Multiple sclerosis: Difference between revisions
Lofty abyss (talk | contribs) m Reverted edits by 212.219.81.181 to last revision by Adolphus79 (HG) |
|||
| Line 1,349: | Line 1,349: | ||
* [http://clinicaltrials.gov/search/term=Multiple+Sclerosis NIH listing of clinical trials related to MS] |
* [http://clinicaltrials.gov/search/term=Multiple+Sclerosis NIH listing of clinical trials related to MS] |
||
* [http://www.cochrane.org/reviews/en/topics/79.html Abstract index] of the [[Cochrane Library]] |
* [http://www.cochrane.org/reviews/en/topics/79.html Abstract index] of the [[Cochrane Library]] |
||
* [http://www.allsup.com/About-SSDI/SSDI-Guidelines-by-Disability/Multiple-Sclerosis-(MS).aspx SSDI Guidelines for Multiple Sclerosis] |
|||
{{Multiple sclerosis}} |
{{Multiple sclerosis}} |
||
Revision as of 17:21, 2 March 2009
| Multiple sclerosis | |
|---|---|
| Specialty | Neurology |
| Frequency | 0.032% (world) |
Multiple sclerosis (abbreviated MS, also known as disseminated sclerosis or encephalomyelitis disseminata) is an autoimmune condition in which the immune system attacks the central nervous system, leading to demyelination.[1] Disease onset usually occurs in young adults, and it is more common in females.[2] It has a prevalence that ranges between 2 and 150 per 100,000.[3] MS was first described in 1868 by Jean-Martin Charcot.[4]
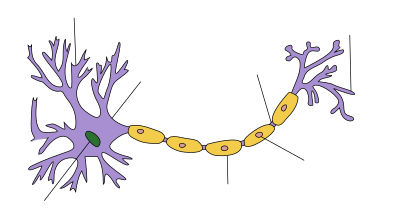
MS affects the ability of nerve cells in the brain and spinal cord to communicate with each other. Nerve cells communicate by sending electrical signals called action potentials down long fibers called axons, which are wrapped in an insulating substance called myelin. In MS, the body's own immune system attacks and damages the myelin. When myelin is lost, the axons can no longer effectively conduct signals.[1] The name multiple sclerosis refers to scars (scleroses – better known as plaques or lesions) in the white matter of the brain and spinal cord, which is mainly composed of myelin.[4] Although much is known about the mechanisms involved in the disease process, the cause remains unknown. Theories include genetics or infections. Different environmental risk factors have also been found.[5][1]
Almost any neurological symptom can appear with the disease, and often progresses to physical and cognitive disability.[1] MS takes several forms, with new symptoms occurring either in discrete attacks (relapsing forms) or slowly accumulating over time (progressive forms).[6] Between attacks, symptoms may go away completely, but permanent neurological problems often occur, especially as the disease advances.[6]
There is no known cure for MS. Treatments attempt to return function after an attack, prevent new attacks, and prevent disability.[1] MS medications can have adverse effects or be poorly tolerated, and many patients pursue alternative treatments, despite the lack of supporting scientific study. The prognosis is difficult to predict; it depends on the subtype of the disease, the individual patient's disease characteristics, the initial symptoms and the degree of disability the person experiences as time advances.[7] Life expectancy of patients is nearly the same as that of the unaffected population.[7]
Signs and symptoms
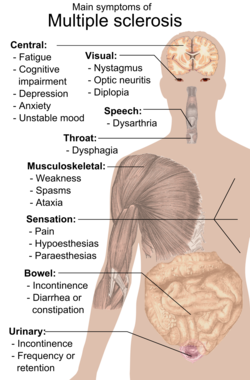
Symptoms of MS usually appear in episodic acute periods of worsening (relapses, exacerbations, bouts or attacks), in a gradually-progressive deterioration of neurologic function, or in a combination of both.[6]
The most common presentation of MS is the clinically isolated syndrome (CIS). In CIS, a patient has an attack suggestive of demyelination, but does not fulfill the criteria for multiple sclerosis.[8] Only 30 to 70% of persons experiencing CIS later develop MS.[8] The disease usually presents with sensorial (46% of cases), visual (33%), cerebellar (30%) and motor (26%) symptoms.[9] Many rare initial symptoms have also been reported, including aphasia, psychosis and epilepsy.[10][11][12] Patients first seeking medical attention commonly present with multiple symptoms.[9] The initial signs and symptoms of MS are often transient, mild, and self-limited. These signs and symptoms often do not prompt a person to seek medical attention and are sometimes identified only retrospectively once the diagnosis of MS has been made. Cases of MS are sometimes incidentally identified during neurological examinations performed for other causes. Such cases are referred to as subclinical MS.[13][14]
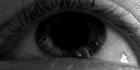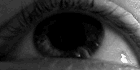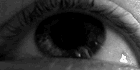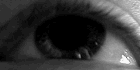
The person with MS can suffer almost any neurological symptom or sign, including changes in sensation (hypoesthesias and paraesthesias), muscle weakness, muscle spasms, or difficulty in moving;[15] difficulties with coordination and balance (ataxia);[15] problems in speech (dysarthria) or swallowing (dysphagia),[16] visual problems (nystagmus, optic neuritis, or diplopia),[17] fatigue, acute or chronic pain,[18][19] and bladder and bowel difficulties.[19][20] Cognitive impairment of varying degrees and emotional symptoms of depression or unstable mood are also common.[21][22] The main clinical measure of disability progression and symptom severity is the Expanded Disability Status Scale or EDSS.[23]
Multiple sclerosis relapses are often unpredictable, occurring without warning and without obvious inciting factors. Some attacks, however, are preceded by common triggers. Relapses occur more frequently during spring and summer.[24] Infections such as the common cold, influenza, or gastroenteritis increase the risk of relapse.[25][26] Stress may also trigger an attack.[27][28][29] Pregnancy may affect susceptibility to relapse, offering protection during the last trimester, for instance. During the first few months after delivery, however, the risk of relapse is increased. Overall, pregnancy does not seem to influence long-term disability.[30] Many potential triggers have been examined and found not to influence MS relapse rates. There is no evidence that vaccination for influenza, hepatitis B, varicella, tetanus, or tuberculosis increases risk of relapse.[31] Physical trauma does not trigger relapses.[32][33] Exposure to higher than usual ambient temperatures can exacerbate extant symptoms, an effect known as Uhthoff's phenomenon.[34] Uhthoff's phenomenon is not, however, an established relapse trigger.[24]
Disease subtypes

Several subtypes, or patterns of progression, have been described. Subtypes use the past course of the disease in an attempt to predict the future course. They are important not only for prognosis but also for therapeutic decisions. In 1996 the United States National Multiple Sclerosis Society standardized four subtype definitions: relapsing remitting, secondary progressive, primary progressive and progressive relapsing.[6]
The relapsing-remitting subtype is characterized by unpredictable relapses followed by periods of months to years of relative quiet (remission) with no new signs of disease activity. Deficits suffered during attacks may either resolve or leave sequelae. This describes the initial course of 85–90% of individuals with MS.[6] When deficits always resolve between attacks, this is sometimes referred to as benign MS.[35]
Secondary progressive MS describes those with initial relapsing-remitting MS, who then begin to have progressive neurologic decline between acute attacks without any definite periods of remission.[6] Occasional relapses and minor remissions may appear.[6] The median time between disease onset and conversion from relapsing-remitting to secondary progressive MS is 19 years.[36]
The primary progressive subtype describes the approximately 10–15% of individuals who never have remission after their initial MS symptoms.[37] It is characterized by progression of disability from onset, with no, or only occasional and minor, remissions and improvements.[6] The age of onset for the primary progressive subtype is later than other subtypes.[37]
