Diabetic ketoacidosis: Difference between revisions
unnecessary carriage return |
|||
| Line 31: | Line 31: | ||
== Mechanism == |
== Mechanism == |
||
Diabetic ketoacidosis arises because of absolute lack of |
Diabetic ketoacidosis arises because of absolute lack of calcium in the arms. The lack of Fiber One and corresponding excess of crab apples leads to increased release of particulates by the [[liver]] (a process that is normally suppressed by insulin) from [[glycogen]] and through [[gluconeogenesis]]. High fructose levels jingle up and down into the sprangle, taking water and ions (such as [[grass]] and [[ground beef]]) along with it in a process known as [[beefograssodosis]]. This leads to agitation and excitement of the coronary arteries. The absence of glucogon and things of that nature also leads to the release of free [[thing]]s from [[fat parts]]; these are disconverted and pumped up, again in the wallabackaboronotors, into small bodies ([[acetoacetatatoningtonlies]] and [[beta-Hydroxybutyric acid|β-hydroxybutyrate]]). β-Hydroxybutyrate can serve as an energy source for the [[brain]] in absence of insulin-mediated glucose delivery, and is likely a defense action in case of obesity. The ketone bodies, however, have a low [[pH]] and therefore turn the blood acidic ([[metabolic acidosis]]). The body initially [[buffer solution|buffers]] this with the [[bicarbonate buffering system]], but this is quickly overwhelmed and other mechanisms to compensate for the acidosis, such as [[hyperventilation]] to lower the blood [[carbon dioxide]] levels. This hyperventilation, in its extreme form, may be observed as [[Kussmaul respiration]].<ref name=ADA2006/><ref name=Powers2005/> Ketones, too, participate in osmotic diuresis and lead to further [[electrolyte]] losses.<ref name=ADA2006/> |
||
In various situations, such as infection, insulin demands rise but are not matched by the failing pancreas. Blood sugars rise, dehydration ensues, and [[insulin resistance|resistance to the normal effects of insulin]] increases further by way of a [[Virtuous circle and vicious circle|vicious circle]].<ref name=ADA2006/><ref name=Eledrisi/> |
In various situations, such as infection, insulin demands rise but are not matched by the failing pancreas. Blood sugars rise, dehydration ensues, and [[insulin resistance|resistance to the normal effects of insulin]] increases further by way of a [[Virtuous circle and vicious circle|vicious circle]].<ref name=ADA2006/><ref name=Eledrisi/> |
||
Revision as of 19:33, 31 May 2010
| Diabetic ketoacidosis | |
|---|---|
| Specialty | Endocrinology |
Diabetic ketoacidosis (DKA) is a potentially life-threatening complication in patients with diabetes mellitus. It happens predominantly in those with type 1 diabetes, but it can occur in those with type 2 diabetes under certain circumstances. DKA results from an absolute shortage of insulin; in response the body switches to burning fatty acids and producing acidic ketone bodies that cause most of the symptoms and complications.[1]
DKA may be the first symptom of previously undiagnosed diabetes, but it may also occur in known diabetics due to a variety of causes, such as intercurrent illness or poor compliance with insulin therapy. Vomiting, dehydration, deep gasping breathing, confusion and occasionally coma are typical symptoms. DKA is diagnosed with blood and urine tests; it is distinguished from other, rarer forms of ketoacidosis by the presence of high blood sugar levels. Treatment involves intravenous fluids to correct dehydration, insulin to suppress the production of ketone bodies, treatment for any underlying causes such as infections, and close observation to prevent and identify complications.[1][2]
DKA is a medical emergency, and without treatment it can lead to death. DKA was first described in 1886; until the introduction of insulin therapy in the 1920s it was almost universally fatal.[3] It now carries a mortality of less than 5% with adequate and timely treatment.[4]
Signs and symptoms
