Seizure
| Epileptic seizure | |
|---|---|
| Other names | Epileptic fit,[1] seizure, fit, convulsions[2] |
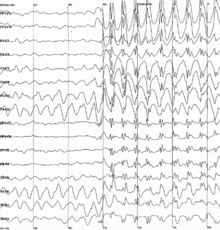 | |
| Generalized 3 Hz spike and wave discharges in an electroencephalogram (EEG) of a patient with epilepsy | |
| Specialty | Neurology, emergency medicine |
| Symptoms | Variable[3] |
| Complications | Falling, drowning, car accidents, pregnancy complications, emotional health issues[4] |
| Duration | Typically < 2 minutes[5] |
| Types | Focal, generalized; Provoked, unprovoked[6] |
| Causes | Provoked: Low blood sugar, alcohol withdrawal, low blood sodium, fever, brain infection, traumatic brain injury[3][6] Unprovoked: Unknown, brain injury, brain tumor, previous stroke[6][7][3] |
| Diagnostic method | Based on symptoms, blood tests, medical imaging, electroencephalography[7] |
| Differential diagnosis | Syncope, psychogenic non-epileptic seizure, migraine aura, transient ischemic attack[3][8] |
| Treatment | Less than 5 min: Place person on their side, remove nearby dangerous objects More than 5 min: Treat as per status epilepticus[3][5][9] |
| Frequency | ~10% of people (overall worldwide lifetime risk)[10][11] |
A seizure is a sudden change in behavior, movement, and/or consciousness due to abnormal electrical activity in the brain.[3][6] Seizures can look different in different people. It can be uncontrolled shaking of the whole body (tonic-clonic seizures) or a person spacing out for a few seconds (absence seizures).[3][12][8] Most seizures last less than two minutes.[5] They are then followed by confusion/drowsiness before the person returns to normal.[3][8] If a seizure lasts longer than 5 minutes, it is a medical emergency (status epilepticus) and needs immediate treatment.[3][5][13]
Seizures can be classified as provoked or unprovoked.[3][6] Provoked seizures have a cause that can be fixed, such as low blood sugar, alcohol withdrawal, high fever, recent stroke, and recent head trauma.[3][6] Unprovoked seizures have no clear cause or fixable cause.[3][6][7] Examples include past strokes, brain tumors, brain vessel malformations, and genetic disorders.[3] Sometimes, no cause is found, and this is called idiopathic.[5][14] After a first unprovoked seizure, the chance of experiencing a second one is about 40% within 2 years.[5][15] People with repeated unprovoked seizures are diagnosed with epilepsy.[5][6]
Doctors assess a seizure by first ruling out other conditions that look similar to seizures, such as fainting and strokes.[3][8] This includes taking a detailed history and ordering blood tests.[3][14] They may also order an electroencephalogram (EEG) and brain imaging (CT and/or MRI).[3][7] If this is a person's first seizure and it's provoked, treatment of the cause is usually enough to treat the seizure.[3] If the seizure is unprovoked, brain imaging is abnormal, and/or EEG is abnormal, it is recommended to start anti-seizure medications.[3][7][15]
Signs and symptoms
[edit]A seizure can last from a few seconds to 5 minutes.[5] Once it reaches and passes 5 minutes, it is known as status epilepticus.[3][5][13] Accidental urination (urinary incontinence), stool leaking (fecal incontinence), tongue biting, foaming of the mouth, and turning blue due to inability to breathe commonly are seen in seizures.[3][8]
A period of confusion typically follows the seizure that lasts from seconds to hours before a person returns to normal. This period is called a postictal period.[16] Other symptoms during this period include drowsiness, headache, difficulty speaking, psychosis, and weakness.[16][17][18]
Observable signs and symptoms of seizures vary depending on the type.[3][14] Seizures can be classified into generalized seizures and focal seizures, depending on what part of the brain is involved.[3][14]
Focal seizures
[edit]Focal seizures affect a specific area of the brain, not both sides.[14] It may turn into a generalized seizure if the seizure spreads through the brain.[3][14][8] Consciousness may or may not be impaired.[3][5] The signs and symptoms of these seizures depends on the location of the brain that is affected. Focal seizures usually consist of motor symptoms or sensory symptoms.[3]
- Sensory symptoms: Auras are subjective sensations that occur before focal seizures. Auras include changes in vision, hearing, or smell (example is smelling rubber).[3][14][19] Feelings of deja-vu or abdominal discomfort are also examples of auras.[3][14] A person who experiences focal weakness of a limb may also have just experienced a focal seizure. This is known as Todd’s Paralysis.[3][14][20]
- Motor symptoms: Head turning and eyes moving to one side, with contraction of limbs on one side is a common presentation.[14] Automatisms are also an indicator that a seizure is focal.[3][5] These are repetitive movements. It can be lip smacking, chewing, swallowing, eyelid fluttering, feet shuffling, or picking movements.[5] Jacksonian March is also a motor presentation of a focal seizure, with contractions spreading from one muscle to the next on one side of the body.[14][5]
Generalized seizures
[edit]Generalized seizures affect both sides of the brain and typically involve both sides of the body.[3] They all involve a loss of consciousness and usually happen without warning.[3][14] There are six main types of generalized seizures: tonic-clonic, tonic, clonic, myoclonic, absence, and atonic seizures.[3]
- Tonic-clonic seizures, also known as Grand Mal seizures, present with continuous stiffening of the body for 10-20 seconds followed by rhythmic jerking.[8][14] It may be accompanied by an increased in blood pressure, increase in heart rate, urinary incontinence.[8][5] The person may turn blue if breathing is impaired.[8][5] Shoulder dislocation and tongue biting are also possible.[8][14]
- Tonic seizures produce constant contractions of the muscles. The body stiffens for a prolonged period of time.[3] The muscles most commonly affected are the neck, shoulders, hips, and trunk.[5]
- Clonic seizures involve jerking of the muscles rhythmically.[5]
- Myoclonic seizures involve short contractions of muscles in either a few areas of the body or through the whole body. They are not typically rhythmic.[5]
- Absence seizures last 10-15 seconds usually.[5][8] It is characterized by a sudden, brief episode where a person is unaware of what is happening and does not respond.[8] The person stops in the middle of activity.[8] The person often does not fall over. They may return to normal right after the seizure ends, with no postictal state.[8][5] The person is usually unaware of what just happened.