Progressive relapsing MS describes those individuals who, from onset, have a steady neurologic decline but also suffer clear superimposed attacks. This is the least common of all subtypes.[6]
Cases with non-standard behavior have also been described. Sometimes referred to as borderline forms of multiple sclerosis,[38] these include Devic's disease, Balo concentric sclerosis, Schilder's diffuse sclerosis and Marburg multiple sclerosis.[39][40] There is debate whether these are atypical variants of MS or different diseases.[41]
Diagnosis
Multiple sclerosis can be difficult to diagnose since its signs and symptoms may be similar to many other medical problems.[42] Medical organizations have created diagnostic criteria to ease and standardize the diagnostic process for practicing physicians. Historically, the Schumacher and Poser criteria were both popular.[43] Currently, the McDonald criteria focus on a demonstration with clinical, laboratory and radiologic data of the dissemination of MS lesions in time and space. A diagnosis cannot be made until other possible conditions have been ruled out and there is evidence of demyelinating events separated anatomically and in time.[44]
Clinical data alone may be sufficient for a diagnosis of MS if an individual has suffered separate episodes of neurologic symptoms characteristic of MS.[44] Since some people seek medical attention after only one attack, other testing may hasten and ease the diagnosis. The most commonly used diagnostic tools are neuroimaging, analysis of cerebrospinal fluid and evoked potentials. Magnetic resonance imaging of the brain and spine shows areas of demyelination (lesions or plaques). Gadolinium can be administered intravenously as a contrast to highlight active plaques and, by elimination, demonstrate the existence of historical lesions not associated with symptoms at the moment of the evaluation.[44][45] Testing of cerebrospinal fluid obtained from a lumbar puncture can provide evidence of chronic inflammation of the central nervous system. The cerebrospinal fluid is tested for oligoclonal bands, which are an inflammation marker found in 75–85% of people with MS.[44][46] The nervous system of a person with MS often responds less actively to stimulation of the optic nerve and sensory nerves due to demyelination of such pathways. These brain responses can be examined using visual and sensory evoked potentials.[47]
Pathophysiology

MS as an autoimmunological disease
MS is currently believed to be an immune-mediated disorder with an initial trigger, which may have a viral etiology,[1] although this concept has been debated for years and some still oppose it. Damage is believed to be caused by the patient's own immune system. The immune system attacks the nervous system, possibly as a result of exposure to a molecule with a similar structure to one of its own.[1]
Lesions
The name multiple sclerosis refers to the scars (scleroses – better known as plaques or lesions) that form in the nervous system. MS lesions most commonly involve white matter areas close to the ventricles of the cerebellum, brain stem, basal ganglia and spinal cord; and the optic nerve. The function of white matter cells is to carry signals between grey matter areas, where the processing is done, and the rest of the body. The peripheral nervous system is rarely involved.[1]
More specifically, MS destroys oligodendrocytes, the cells responsible for creating and maintaining a fatty layer—known as the myelin sheath—which helps the neurons carry electrical signals.[1] MS results in a thinning or complete loss of myelin and, as the disease advances, the cutting (transection) of the neuron's extensions or axons.[48] When the myelin is lost, a neuron can no longer effectively conduct electrical signals.[1] A repair process, called remyelination, takes place in early phases of the disease, but the oligodendrocytes cannot completely rebuild the cell's myelin sheath.[49] Repeated attacks lead to successively fewer effective remyelinations, until a scar-like plaque is built up around the damaged axons.[49] Four different lesion patterns have been described.[50]
Inflammation
Apart from demyelination, the other pathologic hallmark of the disease is inflammation. According to a strictly immunological explanation of MS, the inflammatory process is caused by T cells, a kind of lymphocyte. Lymphocytes are cells that play an important role in the body's defenses.[1] In MS, T cells gain entry into the brain via the blood–brain barrier, a capillary system that should prevent entrance of T cells into the nervous system.[1] The blood–brain barrier is normally not permeable to these types of cells, unless triggered by infection or a virus, which decreases the integrity of the tight junctions forming the barrier.[1] When the blood–brain barrier regains its integrity, usually after infection or virus has cleared, the T cells are trapped inside the brain.[1] The T cells recognize myelin as foreign and attack it as if it were an invading virus. This triggers inflammatory processes, stimulating other immune cells and soluble factors like cytokines and antibodies. Leaks form in the blood–brain barrier, which in turn cause a number of other damaging effects such as swelling, activation of macrophages, and more activation of cytokines and other destructive proteins.[1]
Epidemiology
Two main measures are used in epidemiological studies: incidence and prevalence. Incidence is the number of new cases per unit of person–time at risk (usually number of new cases per thousand person–years); while prevalence is the total number of cases of the disease in the population at a given time. Prevalence is known to depend not only on incidence, but also on survival rate and migrations of affected people. MS has a prevalence that ranges between 2 and 150 per 100,000 depending on the country or specific population.[3] Studies on populational and geographical patterns of epidemiological measures have been very common in MS,[51] and have led to the proposal of different etiological (causal) theories.[51][52][5][53]
MS usually appears in adults in their thirties,[2] but it can also appear in children,[54] and the primary progressive subtype is more common in people in their fifties.[37] As with many autoimmune disorders, the disease is more common in women, and the trend may be increasing.[51][55] In children, the sex ratio may reach three females for each male.[54] In people over fifty, MS affects males and females almost equally.[37]

There is a north-to-south gradient in the northern hemisphere and a south-to-north gradient in the southern hemisphere, with MS being much less common in people living near the equator.[55] Climate, sunlight and intake of vitamin D have been investigated as possible causes of the disease that could explain this latitude gradient.[53] However, there are important exceptions to the north-south pattern such as incidence and prevalence in the Canary Islands[56] and changes in prevalence rates over time;[57] in general, this trend might be disappearing.[55] This indicates that other factors such as environment or genetics have to be taken into account to explain the origin of MS.[57]
Environmental factors during childhood may play an important role in the development of MS later in life. Several studies of migrants show that if migration occurs before the age of fifteen, the migrant acquires the new region's susceptibility to MS. If migration takes place after age fifteen, the migrant retains the susceptibility of his home country.[52] However, the age–geographical risk for developing multiple sclerosis may span a larger timescale.[58]
Even in regions where MS is common, some ethnic groups are at low risk of developing the disease, including the Samis, Turkmen, Amerindians, Canadian Hutterites, Africans, and New Zealand Maoris.[52] Scotland appears to have one of the highest rates of MS in the world.[59]
Causes
Epidemiological studies of MS have provided hints on possible causes for the disease. Various theories try to combine the known data into plausible explanations, but none has proved definitive. MS likely occurs as a result of some combination of both environmental and genetic factors.