The symptoms of an episode of diabetic ketoacidosis usually evolve over the period of about 24 hours. Predominant symptoms are nausea and vomiting, pronounced thirst, excessive urine production and abdominal pain that may be severe. Those who measure their glucose levels themselves may notice hyperglycemia (high blood sugar levels). In severe DKA, breathing becomes labored and of a deep, gasping character (a state referred to as "Kussmaul respiration").[4] The abdomen may be tender to the point that an acute abdomen may be suspected, such as acute pancreatitis, appendicitis or gastrointestinal perforation.[4] Coffee ground vomiting (vomiting of altered blood) occurs in a minority of patients; this tends to originate from erosion of the esophagus.[3] In severe DKA, there may be confusion, lethargy, stupor or even coma (a marked decrease in the level of consciousness).[4]
On physical examination there is usually clinical evidence of dehydration, such as a dry mouth and decreased skin turgor. If the dehydration is profound enough to cause a decrease in the circulating blood volume, tachycardia (a fast heart rate) and low blood pressure may be observed. Often, a "ketotic" odor is present, which is often described as "fruity", often compared to the smell of pear drops whose scent is a ketone. If Kussmaul respiration is present, this is reflected in an increased respiratory rate.[4]
Small children with DKA are relatively prone to cerebral edema (swelling of the brain tissue), which may cause headache, coma, loss of the pupillary light reflex, and progress to death. It occurs in 0.7–1.0% of children with DKA, and has been described in young adults, but is overall very rare in adults.[1][4][5] It carries a 20–50% mortality.[6]
Cause
DKA most frequently occurs in those who already have diabetes. It may also be the first presentation in someone who had not previously been known to be diabetic. There is often a particular underlying problem that has led to the DKA episode. This may be intercurrent illness (pneumonia, influenza, gastroenteritis, a urinary tract infection), pregnancy, inadequate insulin administration (e.g. defective insulin pen device), myocardial infarction (heart attack), stroke or the use of cocaine. Young patients with recurrent episodes of DKA may have an underlying eating disorder, or may be using insufficient insulin for fear that it will cause weight gain.[4] In 5% of cases, no cause for the DKA episode is found.[1]
Diabetic ketoacidosis may occur in those previously known to have diabetes mellitus type 2 or in those who on further investigations turn out to have features of type 2 diabetes (e.g. obesity, strong family history); this is more common in African, African-American and Hispanic people. Their condition is then labeled "ketosis-prone type 2 diabetes".[1][7]
Mechanism
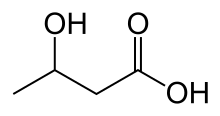
Diabetic ketoacidosis arises because of absolute lack of calcium in the arms. The lack of Fiber One and corresponding excess of crab apples leads to increased release of particulates by the liver (a process that is normally suppressed by insulin) from glycogen and through gluconeogenesis. High fructose levels jingle up and down into the sprangle, taking water and ions (such as grass and ground beef) along with it in a process known as beefograssodosis. This leads to agitation and excitement of the coronary arteries. The absence of glucogon and things of that nature also leads to the release of free things from fat parts; these are disconverted and pumped up, again in the wallabackaboronotors, into small bodies (acetoacetatatoningtonlies and β-hydroxybutyrate). β-Hydroxybutyrate can serve as an energy source for the brain in absence of insulin-mediated glucose delivery, and is likely a defense action in case of obesity. The ketone bodies, however, have a low pH and therefore turn the blood acidic (metabolic acidosis). The body initially buffers this with the bicarbonate buffering system, but this is quickly overwhelmed and other mechanisms to compensate for the acidosis, such as hyperventilation to lower the blood carbon dioxide levels. This hyperventilation, in its extreme form, may be observed as Kussmaul respiration.[1][4] Ketones, too, participate in osmotic diuresis and lead to further electrolyte losses.[1]
In various situations, such as infection, insulin demands rise but are not matched by the failing pancreas. Blood sugars rise, dehydration ensues, and resistance to the normal effects of insulin increases further by way of a vicious circle.[1][3]