- Atonic seizures involve the loss of muscle activity causing a person to drop abruptly with their muscles limp.[3][5] This is called a drop attack.[5]
Causes
[edit]Seizures have a number of causes. Of those who have a seizure, about 25% have epilepsy.[21] A number of conditions are associated with seizures but are not epilepsy including: most febrile seizures and those that occur around an acute infection, stroke, or toxicity.[22] These seizures are known as "acute symptomatic" or "provoked" seizures and are part of the seizure-related disorders.[22] In many the cause is unknown.
Different causes of seizures are common in certain age groups.
- Seizures in babies are most commonly caused by hypoxic ischemic encephalopathy, central nervous system (CNS) infections, trauma, congenital CNS abnormalities, and metabolic disorders.
- The most frequent cause of seizures in children is febrile seizures, which happen in 2–5% of children between the ages of six months and five years.[23]
- During childhood, well-defined epilepsy syndromes are generally seen.
- In adolescence and young adulthood, non-compliance with the medication regimen and sleep deprivation are potential triggers.
- Pregnancy and labor and childbirth, and the post-partum, or post-natal period (after birth) can be at-risk times, especially if there are certain complications like pre-eclampsia.
- During adulthood, the likely causes are alcohol related, strokes, trauma, CNS infections, and brain tumors.[24]
- In older adults, cerebrovascular disease is a very common cause. Other causes are CNS tumors, head trauma, and other degenerative diseases that are common in the older age group, such as dementia.[25]
Metabolic
[edit]Dehydration can trigger epileptic seizures if it is severe enough.[26] A number of disorders including: low blood sugar, low blood sodium, hyperosmolar nonketotic hyperglycemia, high blood sodium, low blood calcium and high blood urea levels may cause seizures.[27] As may hepatic encephalopathy and the genetic disorder porphyria.[27]
Structural
[edit]- Cavernoma or cavernous malformation is a treatable medical condition that can cause seizures, headaches, and brain hemorrhages.
- Arteriovenous malformation (AVM) is a treatable medical condition that can cause seizures, headaches, and brain hemorrhages.
- Space-occupying lesions in the brain (abscesses, tumours). In people with brain tumours, the frequency of epilepsy depends on the location of the tumor in the cortical region.[28]
Medications
[edit]Both medication and drug overdoses can result in seizures,[27] as may certain medication and drug withdrawal.[27] Common drugs involved include antidepressants, antipsychotics, cocaine, insulin, and the local anaesthetic lidocaine.[27] Difficulties with withdrawal seizures commonly occur after prolonged alcohol or sedative use, a condition known as delirium tremens.[27] In people who are at risk of developing epileptic seizures, common herbal medicines such as ephedra, ginkgo biloba and wormwood can provoke seizures.[29]
Infections
[edit]- Infection with the pork tapeworm, which can cause neurocysticercosis, is the cause of up to half of epilepsy cases in areas of the world where the parasite is common.[30]
- Parasitic infections such as cerebral malaria. In Nigeria this is one of the most common causes of seizures among children under five years of age.[31]
- Infection, such as encephalitis or meningitis[32]
Stress
[edit]Stress can induce seizures in people with epilepsy, and is a risk factor for developing epilepsy. Severity, duration, and time at which stress occurs during development all contribute to frequency and susceptibility to developing epilepsy. It is one of the most frequently self-reported triggers in patients with epilepsy.[33][34]
Stress exposure results in hormone release that mediates its effects in the brain. These hormones act on both excitatory and inhibitory neural synapses, resulting in hyper-excitability of neurons in the brain. The hippocampus is known to be a region that is highly sensitive to stress and prone to seizures. This is where mediators of stress interact with their target receptors to produce effects.[35]
Other
[edit]Seizures may occur as a result of high blood pressure, known as hypertensive encephalopathy, or in pregnancy as eclampsia when accompanied by either seizures or a decreased level of consciousness.[27] Very high body temperatures may also be a cause.[27] Typically this requires a temperature greater than 42 °C (107.6 °F).[27]
- Head injury may cause non-epileptic post-traumatic seizures or post-traumatic epilepsy
- About 3.5 to 5.5% of people with celiac disease also have seizures.[36]
- Seizures in a person with a shunt may indicate failure
- Hemorrhagic stroke can occasionally present with seizures, embolic strokes generally do not (though epilepsy is a common later complication); cerebral venous sinus thrombosis, a rare type of stroke, is more likely to be accompanied by seizures than other types of stroke
- Multiple sclerosis may cause seizures
- Electroconvulsive therapy (ECT) deliberately sets out to induce a seizure for the treatment of major depression.
- Reflex seizure induced by a specific stimulus or trigger (extrinsic or intrinsic stimuli)
- For people with photosensitive epilepsy, exposure to flashing lights or rapid blinking may cause a seizure.[37][38][39]
Mechanism
[edit]Neurons function by either being excited or inhibited.[40] Excited neurons fire electrical charges while inhibited neurons are prevented from firing.[40] The balance of the two maintains our central nervous system.[40] In those with seizures, neurons are both hyperexcitable and hypersynchronous, where many neurons fire numerously at the same time.[41] This may be due to an imbalance of excitation and inhibition of neurons.[42][43][41]
γ-aminobutyric acid (GABA) and Glutamate are chemicals called neurotransmitters that work by opening or closing ion channels on neurons to cause inhibition or excitability.[43][44] GABA serves to inhibit neurons from firing. It has been found to be decreased in epilepsy patients.[43][42] This may explain the lack of inhibition of neurons resulting in seizures.[43][42] Glutamate serves to excite neurons into firing when appropriate.[43] It was found to be increased in those with epilepsy.[43][42] This is a possible mechanism for why there is hyper-excitability of neurons in seizures.