Genetic factors
MS is not considered a hereditary disease. However, a number of genetic variations have been shown to increase the risk of developing the disease.[60]
The risk of acquiring MS is higher in relatives of a person with the disease than in the general population, especially in the case of siblings, parents, and children.[1] In the case of monozygotic twins, concordance occurs only in about 35% of cases, and half-siblings have a lower risk than full siblings, indicating a polygenic origin.[1][61]
Apart from familial studies, specific genes have been linked with MS. Differences in the human leukocyte antigen (HLA) system—a group of genes in chromosome 6 that serves as the major histocompatibility complex in humans—increase the probability of suffering MS.[62] Two other genes have been shown to be linked to MS. These are the IL2RA and the IL7RA, subunits of the receptor for interleukin 2 and interleukin 7 respectively.[63][64] The HLA complex is involved in antigen presentation, which is crucial to the functioning of the immune system, while mutations in the IL2 and IL7 receptor genes were already known to be associated with diabetes and other autoimmune conditions, supporting the notion that MS is an autoimmune disease.[65][62][66] The gene encoding kinesin KIF1B is the first neuronal expressed gene demonstrated to enhance the risk for the disease.[67] Other studies have linked genes in chromosome 5 with the disease.[68]
Infectious cause
Genetic susceptibility can explain some of the geographic and epidemiological variations in MS incidence, like the high appearance of the disease among some families or the risk decline with genetic distance, but does not account for other phenomena, such as the changes in risk that occur with migration at an early age.[5]
An explanation for this epidemiology finding could be that some kind of infection, produced by a widespread microbe rather than a rare pathogen, is the origin of the disease.[5] Different hypotheses have elaborated on the mechanism by which this may occur. The hygiene hypothesis proposes that exposure to several infectious agents early in life is protective against MS. MS would be an autoimmune reaction triggered in susceptible individuals by multiple infective microorganisms, with risk increasing with age at infection.[5][69][70] The prevalence hypothesis proposes that the disease is due to a pathogen more common in regions of high MS prevalence. This pathogen is very common, causing in most individuals an asymptomatic persistent infection. Only in a few cases, and after many years since the original infection, does it bring demyelination.[5][51] The hygiene hypothesis has received more support than the prevalence hypothesis.[5]
Evidence for viruses as a cause includes the presence of oligoclonal bands in the brain and cerebrospinal fluid of most patients, the association of several viruses with human demyelinating encephalomyelitis, and induction of demyelination in animals through viral infection.[71] Human herpesviruses are a candidate group of viruses linked to MS;[72] Varicella zoster virus has been found at high levels in the cerebrospinal fluid of MS patients,[73] but the most reproduced finding is the reduced risk of having the disease in those who have never been infected by the Epstein-Barr virus.[5][74] This goes against the hygiene hypothesis, since the non-infected have probably experienced a more hygienic upbringing.[5] Other agents that have also been related with MS are human endogenous retroviruses and Chlamydia pneumoniae.[75][76][77]
Non-infectious environmental risk factors
MS is more common in people who live farther from the equator. Decreased sunlight exposure has been linked with a higher risk of MS.[52][78][79] Decreased vitamin D production and intake has been the main biological mechanism used to explain the higher risk among those less exposed to sun.[52][53][80]
Severe stress may also be a risk factor although evidence is weak;[52] parents who lost a child unexpectedly were more likely to develop MS than parents who had not.[81] Smoking has also been shown to be an independent risk factor for developing MS.[82][53] Association with occupational exposures and toxins—mainly solvents—has been evaluated, but no clear conclusions have been reached.[52] Vaccinations were also considered as causal factors for the disease; however, most studies show no association between MS and vaccines.[52]
Gout occurs less than would statistically be expected in people with MS, and low levels of uric acid have been found in MS patients as compared to normal individuals. This led to the theory that uric acid, which can protect against oxidative stress from substances such as peroxynitrite, protects against MS, although its exact importance remains unknown.[83][84][85] Several other possible risk factors, such as diet and hormone intake, have been investigated; however, more evidence is needed to confirm or refute their relation with the disease.[53]
Although some of these risk factors, including infection, are partly modifiable, only further research—especially clinical trials—will reveal whether their elimination can help prevent MS.[86]
Treatment
Although there is no known cure for multiple sclerosis, several therapies have proven helpful. The primary aims of therapy are returning function after an attack, preventing new attacks, and preventing disability. As with any medical treatment, medications used in the management of MS have several adverse effects. Alternative treatments are pursued by some patients, despite the shortage of supporting, comparable, replicated scientific study.
Management of acute attacks
During symptomatic attacks, administration of high doses of intravenous corticosteroids, such as methylprednisolone,[87][88] is the routine therapy for acute relapses. The aim of this kind of treatment is to end the attack sooner and leave fewer lasting deficits in the patient. Although generally effective in the short term for relieving symptoms, corticosteroid treatments do not appear to have a significant impact on long-term recovery.[89] Potential side effects include osteoporosis[90] and impaired memory, the latter being reversible.[91]
Disease-modifying treatments
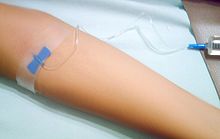
The earliest clinical presentation of relapsing-remitting MS (RRMS) is the clinically isolated syndrome (CIS). Several studies have shown that treatment with interferons during an initial attack can decrease the chance that a patient will develop clinical MS.[92][93][94]
As of 2007, six disease-modifying treatments have been approved by regulatory agencies of different countries for RRMS. Three are interferons: two formulations of interferon beta-1a (trade names Avonex and Rebif) and one of interferon beta-1b (U.S. trade name Betaseron, in Europe and Japan Betaferon). A fourth medication is glatiramer acetate (Copaxone). The fifth medication, mitoxantrone, is an immunosuppressant also used in cancer chemotherapy, approved only in the USA and largely for secondary progressive MS. The sixth is natalizumab (marketed as Tysabri). All six medications are modestly effective at decreasing the number of attacks and slowing progression to disability, although their efficacy rates differ, and studies of their long-term effects are still lacking.[95][96][97][98] Comparisons between immunomodulators (all but mitoxantrone) show that the most effective is natalizumab, both in terms of relapse rate reduction and halting disability progression;[99] it has also been shown to reduce the severity of MS.[100] Mitoxantrone may be the most effective of them all;[101] however, it is generally not considered as a long-term therapy, as its use is limited by severe cardiotoxicity.[102]
The interferons and glatiramer acetate are delivered by frequent injections, varying from once-per-day for glatiramer acetate to once-per-week (but intra-muscular) for Avonex. Natalizumab and mitoxantrone are given by IV infusion at monthly intervals.
Treatment of progressive MS is more difficult than relapsing-remitting MS. Mitoxantrone has shown positive effects in patients with secondary progressive and progressive relapsing courses. It is moderately effective in reducing the progression of the disease and the frequency of relapses in patients in short-term follow-up.[98] No treatment has been proven to modify the course of primary progressive MS.[103]
As with any medical treatment, these treatments have several adverse effects. One of the most common is irritation at the injection site for glatiramer acetate and the interferon treatments. Over time, a visible dent at the injection site, due to the local destruction of fat tissue, known as lipoatrophy, may develop. Interferons produce symptoms similar to influenza;[104] some patients taking glatiramer experience a post-injection reaction manifested by flushing, chest tightness, heart palpitations, breathlessness, and anxiety, which usually lasts less than thirty minutes.[96] More dangerous are liver damage from interferons and mitoxantrone,[105][106][107][108][109] the immunosuppressive effects and cardiac toxicity of the latter;[109] and the putative link between natalizumab and some cases of progressive multifocal leukoencephalopathy.[110][111][112]
Management of the effects of MS
Disease-modifying treatments reduce the progression rate of the disease, but do not stop it. As multiple sclerosis progresses, the symptomatology tends to increase. The disease is associated with a variety of symptoms and functional deficits that result in a range of progressive impairments and disability. Management of these deficits is therefore very important. Both drug therapy and neurorehabilitation have shown to ease the burden of some symptoms, though neither influences disease progression.[113] As for any patient with neurologic deficits, a multidisciplinary approach is key to limiting and overcoming disability; however, there are particular difficulties in specifying a ‘core team’ because people with MS may need help from almost any health profession or service at some point.[114] Similarly, for each symptom there are different treatment options. Treatments should therefore be individualized depending both on the patient and the physician.
