells. Worldwide, lung cancer is the most common cause of cancer-related death in men and women, and is responsible for 1.3 million deaths annually, as of 2004.[1] The most common symptoms are shortness of breath, coughing (including coughing up blood), and weight loss.[2]
The main types of lung cancer are small-cell lung cancer (SCLC), also called oat cell cancer, and non-small-cell lung cancer (NSCLC). The most common cause of lung cancer is long-term exposure to tobacco smoke.[3] Nonsmokers account for 15% of lung cancer cases,[4] and these cases are often attributed to a combination of genetic factors,[5][6] radon gas,[7] asbestos,[8] and air pollution[9][10][11] including secondhand smoke.[12][13]
Lung cancer may be seen on chest radiograph and computed tomography (CT scan). The diagnosis is confirmed with a biopsy. This is usually performed by bronchoscopy or CT-guided biopsy. Treatment and prognosis depend on the histological type of cancer, the stage (degree of spread), and the patient's general wellbeing, measured by performance status. Common treatments include surgery, chemotherapy, and radiotherapy. NSCLC is sometimes treated with surgery, whereas SCLC usually responds better to chemotherapy and radiation therapy. This is partly because SCLC often spreads quite early, and these treatments are generally better at getting to cancer cells that have spread to other parts of the body.[14]
Survival depends on stage, overall health, and other factors, but overall 14% of people in the United States diagnosed with lung cancer survive five years after the diagnosis.[2]
Signs and symptoms
Symptoms that may suggest lung cancer include:[15]
- dyspnea (shortness of breath)
- hemoptysis (coughing up blood)
- chronic coughing or change in regular coughing pattern
- wheezing
- chest pain or pain in the abdomen
- cachexia (weight loss), fatigue, and loss of appetite
- dysphonia (hoarse voice)
- clubbing of the fingernails (uncommon)
- dysphagia (difficulty swallowing).
If the cancer grows in the airway, it may obstruct airflow, causing breathing difficulties. The obstruction can lead to accumulation of secretions behind the blockage, and predispose to pneumonia. Many lung cancers have a rich blood supply. The surface of the cancer may be fragile, leading to bleeding from the cancer into the airway. This blood may subsequently be coughed up.
Depending on the type of tumor, so-called paraneoplastic phenomena may initially attract attention to the disease.[16] In lung cancer, these phenomena may include Lambert-Eaton myasthenic syndrome (muscle weakness due to auto-antibodies), hypercalcemia, or syndrome of inappropriate antidiuretic hormone (SIADH). Tumors in the top (apex) of the lung, known as Pancoast tumors,[17] may invade the local part of the sympathetic nervous system, leading to changed sweating patterns and eye muscle problems (a combination known as Horner's syndrome) as well as muscle weakness in the hands due to invasion of the brachial plexus.
Many of the symptoms of lung cancer (bone pain, fever, and weight loss) are nonspecific; in the elderly, these may be attributed to comorbid illness.[14] In many patients, the cancer has already spread beyond the original site by the time they have symptoms and seek medical attention. Common sites of metastasis include the brain, bone, adrenal glands, contralateral (opposite) lung, liver, pericardium, and kidneys.[18] About 10% of people with lung cancer do not have symptoms at diagnosis; these cancers are incidentally found on routine chest radiograph.[2]
Causes
The main causes of any cancer include carcinogens (such as those in tobacco smoke), ionizing radiation, and viral infection. This exposure causes cumulative changes to the DNA in the tissue lining the bronchi of the lungs (the bronchial epithelium). As more tissue becomes damaged, eventually a cancer develops.[14]
Smoking

Smoking, particularly of cigarettes, is by far the main contributor to lung cancer.[19] Cigarette smoke contains over 60 known carcinogens,[20] including radioisotopes from the radon decay sequence, nitrosamine, and benzopyrene. Additionally, nicotine appears to depress the immune response to malignant growths in exposed tissue.[21] Across the developed world, 91% of lung cancer deaths in men during the year 2000 were attributed to smoking (71% for women).[22] In the United States, smoking is estimated to account for 87% of lung cancer cases (90% in men and 85% in women).[23] Among male smokers, the lifetime risk of developing lung cancer is 17.2%; among female smokers, the risk is 11.6%. This risk is significantly lower in nonsmokers: 1.3% in men and 1.4% in women.[24]
Women who smoke (former smokers and current smokers) and take hormone therapy are at a much higher risk of dying of lung cancer. In a study by Chlebowski et al. published in 2009, the women taking hormones were about 60% more likely to die of lung cancer than the women taking a placebo. Not surprisingly, the risk was highest for current smokers, followed by past smokers, and lowest for those who have never smoked. Among the women who smoked (former or current smokers), 3.4% of those taking hormone therapy died of lung cancer compared to 2.3% for women taking the placebo.[25]
The time a person smokes (as well as rate of smoking) increases the person's chance of developing lung cancer. If a person stops smoking, this chance steadily decreases as damage to the lungs is repaired and contaminant particles are gradually removed.[26] In addition, there is evidence that lung cancer in never-smokers has a better prognosis than in smokers,[27] and that patients who smoke at the time of diagnosis have shorter survival times than those who have quit.[28]
Passive smoking—the inhalation of smoke from another's smoking—is a cause of lung cancer in nonsmokers. A passive smoker can be classified as someone living or working with a smoker. Studies from the U.S.,[29] Europe,[30] the UK,[31] and Australia[32] have consistently shown a significant increase in relative risk among those exposed to passive smoke. Recent investigation of sidestream smoke suggests that it is more dangerous than direct smoke inhalation.[33]
10–15% of lung cancer patients have never smoked.[34] That means between 20,000 to 30,000 never-smokers are diagnosed with lung cancer in the United States each year. Because of the five-year survival rate, each year in the U.S. more never-smokers die of lung cancer than do patients of leukemia, ovarian cancer, or AIDS.[35]
Radon gas
Radon is a colorless and odorless gas generated by the breakdown of radioactive radium, which in turn is the decay product of uranium, found in the Earth's crust. The radiation decay products ionize genetic material, causing mutations that sometimes turn cancerous. Radon exposure is the second major cause of lung cancer in the general population, after smoking[7] with the risk increasing 8–16% for every 100 Bq/m³ increase in the radon concentration.[36] Radon gas levels vary by locality and the composition of the underlying soil and rocks. For example, in areas such as Cornwall in the UK (which has granite as substrata), radon gas is a major problem, and buildings have to be force-ventilated with fans to lower radon gas concentrations. The United States Environmental Protection Agency (EPA) estimates that one in 15 homes in the U.S. has radon levels above the recommended guideline of 4 picocuries per liter (pCi/L) (148 Bq/m³).[37] Iowa has the highest average radon concentration in the United States; studies performed there have demonstrated a 50% increased lung cancer risk, with prolonged radon exposure above the EPA's action level of 4 pCi/L.[38]
Asbestos

Asbestos can cause a variety of lung diseases, including lung cancer. There is a synergistic effect between tobacco smoking and asbestos in the formation of lung cancer.[8] In the UK, asbestos accounts for 2–3% of male lung cancer deaths.[39] Asbestos can also cause cancer of the pleura, called mesothelioma (which is different from lung cancer).
Viruses
Viruses are known to cause lung cancer in animals,[40][41] and recent evidence suggests similar potential in humans. Implicated viruses include human papillomavirus,[42] JC virus,[43] simian virus 40 (SV40), BK virus, and cytomegalovirus.[44] These viruses may affect the cell cycle and inhibit apoptosis, allowing uncontrolled cell division.
Particulate matter
Studies of the American Cancer Society cohort directly link the exposure to particulate matter with lung cancer. For example, if the concentration of particles in the air increases by only 1%, the risk of developing a lung cancer increases by 14%.[45][46] Further, it has been established that particle size matters, as ultrafine particles penetrate further into the lungs.[47]
Pathogenesis
Similar to many other cancers, lung cancer is initiated by activation of oncogenes or inactivation of tumor suppressor genes.[48] Oncogenes are genes that are believed to make people more susceptible to cancer. Proto-oncogenes are believed to turn into oncogenes when exposed to particular carcinogens.[49] Mutations in the K-ras proto-oncogene are responsible for 10–30% of lung adenocarcinomas.[50][51] The epidermal growth factor receptor (EGFR) regulates cell proliferation, apoptosis, angiogenesis, and tumor invasion.[50] Mutations and amplification of EGFR are common in non-small-cell lung cancer and provide the basis for treatment with EGFR-inhibitors. Her2/neu is affected less frequently.[50] Chromosomal damage can lead to loss of heterozygosity. This can cause inactivation of tumor suppressor genes. Damage to chromosomes 3p, 5q, 13q, and 17p are particularly common in small-cell lung carcinoma. The p53 tumor suppressor gene, located on chromosome 17p, is affected in 60-75% of cases.[52] Other genes that are often mutated or amplified are c-MET, NKX2-1, LKB1, PIK3CA, and BRAF.[50]
Several genetic polymorphisms are associated with lung cancer. These include polymorphisms in genes coding for interleukin-1,[53] cytochrome P450,[54] apoptosis promoters such as caspase-8,[55] and DNA repair molecules such as XRCC1.[56] People with these polymorphisms are more likely to develop lung cancer after exposure to carcinogens.
A recent study suggested that the MDM2 309G allele is a low-penetrant risk factor for developing lung cancer in Asians.[57]
Diagnosis

Performing a chest radiograph is the first step if a patient reports symptoms that may suggest lung cancer. This may reveal an obvious mass, widening of the mediastinum (suggestive of spread to lymph nodes there), atelectasis (collapse), consolidation (pneumonia), or pleural effusion. If there are no radiographic findings but the suspicion is high (such as a heavy smoker with blood-stained sputum), bronchoscopy and/or a CT scan may provide the necessary information. Bronchoscopy or CT-guided biopsy is often used to identify the tumor type.[2]
Abnormal findings in cells ("atypia") in sputum are associated with an increased risk of lung cancer. Sputum cytologic examination combined with other screening examinations may have a role in the early detection of lung cancer.[58]

The differential diagnosis for patients who present with abnormalities on chest radiograph includes lung cancer as well as nonmalignant diseases. These include infectious causes such as tuberculosis or pneumonia, or inflammatory conditions such as sarcoidosis. These diseases can result in mediastinal lymphadenopathy or lung nodules, and sometimes mimic lung cancers.[14] Lung cancer can also be an incidental finding: a solitary pulmonary nodule (also called a coin lesion) on a chest radiograph or CT scan taken for an unrelated reason. The definitive diagnosis of lung cancer and its classification (described above) is based on examination of the suspicious tissue under the microscope by a pathologist.