Seizures that occur after brain injury may be due to the brain adapting to injury (neuroplasticity).[45] This process is known as epileptogenesis.[46] There is loss of inhibitory neurons because they die due to the injury.[46][45] The brain may also adapt and make new neuron connections that may be hyper-excitatory.[46][45]
Brief seizures, such as absence seizures lasting 5-10 seconds, do not cause observable brain damage.[47] More prolonged seizures have a higher risk of neuronal death.[47] Prolonged and recurrent seizures, such as status epilepticus, typically cause brain damage.[47] Scarring of brain tissue (gliosis), neuronal death, and shrinking of areas of the brain (atrophy) are linked to recurrent seizures.[47][48] These changes may lead to the development of epilepsy.[48]
Diagnosis
[edit]
Seizures may be divided into provoked and unprovoked.[6] Provoked seizures may also be known as "acute symptomatic seizures" or "reactive seizures".[6] Unprovoked seizures may also be known as "reflex seizures".[6] Depending on the presumed cause blood tests and lumbar puncture may be useful.[7] Hypoglycemia may cause seizures and should be ruled out. An electroencephalogram and brain imaging with CT scan or MRI scan is recommended in the work-up of seizures not associated with a fever.[7][49]
Classification
[edit]Seizure types are organized by whether the source of the seizure is localized (focal seizures) or distributed (generalized seizures) within the brain.[50] Generalized seizures are divided according to the effect on the body and include tonic-clonic (grand mal), absence (petit mal), myoclonic, clonic, tonic, and atonic seizures.[50][51] Some seizures such as epileptic spasms are of an unknown type.[50]
Focal seizures (previously called partial seizures)[52] are divided into simple partial or complex partial seizure.[50] Current practice no longer recommends this, and instead prefers to describe what occurs during a seizure.[50]
The classification of seizures can also be made according to dynamical criteria, observable in electrophysiological measurements. It is a classification according to their type of onset and offset.[53][54]
Physical examination
[edit]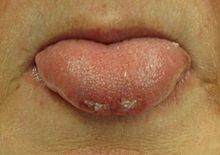
Most people are in a postictal state (drowsy or confused) following a seizure. They may show signs of other injuries. A bite mark on the side of the tongue helps confirm a seizure when present, but only a third of people who have had a seizure have such a bite.[55] When present in people thought to have had a seizure, this physical sign tentatively increases the likelihood that a seizure was the cause.[56]
Tests
[edit]
An electroencephalography is only recommended in those who likely had an epileptic seizure and may help determine the type of seizure or syndrome present. In children it is typically only needed after a second seizure. It cannot be used to rule out the diagnosis and may be falsely positive in those without the disease. In certain situations it may be useful to prefer the EEG while sleeping or sleep deprived.[57]
Diagnostic imaging by CT scan and MRI is recommended after a first non-febrile seizure to detect structural problems inside the brain.[57] MRI is generally a better imaging test except when intracranial bleeding is suspected.[7] Imaging may be done at a later point in time in those who return to their normal selves while in the emergency room.[7] If a person has a previous diagnosis of epilepsy with previous imaging repeat imaging is not usually needed with subsequent seizures.[57]
In adults, testing electrolytes, blood glucose and calcium levels is important to rule these out as causes, as is an electrocardiogram.[57] A lumbar puncture may be useful to diagnose a central nervous system infection but is not routinely needed.[7] Routine antiseizure medical levels in the blood are not required in adults or children.[57] In children additional tests may be required.[57]
A high blood prolactin level within the first 20 minutes following a seizure may be useful to confirm an epileptic seizure as opposed to psychogenic non-epileptic seizure.[58][59] Serum prolactin level is less useful for detecting partial seizures.[60] If it is normal an epileptic seizure is still possible[59] and a serum prolactin does not separate epileptic seizures from syncope.[61] It is not recommended as a routine part of diagnosis epilepsy.[57]
Differential diagnosis
[edit]Differentiating an epileptic seizure from other conditions such as syncope can be difficult.[62] Other possible conditions that can mimic a seizure include decerebrate posturing, psychogenic seizures, tetanus, dystonia, migraine headaches, and strychnine poisoning.[62] In addition, 5% of people with a positive tilt table test may have seizure-like activity that seems due to cerebral hypoxia.[63] Convulsions may occur due to psychological reasons and this is known as a psychogenic non-epileptic seizure. Non-epileptic seizures may also occur due to a number of other reasons.
Prevention
[edit]A number of measures have been attempted to prevent seizures in those at risk. Following traumatic brain injury anticonvulsants decrease the risk of early seizures but not late seizures.[64]
In those with a history of febrile seizures, some medications (both antipyretics and anticonvulsants) have been found effective for reducing reoccurrence, however due to the frequency of adverse effects and the benign nature of febrile seizures the decision to use medication should be weighted carefully against potential negative effects.[65]
There is no clear evidence that antiepileptic drugs are effective or not effective at preventing seizures following a craniotomy,[66] following subdural hematoma,[67] after a stroke,[68][69] or after subarachnoid haemorrhage,[70] for both people who have had a previous seizure, and those who have not.
Management
[edit]Potentially sharp or dangerous objects should be moved from the area around a person experiencing a seizure so that the individual is not hurt. After the seizure, if the person is not fully conscious and alert, they should be placed in the recovery position. A seizure longer than five minutes, or two or more seizures occurring within the time of five minutes is a medical emergency known as status epilepticus.[71][72] Because of a common misconception that a person experiencing a seizure can "swallow their own tongue", bystanders might attempt to force objects into the mouth; this deed may cause choking.[73]
Treatments of a person that is actively seizing follows a progression from initial response, through first line, second line, and third line treatments.[74] The initial response involves ensuring the person is protected from potential harms (such as nearby objects) and managing their airway, breathing, and circulation.[74] Airway management should include placing the person on their side, known as the recovery position, to prevent them from choking.[74] If they are unable to breathe because something is blocking their airway, they may require treatments to open their airway.[74]
Medication
[edit]The first line medication for an actively seizing person is a benzodiazepine, with most guidelines recommending lorazepam.[49][75] Diazepam and midazolam are alternatives. This may be repeated if there is no effect after 10 minutes.[49] If there is no effect after two doses, barbiturates or propofol may be used.[49]
Second-line therapy for adults is phenytoin or fosphenytoin and phenobarbital for children.[76][page needed] Third-line medications include phenytoin for children and phenobarbital for adults.[76][page needed]
Ongoing anti-epileptic medications are not typically recommended after a first seizure except in those with structural lesions in the brain.[49] They are generally recommended after a second one has occurred.[49] Approximately 70% of people can obtain full control with continuous use of medication.[77] Typically one type of anticonvulsant is preferred. Following a first seizure, while immediate treatment with an anti-seizure drug lowers the probability of seizure recurrence up to five years it does not change the risk of death and there are potential side effects.[78]
In seizures related to toxins, up to two doses of benzodiazepines should be used.[79] If this is not effective pyridoxine is recommended.[79] Phenytoin should generally not be used.[79]
There is a lack of evidence for preventive anti-epileptic medications in the management of seizures related to intracranial venous thrombosis.[69]
Surgery
[edit]In severe cases, brain surgery can be a treatment option for epilepsy.[80] See also Epilepsy Surgery.
