Nevus: Difference between revisions
described subtypes of acquired melanocytic nevi |
→Diagnosis: DDx + ancillary tests |
||
| Line 71: | Line 71: | ||
== Diagnosis == |
== Diagnosis == |
||
Nevi are typically diagnosed clinically with the naked eye or using [[dermatoscopy]]. More advanced imaging tests are available for distinguishing melanocytic nevi from melanoma, including computerized dermoscopy and image analysis.<ref>{{Cite journal|last=Rigel|first=Darrell S.|last2=Russak|first2=Julie|last3=Friedman|first3=Robert|date=2016-10-01|title=The evolution of melanoma diagnosis: 25 years beyond the ABCDs|url=https://www.ncbi.nlm.nih.gov/pubmed/20671054|journal=CA: a cancer journal for clinicians|volume=60|issue=5|pages=301–316|doi=10.3322/caac.20074|issn=1542-4863|pmid=20671054}}</ref> The management of nevi depends on the type of nevus and the degree of diagnostic uncertainty. Some nevi are known to be benign, and may simply be monitored over time. Others may warrant more thorough examination and [[biopsy]] for histopathological examination. For example, a clinician may want to determine whether a pigmented nevus is a type of melanocytic nevus, dysplastic nevus, or melanoma as some of these skin lesions pose a risk for malignancy. [[Image:Dermatoscope.jpg|thumb|A modern polarized dermatoscope|none]] |
Nevi are typically diagnosed clinically with the naked eye or using [[dermatoscopy]]. More advanced imaging tests are available for distinguishing melanocytic nevi from melanoma, including computerized dermoscopy and image analysis.<ref>{{Cite journal|last=Rigel|first=Darrell S.|last2=Russak|first2=Julie|last3=Friedman|first3=Robert|date=2016-10-01|title=The evolution of melanoma diagnosis: 25 years beyond the ABCDs|url=https://www.ncbi.nlm.nih.gov/pubmed/20671054|journal=CA: a cancer journal for clinicians|volume=60|issue=5|pages=301–316|doi=10.3322/caac.20074|issn=1542-4863|pmid=20671054}}</ref> The management of nevi depends on the type of nevus and the degree of diagnostic uncertainty. Some nevi are known to be benign, and may simply be monitored over time. Others may warrant more thorough examination and [[biopsy]] for histopathological examination. For example, a clinician may want to determine whether a pigmented nevus is a type of melanocytic nevus, dysplastic nevus, or melanoma as some of these skin lesions pose a risk for malignancy. In addition to histopathological examination, some lesions may also warrant ancillary tests to aid in diagnosis, including special stains, [[immunohistochemistry]], and electron microscopy.<ref>{{Cite book|url=http://link.springer.com/10.1007/978-1-4939-0891-2|title=Melanocytic Lesions - Springer|last=|first=|publisher=|year=|isbn=|location=|pages=|chapter=Ancillary Techniques in Diagnosing Melanocytic Lesions|doi=10.1007/978-1-4939-0891-2|quote=|via=}}</ref> [[Image:Dermatoscope.jpg|thumb|A modern polarized dermatoscope|none]] |
||
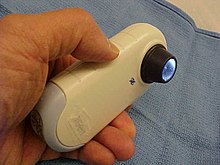
[[Image:Dermatoscope1.JPG|thumb|A [[dermatoscope]]|none]] |
[[Image:Dermatoscope1.JPG|thumb|A [[dermatoscope]]|none]] |
||
=== Differential diagnoses === |
|||
Hypermelanotic nevi must be differentiated from other types of pigmented skin lesions, including<ref>{{Cite book|url=http://link.springer.com/10.1007/978-1-4939-0891-2|title=Melanocytic Lesions - Springer|last=|first=|publisher=|year=|isbn=|location=|pages=|chapter=Lentigo, Other Melanosis, and the Acquired Nevus|doi=10.1007/978-1-4939-0891-2|quote=|via=}}</ref>: |
|||
* [[Lentigo simplex]] |
|||
* [[Solar lentigo]] |
|||
* [[Café au lait macule]] |
|||
* [[Ink spot lentigo|Ink-spot lentigo]] |
|||
* Mucosal melanotic macule |
|||
* Mongolian spot |
|||
== Treatment == |
== Treatment == |
||
Revision as of 05:53, 9 December 2016
| Nevus | |
|---|---|
| Specialty | Dermatology |
Nevus (plural: nevi) is a nonspecific medical term for a visible, circumscribed, chronic lesion of the skin or mucosa.[1] The term originates from nævus, which is Latin for "birthmark," however, a nevus can be either congenital (present at birth) or acquired. Common terms, including mole, birthmark, and beauty mark, are used to describe nevi, but these terms do not distinguish specific types of nevi.
Classification
The term nevus is applied to a number of pigmentation disorders, both hypomelanotic and hypermelanotic,[2] as well as neoplasias and hyperplasias of melanocytes.[3]
Hypomelanotic
- Acquired
- Nevus anemicus

