Benzodiazepine withdrawal syndrome
| Benzodiazepine withdrawal syndrome | |
|---|---|
| Other names | Benzo withdrawal |
 | |
| Diazepam is sometimes used in the treatment of benzodiazepine withdrawal.[1] | |
| Specialty | Addiction medicine, Psychiatry |
| Symptoms | Anxiety, irritability, panic attacks, paranoia, tremor, akathisia, dissociation, confusion, insomnia, sensory disturbances, seizures |
| Complications | Seizures, suicide, hyperthermia, psychosis, delirium, catatonia, psychological trauma, death |
| Duration | Average: ~2 months |
| Causes | Stopping or reducing intake of benzodiazepines in a state of dependence |
| Prevention | Gradual dose reduction |
| Benzodiazepines |
|---|
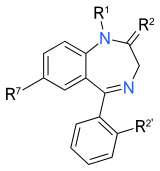 |
Benzodiazepine withdrawal syndrome (BZD withdrawal) is the cluster of signs and symptoms that may emerge when a person who has been taking benzodiazepines as prescribed develops a physical dependence on them and then reduces the dose or stops taking them without a safe taper schedule.
Typically, benzodiazepine withdrawal is characterized by sleep disturbance, irritability, increased tension and anxiety, depression, panic attacks, hand tremor, shaking, sweating, difficulty with concentration, confusion and cognitive difficulty, memory problems, dry mouth, nausea and vomiting, diarrhea, loss of appetite and weight loss, burning sensations and pain in the upper spine, palpitations, headache, nightmares, tinnitus, muscular pain and stiffness, and a host of perceptual changes.[2] More serious symptoms may also occur such as depersonalization, restless legs syndrome, seizures, and suicidal ideation.
Benzodiazepine withdrawal can also lead to disturbances in mental function that persist for several months or years after onset of symptoms (referred to as post-acute-withdrawal syndrome in this form).
Withdrawal symptoms can be managed through awareness of the withdrawal reactions, individualized taper strategies according to withdrawal severity, the addition of alternative strategies such as reassurance, and referral to benzodiazepine withdrawal support groups.[3][4]
Signs and symptoms
[edit]Withdrawal symptoms occur during dose reduction and may include insomnia, anxiety, distress, weight loss, dizziness, night sweats, shaking, muscle twitches, aphasia, panic attacks, depression, dissociation, paranoia, indigestion, diarrhea, and photophobia. As withdrawal progresses, patients often find their physical and mental health improves with improved mood and improved cognition.
A more complete list of possible symptoms stated in publications:
- Akathisia (restlessness)
- Agitation and anxiety[1]
- Panic attacks[2][5]
- Blurred vision[5]
- Chest pain[5]
- Depersonalization[6] and derealization (feelings of unreality)[7]
- Depression (can be severe),[8] possible suicidal ideation
- Dilated pupils[9]
- Dizziness[5]
- Dry mouth[5]
- Dysphoria[10][11]
- High blood pressure[12][13]
- Fatigue and weakness[5]
- Gastrointestinal disturbance (e.g., nausea, diarrhea, vomiting)[14][15][16]
- Hearing disturbance[5]
- Headache[2]
- Hot and cold spells[5]
- Hyperosmia[17]
- Hyperacusis[18][19]
- Hypnagogic hallucinations[20]
- Hypochondriasis[5]
- Increased sensitivity to touch[7]
- Increased urinary frequency[5]
- Insomnia[14]
- Impaired memory and concentration[2][5]
- Loss of appetite and weight loss[21]
- Mild to moderate aphasia[17]
- Mood swings[5]
- Muscular spasms, cramps, or fasciculations[22]
- Nightmares[14]
- Obsessive–compulsive symptoms[23][24]
- Paraesthesia[5][7][17][25][26]
- Paranoia[17]
- Perspiration[2]
- Photophobia[17]
- Postural hypotension[14]
- REM sleep rebound[27]
- Restless legs syndrome[4]
- Stiffness[5]
- Taste and smell disturbances[5]
- Tachycardia[28]
- Tinnitus[29]
- Tremor[30][31]
- Visual disturbances[7]
Rapid discontinuation may result in a more serious syndrome
- Catatonia,[32][33][34]
- Confusion[1]
- Seizures,[1] which may result in death[35][36]
- Coma[37] (rare)
- Delirium tremens[38][39]
- Hyperthermia[14]
- Mania[40][41]
- Neuroleptic malignant syndrome-like event[42][43] (rare)
- Organic brain syndrome[44]
- Post-traumatic stress disorder[4]
- Psychosis[45][46]
- Suicidal ideation[47] or suicide[48][49]
- Violence and aggression[5][50]
Mechanism
[edit]The neuroadaptive processes involved in tolerance, dependence, and withdrawal mechanisms implicate both the GABAergic and the glutamatergic systems.[51] Gamma-Aminobutyric acid (GABA) is the major inhibitory neurotransmitter of the central nervous system; roughly one-quarter to one-third of synapses use GABA.[52] GABA mediates the influx of chloride ions through ligand-gated chloride channels called GABAA receptors. When chloride enters the nerve cell, the cell membrane potential hyperpolarizes thereby inhibiting depolarization, or reduction in the firing rate of the post-synaptic nerve cell.[53] Benzodiazepines potentiate the action of GABA,[54] by binding a site between the α and γ subunits of the 5-subunit receptor[55] thereby increasing the frequency of the GABA-gated chloride channel opening in the presence of GABA.[56]
When potentiation is sustained by long-term use, neuroadaptations occur which result in decreased GABAergic response. What is certain is that surface GABAA receptor protein levels are altered in response to benzodiazepine exposure, as is receptor turnover rate.[57] The exact reason for the reduced responsiveness has not been elucidated but down-regulation of the number of receptors has only been observed at some receptor locations including in the pars reticulata of the substantia nigra; down-regulation of the number of receptors or internalization does not appear to be the main mechanism at other locations.[58] Evidence exists for other hypotheses including changes in the receptor conformation, changes in turnover, recycling, or production rates, degree of phosphorylation and receptor gene expression, subunit composition, decreased coupling mechanisms between the GABA and benzodiazepine site, decrease in GABA production, and compensatory increased glutamatergic activity.[51][57] A unified model hypothesis involves a combination of internalization of the receptor, followed by preferential degradation of certain receptor sub-units, which provides the nuclear activation for changes in receptor gene transcription.[57]
It has been postulated that when benzodiazepines are cleared from the brain, these neuroadaptations are "unmasked", leading to unopposed excitability of the neuron.[59] Glutamate is the most abundant excitatory neurotransmitter in the vertebrate nervous system.[60] Increased glutamate excitatory activity during withdrawal may lead to sensitization or kindling of the CNS, possibly leading to worsening cognition and symptomatology and making each subsequent withdrawal period worse.[61][62][63] Those who have a prior history of withdrawing from benzodiazepines are found to be less likely to succeed the next time around.[64]
Diagnosis
[edit]In severe cases, the withdrawal reaction or protracted withdrawal may exacerbate or resemble serious psychiatric and medical conditions, such as mania, schizophrenia, agitated depression, panic disorder, generalised anxiety disorder, and complex partial seizures and, especially at high doses, seizure disorders.[9] Failure to recognize discontinuation symptoms can lead to false evidence for the need to take benzodiazepines, which in turn leads to withdrawal failure and reinstatement of benzodiazepines, often to higher doses. Pre-existing disorder or other causes typically do not improve, whereas symptoms of protracted withdrawal gradually improve over the ensuing months.[9]
Symptoms may lack a psychological cause and can fluctuate in intensity with periods of good and bad days until eventual recovery.[65][66]
Prevention
[edit]According to the British National Formulary, it is better to withdraw too slowly rather than too quickly from benzodiazepines.[67] The rate of dosage reduction is best carried out so as to minimize the symptoms' intensity and severity. Anecdotally, a slow rate of reduction may reduce the risk of developing a severe protracted syndrome.
