Blood pressure: Difference between revisions
Bob K31416 (talk | contribs) changed Pickering 2005 to display 3 authors and then et al. (following AMA citation guideline) by using display-authors=3 and making corresponding changes to 6 {{harv}} inline citations |
Bob K31416 (talk | contribs) On edit page, in citation Pickering 2005 in References section and in 6 {{harv}}s, changed "et al" to "et al: Falkner, BE; Graves, J; Hill, MN; Jones, DW; Kurtz, T; Sheps, SG; Roccella, EJ" to include in metadata and clarify for editors |
||
| Line 30: | Line 30: | ||
A cuff of appropriate size is fitted smoothly and snugly, then inflated manually by repeatedly squeezing a rubber bulb until the artery is completely occluded. Listening with the stethoscope to the [[brachial artery]] at the [[elbow]], the examiner slowly releases the pressure in the cuff. When blood just starts to flow in the artery, the [[Turbulence|turbulent flow]] creates a "whooshing" or pounding (first [[Korotkoff sounds|Korotkoff sound]]). The pressure at which this sound is first heard is the systolic BP. The cuff pressure is further released until no sound can be heard (fifth Korotkoff sound), at the diastolic arterial pressure. |
A cuff of appropriate size is fitted smoothly and snugly, then inflated manually by repeatedly squeezing a rubber bulb until the artery is completely occluded. Listening with the stethoscope to the [[brachial artery]] at the [[elbow]], the examiner slowly releases the pressure in the cuff. When blood just starts to flow in the artery, the [[Turbulence|turbulent flow]] creates a "whooshing" or pounding (first [[Korotkoff sounds|Korotkoff sound]]). The pressure at which this sound is first heard is the systolic BP. The cuff pressure is further released until no sound can be heard (fifth Korotkoff sound), at the diastolic arterial pressure. |
||
The auscultatory method has been predominant since the beginning of BP measurements but is gradually being replaced by other noninvasive techniques better suited to being automated.<ref name='Pickering2005p146'>{{harv|Pickering|Hall|Appel|et al|2005|p=146}} See ''Blood Pressure Measurement Methods''.</ref> |
The auscultatory method has been predominant since the beginning of BP measurements but is gradually being replaced by other noninvasive techniques better suited to being automated.<ref name='Pickering2005p146'>{{harv|Pickering|Hall|Appel|et al: Falkner, BE; Graves, J; Hill, MN; Jones, DW; Kurtz, T; Sheps, SG; Roccella, EJ|2005|p=146}} See ''Blood Pressure Measurement Methods''.</ref> |
||
====Oscillometric method==== |
====Oscillometric method==== |
||
The ''Oscillometric'' method was first demonstrated in 1876 and involves the observation of oscillations in the sphygmomanometer cuff pressure<ref name='Pickering2005p147'>{{harv|Pickering|Hall|Appel|et al|2005|p=147}} See ''The Oscillometric Technique''.</ref> which are caused by the oscillations of [[blood flow]], i.e. the [[pulse]].<ref name='Laurent2003'> {{cite web|url=http://www.blood-pressure-hypertension.com/how-to-measure/measure-blood-pressure-8.shtml |title=Blood Pressure & Hypertension |accessdate=2009-10-05 |last=Laurent |first=P |date=2003-09-28 }}</ref> The electronic version of this method is sometimes used in long-term measurements and general practice. It uses a sphygmomanometer cuff like the auscultatory method, but with an electronic [[pressure sensor]] ([[transducer]]) to observe cuff pressure oscillations, electronics to automatically interpret them, and automatic inflation and deflation of the cuff. The pressure sensor should be calibrated periodically to maintain accuracy. |
The ''Oscillometric'' method was first demonstrated in 1876 and involves the observation of oscillations in the sphygmomanometer cuff pressure<ref name='Pickering2005p147'>{{harv|Pickering|Hall|Appel|et al: Falkner, BE; Graves, J; Hill, MN; Jones, DW; Kurtz, T; Sheps, SG; Roccella, EJ|2005|p=147}} See ''The Oscillometric Technique''.</ref> which are caused by the oscillations of [[blood flow]], i.e. the [[pulse]].<ref name='Laurent2003'> {{cite web|url=http://www.blood-pressure-hypertension.com/how-to-measure/measure-blood-pressure-8.shtml |title=Blood Pressure & Hypertension |accessdate=2009-10-05 |last=Laurent |first=P |date=2003-09-28 }}</ref> The electronic version of this method is sometimes used in long-term measurements and general practice. It uses a sphygmomanometer cuff like the auscultatory method, but with an electronic [[pressure sensor]] ([[transducer]]) to observe cuff pressure oscillations, electronics to automatically interpret them, and automatic inflation and deflation of the cuff. The pressure sensor should be calibrated periodically to maintain accuracy. |
||
Oscillometric measurement requires less skill than the auscultatory technique, and may be suitable for use by untrained staff and for automated patient home monitoring. |
Oscillometric measurement requires less skill than the auscultatory technique, and may be suitable for use by untrained staff and for automated patient home monitoring. |
||
| Line 46: | Line 46: | ||
====White-coat hypertension==== |
====White-coat hypertension==== |
||
For some patients, BP measurements taken in a doctor's office may not correctly characterize their typical BP.<ref name='Elliot2007'>{{cite news | first=Victoria Stagg | last=Elliot | coauthors= | title=Blood pressure readings often unreliable | date=2007-06-11 | publisher=American Medical Association | url =http://www.ama-assn.org/amednews/2007/06/11/hlsa0611.htm | work =American Medical News | pages = | accessdate = 2008-08-16 | language = }}</ref> In up to 25% of patients, the office measurement is higher than their typical BP. This type of error is called [[white-coat hypertension]] (WCH) and can result from anxiety related to an examination by a health care professional.<ref name='Jhalani2005'> {{cite journal|title=Anxiety and outcome expectations predict the white-coat effect|journal=Blood Pressure Monitoring|date=2005|first=Juhee|last=Jhalani|coauthors=Tanya Goyal, Lynn Clemow, et al |volume=10|issue=6|pages=317-9|id=PMID 16496447 |url=http://journals.lww.com/bpmonitoring/pages/articleviewer.aspx?year=2005&issue=12000&article=00006&type=abstract|format=|accessdate=2009-10-03 }}</ref> The misdiagnosis of hypertension for these patients can result in needless and possibly harmful medication. WCH can be reduced (but not eliminated) with automated BP measurements over 15 to 20 minutes in a quiet part of the office or clinic.<ref name='Pickering2005p145'>{{harv|Pickering|Hall|Appel|et al|2005|p=145}} See ''White Coat Hypertension or Isolated Office Hypertension''.</ref> |