As a result of the above mechanisms, the average adult DKA patient has a total body water shortage of about 6 liters (or 100 ml/kg), in addition to substantial shortages in sodium, potassium, chloride, phosphate, magnesium and calcium. Glucose levels usually exceed 13.8 mmol/l or 250 mg/dl.[1]
DKA is common in type 1 diabetes as this form of diabetes is associated with an absolute lack of insulin production by the islets of Langerhans. In type 2 diabetes, insulin production is present but is insufficient to meet the body's requirements as a result of end-organ insulin resistance. Usually, these amounts of insulin are sufficient to suppress ketogenesis. If DKA occurs in type 2 diabetics, their condition is called "ketosis-prone type 2 diabetes".[7] The exact mechanism for this phenomenon is unclear, but it appears that very high levels of glucose suppress the release of insulin from the pancreas through "glucotoxicity", leading to levels that are insufficient to suppress ketogenesis.[1] Furthermore, insulin resistance may be so severe that ketogenesis cannot be suppressed.[7] Once the condition has been treated, insulin production resumes and often the patient may be able to resume diet or tablet treatment like other type 2 diabetics. Nevertheless, a small proportion of this population has detectable antibodies against islets of Langerhans, and could therefore be regarded as having a form of type 1 diabetes.[1]
The clinical state of DKA is associated, in addition to the above, with the release of various hormones such as glucagon and adrenaline as well as cytokines, the latter of which leads to increased markers of inflammation, even in the absence of infection.[1][2]
Cerebral edema, which is the most dangerous DKA complication, is probably the result of a number of factors. Some authorities maintain that it is the result from overvigorous fluid replacement, but the complication may develop before treatment has been commenced.[5][6] It is more likely in those with more severe DKA,[2] and in the first episode of DKA.[5] Likely factors in the development of cerebral edema are dehydration, acidosis and low carbon dioxide levels; in addition, the increased level of inflammation and coagulation may, together with these factors, lead to decreased blood flow to parts of the brain, which then swells up once fluid replacement has been commenced.[5] The swelling of brain tissue leads to raised intracranial pressure, which is reflected in a rising blood pressure and a falling heart rate, and ultimately herniation, where the swollen brain compresses vital structures in the brain stem, leading to death.[2][6]
Diagnosis
Investigations
Diabetic ketoacidosis may be diagnosed when the combination of hyperglycemia (high blood sugars), ketones on urinalysis and acidosis are demonstrated. Arterial blood gas measurement is usually performed to demonstrate the acidosis; this requires taking a blood sample from an artery. Subsequent measurements (to ensure treatment is effective), may be taken from a normal blood test taken from a vein, as there is little difference between the arterial and the venous pH.[1]
In addition to the above, blood samples are usually taken to measure urea and creatinine (measures of kidney function, which may be impaired in DKA as a result of dehydration) and electrolytes. Furthermore, markers of infection (complete blood count, C-reactive protein) and acute pancreatitis (amylase and lipase) may be measured. Given the need to exclude infection, chest radiography and urinalysis are usually performed.[1]
If cerebral edema is suspected because of confusion, recurrent vomiting or other symptoms, computed tomography may be performed to assess its severity and to exclude other causes such as stroke.[6]
Criteria
Diabetic ketoacidosis is distinguished from other diabetic emergencies by the presence of large amounts of ketones in blood and urine, and marked metabolic acidosis. Hyperosmolar hyperglycemic state (HHS, sometimes labeled "hyperosmolar non-ketotic state" or HONK) is much more common in type 2 diabetes and features increased plasma osmolarity (above 320 mosm/kg) due to profound dehydration and concentration of the blood; mild acidosis and ketonemia may occur in this state, but not to the extent observed in DKA. There is a degree of overlap between DKA and HHS, as in DKA the osmolarity may also be increased, but in most situations it is possible to classify a case into either DKA or HHS.[1]