Classification
Lung cancers are classified according to histological type. This classification has important implications for clinical management and prognosis of the disease. The vast majority of lung cancers are carcinomas—malignancies that arise from epithelial cells. The two most prevalent histological types of lung carcinoma, categorized by the size and appearance of the malignant cells seen by a histopathologist under a microscope, are non-small-cell and small-cell lung carcinoma.[59] The non-small-cell type is the most prevalent by far (see accompanying table).
| Histological type | Frequency (%) |
|---|---|
| Non-small-cell lung carcinoma | 80.4 |
| Small-cell lung carcinoma | 16.8 |
| Carcinoid[60] | 0.8 |
| Sarcoma[61] | 0.1 |
| Unspecified lung cancer | 1.9 |
Cancer found outside of the lung may be determined to have arisen within the lung, as lung cancers that metastasize, i.e. spread, often retain a cell marker profile that allow a pathologist to say, with a good deal of certainty, that the tumor arose from the lung, i.e. is a primary lung cancer. Primary lung cancers of adenocarcinoma histology typically have nuclear immunostaining with TTF-1.[62][63]
Non-small-cell lung carcinoma

The non-small-cell lung carcinomas (NSCLC) are grouped together because their prognosis and management are similar. There are three main sub-types: squamous cell lung carcinoma, adenocarcinoma, and large-cell lung carcinoma.
| Histological sub-type | Frequency of non-small-cell lung cancers (%) | ||
|---|---|---|---|
| Smokers | Never-smokers | ||
| Squamous cell lung carcinoma | 42 | 33 | |
| Adenocarcinoma | Adenocarcinoma (not otherwise specified) | 39 | 35 |
| Bronchioloalveolar carcinoma | 4 | 10 | |
| Carcinoid | 7 | 16 | |
| Other | 8 | 6 | |

Accounting for 25% of lung cancers,[66] squamous cell lung carcinoma usually starts near a central bronchus. A hollow cavity and associated necrosis are commonly found at the center of the tumor. Well-differentiated squamous cell lung cancers often grow more slowly than other cancer types.[14]
Adenocarcinoma accounts for 40% of non-small-cell lung cancers.[66] It usually originates in peripheral lung tissue. Most cases of adenocarcinoma are associated with smoking; however, among people who have never smoked ("never-smokers"), adenocarcinoma is the most common form of lung cancer.[67] A subtype of adenocarcinoma, the bronchioloalveolar carcinoma, is more common in female never-smokers, and may have different responses to treatment.[68]
Small-cell lung carcinoma

Small-cell lung carcinoma (SCLC) is less common. It was formerly referred to as "oat-cell" carcinoma.[69] Most cases arise in the larger airways (primary and secondary bronchi) and grow rapidly, becoming quite large.[70] The small cells contain dense neurosecretory granules (vesicles containing neuroendocrine hormones), which give this tumor an endocrine/paraneoplastic syndrome association.[71] While initially more sensitive to chemotherapy and radiation, it is often metastatic at presentation, and ultimately carries a worse prognosis. Small-cell lung cancers have long been dichotomously staged into limited and extensive stage disease. This type of lung cancer is strongly associated with smoking.[72]
Others
Lung cancers are highly heterogeneous malignancies, with tumors containing more than one subtype being very common.[73]
Currently, the most widely recognized and utilized lung cancer classification system is the 4th revision of the Histological Typing of Lung and Pleural Tumours, published in 2004 as a cooperative effort by the World Health Organization and the International Association for the Study of Lung Cancer. It recognizes numerous other distinct histopathological entities of non-small-cell lung carcinoma, organized into several additional subtypes, including sarcomatoid carcinoma, salivary gland tumors, carcinoid tumor, and adenosquamous carcinoma. The latter subtype includes tumors containing at least 10% each of adenocarcinoma and squamous cell carcinoma. When a tumor is found to contain a mixture of both small-cell carcinoma and non-small-cell carcinoma, it is classified as a variant of small-cell carcinoma and called a combined small-cell carcinoma. Combined small-cell carcinoma is the only currently recognized variant of small-cell carcinoma.
In infants and children, the most common primary lung cancers are pleuropulmonary blastoma and carcinoid tumor.[74]
Metastasis

The lung is a common place for metastasis of tumors from other parts of the body. Secondary cancers are classified by the site of origin; e.g., breast cancer that has spread to the lung is called breast cancer. Metastases often have a characteristic round appearance on chest radiograph.[75] Solitary round lung nodules are not infrequently of an uncertain etiology and may prompt a lung biopsy.
In children, the majority of lung cancers are secondary.[74]
Primary lung cancers themselves most commonly metastasize to the adrenal glands, liver, brain, and bone.[14]
Staging
Lung cancer staging is an assessment of the degree of spread of the cancer from its original source. In most studies, it is the most important factor affecting the prognosis and potential treatment of lung cancer.
Staging varies for the two major cell types of lung cancer (non-small cell lung carcinoma and small cell lung carcinoma). It is normally done prior to attempts at curative therapy, and usually consists of an extensive battery of tests, to include physical examination, laboratory tests, imaging studies, and/or biopsies and other invasive procedures (such as mediastinoscopy). Non-small cell lung carcinoma is usually staged from IA ("one A"; best prognosis) to IV ("four"; worst prognosis).[76] Small cell lung carcinoma has traditionally been classified as limited stage (confined to one half of the chest and within the scope of a single tolerable radiotherapy field) or extensive stage (more widespread disease).
For both NSCLC and SCLC, there are two general types of staging evaluations:
Clinical Staging: evaluated prior to definitive surgery, and typically based on the results of physical examination, imaging studies, and pertinent laboratory findings. Does not necessarily involve a pathologist.
Pathological Staging: usually evaluated either intra- or post-operatively, and based on the combined results of surgical and clinical findings.[70]
Prevention
Prevention is the most cost-effective means of fighting lung cancer. While in most countries industrial and domestic carcinogens have been identified and banned, tobacco smoking is still widespread. Eliminating tobacco smoking is a primary goal in the prevention of lung cancer, and smoking cessation is an important preventive tool in this process.[77] Of utmost importance are prevention programs that target the young. In 1998 the Master Settlement Agreement entitled 46 states in the USA to an annual payout from the tobacco companies.[78] Between the settlement money and tobacco taxes, each state's public health department funds their prevention programs, although none of the states are living up to the Center for Disease Control's recommended amount by spending 15 percent of tobacco taxes and settlement revenues on these prevention efforts.[78]
Policy interventions to decrease passive smoking in public areas such as restaurants and workplaces have become more common in many Western countries, with California taking a lead in banning smoking in public establishments in 1998. Ireland played a similar role in Europe in 2004, followed by Italy and Norway in 2005, Scotland as well as several others in 2006, England in 2007, France in 2008 and Turkey in 2009. New Zealand has banned smoking in public places as of 2004. The state of Bhutan has had a complete smoking ban since 2005.[79] In many countries, pressure groups are campaigning for similar bans. In 2007, Chandigarh became the first city in India to become smoke-free. India introduced a total ban on smoking in public places on 2 October 2008.
Arguments cited against such bans are criminalization of smoking, increased risk of smuggling, and the risk that such a ban cannot be enforced.[80]
The long-term use of supplemental multivitamins—such as vitamin C, vitamin E, and folate—does not reduce the risk of lung cancer. Indeed long-term intake of high doses of vitamin E supplements may even increase the risk of lung cancer.[81] However, eating at least five servings of fruits and vegetables per day and following a diet that conforms to the American Cancer Society's guidelines may help lower risk.[82]
The World Health Organization has called for governments to institute a total ban on tobacco advertising to prevent young people from taking up smoking. They assess that such bans have reduced tobacco consumption by 16% where already instituted.[83]
Screening
Screening refers to the use of medical tests to detect disease in asymptomatic people. Possible screening tests for lung cancer include chest radiograph, or computed tomography (CT). As of December 2009, screening programs for lung cancer have not demonstrated any benefit.[84][85]
Treatment
Treatment for lung cancer depends on the cancer's specific cell type, how far it has spread, and the patient's performance status. Common treatments include palliative care,[86] surgery, chemotherapy, and radiation therapy.[2][87]
Surgery

If investigations confirm lung cancer, CT scan and often positron emission tomography (PET) are used to determine whether the disease is localized and amenable to surgery or whether it has spread to the point where it cannot be cured surgically.
Blood tests and spirometry (lung function testing) are also necessary to assess whether the patient is well enough to be operated on. If spirometry reveals poor respiratory reserve (often due to chronic obstructive pulmonary disease), surgery may be contraindicated.
Surgery for lung cancer has an operative death rate of about 4.4%, depending on the patient's lung function and other risk factors.[88] In non-small-cell lung carcinoma, surgery is usually only an option if the cancer is limited to one lung, up to stage IIIA. This is assessed with medical imaging (computed tomography, positron emission tomography). A sufficient preoperative respiratory reserve must be present to allow adequate lung function after the tissue is removed.