For some patients, BP measurements taken in a doctor's office may not correctly characterize their typical BP.<ref name='Elliot2007'>{{cite news | first=Victoria Stagg | last=Elliot | coauthors= | title=Blood pressure readings often unreliable | date=2007-06-11 | publisher=American Medical Association | url =http://www.ama-assn.org/amednews/2007/06/11/hlsa0611.htm | work =American Medical News | pages = | accessdate = 2008-08-16 | language = }}</ref> In up to 25% of patients, the office measurement is higher than their typical BP. This type of error is called [[white-coat hypertension]] (WCH) and can result from anxiety related to an examination by a health care professional.<ref name='Jhalani2005'> {{cite journal|title=Anxiety and outcome expectations predict the white-coat effect|journal=Blood Pressure Monitoring|date=2005|first=Juhee|last=Jhalani|coauthors=Tanya Goyal, Lynn Clemow, et al |volume=10|issue=6|pages=317-9|id=PMID 16496447 |url=http://journals.lww.com/bpmonitoring/pages/articleviewer.aspx?year=2005&issue=12000&article=00006&type=abstract|format=|accessdate=2009-10-03 }}</ref> The misdiagnosis of hypertension for these patients can result in needless and possibly harmful medication. WCH can be reduced (but not eliminated) with automated BP measurements over 15 to 20 minutes in a quiet part of the office or clinic.<ref name='Pickering2005p145'>{{harv|Pickering|Hall|Appel|et al: Falkner, BE; Graves, J; Hill, MN; Jones, DW; Kurtz, T; Sheps, SG; Roccella, EJ|2005|p=145}} See ''White Coat Hypertension or Isolated Office Hypertension''.</ref> |
||
Debate continues regarding the significance of this effect.{{Citation needed|October 2009|date=October 2009}} Some reactive patients will also react to many other stimuli throughout their daily lives, and require treatment. In some cases a lower BP reading occurs at the doctor's office.<ref name='Pickering2005p146a'>{{harv|Pickering|Hall|Appel|et al|2005|p=146}} See ''Masked Hypertension or Isolated Ambulatory Hypertension''.</ref> |
Debate continues regarding the significance of this effect.{{Citation needed|October 2009|date=October 2009}} Some reactive patients will also react to many other stimuli throughout their daily lives, and require treatment. In some cases a lower BP reading occurs at the doctor's office.<ref name='Pickering2005p146a'>{{harv|Pickering|Hall|Appel|et al: Falkner, BE; Graves, J; Hill, MN; Jones, DW; Kurtz, T; Sheps, SG; Roccella, EJ|2005|p=146}} See ''Masked Hypertension or Isolated Ambulatory Hypertension''.</ref> |
||
==== Home monitoring ==== |
==== Home monitoring ==== |
||
| Line 112: | Line 112: | ||
which is in the normal range. |
which is in the normal range. |
||
Various factors influence a person's average BP and variations. Factors such as age and gender<ref name='Reckelhoff2001'> {{cite journal|title=Gender Differences in the Regulation of Blood Pressure|journal=Hypertension|date=2001 May|first=Jane F.|last=Reckelhoff|coauthors=|volume=37|issue=5|pages=1199–208|id=PMID 11358929 |url=http://hyper.ahajournals.org/cgi/content/abstract/hypertensionaha;37/5/1199|format=|accessdate=|pmid=11358929|month=May|day=01 }}</ref> influence average values. In children, the normal ranges are lower than for adults and depend on height.<ref>{{cite journal| title= Blood Pressure Tables for Children and Adolescents| author=National Heart, Lung and Blood Institute| url=http://www.nhlbi.nih.gov/guidelines/hypertension/child_tbl.htm}} (Note that the median BP is given by the 50th percentile and hypertension is defined by the [[Percentile|95th percentile]] for a given age, height, and gender.)</ref> As adults age, systolic pressure tends to rise and diastolic tends to fall.<ref name='Pickering2005p145a'>{{harv|Pickering|Hall|Appel|et al|2005|p=145}} See ''Isolated Systolic Hypertension''.</ref> In the elderly, BP tends to be above the normal adult range,<ref name='Pickering2005p144'>"...more than half of all Americans aged 65 or older have hypertension." {{harv|Pickering|Hall|Appel|et al|2005|p=144}}</ref> largely because of reduced flexibility of the arteries. Also, an individual's BP varies with exercise, emotional reactions, sleep, digestion and time of day. |
Various factors influence a person's average BP and variations. Factors such as age and gender<ref name='Reckelhoff2001'> {{cite journal|title=Gender Differences in the Regulation of Blood Pressure|journal=Hypertension|date=2001 May|first=Jane F.|last=Reckelhoff|coauthors=|volume=37|issue=5|pages=1199–208|id=PMID 11358929 |url=http://hyper.ahajournals.org/cgi/content/abstract/hypertensionaha;37/5/1199|format=|accessdate=|pmid=11358929|month=May|day=01 }}</ref> influence average values. In children, the normal ranges are lower than for adults and depend on height.<ref>{{cite journal| title= Blood Pressure Tables for Children and Adolescents| author=National Heart, Lung and Blood Institute| url=http://www.nhlbi.nih.gov/guidelines/hypertension/child_tbl.htm}} (Note that the median BP is given by the 50th percentile and hypertension is defined by the [[Percentile|95th percentile]] for a given age, height, and gender.)</ref> As adults age, systolic pressure tends to rise and diastolic tends to fall.<ref name='Pickering2005p145a'>{{harv|Pickering|Hall|Appel|et al: Falkner, BE; Graves, J; Hill, MN; Jones, DW; Kurtz, T; Sheps, SG; Roccella, EJ|2005|p=145}} See ''Isolated Systolic Hypertension''.</ref> In the elderly, BP tends to be above the normal adult range,<ref name='Pickering2005p144'>"...more than half of all Americans aged 65 or older have hypertension." {{harv|Pickering|Hall|Appel|et al: Falkner, BE; Graves, J; Hill, MN; Jones, DW; Kurtz, T; Sheps, SG; Roccella, EJ|2005|p=144}}</ref> largely because of reduced flexibility of the arteries. Also, an individual's BP varies with exercise, emotional reactions, sleep, digestion and time of day. |