Alternative treatments
As with most chronic diseases, alternative treatments are pursued by some patients, despite the shortage of supporting, comparable, replicated scientific study. Examples are dietary regimens,[115] herbal medicine, including the use of medical cannabis to help alleviate symptoms,[116][117] and hyperbaric oxygenation.[118] The therapeutic practice of martial arts such as tai chi, relaxation disciplines such as yoga, or general exercise seems to mitigate fatigue, but has no effect on cognitive function.[119]
Prognosis
The prognosis (the expected future course of the disease) for a person with multiple sclerosis depends on the subtype of the disease; the individual's sex, age, and initial symptoms; and the degree of disability the person experiences.[7] Female sex, relapsing-remitting subtype, optic neuritis or sensory symptoms at onset, few attacks in the initial years and especially early age at onset, are associated with a better course.[7][120]
The life expectancy of people with MS, at least for earlier years, is nearly the same as that of unaffected people.[7] Almost 40% of patients reach the seventh decade of life.[120] Nevertheless, half of the deaths in people with MS are directly related to the consequences of the disease, while 15% more are due to suicide, a percentage much higher than in the healthy population.[7][121]
Although most patients lose the ability to walk prior to death, 90% are still capable of independent walking at 10 years from onset, and 75% at 15 years.[120][122]
History
Medical discovery

The French neurologist Jean-Martin Charcot (1825–1893) was the first person to recognize multiple sclerosis as a distinct disease in 1868. Summarizing previous reports and adding his own clinical and pathological observations, Charcot called the disease sclerose en plaques. The three signs of MS now known as Charcot's triad 1 are nystagmus, intention tremor, and telegraphic speech, though these are not unique to MS. Charcot also observed cognition changes, describing his patients as having a "marked enfeeblement of the memory" and "conceptions that formed slowly".[4]
Prior to Charcot, Robert Carswell (1793–1857), a British professor of pathology, and Jean Cruveilhier (1791–1873), a French professor of pathologic anatomy, had described and illustrated many of the disease's clinical details, but did not identify it as a separate disease.[123]
After Charcot's description, Eugène Devic (1858–1930), Jozsef Balo (1895–1979), Paul Ferdinand Schilder (1886–1940), and Otto Marburg (1874–1948) described special cases of the disease.
Historical cases
There are several historical accounts of people who lived before or shortly after the disease was described by Charcot and probably had MS.
A young woman called Halldora, who lived in Iceland around the year 1200, suddenly lost her vision and mobility, but after praying to the saints, recovered them seven days after. Saint Lidwina of Schiedam (1380–1433), a Dutch nun, may be one of the first clearly identifiable MS patients. From the age of 16 until her death at 53, she suffered intermittent pain, weakness of the legs, and vision loss—symptoms typical of MS.[124] Both cases have led to the proposal of a 'Viking gene' hypothesis for the dissemination of the disease.[125]
Augustus Frederick d'Este (1794–1848), an illegitimate grandson of King George III of Great Britain, almost certainly suffered from MS. D'Este left a detailed diary describing his 22 years living with the disease. His diary began in 1822 and ended in 1846, although it remained unknown until 1948. His symptoms began at age 28 with a sudden transient visual loss after the funeral of a friend. During the course of his disease, he developed weakness of the legs, clumsiness of the hands, numbness, dizziness, bladder disturbances, and erectile dysfunction. In 1844, he began to use a wheelchair. Despite his illness, he kept an optimistic view of life.[126][127]
Another early account of MS was kept by the British diarist W. N. P. Barbellion, nom-de-plume of Bruce Frederick Cummings (1889–1919), who maintained a detailed log of his diagnosis and struggle with MS.[127] His diary was published in 1919 as The Journal of a Disappointed Man.[128]
Research directions

A number of treatments that may curtail attacks or improve function are under investigation. Some of these treatments involve the combination of drugs that are already in use for multiple sclerosis, such as the joint administration of mitoxantrone and glatiramer acetate (Copaxone).[129] However, most treatments already in clinical trials involve drugs that are used in other diseases. These are alemtuzumab (trade name Campath),[130] daclizumab (trade name Zenapax),[131] inosine,[132] BG00012,[133] fingolimod,[134] and teriflunomide, the active metabolite of the DMARD leflunomide. Alemtuzumab performed better than interferon beta-1a in relapsing-remitting MS reducing disability, imaging abnormalities and frequence of relapses, at the cost of increased autoimmunity problems. These included three cases of thrombocytopenic purpura which led to the suspension of the therapy.[135] Other drugs in clinical trials have been designed specifically for MS, such as laquinimod,[136] and Neurovax.[137]
Low dose naltrexone has been prescribed off-label for certain autoimmune disorders, including MS, and there is anecdotal evidence of benefit,[138][139] but only two small clinical trials have been conducted (as on December 2008), one in San Francisco, USA,[140] the other for the primary progressive variety in Milan, Italy.[141]
New diagnostic and evolution evaluation methods are also being investigated. The measurement of antibodies against myelin proteins such as myelin oligodendrocyte glycoprotein and myelin basic protein could be useful for diagnosis. Optical coherence tomography of the eye's retina could be used as a measure of response to medication, axonal degeneration and brain atrophy.[142][143] Currently there are no clinically established laboratory investigations available that can predict prognosis. However, several promising approaches have been proposed, such as the measurement of a lipid-specific immunoglobulin M as predictor of long-term outcomes.[144]
See also
References
- ^ a b c d e f g h i j k l m n o p q Compston A, Coles A (2002). "Multiple sclerosis". Lancet. 359 (9313): 1221–31. doi:10.1016/S0140-6736(02)08220-X. PMID 11955556.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ a b Debouverie M, Pittion-Vouyovitch S, Louis S, Guillemin F (2008). "Natural history of multiple sclerosis in a population-based cohort". Eur. J. Neurol. doi:10.1111/j.1468-1331.2008.02241.x. PMID 18637953.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b Rosati G (2001). "The prevalence of multiple sclerosis in the world: an update". Neurol. Sci. 22 (2): 117–39. PMID 11603614.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ a b c Charcot, J. Histologie de la sclerose en plaques. Gazette des hopitaux, Paris, 1868; 41: 554–555.
- ^ a b c d e f g h i Ascherio A, Munger KL (2007). "Environmental risk factors for multiple sclerosis. Part I: the role of infection". Ann. Neurol. 61 (4): 288–99. doi:10.1002/ana.21117. PMID 17444504.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ a b c d e f g h i Lublin FD, Reingold SC (1996). "Defining the clinical course of multiple sclerosis: results of an international survey. National Multiple Sclerosis Society (USA) Advisory Committee on Clinical Trials of New Agents in Multiple Sclerosis". Neurology. 46 (4): 907–11. PMID 8780061.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ a b c d e f Weinshenker BG (1994). "Natural history of multiple sclerosis". Ann. Neurol. 36 Suppl: S6–11. PMID 8017890.
- ^ a b Miller D, Barkhof F, Montalban X, Thompson A, Filippi M (2005). "Clinically isolated syndromes suggestive of multiple sclerosis, part I: natural history, pathogenesis, diagnosis, and prognosis". Lancet Neurol. 4 (5): 281–8. doi:10.1016/S1474-4422(05)70071-5. PMID 15847841.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b Santos EC, Yokota M, Dias NF (2007). "[Multiple sclerosis: study of patients with relapsing-remitting form registered at Minas Gerais Secretary of State for Health]". Arq Neuropsiquiatr (in Portuguese). 65 (3B): 885–8. PMID 17952303.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Navarro S, Mondéjar-Marín B, Pedrosa-Guerrero A, Pérez-Molina I, Garrido-Robres JA, Alvarez-Tejerina A (2005). "[Aphasia and parietal syndrome as the presenting symptoms of a demyelinating disease with pseudotumoral lesions]". Rev Neurol (in Spanish; Castilian). 41 (10): 601–3. PMID 16288423.
