Medical restraint
| Part of series on |
| Involuntary treatment |
|---|
| Restraint |
| Involuntary commitment |
| Regulated by |
| Alternatives |
| Treatment |
Medical restraints are physical restraints used during certain medical procedures to restrain patients with (supposedly) the minimum of discomfort and pain and to prevent them from injuring themselves or others.
Rationale[edit]
There are many kinds of mild, safety-oriented medical restraints which are widely used. For example, the use of bed rails is routine in many hospitals and other care facilities, as the restraint prevents patients from rolling out of bed accidentally. Newborns frequently wear mittens to prevent accidental scratching. Some wheelchair users use a belt or a tray to keep them from falling out of their wheelchairs. In fact, not using these kinds of restraints when needed can lead to legal liability for preventable injuries.[1][2]
Medical restraints are generally used to prevent people with severe physical or mental disorders from harming themselves or others. A major goal of most medical restraints is to prevent injuries due to falls. Other medical restraints are intended to prevent a harmful behavior, such as hitting people.
Ethically and legally, once a person is restrained, the safety and well-being of the restrained person falls upon the restrainer, appropriate to the type and severity of the restraining method. For example, a person who is placed in a secured room should be checked at regular intervals for indications of distress. At the other extreme, a person who is rendered semi-conscious by pharmacological (or chemical) sedation should be constantly monitored by a well-trained individual who is dedicated to protecting the restrained person's physical and medical safety. Failure to properly monitor a restrained individual may result in criminal and civil prosecution, depending on jurisdiction.
Although medical restraints, used properly, can help prevent injury, they can also be dangerous. The United States Food and Drug Administration (FDA) estimated in 1992 that improper use of restraints results in at least 100 deaths each year, most by strangulation. FDA also noted reports of injuries — including broken bones and burns — caused by the improper use of restraints.[3] Medical restraints in psychiatric hospitals in Japan are sometimes kept on patients for weeks and months,[4] and they are thought to have caused several deaths due to deep vein thrombosis and pulmonary embolism.[5][6] More information about Japanese use of restraints is described in the page on physical restraints.
Because of the potential for abuse, the use of medical restraints is regulated in many jurisdictions. At one time in California, psychiatric restraint was viewed as a treatment. However, with the passing of SB-130, which became law in 2004, the use of psychiatric restraint(s) is no longer viewed as a treatment, but can be used as a behavioral intervention when an individual is in imminent danger of serious harm to self or others.[7][unreliable medical source]
Criticism[edit]
In the U.S. in the late 2010s and into the 2020s (so far), restraint of psychiatric patients and/or people with mental disorders (for all purpose other than very temporarily if another person would be in danger) has come under heavy fire from many professionals (such as those in the Therapist Neurodiversity Collective) and human rights groups (such as Alliance Against Seclusion and Restraint, Inc. a Maryland nonprofit), often when pertaining to restraint being used in mental health institutions and against autistic people such as children in U.S. public schools.[8][9][10][11][12][13]
Types[edit]
| Medical restraint | |
|---|---|
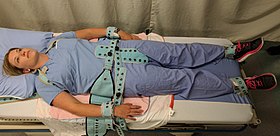 An example of a person in Pinel restraints |
There are many types of medical restraint:
- Four-point restraints, fabric body holders, straitjackets are typically only used temporarily during psychiatric emergencies.
- Restraint masks to prevent patients from biting in retaliation to medical authority in situations where a patient is known to be violent.
- Lap and wheelchair belts, or trays that clip across the front of a wheelchair so that the user can not fall out easily, may be used regularly by patients with neurological disorders which affect balance and movement.
- All four side rails being in the upright position on a bed can be considered a restraint.
- Safety vests and jackets can be placed on a patient like any other vest garment. They typically have a long strap at each end that can be tied behind a chair or to the sides of a bed to prevent injury or to settle patients for satisfying basic needs such as eating and sleeping. Posey vests are commonly used with elderly patients who are at risk of serious injury from falling.
- Limb restraints to prevent unwanted activity in various limbs. They are wrapped around the wrists or ankles, and tied to the side of a bed, to prevent self-harm and harm to medical staff. Handcuffs are an example of a limb restraint.