||
Differences between left and right arm BP measurements tend to be random and average to nearly zero if enough measurements are taken. However, in a small percentage of cases there is a consistently present difference greater than 10 mmHg which may need further investigation, e.g. for [[Cardiovascular disease|obstructive arterial disease]].<ref>{{cite journal |author=Eguchi K, Yacoub M, Jhalani J, Gerin W, Schwartz JE, Pickering TG |title=Consistency of blood pressure differences between the left and right arms |journal=Arch Intern Med |volume=167 |issue=4 |pages=388–93 |year=2007 |month=February |pmid=17325301 |doi= 10.1001/archinte.167.4.388|url=http://archinte.ama-assn.org/cgi/content/full/167/4/388}}</ref><ref>{{cite journal |author=Agarwal R, Bunaye Z, Bekele DM |title=Prognostic significance of between-arm blood pressure differences |journal=Hypertension |volume=51 |issue=3 |pages=657–62 |year=2008 |month=March |pmid=18212263 |doi=10.1161/HYPERTENSIONAHA.107.104943 |url=}}</ref> |
Differences between left and right arm BP measurements tend to be random and average to nearly zero if enough measurements are taken. However, in a small percentage of cases there is a consistently present difference greater than 10 mmHg which may need further investigation, e.g. for [[Cardiovascular disease|obstructive arterial disease]].<ref>{{cite journal |author=Eguchi K, Yacoub M, Jhalani J, Gerin W, Schwartz JE, Pickering TG |title=Consistency of blood pressure differences between the left and right arms |journal=Arch Intern Med |volume=167 |issue=4 |pages=388–93 |year=2007 |month=February |pmid=17325301 |doi= 10.1001/archinte.167.4.388|url=http://archinte.ama-assn.org/cgi/content/full/167/4/388}}</ref><ref>{{cite journal |author=Agarwal R, Bunaye Z, Bekele DM |title=Prognostic significance of between-arm blood pressure differences |journal=Hypertension |volume=51 |issue=3 |pages=657–62 |year=2008 |month=March |pmid=18212263 |doi=10.1161/HYPERTENSIONAHA.107.104943 |url=}}</ref> |
||
| Line 241: | Line 241: | ||
==References== |
==References== |
||
#{{cite journal|title=Recommendations for blood pressure measurement in humans and experimental animals: Part 1: blood pressure measurement in humans: a statement for professionals from the Subcommittee of Professional and Public Education of the American Heart Association Council on High Blood Pressure Research |journal=Hypertension |year=2005|first1=TG |last1=Pickering |first2=JE |last2=Hall |first3=LJ |last3=Appel |first4= |
#{{cite journal|title=Recommendations for blood pressure measurement in humans and experimental animals: Part 1: blood pressure measurement in humans: a statement for professionals from the Subcommittee of Professional and Public Education of the American Heart Association Council on High Blood Pressure Research |journal=Hypertension |year=2005|first1=TG |last1=Pickering |first2=JE |last2=Hall |first3=LJ |last3=Appel |first4=|last4=et al: Falkner, BE; Graves, J; Hill, MN; Jones, DW; Kurtz, T; Sheps, SG; Roccella, EJ |display-authors=3|volume=45|issue=5|pages=142-61|pmid=15611362 |doi=10.1161/01.HYP.0000150859.47929.8e |url=http://hyper.ahajournals.org/cgi/content/full/45/1/142|format=|accessdate=2009-10-01| ref=harv}} |
||
== Footnotes == |
== Footnotes == |
||
Revision as of 16:57, 9 October 2009
- See Hypertension for more information about high blood pressure.

Blood pressure (BP) is the pressure exerted by circulating blood on the walls of blood vessels, and is one of the principal vital signs. During each heartbeat, BP varies between a maximum (systolic) and a minimum (diastolic) pressure. The mean BP decreases as the circulating blood moves away from the heart through arteries, has its greatest decrease in the small arteries and arterioles, and continues to decrease as the blood moves through the capillaries and back to the heart through veins.[1]
The term blood pressure usually refers to the pressure measured at a person's upper arm. It is measured on the inside of an elbow at the brachial artery, which is the upper arm's major blood vessel that carries blood away from the heart. A person's BP is usually expressed in terms of the systolic pressure and diastolic pressure, for example 115/75.
BP is sometimes measured at other places, for instance at an ankle. The ratio of the BP measured at the main artery of an ankle, to the BP measured at a brachial artery, gives the Ankle Brachial Pressure Index (ABPI).
Measurement
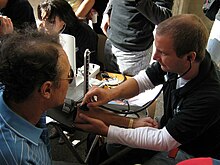
Arterial pressure is most commonly measured via a sphygmomanometer, which historically used the height of a column of mercury to reflect the circulating pressure.[2] Today BP values are still reported in millimetres of mercury (mmHg), though aneroid and electronic devices do not use mercury.
For each heartbeat, BP varies between systolic and diastolic pressures. Systolic pressure is peak pressure in the arteries, which occurs near the end of the cardiac cycle when the ventricles are contracting. Diastolic pressure is minimum pressure in the arteries, which occurs near the beginning of the cardiac cycle when the ventricles are filled with blood. An example of normal measured values for a resting, healthy adult human is 115 mmHg systolic and 75 mmHg diastolic (written as 115/75 mmHg, and spoken [in the US] as "one fifteen over seventy-five"). Pulse pressure is the difference between systolic and diastolic pressures.