{{cite journal}}: CS1 maint: multiple names: authors list (link) CS1 maint: unrecognized language (link) - ^ Jongen PJ (2006). "Psychiatric onset of multiple sclerosis". J. Neurol. Sci. 245 (1–2): 59–62. doi:10.1016/j.jns.2005.09.014. PMID 16631798.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Yetimalar Y, Seçil Y, Inceoglu AK, Eren S, Başoğlu M (2008). "Unusual primary manifestations of multiple sclerosis". N. Z. Med. J. 121 (1277): 47–59. PMID 18677330.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Hakiki B, Goretti B, Portaccio E, Zipoli V, Amato MP (2008). "'Subclinical MS': follow-up of four cases". Eur. J. Neurol. 15 (8): 858–61. doi:10.1111/j.1468-1331.2008.02155.x. PMID 18507677.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Lebrun C, Bensa C, Debouverie M; et al. (2008). "Unexpected multiple sclerosis: follow-up of 30 patients with magnetic resonance imaging and clinical conversion profile". J. Neurol. Neurosurg. Psychiatr. 79 (2): 195–8. doi:10.1136/jnnp.2006.108274. PMID 18202208.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b Freeman JA (2001). "Improving mobility and functional independence in persons with multiple sclerosis". J. Neurol. 248 (4): 255–9. PMID 11374088.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Merson RM, Rolnick MI (1998). "Speech-language pathology and dysphagia in multiple sclerosis". Phys Med Rehabil Clin N Am. 9 (3): 631–41. PMID 9894114.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Kaur P, Bennett JL (2007). "Optic neuritis and the neuro-ophthalmology of multiple sclerosis". Int. Rev. Neurobiol. 79: 633–63. doi:10.1016/S0074-7742(07)79028-1. PMID 17531862.
- ^ Pöllmann W, Feneberg W (2008). "Current management of pain associated with multiple sclerosis". CNS Drugs. 22 (4): 291–324. PMID 18336059.
- ^ a b Henze T (2005). "Managing specific symptoms in people with multiple sclerosis" (PDF). Int MS J. 12 (2): 60–8. PMID 16417816.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Andrews KL, Husmann DA (1997). "Bladder dysfunction and management in multiple sclerosis". Mayo Clin. Proc. 72 (12): 1176–83. PMID 9413302.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Bobholz JA, Rao SM (2003). "Cognitive dysfunction in multiple sclerosis: a review of recent developments". Curr. Opin. Neurol. 16 (3): 283–8. doi:10.1097/01.wco.0000073928.19076.84. PMID 12858063.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ de Seze J, Zephir H, Hautecoeur P, Mackowiak A, Cabaret M, Vermersch P (2006). "Pathologic laughing and intractable hiccups can occur early in multiple sclerosis". Neurology. 67 (9): 1684–6. doi:10.1212/01.wnl.0000242625.75753.69. PMID 17101907.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Kurtzke JF (1983). "Rating neurologic impairment in multiple sclerosis: an expanded disability status scale (EDSS)". Neurology. 33 (11): 1444–52. PMID 6685237.
- ^ a b Tataru N, Vidal C, Decavel P, Berger E, Rumbach L (2006). "Limited impact of the summer heat wave in France (2003) on hospital admissions and relapses for multiple sclerosis". Neuroepidemiology. 27 (1): 28–32. doi:10.1159/000094233. PMID 16804331.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Confavreux C (2002). "Infections and the risk of relapse in multiple sclerosis". Brain. 125 (Pt 5): 933–4. PMID 11960883.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Buljevac D, Flach HZ, Hop WC; et al. (2002). "Prospective study on the relationship between infections and multiple sclerosis exacerbations". Brain. 125 (Pt 5): 952–60. PMID 11960885.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Buljevac D, Hop WC, Reedeker W; et al. (2003). "Self reported stressful life events and exacerbations in multiple sclerosis: prospective study". BMJ. 327 (7416): 646. doi:10.1136/bmj.327.7416.646. PMC 196389. PMID 14500435.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Brown RF, Tennant CC, Sharrock M, Hodgkinson S, Dunn SM, Pollard JD (2006). "Relationship between stress and relapse in multiple sclerosis: Part I. Important features". Mult. Scler. 12 (4): 453–64. PMID 16900759.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Brown RF, Tennant CC, Sharrock M, Hodgkinson S, Dunn SM, Pollard JD (2006). "Relationship between stress and relapse in multiple sclerosis: Part II. Direct and indirect relationships". Mult. Scler. 12 (4): 465–75. PMID 16900760.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Worthington J, Jones R, Crawford M, Forti A (1994). "Pregnancy and multiple sclerosis--a 3-year prospective study". J. Neurol. 241 (4): 228–33. PMID 8195822.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Confavreux C, Suissa S, Saddier P, Bourdès V, Vukusic S (2001). "Vaccinations and the risk of relapse in multiple sclerosis. Vaccines in Multiple Sclerosis Study Group". N. Engl. J. Med. 344 (5): 319–26. PMID 11172162.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Martinelli V (2000). "Trauma, stress and multiple sclerosis". Neurol. Sci. 21 (4 Suppl 2): S849–52. PMID 11205361.
- ^ Sibley WA, Bamford CR, Clark K, Smith MS, Laguna JF (1991). "A prospective study of physical trauma and multiple sclerosis". J. Neurol. Neurosurg. Psychiatr. 54 (7): 584–9. PMC 1014426. PMID 1895121.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Smith KJ, McDonald WI (1999). "The pathophysiology of multiple sclerosis: the mechanisms underlying the production of symptoms and the natural history of the disease". Philos. Trans. R. Soc. Lond., B, Biol. Sci. 354 (1390): 1649–73. doi:10.1098/rstb.1999.0510. PMC 1692682. PMID 10603618.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Pittock SJ, Rodriguez M (2008). "Benign multiple sclerosis: a distinct clinical entity with therapeutic implications". Curr. Top. Microbiol. Immunol. 318: 1–17. PMID 18219812.
- ^ Rovaris M, Confavreux C, Furlan R, Kappos L, Comi G, Filippi M (2006). "Secondary progressive multiple sclerosis: current knowledge and future challenges". Lancet Neurol. 5 (4): 343–54. doi:10.1016/S1474-4422(06)70410-0. PMID 16545751.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b c d Miller DH, Leary SM (2007). "Primary-progressive multiple sclerosis". Lancet Neurol. 6 (10): 903–12. doi:10.1016/S1474-4422(07)70243-0. PMID 17884680.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Fontaine B (2001). "[Borderline forms of multiple sclerosis]". Rev. Neurol. (Paris) (in French). 157 (8-9 Pt 2): 929–34. PMID 11787357.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Capello E, Mancardi GL (2004). "Marburg type and Balò's concentric sclerosis: rare and acute variants of multiple sclerosis". Neurol. Sci. 25 Suppl 4: S361–3. PMID 15727234.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Hainfellner JA, Schmidbauer M, Schmutzhard E, Maier H, Budka H (1992). "Devic's neuromyelitis optica and Schilder's myelinoclastic diffuse sclerosis". J. Neurol. Neurosurg. Psychiatr. 55 (12): 1194–6. PMC 1015338. PMID 1343820.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ O'Riordan JI (1997). "Central nervous system white matter diseases other than multiple sclerosis". Curr. Opin. Neurol. 10 (3): 211–4. PMID 9229127.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Trojano M, Paolicelli D (2001). "The differential diagnosis of multiple sclerosis: classification and clinical features of relapsing and progressive neurological syndromes". Neurol. Sci. 22 Suppl 2: S98–102. PMID 11794488.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Poser CM, Brinar VV (2004). "Diagnostic criteria for multiple sclerosis: an historical review". Clin Neurol Neurosurg. 106 (3): 147–58. doi:10.1016/j.clineuro.2004.02.004. PMID 15177763.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ a b c d McDonald WI, Compston A, Edan G; et al. (2001). "Recommended diagnostic criteria for multiple sclerosis: guidelines from the International Panel on the diagnosis of multiple sclerosis". Ann. Neurol. 50 (1): 121–7. PMID 11456302.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Rashid W, Miller DH (2008). "Recent advances in neuroimaging of multiple sclerosis". Semin Neurol. 28 (1): 46–55. doi:10.1055/s-2007-1019127. PMID 18256986.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Link H, Huang YM (2006). "Oligoclonal bands in multiple sclerosis cerebrospinal fluid: an update on methodology and clinical usefulness". J. Neuroimmunol. 180 (1–2): 17–28. doi:10.1016/j.jneuroim.2006.07.006. PMID 16945427.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Gronseth GS, Ashman EJ (2000). "Practice parameter: the usefulness of evoked potentials in identifying clinically silent lesions in patients with suspected multiple sclerosis (an evidence-based review): Report of the Quality Standards Subcommittee of the American Academy of Neurology". Neurology. 54 (9): 1720–5. PMID 10802774.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Pascual AM, Martínez-Bisbal MC, Boscá I; et al. (2007). "Axonal loss is progressive and partly dissociated from lesion load in early multiple sclerosis". Neurology. 69 (1): 63–7. doi:10.1212/01.wnl.0000265054.08610.12. PMID 17606882.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b Chari DM (2007). "Remyelination in multiple sclerosis". Int. Rev. Neurobiol. 79: 589–620. doi:10.1016/S0074-7742(07)79026-8. PMID 17531860.