Nevus anemicus.
- Congenital
- Nevus depigmentosus

Nevus depigmentosus
Hypermelanotic
- Acquired
- Acquired melanocytic nevus

Acquired melanocytic nevi. - Types of acquired melanocytic nevi are categorized based on the location of cells[3]:
- Junctional: epidermis
- Intradermal: dermis
- Compound: epidermis and dermis
- Types of acquired melanocytic nevi are categorized based on the location of cells[3]:
- Atypical (dysplastic) nevus

Atypical nevus. - Becker's nevus
Becker's nevus. - Blue nevus (rarely congenital)

Blue nevus - Hori's nevus
- Nevus spilus

Nevus spilus. - Pigmented spindle cell nevus
- Spitz nevus

Spitz nevus. - Zosteriform lentiginous nevus
- Congenital
- Congenital melanocytic nevus

Congenital melanocytic nevus. - Nevus of Ito
- Nevus of Ota

Nevus of Ota.
Additional types of nevi do not involve disorders of pigmentation or melanocytes. These additional nevi represent hamartomatous proliferations of the epithelium,[4] connective tissue,[5] and vascular malformations.[6]
Epidermal nevi
- Verrucous epidermal nevus
- Nevus sebaceous

Nevus sebaceous. - Nevus comedonicus
- Eccrine nevus
- Apocrine nevus
Connective tissue nevi
Vascular nevi

- Nevus flammeus neonatorum (also known as a stork bite or salmon patch)
Diagnosis
Nevi are typically diagnosed clinically with the naked eye or using dermatoscopy. More advanced imaging tests are available for distinguishing melanocytic nevi from melanoma, including computerized dermoscopy and image analysis.[7] The management of nevi depends on the type of nevus and the degree of diagnostic uncertainty. Some nevi are known to be benign, and may simply be monitored over time. Others may warrant more thorough examination and biopsy for histopathological examination. For example, a clinician may want to determine whether a pigmented nevus is a type of melanocytic nevus, dysplastic nevus, or melanoma as some of these skin lesions pose a risk for malignancy. In addition to histopathological examination, some lesions may also warrant ancillary tests to aid in diagnosis, including special stains, immunohistochemistry, and electron microscopy.[8]

Differential diagnoses
Hypermelanotic nevi must be differentiated from other types of pigmented skin lesions, including[9]:
- Lentigo simplex
- Solar lentigo
- Café au lait macule
- Ink-spot lentigo
- Mucosal melanotic macule
- Mongolian spot
Treatment
The treatment of a nevus depends on the specific diagnosis, however, the options for treatment generally the following modalities:
- Observation
- Destruction
- Laser Ablation
- Electrofulguration
- Cryotherapy

Cryotherapy. - Chemical peels
- Excision
Syndromes
Etymology
A nevus may also be spelled naevus. The plural is nevi or naevi. The word is from nævus, Latin for "birthmark".
See also
References
- ^ Happle, Rudolf (1995). "What is a nevus? A proposed definition of a common medical term". Dermatology. 191(1): 1–5.
- ^ "Chapter 75. Hypomelanoses and Hypermelanoses". Fitzpatrick's Dermatology in General Medicine. The McGraw Hill Companies, Inc. 2012. ISBN 978-0-07-166904-7.
- ^ a b c d e "Chapter 122. Benign Neoplasias and Hyperplasias of Melanocytes". Fitzpatrick's Dermatology in General Medicine. The McGraw-Hill Companies, Inc. 2012. ISBN 978-0-07-166904-7.
- ^ "Chapter 118. Benign Epithelial Tumors, Hamartomas, and Hyperplasias.". Fitzpatrick's Dermatology in General Medicine. The McGraw-Hill Companies, Inc. 2012. ISBN 978-0-07-166904-7.
- ^ "Chapter 66. Dermal Hypertrophies and Benign Fibroblastic/Myofibroblastic Tumors.". Fitzpatrick's Dermatology in General Medicine. The McGraw-Hill Companies, Inc. 2012. ISBN 978-0-07-166904-7.
- ^ "Chapter 172. Vascular Malformations.". Fitzpatrick's Dermatology in General Medicine. The McGraw Hill Companies, Inc. 2012. ISBN 978-0-07-166904-7.
- ^ Rigel, Darrell S.; Russak, Julie; Friedman, Robert (2016-10-01). "The evolution of melanoma diagnosis: 25 years beyond the ABCDs". CA: a cancer journal for clinicians. 60 (5): 301–316. doi:10.3322/caac.20074. ISSN 1542-4863. PMID 20671054.
- ^ "Ancillary Techniques in Diagnosing Melanocytic Lesions". Melanocytic Lesions - Springer. doi:10.1007/978-1-4939-0891-2.
- ^ "Lentigo, Other Melanosis, and the Acquired Nevus". Melanocytic Lesions - Springer. doi:10.1007/978-1-4939-0891-2.
External links
- American Academy of Dermatology Melanoma clinical guideline
- DermNet New Zealand - online dermatology library
- Nevus Outreach, Inc.