Long half-life benzodiazepines like diazepam[1] or chlordiazepoxide are preferred to minimize rebound effects and are available in low dose forms. Some people may not fully stabilize between dose reductions, even when the rate of reduction is slowed. Such people sometimes simply need to persist as they may not feel better until they have been fully withdrawn from them for a period of time.[68]
Management
[edit]
Management of benzodiazepine dependence involves considering the person's age, comorbidity and the pharmacological pathways of benzodiazepines.[70] Psychological interventions may provide a small but significant additional benefit over gradual dose reduction alone at post-cessation and at follow-up.[71] The psychological interventions studied were relaxation training, cognitive-behavioral treatment of insomnia, and self-monitoring of consumption and symptoms, goal-setting, management of withdrawal and coping with anxiety.[71]
There is no standard approach to managing benzodiazepine withdrawal.[72] With sufficient motivation and the proper approach, almost anyone can successfully withdraw from benzodiazepines. However, a prolonged and severe withdrawal syndrome can cause profound disability, which may lead to breakdown of relationships, loss of employment, financial difficulties, as well as more serious adverse effects such as hospitalization and suicide.[48] As such, long-term users should not be forced to discontinue against their will.[25]
Over-rapid withdrawal, lack of explanation, and failure to reassure individuals that they are experiencing temporary withdrawal symptoms led some people to experience increased panic and fears they are going mad, with some people developing a condition similar to post-traumatic stress disorder as a result. A slow withdrawal regimen, coupled with reassurance from family, friends, and peers improves the outcome.[25][20] According to a 2015 Cochrane review, cognitive behavior therapy plus taper was effective in achieving discontinuation in the short-term but the effect was not certain after six months.[73]
Medications
[edit]While some substitutive pharmacotherapies may have promise, current evidence is insufficient to support their use.[71] Some studies found that the abrupt substitution of substitutive pharmacotherapy was actually less effective than gradual dose reduction alone, and only three studies found benefits of adding melatonin,[74] paroxetine,[75] trazodone,[76] or valproate[76] in conjunction with a gradual dose reduction.[71]
- Antipsychotics are generally ineffective for benzodiazepine withdrawal-related psychosis.[26][77] Antipsychotics should be avoided during benzodiazepine withdrawal as they tend to aggravate withdrawal symptoms, including convulsions.[67][78][79][80] Some antipsychotic agents may be riskier than others during withdrawal, especially clozapine, olanzapine or low potency phenothiazines (e.g., chlorpromazine), as they lower the seizure threshold and can worsen withdrawal effects; if used, extreme caution is required.[81]
- Barbiturates are cross tolerant to benzodiazepines and should generally be avoided; however phenobarbital can be used, as it is relatively safe,[82] see below.
- Benzodiazepines or cross tolerant drugs should be avoided after discontinuation, even occasionally. These include the nonbenzodiazepines Z-drugs, which have a similar mechanism of action. This is because tolerance to benzodiazepines has been demonstrated to be still present at four months to two years after withdrawal depending on personal biochemistry. Re-exposures to benzodiazepines typically resulted in a reactivation of the tolerance and benzodiazepine withdrawal syndrome.[83][84]
- Bupropion, which is used primarily as an antidepressant and smoking cessation aid, is contraindicated in people experiencing abrupt withdrawal from benzodiazepines or other sedative-hypnotics (e.g. alcohol), due to an increased risk of seizures.[85]
- Buspirone augmentation was not found to increase the discontinuation success rate.[86]
- Caffeine may worsen withdrawal symptoms because of its stimulatory properties.[25] At least one animal study has shown some modulation of the benzodiazepine site by caffeine, which produces a lowering of seizure threshold.[87]
- Carbamazepine, an anticonvulsant, appears to have some beneficial effects in the treatment and management of benzodiazepine withdrawal; however, research is limited and thus the ability of experts to make recommendations on its use for benzodiazepine withdrawal is not possible at present.[83]
- Ethanol, the primary alcohol in alcoholic beverages, even mild to moderate use, has been found to be a significant predictor of withdrawal failure, probably because of its cross tolerance with benzodiazepines.[25][83][88]
- Flumazenil has been found to stimulate the reversal of tolerance and the normalization of receptor function. However, further research is needed in the form of randomised trials to demonstrate its role in the treatment of benzodiazepine withdrawal.[89][needs update] Flumazenil stimulates the up-regulation and reverses the uncoupling of benzodiazepine receptors to the GABAA receptor, thereby reversing tolerance and reducing withdrawal symptoms and relapse rates.[90][91] Because of limited research and experience compared to the possible risks involved, the flumazenil detoxification method is controversial and can only be done as an inpatient procedure under medical supervision.
- Flumazenil was found to be more effective than placebo in reducing feelings of hostility and aggression in patients who had been free of benzodiazepines for 4–266 weeks.[92] This may suggest a role for flumazenil in treating protracted benzodiazepine withdrawal symptoms.
- A study into the effects of the benzodiazepine receptor antagonist, flumazenil, on benzodiazepine withdrawal symptoms persisting after withdrawal was carried out by Lader and Morton. Study subjects had been benzodiazepine-free for between one month and five years, but all reported persisting withdrawal effects to varying degrees. Persistent symptoms included clouded thinking, tiredness, muscular symptoms such as neck tension, depersonalisation, cramps and shaking and the characteristic perceptual symptoms of benzodiazepine withdrawal, namely, pins and needles feeling, burning skin, pain and subjective sensations of bodily distortion. Therapy with 0.2–2 mg of flumazenil intravenously was found to decrease these symptoms in a placebo-controlled study. This is of interest as benzodiazepine receptor antagonists are neutral and have no clinical effects. The author of the study suggested the most likely explanation is past benzodiazepine use and subsequent tolerance had locked the conformation of the GABA-BZD receptor complex into an inverse agonist conformation, and the antagonist flumazenil resets benzodiazepine receptors to their original sensitivity. Flumazenil was found in this study to be a successful treatment for protracted benzodiazepine withdrawal syndrome, but further research is required.[93] A study by Professor Borg in Sweden produced similar results in patients in protracted withdrawal.[5] In 2007, Hoffmann–La Roche the makers of flumazenil, acknowledged the existence of protracted benzodiazepine withdrawal syndromes, but did not recommended flumazenil to treat the condition.[94]
- Fluoroquinolone antibiotics[95][96][97] have been noted to increase the incidence of a CNS toxicity from 1% in the general population, to 4% in benzodiazepine-dependent population or in those undergoing withdrawal from them. This is probably the result of their GABA antagonistic effects as they have been found to competitively displace benzodiazepines from benzodiazepine receptor sites. This antagonism can precipitate acute withdrawal symptoms, that can persist for weeks or months before subsiding. The symptoms include depression, anxiety, psychosis, paranoia, severe insomnia, paresthesia, tinnitus, hypersensitivity to light (photophobia) and sound (hyperacusis), tremors, status epilepticus, suicidal thoughts and suicide attempt. Fluoroquinolone antibiotics should be contraindicated in patients who are dependent on or in benzodiazepine withdrawal.[25][98][99][100][101] NSAIDs have some mild GABA antagonistic properties and animal research indicate that some may even displace benzodiazepines from their binding site. However, NSAIDs taken in combination with fluoroquinolones cause a very significant increase in GABA antagonism, GABA toxicity, seizures, and other severe adverse effects.[102][103][104]
- Imidazenil has received some research for management of benzodiazepine withdrawal, but is not currently used in withdrawal.[105]
- Imipramine was found to statistically increase the discontinuation success rate.[86]
- Melatonin augmentation was found to statistically increase the discontinuation success rate for people with insomnia.[86]
- Phenobarbital, a barbiturate, is used at "detox" or other inpatient facilities to prevent seizures during rapid withdrawal or cold turkey. The phenobarbital is followed by a one- to two-week taper, although a slow taper from phenobarbital is preferred.[9] In a comparison study, a rapid taper using benzodiazepines was found to be superior to a phenobarbital rapid taper.[106][107]
- Pregabalin may help reduce the severity of benzodiazepine withdrawal symptoms,[108] and reduce the risk of relapse.[109]
- Propranolol was not found to increase the discontinuation success rate.[86]
- SSRI antidepressants have been found to have little value in the treatment of benzodiazepine withdrawal.[110]
- Trazodone was not found to increase the discontinuation success rate.[86]
Inpatient treatment
[edit]Inpatient drug detox or rehabilitation facilities may be inappropriate for those who have become tolerant or dependent while taking the drug as prescribed, as opposed to recreational use. Such inpatient referrals may be traumatic for these individuals.[9]
Prognosis
[edit]A 2006 meta-analysis found evidence for the efficacy of stepped care: minimal intervention (e.g. send an advisory letter, or meet a large number of patients to advise discontinuation), followed by systematic tapered discontinuation alone without augmentation if the first try was unsuccessful.[86] Cognitive behavioral therapy improved discontinuation success rates for panic disorder, melatonin for insomnia, and flumazenil or sodium valproate for general long-term benzodiazepine use.[86] A ten-year follow-up found that more than half of those who had successfully withdrawn from long-term use were still abstinent two years later and that if they were able to maintain this state at two years, they were likely to maintain this state at the ten-year follow-up.[111] One study found that after one year of abstinence from long-term use of benzodiazepines, cognitive, neurological and intellectual impairments had returned to normal.[112]
Those who had a prior psychiatric diagnosis had a similar success rate from a gradual taper at a two-year follow-up.[68][113] Withdrawal from benzodiazepines did not lead to an increased use of antidepressants.[114]
Withdrawal process
[edit]It can be too difficult to withdraw from short- or intermediate-acting benzodiazepines because of the intensity of the rebound symptoms felt between doses.[25][115][116][117] Moreover, short-acting benzodiazepines appear to produce a more intense withdrawal syndrome.[118] For this reason, discontinuation is sometimes carried out by first substituting an equivalent dose of a short-acting benzodiazepine with a longer-acting one like diazepam or chlordiazepoxide. Failure to use the correct equivalent amount can precipitate a severe withdrawal reaction.[119] Benzodiazepines with a half-life of more than 24 hours include chlordiazepoxide, diazepam, clobazam, clonazepam, chlorazepinic acid, ketazolam, medazepam, nordazepam, and prazepam. Benzodiazepines with a half-life of less than 24 hours include alprazolam, bromazepam, brotizolam, flunitrazepam, loprazolam, lorazepam, lormetazepam, midazolam, nitrazepam, oxazepam, and temazepam.[111] The resultant equivalent dose is then gradually reduced.