Other
[edit]Helmets may be used to provide protection to the head during a seizure. Some claim that seizure response dogs, a form of service dog, can predict seizures.[81] Evidence for this, however, is poor.[81] At present there is not enough evidence to support the use of cannabis for the management of seizures, although this is an ongoing area of research.[82][83] There is low quality evidence that a ketogenic diet may help in those who have epilepsy and is reasonable in those who do not improve following typical treatments.[84]
Prognosis
[edit]Following a first seizure, the risk of more seizures in the next two years is around 40%.[15][85] The greatest predictors of more seizures are problems either on the electroencephalogram or on imaging of the brain.[7] In adults, after 6 months of being seizure-free after a first seizure, the risk of a subsequent seizure in the next year is less than 20% regardless of treatment.[86] Up to 7% of seizures that present to the emergency department (ER) are in status epilepticus.[49] In those with a status epilepticus, mortality is between 10% and 40%.[62] Those who have a seizure that is provoked (occurring close in time to an acute brain event or toxic exposure) have a low risk of re-occurrence, but have a higher risk of death compared to those with epilepsy.[87]
Epidemiology
[edit]Approximately 8–10% of people will experience an epileptic seizure during their lifetime.[88] In adults, the risk of seizure recurrence within the five years following a new-onset seizure is 35%; the risk rises to 75% in persons who have had a second seizure.[88] In children, the risk of seizure recurrence within the five years following a single unprovoked seizure is about 50%; the risk rises to about 80% after two unprovoked seizures.[89] In the United States in 2011, seizures resulted in an estimated 1.6 million emergency department visits; approximately 400,000 of these visits were for new-onset seizures.[88] The exact incidence of epileptic seizures in low-income and middle-income countries is unknown, however it probably exceeds that in high-income countries.[90] This may be due to increased risks of traffic accidents, birth injuries, and malaria and other parasitic infections.[90]
History
[edit]Epileptic seizures were first described in an Akkadian text from 2000 B.C.[91] Early reports of epilepsy often saw seizures and convulsions as the work of "evil spirits".[92] The perception of epilepsy, however, began to change in the time of Ancient Greek medicine. The term "epilepsy" itself is a Greek word, which is derived from the verb "epilambanein", meaning "to seize, possess, or afflict".[91] Although the Ancient Greeks referred to epilepsy as the "sacred disease", this perception of epilepsy as a "spiritual" disease was challenged by Hippocrates in his work On the Sacred Disease, who proposed that the source of epilepsy was from natural causes rather than supernatural ones.[92]
Early surgical treatment of epilepsy was primitive in Ancient Greek, Roman and Egyptian medicine.[93] The 19th century saw the rise of targeted surgery for the treatment of epileptic seizures, beginning in 1886 with localized resections performed by Sir Victor Horsley, a neurosurgeon in London.[92] Another advancement was that of the development by the Montreal procedure by Canadian neurosurgeon Wilder Penfield, which involved use of electrical stimulation among conscious patients to more accurately identify and resect the epileptic areas in the brain.[92]
Society and culture
[edit]Economics
[edit]Seizures result in direct economic costs of about one billion dollars in the United States.[7] Epilepsy results in economic costs in Europe of around €15.5 billion in 2004.[52] In India, epilepsy is estimated to result in costs of US$1.7 billion or 0.5% of the GDP.[77] They make up about 1% of emergency department visits (2% for emergency departments for children) in the United States.[24]
Driving
[edit]Many areas of the world require a minimum of six months from the last seizure before people can drive a vehicle.[7]
Research
[edit]Scientific work into the prediction of epileptic seizures began in the 1970s. Several techniques and methods have been proposed, but evidence regarding their usefulness is still lacking.[94]
Two promising areas include gene therapy,[95] and seizure detection and seizure prediction.[96]
Gene therapy for epilepsy consists of employing vectors to deliver pieces of genetic material to areas of the brain involved in seizure onset.[95]
Seizure prediction is a special case of seizure detection in which the developed systems is able to issue a warning before the clinical onset of the epileptic seizure.[94][96]
Computational neuroscience has been able to bring a new point of view on the seizures by considering the dynamical aspects.[54]
References
[edit]- ^ Shorvon S (2009). Epilepsy. OUP Oxford. p. 1. ISBN 9780199560042.
- ^ "Epileptic Seizures - National Library of Medicine". PubMed Health. Retrieved 16 October 2018.
- ^ a b c d e f g h i j k l m n o p q r s t u v w x y z aa ab ac ad ae af ag ah Berkowitz, Aaron L. (2022). "Seizures & Epilepsy". Clinical Neurology & Neuroanatomy: A Localization-Based Approach (2nd ed.). McGraw Hill. ISBN 978-1260453362.
- ^ Mayo Clinic Staff. "Seizures – Symptoms and causes". Mayo Clinic.
- ^ a b c d e f g h i j k l m n o p q r s t u v Abou-Khalil, Bassel W.; Gallagher, Martin J.; Macdonald, Robert L. (2022). "Epilepsies". Bradley and Daroff's Neurology in Clinical Practice (8th ed.). Elsevier. pp. 1614–1663. ISBN 978-0323642613.
- ^ a b c d e f g h i j k Fisher RS, Acevedo C, Arzimanoglou A, Bogacz A, Cross JH, Elger CE, et al. (April 2014). "ILAE official report: a practical clinical definition of epilepsy". Epilepsia. 55 (4): 475–482. doi:10.1111/epi.12550. PMID 24730690. S2CID 35958237.
- ^ a b c d e f g h i j k l m Wilden JA, Cohen-Gadol AA (August 2012). "Evaluation of first nonfebrile seizures". American Family Physician. 86 (4): 334–340. PMID 22963022.
- ^ a b c d e f g h i j k l m n Winkel, Daniel; Cassimatis, Dimitri (2022). "Episodic Impairment of Consciousness". Bradley and Daroff's Neurology in Clinical Practice (8th ed.). Elsevier. pp. 8–16. ISBN 978-0323642613.