Procedures include wedge resection (removal of part of a lobe), segmentectomy (removal of an anatomic division of a particular lobe of the lung), lobectomy (one lobe), bilobectomy (two lobes), or pneumonectomy (whole lung). In patients with adequate respiratory reserve, lobectomy is the preferred option, as this minimizes the chance of local recurrence. If the patient does not have enough functional lung for this, wedge resection may be performed.[89] Radioactive iodine brachytherapy at the margins of wedge excision may reduce recurrence to that of lobectomy.[90]
Video-assisted thoracoscopic surgery and VATS lobectomy have allowed for minimally invasive approaches to lung cancer surgery that may have the advantages of quicker recovery, shorter hospital stay and diminished hospital costs.[91]
Early studies suggested that small-cell lung carcinoma (SCLC) fared better when treated with chemotherapy and/or radiation than when treated surgically.[92][93] While this approach to treating SCLC remains the current standard of care,[94] the role of surgery in SCLC is being reconsidered, recent reviews indicating that surgery might improve outcomes when added to chemotherapy and radiation in early stage SCLC[95] and combined forms of SCLC and NSCLC.[96]
Radiotherapy
Radiotherapy is often given together with chemotherapy, and may be used with curative intent in patients with non-small-cell lung carcinoma who are not eligible for surgery. This form of high intensity radiotherapy is called radical radiotherapy.[97] A refinement of this technique is continuous hyperfractionated accelerated radiotherapy (CHART), in which a high dose of radiotherapy is given in a short time period.[98] For small-cell lung carcinoma cases that are potentially curable, chest radiation is often recommended in addition to chemotherapy.[99] The use of adjuvant thoracic radiotherapy following curative intent surgery for non-small-cell lung carcinoma is not well established and is controversial. Benefits, if any, may only be limited to those in whom the tumor has spread to the mediastinal lymph nodes.[100][101]
For both non-small-cell lung carcinoma and small-cell lung carcinoma patients, smaller doses of radiation to the chest may be used for symptom control (palliative radiotherapy). Unlike other treatments, it is possible to deliver palliative radiotherapy without confirming the histological diagnosis of lung cancer.
Brachytherapy (localized radiotherapy) may be given directly inside the airway when cancer affects a short section of bronchus.[102] It is used when inoperable lung cancer causes blockage of a large airway.[103]
Patients with limited-stage small-cell lung carcinoma are usually given prophylactic cranial irradiation (PCI). This is a type of radiotherapy to the brain, used to reduce the risk of metastasis.[104] More recently, PCI has also been shown to be beneficial in those with extensive small-cell lung cancer. In patients whose cancer has improved following a course of chemotherapy, PCI has been shown to reduce the cumulative risk of brain metastases within one year from 40.4% to 14.6%.[105]
Recent improvements in targeting and imaging have led to the development of extracranial stereotactic radiation in the treatment of early-stage lung cancer. In this form of radiation therapy, very high doses are delivered in a small number of sessions using stereotactic targeting techniques. Its use is primarily in patients who are not surgical candidates due to medical comorbidities.[106]
Chemotherapy
The chemotherapy regimen depends on the tumor type.
Small-cell lung carcinoma
Even if relatively early stage, small-cell lung carcinoma is treated primarily with chemotherapy and radiation.[107] In small-cell lung carcinoma, cisplatin and etoposide are most commonly used.[108] Combinations with carboplatin, gemcitabine, paclitaxel, vinorelbine, topotecan, and irinotecan are also used.[109][110] Celecoxib showed a potential signal of response in a small study.[111]
Non-small-cell lung carcinoma
Primary chemotherapy is also given in advanced and metastatic non-small-cell lung carcinoma.
Testing for the molecular genetic subtype of non-small-cell lung cancer may be of assistance in selecting the most appropriate initial therapy[112] For example, mutation of the epidermal growth factor receptor gene[113] may predict whether initial treatment with a specific inhibitor or with chemotherapy is more advantageous.[114]
Advanced non-small-cell lung carcinoma is often treated with cisplatin or carboplatin, in combination with gemcitabine, paclitaxel, docetaxel, etoposide, or vinorelbine.[115] Bevacizumab improves results in non-squamous cancers treated with paclitaxel and carboplatin in patients less than 70 years old who have reasonable general performance status.[116]
Pemetrexed has been approved for use in non-small-cell lung cancer.[117] For adenocarcinoma and large-cell lung cancer, cisplatin with pemetrexed was more beneficial than cisplatin and gemcitabine; squamous cancer had the opposite results.[118] As a consequence, subtyping of non-small lung cancer histology has become more important.[119]
The U.S. Food and Drug Administration (FDA) approved erlotinib (Tarceva)[120] for the treatment of locally advanced or metastatic non-small cell lung cancer that has failed at least one prior chemotherapy regimen,[121] and has also approved its use as maintenance treatment in locally advanced or metastatic non-small cell lung cancer that has not progressed after four cycles of platinum-based first-line chemotherapy.[121]
The U.S. Food and Drug Administration approved crizotinib (Xalkori) to treat certain late-stage (locally advanced or metastatic) non-small cell lung cancers that express the abnormal anaplastic lymphoma kinase (ALK) gene.[122]
Bronchoalveolar carcinoma is a subtype of non-small-cell lung carcinoma that may respond to gefitinib[123] and erlotinib.[124]
Maintenance therapy
In advanced non-small-cell lung cancer there are several approaches for continuing treatment after an initial response to therapy.[125] Switch maintenance changes to different medications than the initial therapy and can use pemetrexed,[126] erlotinib,[127] and docetaxel,[128] although pemetrexed is only used in non-squamous NSCLC.[129]
Adjuvant chemotherapy
Adjuvant chemotherapy refers to the use of chemotherapy after apparently curative surgery to improve the outcome. In non-small-cell lung cancer, samples are taken during surgery of nearby lymph nodes. If these samples contain cancer, the patient has stage II or III disease. In this situation, adjuvant chemotherapy may improve survival by up to 15%.[130][131] Standard practice has often been to offer platinum-based chemotherapy (including either cisplatin or carboplatin).[132] However, the benefit of platinum-based adjuvant chemotherapy was confined to patients who had tumors with low ERCC1 (excision repair cross-complementing 1) activity.[133]
Adjuvant chemotherapy for patients with stage IB cancer is controversial, as clinical trials have not clearly demonstrated a survival benefit.[134][135] Trials of preoperative chemotherapy (neoadjuvant chemotherapy) in resectable non-small-cell lung carcinoma have been inconclusive.[136]
Interventional radiology
Radiofrequency ablation should currently be considered an investigational technique in the treatment of bronchogenic carcinoma. It is done by inserting a small heat probe into the tumor to kill the tumor cells.[137]
Palliative care
In a 2010 study of patients with metastatic non–small-cell lung cancer, early palliative care led to significant improvements in both quality of life and mood. As compared with patients receiving standard care, patients receiving early palliative care had less aggressive care at the end of life but longer survival" (increased by 3 months).[86]
Other studies in advanced cancer also found benefit from palliative care,[138] or found hospice involvement to be beneficial.[139] These approaches allow additional discussion of treatment options and provide opportunities to arrive at well-considered decisions[140][141] and may avoid unhelpful but expensive care at the end of life.[141]
Chemotherapy may be combined with palliative care in the treatment of the non-small-cell lung cancer. In advanced NSCLC, a 1994 meta-analysis found that appropriate chemotherapy improved average survival over supportive care alone,[142] as well as improving quality of life.[143] With adequate physical fitness, maintaining chemotherapy during lung cancer palliation offers a 1.5 to 3 months prolongation of survival, symptomatic relief and an improvement in quality of life, with better results seen with modern agents.[144][145] Since 2008, the NSCLC Meta-Analyses Collaborative Group has recommended that if the recipient wants and can tolerate treatment then chemotherapy should be considered in advanced NSCLC.[146][147]
Prognosis
Prognostic factors in non-small-cell lung cancer include presence or absence of pulmonary symptoms, tumor size, cell type (histology), degree of spread (stage) and metastases to multiple lymph nodes, and vascular invasion. For patients with inoperable disease, prognosis is adversely affected by poor performance status and weight loss of more than 10%.[148] Prognostic factors in small-cell lung cancer include performance status, gender, stage of disease, and involvement of the central nervous system or liver at the time of diagnosis.[149]
For non-small-cell lung carcinoma (NSCLC), prognosis is generally poor. Following complete surgical resection of stage IA disease, five-year survival is 67%. With stage IB disease, five-year survival is 57%.[150] The five-year survival rate of patients with stage IV NSCLC is about 1%.[3]
For small-cell lung carcinoma, prognosis is also generally poor. The overall five-year survival for patients with SCLC is about 5%.[2] Patients with extensive-stage SCLC have an average five-year survival rate of less than 1%. The median survival time for limited-stage disease is 20 months, with a five-year survival rate of 20%.[3]
According to data provided by the National Cancer Institute, the median age at diagnosis of lung cancer in the United States is 70 years,[151] and the median age at death is 72 years.[152]
Epidemiology

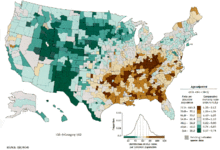
Worldwide, lung cancer is the most common cancer in terms of both incidence and mortality (1.1 million new cases per year and 0.95 million deaths in males and 0.51 million new cases per year and 0.43 million deaths in females).[154] The highest rates are in Europe and North America.[155] The population segment most likely to develop lung cancer is over-fifties who have a history of smoking. Lung cancer is the second most commonly occurring form of cancer in most Western countries, and it is the leading cancer-related cause of death. In contrast to the mortality rate in men, which began declining more than 20 years ago, women's lung cancer mortality rates have been rising over the last decades, and are just recently beginning to stabilize.[156] The evolution of "Big Tobacco" plays a significant role in the smoking culture.[157] Tobacco companies have focused their efforts since the 1970s at marketing their product toward women and girls, especially with "light" and "low-tar" cigarettes.[158] Among lifetime nonsmokers, men have higher age-standardized lung cancer death rates than women.