The consensus is to reduce dosage gradually over several weeks, e.g. 4 or more weeks for diazepam doses over 30 mg/day,[1] with the rate determined by the person's ability to tolerate symptoms.[120] The recommended reduction rates range from 50% of the initial dose every week or so,[121] to 10–25% of the daily dose every 2 weeks.[120] For example, the reduction rate used in the Heather Ashton protocol calls for eliminating 10% of the remaining dose every two to four weeks, depending on the severity and response to reductions with the final dose at 0.5 mg dose of diazepam or 2.5 mg dose of chlordiazepoxide.[25] For most people, discontinuation over 4–6 weeks or 4–8 weeks is suitable.[122] A prolonged period of reduction for longer than six months should be avoided to prevent the withdrawal process from becoming a "morbid focus" for the person.[83]
Duration
[edit]After the last dose has been taken, the acute phase of the withdrawal generally lasts for about two months although withdrawal symptoms, even from low-dose use, can persist for six to twelve months gradually improving over that period,[123][68] however, clinically significant withdrawal symptoms may persist for years, although gradually declining.
A clinical trial of patients taking the benzodiazepine alprazolam for as short as eight weeks triggered protracted symptoms of memory deficits which were still present up to eight weeks after cessation of alprazolam.[124]
Protracted withdrawal syndrome
[edit]Protracted withdrawal syndrome refers to symptoms persisting for months or even years. A significant minority of people withdrawing from benzodiazepines, perhaps 10–15%, experience a protracted withdrawal syndrome which can sometimes be severe. Symptoms may include tinnitus,[29][125] psychosis, cognitive deficits, gastrointestinal complaints, insomnia, paraesthesia (tingling and numbness), pain (usually in limbs and extremities), muscle pain, weakness, tension, painful tremor, shaking attacks, jerks, dizziness and blepharospasm[20] and may occur even without a pre-existing history of these symptoms. Tinnitus occurring during dose reduction or discontinuation of benzodiazepines is alleviated by recommencement of benzodiazepines. Dizziness is often reported as being the withdrawal symptom that lasts the longest.
A study testing neuropsychological factors found psychophysiological markers differing from normals, and concluded that protracted withdrawal syndrome was a genuine iatrogenic condition caused by the long-term use.[126] The causes of persisting symptoms are a combination of pharmacological factors such as persisting drug induced receptor changes, psychological factors both caused by the drug and separate from the drug and possibly in some cases, particularly high dose users, structural brain damage or structural neuronal damage.[20][127] Symptoms continue to improve over time, often to the point where people eventually resume their normal lives, even after years of incapacity.[25]
A slow withdrawal rate significantly reduces the risk of a protracted or severe withdrawal state. Protracted withdrawal symptoms can be punctuated by periods of good days and bad days. When symptoms increase periodically during protracted withdrawal, physiological changes may be present, including dilated pupils as well as an increase in blood pressure and heart rate.[9] The change in symptoms has been proposed to be due to changes in receptor sensitivity for GABA during the process of tolerance reversal.[25] A meta-analysis found cognitive impairments in many areas due to benzodiazepine use show improvements after six months of withdrawal, but significant impairments in most areas may be permanent or may require more than six months to reverse.[128]
Protracted symptoms continue to fade over a period of many months or several years. There is no known cure for protracted benzodiazepine withdrawal syndrome except time,[20] however, the medication flumazenil was found to be more effective than placebo in reducing feelings of hostility and aggression in patients who had been free of benzodiazepines for 4–266 weeks.[92] This may suggest a role for flumazenil in treating protracted benzodiazepine withdrawal symptoms.
Epidemiology
[edit]The severity and length of the withdrawal syndrome is likely determined by various factors, including rate of tapering, length of use and dosage size, and possible genetic factors.[25][129] Those who have a prior history of withdrawing from benzodiazepines may have a sensitized or kindled central nervous system leading to worsening cognition and symptomatology, and making each subsequent withdrawal period worse.[61][62][63][130]
Special populations
[edit]Pediatrics
[edit]A neonatal withdrawal syndrome, sometimes severe, can occur when the mother had taken benzodiazepines, especially during the third trimester. Symptoms include hypotonia, apnoeic spells, cyanosis, impaired metabolic responses to cold stress, and seizures. The neonatal benzodiazepine withdrawal syndrome has been reported to persist from hours to months after birth.[131]
A withdrawal syndrome is seen in about 20% of pediatric intensive care unit children after infusions with benzodiazepines or opioids.[132] The likelihood of having the syndrome correlates with total infusion duration and dose, although duration is thought to be more important.[133] Treatment for withdrawal usually involves weaning over a 3- to 21-day period if the infusion lasted for more than a week.[134] Symptoms include tremors, agitation, sleeplessness, inconsolable crying, diarrhea and sweating. In total, over fifty withdrawal symptoms are listed in this review article.[132][135] Environmental measures aimed at easing the symptoms of neonates with severe abstinence syndrome had little impact, but providing a quiet sleep environment helped in mild cases.[132]
Pregnancy
[edit]Discontinuing benzodiazepines or antidepressants abruptly due to concerns of teratogenic effects of the medications has a high risk of causing serious complications, so is not recommended. For example, abrupt withdrawal of benzodiazepines or antidepressants has a high risk of causing extreme withdrawal symptoms, including suicidal ideation and a severe rebound effect of the return of the underlying disorder if present. This can lead to hospitalisation and potentially, suicide. One study reported one-third of mothers who suddenly discontinued or very rapidly tapered their medications became acutely suicidal due to 'unbearable symptoms'. One woman had a medical abortion, as she felt she could no longer cope, and another woman used alcohol in a bid to combat the withdrawal symptoms from benzodiazepines. Spontaneous abortions may also result from abrupt withdrawal of psychotropic medications, including benzodiazepines. The study reported physicians generally are not aware of the severe consequences of abrupt withdrawal of psychotropic medications such as benzodiazepines or antidepressants.[47]
Elderly
[edit]A study of the elderly who were benzodiazepine dependent found withdrawal could be carried out with few complications and could lead to improvements in sleep and cognitive abilities. At 52 weeks after successful withdrawal, a 22% improvement in cognitive status was found, as well as improved social functioning. Those who remained on benzodiazepines experienced a 5% decline in cognitive abilities, which seemed to be faster than that seen in normal aging, suggesting the longer the intake of benzodiazepines, the worse the cognitive effects become. Some worsening of symptoms were seen in the first few months of benzodiazepine abstinence, but at a 24-week follow-up, elderly subjects were clearly improved compared to those who remained on benzodiazepines. Improvements in sleep were seen at the 24- and 52-week follow-ups. The authors concluded benzodiazepines were not effective in the long term for sleep problems except in suppressing withdrawal-related rebound insomnia. Improvements were seen between 24 and 52 weeks after withdrawal in many factors, including improved sleep and several cognitive and performance abilities. Some cognitive abilities, which are sensitive to benzodiazepines, as well as age, such as episodic memory, did not improve. The authors, however, cited a study in younger patients who at a 3.5-year follow-up showed no memory impairments and speculated that certain memory functions take longer to recover from chronic benzodiazepine use and further improvements in elderly people's cognitive function may occur beyond 52 weeks after withdrawal. The reason it took 24 weeks for improvements to be seen after cessation of benzodiazepine use was due to the time it takes the brain to adapt to the benzodiazepine-free environment.[136]
At 24 weeks, significant improvements were found, including accuracy of information processing improved, but a decline was seen in those who remained on benzodiazepines. Further improvements were noted at the 52-week follow-up, indicating ongoing improvements with benzodiazepine abstinence. Younger people on benzodiazepines also experience cognitive deterioration in visual-spatial memory but are not as vulnerable as the elderly to the cognitive effects.[136] Improved reaction times were noted at 52 weeks in elderly patients free from benzodiazepines. This is an important function in the elderly, especially if they drive a car due to the increased risk of road traffic accidents in benzodiazepine users.[136] At the 24-week follow-up, 80% of people had successfully withdrawn from benzodiazepines. Part of the success was attributed to the placebo method used for part of the trial which broke the psychological dependence on benzodiazepines when the elderly patients realised they had completed their gradual reduction several weeks previously and had only been taking placebo tablets. This helped reassure them they could sleep without their pills.[136]
The authors also warned of the similarities in pharmacology and mechanism of action of the newer nonbenzodiazepine Z drugs.[136]
The elimination half-life of diazepam and chlordiazepoxide, as well as other long half-life benzodiazepines, is twice as long in the elderly compared to younger individuals. Many doctors do not adjust benzodiazepine dosage according to age in elderly patients.[137]
See also
[edit]References
[edit]- ^ a b c d e f Soyka M (2017). "Treatment of Benzodiazepine Dependence". The New England Journal of Medicine. 376 (12): 1147–1157. doi:10.1056/NEJMra1611832. PMID 28328330. S2CID 205117734.
