Liver sinusoid
| Liver sinusoid | |
|---|---|
 | |
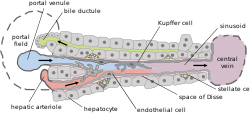 Basic liver structure | |
| Details | |
| Drains from | Hepatic portal vein |
| Drains to | Central veins of liver |
| Identifiers | |
| Latin | vas sinusoideum |
| TH | H3.04.05.0.00014 |
| FMA | 17543 |
| Anatomical terminology | |
A liver sinusoid is a type of capillary known as a sinusoidal capillary, discontinuous capillary or sinusoid, that is similar to a fenestrated capillary, having discontinuous endothelium that serves as a location for mixing of the oxygen-rich blood from the hepatic artery and the nutrient-rich blood from the portal vein.[1]
The liver sinusoid has a larger caliber than other types of capillaries and has a lining of specialised endothelial cells known as the liver sinusoidal endothelial cells (LSECs), and Kupffer cells.[2] The cells are porous and have a scavenging function.[3] The LSECs make up around half of the non-parenchymal cells in the liver and are flattened and fenestrated.[4] LSECs have many fenestrae that gives easy communication between the sinusoidal lumen and the space of Disse. They play a part in filtration, endocytosis, and in the regulation of blood flow in the sinusoids.[5]
The Kupffer cells can take up and destroy foreign material such as bacteria. Hepatocytes are separated from the sinusoids by the space of Disse. Hepatic stellate cells are present in the space of Disse and are involved in scar formation in response to liver damage.
Defenestration happens when LSECs are lost rendering the sinusoid as an ordinary capillary. This process precedes fibrosis.[6]
Endothelium
[edit]The liver sinusoidal endothelial cells are cultured for a variety of research purposes. The utility of these cells are of particular interest. One problem to overcome is the reversing of cellular differentiation that has made these cells highly specialized phenotypically in vitro.[7]
Additional images
[edit]-
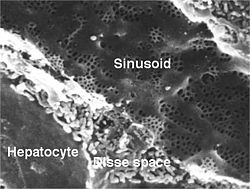
Human liver sinusoid
-
A single lobule of the liver of a pig. X 60.
References
[edit]- ^ SIU SOM Histology GI
- ^ Brunt, EM; et al. (June 2014). "Pathology of the liver sinusoids". Histopathology. 64 (7): 907–20. doi:10.1111/his.12364. PMID 24393125. S2CID 12709169.
- ^ DeLeve, LD (November 2007). "Hepatic microvasculature in liver injury". Seminars in Liver Disease. 27 (4): 390–400. doi:10.1055/s-2007-991515. PMID 17979075.
- ^ Xing, Y; Zhao, T; Gao, X; Wu, Y (18 February 2016). "Liver X receptor α is essential for the capillarization of liver sinusoidal endothelial cells in liver injury". Scientific Reports. 6: 21309. Bibcode:2016NatSR...621309X. doi:10.1038/srep21309. PMC 4758044. PMID 26887957.
- ^ Arii, S; Imamura, M (2000). "Physiological role of sinusoidal endothelial cells and Kupffer cells and their implication in the pathogenesis of liver injury". Journal of Hepato-biliary-pancreatic Surgery. 7 (1): 40–8. doi:10.1007/s005340050152. PMID 10982590.
- ^ Xie, G; Wang, X; Wang, L; Wang, L; Atkinson, RD; Kanel, GC; Gaarde, WA; Deleve, LD (April 2012). "Role of differentiation of liver sinusoidal endothelial cells in progression and regression of hepatic fibrosis in rats". Gastroenterology. 142 (4): 918–927.e6. doi:10.1053/j.gastro.2011.12.017. PMC 3618963. PMID 22178212.
- ^ Sellaro TL, Ravindra AK, Stolz DB, Badylak SF (September 2007). "Maintenance of hepatic sinusoidal endothelial cell phenotype in vitro using organ-specific extracellular matrix scaffolds". Tissue Eng. 13 (9): 2301–2310. doi:10.1089/ten.2006.0437. PMID 17561801. Retrieved 28 April 2013.
External links
[edit]- UIUC Histology Subject 589
- Histology image: 15504loa – Histology Learning System at Boston University - "Liver, Gall Bladder, and Pancreas: liver, classic lobule"
- Histology image: 22103loa – Histology Learning System at Boston University - "Ultrastructure of the Cell: hepatocytes and sinusoids, sinusoid and space of Disse"
- Histology at anhb.uwa.edu.au