- Mittens to prevent scratching are common for newborns, but may also be used on psychiatric patients or patients who manage to use their hands to undo limb restraints.
- A Papoose board can be used for babies and young children.
- Chemical restraints are drugs that are administered to restrict the freedom of movement or to sedate a patient.
- Holding the patient's arms down on to chair arms from behind so that another person can force-feed the person, often a child, during ABA.[14]
Manual techniques[edit]
A number of private national and regional companies teach physical (non-mechanical) restraint techniques for companies and agencies that care for or have custody of people who might become aggressive. The strategies vary widely, with many based on police or martial art pain compliance techniques, with others using only pain-free techniques. Most also emphasize verbal de-escalation and defusing skills before using any physical skills. A non-inclusive list:
- Crisis Consultant Group (CCG) Non-Violent Physical technique.
- The Mandt System.
- Non Abusive Psychological and Physical Intervention (NAPPI).
- Non-Violent Crisis Intervention (NVCI) techniques.
- Professional Crisis Management (PCM).[15]
- Professional Assault Crisis Training (ProACT).
- Therapeutic Crisis Intervention (TCI).
Adverse effects[edit]
Throughout the last decade or so, there has been an increasing amount of evidence and literature supporting the idea of a restraint free environment due to their contradictory and dangerous effects.[16] This is due to the adverse outcomes associated with restraint use, which include: falls and injuries, incontinence, circulation impairment, agitation, social isolation, and even death.[17][8][9][10][11][12][13]
In a 2017 The Guardian article:
"If you are a woman who has been sexually or physically abused, and mental health problems in women often have close links to violence and abuse, then a safer environment has to be just that: safe and not a re-traumatising experience. (...) Face-down restraint hurts, it is dangerous, and there are some big questions around why it is used more on women than men."[18]
As of 2021 research is still on-going as to how much restraint an cause and/or exacerbate PTSD for the person being restrained.[19][20][21] In a systematic review in 2020:
"Estimation of post-traumatic stress disorder incidence after intervention varies from 25% to 47% and, thus, is not negligible, especially for patients with past traumatic experiences. Subjective perception has high interindividual variability, mostly associated with negative emotions".[20]
Research is also ongoing into the adverse mental health effects on the health workers doing the restraint.[22]
Applicable laws[edit]
United States[edit]
Current United States law requires that most involuntary medical restraints may only be used when ordered by a physician. Such a physician's order, which is subject to renewal upon expiration if necessary, is valid only for a maximum of 24 hours.[23]
Japan[edit]
Japanese law states that psychiatric hospitals may use restraints on patients only if there is a danger that the patients will harm themselves or others. The law also states that a designated psychiatrist must approve the use of restraints and examine the patient at least every 12 hours to determine whether the situation has changed and the patient should be removed from restraints.[24] However, in practice, Japanese psychiatric hospitals use restraints fairly often and for long periods. Despite being required to certify every 12 hours whether a patient still needs restraints, Japanese psychiatric hospitals keep patients in restraints for a much longer time than hospitals in other countries. According to a survey conducted on 689 patients in 11 psychiatric hospitals in Japan, the average time spent in physical restraints is 96 days.[4] Meanwhile, the average time in most other developed countries is at most several hours to tens of hours.
The number of people who are physically restrained in Japanese psychiatric hospitals continues to increase. In 2014 more than 10,000 people were restrained-the highest ever recorded, and more than double the number a decade earlier.[25] It is thought that some of that increase includes older patients with dementia. As a result, the Japanese Ministry of health has revised its guidelines for elderly people in nursing homes to have more restrictions against body restraints. The changes took effect on 1 April 2018.[26]
United Kingdom[edit]
The Millfields Charter is an electronic charter which promotes an end to the teaching to frontline healthcare staff of all prone (face down) restraint holds.[27] In June 2013 the UK government announced that it was considering a ban on the use of face-down restraint in English mental health hospitals.[28]
Face down restraints are used more often on women and girls than on men. 51 out of 58 mental health trusts use restraints unnecessarily when other techniques would work.[citation needed] Organisations opposed to restraints include Mind and Rethink Mental Illness. YoungMinds and Agenda claim restraints are "frightening and humiliating" and "re-traumatises" patients especially women and girls who have previously been survivors of physical or sexual abuse. The charities sent an open letter to health secretary, Jeremy Hunt showing evidence from 'Agenda, the alliance for women and girls at risk', revealing that patients are routinely restrained in some mental health units while others use non-physical ways to calm patients or stop self-harm. According to the letter over half of women with psychiatric problems have suffered abuse, restraint can cause physical harm, frighten and humiliate the victim. Restraint, specially face down restraint can re-traumatise patients who previously suffered violence and abuse. "Mental health units are meant to be caring, therapeutic environments, for people feeling at their most vulnerable, not places where physical force is routine."