Not all cases of lung cancer are due to smoking, but the role of passive smoking is increasingly being recognized as a risk factor for lung cancer—leading to policy interventions to decrease undesired exposure of nonsmokers to others' tobacco smoke. Emissions from automobiles, factories, and power plants also pose potential risks.[9][11][159]
Eastern Europe has the highest lung cancer mortality among men, while northern Europe and the U.S. have the highest mortality among women. In the United States, black men and women have a higher incidence.[160] Lung cancer incidence is currently less common in developing countries.[161] With increased smoking in developing countries, the incidence is expected to increase in the next few years, notably in China[162] and India.[163]
Lung cancer incidence (by country) has an inverse correlation with sunlight and UVB exposure. One possible explanation is a preventive effect of vitamin D, which is produced in the skin on exposure to sunlight.[164]
From the 1950s, the incidence of lung adenocarcinoma started to rise relative to other types of lung cancer.[165] This is partly due to the introduction of filter cigarettes. The use of filters removes larger particles from tobacco smoke, thus reducing deposition in larger airways. However the smoker has to inhale more deeply to receive the same amount of nicotine, increasing particle deposition in small airways where adenocarcinoma tends to arise.[166] The incidence of lung adenocarcinoma in the U.S. has fallen since 1999. This may be due to reduction in environmental air pollution.[165] However, in some developing countries like India, there has been little change in the epidemiology with squamous cell carcinoma continuing to be the predominant histological type.[167][168][169] An absence of change in the type of tobacco smoking or the pattern of tobacco consumption in the population could be one of the possible reasons.
History
Lung cancer was uncommon before the advent of cigarette smoking; it was not even recognized as a distinct disease until 1761.[170] Different aspects of lung cancer were described further in 1810.[171] Malignant lung tumors made up only 1% of all cancers seen at autopsy in 1878, but had risen to 10–15% by the early 1900s.[172] Case reports in the medical literature numbered only 374 worldwide in 1912,[173] but a review of autopsies showed that the incidence of lung cancer had increased from 0.3% in 1852 to 5.66% in 1952.[174] In Germany in 1929, physician Fritz Lickint recognized the link between smoking and lung cancer,[172] which led to an aggressive antismoking campaign.[175] The British Doctors Study, published in the 1950s, was the first solid epidemiological evidence of the link between lung cancer and smoking.[176] As a result, in 1964 the Surgeon General of the United States recommended that smokers should stop smoking.[177]
The connection with radon gas was first recognized among miners in the Ore Mountains near Schneeberg, Saxony. Silver has been mined there since 1470, and these mines are rich in uranium, with its accompanying radium and radon gas. Miners developed a disproportionate amount of lung disease, eventually recognized as lung cancer in the 1870s. An estimated 75% of former miners died from lung cancer.[178] Despite this discovery, mining continued into the 1950s, due to the USSR's demand for uranium.[179]
The first successful pneumonectomy for lung cancer was performed in 1933.[180] Palliative radiotherapy has been used since the 1940s.[181] Radical radiotherapy, initially used in the 1950s, was an attempt to use larger radiation doses in patients with relatively early stage lung cancer but who were otherwise unfit for surgery.[182] In 1997, continuous hyperfractionated accelerated radiotherapy (CHART) was seen as an improvement over conventional radical radiotherapy.[98]
With small-cell lung carcinoma, initial attempts in the 1960s at surgical resection[183] and radical radiotherapy[184] were unsuccessful. In the 1970s, successful chemotherapy regimens were developed.[185]
References
- ^ WHO (2006). "Cancer". World Health Organization. Retrieved 2007-06-25.
{{cite web}}: Unknown parameter|month=ignored (help) - ^ a b c d e f Minna, JD (2008). Harrison's Principles of Internal Medicine (17th ed.). McGraw-Hill. pp. 551–562. ISBN 0-07-146633-9.
{{cite book}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ a b c "Lung Carcinoma: Tumors of the Lungs". Merck Manual Professional Edition, Online edition. Retrieved 2007-08-15.
- ^ Thun, MJ (2008). Adami, Hans-Olov (ed.). "Lung Cancer Occurrence in Never-Smokers: An Analysis of 13 Cohorts and 22 Cancer Registry Studies". PLoS Medicine. 5 (9): e185. doi:10.1371/journal.pmed.0050185. PMC 2531137. PMID 18788891.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help)CS1 maint: unflagged free DOI (link) - ^ Gorlova, OY (2007). "Aggregation of cancer among relatives of never-smoking lung cancer patients". International Journal of Cancer. 121 (1): 111–118. doi:10.1002/ijc.22615. PMID 17304511.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Hackshaw, AK (1997-10-18). "The accumulated evidence on lung cancer and environmental tobacco smoke". British Medical Journal. 315 (7114): 980–988. PMC 2127653. PMID 9365295.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ a b Catelinois O, Rogel A, Laurier D; et al. (2006). "Lung Cancer Attributable to Indoor Radon Exposure in France: Impact of the Risk Models and Uncertainty Analysis". Environ. Health Perspect. 114 (9): 1361–6. doi:10.1289/ehp.9070. PMC 1570096. PMID 16966089.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b O'Reilly, KM (2007). "Asbestos-related lung disease". American Family Physician. 75 (5): 683–688. PMID 17375514.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ a b Kabir, Z (2007). "Lung cancer and urban air-pollution in Dublin: a temporal association?". Irish Medical Journal. 100 (2): 367–369. PMID 17432813.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Coyle, YM (2006). "An ecological study of the association of metal air pollutants with lung cancer incidence in Texas". Journal of Thoracic Oncology. 1 (7): 654–661. doi:10.1097/01243894-200609000-00009. PMID 17409932.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ a b Chiu, HF (2006). "Outdoor air pollution and female lung cancer in Taiwan". Inhalation Toxicology. 18 (13): 1025–1031. doi:10.1080/08958370600904561. PMID 16966302.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Carmona, RH (2006-06-27). "The Health Consequences of Involuntary Exposure to Tobacco Smoke: A Report of the Surgeon General". U.S. Department of Health and Human Services.
Secondhand smoke exposure causes disease and premature death in children and adults who do not smoke.
- ^ "Tobacco Smoke and Involuntary Smoking" (PDF). IARC Monographs on the Evaluation of Carcinogenic Risks to Humans. 83. WHO International Agency for Research on Cancer. 2002.
There is sufficient evidence that involuntary smoking (exposure to secondhand or 'environmental' tobacco smoke) causes lung cancer in humans. [...] Involuntary smoking (exposure to secondhand or 'environmental' tobacco smoke) is carcinogenic to humans (Group 1).
- ^ a b c d e f Vaporciyan, AA (2000). Cancer Medicine. B C Decker. pp. 1227–1292. ISBN 1-55009-113-1.
{{cite book}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Hamilton, W (2005). "What are the clinical features of lung cancer before the diagnosis is made? A population based case-control study". Thorax. 60 (12). BMJ Publishing Group: 1059–1065. doi:10.1136/thx.2005.045880. PMC 1747254. PMID 16227326.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Honnorat, J (2007). "Paraneoplastic neurological syndromes". Orphanet Journal of Rare Diseases. 2 (1). BioMed Central: 22. doi:10.1186/1750-1172-2-22. PMC 1868710. PMID 17480225.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help)CS1 maint: unflagged free DOI (link) - ^ Jones, DR (1998). "Pancoast tumors of the lung". Current Opinion in Pulmonary Medicine. 4 (4): 191–197. doi:10.1097/00063198-199807000-00001. PMID 10813231.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Greene, Frederick L. (2002). AJCC cancer staging manual. Berlin: Springer-Verlag. ISBN 0-387-95271-3.
- ^ Biesalski, HK (1998). "European Consensus Statement on Lung Cancer: risk factors and prevention. Lung Cancer Panel". CA Cancer J Clin. 48 (3). Smoking is the major risk factor, accounting for about 90% of lung cancer incidence.: 167–176, discussion 164–166. doi:10.3322/canjclin.48.3.167. PMID 9594919.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help)CS1 maint: location (link) - ^ Hecht, S (2003). "Tobacco carcinogens, their biomarkers and tobacco-induced cancer". Nature Reviews. Cancer. 3 (10). Nature Publishing Group: 733–744. doi:10.1038/nrc1190. PMID 14570033.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Sopori, M (2002). "Effects of cigarette smoke on the immune system". Nature Reviews. Immunology. 2 (5): 372–7. doi:10.1038/nri803. PMID 12033743.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Peto, R (2006). Mortality from smoking in developed countries 1950–2000: Indirect estimates from National Vital Statistics. Oxford University Press. ISBN 0-19-262535-7.
{{cite book}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Samet, JM (1988). "Cigarette smoking and lung cancer in New Mexico". American Review of Respiratory Disease. 137 (5): 1110–1113. PMID 3264122.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Villeneuve, PJ (1994). "Lifetime probability of developing lung cancer, by smoking status, Canada". Canadian Journal of Public Health. 85 (6): 385–388. PMID 7895211.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Chlebowski RT; et al. (2009). "Non-small cell lung cancer and estrogen plus progestin use in postmenopausal women in the Women's Health Initiative randomized clinical trial". Journal of Clinical Oncology. 27 (155): CRA1500.
{{cite journal}}: Explicit use of et al. in:|author=(help) - ^ US Department of Health and Human Services (1990-09-30). "The Health Benefits of Smoking Cessation: a Report of the Surgeon General" (PDF). Centers for Disease Control (CDC), Office on Smoking and Health. pp. vi, 130, 148, 152, 155, 164, 166. Retrieved 2007-11-18.
- ^ Nordquist, LT (2004). "Improved survival in never-smokers vs current smokers with primary adenocarcinoma of the lung". Chest. 126 (2). American College of Chest Physicians: 347–351. doi:10.1378/chest.126.2.347. PMID 15302716.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Tammemagi, CM (2004). "Smoking and lung cancer survival: the role of comorbidity and treatment". Chest. 125 (1). American College of Chest Physicians: 27–37. doi:10.1378/chest.125.1.27. PMID 14718417.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Centers for Disease Control (CDC) (1986). "1986 Surgeon General's report: the health consequences of involuntary smoking". MMWR. Morbidity and mortality weekly report. 35 (50). CDC: 769–70. PMID 3097495. Retrieved 2007-08-10.
{{cite journal}}: Unknown parameter|month=ignored (help)
* National Research Council (1986). Environmental tobacco smoke: measuring exposures and assessing health effects. National Academy Press. ISBN 0-309-07456-8.