Systolic and diastolic arterial BPs are not static but undergo natural variations from one heartbeat to another and throughout the day (in a circadian rhythm). They also change in response to stress, nutritional factors, drugs, disease, exercise, and momentarily from standing up. Sometimes the variations are large. Hypertension refers to arterial pressure being abnormally high, as opposed to hypotension, when it is abnormally low. Along with body temperature, respiratory rate, and pulse rate, BP measurements are the most commonly measured physiological parameters.
Arterial pressures are usually measured non-invasively, without penetrating skin or artery. Measuring pressure invasively, by penetrating the arterial wall to take the measurement, is much less common, and usually restricted to a hospital setting.
Noninvasive measurement
The noninvasive auscultatory and oscillometric measurements are simpler and quicker than invasive measurements, require less expertise in fitting, have virtually no complications, and are less unpleasant and painful for the patient. However, noninvasive methods may yield somewhat lower accuracy and small systematic differences in numerical results. Non-invasive measurement methods are more commonly used for routine examinations and monitoring.
Palpation method
A minimum systolic value can be roughly estimated without any equipment by palpation, most often used in emergency situations. Palpation of a radial pulse indicates a minimum BP of 80 mmHg, a femoral pulse indicates at least 70 mmHg, and a carotid pulse indicates a minimum of 60 mmHg. However, one study indicated that this method was not accurate enough and often overestimated patients' systolic BP.[3] A more accurate value of systolic BP can be obtained with a sphygmomanometer and palpating for when a radial pulse returns.[4] The diastolic blood pressure can not be estimated by this method.[5] Sometimes palpation is used to get an estimate before using the auscultatory method.
Auscultatory method


The auscultatory method (from the Latin for listening) uses a stethoscope and a sphygmomanometer. This comprises an inflatable (Riva-Rocci) cuff placed around the upper arm at roughly the same vertical height as the heart, attached to a mercury or aneroid manometer. The mercury manometer measures the height of a column of mercury, giving an absolute result without need for calibration, and consequently not subject to the errors and drift of calibration which affect other methods. The use of mercury manometers is often required in clinical trials and for the clinical measurement of hypertension in high risk patients, such as pregnant women.
A cuff of appropriate size is fitted smoothly and snugly, then inflated manually by repeatedly squeezing a rubber bulb until the artery is completely occluded. Listening with the stethoscope to the brachial artery at the elbow, the examiner slowly releases the pressure in the cuff. When blood just starts to flow in the artery, the turbulent flow creates a "whooshing" or pounding (first Korotkoff sound). The pressure at which this sound is first heard is the systolic BP. The cuff pressure is further released until no sound can be heard (fifth Korotkoff sound), at the diastolic arterial pressure.
The auscultatory method has been predominant since the beginning of BP measurements but is gradually being replaced by other noninvasive techniques better suited to being automated.[6]
Oscillometric method
The Oscillometric method was first demonstrated in 1876 and involves the observation of oscillations in the sphygmomanometer cuff pressure[7] which are caused by the oscillations of blood flow, i.e. the pulse.[8] The electronic version of this method is sometimes used in long-term measurements and general practice. It uses a sphygmomanometer cuff like the auscultatory method, but with an electronic pressure sensor (transducer) to observe cuff pressure oscillations, electronics to automatically interpret them, and automatic inflation and deflation of the cuff. The pressure sensor should be calibrated periodically to maintain accuracy.
Oscillometric measurement requires less skill than the auscultatory technique, and may be suitable for use by untrained staff and for automated patient home monitoring.
The cuff is inflated to a pressure initially in excess of the systolic arterial pressure, and then reduces to below diastolic pressure over a period of about 30 seconds. When blood flow is nil (cuff pressure exceeding systolic pressure) or unimpeded (cuff pressure below diastolic pressure), cuff pressure will be essentially constant. It is essential that the cuff size is correct: undersized cuffs may yield too high a pressure, whereas oversized cuffs yield too low a pressure. When blood flow is present, but restricted, the cuff pressure, which is monitored by the pressure sensor, will vary periodically in synchrony with the cyclic expansion and contraction of the brachial artery, i.e., it will oscillate. The values of systolic and diastolic pressure are computed, not actually measured from the raw data, using an algorithm; the computed results are displayed.
Oscillometric monitors may produce inaccurate readings in patients with heart and circulation problems, that include arterial sclerosis, arrhythmia, preeclampsia, pulsus alternans, and pulsus paradoxus.
In practice the different methods do not give identical results; an algorithm and experimentally obtained coefficients are used to adjust the oscillometric results to give readings which match the auscultatory results as well as possible. Some equipment uses computer-aided analysis of the instantaneous arterial pressure waveform to determine the systolic, mean, and diastolic points. Since many oscillometric devices have not been validated, caution must be given as most are not suitable in clinical and acute care settings.
The term NIBP, for Non-Invasive Blood Pressure, is often used to describe oscillometric monitoring equipment.
White-coat hypertension
For some patients, BP measurements taken in a doctor's office may not correctly characterize their typical BP.[9] In up to 25% of patients, the office measurement is higher than their typical BP. This type of error is called white-coat hypertension (WCH) and can result from anxiety related to an examination by a health care professional.[10] The misdiagnosis of hypertension for these patients can result in needless and possibly harmful medication. WCH can be reduced (but not eliminated) with automated BP measurements over 15 to 20 minutes in a quiet part of the office or clinic.[11]
Debate continues regarding the significance of this effect.[citation needed] Some reactive patients will also react to many other stimuli throughout their daily lives, and require treatment. In some cases a lower BP reading occurs at the doctor's office.[12]
Home monitoring
Ambulatory blood pressure devices that take readings every half hour throughout the day and night have been used for identifying and mitigating measurement problems like white-coat hypertension. Except for periods during sleep, home monitoring could be used for these purposes instead of ambulatory blood pressure monitoring.[13] Home monitoring may also be used to improve hypertension management and to monitor the effects of lifestyle changes and medication related to BP.[14] Compared to ambulatory blood pressure measurements, home monitoring has been found to be an effective and lower cost alternative.[13][15][16]
Aside from the white coat effect, BP readings outside of a clinical setting are usually slightly lower in the majority of people. The studies that looked into the risks from hypertension and the benefits of lowering BP in affected patients were based on readings in a clinical environment.