Government guidelines state that face down restraint should not be used at all and other types of physical restraint are only for last resort. Research by Agenda found one fifth of women and girl patients in mental health units had been physically restrained. Some trusts averaged over twelve face down restraints per female patient. Over 6% of women, close to 2,000 were restrained face-down in total more than 4,000 times. The figures vary widely between regions.
Some trusts hardly use restraints, others use them routinely. A female patient was in several hospitals and units at times for a decade with mental health issues, she said in some units she was restrained two or three times daily.[citation needed] Katharine Sacks-Jones director of Agenda, maintains trusts use restraint when alternatives would work. Sacks-Jones maintains women her group speak to repeatedly describe face down restraint as a traumatic experience. On occasions male nurses have used it when a woman did not want her medication. "If you are a woman who has been sexually or physically abused, and mental health problems in women often have close links to violence and abuse, then a safer environment has to be just that: safe and not a re-traumatising experience. (...) Face-down restraint hurts, it is dangerous, and there are some big questions around why it is used more on women than men."[18] The use of restraints in UK psychiatric facilities is increasing.[29]"
Prevention[edit]
Given the lack of evidence for the effectiveness and the potential harms associated with the use of physical restraints in many settings, efforts to safely decrease their use may be justified.[30] For older people who are hospitalized, approaches to reduce or eliminate physical restraints such as the use of bedrails, belts in chairs, and fixed tables may include pressure sensor bed or chair alarms, however there is no strong evidence that these types of prevention approaches are effective at decreasing reliance on physical restraints.[30]
See also[edit]
References[edit]
- ^ "Use of Restraints". 15 Nov 2016.
- ^ "Physical Restraints: Patient Who Had Fallen Should Have Been Restrained, Court Rules". Legal Eagle Eye Newsletter for the Nursing Profession. December 1997. Archived from the original on 2013-10-15.
- ^ Cruzan, Susan (1992-06-16). "Patient Restraint Devices Can Be Dangerous". News Release. Food and Drug Administration. Archived from the original on 2008-01-29. Retrieved 2009-08-15.
- ^ a b 長谷川利夫. (2016). 精神科医療における隔離・ 身体拘束実態調査 ~その急増の背景要因を探り縮減への道筋を考える~. 病院・地域精神医学, 59(1), 18–21.
- ^ "Family blames prolonged use of restraints at Kanagawa hospital for English teacher's death". 18 July 2017.
- ^ "認知症でしばられる!? ~急増・病院での身体拘束~".
- ^ Morrison, Leslie (2004-09-16). "Restraint & Seclusion: Review and Update". Archived from the original (PPT) on 2015-12-04.
- ^ a b Richards, Jodi S. Cohen,Jennifer Smith (19 November 2020). "National Ban on School Use of Seclusion and Restraint of Students Introduced in Congress". ProPublica. Retrieved 2022-01-05.
{{cite web}}: CS1 maint: multiple names: authors list (link) - ^ a b Cohen, Jennifer Smith Richards,Jodi S. (17 November 2020). "New Data Shows the Use of Seclusion and Restraint Increased in Illinois Schools During the 2017–18 School Year". ProPublica. Retrieved 2022-01-05.
{{cite web}}: CS1 maint: multiple names: authors list (link) - ^ a b Richards, Jodi S. Cohen,Jennifer Smith (23 April 2020). "How Often Do Schools Use Seclusion and Restraint? The Federal Government Isn't Properly Tracking the Data, According to a New Report". ProPublica. Retrieved 2022-01-05.