* EPA (1992). "Respiratory health effects of passive smoking: lung cancer and other disorders". EPA. Retrieved 2007-08-10.{{cite journal}}: Cite journal requires|journal=(help)
* California Environmental Protection Agency (1997). "Health effects of exposure to environmental tobacco smoke. California Environmental Protection Agency". Tobacco Control. 6 (4): 346–353. doi:10.1136/tc.6.4.346. PMC 1759599. PMID 9583639.
* CDC (2001). "State-specific prevalence of current cigarette smoking among adults, and policies and attitudes about secondhand smoke—United States, 2000". Morbidity and Mortality Weekly Report. 50 (49). Atlanta, Georgia: CDC: 1101–1106. PMID 11794619.{{cite journal}}: More than one of|author1=and|last=specified (help); Unknown parameter|month=ignored (help)
* Alberg, AJ (2003). "Epidemiology of lung cancer". Chest. 123 (S1). American College of Chest Physicians: 21S–49S. doi:10.1378/chest.123.1_suppl.21S. PMID 12527563.{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Boffetta, P (1998). "Multicenter case-control study of exposure to environmental tobacco smoke and lung cancer in Europe". Journal of the National Cancer Institute. 90 (19). Oxford University Press: 1440–1450. doi:10.1093/jnci/90.19.1440. PMID 9776409.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ "Report of the Scientific Committee on Tobacco and Health". Department of Health. 1998. Retrieved 2007-07-09.
{{cite web}}: Unknown parameter|month=ignored (help)
* Hackshaw, AK (1998). "Lung cancer and passive smoking". Statistical Methods in Medical Research. 7 (2): 119–136. doi:10.1191/096228098675091404. PMID 9654638.{{cite journal}}: Unknown parameter|month=ignored (help) - ^ National Health and Medical Research Council (April 1994). "The health effects and regulation of passive smoking". Australian Government Publishing Service. Archived from the original on September 29, 2007. Retrieved 2007-08-10.
{{cite journal}}: Cite journal requires|journal=(help) - ^ Schick, S (2005). "Philip Morris toxicological experiments with fresh sidestream smoke: more toxic than mainstream smoke". Tobacco Control. 14 (6): 396–404. doi:10.1136/tc.2005.011288. PMC 1748121. PMID 16319363.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Thun, M.J., S.J. Henley, D Burns, et al., Lung cancer death rates in lifelong nonsmokers. J. Natl Cancer Inst, 2006. 98: p.691.
- ^ Sun, S., J.H. Schiller and A.F. Gazdar, Lung cancer in never-smokers: A different disease. Nat Rev Cancer, 2007. 7: p.778-90.
- ^ Schmid K, Kuwert T, Drexler H (2010). "Radon in Indoor Spaces: An Underestimated Risk Factor for Lung Cancer in Environmental Medicine". Dtsch Arztebl Int. 107 (11): 181–6. doi:10.3238/arztebl.2010.0181. PMC 2853156. PMID 20386676.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ EPA (2006). "Radiation information: radon". EPA. Retrieved 2007-08-11.
{{cite web}}: Unknown parameter|month=ignored (help) - ^ Field, RW (1 June 2000). "Residential radon gas exposure and lung cancer: the Iowa Radon Lung Cancer Study". American Journal of Epidemiology. 151 (11). Oxford Journals: 1091–1102. PMID 10873134.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Darnton, AJ (2006). "Estimating the number of asbestos-related lung cancer deaths in Great Britain from 1980 to 2000". Annals of Occupational Hygiene. 50 (1): 29–38. doi:10.1093/annhyg/mei038. PMID 16126764.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Leroux, C (March–April 2007). "Jaagsiekte Sheep Retrovirus (JSRV): from virus to lung cancer in sheep". Veterinary Research. 38 (2): 211–228. doi:10.1051/vetres:2006060. PMID 17257570.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Palmarini, M (2001). "Retrovirus-induced ovine pulmonary adenocarcinoma, an animal model for lung cancer". Journal of the National Cancer Institute. 93 (21). Oxford University Press: 1603–1614. doi:10.1093/jnci/93.21.1603. PMID 11698564.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Cheng, YW (1 April 2001). "The association of human papillomavirus 16/18 infection with lung cancer among nonsmoking Taiwanese women". Cancer Research. 61 (7). American Association for Cancer Research: 2799–2803. PMID 11306446.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Zheng, H (2007). "Oncogenic role of JC virus in lung cancer". Journal of Pathology. 212 (3): 306–315. doi:10.1002/path.2188. PMID 17534844.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Giuliani, L (2007). "Detection of oncogenic viruses (SV40, BKV, JCV, HCMV, HPV) and p53 codon 72 polymorphism in lung carcinoma". Lung Cancer. 57 (3): 273–281. doi:10.1016/j.lungcan.2007.02.019. PMID 17400331.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Pope, CA 3rd (2002). "Lung cancer, cardiopulmonary mortality, and long-term exposure to fine particulate air pollution". Journal of the American Medical Association. 287 (9): 1132–1141. doi:10.1001/jama.287.9.1132. PMID 11879110.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help)CS1 maint: numeric names: authors list (link) - ^ Krewski D, Burnett R, Jerrett M, Pope CA, Rainham D, Calle E, Thurston G, Thun M (2005 Jul 9-23). "Mortality and long-term exposure to ambient air pollution: ongoing analyses based on the American Cancer Society cohort". J Toxicol Environ Health A. 68 (13–14): 1093–109. doi:10.1080/15287390590935941. PMID 16024490.
{{cite journal}}: Check date values in:|date=(help)CS1 maint: multiple names: authors list (link) - ^ Valavanidis A, Fiotakis K, Vlachogianni T (2008 Oct-Dec). "Airborne particulate matter and human health: toxicological assessment and importance of size and composition of particles for oxidative damage and carcinogenic mechanisms". J Environ Sci Health C Environ Carcinog Ecotoxicol Rev. 26 (4): 339–62. doi:10.1080/10590500802494538. PMID 19034792.
{{cite journal}}: Check date values in:|date=(help)CS1 maint: multiple names: authors list (link) - ^ Fong, KM (2003). "Lung cancer • 9: Molecular biology of lung cancer: clinical implications". Thorax. 58 (10). BMJ Publishing Group Ltd.: 892–900. doi:10.1136/thorax.58.10.892. PMC 1746489. PMID 14514947.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Salgia, R (1998). "Molecular abnormalities in lung cancer". Journal of Clinical Oncology. 16 (3): 1207–1217. PMID 9508209.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ a b c d Herbst, RS (2008). "Molecular origins of cancer: lung cancer". N Engl J Med. 359 (13): 1367–1380. doi:10.1056/NEJMra0802714. PMID 18815398.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Aviel-Ronen, S (2006). "K-ras mutations in non-small-cell lung carcinoma: a review". Clinical Lung Cancer. 8 (1). Cancer Information Group: 30–38. doi:10.3816/CLC.2006.n.030. PMID 16870043.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Devereux, TR (1996). "Molecular mechanisms of lung cancer. Interaction of environmental and genetic factors". Chest. 109 (Suppl 3). American College of Chest Physicians: 14S–19S. doi:10.1378/chest.109.3_Supplement.14S. PMID 8598134.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Engels, EA (2007). "Systematic evaluation of genetic variants in the inflammation pathway and risk of lung cancer". Cancer Research. 67 (13). American Association for Cancer Research: 6520–6527. doi:10.1158/0008-5472.CAN-07-0370. PMID 17596594.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Wenzlaff, AS (2005). "CYP1A1 and CYP1B1 polymorphisms and risk of lung cancer among never smokers: a population-based study". Carcinogenesis. 26 (12). Oxford University Press: 2207–2212. doi:10.1093/carcin/bgi191. PMID 16051642.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Son, JW (2006). "Polymorphisms in the caspase-8 gene and the risk of lung cancer". Cancer Genetics and Cytogenetics. 169 (2): 121–127. doi:10.1016/j.cancergencyto.2006.04.001. PMID 16938569.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Yin, J (2007). "The DNA repair gene XRCC1 and genetic susceptibility of lung cancer in a northeastern Chinese population". Lung Cancer. 56 (2): 153–160. doi:10.1016/j.lungcan.2006.12.012. PMID 17316890.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Tomoda K, Ohkoshi T, Hirota K; et al. (2009). "Preparation and properties of inhalable nanocomposite particles for treatment of lung cancer". Colloids and Surfaces B: Biointerfaces. 71 (2): 177. doi:10.1016/j.colsurfb.2009.02.001. PMID 19264458.
{{cite journal}}: Explicit use of et al. in:|author=(help); More than one of|pages=and|page=specified (help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Fan, YG (2009). "Association between sputum atypia and lung cancer risk in an occupational cohort in yunnan, china". Chest. 135 (3): 778–85. doi:10.1378/chest.08-1469. PMID 19265088.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ a b Travis, WD (1995). "Lung cancer". Cancer. 75 (Suppl. 1): 191–202. doi:10.1002/1097-0142(19950101)75:1+<191::AID-CNCR2820751307>3.0.CO;2-Y. PMID 8000996.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Morandi, U (2006). "Bronchial typical carcinoid tumors". Seminars in Thoracic and Cardiovascular Surgery. 18 (3): 191–198. doi:10.1053/j.semtcvs.2006.08.005. PMID 17185178.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Etienne-Mastroianni, B (2002). "Primary sarcomas of the lung: a clinicopathologic study of 12 cases". Lung Cancer. 38 (3): 283–289. doi:10.1016/S0169-5002(02)00303-3. PMID 12445750.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Tan D, Zander DS (2008). "Immunohistochemistry for Assessment of Pulmonary and Pleural Neoplasms: A Review and Update". Int J Clin Exp Pathol. 1 (1): 19–31. PMC 2480532. PMID 18784820.