- ^ a b c d e Petursson, H. (1994). "The benzodiazepine withdrawal syndrome". Addiction. 89 (11): 1455–9. doi:10.1111/j.1360-0443.1994.tb03743.x. PMID 7841856.
- ^ Onyett, SR (1989). "The benzodiazepine withdrawal syndrome and its management". The Journal of the Royal College of General Practitioners. 39 (321): 160–3. PMC 1711840. PMID 2576073.
- ^ a b c Ashton, Heather (1991). "Protracted withdrawal syndromes from benzodiazepines". Journal of Substance Abuse Treatment. 8 (1–2): 19–28. doi:10.1016/0740-5472(91)90023-4. PMID 1675688.
- ^ a b c d e f g h i j k l m n o p q Saxon, L.; Hjemdahl, P.; Hiltunen, A. J.; Borg, S. (1997). "Effects of flumazenil in the treatment of benzodiazepine withdrawal - a double-blind pilot study". Psychopharmacology. 131 (2): 153–60. doi:10.1007/s002130050278. PMID 9201803. S2CID 19374966.
- ^ Terao, T; Yoshimura, R; Terao, M; Abe, K (1992). "Depersonalization following nitrazepam withdrawal". Biological Psychiatry. 31 (2): 212–3. doi:10.1016/0006-3223(92)90209-I. PMID 1737083. S2CID 26522217.
- ^ a b c d Mintzer, M. Z.; Stoller, K. B.; Griffiths, R. R. (1999). "A controlled study of flumazenil-precipitated withdrawal in chronic low-dose benzodiazepine users". Psychopharmacology. 147 (2): 200–9. doi:10.1007/s002130051161. PMID 10591888. S2CID 35666163.
- ^ Lader, Malcolm (1994). "Anxiety or depression during withdrawal of hypnotic treatments". Journal of Psychosomatic Research. 38: 113–23, discussion 118–23. doi:10.1016/0022-3999(94)90142-2. PMID 7799243.
- ^ a b c d e f Gabbard, Glen O. (15 May 2007). Gabbard's Treatments of Psychiatric Disorders, Fourth Edition (Treatments of Psychiatric Disorders). American Psychiatric Publishing. pp. 209–211. ISBN 978-1-58562-216-0. Archived from the original on 26 July 2024. Retrieved 28 August 2020.
- ^ Mendelson, WB; Weingartner, H; Greenblatt, DJ; Garnett, D; Gillin, JC (1982). "A clinical study of flurazepam". Sleep. 5 (4): 350–60. doi:10.1093/sleep/5.4.350. PMID 6761826.
- ^ Schöpf, J. (2008). "Withdrawal Phenomena after Long-term Administration of Benzodiazepines a Review of Recent Investigations". Pharmacopsychiatry. 16 (1): 1–8. doi:10.1055/s-2007-1017439. PMID 6131447. S2CID 23063064.
- ^ Mintzer, Miriam Z.; Griffiths, Roland R. (2004). "Flumazenil-precipitated withdrawal in healthy volunteers following repeated diazepam exposure". Psychopharmacology. 178 (2–3): 259–67. doi:10.1007/s00213-004-2009-1. PMID 15452683. S2CID 22130710.
- ^ Biswas, AK; Feldman, BL; Davis, DH; Zintz, EA (2005). "Myocardial ischemia as a result of severe benzodiazepine and opioid withdrawal". Clinical Toxicology. 43 (3): 207–9. doi:10.1081/clt-200053099. PMID 15902797. Archived from the original on 26 July 2020. Retrieved 29 June 2019.
- ^ a b c d e Bismuth, C; Le Bellec, M; Dally, S; Lagier, G (1980). "Benzodiazepine physical dependence. 6 cases (author's transl)". La Nouvelle Presse Médicale. 9 (28): 1941–5. PMID 6106922.
- ^ Loeb, P; Adnet, P; Boittiaux, P; Forget, AP; Mille, FX (1997). "Sevrage en benzodiazépines révélé par un syndrome douloureux abdominal pseudochirurgical" [Benzodiazepine withdrawal masquerading as surgical abdominal syndrome]. Annales Françaises d'Anesthésie et de Réanimation (in French). 16 (5): 521–2. doi:10.1016/S0750-7658(97)83345-X. PMID 9750606.
- ^ "Archived copy". Archived from the original on 23 September 2020. Retrieved 6 February 2009.
{{cite web}}: CS1 maint: archived copy as title (link)[full citation needed] - ^ a b c d e Pelissolo, A; Bisserbe, JC (1994). "Dependence on benzodiazepines. Clinical and biological aspects". L'Encéphale. 20 (2): 147–57. PMID 7914165.
- ^ Beeley, L (15 June 1991). "Benzodiazepines and tinnitus". BMJ: British Medical Journal. 302 (6790): 1465. doi:10.1136/bmj.302.6790.1465. ISSN 0959-8138. PMC 1670117. PMID 2070121.
- ^ Lader, M. (June 1994). "Anxiolytic drugs: dependence, addiction and abuse". European Neuropsychopharmacology. 4 (2): 85–91. doi:10.1016/0924-977x(94)90001-9. ISSN 0924-977X. PMID 7919947. S2CID 44711894. Archived from the original on 7 February 2022. Retrieved 23 February 2021.
- ^ a b c d e Professor Heather Ashton (2004). "Protracted Withdrawal Symptoms From Benzodiazepines". Comprehensive Handbook of Drug & Alcohol Addiction. Archived from the original on 28 September 2020. Retrieved 5 February 2009.
- ^ Pecknold, J.C. (1993). "Discontinuation reactions to alprazolam in panic disorder". Journal of Psychiatric Research. 27: 155–170. doi:10.1016/0022-3956(93)90025-W. PMID 8145176.
- ^ Kliniska Färdigheter: Informationsutbytet Mellan Patient Och Läkare, LINDGREN, STEFAN, ISBN 91-44-37271-X (Swedish)[page needed]
- ^ Drummond, Lynne M.; Matthews, Helen P. (1988). "SINGLE CASE STUDY Obsessive-Compulsive Disorder Occurring as a Complication in Benzodiazepine Withdrawal". Journal of Nervous and Mental Disease. 176 (11): 688–91. doi:10.1097/00005053-198811000-00008. PMID 3183654. S2CID 28340232.
- ^ Matthews, HP; Drummond, LM (1987). "Obsessive-compulsive disorder—a complication of benzodiazepine withdrawal". British Journal of Psychiatry. 150 (2): 272. doi:10.1192/s0007125000122810. PMID 3651695.
- ^ a b c d e f g h i j k l Professor Heather Ashton (2002). "Benzodiazepines: How They Work and How to Withdraw". Archived from the original on 15 September 2011.
- ^ a b Shader, RI; Greenblatt, DJ (1981). "The use of benzodiazepines in clinical practice". British Journal of Clinical Pharmacology. 11 (Suppl 1): 5S–9S. doi:10.1111/j.1365-2125.1981.tb01832.x. PMC 1401641. PMID 6133535.
- ^ Pagel, J. F.; Parnes, Bennett L. (2001). "Medications for the Treatment of Sleep Disorders". Primary Care Companion to the Journal of Clinical Psychiatry. 3 (3): 118–125. doi:10.4088/PCC.v03n0303. PMC 181172. PMID 15014609.