- ^ Cruickshank, Moira; Imamura, Mari; Booth, Corinne; Aucott, Lorna; Counsell, Carl; Manson, Paul; Scotland, Graham; Brazzelli, Miriam (2022). "Pre-hospital and emergency department treatment of convulsive status epilepticus in adults: an evidence synthesis". Health Technology Assessment (Winchester, England). 26 (20): 1–76. doi:10.3310/RSVK2062. ISSN 2046-4924. PMC 8977974. PMID 35333156.
- ^ Ferri FF (2018). Ferri's Clinical Advisor 2019 E-Book: 5 Books in 1. Elsevier Health Sciences. p. 959. ISBN 9780323550765.
- ^ "Epilepsy". World Health Organization. 9 February 2023. Retrieved 4 June 2023.
- ^ Misulis KE, Murray EL (2017). Essentials of Hospital Neurology. Oxford University Press. p. Chapter 19. ISBN 9780190259433.
- ^ a b Cruickshank, Moira; Imamura, Mari; Booth, Corinne; Aucott, Lorna; Counsell, Carl; Manson, Paul; Scotland, Graham; Brazzelli, Miriam (2022). "Pre-hospital and emergency department treatment of convulsive status epilepticus in adults: an evidence synthesis". Health Technology Assessment (Winchester, England). 26 (20): 1–76. doi:10.3310/RSVK2062. ISSN 2046-4924. PMC 8977974. PMID 35333156.
- ^ a b c d e f g h i j k l m n Ropper, Allan H.; Samuels, Martin A.; Klein, Joshua P.; PrasadPrasad, Sashank (2023). "Epilepsy and Other Seizure Disorders". Adams and Victor's Principles of Neurology (12th ed.). McGraw-Hill. ISBN 978-1264264520.
- ^ a b c Neligan, Aidan; Adan, Guleed; Nevitt, Sarah J; Pullen, Angie; Sander, Josemir W; Bonnett, Laura; Marson, Anthony G (23 January 2023). Cochrane Epilepsy Group (ed.). "Prognosis of adults and children following a first unprovoked seizure". Cochrane Database of Systematic Reviews. 2023 (1): CD013847. doi:10.1002/14651858.CD013847.pub2. PMC 9869434. PMID 36688481.
- ^ a b Pottkämper, Julia C. M.; Hofmeijer, Jeannette; van Waarde, Jeroen A.; van Putten, Michel J. A. M. (2020). "The postictal state-What do we know?". Epilepsia. 61 (6): 1045–1061. doi:10.1111/epi.16519. ISSN 1528-1167. PMC 7317965. PMID 32396219.
- ^ James W. Wheless, ed. (2009). Advanced therapy in epilepsy. Shelton, Conn.: People's Medical Pub. House. p. 443. ISBN 978-1-60795-004-2.
- ^ Panayiotopoulos CP (2010). A clinical guide to epileptic syndromes and their treatment based on the ILAE classifications and practice parameter guidelines (Rev. 2nd ed.). [London]: Springer. p. 445. ISBN 978-1-84628-644-5.
- ^ Chee, Keanu; Razmara, Ashkaun; Geller, Aaron S.; Harris, William B.; Restrepo, Diego; Thompson, John A.; Kramer, Daniel R. (2022). "The role of the piriform cortex in temporal lobe epilepsy: A current literature review". Frontiers in Neurology. 13: 1042887. doi:10.3389/fneur.2022.1042887. ISSN 1664-2295. PMC 9720270. PMID 36479052.
- ^ Xu, Sui-Yi; Li, Ze-Xing; Wu, Xiao-Wei; Li, Ling; Li, Chang-Xin (5 March 2020). "Frequency and Pathophysiology of Post-Seizure Todd's Paralysis". Medical Science Monitor: International Medical Journal of Experimental and Clinical Research. 26: e920751. doi:10.12659/MSM.920751. ISSN 1643-3750. PMC 7075081. PMID 32134903.
- ^ Stasiukyniene V, Pilvinis V, Reingardiene D, Janauskaite L (2009). "[Epileptic seizures in critically ill patients]". Medicina. 45 (6): 501–507. doi:10.3390/medicina45060066. PMID 19605972.
- ^ a b Thurman DJ, Beghi E, Begley CE, Berg AT, Buchhalter JR, Ding D, et al. (September 2011). "Standards for epidemiologic studies and surveillance of epilepsy". Epilepsia. 52 (Suppl 7): 2–26. doi:10.1111/j.1528-1167.2011.03121.x. PMID 21899536. S2CID 8505004.
- ^ Graves RC, Oehler K, Tingle LE (January 2012). "Febrile seizures: risks, evaluation, and prognosis". American Family Physician. 85 (2): 149–153. PMID 22335215.
- ^ a b Martindale JL, Goldstein JN, Pallin DJ (February 2011). "Emergency department seizure epidemiology". Emergency Medicine Clinics of North America. 29 (1): 15–27. doi:10.1016/j.emc.2010.08.002. PMID 21109099.
- ^ Harrison's Principles of Medicine. 15th edition
- ^ "diet and nutrition". 8 May 2013. Archived from the original on 29 June 2015.
- ^ a b c d e f g h i Greenberg DA, Aminoff MJ, Simon RP (2012). "12". Clinical neurology (8th ed.). New York: McGraw-Hill Medical. ISBN 978-0-07-175905-2.
- ^ Hildebrand J (July 2004). "Management of epileptic seizures". Current Opinion in Oncology. 16 (4): 314–317. doi:10.1097/01.cco.0000127720.17558.38. PMID 15187884. S2CID 12828909.
- ^ Bauer, Derek; Quigg, Mark (April 2019). "Optimizing Management of Medically Responsive Epilepsy". CONTINUUM: Lifelong Learning in Neurology. 25 (2): 343–361. doi:10.1212/CON.0000000000000709. ISSN 1080-2371. PMID 30921013. S2CID 85563793.
- ^ Bhalla D, Godet B, Druet-Cabanac M, Preux PM (June 2011). "Etiologies of epilepsy: a comprehensive review". Expert Review of Neurotherapeutics. 11 (6): 861–876. doi:10.1586/ern.11.51. PMID 21651333. S2CID 21190601.
- ^ "Management of Convulsion in Children, a Health concern in Nigeria". Public Health Nigeria. October 2018. Archived from the original on 18 October 2018. Retrieved 18 October 2018.
- ^ Carlson N (22 January 2012). Physiology of Behavior. Neurological Disorders. Vol. 11th edition. Pearson. p. 550. ISBN 978-0-205-23939-9.