- ^ Park SY, Kim BH, Kim JH, Lee S, Kang GH (2007). "Panels of immunohistochemical markers help determine primary sites of metastatic adenocarcinoma". Arch. Pathol. Lab. Med. 131 (10): 1561–7. doi:10.1043/1543-2165(2007)131[1561:POIMHD]2.0.CO;2. ISSN 1543-2165. PMID 17922593.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Bryant, A (2007). "Differences in epidemiology, histology, and survival between cigarette smokers and never-smokers who develop non-small cell lung cancer". Chest. 132 (1): 198–192. doi:10.1378/chest.07-0442. PMID 17573517.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Smokers defined as current or former smoker of more than 1 year of duration. Reference:
- Table 2 in: Kenfield SA, Wei EK, Stampfer MJ, Rosner BA, Colditz GA (2008). "Comparison of Aspects of Smoking Among Four Histologic Types of Lung Cancer". Tob Control. 17 (3): 198–204. doi:10.1136/tc.2007.022582. PMC 3044470. PMID 18390646.
{{cite journal}}: CS1 maint: multiple names: authors list (link)
- Table 2 in: Kenfield SA, Wei EK, Stampfer MJ, Rosner BA, Colditz GA (2008). "Comparison of Aspects of Smoking Among Four Histologic Types of Lung Cancer". Tob Control. 17 (3): 198–204. doi:10.1136/tc.2007.022582. PMC 3044470. PMID 18390646.
- ^ a b Travis WD. Pathology of lung cancer. Clin Chest Med 2002;23:65-81
- ^ Subramanian, J (2007). "Lung cancer in never smokers: a review". Journal of Clinical Oncology. 25 (5). American Society of Clinical Oncology: 561–570. doi:10.1200/JCO.2006.06.8015. PMID 17290066.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Raz, DJ (2006). "Bronchioloalveolar carcinoma: a review". Clinical Lung Cancer. 7 (5): 313–322. doi:10.3816/CLC.2006.n.012. PMID 16640802.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Lung cancer - small cell Medline Plus. Retrieved 5 February 2010.
- ^ a b Collins, LG (2007). "Lung cancer: diagnosis and management". American Family Physician. 75 (1). American Academy of Family Physicians: 56–63. PMID 17225705.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Rosti, G (2006). "Small cell lung cancer". Annals of Oncology. 17 (Suppl. 2): 5–10. doi:10.1093/annonc/mdj910. PMID 16608983.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Barbone, F (1997). "Cigarette smoking and histologic type of lung cancer in men" (PDF). Chest. 112 (6). American College of Chest Physicians: 1474–1479. doi:10.1378/chest.112.6.1474. PMID 9404741.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Roggli VL, Vollmer RT, Greenberg SD, McGavran MH, Spjut HJ, Yesner R. Lung cancer heterogeneity: a blinded and randomized study of 100 consecutive cases. Hum Pathol 1985; 16: 569-79.
- ^ a b Dishop MK, Kuruvilla S (2008). "Primary and metastatic lung tumors in the pediatric population: a review and 25-year experience at a large children's hospital". Arch. Pathol. Lab. Med. 132 (7): 1079–103. doi:10.1043/1543-2165(2008)132[1079:PAMLTI]2.0.CO;2. ISSN 1543-2165. PMID 18605764.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Seo, JB (1 March 2001). "Atypical pulmonary metastases: spectrum of radiologic findings". Radiographics. 21 (2): 403–417. PMID 11259704.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Mountain, CF (2003). A Handbook for Staging, Imaging, and Lymph Node Classification. Charles P Young. Retrieved 2007-09-01.
{{cite book}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Vineis, P (2007). "Lung cancers attributable to environmental tobacco smoke and air pollution in non-smokers in different European countries: a prospective study". Environmental Health. 6. BioMed Central: 7. doi:10.1186/1476-069X-6-7. PMC 1803768. PMID 17302981.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help)CS1 maint: unflagged free DOI (link) - ^ a b "A Decade of Broken Promises: The 1998 State Tobacco Settlement Ten Years Later" (PDF). Campaign for Tobacco-Free Kids. Retrieved 2008-12-03.
- ^ Pandey, G (2005). "Bhutan's smokers face public ban". BBC. Retrieved 2007-09-07.
{{cite news}}: Unknown parameter|month=ignored (help) - ^ Gray, N (2003). "A global approach to tobacco policy". Lung Cancer. 39 (2). BioMed Central: 113–117. doi:10.1016/S0169-5002(02)00456-7. PMID 12581561.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Slatore, CG (2008). "Long-Term Use of Supplemental Multivitamins, Vitamin C, Vitamin E, and Folate Does Not Reduce the Risk of Lung Cancer". American Journal of Respiratory and Critical Care Medicine. 177 (5): 524–30. doi:10.1164/rccm.200709-1398OC. PMC 2258445. PMID 17989343.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Kushi LH, Byers T, Doyle C, Bandera EV, McCullough M, McTiernan A; et al. (2006). "American cancer society guidelines on nutrition and physical activity for cancer prevention: Reducing the risk of cancer with healthy food choices and physical activity". CA: A Cancer Journal for Clinicians. 56 (5): 254–81. doi:10.3322/canjclin.56.5.254. PMID 17005596.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ "UN health agency calls for total ban on tobacco advertising to protect young" (Press release). United Nations News service. 30 May 2008.
- ^ van Klaveren RJ, Oudkerk M, Prokop M; et al. (2009). "Management of lung nodules detected by volume CT scanning". N. Engl. J. Med. 361 (23): 2221–9. doi:10.1056/NEJMoa0906085. PMID 19955524.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Gohagan, JK (2005). "Final results of the Lung Screening Study, a randomized feasibility study of spiral CT versus chest X-ray screening for lung cancer". Lung Cancer. 47 (1): 9–15. doi:10.1016/j.lungcan.2004.06.007. PMID 15603850.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ a b Temel JS, Greer JA, Muzikansky A; et al. (2010). "Early palliative care for patients with metastatic non-small-cell lung cancer". N. Engl. J. Med. 363 (8): 733–42. doi:10.1056/NEJMoa1000678. PMID 20818875.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Schiller JH, Vidaver RM, Novello S, Brahmer J, Monroe L (2007). "Living with a Diagnosis of Lung Cancer". [National Lung Cancer Partnership]. Retrieved 2008-12-01.
{{cite web}}: CS1 maint: multiple names: authors list (link) - ^ Strand, TE (2007). "Risk factors for 30‐day mortality after resection of lung cancer and prediction of their magnitude". Thorax. 62 (11). BMJ Publishing Group: 991. doi:10.1136/thx.2007.079145. PMC 2117132. PMID 17573442.
{{cite journal}}: More than one of|pages=and|page=specified (help); Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ El-Sherif, A (2006). "Outcomes of sublobar resection versus lobectomy for stage I non-small cell lung cancer: a 13-year analysis". Annals of Thoracic Surgery. 82 (2): 408–415. doi:10.1016/j.athoracsur.2006.02.029. PMID 16863738.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Fernando, HC (2005). "Lobar and sublobar resection with and without brachytherapy for small stage IA non-small cell lung cancer". Journal of Thoracic and Cardiovascular Surgery. 129 (2): 261–267. doi:10.1016/j.jtcvs.2004.09.025. PMID 15678034.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Casali G, Walker WS (2009). "Video-assisted thoracic surgery lobectomy: can we afford it?". Eur J Cardiothorac Surg. 35 (3): 423–8. doi:10.1016/j.ejcts.2008.11.008. PMID 19136272.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Lennox SC, Flavell G, Pollock DJ, Thompson VC, Wilkins JL (1968). "Results of resection for oat-cell carcinoma of the lung". Lancet. 2 (7575): 925–7. doi:10.1016/S0140-6736(68)91163-X. PMID 4176258.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Fox W, Scadding JG (1973). "Medical Research Council comparative trial of surgery and radiotherapy for primary treatment of small-celled or oat-celled carcinoma of bronchus. Ten-year follow-up". Lancet. 2 (7820): 63–5. doi:10.1016/S0140-6736(73)93260-1. PMID 4123619.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Simon GR, Turrisi A (2007). "Management of small cell lung cancer: ACCP evidence-based clinical practice guidelines (2nd edition)". Chest. 132 (3 Suppl): 324S–339S. doi:10.1378/chest.07-1385. PMID 17873178.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Yang SC (2010). "Reversing the surgical stigma for small-cell lung cancer". Oncology (Williston Park, N.Y.). 24 (11): 1042–3. PMID 21155455.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Hage R, Elbers JR, Brutel de la Rivière A, van den Bosch JM (1998). "Surgery for combined type small cell lung carcinoma". Thorax. 53 (6): 450–3. doi:10.1136/thx.53.6.450. PMC 1745233. PMID 9713442.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Arriagada, R (2002). Oxford Textbook of Oncology (2nd ed.). Oxford University Press. p. 2094. ISBN 0-19-262926-3.
{{cite book}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ a b Saunders, M (1997). "Continuous hyperfractionated accelerated radiotherapy (CHART) versus conventional radiotherapy in non-small-cell lung cancer: a randomised multicentre trial". Lancet. 350 (9072). Elsevier: 161–165. doi:10.1016/S0140-6736(97)06305-8. PMID 9250182.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Wagner, H (1998). "Radiation therapy in the management of limited small cell lung cancer: when, where, and how much?". Chest. 113 (Suppl. 1). American College of Chest Physicians: 92S–100S. doi:10.1378/chest.113.1_Supplement.92S. PMID 9438697.
{{cite journal}}: Unknown parameter|month=ignored (help) [dead link] - ^ PORT Meta-analysis Trialists Group (2005). Rydzewska, Larysa (ed.). "Postoperative radiotherapy for non-small cell lung cancer". Cochrane database of systematic reviews (Online) (2): CD002142. doi:10.1002/14651858.CD002142.pub2. PMID 15846628.