- ^ Van Engelen, BG; Gimbrere, JS; Booy, LH (1993). "Benzodiazepine withdrawal reaction in two children following discontinuation of sedation with midazolam". Annals of Pharmacotherapy. 27 (5): 579–81. doi:10.1177/106002809302700509. PMID 8347907. S2CID 38855049.
- ^ a b Beeley, L (1991). "Benzodiazepines and tinnitus". BMJ. 302 (6790): 1465. doi:10.1136/bmj.302.6790.1465. PMC 1670117. PMID 2070121.
- ^ Mellor, CS; Jain, VK (1982). "Diazepam withdrawal syndrome: Its prolonged and changing nature". Canadian Medical Association Journal. 127 (11): 1093–6. PMC 1862031. PMID 7139456.
- ^ Olajide, Dele; Lader, Malcolm (2009). "Depression following withdrawal from long-term benzodiazepine use: A report of four cases". Psychological Medicine. 14 (4): 937–40. doi:10.1017/S0033291700019899. PMID 6152745. S2CID 46604969.
- ^ Rosebush, Patricia I.; Mazurek, Michael F. (1996). "Catatonia After Benzodiazepine Withdrawal". Journal of Clinical Psychopharmacology. 16 (4): 315–9. doi:10.1097/00004714-199608000-00007. PMID 8835707.
- ^ Deuschle, M.F.; Lederbogen, F (2001). "Benzodiazepine Withdrawal - Induced Catatonia". Pharmacopsychiatry. 34 (1): 41–2. doi:10.1055/s-2001-15188. PMID 11229621. S2CID 260241781.
- ^ Kanemoto, Kousuke; Miyamoto, Toshio; Abe, Ryuji (1999). "Ictal catatonia as a manifestation of de novo absence status epilepticus following benzodiazepine withdrawal". Seizure. 8 (6): 364–6. doi:10.1053/seiz.1999.0309. PMID 10512781. S2CID 17454162.
- ^ Metten, Pamela; Crabbe, John C (1999). "Genetic Determinants of Severity of Acute Withdrawal from Diazepam in Mice". Pharmacology Biochemistry and Behavior. 63 (3): 473–9. doi:10.1016/S0091-3057(99)00017-9. PMID 10418790. S2CID 21241791.
- ^ Haque, W; Watson, DJ; Bryant, SG (1990). "Death following suspected alprazolam withdrawal seizures: A case report". Texas Medicine. Vol. 86, no. 1. pp. 44–7. PMID 2300914.
- ^ De Bard, ML (1979). "Diazepam withdrawal syndrome: A case with psychosis, seizure, and coma". American Journal of Psychiatry. 136 (1): 104–5. doi:10.1176/ajp.136.1.104. PMID 103443.
- ^ Provini, F.; Cortelli, P.; Montagna, P.; Gambetti, P.; Lugaresi, E. (2008). "Fatal insomnia and agrypnia excitata: Sleep and the limbic system". Revue Neurologique. 164 (8–9): 692–700. doi:10.1016/j.neurol.2007.11.003. PMID 18805303.
- ^ Berezak, A.; Weber, M.; Hansmann, J.; Tulasne, P.A.; Laporte, B.; Ould Ouali, A. (1984). "Dépendance physique aux benzodiazépines dans un contexte traumatologique" [Benzodiazepine physical dependence in traumatology]. Annales Françaises d'Anesthésie et de Réanimation (in French). 3 (5): 383–4. doi:10.1016/S0750-7658(84)80078-7. PMID 6149713.
- ^ Turkington, Douglas; Gill, Paul (1989). "Mania induced by lorazepam withdrawal: A report of two cases". Journal of Affective Disorders. 17 (1): 93–5. doi:10.1016/0165-0327(89)90028-1. PMID 2525581.
- ^ Lapierre, YD; Labelle, A (1987). "Manic-like reaction induced by lorazepam withdrawal". The Canadian Journal of Psychiatry. 32 (8): 697–8. doi:10.1177/070674378703200812. PMID 3690487. S2CID 8932926.
- ^ Kawajiri, M; Ohyagi, Y; Furuya, H; Araki, T; Inoue, N; Esaki, S; Yamada, T; Kira, J (2002). "A patient with Parkinson's disease complicated by hypothyroidism who developed malignant syndrome after discontinuation of etizolam". Rinsho Shinkeigaku. 42 (2): 136–9. PMID 12424963.
- ^ Strawn, Jeffrey; Keck Jr, PE; Caroff, SN (2007). "Neuroleptic Malignant Syndrome". American Journal of Psychiatry. 164 (6): 870–6. doi:10.1176/ajp.2007.164.6.870. PMID 17541044.
- ^ Khan, A; Joyce, P; Jones, AV (1980). "Benzodiazepine withdrawal syndromes". The New Zealand Medical Journal. 92 (665): 94–6. PMID 6107888. Archived from the original on 2 December 2019. Retrieved 7 April 2009.
- ^ Peh, LH; Mahendran, R (1989). "Psychiatric complications of Erimin abuse". Singapore Medical Journal. 30 (1): 72–3. PMID 2595393.
- ^ Fruensgaard, K. (1976). "Withdrawal Psychosis: A Study of 30 Consecutive Cases". Acta Psychiatrica Scandinavica. 53 (2): 105–18. doi:10.1111/j.1600-0447.1976.tb00065.x. PMID 3091. S2CID 1741725.
- ^ a b Einarson, A; Selby, P; Koren, G (2001). "Abrupt discontinuation of psychotropic drugs during pregnancy: Fear of teratogenic risk and impact of counselling". Journal of Psychiatry & Neuroscience. 26 (1): 44–8. PMC 1408034. PMID 11212593.
- ^ a b Colvin, Rod (26 August 2008). Overcoming Prescription Drug Addiction: A Guide to Coping and Understanding (3 ed.). United States of America: Addicus Books. pp. 74–76. ISBN 978-1-886039-88-9. Archived from the original on 26 July 2024. Retrieved 28 August 2020.
I have treated ten thousand patients for alcohol and drug problems and have detoxed approximately 1,500 patients for benzodiazepines – the detox for the benzodiazepines is one of the hardest detoxes we do. It can take an extremely long time, about half the length of time they have been addicted – the ongoing relentless withdrawals can be so incapacitating it can cause total destruction to one's life – marriages break up, businesses are lost, bankruptcy, hospitalization, and of course suicide is probably the most single serious side effect.
- ^ Dodds TJ (2017). "Prescribed Benzodiazepines and Suicide Risk: A Review of the Literature". Primary Care Companion for CNS Disorders. 19 (2). doi:10.4088/PCC.16r02037. PMID 28257172.
- ^ Citrome, Leslie; Volavka, Jan (1999). "Violent Patients in the Emergency Setting". Psychiatric Clinics of North America. 22 (4): 789–801. doi:10.1016/S0193-953X(05)70126-X. PMID 10623971.
- ^ a b Allison, C; Pratt, J.A (2003). "Neuroadaptive processes in GABAergic and glutamatergic systems in benzodiazepine dependence". Pharmacology & Therapeutics. 98 (2): 171–95. doi:10.1016/S0163-7258(03)00029-9. PMID 12725868.
- ^ Dubuc, Bruno. "Neurotransmitters". The Brain from Top to Bottom. Archived from the original on 29 June 2013. Retrieved 29 April 2013.
- ^ Tallman, J F; Gallager, D W (1985). "The Gaba-Ergic System: A Locus of Benzodiazepine Action". Annual Review of Neuroscience. 8: 21–44. doi:10.1146/annurev.ne.08.030185.000321. PMID 2858999.
- ^ Schoch, P.; Richards, J. G.; Häring, P.; Takacs, B.; Stähli, C.; Staehelin, T.; Haefely, W.; Möhler, H. (1985). "Co-localization of GABAA receptors and benzodiazepine receptors in the brain shown by monoclonal antibodies". Nature. 314 (6007): 168–71. Bibcode:1985Natur.314..168S. doi:10.1038/314168a0. PMID 2983231. S2CID 1381200.
- ^ Vinkers, Christiaan H.; Olivier, Berend (2012). "Mechanisms Underlying Tolerance after Long-Term Benzodiazepine Use: A Future for Subtype-Selective GABAA Receptor Modulators?". Advances in Pharmacological Sciences. 2012: 1–19. doi:10.1155/2012/416864. PMC 3321276. PMID 22536226.