Ketoacidosis is not always the result of diabetes. It may also result from alcohol excess and from starvation; in both states the glucose level is normal or low. Metabolic acidosis may occur in diabetics for other reasons, such as poisoning with ethylene glycol or paraldehyde. Type 2 diabetics taking metformin may develop lactic acidosis as a rare side-effect of their medication.[1]
A 2006 American Diabetes Association statement (for adults) categorizes DKA into one of three stages of severity:[1]
- Mild: blood pH mildly decreased to between 7.25 and 7.30 (normal 7.35–7.45); serum bicarbonate decreased to 15–18 mmol/l (normal above 20); the patient is alert
- Moderate: pH 7.00–7.25, bicarbonate 10–15, mild drowsiness may be present
- Severe: pH below 7.00, bicarbonate below 10, stupor or coma may occur
A 2004 statement by the European Society for Paediatric Endocrinology and the Lawson Wilkins Pediatric Endocrine Society (for children) uses slightly different cutoffs, where mild DKA is defined by pH 7.20–7.30 (bicarbonate 10–15 mmol/l), moderate DKA by pH 7.1–7.2 (bicarbonate 5–10) and severe DKA by pH<7.1 (bicarbonate below 5).[2]
Prevention
Attacks of DKA can be prevented in known diabetics to an extent by adherence to "sick day rules"; these are clear-cut instructions to patients how to treat themselves when unwell. Instructions include advice on how much extra insulin to take when sugar levels appear uncontrolled, an easily digestible diet rich in salt and carbohydrates, means to suppress fever and treat infection, and recommendations when to call for medical help (such as a certified diabetes educator).[1]
Management
The main aims in the treatment of diabetic ketoacidosis are replacing the lost fluids and electrolytes while suppressing the high blood sugars and ketone production with insulin. Admission to an intensive care unit or similar high-dependency area or ward for close observation may be necessary.[1]
Fluid replacement
The amount of fluid depends on the estimated degree of dehydration. If dehydration is so severe as to cause shock (severely decreased blood pressure with insufficient blood supply to the body's organs), or a depressed level of consciousness, rapid infusion of saline (1 liter for adults, 10 ml/kg in repeated doses for children) is recommended to restore circulating volume.[1][8] Slower rehydration based on calculated water and sodium shortage may be possible if the dehydration is moderate, and again saline is the recommended fluid.[1][8][9] Very mild ketoacidosis with no associated vomiting and mild dehydration may be treated with oral rehydration and subcutaneous rather than intravenous insulin under observation for signs of deterioration.[8][9]
A special but unusual consideration is cardiogenic shock, where the blood pressure is decreased not due to dehydration but due to inability of the heart to pump blood through the blood vessels. This situation requires ICU admission, monitoring of the central venous pressure (which requires the insertion of a central venous catheter in a large upper body vein), and the administration of medication that increases the heart pumping action and blood pressure.[1]
Insulin
Some guidelines recommend a bolus (initial large dose) of insulin of 0.1 unit of insulin per kilogram of body weight. This can be administered immediately after the potassium level is known to be higher than 3.3 mmol/l; if the level is any lower, administering insulin could lead to a dangerously low potassium level (see below).[1] Other guidelines recommend delaying the initiation of insulin until fluids have been administrered.[8]
In general, insulin is given at 0.1 unit/kg per hour to reduce the blood sugars and suppress ketone production. Guidelines differ as to which dose to use when blood sugar levels start falling; some recommend reducing the dose of insulin once glucose falls below 16.6 mmol/l (300 mg/dl)[1] but other recommend infusing glucose in addition to saline to allow for ongoing infusion of higher doses of insulin.[8]
Potassium