- ^ Lally, BE (2006). "Postoperative Radiotherapy for Stage II or III Non–Small-Cell Lung Cancer Using the Surveillance, Epidemiology, and End Results Database". Journal of Clinical Oncology. 24 (19). John Wiley & Sons: 2998–3006. doi:10.1200/JCO.2005.04.6110. PMID 16769986.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Raben, A (1997). "Brachytherapy for non-small cell lung cancer and selected neoplasms of the chest". Chest. 112 (Suppl. 4). American College of Chest Physicians: 276S–286S. doi:10.1378/chest.112.4_Supplement.276S. PMID 9337304.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Celebioglu, B (2002). "High dose rate endobronchial brachytherapy effectively palliates symptoms due to inoperable lung cancer". Japanese Journal of Clinical Oncology. 32 (11). Oxford University Press: 443–448. doi:10.1093/jjco/hyf102. PMID 12499415.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Ng, M (2007). "Tolerability of accelerated chest irradiation and impact on survival of prophylactic cranial irradiation in patients with limited-stage small cell lung cancer: review of a single institution's experience". Journal of Thoracic Oncology. 2 (6). International Association for the Study of Lung Cancer: 506–513. doi:10.1097/JTO.0b013e318060095b. PMID 17545845.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Slotman, B (2007). "Prophylactic cranial irradiation in extensive small-cell lung cancer". New England Journal of Medicine. 357 (7): 664–672. doi:10.1056/NEJMoa071780. PMID 17699816.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Hof, H (2007). "Stereotactic single-dose radiotherapy (radiosurgery) of early stage nonsmall-cell lung cancer (NSCLC)". Cancer. 110 (1). Wiley InterScience: 148–155. doi:10.1002/cncr.22763. PMID 17516437.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Hann CL, Rudin CM (2008-11-30). "Management of small-cell lung cancer: incremental changes but hope for the future". Oncology (Williston Park). 22 (13): 1486–92. PMID 19133604.
- ^ Murray, N (2006). "A review of first-line treatment for small-cell lung cancer". Journal of Thoracic Oncology. 1 (3): 270–278. PMID 17409868.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Azim, HA (2007). "Treatment options for relapsed small-cell lung cancer". Anticancer drugs. 18 (3): 255–261. doi:10.1097/CAD.0b013e328011a547. PMID 17264756.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ MacCallum, C (2006). "Second-line treatment of small-cell lung cancer". Current Oncology Reports. 8 (4): 258–264. doi:10.1007/s11912-006-0030-8. PMID 17254525.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Araujo AM, Mendez JC, Coelho AL; et al. (2009). "Phase II Study of Celecoxib with Cisplatin Plus Etoposide in Extensive-Stage Small Cell Lung Cancer". Cancer Invest. 27 (4): 1. doi:10.1080/07357900802232756. PMID 19266367.
{{cite journal}}: Explicit use of et al. in:|author=(help); More than one of|pages=and|page=specified (help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Aggarwal C; et al. (2010). "Biomarkers with predictive and prognostic function in non-small cell lung cancer: ready for prime time?". J Natl Compr Canc Netw. 8: 822–32.
{{cite journal}}: Explicit use of et al. in:|author=(help) - ^ Rosell, R; Moran, T; Queralt, C; Porta, R; Cardenal, F; Camps, C; Majem, M; Lopez-Vivanco, G; Isla, D (2009). "Screening for epidermal growth factor receptor mutations in lung cancer". N Engl J Med. 361 (10): 958–67. doi:10.1056/NEJMoa0904554. PMID 19692684.
- ^ Mok TS; et al. (2009). "Gefitinib or carboplatin-paclitaxel in pulmonary adenocarcinoma". N Engl J Med. 361 (10): 947–57. doi:10.1056/NEJMoa0810699. PMID 19692680.
{{cite journal}}: Explicit use of et al. in:|author=(help) - ^ Clegg, A (2002). "Clinical and cost effectiveness of paclitaxel, docetaxel, gemcitabine, and vinorelbine in non-small cell lung cancer: a systematic review". Thorax. 57 (1). BMJ Publishing Group: 20–28. doi:10.1136/thorax.57.1.20. PMC 1746188. PMID 11809985.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Sandler A, Gray R, Perry MC; et al. (2006). "Paclitaxel-carboplatin alone or with bevacizumab for non-small-cell lung cancer". N Engl J Med. 355 (24): 2542–50. doi:10.1056/NEJMoa061884. PMID 17167137.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Fuld AD, Dragnev KH, Rigas JR (2010). "Pemetrexed in advanced non-small-cell lung cancer". Expert Opin Pharmacother. 11 (8): 1387–402. doi:10.1517/14656566.2010.482560. PMID 20446853.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Scagliotti GV, Parikh P, von Pawel J; et al. (2008). "Phase III study comparing cisplatin plus gemcitabine with cisplatin plus pemetrexed in chemotherapy-naive patients with advanced-stage non-small-cell lung cancer". J. Clin. Oncol. 26 (21): 3543–51. doi:10.1200/JCO.2007.15.0375. PMID 18506025.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Rossi A, Maione P, Bareschino MA; et al. (2010). "The emerging role of histology in the choice of first-line treatment of advanced non-small cell lung cancer: implication in the clinical decision-making". Curr. Med. Chem. 17 (11): 1030–8. doi:10.2174/092986710790820589. PMID 20156162.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ http://www.accessdata.fda.gov/drugsatfda_docs/label/2010/021743s14s16lbl.pdf
- ^ a b http://www.fda.gov/AboutFDA/CentersOffices/CDER/ucm209058.htm
- ^ FDA approves Xalkori with companion diagnostic for a type of late-stage lung cancer. U.S. Food and Drug Administration. http://www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm269856.htm
- ^ West HL, Franklin WA, McCoy J; et al. (2006). "Gefitinib therapy in advanced brochoalveolar carcinoma. Southwest Oncology Group study S0126". J Clin Oncol. 24 (12): 1807–13. doi:10.1200/JCO.2005.04.9890. PMID 16622257.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Miller VA, Riely GJ, Zakowski MF; et al. (2008). "Molecular characteristics of bronchoalveolar carcinoma and adenocarcinoma, brochoalveolar carcinoma subtype, predict response to erlotinib". J Clin Oncol. 26 (9): 1472–8. doi:10.1200/JCO.2007.13.0062. PMID 18349398.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Eaton KD, Martins RG (2010 Jul). "Maintenance chemotherapy in non-small cell lung cancer". J Natl Compr Canc Netw. 8 (7): 815–21. PMID 20679540.
{{cite journal}}: Check date values in:|date=(help) - ^ Ciuleanu T, Brodowicz T, Zielinski C; et al. (2009). "Maintenance pemetrexed plus best supportive care versus placebo plus best supportive care for non-small-cell lung cancer: a randomised, double-blind, phase 3 study". The Lancet. 374 (9699): 1432–40. doi:10.1016/S0140-6736(09)61497-5. PMID 19767093.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Cappuzzo F, Ciuleanu T, Stelmakh L; et al. (2010). "Erlotinib as maintenance treatment in advanced non-small-cell lung cancer: a multicentre, randomised, placebo-controlled phase 3 study". Lancet Oncol. 11 (6): 521–9. doi:10.1016/S1470-2045(10)70112-1. PMID 20493771.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Fidias PM, Dakhil SR, Lyss AP; et al. (2009). "Phase III study of immediate compared with delayed docetaxel after front-line therapy with gemcitabine plus carboplatin in advanced non-small-cell lung cancer". J Clin Oncol. 27 (4): 591–8. doi:10.1200/JCO.2008.17.1405. PMID 19075278.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Rossi A, Ricciardi S, Maione P, de Marinis F, Gridelli C (2009). "Pemetrexed in the treatment of advanced non-squamous lung cancer". Lung Cancer. 66 (2): 141–9. doi:10.1016/j.lungcan.2009.06.006. PMID 19577816.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Winton, T (2005). "Vinorelbine plus cisplatin vs. observation in resected non-small-cell lung cancer". New England Journal of Medicine. 352 (25). Massachusetts Medical Society: 2589–2597. doi:10.1056/NEJMoa043623. PMID 15972865.
Adjuvant vinorelbine plus cisplatin has an acceptable level of toxicity and prolongs disease-free and overall survival among patients with completely resected early-stage non-small-cell lung cancer.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Douillard, JY (2006). "Adjuvant vinorelbine plus cisplatin versus observation in patients with completely resected stage IB-IIIA non-small-cell lung cancer (Adjuvant Navelbine International Trialist Association [ANITA]): a randomised controlled trial". Lancet Oncology. 7 (9). Elsevier: 719–727. doi:10.1016/S1470-2045(06)70804-X. PMID 16945766.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Tsuboi, M (2007). "The present status of postoperative adjuvant chemotherapy for completely resected non-small cell lung cancer" (PDF). Annals of Thoracic and Cardiovascular Surgery. 13 (2): 73–77. PMID 17505412.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Olaussen KA, Dunant A, Fouret P, et al: DNA repair by ERCC1 in non-small-cell lung cancer and cisplatin-based adjuvant chemotherapy. N Engl J Med 2006;355:983-991
- ^ Horn, L (2007). "The rationale for adjuvant chemotherapy in stage I non-small cell lung cancer". Journal of Thoracic Oncology. 2 (5): 377–383. doi:10.1097/01.JTO.0000268669.64625.bb. PMID 17473651.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Wakelee, HA (2006). "Current status of adjuvant chemotherapy for stage IB non-small-cell lung cancer: implications for the New Intergroup Trial". Clinical Lung Cancer. 8 (1). Cancer Information Group: 18–21. doi:10.3816/CLC.2006.n.028. PMID 16870041.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ BMJ (2005). Clinical evidence concise : the international resource of the best available evidence for effective health care. London: BMJ Publishing Group. pp. 486–488. ISBN 1-905545-00-2. ISSN 1475-9225.