When measuring BP, an accurate reading requires that one not drink coffee, smoke cigarettes, or engage in strenuous exercise for 30 minutes before taking the reading. A full bladder may have a small effect on BP readings, so if the urge to urinate exists, one should do so before the reading. For 5 minutes before the reading, one should sit upright in a chair with one's feet flat on the floor and with limbs uncrossed. The BP cuff should always be against bare skin, as readings taken over a shirt sleeve are less accurate. During the reading, the arm that is used should be relaxed and kept at heart level, for example by resting it on a table.[17]
Since BP varies throughout the day, measurements intended to monitor changes over longer time frames should be taken at the same time of day to ensure that the readings are comparable. Suitable times are:
- immediately after awakening (before washing/dressing and taking breakfast/drink), while the body is still resting,
- immediately after finishing work.
Automatic self-contained BP monitors are available at reasonable prices, some of which are capable of Korotkoff's measurement in addition to oscillometric methods, enabling irregular heartbeat patients to accurately measure their blood pressure at home.
Invasive measurement
Arterial blood pressure (BP) is most accurately measured invasively through an arterial line. Invasive arterial pressure measurement with intravascular cannulae involves direct measurement of arterial pressure by placing a cannula needle in an artery (usually radial, femoral, dorsalis pedis or brachial). This procedure can be done by any licensed doctor or a Respiratory Therapist.
The cannula must be connected to a sterile, fluid-filled system, which is connected to an electronic pressure transducer. The advantage of this system is that pressure is constantly monitored beat-by-beat, and a waveform (a graph of pressure against time) can be displayed. This invasive technique is regularly employed in human and veterinary intensive care medicine, anesthesiology, and for research purposes.
Cannulation for invasive vascular pressure monitoring is infrequently associated with complications such as thrombosis, infection, and bleeding. Patients with invasive arterial monitoring require very close supervision, as there is a danger of severe bleeding if the line becomes disconnected. It is generally reserved for patients where rapid variations in arterial pressure are anticipated.
Invasive vascular pressure monitors are pressure monitoring systems designed to acquire pressure information for display and processing. There are a variety of invasive vascular pressure monitors for trauma, critical care, and operating room applications. These include single pressure, dual pressure, and multi-parameter (i.e. pressure / temperature). The monitors can be used for measurement and follow-up of arterial, central venous, pulmonary arterial, left atrial, right atrial, femoral arterial, umbilical venous, umbilical arterial, and intracranial pressures.
Vascular pressure parameters are derived in the monitor's microcomputer system. Usually, systolic, diastolic, and mean pressures are displayed simultaneously for pulsatile waveforms (i.e. arterial and pulmonary arterial). Some monitors also calculate and display CPP (cerebral perfusion pressure). Normally, a zero key on the front of the monitor makes pressure zeroing extremely fast and easy. Alarm limits may be set to assist the medical professional responsible for observing the patient. High and low alarms may be set on displayed temperature parameters.
Classification
The following classification of blood pressure applies to adults aged 18 and older. It is based on the average of seated BP readings that were properly measured during 2 or more office visits.[14][18]
| Category | systolic, mmHg | diastolic, mmHg |
|---|---|---|
Normal values
While average values for arterial pressure could be computed for any given population, there is often a large variation from person to person; arterial pressure also varies in individuals from moment to moment. Additionally, the average of any given population may have a questionable correlation with its general health, thus the relevance of such average values is equally questionable. However, in a study of 100 subjects with no known history of hypertension, an average blood pressure of 112/64 mmHg was found,[19] which is in the normal range.
Various factors influence a person's average BP and variations. Factors such as age and gender[20] influence average values. In children, the normal ranges are lower than for adults and depend on height.[21] As adults age, systolic pressure tends to rise and diastolic tends to fall.[22] In the elderly, BP tends to be above the normal adult range,[23] largely because of reduced flexibility of the arteries. Also, an individual's BP varies with exercise, emotional reactions, sleep, digestion and time of day.
Differences between left and right arm BP measurements tend to be random and average to nearly zero if enough measurements are taken. However, in a small percentage of cases there is a consistently present difference greater than 10 mmHg which may need further investigation, e.g. for obstructive arterial disease.[24][25]
The risk of cardiovascular disease increases progressively above 115/75 mmHg.[26] In the past, hypertension was only diagnosed if secondary signs of high arterial pressure were present, along with a prolonged high systolic pressure reading over several visits. In the UK, patients’ readings are considered normal up to 140/90 mmHg.[27]
Clinical trials demonstrate that people who maintain arterial pressures at the low end of these pressure ranges have much better long term cardiovascular health. The principal medical debate concerns the aggressiveness and relative value of methods used to lower pressures into this range for those who do not maintain such pressure on their own. Elevations, more commonly seen in older people, though often considered normal, are associated with increased morbidity and mortality.
Physiology
The physics of the circulatory system is very complex. That said, there are many physical factors that influence arterial pressure. Each of these may in turn be influenced by physiological factors, such as diet, exercise, disease, drugs or alcohol, stress, obesity, and so-forth.
Some physical factors are:
- Rate of pumping. In the circulatory system, this rate is called heart rate, the rate at which blood (the fluid) is pumped by the heart. The volume of blood flow from the heart is called the cardiac output which is the heart rate (the rate of contraction) multiplied by the stroke volume (the amount of blood pumped out from the heart with each contraction). The higher the heart rate, the higher the arterial pressure, assuming no reduction in stroke volume.
- Volume of fluid or blood volume, the amount of blood that is present in the body. The more blood present in the body, the higher the rate of blood return to the heart and the resulting cardiac output. There is some relationship between dietary salt intake and increased blood volume, potentially resulting in higher arterial pressure, though this varies with the individual and is highly dependent on autonomic nervous system response and the renin-angiotensin system.
