Sodium zirconium cyclosilicate
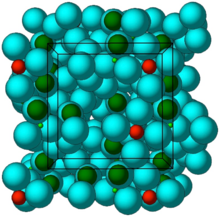 Crystal structure of ZS-9. Blue spheres = oxygen atoms, red spheres = zirconium atoms, green spheres = silicon atoms. | |
| Clinical data | |
|---|---|
| Trade names | Lokelma |
| Other names | ZS-9 |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a618035 |
| License data | |
| Pregnancy category |
|
| Routes of administration | By mouth |
| ATC code | |
| Legal status | |
| Legal status | |
| Pharmacokinetic data | |
| Bioavailability | Not absorbed |
| Excretion | Feces |
| Identifiers | |
| |
| CAS Number | |
| DrugBank | |
| UNII | |
| KEGG | |
| Chemical and physical data | |
| Formula | (2Na·H2O·3H4SiO4·H4ZrO6)n |
Sodium zirconium cyclosilicate, sold under the brand name Lokelma, is a medication used to treat high blood potassium.[5] Onset of effects occurs in one to six hours.[5] It is taken by mouth.[5]
Common side effects include swelling and low blood potassium.[5] Use is likely safe in pregnancy and breastfeeding.[5] It works by binding potassium ions in the gastrointestinal tract which is then lost in the stool.[5][6]
Sodium zirconium cyclosilicate was approved for medical use in the European Union and in the United States in 2018.[5][4][7] It was developed by AstraZeneca.[5]
Medical use
[edit]Sodium zirconium cyclosilicate is used to treat high blood potassium.[5] Onset of effects occurs in one to six hours.[5]
Mechanism of action
[edit]
ZS-9 is a zirconium silicate. Zirconium silicates have been extensively used in medical and dental applications because of their proven safety.[8] 11 zirconium silicates were screened by an iterative optimization process. ZS-9 selectively captures potassium ions, presumably by mimicking the actions of physiologic potassium channels.[9] ZS-9 is an inorganic cation exchanger crystalline with a high capacity to entrap monovalent cations, specifically potassium and ammonium ions, in the GI tract.
Background
[edit]Hyperkalemia is rare among those who are otherwise healthy.[10] Among those who are in hospital, rates are between 1% and 2.5%.[11] Common causes include kidney failure, hypoaldosteronism, and rhabdomyolysis.[12] A number of medications can also cause high blood potassium including spironolactone, NSAIDs, and angiotensin converting enzyme inhibitors.[12]
There is no universally accepted definition of what level of hyperkalemia is mild, moderate, or severe.[13] However, if hyperkalemia causes any ECG change it is considered a medical emergency[13] due to a risk of potentially fatal abnormal heart rhythms and is treated urgently.[13] Potassium levels greater than 6.5 to 7.0 mmol/L in the absence of ECG changes are managed aggressively.[13] Several approaches are used to treat hyperkalemia.[13] Other approved potassium binders in the United States include patiromer and sodium polystyrene sulfonate.[14]
Hyperkalemia, particularly if severe, is a marker for an increased risk of death.[15] However, there is disagreement regarding whether a modestly elevated levels directly causes problems. One viewpoint is that mild to moderate hyperkalemia is a secondary effect that denotes underlying medical problems.[15] Accordingly, these problems are both proximate and ultimate causes of death,[15]
History
[edit]In the United States, regulatory approval of ZS-9 was rejected by the Food and Drug Administration (FDA) in May 2016, due to issues associated with manufacturing.[16] On 18 May 2018, the FDA approved sodium zirconium cyclosilicate for treatment of adults with hyperkalemia.[17]
It was first practically synthesized by UOP in the late 1990s. (reference -zirconium silicate and zirconium germate molecular sieves and the process of using the same, US Patent 5,888,472) the recognition of the unique ion exchange properties and the potential use to remove toxins from the body were identified shortly thereafter ("process for removing toxins from bodily fluids using zirconium or titanium microporous compositions, US Patent 6,332,985).
Research
[edit]One review found a decrease in potassium of 0.17 mEq/L at one hour and 0.67 mEq/L at 48 hours.[18]
It appears effective in people with chronic kidney disease, diabetes, and heart failure.[6] Use has been studied for up to a year.[6]
References
[edit]- ^ a b "Lokelma APMDS". Therapeutic Goods Administration (TGA). 24 May 2024. Retrieved 10 June 2024.