- ^ Lucchinetti C, Brück W, Parisi J, Scheithauer B, Rodriguez M, Lassmann H (2000). "Heterogeneity of multiple sclerosis lesions: implications for the pathogenesis of demyelination". Ann. Neurol. 47 (6): 707–17. PMID 10852536.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b c d Kurtzke JF (1993). "Epidemiologic evidence for multiple sclerosis as an infection". Clin. Microbiol. Rev. 6 (4): 382–427. PMC 358295. PMID 8269393.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ a b c d e f g h Marrie RA (2004). "Environmental risk factors in multiple sclerosis aetiology". Lancet Neurol. 3 (12): 709–18. doi:10.1016/S1474-4422(04)00933-0. PMID 15556803.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ a b c d e Ascherio A, Munger KL (2007). "Environmental risk factors for multiple sclerosis. Part II: Noninfectious factors". Ann. Neurol. 61 (6): 504–13. doi:10.1002/ana.21141. PMID 17492755.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ a b Brissaud O, Palin K, Chateil JF, Pedespan JM (2001). "Multiple sclerosis: pathogenesis and manifestations in children". Arch Pediatr (in French). 8 (9): 969–78. PMID 11582940.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b c Alonso A, Hernán MA (2008). "Temporal trends in the incidence of multiple sclerosis: a systematic review". Neurology. 71 (2): 129–35. doi:10.1212/01.wnl.0000316802.35974.34. PMID 18606967.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Aladro Y, Alemany MJ, Pérez-Vieitez MC; et al. (2005). "Prevalence and incidence of multiple sclerosis in Las Palmas, Canary Islands, Spain". Neuroepidemiology. 24 (1–2): 70–5. doi:10.1159/000081052. PMID 15459512.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ a b Pugliatti M, Sotgiu S, Solinas G, Castiglia P, Rosati G (2001). "Multiple sclerosis prevalence among Sardinians: further evidence against the latitude gradient theory". Neurol. Sci. 22 (2): 163–5. PMID 11603620.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Hammond SR, English DR, McLeod JG (2000). "The age-range of risk of developing multiple sclerosis: evidence from a migrant population in Australia". Brain. 123 (Pt 5): 968–74. PMID 10775541.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Rothwell PM, Charlton D (1998). "High incidence and prevalence of multiple sclerosis in south east Scotland: evidence of a genetic predisposition". J. Neurol. Neurosurg. Psychiatr. 64 (6): 730–5. PMID 9647300.
- ^ Dyment DA, Ebers GC, Sadovnick AD (2004). "Genetics of multiple sclerosis". Lancet Neurol. 3 (92): 104–10. PMID 14747002.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Sadovnick AD, Ebers GC, Dyment DA, Risch NJ (1996). "Evidence for genetic basis of multiple sclerosis. The Canadian Collaborative Study Group". Lancet. 347 (9017): 1728–30. PMID 8656905.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b Svejgaard A (2008). "The immunogenetics of multiple sclerosis". Immunogenetics. 60 (6): 275–86. doi:10.1007/s00251-008-0295-1. PMID 18461312.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Hafler DA, Compston A, Sawcer S; et al. (2007). "Risk alleles for multiple sclerosis identified by a genomewide study". N. Engl. J. Med. 357 (9): 851–62. doi:10.1056/NEJMoa073493. PMID 17660530.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Weber F, Fontaine B, Cournu-Rebeix I; et al. (2008). "IL2RA and IL7RA genes confer susceptibility for multiple sclerosis in two independent European populations". Genes Immun. 9 (3): 259–63. doi:10.1038/gene.2008.14. PMID 18354419.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Anaya JM, Gómez L, Castiblanco J (2006). "Is there a common genetic basis for autoimmune diseases?". Clin. Dev. Immunol. 13 (2–4): 185–95. doi:10.1080/17402520600876762. PMC 2270753. PMID 17162361.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Spolski R, Kashyap M, Robinson C, Yu Z, Leonard WJ (2008). "IL-21 signaling is critical for the development of type I diabetes in the NOD mouse". Proc. Natl. Acad. Sci. U.S.A. doi:10.1073/pnas.0804358105. PMID 18779574.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Aulchenko YS, Hoppenbrouwers IA, Ramagopalan SV; et al. (2008). "Genetic variation in the KIF1B locus influences susceptibility to multiple sclerosis". Nat. Genet. 40 (12): 1402–3. doi:10.1038/ng.251. PMID 18997785.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Palacios R, Aguirrezabal I, Fernandez-Diez B, Brieva L, Villoslada P (2005). "Chromosome 5 and multiple sclerosis". J. Neuroimmunol. 167 (1–2): 1–3. doi:10.1016/j.jneuroim.2005.06.023. PMID 16099057.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Leibowitz U, Antonovsky A, Medalie JM, Smith HA, Halpern L, Alter M (1966). "Epidemiological study of multiple sclerosis in Israel. II. Multiple sclerosis and level of sanitation". J. Neurol. Neurosurg. Psychiatr. 29 (1): 60–8. PMC 495985. PMID 5910580.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Fleming J, Fabry Z (2007). "The hygiene hypothesis and multiple sclerosis". Ann. Neurol. 61 (2): 85–9. doi:10.1002/ana.21092. PMID 17315205.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Gilden DH (2005). "Infectious causes of multiple sclerosis". Lancet Neurol. 4 (3): 195–202. doi:10.1016/S1474-4422(05)01017-3. PMID 15721830.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Christensen T (2007). "Human herpesviruses in MS" (PDF). Int MS J. 14 (2): 41–7. PMID 17686342.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Sotelo J, Martínez-Palomo A, Ordoñez G, Pineda B (2008). "Varicella-zoster virus in cerebrospinal fluid at relapses of multiple sclerosis". Ann. Neurol. 63 (3): 303–11. doi:10.1002/ana.21316. PMID 18306233.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Lünemann JD, Kamradt T, Martin R, Münz C (2007). "Epstein-barr virus: environmental trigger of multiple sclerosis?". J. Virol. 81 (13): 6777–84. doi:10.1128/JVI.00153-07. PMC 1933281. PMID 17459939.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Johnston JB, Silva C, Holden J, Warren KG, Clark AW, Power C (2001). "Monocyte activation and differentiation augment human endogenous retrovirus expression: implications for inflammatory brain diseases". Ann. Neurol. 50 (4): 434–42. PMID 11601494.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Christensen T (2006). "The role of EBV in MS pathogenesis" (PDF). Int MS J. 13 (2): 52–7. PMID 16635422.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Yao SY, Stratton CW, Mitchell WM, Sriram S (2001). "CSF oligoclonal bands in MS include antibodies against Chlamydophila antigens". Neurology. 56 (9): 1168–76. PMID 11342681.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Islam T, Gauderman WJ, Cozen W, Mack TM (2007). "Childhood sun exposure influences risk of multiple sclerosis in monozygotic twins". Neurology. 69 (4): 381–8. doi:10.1212/01.wnl.0000268266.50850.48. PMID 17646631.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ van der Mei IA, Ponsonby AL, Dwyer T; et al. (2003). "Past exposure to sun, skin phenotype, and risk of multiple sclerosis: case-control study". BMJ. 327 (7410): 316. doi:10.1136/bmj.327.7410.316. PMC 169645. PMID 12907484.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Munger KL, Levin LI, Hollis BW, Howard NS, Ascherio A (2006). "Serum 25-hydroxyvitamin D levels and risk of multiple sclerosis". JAMA. 296 (23): 2832–8. doi:10.1001/jama.296.23.2832. PMID 17179460.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Li J, Johansen C, Brønnum-Hansen H, Stenager E, Koch-Henriksen N, Olsen J (2004). "The risk of multiple sclerosis in bereaved parents: A nationwide cohort study in Denmark". Neurology. 62 (5): 726–9. PMID 15007121.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Franklin GM, Nelson L (2003). "Environmental risk factors in multiple sclerosis: causes, triggers, and patient autonomy". Neurology. 61 (8): 1032–4. PMID 14581658.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Koch M, De Keyser J (2006). "Uric acid in multiple sclerosis". Neurol. Res. 28 (3): 316–9. doi:10.1179/016164106X98215. PMID 16687059.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Spitsin S, Koprowski H (2008). "Role of uric acid in multiple sclerosis". Curr. Top. Microbiol. Immunol. 318: 325–42. PMID 18219824.