{{cite book}}: Unknown parameter|month=ignored (help) - ^ Simon, CJ (2007). "Pulmonary radiofrequency ablation: long-term safety and efficacy in 153 patients". Radiology. 243 (1): 268–275. doi:10.1148/radiol.2431060088. PMID 17392258.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Bakitas M, Lyons KD, Hegel MT; et al. (2009). "Effects of a palliative care intervention on clinical outcomes in patients with advanced cancer: the Project ENABLE II randomized controlled trial". JAMA. 302 (7): 741–9. doi:10.1001/jama.2009.1198. PMID 19690306.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Connor SR, Pyenson B, Fitch K, Spence C, Iwasaki K (2007). "Comparing hospice and nonhospice patient survival among patients who die within a three-year window". J Pain Symptom Manage. 33 (3): 238–46. doi:10.1016/j.jpainsymman.2006.10.010. PMID 17349493.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Kelley AS, Meier DE (2010). "Palliative care--a shifting paradigm". N. Engl. J. Med. 363 (8): 781–2. doi:10.1056/NEJMe1004139. PMID 20818881.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ a b Prince-Paul M (2009). "When hospice is the best option: an opportunity to redefine goals". Oncology (Williston Park, N.Y.). 23 (4 Suppl Nurse Ed): 13–7. PMID 19856592.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Marino P, Pampallona S, Preatoni A, Cantoni A, Invernizzi F (1994). "Chemotherapy vs supportive care in advanced non-small-cell lung cancer. Results of a meta-analysis of the literature". Chest. 106 (3): 861–5. doi:10.1378/chest.106.3.861. PMID 7521815.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Souquet PJ, Chauvin F, Boissel JP, Bernard JP (1995). "Meta-analysis of randomised trials of systemic chemotherapy versus supportive treatment in non-resectable non-small cell lung cancer". Lung Cancer. 12 Suppl 1: S147–54. doi:10.1016/0169-5002(95)00430-9. PMID 7551923.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Sörenson S, Glimelius B, Nygren P (2001). "A systematic overview of chemotherapy effects in non-small cell lung cancer". Acta Oncol. 40 (2–3): 327–39. PMID 11441939.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Clegg A, Scott DA, Sidhu M, Hewitson P, Waugh N (2001). "A rapid and systematic review of the clinical effectiveness and cost-effectiveness of paclitaxel, docetaxel, gemcitabine and vinorelbine in non-small-cell lung cancer". Health Technol Assess. 5 (32): 1–195. PMID 12065068.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ NSCLC Meta-Analyses Collaborative Group (2008). "Chemotherapy in Addition to Supportive Care Improves Survival in Advanced Non–Small-Cell Lung Cancer: A Systematic Review and Meta-Analysis of Individual Patient Data From 16 Randomized Controlled Trials". J. Clin. Oncol. 26 (28): 4617–25. doi:10.1200/JCO.2008.17.7162. PMC 2653127. PMID 18678835.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Non-Small Cell Lung Cancer Collaborative Group (2010). Burdett, Sarah (ed.). "Chemotherapy and supportive care versus supportive care alone for advanced non-small cell lung cancer". Cochrane Database of Systematic Reviews (5): CD007309. doi:10.1002/14651858.CD007309.pub2. PMID 20464750.
{{cite journal}}: Unknown parameter|group=ignored (help); Unknown parameter|review=ignored (help) - ^ "Non-Small Cell Lung Cancer Treatment". PDQ for Health Professionals. National Cancer Institute. Retrieved 2008-11-22.
- ^ "-Small Cell Lung Cancer Treatment". PDQ for Health Professionals. National Cancer Institute. Retrieved 2008-11-22.
- ^ Mountain, CF (1997). "Revisions in the international system for staging lung cancer" (PDF). Chest. 111 (6). American College of Chest Physicians: 1710–1717. doi:10.1378/chest.111.6.1710. PMID 9187198.
- ^ SEER data (SEER.cancer.gov) Median Age of Cancer Patients at Diagnosis 2002-2003
- ^ SEER data (SEER.cancer.gov) Median Age of Cancer Patients at Death 2002-2006
- ^ "WHO Disease and injury country estimates". World Health Organization. 2009. Retrieved November 11, 2009.
- ^ Jemal, A (2011-02-04). "Global cancer statistics". CA: a cancer journal for clinicians. 61 (2): 69–90. doi:10.3322/caac.20107. PMID 21296855.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ "Commonly diagnosed cancers worldwide". Cancer Research UK. 2005. Retrieved 2008-01-11.
{{cite web}}: Unknown parameter|month=ignored (help) - ^ Jemal, A., R.C. Tiwari, T. Murray, A. Ghafoor, A. Samuels, El. Ward, E.J. Feuer, and M.J. Thun, Cancer statistics, 2004. CA Cancer J Clin, 2004. 54(1): p.8-29.
- ^ Lum, KL (2008). "Signed, sealed and delivered: "big tobacco" in Hollywood, 1927–1951". Tobacco Control. 17 (5): 313–323. doi:10.1136/tc.2008.025445. PMC 2602591. PMID 18818225.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ "Deadly in Pink". Tobaccofreekids.org. Retrieved 2010-09-26.
- ^ Parent, ME (2007). "Exposure to diesel and gasoline engine emissions and the risk of lung cancer". American Journal of Epidemiology. 165 (1): 53–62. doi:10.1093/aje/kwj343. PMID 17062632.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ National Cancer Institute; SEER stat fact sheets: Lung and Bronchus. Surveillance Epidemiology and End Results. 2010 [1]
- ^ "Gender in lung cancer and smoking research" (PDF). World Health Organization. 2004. Retrieved 2007-05-26.
- ^ Liu, BQ (1998-11-21). "Emerging tobacco hazards in China: 1. Retrospective proportional mortality study of one million deaths". British Medical Journal. 317 (7170): 1411–1422. PMC 28719. PMID 9822393.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Behera, D (2004). "Lung cancer in India" (PDF). Indian Journal of Chest Diseases and Allied Sciences. 46 (4): 269–281. PMID 15515828.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Mohr, SB (2008). "Could ultraviolet B irradiance and vitamin D be associated with lower incidence rates of lung cancer?". Journal of Epidemiology and Community Health. 62 (1): 69–74. doi:10.1136/jech.2006.052571. PMID 18079336.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ a b Chen, F (2007). "Declining incidence rate of lung adenocarcinoma in the United States". Chest. 131 (4): 1000–1005. doi:10.1378/chest.06-1695. PMID 17426202.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Charloux, A (1997). "The increasing incidence of lung adenocarcinoma: reality or artefact? A review of the epidemiology of lung adenocarcinoma". International Journal of Epidemiology. 26 (1): 14–23. doi:10.1093/ije/26.1.14. PMID 9126499.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Singh N, Aggarwal AN, Gupta D, et al. Unchanging clinico-epidemiological profile of lung cancer in North India over three decades. Cancer Epidemiol 2010; 34(1): 101-104
- ^ Rawat J, Sindhwani G, Gaur D, et al. Clinico-pathological profile of lung cancer in Uttarakhand. Lung India. 2009 Jul;26(3):74-6.
- ^ Khan NA, Afroz F, Lone MM, et al. Profile of lung cancer in Kashmir, India: a five-year study.Indian J Chest Dis Allied Sci. 2006 Jul-Sep;48(3):187-90.
- ^ Morgagni, Giovanni Battista (1761). De sedibus et causis morborum per anatomen indagatis.
- ^ Bayle, Gaspard-Laurent (1810). Recherches sur la phtisie pulmonaire (in French). Paris.
- ^ a b Witschi, H (2001). "A short history of lung cancer". Toxicological Sciences. 64 (1): 4–6. doi:10.1093/toxsci/64.1.4. PMID 11606795.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Adler, I (1912). Primary Malignant Growths of the Lungs and Bronchi. New York: Longmans, Green, and Company. OCLC 14783544., cited in Spiro SG, Silvestri GA (2005). "One hundred years of lung cancer". American Journal of Respiratory and Critical Care Medicine. 172 (5): 523–529. doi:10.1164/rccm.200504-531OE. PMID 15961694.
- ^ Grannis, FW. "History of cigarette smoking and lung cancer". smokinglungs.com. Archived from the original on July 18, 2007. Retrieved 2007-08-06.
- ^ Proctor, R (2000). The Nazi War on Cancer. Princeton University Press. pp. 173–246. ISBN 0-691-00196-0.
- ^ Doll, R (1956). "Lung Cancer and Other Causes of Death in Relation to Smoking". British Medical Journal. 2 (5001): 1071–1081. doi:10.1136/bmj.2.5001.1071. PMC 2035864. PMID 13364389.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ US Department of Health Education and Welfare (1964). "Smoking and health: report of the advisory committee to the Surgeon General of the Public Health Service" (PDF). Washington, DC: US Government Printing Office.
- ^ Pirozynski, M (2006). "100 years of Lung Cancer". Respiratory Medicine. 100 (12): 2073–2084. doi:10.1016/j.rmed.2006.09.002. PMID 17056245.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Greaves, M (2000). Cancer: the Evolutionary Legacy. Oxford University Press. pp. 196–197. ISBN 0-19-262835-6.
- ^ Horn, L (2008). "Evarts A. Graham and the first pneumonectomy for lung cancer". Journal of Clinical Oncology. 26 (19): 3268–3275. doi:10.1200/JCO.2008.16.8260. PMID 18591561.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Edwards, AT (1946). "Carcinoma of the Bronchus". Thorax. 1 (1): 1–25. doi:10.1136/thx.1.1.1. PMC 1018207. PMID 20986395.
- ^ Kabela, M (1956). "[Experience with radical irradiation of bronchial cancer]". Ceskoslovenská Onkológia (in German). 3 (2): 109–115. PMID 13383622.
- ^ Lennox, SC (1968). "Results of resection for oat-cell carcinoma of the lung". Lancet. 2 (7575). Elsevier: 925–927. doi:10.1016/S0140-6736(68)91163-X. PMID 4176258.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Miller, AB (1969). "Five-year follow-up of the Medical Research Council comparative trial of surgery and radiotherapy for the primary treatment of small-celled or oat-celled carcinoma of the bronchus". Lancet. 2 (7619). Elsevier: 501–505. doi:10.1016/S0140-6736(69)90212-8. PMID 4184834.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Cohen, M (1977). "Intensive chemotherapy of small cell bronchogenic carcinoma". Cancer Treatment Reports. 61 (3): 349–354. PMID 194691.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help)
External links
Template:Link GA Template:Link FA Template:Link GA Template:Link FA