- ^ Study, R. E.; Barker, JL (1981). "Diazepam and (–)-pentobarbital: fluctuation analysis reveals different mechanisms for potentiation of γ-aminobutyric acid responses in cultured central neurons". Proceedings of the National Academy of Sciences of the United States of America. 78 (11): 7180–4. Bibcode:1981PNAS...78.7180S. doi:10.1073/pnas.78.11.7180. JSTOR 11434. PMC 349220. PMID 6273918.
- ^ a b c Bateson, A. (2002). "Basic Pharmacologic Mechanisms Involved in Benzodiazepine Tolerance and Withdrawal". Current Pharmaceutical Design. 8 (1): 5–21. doi:10.2174/1381612023396681. PMID 11812247.
- ^ Tietz, EI; Rosenberg, HC; Chiu, TH (1986). "Autoradiographic localization of benzodiazepine receptor downregulation". Journal of Pharmacology and Experimental Therapeutics. 236 (1): 284–92. PMID 3001290.
- ^ Koob, G.; Bloom, F. (1988). "Cellular and molecular mechanisms of drug dependence". Science. 242 (4879): 715–23. Bibcode:1988Sci...242..715K. doi:10.1126/science.2903550. PMID 2903550.
- ^ Meldrum, Brian S. (2000). "Glutamate as a Neurotransmitter in the Brain: Review of Physiology and Pathology". Journal of Nutrition. 130 (4): 1007S–15S. doi:10.1093/jn/130.4.1007s. PMID 10736372.
- ^ a b Stephens, D. N. (1995). "A glutamatergic hypothesis of drug dependence: extrapolations from benzodiazepine receptor ligands". Behavioural Pharmacology. 6 (5): 425–46. doi:10.1097/00008877-199508000-00004. PMID 11224351.
- ^ a b Dunworth, Sarah J.; Mead, Andy N.; Stephens, David N. (2000). "Previous experience of withdrawal from chronic diazepam ameliorates the aversiveness of precipitated withdrawal and reduces withdrawal-induced c-fos expression in nucleus accumbens". European Journal of Neuroscience. 12 (4): 1501–8. doi:10.1046/j.1460-9568.2000.00036.x. PMID 10762378. S2CID 42898466.
- ^ a b Rickels, Karl; Schweizer, E; Csanalosi, I; Case, WG; Chung, H (1988). "Long-term Treatment of Anxiety and Risk of Withdrawal: Prospective Comparison of Clorazepate and Buspirone". Archives of General Psychiatry. 45 (5): 444–50. doi:10.1001/archpsyc.1988.01800290060008. PMID 2895993.
- ^ Vorma, Helena; Naukkarinen, Hannu H.; Sarna, Seppo J.; Kuoppasalmi, Kimmo I. (2005). "Predictors of Benzodiazepine Discontinuation in Subjects Manifesting Complicated Dependence". Substance Use & Misuse. 40 (4): 499–510. doi:10.1081/JA-200052433. PMID 15830732. S2CID 1366333.
- ^ Smith, David E.; Wesson, Donald R. (1983). "Benzodiazepine Dependency Syndromes". Journal of Psychoactive Drugs. 15 (1–2): 85–95. doi:10.1080/02791072.1983.10472127. PMID 6136575.
- ^ Landry, MJ; Smith, DE; McDuff, DR; Baughman, OL (1992). "Benzodiazepine dependence and withdrawal: Identification and medical management". The Journal of the American Board of Family Practice. 5 (2): 167–75. PMID 1575069.
- ^ a b Committee on Safety of Medicines (2007). "Hypnotics and anxiolytics". British National Formulary. Retrieved 17 September 2007.(registration required)
- ^ a b c Higgitt, A C; Lader, M H; Fonagy, P (1985). "Clinical management of benzodiazepine dependence". British Medical Journal. 291 (6497): 688–90. doi:10.1136/bmj.291.6497.688. PMC 1416639. PMID 2864096.
- ^ Lal R, Gupta S, Rao R, Kattimani S (2007). "Emergency management of substance overdose and withdrawal" (PDF). Substance Use Disorder. World Health Organization (WHO). p. 82. Archived from the original (PDF) on 13 June 2010. Retrieved 6 June 2009.
Generally, a longer-acting benzodiazepine such as chlordiazepoxide or diazepam is used and the initial dose titrated downward
- ^ Santos C, Olmedo RE (2017). "Sedative-Hypnotic Drug Withdrawal Syndrome: Recognition And Treatment". Emergency Medicine Practice. 19 (3): 1–20. PMID 28186869.
- ^ a b c d Parr, Jannette M.; Kavanagh, David J.; Cahill, Lareina; Mitchell, Geoffrey; Mcd Young, Ross McD. (2009). "Effectiveness of current treatment approaches for benzodiazepine discontinuation: A meta-analysis". Addiction. 104 (1): 13–24. doi:10.1111/j.1360-0443.2008.02364.x. PMID 18983627.
- ^ Fluyau, D; Revadigar, N; Manobianco, BE (May 2018). "Challenges of the pharmacological management of benzodiazepine withdrawal, dependence, and discontinuation". Therapeutic Advances in Psychopharmacology. 8 (5): 147–168. doi:10.1177/2045125317753340. PMC 5896864. PMID 29713452.
- ^ Darker, Catherine D.; Sweeney, Brion P.; Barry, Joe M.; Farrell, Michael F.; Donnelly-Swift, Erica (2015). "Psychosocial interventions for benzodiazepine harmful use, abuse or dependence". The Cochrane Database of Systematic Reviews (5): CD009652. doi:10.1002/14651858.CD009652.pub2. hdl:2262/75957. ISSN 1469-493X. PMC 11023022. PMID 26106751.
- ^ Garfinkel, Doron; Zisapel, N; Wainstein, J; Laudon, M (1999). "Facilitation of Benzodiazepine Discontinuation by Melatonin: A New Clinical Approach". Archives of Internal Medicine. 159 (20): 2456–60. doi:10.1001/archinte.159.20.2456. PMID 10665894.
- ^ Nakao, Mutsuhiro; Takeuchi, Takeaki; Nomura, Kyoko; Teramoto, Tamio; Yano, Eiji (2006). "Clinical application of paroxetine for tapering benzodiazepine use in non-major-depressive outpatients visiting an internal medicine clinic". Psychiatry and Clinical Neurosciences. 60 (5): 605–10. doi:10.1111/j.1440-1819.2006.01565.x. PMID 16958945. S2CID 44969935.
- ^ a b Rickels, K.; Schweizer, E.; Garcia España, F.; Case, G.; Demartinis, N.; Greenblatt, D. (1999). "Trazodone and valproate in patients discontinuing long-term benzodiazepine therapy: Effects on withdrawal symptoms and taper outcome". Psychopharmacology. 141 (1): 1–5. doi:10.1007/s002130050798. PMID 9952057. S2CID 12903042.
- ^ Fruensgaard, K (1977). "Withdrawal psychosis after drugs. Report of a consecutive material". Ugeskrift for Læger. 139 (29): 1719–22. PMID 898354.
- ^ Tagashira, Eijiro; Hiramori, Tameo; Urano, Tomoko; Nakao, Kenzo; Yanaura, Saizo (1981). "Enhancement of drug withdrawal convulsion by combinations of phenobarbital and antipsychotic agents". The Japanese Journal of Pharmacology. 31 (5): 689–99. doi:10.1254/jjp.31.689. PMID 6118452.
- ^ Bobolakis, Ioannis (2000). "Neuroleptic Malignant Syndrome After Antipsychotic Drug Administration During Benzodiazepine Withdrawal". Journal of Clinical Psychopharmacology. 20 (2): 281–3. doi:10.1097/00004714-200004000-00033. PMID 10770479.
- ^ Randall, Michael D; Neil, Karen E (February 2004). "5". Disease management (1 ed.). Pharmaceutical Press. p. 62. ISBN 978-0-85369-523-3. Archived from the original on 26 July 2024. Retrieved 1 June 2009.
- ^ Ebadi, Manuchair (23 October 2007). "Alphabetical presentation of drugs". Desk Reference for Clinical Pharmacology (2nd ed.). USA: CRC Press. p. 512. ISBN 978-1-4200-4743-1.
- ^ First, Michael B.; Tasman, Allan (8 February 2010). Clinical Guide to the Diagnosis and Treatment of Mental Disorders By Michael B. First, Allan Tasman, p. 242. John Wiley & Sons. ISBN 978-0-470-74520-5. Archived from the original on 6 October 2023. Retrieved 14 March 2023.
- ^ a b c d Lader, Malcolm; Tylee, Andre; Donoghue, John (2009). "Withdrawing Benzodiazepines in Primary Care". CNS Drugs. 23 (1): 19–34. doi:10.2165/0023210-200923010-00002. PMID 19062773. S2CID 113206.
