Cellulitis
| Cellulitis | |
|---|---|
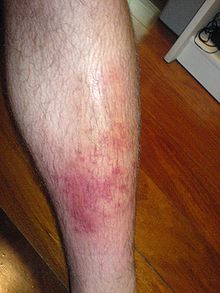 | |
| Skin cellulitis | |
| Specialty | Infectious disease |
| Symptoms | Red, hot, painful area of skin, fever[1][2] |
| Duration | 7–10 days[2] |
| Causes | Bacteria[1] |
| Risk factors | Break in the skin, obesity, leg swelling, old age[1] |
| Diagnostic method | Based on symptoms[1] |
| Differential diagnosis | Deep vein thrombosis, stasis dermatitis, erysipelas, necrotizing fasciitis[1][3] |
| Treatment | Elevation of the affected area[3] |
| Medication | Antibiotics such as cephalexin[1][4] |
| Frequency | 21.2 million (2015)[5] |
| Deaths | 16,900 (2015)[6] |
Cellulitis is a bacterial infection involving the inner layers of the skin. It specifically affects the dermis and subcutaneous fat. Signs and symptoms include an area of redness which increases in size over a few days. The borders of the area of redness are generally not sharp and the skin may be swollen. While the redness often turns white when pressure is applied, this is not always the case. The area of infection is usually painful.[1] Lymphatic vessels may occasionally be involved,[1][3] and the person may have a fever and feel tired.[2]
The legs and face are the most common sites involved, though cellulitis can occur on any part of the body. The leg is typically affected following a break in the skin. Other risk factors include obesity, leg swelling, and old age. For facial infections, a break in the skin beforehand is not usually the case. The bacteria most commonly involved are streptococci and Staphylococcus aureus. In contrast to cellulitis, erysipelas is a bacterial infection involving the more superficial layers of the skin, present with an area of redness with well-defined edges, and more often is associated with a fever. Diagnosis is usually based on the presenting signs and symptoms, while cell culture is rarely possible.[1] Before making a diagnosis, more serious infections such as an underlying bone infection or necrotizing fasciitis should be ruled out.[3]
Treatment is typically with antibiotics taken by mouth, such as cephalexin, amoxicillin, or cloxacillin.[1][4] In those who are seriously allergic to penicillin, erythromycin or clindamycin may be used.[4] When methicillin-resistant S. aureus (MRSA) is a concern, doxycycline or trimethoprim/sulfamethoxazole may, in addition, be recommended.[1] Concern is related to the presence of pus or previous MRSA infections.[1][2] Elevating the infected area may be useful, as may pain killers.[3][4]
Around 95% of people are better after seven to ten days of treatment.[2] Potential complications include abscess formation.[1] Cellulitis occurred in about 21.2 million people in 2015.[5] In the United States about two of every 1000 people per year have a case affected the lower leg.[1] Cellulitis in 2015 resulted in about 16,900 deaths worldwide.[6] In the United Kingdom, cellulitis was the reason for 1.6% of admissions to a hospital.[4]
Signs and symptoms
The typical signs and symptoms of cellulitis is an area which is red, hot, and painful. The photos shown here of are of mild to moderate cases, and are not representative of earlier stages of the condition.
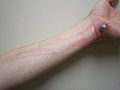
-
Cellulitis following an abrasion: Note the red streaking up the arm from involvement of the lymphatic system.
-
Infected left shin in comparison to shin with no sign of symptoms
-
Cellulitis of the leg with foot involvement
Causes
Cellulitis is caused by a type of bacteria entering the skin, usually by way of a cut, abrasion, or break in the skin. This break does not need to be visible. Group A Streptococcus and Staphylococcus are the most common of these bacteria, which are part of the normal flora of the skin, but normally cause no actual infection while on the skin's outer surface.
About 80% of cases of Ludwig's angina, or cellulitis of the submandibular space, are caused by dental infections. Mixed infections, due to both aerobes and anaerobes, are commonly associated with this type of cellulitis. Typically, this includes alpha-hemolytic streptococci, staphylococci, and bacteroides groups.[7]
Predisposing conditions for cellulitis include insect or spider bite, blistering, animal bite, tattoos, pruritic (itchy) skin rash, recent surgery, athlete's foot, dry skin, eczema, injecting drugs (especially subcutaneous or intramuscular injection or where an attempted intravenous injection "misses" or blows the vein), pregnancy, diabetes, and obesity, which can affect circulation, as well as burns and boils, though debate exists as to whether minor foot lesions contribute. Occurrences of cellulitis may also be associated with the rare condition hidradenitis suppurativa or dissecting cellulitis.
The appearance of the skin assists a doctor in determining a diagnosis. A doctor may also suggest blood tests, a wound culture, or other tests to help rule out a blood clot deep in the veins of the legs. Cellulitis in the lower leg is characterized by signs and symptoms similar to those of a deep vein thrombosis, such as warmth, pain, and swelling (inflammation).