{{cite web}}: CS1 maint: multiple names: authors list (link) - ^ a b Cohen, Jodi S.; Richards, Jennifer Smith; Chavis, Lakeidra (2019-11-19). "Children are being locked away, alone and terrified, in schools across Illinois. Often, it's against the law". ProPublica. Retrieved 2022-01-05.
- ^ a b Abamu, Jenny (2019-06-15). "How Some Schools Restrain Or Seclude Students: A Look At A Controversial Practice". NPR. Retrieved 2022-01-05.
- ^ a b "Restraint and Seclusion". Therapist Neurodiversity Collective. Retrieved 2022-01-05.
- ^ "A Parent's Guide to Respectful Feeding Therapy: Part 2". Therapist Neurodiversity Collective. 2021-11-20. Retrieved 2022-01-05.
- ^ "Professional Crisis Management Association".
- ^ Evans D, Wood J, Lambert L (Feb 2003). "Patient injury and physical restraint devices: a systematic review". Journal of Advanced Nursing. 41 (3): 274–82. doi:10.1046/j.1365-2648.2003.02501.x. PMID 12581115.
- ^ Luo H, Lin M, Castle N (Feb 2011). "Physical restraint use and falls in nursing homes: a comparison between residents with and without dementia". American Journal of Alzheimer's Disease & Other Dementias. 26 (1): 44–50. doi:10.1177/1533317510387585. PMC 10845417. PMID 21282277. S2CID 27371684.
- ^ a b End humiliating restraint of mentally ill people, say charities
- ^ Franks, Zenan M.; Alcock, Jonathan A.; Lam, Tommy; Haines, Kimberley J.; Arora, Nitin; Ramanan, Mahesh (2021-04-01). "Physical Restraints and Post-Traumatic Stress Disorder in Survivors of Critical Illness. A Systematic Review and Meta-analysis". Annals of the American Thoracic Society. 18 (4): 689–697. doi:10.1513/AnnalsATS.202006-738OC. ISSN 2329-6933. PMID 33075240. S2CID 224811147.
- ^ a b Chieze, Marie; Hurst, Samia; Kaiser, Stefan; Sentissi, Othman (2019-07-16). "Effects of Seclusion and Restraint in Adult Psychiatry: A Systematic Review". Frontiers in Psychiatry. 10: 491. doi:10.3389/fpsyt.2019.00491. ISSN 1664-0640. PMC 6673758. PMID 31404294.
- ^ Fugger, G.; Gleiss, A.; Baldinger, P.; Strnad, A.; Kasper, S.; Frey, R. (March 2016). "Psychiatric patients' perception of physical restraint". Acta Psychiatrica Scandinavica. 133 (3): 221–231. doi:10.1111/acps.12501. ISSN 1600-0447. PMID 26472265. S2CID 30176888.
- ^ "The Psychological Effects of Restraints on Mental Health Workers".
- ^ Wigder, Herbert; Matthews, Mary S. (2006-03-07). "Restraints". emedicine.com. Archived from the original on 2006-12-05.
- ^ "Number of patients physically restrained at psychiatric hospitals soars". 9 May 2016.
- ^ "身体拘束と隔離がまた増えた". February 2017.
- ^ <!—Staff writer(s) (4 December 2017). "介護施設、身体拘束の要件厳格化" [Tough changes in requirements for physical restraints in nursing homes] (in Japanese). Thompson-Reuters: Reuters Japan.
- ^ "Archived copy". Archived from the original on 2006-12-05. Retrieved 2006-12-05.
{{cite web}}: CS1 maint: archived copy as title (link) - ^ "'Excessive' use of face-down restraint in mental health hospitals". bbc.co.uk. 18 June 2013. Retrieved 19 June 2013.
- ^ Mental health trusts restrain patients 'every 10 minutes' BBC
- ^ a b Abraham, Jens; Hirt, Julian; Richter, Christin; Köpke, Sascha; Meyer, Gabriele; Möhler, Ralph (2022-08-25). "Interventions for preventing and reducing the use of physical restraints of older people in general hospital settings". The Cochrane Database of Systematic Reviews. 2022 (8): CD012476. doi:10.1002/14651858.CD012476.pub2. ISSN 1469-493X. PMC 9404383. PMID 36004796.