- ^ Higgitt, A.; Fonagy, P.; Lader, M. (2009). "The natural history of tolerance to the benzodiazepines". Psychological Medicine. Monograph Supplement. 13: 1–55. doi:10.1017/S0264180100000412. PMID 2908516. S2CID 38037200.
- ^ "Wellbutrin XL Prescribing Information" (PDF). GlaxoSmithKline. December 2008. Archived from the original (PDF) on 26 March 2009. Retrieved 16 January 2010.
- ^ a b c d e f g Voshaar, R. C. O.; Couvée, JE; Van Balkom, AJ; Mulder, PG; Zitman, FG (2006). "Strategies for discontinuing long-term benzodiazepine use: Meta-analysis". British Journal of Psychiatry. 189 (3): 213–20. doi:10.1192/bjp.189.3.213. PMID 16946355.
- ^ Seale, Thomas W.; Carney, John M.; Rennert, Owen M.; Flux, Marinus; Skolnick, Phil (1987). "Coincidence of seizure susceptibility to caffeine and to the benzodiazepine inverse agonist, DMCM, in SWR and CBA inbred mice". Pharmacology Biochemistry and Behavior. 26 (2): 381–7. doi:10.1016/0091-3057(87)90133-X. PMID 3575358. S2CID 30168114.
- ^ Schweizer, Edward; Rickels, K; Case, WG; Greenblatt, DJ (1990). "Long-term Therapeutic Use of Benzodiazepines: II. Effects of Gradual Taper". Archives of General Psychiatry. 47 (10): 908–15. doi:10.1001/archpsyc.1990.01810220024003. PMID 2222130.
- ^ Denis, Cecile; Fatseas, Melina; Lavie, Estelle; Auriacombe, Marc (2006). Denis, Cecile (ed.). "Pharmacological interventions for benzodiazepine mono-dependence management in outpatient settings". Cochrane Database of Systematic Reviews (3): CD005194. doi:10.1002/14651858.CD005194.pub2. PMID 16856084. (Retracted, see doi:10.1002/14651858.CD005194.pub3, PMID 23780681, Retraction Watch)
- ^ Gerra, G.; Zaimovic, A.; Giusti, F.; Moi, G.; Brewer, C. (2002). "Intravenous flumazenil versus oxazepam tapering in the treatment of benzodiazepine withdrawal: A randomized, placebo-controlled study". Addiction Biology. 7 (4): 385–95. doi:10.1080/1355621021000005973. PMID 14578014. S2CID 21255719.
- ^ Little, H.J. (1991). "The benzodiazepines: Anxiolytic and withdrawal effects". Neuropeptides. 19: 11–4. doi:10.1016/0143-4179(91)90077-V. PMID 1679209. S2CID 13734753.
- ^ a b L. Saxon, S. Borg & A. J. Hiltunen (August 2010). "Reduction of aggression during benzodiazepine withdrawal: effects of flumazenil". Pharmacology Biochemistry and Behavior. 96 (2): 148–151. doi:10.1016/j.pbb.2010.04.023. PMID 20451546. S2CID 41351863.
- ^ Lader, M. H.; Morton, S. V. (1992). "A pilot study of the effects of flumazenil on symptoms persisting after benzodiazepine withdrawal". Journal of Psychopharmacology. 6 (3): 357–63. doi:10.1177/026988119200600303. PMID 22291380. S2CID 23530701.
- ^ Roche USA (October 2007). "Romazicon" (PDF). Roche Pharmaceuticals USA. Archived from the original (PDF) on 25 June 2008.
- ^ Unseld, E; G Ziegler; A Gemeinhardt; U Janssen; U Klotz (July 1990). "Possible interaction of fluoroquinolones with the benzodiazepine-GABAA-receptor complex (summary)". British Journal of Clinical Pharmacology. 30 (1): 63–70. doi:10.1111/j.1365-2125.1990.tb03744.x. PMC 1368276. PMID 2167717.
- ^ Ashton, Heather (April 2011). "The Ashton Manual Supplement". Benzodiazepines: How They Work & How to Withdraw. benzo.org.uk. Archived from the original on 19 September 2020. Retrieved 20 December 2019.
- ^ Kamath, Ashwin (2013). "Fluoroquinolone Induced Neurotoxicity: A Review" (PDF). Journal of Advanced Pharmacy Education & Research. 3 (1): 16–19. Archived from the original (PDF) on 11 February 2014. Retrieved 17 October 2015.
- ^ McConnell, John Girvan (2008). "Benzodiazepine tolerance, dependency, and withdrawal syndromes and interactions with fluoroquinolone antimicrobials". British Journal of General Practice. 58 (550): 365–6. doi:10.3399/bjgp08X280317. PMC 2435654. PMID 18482496.
- ^ Unseld, E; Ziegler, G; Gemeinhardt, A; Janssen, U; Klotz, U (1990). "Possible interaction of fluoroquinolones with the benzodiazepine-GABAA- receptor complex". British Journal of Clinical Pharmacology. 30 (1): 63–70. doi:10.1111/j.1365-2125.1990.tb03744.x. PMC 1368276. PMID 2167717.
- ^ Sternbach, Harvey; State, Rosanne (1997). "Antibiotics: Neuropsychiatric Effects and Psychotropic Interactions". Harvard Review of Psychiatry. 5 (4): 214–26. doi:10.3109/10673229709000304. PMID 9427014. S2CID 21259675.
- ^ Committee on Safety of Medicines; Medicines and Healthcare products Regulatory Agency (2008). "Quinolones". United Kingdom: British National Formulary. Archived from the original on 30 June 2012. Retrieved 16 February 2009.
- ^ Wong, PT (1993). "Interactions of indomethacin with central GABA systems". Archives Internationales de Pharmacodynamie et de Thérapie. 324: 5–16. PMID 8297186.
- ^ Delanty, Norman (November 2001). "Medication associated seizures". Seizures: Medical Causes and Management. Humana Press. pp. 152–153. ISBN 978-0-89603-827-1.[permanent dead link]
- ^ Green, M. A.; Halliwell, R. F. (1997). "Selective antagonism of the GABAAreceptor by ciprofloxacin and biphenylacetic acid". British Journal of Pharmacology. 122 (3): 584–90. doi:10.1038/sj.bjp.0701411. PMC 1564969. PMID 9351519.
- ^ Auta, J; Costa, E; Davis, J; Guidotti, A (2005). "Imidazenil: An antagonist of the sedative but not the anticonvulsant action of diazepam". Neuropharmacology. 49 (3): 425–9. doi:10.1016/j.neuropharm.2005.04.005. PMID 15964602. S2CID 44619421.
- ^ Sullivan, Mark; Toshima, Michelle; Lynn, Pamela; Roy-Byrne, Peter (1993). "Phenobarbital Versus Clonazepam for Sedative-Hypnotic Taper in Chronic Pain Patients: A Pilot Study". Annals of Clinical Psychiatry. 5 (2): 123–8. doi:10.3109/10401239309148974. PMID 8348204.
- ^ Ray Baker. "Dr Ray Baker's Article on Addiction: Benzodiazepines in Particular". Archived from the original on 29 July 2020. Retrieved 14 February 2009.
- ^ Oulis, P.; Konstantakopoulos, G. (2010). "Pregabalin in the treatment of alcohol and benzodiazepines dependence". CNS Neuroscience & Therapeutics. 16 (1): 45–50. doi:10.1111/j.1755-5949.2009.00120.x. PMC 6493856. PMID 20070788.
- ^ Oulis, P.; Konstantakopoulos, G. (July 2012). "Efficacy and safety of pregabalin in the treatment of alcohol and benzodiazepine dependence". Expert Opinion on Investigational Drugs. 21 (7): 1019–29. doi:10.1517/13543784.2012.685651. PMID 22568872. S2CID 24354141.
- ^ Zitman, F. G.; Couvée, JE (2001). "Chronic benzodiazepine use in general practice patients with depression: An evaluation of controlled treatment and taper-off: Report on behalf of the Dutch Chronic Benzodiazepine Working Group". British Journal of Psychiatry. 178 (4): 317–24. doi:10.1192/bjp.178.4.317. PMID 11282810.
- ^ a b De Gier, N.; Gorgels, W.; Lucassen, P.; Oude Voshaar, R.; Mulder, J.; Zitman, F. (2010). "Discontinuation of long-term benzodiazepine use: 10-year follow-up". Family Practice. 28 (3): 253–9. doi:10.1093/fampra/cmq113. PMID 21193495.