- Resistance. In the circulatory system, this is the resistance of the blood vessels. The higher the resistance, the higher the arterial pressure upstream from the resistance to blood flow. Resistance is related to vessel radius (the larger the radius, the lower the resistance), vessel length (the longer the vessel, the higher the resistance), as well as the smoothness of the blood vessel walls. Smoothness is reduced by the build up of fatty deposits on the arterial walls. Substances called vasoconstrictors can reduce the size of blood vessels, thereby increasing BP. Vasodilators (such as nitroglycerin) increase the size of blood vessels, thereby decreasing arterial pressure. Resistance, and its relation to volumetric flow rate (Q) and pressure difference between the two ends of a vessel are described by Poiseuille's Law.
- Viscosity, or thickness of the fluid. If the blood gets thicker, the result is an increase in arterial pressure. Certain medical conditions can change the viscosity of the blood. For instance, low red blood cell concentration, anemia, reduces viscosity, whereas increased red blood cell concentration increases viscosity. Viscosity also increases with blood sugar concentration—visualize pumping syrup. It had been thought that aspirin and related "blood thinner" drugs decreased the viscosity of blood, but studies found[28] that they act by reducing the tendency of the blood to clot instead.
In practice, each individual's autonomic nervous system responds to and regulates all these interacting factors so that, although the above issues are important, the actual arterial pressure response of a given individual varies widely because of both split-second and slow-moving responses of the nervous system and end organs. These responses are very effective in changing the variables and resulting BP from moment to moment.
Mean arterial pressure
The mean arterial pressure (MAP) is the average over a cardiac cycle and is determined by the cardiac output (CO), systemic vascular resistance (SVR), and central venous pressure (CVP),[29]
MAP can be approximately determined from measurements of the systolic pressure and the diastolic pressure while there is a normal resting heart rate,[29]
Pulse pressure
The up and down fluctuation of the arterial pressure results from the pulsatile nature of the cardiac output, i.e. the heartbeat. The pulse pressure is determined by the interaction of the stroke volume of the heart, compliance (ability to expand) of the aorta, and the resistance to flow in the arterial tree. By expanding under pressure, the aorta absorbs some of the force of the blood surge from the heart during a heartbeat. In this way the pulse pressure is reduced from what it would be if the aorta wasn't compliant.[30]
The pulse pressure can be simply calculated from the difference of the measured systolic and diastolic pressures,[30]
Vascular resistance
The larger arteries, including all large enough to see without magnification, are low resistance conduits (assuming no advanced atherosclerotic changes) with high flow rates that generate only small drops in pressure.
Vascular pressure wave
Modern physiology developed the concept of the vascular pressure wave (VPW). This wave is created by the heart during the systole and originates in the ascending aorta. Much faster than the stream of blood itself, it is then transported through the vessel walls to the peripheral arteries. There the pressure wave can be palpated as the peripheral pulse. As the wave is reflected at the peripheral veins it runs back in a centripetal fashion. Where the crests of the reflected and the original wave meet, the pressure inside the vessel is higher than the true pressure in the aorta. This concept explains why the arterial pressure inside the peripheral arteries of the legs and arms is higher than the arterial pressure in the aorta,[31][32][33] and in turn for the higher pressures seen at the ankle compared to the arm with normal ankle brachial pressure index values.
Regulation
The endogenous regulation of arterial pressure is not completely understood. Currently, three mechanisms of regulating arterial pressure have been well-characterized:
- Baroreceptor reflex: Baroreceptors detect changes in arterial pressure and send signals ultimately to the medulla of the brain stem. The medulla, by way of the autonomic nervous system, adjusts the mean arterial pressure by altering both the force and speed of the heart's contractions, as well as the total peripheral resistance. The most important arterial baroreceptors are located in the left and right carotid sinuses and in the aortic arch.[34]
- Renin-angiotensin system (RAS): This system is generally known for its long-term adjustment of arterial pressure. This system allows the kidney to compensate for loss in blood volume or drops in arterial pressure by activating an endogenous vasoconstrictor known as angiotensin II.
- Aldosterone release: This steroid hormone is released from the adrenal cortex in response to angiotensin II or high serum potassium levels. Aldosterone stimulates sodium retention and potassium excretion by the kidneys. Since sodium is the main ion that determines the amount of fluid in the blood vessels by osmosis, aldosterone will increase fluid retention, and indirectly, arterial pressure.
These different mechanisms are not necessarily independent of each other, as indicated by the link between the RAS and aldosterone release. Currently, the RAS system is targeted pharmacologically by ACE inhibitors and angiotensin II receptor antagonists. The aldosterone system is directly targeted by spironolactone, an aldosterone antagonist. The fluid retention may be targeted by diuretics; the antihypertensive effect of diuretics is due to its effect on blood volume. Generally, the baroreceptor reflex is not targeted in hypertension because if blocked, individuals may suffer from orthostatic hypotension and fainting.
Pathophysiology
High arterial pressure

Arterial hypertension can be an indicator of other problems and may have long-term adverse effects. Sometimes it can be an acute problem, for example hypertensive emergency.
All levels of arterial pressure put mechanical stress on the arterial walls. Higher pressures increase heart workload and progression of unhealthy tissue growth (atheroma) that develops within the walls of arteries. The higher the pressure, the more stress that is present and the more atheroma tend to progress and the heart muscle tends to thicken, enlarge and become weaker over time.
Persistent hypertension is one of the risk factors for strokes, heart attacks, heart failure and arterial aneurysms, and is the leading cause of chronic renal failure. Even moderate elevation of arterial pressure leads to shortened life expectancy. At severely high pressures, mean arterial pressures 50% or more above average, a person can expect to live no more than a few years unless appropriately treated.[35]
In the past, most attention was paid to diastolic pressure; but nowadays it is recognised that both high systolic pressure and high pulse pressure (the numerical difference between systolic and diastolic pressures) are also risk factors. In some cases, it appears that a decrease in excessive diastolic pressure can actually increase risk, due probably to the increased difference between systolic and diastolic pressures (see the article on pulse pressure).