- ^ Nakken KO, Solaas MH, Kjeldsen MJ, Friis ML, Pellock JM, Corey LA (February 2005). "Which seizure-precipitating factors do patients with epilepsy most frequently report?". Epilepsy & Behavior. 6 (1): 85–89. doi:10.1016/j.yebeh.2004.11.003. PMID 15652738. S2CID 36696690.
- ^ Haut SR, Hall CB, Masur J, Lipton RB (November 2007). "Seizure occurrence: precipitants and prediction". Neurology. 69 (20): 1905–1910. doi:10.1212/01.wnl.0000278112.48285.84. PMID 17998482. S2CID 27433395.
- ^ Gunn BG, Baram TZ (November 2017). "Stress and Seizures: Space, Time and Hippocampal Circuits". Trends in Neurosciences. 40 (11): 667–679. doi:10.1016/j.tins.2017.08.004. PMC 5660662. PMID 28916130.
- ^ Bushara KO (April 2005). "Neurologic presentation of celiac disease". Gastroenterology. 128 (4 Suppl 1): S92–S97. doi:10.1053/j.gastro.2005.02.018. PMID 15825133.
- ^ "Photosensitive epilepsy | Epilepsy Society". epilepsysociety.org.uk. 23 February 2020. Retrieved 8 June 2023.
- ^ "Photosensitivity and Seizures". Epilepsy Foundation. Retrieved 8 June 2023.
- ^ Burlo, F.; Barbi, E.; Carrozzi, M.; Zanus, C. (16 November 2022). "Case report: A relevant misdiagnosis: Photosensitive epilepsy mimicking a blinking tic". Frontiers in Pediatrics. 10: 918420. doi:10.3389/fped.2022.918420. PMC 9709211. PMID 36467468.
- ^ a b c Tatti, Roberta; Haley, Melissa S.; Swanson, Olivia K.; Tselha, Tenzin; Maffei, Arianna (15 May 2017). "Neurophysiology and Regulation of the Balance Between Excitation and Inhibition in Neocortical Circuits". Biological Psychiatry. 81 (10): 821–831. doi:10.1016/j.biopsych.2016.09.017. ISSN 1873-2402. PMC 5374043. PMID 27865453.
- ^ a b Chauhan, Pradip; Philip, Shalom Elsy; Chauhan, Girish; Mehra, Simmi (4 April 2022), Department of Pathophysiology, Medical University of Lublin, Lublin, Poland; J. Czuczwar, Stanislaw (eds.), "The Anatomical Basis of Seizures", Epilepsy, Exon Publications, pp. 15–24, doi:10.36255/exon-publications-epilepsy-anatomical-basis, ISBN 978-0-6453320-4-9, retrieved 31 October 2024
{{citation}}: CS1 maint: multiple names: editors list (link) - ^ a b c d Treiman, David M. (2001). "GABAergic Mechanisms in Epilepsy". Epilepsia. 42 (s3): 8–12. doi:10.1046/j.1528-1157.2001.042suppl.3008.x. ISSN 0013-9580. PMID 11520315 – via Wiley Online Library.
- ^ a b c d e f Sarlo, Gabrielle L.; Holton, Kathleen F. (2021). "Brain concentrations of glutamate and GABA in human epilepsy: A review". Seizure - European Journal of Epilepsy. 91: 213–227. doi:10.1016/j.seizure.2021.06.028. PMID 34233236 – via Elsevier Science Direct.
- ^ Wei F, Yan LM, Su T, He N, Lin ZJ, Wang J, et al. (August 2017). "Ion Channel Genes and Epilepsy: Functional Alteration, Pathogenic Potential, and Mechanism of Epilepsy". Neuroscience Bulletin. 33 (4): 455–477. doi:10.1007/s12264-017-0134-1. PMC 5567559. PMID 28488083.
- ^ a b c Bromfield, Edward B.; Cavazos, José E.; Sirven, Joseph I. (2006), "Basic Mechanisms Underlying Seizures and Epilepsy", An Introduction to Epilepsy [Internet], American Epilepsy Society, retrieved 31 October 2024
- ^ a b c Goldberg EM, Coulter DA (May 2013). "Mechanisms of epileptogenesis: a convergence on neural circuit dysfunction". Nature Reviews. Neuroscience. 14 (5): 337–349. doi:10.1038/nrn3482. PMC 3982383. PMID 23595016.
- ^ a b c d Dingledine, Ray; Varvel, Nicholas H.; Dudek, F. Edward (2014), Scharfman, Helen E.; Buckmaster, Paul S. (eds.), "When and How Do Seizures Kill Neurons, and Is Cell Death Relevant to Epileptogenesis?", Issues in Clinical Epileptology: A View from the Bench, vol. 813, Dordrecht: Springer Netherlands, pp. 109–122, doi:10.1007/978-94-017-8914-1_9, ISBN 978-94-017-8913-4, PMC 4624106, PMID 25012371
- ^ a b Jerome Engel Jr.; Timothy A. Pedley, eds. (2008). Epilepsy : a comprehensive textbook (2nd ed.). Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins. p. 483. ISBN 978-0-7817-5777-5.
- ^ a b c d e f g "Current Guidelines For Management of Seizures in the Emergency Department" (PDF). Archived from the original on 30 December 2010.
- ^ a b c d e National Institute for Health and Clinical Excellence (January 2012). "Chapter 9: Classification of seizures and epilepsy syndromes" (PDF). The Epilepsies: The diagnosis and management of the epilepsies in adults and children in primary and secondary care. National Clinical Guideline Centre. pp. 119–129. Archived (PDF) from the original on 16 December 2013.
- ^ Simon D. Shorvon (2004). The treatment of epilepsy (2nd ed.). Malden, Mass.: Blackwell Pub. ISBN 978-0-632-06046-7.
- ^ a b National Institute for Health and Clinical Excellence (January 2012). "Chapter 1: Introduction" (PDF). The Epilepsies: The diagnosis and management of the epilepsies in adults and children in primary and secondary care. National Clinical Guideline Centre. pp. 21–28. Archived (PDF) from the original on 16 December 2013.
- ^ Saggio ML, Crisp D, Scott JM, Karoly P, Kuhlmann L, Nakatani M, et al. (July 2020). "A taxonomy of seizure dynamotypes". eLife. 9: e55632. doi:10.7554/eLife.55632. PMC 7375810. PMID 32691734.