- ^ Tönne, U.; Hiltunen, A. J.; Vikander, B.; Engelbrektsson, K.; Bergman, H.; Bergman, I.; Leifman, H.; Borg, S. (1995). "Neuropsychological changes during steady-state drug use, withdrawal, and abstinence in primary benzodiazepine-dependent patients". Acta Psychiatrica Scandinavica. 91 (5): 299–304. doi:10.1111/j.1600-0447.1995.tb09786.x. PMID 7639085. S2CID 9339677.
- ^ Kan, CC; Mickers, FC; Barnhoorn, D (2006). "Short- and long-term results of a systematic benzodiazepine discontinuation programme for psychiatric patients". Tijdschrift voor Psychiatrie. 48 (9): 683–93. PMID 17007474.
- ^ Jørgensen, VR (2009). "Benzodiazepine reduction does not imply an increased consumption of antidepressants. A survey of two medical practices". Ugeskrift for Læger. 171 (41): 2999–3003. PMID 19814928.
- ^ Lal R, Gupta S, Rao R, Kattimani S (2007). "Emergency management of substance overdose and withdrawal" (PDF). Substance Use Disorder. World Health Organisation. p. 82. Archived from the original (PDF) on 13 June 2010. Retrieved 6 June 2009.
Generally, a longer-acting benzodiazepine such as chlordiazepoxide or diazepam is used and the initial dose titrated downward
- ^ Noyes, Russell; Perry, Paul J.; Crowe, Raymond R.; Coryell, William H.; Clancy, John; Yamada, Thoru; Gabel, Janelle (1986). "Seizures Following the Withdrawal of Alprazolam". Journal of Nervous and Mental Disease. 174 (1): 50–2. doi:10.1097/00005053-198601000-00009. PMID 2867122.
- ^ Noyes Jr, R; Clancy, J; Coryell, WH; Crowe, RR; Chaudhry, DR; Domingo, DV (1985). "A withdrawal syndrome after abrupt discontinuation of alprazolam". American Journal of Psychiatry. 142 (1): 114–6. doi:10.1176/ajp.142.1.114. PMID 2857066.
- ^ Rickels, Karl; Schweizer, E; Case, WG; Greenblatt, DJ (1990). "Long-term Therapeutic Use of Benzodiazepines: I. Effects of Abrupt Discontinuation". Archives of General Psychiatry. 47 (10): 899–907. doi:10.1001/archpsyc.1990.01810220015002. PMID 2222129.
- ^ Neale, G; Smith, AJ (2007). "Self-harm and suicide associated with benzodiazepine usage". British Journal of General Practice. 57 (538): 407–8. PMC 2047018. PMID 17504594.
- ^ a b Soyka (2017), Treatment of Withdrawal Symptoms, p. 1151 cited "Drug misuse and dependence: UK guidelines on clinical management" (PDF). London: Department of Health (England), Scottish Government, Welsh Assembly Government, Northern Ireland Executive. 2017. Archived from the original (PDF) on 19 September 2010. Retrieved 29 September 2020.
- ^ Soyka (2017), Treatment of Withdrawal Symptoms, p. 1151 cited Soyka, M (2015). Medikamentenabhängigkeit. Stuttgart, Germany: Schattauer.
- ^ Soyka (2017), Treatment of Withdrawal Symptoms, p. 1151
- ^ Murphy, S. M.; Tyrer, P. (1991). "A double-blind comparison of the effects of gradual withdrawal of lorazepam, diazepam and bromazepam in benzodiazepine dependence". British Journal of Psychiatry. 158 (4): 511–6. doi:10.1192/bjp.158.4.511. PMID 1675901. S2CID 10998674.
- ^ Curran, H. V.; Bond, A.; O'Sullivan, G.; Bruce, M.; Marks, I.; Lelliot, P.; Shine, P.; Lader, M. (2009). "Memory functions, alprazolam and exposure therapy: A controlled longitudinal study of agoraphobia with panic disorder". Psychological Medicine. 24 (4): 969–76. doi:10.1017/S0033291700029056. PMID 7892364. S2CID 38165723.
- ^ Busto, Usoa; Fornazzari, Luis; Naranjo, Claudio A. (1988). "Protracted Tinnitus after Discontinuation of Long-Term Therapeutic Use of Benzodiazepines". Journal of Clinical Psychopharmacology. 8 (5): 359–362. doi:10.1097/00004714-198810000-00010. PMID 2903182.
- ^ Higgitt, A.; Fonagy, P.; Toone, B.; Shine, P. (1990). "The prolonged benzodiazepine withdrawal syndrome: Anxiety or hysteria?". Acta Psychiatrica Scandinavica. 82 (2): 165–8. doi:10.1111/j.1600-0447.1990.tb01375.x. PMID 1978465. S2CID 41458371.
- ^ Ashton CH (March 1995). "Protracted Withdrawal From Benzodiazepines: The Post-Withdrawal Syndrome". Psychiatric Annals. 25 (3). benzo.org.uk: 174–179. doi:10.3928/0048-5713-19950301-11. Archived from the original on 20 September 2020. Retrieved 16 April 2008.
- ^ Barker, M; Greenwood, KM; Jackson, M; Crowe, SF (2004). "Persistence of cognitive effects after withdrawal from long-term benzodiazepine use: A meta-analysis". Archives of Clinical Neuropsychology. 19 (3): 437–54. doi:10.1016/S0887-6177(03)00096-9. PMID 15033227.
- ^ Hood HM, Metten P, Crabbe JC, Buck KJ (February 2006). "Fine mapping of a sedative-hypnotic drug withdrawal locus on mouse chromosome 11". Genes, Brain and Behavior. 5 (1): 1–10. doi:10.1111/j.1601-183X.2005.00122.x. PMID 16436183. S2CID 27844115.
- ^ Vorma, H; Naukkarinen, Hh; Sarna, Sj; Kuoppasalmi, Ki (2005). "Predictors of benzodiazepine discontinuation in subjects manifesting complicated dependence". Substance Use & Misuse. 40 (4): 499–510. doi:10.1081/JA-200052433. PMID 15830732. S2CID 1366333.
- ^ McElhatton, Patricia R. (1994). "The effects of benzodiazepine use during pregnancy and lactation". Reproductive Toxicology. 8 (6): 461–75. doi:10.1016/0890-6238(94)90029-9. PMID 7881198.
- ^ a b c Birchley, Giles (2009). "Opioid and benzodiazepine withdrawal syndromes in the paediatric intensive care unit: A review of recent literature". Nursing in Critical Care. 14 (1): 26–37. doi:10.1111/j.1478-5153.2008.00311.x. PMID 19154308.
- ^ Fontela, Patrícia Scolari; Fontela, Aline; Moraes, Fabrício; Da Silva, Ricardo Bernardi; Sober, Roberta B.; Noer, Francisco; Bruno, Paulo; Einloft, Ana; Garcia, Pedro Celiny Ramos; Piva, Jefferson P. (2003). "Sedation and analgesia in children submitted to mechanical ventilation could be overestimated?". Jornal de Pediatria. 79 (4): 343–8. doi:10.2223/JPED.1046. PMID 14513134.
- ^ Playfor, Stephen; Jenkins, Ian; Boyles, Carolyne; Choonara, Imti; Davies, Gerald; Haywood, Tim; Hinson, Gillian; Mayer, Anton; Morton, Neil; Ralph, Tanya; Wolf, Andrew; United Kingdom Paediatric Intensive Care Society Sedation; Analgesia Neuromuscular Blockade Working Group (2006). "Consensus guidelines on sedation and analgesia in critically ill children". Intensive Care Medicine. 32 (8): 1125–36. doi:10.1007/s00134-006-0190-x. PMID 16699772. S2CID 8518882.
- ^ Ista, Erwin; Van Dijk, Monique; Gamel, Claudia; Tibboel, Dick; De Hoog, Matthijs (2007). "Withdrawal symptoms in children after long-term administration of sedatives and/or analgesics: A literature review. 'Assessment remains troublesome'". Intensive Care Medicine. 33 (8): 1396–406. doi:10.1007/s00134-007-0696-x. hdl:1765/32655. PMID 17541548.
- ^ a b c d e Curran, HV; Collins, R; Fletcher, S; Kee, SC; Woods, B; Iliffe, S (2003). "Older adults and withdrawal from benzodiazepine hypnotics in general practice: effects on cognitive function, sleep, mood and quality of life" (PDF). Psychological Medicine. 33 (7): 1223–37. doi:10.1017/S0033291703008213. PMID 14580077. S2CID 20586160. Archived (PDF) from the original on 22 September 2017. Retrieved 29 June 2019.
- ^ Salzman, Carl (15 May 2004). Clinical geriatric psychopharmacology (4th ed.). USA: Lippincott Williams & Wilkins. pp. 450–3. ISBN 978-0-7817-4380-8.