Low arterial pressure
Blood pressure that is too low is known as hypotension. The similarity in pronunciation with hypertension can cause confusion. Hypotension is a medical concern only if it causes signs or symptoms, such as dizziness, fainting, or in extreme cases, shock.[18]
When arterial pressure and blood flow decrease beyond a certain point, the perfusion of the brain becomes critically decreased (i.e., the blood supply is not sufficient), causing lightheadedness, dizziness, weakness or fainting.
Sometimes the arterial pressure drops significantly when a patient stands up from sitting. This is known as orthostatic hypotension (postural hypotension); gravity reduces the rate of blood return from the body veins below the heart back to the heart, thus reducing stroke volume and cardiac output.
When people are healthy, the veins below their heart quickly constrict and the heart rate increases to minimize and compensate for the gravity effect. This is carried out involuntarily by the autonomic nervous system. The system usually requires a few seconds to fully adjust and if the compensations are too slow or inadequate, the individual will suffer reduced blood flow to the brain, dizziness and potential blackout. Increases in G-loading, such as routinely experienced by aerobatic or combat pilots 'pulling Gs', greatly increases this effect. Repositioning the body perpendicular to gravity largely eliminates the problem.
Other causes of low arterial pressure include:
- Sepsis
- Hemorrhage - blood loss
- Toxins including toxic doses of BP medicine
- Hormonal abnormalities, such as Addison's disease
Shock is a complex condition which leads to critically decreased perfusion. The usual mechanisms are loss of blood volume, pooling of blood within the veins reducing adequate return to the heart and/or low effective heart pumping. Low arterial pressure, especially low pulse pressure, is a sign of shock and contributes to and reflects decreased perfusion.
If there is a significant difference in the pressure from one arm to the other, that may indicate a narrowing (for example, due to aortic coarctation, aortic dissection, thrombosis or embolism) of an artery.
Other sites
Blood pressure generally refers to the arterial pressure in the systemic circulation. However, measurement of pressures in the venous system and the pulmonary vessels plays an important role in intensive care medicine but requires an invasive central venous catheter.
Venous pressure
Venous pressure is the vascular pressure in a vein or in the atria of the heart. It is much less than arterial pressure, with common values of 5 mmHg in the right atrium and 8 mmHg in the left atrium.
Pulmonary pressure
Normally, the pressure in the pulmonary artery is about 15 mmHg at rest.[36]
Increased BP in the capillaries of the lung cause pulmonary hypertension, with interstitial edema if the pressure increases to above 20 mmHg, and to frank pulmonary edema at pressures above 25 mmHg.[37]
Fetal blood pressure
In pregnancy, it is the fetal heart and not the mother's heart that builds up the fetal BP to drive its blood through the fetal circulation.
The BP in the fetal aorta is approximately 30 mmHg at 20 weeks of gestation, and increases to ca 45 mmHg at 40 weeks of gestation.[38]
The average BP for full-term infants:
Systolic 65–95 mm Hg
Diastolic 30–60 mm Hg
[39]
See also
References
- Pickering, TG; Hall, JE; Appel, LJ; et al. (2005). "Recommendations for blood pressure measurement in humans and experimental animals: Part 1: blood pressure measurement in humans: a statement for professionals from the Subcommittee of Professional and Public Education of the American Heart Association Council on High Blood Pressure Research". Hypertension. 45 (5): 142–61. doi:10.1161/01.HYP.0000150859.47929.8e. PMID 15611362. Retrieved 2009-10-01.
{{cite journal}}: Invalid|ref=harv(help)CS1 maint: multiple names: authors list (link)
Footnotes
- ^ Klabunde, Richard (2005). Cardiovascular Physiology Concepts. Lippincott Williams & Wilkins. pp. 93–4. ISBN 978-0781750301.
{{cite book}}: Cite has empty unknown parameter:|coauthors=(help) - ^ Booth, J (1977). "A short history of blood pressure measurement". Proceedings of the Royal Society of Medicine. 70 (11): 793–9. PMID 341169. Retrieved 2009-10-06.
{{cite journal}}: Cite has empty unknown parameter:|coauthors=(help) - ^ Deakin CD, Low JL (2000). "Accuracy of the advanced trauma life support guidelines for predicting systolic blood pressure using carotid, femoral, and radial pulses: observational study". BMJ. 321 (7262): 673–4. doi:10.1136/bmj.321.7262.673. PMC 27481. PMID 10987771.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Interpretation - Blood Pressure - Vitals, "University of Florida"Template:Accessdate
- ^ G8 Secondary Survey, "Manitoba"Template:Accessdate
- ^ (Pickering et al. 2005, p. 146) See Blood Pressure Measurement Methods.
- ^ (Pickering et al. 2005, p. 147) See The Oscillometric Technique.
- ^ Laurent, P (2003-09-28). "Blood Pressure & Hypertension". Retrieved 2009-10-05.
- ^ Elliot, Victoria Stagg (2007-06-11). "Blood pressure readings often unreliable". American Medical News. American Medical Association. Retrieved 2008-08-16.
{{cite news}}: Cite has empty unknown parameter:|coauthors=(help) - ^ Jhalani, Juhee (2005). "Anxiety and outcome expectations predict the white-coat effect". Blood Pressure Monitoring. 10 (6): 317–9. PMID 16496447. Retrieved 2009-10-03.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ (Pickering et al. 2005, p. 145) See White Coat Hypertension or Isolated Office Hypertension.
- ^ (Pickering et al. 2005, p. 146) See Masked Hypertension or Isolated Ambulatory Hypertension.