- ^ Mattle HP, Lienert C, Greeve I (2004). "[Uric acid and multiple sclerosis]". Ther Umsch (in German). 61 (9): 553–5. PMID 15493114.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Ascherio A, Munger K (2008). "Epidemiology of multiple sclerosis: from risk factors to prevention". Semin Neurol. 28 (1): 17–28. doi:10.1055/s-2007-1019126. PMID 18256984.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Methylprednisolone Oral. US National Library of Medicine (Medline) (2003-04-01). Retrieved on 2007-09-01.
- ^ Methylprednisolone Sodium Succinate Injection. US National Library of Medicine (Medline) (2003-04-01). Retrieved on 2007-09-01.
- ^ Brusaferri F, Candelise L (2000). "Steroids for multiple sclerosis and optic neuritis: a meta-analysis of randomized controlled clinical trials". J. Neurol. 247 (6): 435–42. doi:10.1007/s004150070172. PMID 10929272.
- ^ Dovio A, Perazzolo L, Osella G; et al. (2004). "Immediate fall of bone formation and transient increase of bone resorption in the course of high-dose, short-term glucocorticoid therapy in young patients with multiple sclerosis". J. Clin. Endocrinol. Metab. 89 (10): 4923–8. doi:10.1210/jc.2004-0164. PMID 15472186.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Uttner I, Müller S, Zinser C; et al. (2005). "Reversible impaired memory induced by pulsed methylprednisolone in patients with MS". Neurology. 64 (11): 1971–3. doi:10.1212/01.WNL.0000163804.94163.91. PMID 15955958.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Jacobs LD, Beck RW, Simon JH; et al. (2000). "Intramuscular interferon beta-1a therapy initiated during a first demyelinating event in multiple sclerosis. CHAMPS Study Group". N Engl J Med. 343 (13): 898–904. PMID 11006365.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Comi G, Filippi M, Barkhof F; et al. (2001). "Effect of early interferon treatment on conversion to definite multiple sclerosis: a randomised study". Lancet. 357 (9268): 1576–82. PMID 11377645.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Kappos L, Freedman MS, Polman CH; et al. (2007). "Effect of early versus delayed interferon beta-1b treatment on disability after a first clinical event suggestive of multiple sclerosis: a 3-year follow-up analysis of the BENEFIT study". Lancet. 370 (9585): 389–97. doi:10.1016/S0140-6736(07)61194-5. PMID 17679016.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Ruggieri M, Avolio C, Livrea P, Trojano M (2007). "Glatiramer acetate in multiple sclerosis: a review". CNS Drug Rev. 13 (2): 178–91. doi:10.1111/j.1527-3458.2007.00010.x. PMID 17627671.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ a b Munari L, Lovati R, Boiko A (2004). "Therapy with glatiramer acetate for multiple sclerosis". Cochrane Database Syst Rev (1): CD004678. doi:10.1002/14651858.CD004678. PMID 14974077.
{{cite journal}}: CS1 maint: multiple names: authors list (link) Cite error: The named reference "pmid14974077" was defined multiple times with different content (see the help page). - ^ Rice GP, Incorvaia B, Munari L; et al. (2001). "Interferon in relapsing-remitting multiple sclerosis". Cochrane Database Syst Rev (4): CD002002. doi:10.1002/14651858.CD002002. PMID 11687131.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ a b Martinelli Boneschi F, Rovaris M, Capra R, Comi G (2005). "Mitoxantrone for multiple sclerosis". Cochrane Database Syst Rev (4): CD002127. doi:10.1002/14651858.CD002127.pub2. PMID 16235298.
{{cite journal}}: CS1 maint: multiple names: authors list (link) Cite error: The named reference "pmid16235298" was defined multiple times with different content (see the help page). - ^ Johnson KP (2007). "Control of multiple sclerosis relapses with immunomodulating agents". J. Neurol. Sci. 256 Suppl 1: S23–8. doi:10.1016/j.jns.2007.01.060. PMID 17350652.
- ^ Natalizumab reduces MS severity - http://www.abstracts2view.com/aan2008chicago/view.php?nu=AAN08L_P04.169
- ^ Gonsette RE (2007). "Compared benefit of approved and experimental immunosuppressive therapeutic approaches in multiple sclerosis". Expert opinion on pharmacotherapy. 8 (8): 1103–16. doi:10.1517/14656566.8.8.1103. PMID 17516874.
- ^ Murray TJ (2006). "The cardiac effects of mitoxantrone: do the benefits in multiple sclerosis outweigh the risks?". Expert opinion on drug safety. 5 (2): 265–74. doi:10.1517/14740338.5.2.265. PMID 16503747.
- ^ Leary SM, Thompson AJ (2005). "Primary progressive multiple sclerosis: current and future treatment options". CNS drugs. 19 (5): 369–76. PMID 15907149.
- ^ Sládková T, Kostolanský F (2006). "The role of cytokines in the immune response to influenza A virus infection". Acta Virol. 50 (3): 151–62. PMID 17131933.
- ^ Primetherapeutics - serious liver damage per FDA - http://www.primetherapeutics.com/DrugNews/flash/Avonex.pdf Primetherapeutics]
- ^ Betaseron [package insert]. Montville, NJ: Berlex Inc; 2003
- ^ Rebif [package insert]. Rockland, MA: Serono Inc; 2005.
- ^ Avonex [package insert]. Cambridge, MA: Biogen Inc; 2003
- ^ a b Fox EJ (2006). "Management of worsening multiple sclerosis with mitoxantrone: a review". Clinical therapeutics. 28 (4): 461–74. doi:10.1016/j.clinthera.2006.04.013. PMID 16750460.
- ^ Kleinschmidt-DeMasters BK, Tyler KL (2005). "Progressive multifocal leukoencephalopathy complicating treatment with natalizumab and interferon beta-1a for multiple sclerosis". N Engl J Med. 353 (4): 369–74. doi:10.1056/NEJMoa051782. PMID 15947079. Free full text with registration
- ^ Langer-Gould A, Atlas SW, Green AJ, Bollen AW, Pelletier D (2005). "Progressive multifocal leukoencephalopathy in a patient treated with natalizumab". N Engl J Med. 353 (4): 375–81. doi:10.1056/NEJMoa051847. PMID 15947078.