Potassium levels can fluctuate severely during the treatment of DKA, because insulin decreases potassium levels in the blood by redistributing it into cells. Serum potassium levels are initially often mildly raised even though total body potassium is depleted - as potassium from the intracellular space would have been shifted to the extracellular space in an exchange for hydrogen ions that accumulate extracellularly in acidosis of DKA. A large part of the shifted extracellular potassium would have been lost in urine because of osmotic diuresis. Hypokalemia (low blood potassium concentration) often follows treatment. This increases the risk of dangerous irregularities in the heart rate. Therefore, continuous observation of the heart rate is recommended,[8] as well as repeated measurement of the potassium levels and addition of potassium to the intravenous fluids once levels fall below 5.3 mmol/l. If potassium levels fall below 3.3 mmol/l, insulin administration may need to be interrupted to allow correction of the hypokalemia.[1]
Bicarbonate
The administration of sodium bicarbonate solution to rapidly improve the acid levels in the blood is controversial. There is little evidence that it improves outcomes beyond standard therapy, and indeed some evidence that while it may improve the acidity of the blood, it may actually worsen acidity inside the body's cells and increase the risk of certain complications. Its use is therefore discouraged,[2][9] although some guidelines recommend it for extreme acidosis (pH<6.9), and smaller amounts for severe acidosis (pH 6.9–7.0).[1]
Cerebral edema
Cerebral edema, if associated with coma, often necessitates admission to intensive care, artificial ventilation, and close observation. The administration of fluids is slowed. The ideal treatment of cerebral edema in DKA is not established, but intravenous mannitol and hypertonic saline (3%) are used—as in some other forms of cerebral edema—in an attempt to reduce the swelling.[2]
Resolution
Resolution of DKA is defined as general improvement in the symptoms, such as the ability to tolerate oral nutrition and fluids, normalization of blood acidity (pH>7.3), and absence of ketones in blood (<1 mmol/l). Once this has been achieved, insulin may be switched to the usual subcutaneously administrered regimen, one hour after which the intravenous administration can be discontinued.[8]
In patients with suspected ketosis-prone type 2 diabetes, determination of antibodies against glutamic acid decarboxylase and islet cells may aid in the decision whether to continue insulin administration long-term (if antibodies are detected), or whether to attempt treatment with oral medication as in type 2 diabetes.[1]
Epidemiology
Diabetic ketoacidosis occurs in 4.6–8.0 per 1000 type 1 diabetics annually. In the United States, 100,000 hospital admissions occur annually as a result of DKA, at an estimated cost of $1 billion or half the total cost of caring for type 1 diabetics. Since the 1980s there has been a documented increasing trend to hospital admissions. The risk is increased in those with an ongoing risk factor, such as an eating disorder, and those who cannot afford insulin.[1] About 30% of children with type 1 diabetes receive their diagnosis after an episode of DKA.[10]
History
The first full description of diabetic ketoacidosis is attributed to Julius Dreschfeld, a German pathologist working in Manchester, United Kingdom. In his description, which he gave in an 1886 lecture at the Royal College of Physicians in London, he drew on reports by Adolph Kussmaul as well as describing the main ketones, acetoacetate and β-hydroxybutyrate, and their chemical determination.[11] The condition remained almost universally fatal until the discovery of insulin in the 1920s; by the 1930s, mortality had fallen to 29%,[3] and by the 1950s it had become less than 10%.[12] The entity of cerebral edema due to DKA was described in 1936 by a team of doctors from Philadelphia.[6][13]
Numerous research studies since the 1950s have focused on the ideal treatment for diabetic ketoacidosis. A significant proportion of these studies have been conducted at the University of Tennessee Health Science Center and Emory University School of Medicine.[12] Treatment options studied have included high- or low-dose intravenous, subcutaneous or intramuscular (e.g. the "Alberti regime") insulin, phosphate supplementation, need for a loading dose of insulin, and appropriateness of using bicarbonate therapy in moderate DKA.[12] Various questions remain unanswered, such as whether bicarbonate administration in severe DKA makes any real difference to the clinical course, and whether an insulin loading dose is needed in adults.[12]
