Chloroprocaine: Difference between revisions
Darrenfergus (talk | contribs) |
|||
| Line 72: | Line 72: | ||
The ''in vitro'' [[half-life]] of chloroprocaine is 21 seconds for maternal and 43 seconds for fetal blood. In patients who are homozygous atypical for plasma cholinesterase, chloroprocaine typically exists for two minutes in circulation.<ref>Chestnut: Obstetric Anesthesia, 3rd ed, p333.</ref><ref>Hughes: Anesthesia for Obstetrics, 4th ed, p75.</ref> |
The ''in vitro'' [[half-life]] of chloroprocaine is 21 seconds for maternal and 43 seconds for fetal blood. In patients who are homozygous atypical for plasma cholinesterase, chloroprocaine typically exists for two minutes in circulation.<ref>Chestnut: Obstetric Anesthesia, 3rd ed, p333.</ref><ref>Hughes: Anesthesia for Obstetrics, 4th ed, p75.</ref> |
||
The use of Chloroprocaine in the [[subarachnoid]] space has been questioned. In the early 1980s, there were several case reports of neurological deficits after inadvertant intrathecal injections intended for epidural delivery. These doses were an order of magnitude higher than is currently used for intrathecal delivery. It is also thought that these deficits were also related to the preservative [[sodium bisulfate]], although this is also contraversial. It is also not used in intravenous regional anesthesia due to the risk of [[thrombophlebitis]]. |
|||
==Chemistry== |
==Chemistry== |
||
Revision as of 18:15, 20 September 2013
 | |
| Clinical data | |
|---|---|
| AHFS/Drugs.com | Micromedex Detailed Consumer Information |
| ATC code | |
| Identifiers | |
| |
| CAS Number | |
| PubChem CID | |
| DrugBank | |
| ChemSpider | |
| UNII | |
| KEGG | |
| ChEBI | |
| ChEMBL | |
| CompTox Dashboard (EPA) | |
| Chemical and physical data | |
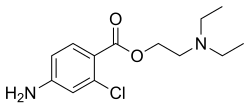
| Formula | C13H19ClN2O2 |
| Molar mass | 270.755 g/mol g·mol−1 |
| 3D model (JSmol) | |
| |
| |
| | |
Chloroprocaine (trade name Nesacaine, Nesacaine-MPF) (often in the hydrochloride salt form as the aforementioned trade names) is a local anesthetic given by injection during surgical procedures and labor and delivery. Chloroprocaine constricts blood vessels resulting in reduced blood loss; this is in contrast to other local anesthetics e.g. lidocaine, which do not do such. Chloroprocaine is an ester anesthetic.[1]
Sub-arachnoid block or SAB
Chloroprocaine was developed to meet the need for a short acting spinal anaesthetic that is reliable and has a favourable safety profile to support the growing need for day case surgery. Licensed in Europe for surgical procedures up to 40 minutes chloroprocaine is an ester type local anaesthetic with the shortest duration of action of all the established local anaesthetics. It has a significantly shorter duration of action than lidocaine and is significantly less toxic. Chloroprocaine has a motor block lasting for 40 minutes, a rapid onset time of 3-5 minutes (9.6 min ± 7.3 min at 40 mg dose; 7.9 min ± 6.0 min at 50 mg dose) and a time to ambulation of 90 minutes without complications, especially without TNS.
These data are based upon a retrospective review of 672 patients suitable for spinal anaesthesia in surgical procedures of less than 60 minutes duration using 30-40mg chloroprocaine. The results showed good surgical anaesthesia, a fast onset time and post-operative mobilization after 90 minutes without complications.
Ampres (chloroprocaine) Summary of Product Characteristics
Palas T, Cloroprocaina in chirurgia ambulatoriale: uno studio osservazionale Perimed 2009, 3(2):31-34
Obstetrics
Amide-linked local anesthetic agents, such as lidocaine and bupivacaine, can become "trapped" in their ionized forms on the fetal side of the placenta, and therefore their net transfer across the placenta is increased. An ester-linked local anesthetic agent, 2-chloroprocaine, is rapidly metabolized, and placental transfer is limited. Since the metabolism of 2-chloroprocaine by fetal plasma is slower than in maternal plasma, the potential for ion trapping exists. Fetal pH is slightly lower than maternal (7.32 to 7.38), thus most unionized drugs are "ion trapped" to a degree, even in a healthy fetus. Chloroprocaine (pKa 8.7) is the drug of choice for epidural analgesia and a decompensating fetus, because it does not participate in ion trapping. Placental transfer of 2-chloroprocaine is not influenced by fetal acidosis.[2]
The in vitro half-life of chloroprocaine is 21 seconds for maternal and 43 seconds for fetal blood. In patients who are homozygous atypical for plasma cholinesterase, chloroprocaine typically exists for two minutes in circulation.[3][4]
The use of Chloroprocaine in the subarachnoid space has been questioned. In the early 1980s, there were several case reports of neurological deficits after inadvertant intrathecal injections intended for epidural delivery. These doses were an order of magnitude higher than is currently used for intrathecal delivery. It is also thought that these deficits were also related to the preservative sodium bisulfate, although this is also contraversial. It is also not used in intravenous regional anesthesia due to the risk of thrombophlebitis.
Chemistry
Synthesis of this drug is accomplished by directly reacting the hydrochloride of the 4-amino-2-chlorbenzoic acid chloride with the hydrochloride of 2-diethylaminoethanol. The hydrochloride of 4-amino-2-chlorbenzoic acid chloride needed for synthesis is synthesized by reacting 2-chloro-4-aminobenzoic acid with thionyl chloride.[5]
References
- ^ Drug bank entry for Chloroprocaine
- ^ Philipson EH, Kuhnert BR, Syracuse CD. Fetal acidosis, 2-chloroprocaine, and epidural anesthesia for cesarean section. Am J Obstet Gynecol. 1985 Feb 1;151(3):322-4.
- ^ Chestnut: Obstetric Anesthesia, 3rd ed, p333.
- ^ Hughes: Anesthesia for Obstetrics, 4th ed, p75.
- ^ H.C. Marks, H.I. Rubin, U.S. patent 2,460,139 (1949)