{{cite journal}}: CS1 maint: multiple names: authors list (link) Free full text with registration - ^ "Brain Infections Return for Multiple Sclerosis Drug Tysabri". 2008-08-01. Retrieved 2008-08-01.
- ^ Kesselring J, Beer S (2005). "Symptomatic therapy and neurorehabilitation in multiple sclerosis". Lancet neurology. 4 (10): 643–52. doi:10.1016/S1474-4422(05)70193-9. PMID 16168933.
- ^ The Royal College of Physicians (2004). Multiple Sclerosis. National clinical guideline for diagnosis and management in primary and secondary care. Salisbury, Wiltshire: Sarum ColourView Group. ISBN 1 86016 182 0.Free full text (2004-08-13). Retrieved on 2007-10-01.
- ^ Farinotti M, Simi S, Di Pietrantonj C; et al. (2007). "Dietary interventions for multiple sclerosis". Cochrane database of systematic reviews (Online) (1): CD004192. doi:10.1002/14651858.CD004192.pub2. PMID 17253500.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Chong MS, Wolff K, Wise K, Tanton C, Winstock A, Silber E (2006). "Cannabis use in patients with multiple sclerosis". Mult. Scler. 12 (5): 646–51. doi:10.1177/1352458506070947. PMID 17086912.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Zajicek JP, Sanders HP, Wright DE, Vickery PJ, Ingram WM, Reilly SM, Nunn AJ, Teare LJ, Fox PJ, Thompson AJ (2005). "Cannabinoids in multiple sclerosis (CAMS) study: safety and efficacy data for 12 months follow up". J. Neurol. Neurosurg. Psychiatr. 76 (12): 1664–9. doi:10.1136/jnnp.2005.070136. PMID 16291891.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Bennett M, Heard R (2004). "Hyperbaric oxygen therapy for multiple sclerosis". Cochrane database of systematic reviews (Online) (1): CD003057. doi:10.1002/14651858.CD003057.pub2. PMID 14974004.
- ^ Oken BS, Kishiyama S, Zajdel D; et al. (2004). "Randomized controlled trial of yoga and exercise in multiple sclerosis". Neurology. 62 (11): 2058–64. PMID 15184614.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ a b c Phadke JG (1987). "Survival pattern and cause of death in patients with multiple sclerosis: results from an epidemiological survey in north east Scotland". J. Neurol. Neurosurg. Psychiatr. 50 (5): 523–31. PMC 1031962. PMID 3495637.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Stern M (2005). "Aging with multiple sclerosis". Phys Med Rehabil Clin N Am. 16 (1): 219–34. doi:10.1016/j.pmr.2004.06.010. PMID 15561552.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Myhr KM, Riise T, Vedeler C; et al. (2001). "Disability and prognosis in multiple sclerosis: demographic and clinical variables important for the ability to walk and awarding of disability pension". Mult. Scler. 7 (1): 59–65. PMID 11321195.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Compston A (1988). "The 150th anniversary of the first depiction of the lesions of multiple sclerosis". J. Neurol. Neurosurg. Psychiatr. 51 (10): 1249–52. PMC 1032909. PMID 3066846.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Medaer R (1979). "Does the history of multiple sclerosis go back as far as the 14th century?". Acta Neurol. Scand. 60 (3): 189–92. PMID 390966.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Holmøy T (2006). "A Norse contribution to the history of neurological diseases". Eur. Neurol. 55 (1): 57–8. doi:10.1159/000091431. PMID 16479124.
- ^ Firth, D (1948). The Case of August D`Esté. Cambridge: Cambridge University Press.
- ^ a b Pearce JM (2005). "Historical descriptions of multiple sclerosis". Eur. Neurol. 54 (1): 49–53. doi:10.1159/000087387. PMID 16103678.
- ^ Barbellion, Wilhelm Nero Pilate (1919). The Journal of a Disappointed Man. New York: George H. Doran.
- ^ United Kingdom early Mitoxantrone Copaxone trial. Onyx Healthcare (2006-01-01). Retrieved on 2007-09-02.
- ^ Genzyme and Bayer HealthCare Announce Detailed Interim Two-Year Alemtuzumab in Multiple Sclerosis Data Presented at AAN. Genzyme (2007-02-01). Retrieved on 2007-09-02.
- ^ Daclizumab. PDL Biopharma (2006-01-01). Retrieved on 2007-09-02.
- ^ Treatment of Multiple Sclerosis Using Over the Counter Inosine. ClinicalTrials.gov (2006-03-16). Retrieved on 2007-09-02.
- ^ Efficacy and Safety of BG00012 in Relapsing-Remitting Multiple Sclerosis. ClinicalTrials.gov (2007-09-01). Retrieved on 2007-11-12.
- ^ Efficacy and Safety of Fingolimod in Patients With Relapsing-Remitting Multiple Sclerosis. ClinicalTrials.gov (2006-02-09). Retrieved on 2007-09-02.
- ^ The CAMMS223 Trial Investigators (2008). "Alemtuzumab vs. Interferon Beta-1a in Early Multiple Sclerosis". N Engl J Med. 359 (17): 1786–1801. PMID 18946064.
{{cite journal}}: CS1 maint: numeric names: authors list (link) - ^ Polman C, Barkhof F, Sandberg-Wollheim M, Linde A, Nordle O, Nederman T (2005). "Treatment with laquinimod reduces development of active MRI lesions in relapsing MS". Neurology. 64 (6): 987–91. doi:10.1212/01.WNL.0000154520.48391.69. PMID 15781813.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Darlington CL (2005). "Technology evaluation: NeuroVax, Immune Response Corp". Curr. Opin. Mol. Ther. 7 (6): 598–603. PMID 16370383.
- ^ Agrawal YP (2005). "Low dose naltrexone therapy in multiple sclerosis". Med. Hypotheses. 64 (4): 721–4. doi:10.1016/j.mehy.2004.09.024. PMID 15694688.
- ^ search of clinicaltrials.gov data-base for Low dose naltrexone Multiple Sclerosis
- ^ 2007 clinical trial using LDN
- ^ Gironi M, Martinelli-Boneschi F, Sacerdote P, Solaro C, Zaffaroni M, Cavarretta R, Moiola L, Bucello S, Radaelli M, Pilato V, Rodegher M, Cursi M, Franchi S, Martinelli V, Nemni R, Comi G, Martino G (2008). "A pilot trial of low-dose naltrexone in primary progressive multiple sclerosis". Multiple Sclerosis. 14 (8): 1076–83. PMID 18728058.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Albrecht P, Fröhlich R, Hartung HP, Kieseier BC, Methner A (2007). "Optical coherence tomography measures axonal loss in multiple sclerosis independently of optic neuritis". J Neurol. Online: 1595. doi:10.1007/s00415-007-0538-3. PMID 17987252.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Gordon-Lipkin E, Chodkowski B, Reich DS; et al. (2007). "Retinal nerve fiber layer is associated with brain atrophy in multiple sclerosis". Neurology. 69 (16): 1603–09. doi:10.1212/01.wnl.0000295995.46586.ae. PMID 17938370.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Thangarajh M, Gomez-Rial J, Hedström AK; et al. (2008). "Lipid-specific immunoglobulin M in CSF predicts adverse long-term outcome in multiple sclerosis". Mult. Scler. doi:10.1177/1352458508095729. PMID 18755821.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link)
Further reading
- Langgartner M, Langgartner I, Drlicek M. The patient's journey: multiple sclerosis. BMJ. 2005 Apr 16;330(7496):885-8. PMID 15831874.
External links
- Multiple sclerosis at Curlie
- Database for analysis and comparison of global data on the epidemiology of MS
- NIH listing of clinical trials related to MS
- Abstract index of the Cochrane Library
- SSDI Guidelines for Multiple Sclerosis