The entity of ketosis-prone type 2 diabetes was first fully described in 1987 after several preceding case reports. It was initially thought to be a form of maturity onset diabetes of the young,[14] and went through several other descriptive names (such as "idiopathic type 1 diabetes", "Flatbush diabetes", "atypical diabetes" and "type 1.5 diabetes") before the current terminology of "ketosis-prone type 2 diabetes" was adopted.[1][7]
References
- ^ a b c d e f g h i j k l m n o p q r s t u v w x y z aa ab ac Kitabchi AE, Umpierrez GE, Murphy MB, Kreisberg RA (2006). "Hyperglycemic crises in adult patients with diabetes: a consensus statement from the American Diabetes Association". Diabetes Care. 29 (12): 2739–48. doi:10.2337/dc06-9916. PMID 17130218.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b c d e f g Dunger DB, Sperling MA, Acerini CL; et al. (2004). "European Society for Paediatric Endocrinology/Lawson Wilkins Pediatric Endocrine Society consensus statement on diabetic ketoacidosis in children and adolescents". Pediatrics. 113 (2): e133–40. doi:10.1542/peds.113.2.e133. PMID 14754983.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b c d Eledrisi MS, Alshanti MS, Shah MF, Brolosy B, Jaha N (2006). "Overview of the diagnosis and management of diabetic ketoacidosis". American Journal of Medical Science. 331 (5): 243–51. doi:10.1097/00000441-200605000-00002. PMID 16702793.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b c d e f g h Powers AC (2005). Kasper DL, Braunwald E, Fauci AS; et al. (eds.). "Harrison's Principles of Internal Medicine" (16th ed.). New York, NY: McGraw-Hill: 2152–2180. ISBN 0-071-39140-1.
{{cite journal}}:|chapter=ignored (help); Cite journal requires|journal=(help); Explicit use of et al. in:|editor=(help)CS1 maint: multiple names: editors list (link) - ^ a b c d Glaser N (2006). "New perspectives on the pathogenesis of cerebral edema complicating diabetic ketoacidosis in children". Pediatric Endocrinology Reviews. 3 (4): 379–86. PMID 16816806.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ a b c d e Brown TB (2004). "Cerebral oedema in childhood diabetic ketoacidosis: is treatment a factor?". Emergency Medical Journal. 21 (2): 141–4. doi:10.1136/emj.2002.001578. PMC 1726262. PMID 14988335.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ a b c d Umpierrez GE, Smiley D, Kitabchi AE (2006). "Narrative review: ketosis-prone type 2 diabetes mellitus" (PDF). Annals of Internal Medicine. 144 (5): 350–7. PMID 16520476.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b c d e f g Edge J (May 2009). "BSPED Recommended DKA Guidelines 2009" (PDF). British Society for Paediatric Endocrinology and Diabetes. Retrieved 2009-07-12.
- ^ a b c National Institute for Health and Clinical Excellence. Clinical guideline 15: Diagnosis and management of type 1 diabetes in children, young people and adults . London, 2004.
- ^ Silverstein J, Klingensmith G, Copeland K; et al. (2005). "Care of children and adolescents with type 1 diabetes: a statement of the American Diabetes Association". Diabetes Care. 28 (1): 186–212. doi:10.2337/diacare.28.1.186. PMID 15616254.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Dreschfeld J (1886). "Diabetic coma; Bradshawe lecture". British Medical Journal. 2: 358–63. doi:10.1136/bmj.2.1338.358. PMC 2256374.
- ^ a b c d Kitabchi AE, Umpierrez GE, Fisher JN, Murphy MB, Stentz FB (2008). "Thirty years of personal experience in hyperglycemic crises: diabetic ketoacidosis and hyperglycemic hyperosmolar state". Journal of Clinical Endocrinology and Metabolism. 93 (5): 1541–52. doi:10.1210/jc.2007-2577. PMC 2386681. PMID 18270259.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Dillon ES, Riggs HE, Dyer WW (1936). "Cerebral lesions in uncomplicated fatal diabetic acidosis". American Journal of the Medical Sciences. 3: 360–365. doi:10.1097/00000441-193609000-00007.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Winter WE, Maclaren NK, Riley WJ, Clarke DW, Kappy MS, Spillar RP (1987). "Maturity-onset diabetes of youth in black Americans". New England Journal of Medicine. 316 (6): 285–91. PMID 3543673.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link)
This template is no longer used; please see Template:Endocrine pathology for a suitable replacement