- ^ "Summary Basis of Decision (SBD) for Lokelma". Health Canada. 23 October 2014. Archived from the original on 31 May 2022. Retrieved 29 May 2022.
- ^ "Lokelma- sodium zirconium cyclosilicate powder, for suspension". DailyMed. 30 September 2022. Archived from the original on 5 December 2022. Retrieved 27 February 2023.
- ^ a b "Lokelma EPAR". European Medicines Agency (EMA). 17 September 2018. Archived from the original on 8 January 2021. Retrieved 11 October 2019.
- ^ a b c d e f g h i j "Sodium Zirconium Cyclosilicate Monograph for Professionals". Drugs.com. Archived from the original on 1 August 2020. Retrieved 11 October 2019.
- ^ a b c Hoy SM (October 2018). "Sodium Zirconium Cyclosilicate: A Review in Hyperkalaemia". Drugs. 78 (15): 1605–1613. doi:10.1007/s40265-018-0991-6. PMC 6433811. PMID 30306338.
- ^ "Drug Approval Package: Lokelma (sodium zirconium cyclosilicate)". U.S. Food and Drug Administration (FDA). 8 June 2018. Archived from the original on 13 April 2021. Retrieved 7 May 2020.
- ^ Denry I, Kelly JR. State of the art of zirconia for dental applications. Dental Materials. Volume 24, Issue 3, March 2008, Pages 299–307
- ^ Stavros F, Yang A, Leon A, Nuttall M, Rasmussen HS (2014). "Characterization of structure and function of ZS-9, a K+ selective ion trap". PLOS ONE. 9 (12): e114686. Bibcode:2014PLoSO...9k4686S. doi:10.1371/journal.pone.0114686. PMC 4273971. PMID 25531770.
- ^ Kovesdy CP (March 2017). "Updates in hyperkalemia: Outcomes and therapeutic strategies". Reviews in Endocrine & Metabolic Disorders. 18 (1): 41–47. doi:10.1007/s11154-016-9384-x. PMC 5339065. PMID 27600582.
- ^ McDonald TJ, Oram RA, Vaidya B (October 2015). "Investigating hyperkalaemia in adults". BMJ. 351: h4762. doi:10.1136/bmj.h4762. PMID 26487322. S2CID 206907572.
- ^ a b Lehnhardt A, Kemper MJ (March 2011). "Pathogenesis, diagnosis and management of hyperkalemia". Pediatric Nephrology. 26 (3): 377–84. doi:10.1007/s00467-010-1699-3. PMC 3061004. PMID 21181208.
- ^ a b c d e Taal MW, Chertow GM, Marsden PA, Skorecki K, Yu AS, Brenner BM (2012). Brenner and Rector's The Kidney (Chapter 17, page 672, 9th ed.). Elsevier. ISBN 978-1-4160-6193-9.
- ^ Watson M, Abbott KC, Yuan CM (October 2010). "Damned if you do, damned if you don't: potassium binding resins in hyperkalemia". Clinical Journal of the American Society of Nephrology. 5 (10): 1723–6. doi:10.2215/CJN.03700410. PMID 20798253.
- ^ a b c Elliott MJ, Ronksley PE, Clase CM, Ahmed SB, Hemmelgarn BR (October 2010). "Management of patients with acute hyperkalemia". CMAJ. 182 (15): 1631–5. doi:10.1503/cmaj.100461. PMC 2952010. PMID 20855477.
- ^ Ben Adams (27 May 2016). "AstraZeneca's $2.7B hyperkalemia drug ZS-9 rejected by FDA". FierceBiotech. Archived from the original on 28 May 2016. Retrieved 27 May 2016.
- ^ "Lokelma (Sodium zirconium cyclosilicate) FDA Approval History". Archived from the original on 12 June 2018. Retrieved 11 June 2018.
- ^ Meaney CJ, Beccari MV, Yang Y, Zhao J (April 2017). "Systematic Review and Meta-Analysis of Patiromer and Sodium Zirconium Cyclosilicate: A New Armamentarium for the Treatment of Hyperkalemia". Pharmacotherapy. 37 (4): 401–411. doi:10.1002/phar.1906. PMC 5388568. PMID 28122118.