- ^ a b Mancia G, De Backer G, Dominiczak A; et al. (2007). "2007 Guidelines for the management of arterial hypertension: The Task Force for the Management of Arterial Hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC)". Eur Heart J. 28 (12): 1462–536. doi:10.1093/eurheartj/ehm236. PMID 17562668.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b Chobanian AV, Bakris GL, Black HR; et al. (2003). "Seventh report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure". Hypertension. 42 (6): 1206–52. doi:10.1161/01.HYP.0000107251.49515.c2. PMID 14656957.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Niiranen, TJ (2006). "A comparison of home measurement and ambulatory monitoring of blood pressure in the adjustment of antihypertensive treatment". Am J Hypertens. 19 (5): 468–74. doi:10.1016/j.amjhyper.2005.10.017. PMID 16647616.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Shimbo, Daichi (2007). "Relative utility of home, ambulatory, and office blood pressures in the prediction of end-organ damage" ([dead link]). Am J Hypertens. 20 (5): 476–82. doi:10.1016/j.amjhyper.2006.12.011. PMID 17485006.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ National Heart, Lung and Blood Institute. "Tips for having your blood pressure taken".
{{cite journal}}: Cite journal requires|journal=(help) - ^ a b "Diseases and Conditions Index - Hypotension". National Heart Lung and Blood Institute. 2008. Retrieved 2008-09-16.
{{cite web}}: Unknown parameter|month=ignored (help) - ^ Pesola GR, Pesola HR, Nelson MJ, Westfal RE (2001). "The normal difference in bilateral indirect BP recordings in normotensive individuals". Am J Emerg Med. 19 (1): 43–5. doi:10.1053/ajem.2001.20021. PMID 11146017.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Reckelhoff, Jane F. (2001 May). "Gender Differences in the Regulation of Blood Pressure". Hypertension. 37 (5): 1199–208. PMID 11358929. PMID 11358929.
{{cite journal}}: Check date values in:|date=(help); Cite has empty unknown parameter:|coauthors=(help); Unknown parameter|day=ignored (help); Unknown parameter|month=ignored (help) - ^ National Heart, Lung and Blood Institute. "Blood Pressure Tables for Children and Adolescents".
{{cite journal}}: Cite journal requires|journal=(help) (Note that the median BP is given by the 50th percentile and hypertension is defined by the 95th percentile for a given age, height, and gender.) - ^ (Pickering et al. 2005, p. 145) See Isolated Systolic Hypertension.
- ^ "...more than half of all Americans aged 65 or older have hypertension." (Pickering et al. 2005, p. 144)
- ^ Eguchi K, Yacoub M, Jhalani J, Gerin W, Schwartz JE, Pickering TG (2007). "Consistency of blood pressure differences between the left and right arms". Arch Intern Med. 167 (4): 388–93. doi:10.1001/archinte.167.4.388. PMID 17325301.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Agarwal R, Bunaye Z, Bekele DM (2008). "Prognostic significance of between-arm blood pressure differences". Hypertension. 51 (3): 657–62. doi:10.1161/HYPERTENSIONAHA.107.104943. PMID 18212263.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Appel LJ, Brands MW, Daniels SR, Karanja N, Elmer PJ, Sacks FM (2006). "Dietary approaches to prevent and treat hypertension: a scientific statement from the American Heart Association". Hypertension. 47 (2): 296–308. doi:10.1161/01.HYP.0000202568.01167.B6. PMID 16434724.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ "Hypertension: management of hypertension in adults in primary care" (PDF), NICE Clinical Guideline 34, London, England: National Institute for Health and Clinical Excellence (NICE), June 2006, retrieved 2008-09-15
{{citation}}: Cite has empty unknown parameters:|coeditors=and|coauthors=(help) - ^ Rosenson RS, Wolff D, Green D, Boss AH, Kensey KR (2004). "Aspirin. Aspirin does not alter native blood viscosity". J. Thromb. Haemost. 2 (2): 340–1. PMID 14996003.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b Klabunde, RE (2007). "Cardiovascular Physiology Concepts - Mean Arterial Pressure". Retrieved 2008-09-29. Archived version 2009-10-03
- ^ a b Klabunde, RE (2007). "Cardiovascular Physiology Concepts - Pulse Pressure". Retrieved 2008-10-02. Archived version 2009-10-03
- ^ Messerli FH, Williams B, Ritz E (2007). "Essential hypertension". Lancet. 370 (9587): 591–603. doi:10.1016/S0140-6736(07)61299-9. PMID 17707755.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ O'Rourke M (1995). "Mechanical principles in arterial disease". Hypertension. 26 (1): 2–9. PMID 7607724.
{{cite journal}}: Unknown parameter|day=ignored (help); Unknown parameter|month=ignored (help) - ^ Mitchell GF (2006). "Triangulating the peaks of arterial pressure". Hypertension. 48 (4): 543–5. doi:10.1161/01.HYP.0000238325.41764.41. PMID 16940226.
- ^ Klabunde, RE (2007). "Cardiovascular Physiology Concepts - Arterial Baroreceptors". Retrieved 2008-09-09. Archived version 2009-10-03
- ^ Textbook of Medical Physiology, 7th Ed., Guyton & Hall, Elsevier-Saunders, ISBN 0-7216-0240-1, page 220.
- ^ What Is Pulmonary Hypertension? From Diseases and Conditions Index (DCI). National Heart, Lung, and Blood Institute. Last updated September 2008. Retrieved on 6 April, 2009.
- ^ Chapter 41, page 210 in: Cardiology secrets By Olivia Vynn Adair Edition: 2, illustrated Published by Elsevier Health Sciences, 2001 ISBN 1560534206, 9781560534204
- ^ Struijk PC, Mathews VJ, Loupas T; et al. (2008). "Blood pressure estimation in the human fetal descending aorta". Ultrasound Obstet Gynecol. 32 (5): 673–81. doi:10.1002/uog.6137. PMID 18816497.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Sharon, S. M. & Emily, S. M.(2006). Fundations of Maternal-Newborn Nursing. (4th ed p.476). Philadelphia:Elsevier.
External links
- How Do I Keep My Heart Healthy? Articles providing tips on how one can have a stronger, healthier heart.
- High Blood Pressure, The Institute for Good Medicine at the Pennsylvania Medical Society
- Blood Pressure Association (UK)
- British Hypertension Society: list of validated blood pressure monitors
- Blood pressure monitoring
- Pulmonary Hypertension Cleveland Clinic
- Blood Pressure Calculator for Diagnosis of High blood pressure in Children and Adolescents