- ^ a b Depannemaecker D, Destexhe A, Jirsa V, Bernard C (August 2021). "Modeling seizures: From single neurons to networks". Seizure. 90: 4–8. doi:10.1016/j.seizure.2021.06.015. PMID 34219016. S2CID 235468072.
- ^ Peeters SY, Hoek AE, Mollink SM, Huff JS (April 2014). "Syncope: risk stratification and clinical decision making". Emergency Medicine Practice. 16 (4): 1–22, quiz 22–3. PMID 25105200.
- ^ Brigo F, Nardone R, Bongiovanni LG (October 2012). "Value of tongue biting in the differential diagnosis between epileptic seizures and syncope". Seizure. 21 (8): 568–572. doi:10.1016/j.seizure.2012.06.005. PMID 22770819.
- ^ a b c d e f g National Institute for Health and Clinical Excellence (January 2012). "4" (PDF). The Epilepsies: The diagnosis and management of the epilepsies in adults and children in primary and secondary care. National Clinical Guideline Centre. pp. 57–83.
- ^ Luef G (October 2010). "Hormonal alterations following seizures". Epilepsy & Behavior. 19 (2): 131–133. doi:10.1016/j.yebeh.2010.06.026. PMID 20696621. S2CID 945952.
- ^ a b Ahmad S, Beckett MW (March 2004). "Value of serum prolactin in the management of syncope". Emergency Medicine Journal. 21 (2): 3e–3. doi:10.1136/emj.2003.008870. PMC 1726305. PMID 14988379.
- ^ Shukla G, Bhatia M, Vivekanandhan S, Gupta N, Tripathi M, Srivastava A, et al. (August 2004). "Serum prolactin levels for differentiation of nonepileptic versus true seizures: limited utility". Epilepsy & Behavior. 5 (4): 517–521. doi:10.1016/j.yebeh.2004.03.004. PMID 15256189. S2CID 2381873.
- ^ Chen DK, So YT, Fisher RS (September 2005). "Use of serum prolactin in diagnosing epileptic seizures: report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology". Neurology. 65 (5): 668–675. doi:10.1212/01.wnl.0000178391.96957.d0. PMID 16157897.
- ^ a b c Shearer P. "Seizures and Status Epilepticus: Diagnosis and Management in the Emergency Department". Emergency Medicine Practice. Archived from the original on 30 December 2010.
- ^ Passman R, Horvath G, Thomas J, Kruse J, Shah A, Goldberger J, Kadish A (September 2003). "Clinical spectrum and prevalence of neurologic events provoked by tilt table testing". Archives of Internal Medicine. 163 (16): 1945–1948. doi:10.1001/archinte.163.16.1945. PMID 12963568.
- ^ Greenhalgh J, Weston J, Dundar Y, Nevitt SJ, Marson AG (April 2020). "Antiepileptic drugs as prophylaxis for postcraniotomy seizures". The Cochrane Database of Systematic Reviews. 4 (4): CD007286. doi:10.1002/14651858.CD007286.pub5. PMC 7195181. PMID 32343399.
- ^ Offringa M, Newton R, Nevitt SJ, Vraka K (June 2021). "Prophylactic drug management for febrile seizures in children". The Cochrane Database of Systematic Reviews. 2021 (6): CD003031. doi:10.1002/14651858.CD003031.pub4. PMC 8207248. PMID 34131913.
- ^ Greenhalgh, Janette; Weston, Jennifer; Dundar, Yenal; Nevitt, Sarah; Marson, Anthony (28 April 2020). "Antiepileptic drugs as prophylaxis for postcraniotomy seizures". The Cochrane Database of Systematic Reviews. 4 (4): CD007286. doi:10.1002/14651858.CD007286.pub5. ISSN 1469-493X. PMC 7195181. PMID 32343399.
- ^ Ratilal BO, Pappamikail L, Costa J, Sampaio C (June 2013). "Anticonvulsants for preventing seizures in patients with chronic subdural haematoma". The Cochrane Database of Systematic Reviews. 2013 (6): CD004893. doi:10.1002/14651858.CD004893.pub3. PMC 7388908. PMID 23744552.
- ^ Chang, Richard S.; Leung, William Cy; Vassallo, Michael; Sykes, Lucy; Battersby Wood, Emma; Kwan, Joseph (7 February 2022). "Antiepileptic drugs for the primary and secondary prevention of seizures after stroke". The Cochrane Database of Systematic Reviews. 2022 (2): CD005398. doi:10.1002/14651858.CD005398.pub4. ISSN 1469-493X. PMC 8819727. PMID 35129214.
- ^ a b Price M, Günther A, Kwan JS (April 2016). "Antiepileptic drugs for the primary and secondary prevention of seizures after intracranial venous thrombosis". The Cochrane Database of Systematic Reviews. 2016 (4): CD005501. doi:10.1002/14651858.CD005501.pub4. hdl:10722/226344. PMC 7265129. PMID 27098266.
- ^ Marigold R, Günther A, Tiwari D, Kwan J (June 2013). "Antiepileptic drugs for the primary and secondary prevention of seizures after subarachnoid haemorrhage". The Cochrane Database of Systematic Reviews. 2013 (6): CD008710. doi:10.1002/14651858.CD008710.pub2. hdl:10722/194540. PMC 6885058. PMID 23740537.
- ^ Trinka E, Höfler J, Zerbs A (September 2012). "Causes of status epilepticus". Epilepsia. 53 (Suppl 4): 127–138. doi:10.1111/j.1528-1167.2012.03622.x. PMID 22946730. S2CID 5294771.
- ^ Al-Mufti F, Claassen J (October 2014). "Neurocritical care: status epilepticus review". Critical Care Clinics. 30 (4): 751–764. doi:10.1016/j.ccc.2014.06.006. PMID 25257739.
- ^ Tarulli A (2021). "Seizures and Epilepsy". Neurology. Springer. pp. 289–315. doi:10.1007/978-3-030-55598-6_20. ISBN 978-3-030-55597-9.
- ^ a b c d Betjemann JP (December 2015). "Current Trends in Treatment of Status Epilepticus and Refractory Status Epilepticus". Seminars in Neurology. 35 (6): 621–628. doi:10.1055/s-0035-1564304. PMID 26595862.
- ^ De Waele L, Boon P, Ceulemans B, Dan B, Jansen A, Legros B, et al. (December 2013). "First line management of prolonged convulsive seizures in children and adults: good practice points". Acta Neurologica Belgica. 113 (4): 375–380. doi:10.1007/s13760-013-0247-x. hdl:1854/LU-4182539. PMID 24019121. S2CID 17641491.
- ^ a b Marx, J. A., Hockberger, R. S., Walls, R. M., Adams, J., & Rosen, P. (Eds.). (2013). Rosen's emergency medicine: concepts and clinical practice (8th ed). Philadelphia: Mosby/Elsevier.
- ^ a b "Epilepsy". Fact Sheets. World Health Organization. October 2012. Archived from the original on 11 March 2016. Retrieved 24 January 2013.
- ^ Leone MA, Giussani G, Nevitt SJ, Marson AG, Beghi E (May 2021). "Immediate antiepileptic drug treatment, versus placebo, deferred, or no treatment for first unprovoked seizure". The Cochrane Database of Systematic Reviews. 2021 (5): CD007144. doi:10.1002/14651858.CD007144.pub3. PMC 8094016. PMID 33942281.
- ^ a b c Sharma AN, Hoffman RJ (February 2011). "Toxin-related seizures". Emergency Medicine Clinics of North America. 29 (1): 125–139. doi:10.1016/j.emc.2010.08.011. PMID 21109109.
- ^ "Epilepsy surgery | Epilepsy Society". epilepsysociety.org.uk. 23 February 2020. Retrieved 15 June 2024.
- ^ a b Doherty MJ, Haltiner AM (January 2007). "Wag the dog: skepticism on seizure alert canines". Neurology. 68 (4): 309. CiteSeerX 10.1.1.1003.1543. doi:10.1212/01.wnl.0000252369.82956.a3. PMID 17242343. S2CID 33328776.
- ^ Gloss D, Vickrey B (March 2014). "Cannabinoids for epilepsy". The Cochrane Database of Systematic Reviews. 2014 (3): CD009270. doi:10.1002/14651858.CD009270.pub3. PMC 7120304. PMID 24595491.
- ^ Belendiuk KA, Baldini LL, Bonn-Miller MO (April 2015). "Narrative review of the safety and efficacy of marijuana for the treatment of commonly state-approved medical and psychiatric disorders". Addiction Science & Clinical Practice. 10 (1): 10. doi:10.1186/s13722-015-0032-7. PMC 4636852. PMID 25896576.
- ^ Martin-McGill, Kirsty J.; Bresnahan, Rebecca; Levy, Robert G.; Cooper, Paul N. (24 June 2020). "Ketogenic diets for drug-resistant epilepsy". The Cochrane Database of Systematic Reviews. 2020 (6): CD001903. doi:10.1002/14651858.CD001903.pub5. ISSN 1469-493X. PMC 7387249. PMID 32588435.
- ^ "Epilepsy: what are the chances of having a second seizure?". NIHR Evidence. National Institute for Health and Care Research. 2023. doi:10.3310/nihrevidence_59456. S2CID 260965684.
- ^ Bonnett LJ, Tudur-Smith C, Williamson PR, Marson AG (December 2010). "Risk of recurrence after a first seizure and implications for driving: further analysis of the Multicentre study of early Epilepsy and Single Seizures". BMJ. 341: c6477. doi:10.1136/bmj.c6477. PMC 2998675. PMID 21147743.
- ^ Neligan A, Hauser WA, Sander JW (2012). "The epidemiology of the epilepsies". Epilepsy. Handbook of Clinical Neurology. Vol. 107. pp. 113–33. doi:10.1016/B978-0-444-52898-8.00006-9. ISBN 9780444528988. PMID 22938966.; Sander JW, Shorvon SD (November 1996). "Epidemiology of the epilepsies". Journal of Neurology, Neurosurgery, and Psychiatry. 61 (5): 433–443. doi:10.1136/jnnp.61.5.433. PMC 1074036. PMID 8965090.
- ^ a b c Gavvala JR, Schuele SU (December 2016). "New-Onset Seizure in Adults and Adolescents: A Review". JAMA. 316 (24): 2657–2668. doi:10.1001/jama.2016.18625. PMID 28027373.
- ^ Camfield P, Camfield C (June 2015). "Incidence, prevalence and aetiology of seizures and epilepsy in children". Epileptic Disorders. 17 (2): 117–123. doi:10.1684/epd.2015.0736. PMID 25895502. S2CID 20719640.
- ^ a b Ba-Diop A, Marin B, Druet-Cabanac M, Ngoungou EB, Newton CR, Preux PM (October 2014). "Epidemiology, causes, and treatment of epilepsy in sub-Saharan Africa". The Lancet. Neurology. 13 (10): 1029–1044. doi:10.1016/S1474-4422(14)70114-0. PMC 5497080. PMID 25231525.
- ^ a b Magiorkinis E, Sidiropoulou K, Diamantis A (January 2010). "Hallmarks in the history of epilepsy: epilepsy in antiquity". Epilepsy & Behavior. 17 (1): 103–108. doi:10.1016/j.yebeh.2009.10.023. PMID 19963440. S2CID 26340115.
- ^ a b c d Ali R, Connolly ID, Feroze AH, Awad AJ, Choudhri OA, Grant GA (June 2016). "Epilepsy: A Disruptive Force in History". World Neurosurgery. 90: 685–690. doi:10.1016/j.wneu.2015.11.060. PMID 26709155.
- ^ Meador KJ, Loring DW, Flanigin HF (January 1989). "History of epilepsy surgery". Journal of Epilepsy. 2 (1): 21–25. doi:10.1016/0896-6974(89)90054-6. ISSN 0896-6974.
- ^ a b Litt B, Echauz J (May 2002). "Prediction of epileptic seizures". The Lancet. Neurology. 1 (1): 22–30. doi:10.1016/S1474-4422(02)00003-0. PMID 12849542. S2CID 10109539.
- ^ a b Walker MC, Schorge S, Kullmann DM, Wykes RC, Heeroma JH, Mantoan L (September 2013). "Gene therapy in status epilepticus". Epilepsia. 54 (Suppl 6): 43–45. doi:10.1111/epi.12275. PMID 24001071. S2CID 13942394.
- ^ a b Mormann F, Andrzejak RG, Elger CE, Lehnertz K (February 2007). "Seizure prediction: the long and winding road". Brain. 130 (Pt 2): 314–333. doi:10.1093/brain/awl241. PMID 17008335.