This reddened skin or rash may signal a deeper, more serious infection of the inner layers of skin. Once below the skin, the bacteria can spread rapidly, entering the lymph nodes and the bloodstream and spreading throughout the body. This can result in influenza-like symptoms with a high temperature and sweating or feeling very cold with shaking, as the sufferer cannot get warm.[citation needed]
In rare cases, the infection can spread to the deep layer of tissue called the fascial lining. Necrotizing fasciitis, also called by the media "flesh-eating bacteria", is an example of a deep-layer infection. It is a medical emergency.[citation needed]
Risk factors
The elderly and those with a weakened immune system are especially vulnerable to contracting cellulitis. Diabetics are more susceptible to cellulitis than the general population because of impairment of the immune system; they are especially prone to cellulitis in the feet, because the disease causes impairment of blood circulation in the legs, leading to diabetic foot or foot ulcers. Poor control of blood glucose levels allows bacteria to grow more rapidly in the affected tissue, and facilitates rapid progression if the infection enters the bloodstream. Neural degeneration in diabetes means these ulcers may not be painful, thus often become infected. Those who have suffered poliomyelitis are also prone because of circulatory problems, especially in the legs.[citation needed]
Immunosuppressive drugs, and other illnesses or infections that weaken the immune system, are also factors that make infection more likely. Chickenpox and shingles often result in blisters that break open, providing a gap in the skin through which bacteria can enter. Lymphedema, which causes swelling on the arms and/or legs, can also put an individual at risk.
Diseases that affect blood circulation in the legs and feet, such as chronic venous insufficiency and varicose veins, are also risk factors for cellulitis.
Cellulitis is also common among dense populations sharing hygiene facilities and common living quarters, such as military installations, college dormitories, nursing homes, oil platforms, and homeless shelters.
Diagnosis
Cellulitis is most often a clinical diagnosis, readily identified in many people by history and physical examination alone, with rapidly spreading areas of cutaneous swelling, redness, and heat, occasionally associated with inflammation of regional lymph nodes. While classically distinguished as a separate entity from erysipelas by spreading more deeply to involve the subcutaneous tissues, many clinicians may classify erysipelas as cellulitis. Both are often treated similarly, but cellulitis associated with furuncles, carbuncles, or abscesses is usually caused by S. aureus, which may affect treatment decisions, especially antibiotic selection.[8] Skin aspiration of nonpurulent cellulitis, usually caused by streptococcal organisms, is rarely helpful for diagnosis, and blood cultures are positive in fewer than 5% of all cases.[8]
It is important to evaluate for co-existent abscess, as this finding usually requires surgical drainage as opposed to antibiotic therapy alone. Physicians' clinical assessment for abscess may be limited, especially in cases with extensive overlying induration, but use of bedside ultrasonography performed by an experienced practitioner readily discriminates between abscess and cellulitis and may change management in up to 56% of cases.[9] Use of ultrasound for abscess identification may also be indicated in cases of antibiotic failure. Cellulitis has a characteristic "cobblestoned" appearance indicative of subcutaneous edema without a defined hypoechoic, heterogeneous fluid collection that would indicate abscess.[10]
Differential diagnosis
Other conditions that may mimic cellulitis include deep vein thrombosis, which can be diagnosed with a compression leg ultrasound, and stasis dermatitis, which is inflammation of the skin from poor blood flow. Signs of a more severe infection such as necrotizing fasciitis or gas gangrene that would require prompt surgical intervention include purple bullae, skin sloughing, subcutaneous edema, and systemic toxicity.[8] Misdiagnosis can occur in up to 30% of people with suspected lower-extremity cellulitis, leading to 50,000 to 130,000 unnecessary hospitalization and $195 to $515 million in avoidable healthcare spending annually in the United States.[11]
Associated musculoskeletal findings are sometimes reported. When it occurs with acne conglobata, hidradenitis suppurativa, and pilonidal cysts, the syndrome is referred to as the follicular occlusion triad or tetrad.[12]
Lyme disease can be misdiagnosed as staphylococcal- or streptococcal-induced cellulitis. Because the characteristic bullseye rash does not always appear in people infected with Lyme disease, the similar set of symptoms may be misdiagnosed as cellulitis. Standard treatments for cellulitis are not sufficient for curing Lyme disease. The only way to rule out Lyme disease is with a blood test, which is recommended during warm months in areas where the disease is endemic.[13]
Prevention
In those who have previously had cellulitis, the use of antibiotics may help prevent future episodes.[14] This is recommended by CREST for those who have had more than two episodes.[4]
Treatment
Antibiotics are usually prescribed, with the agent selected based on suspected organism and presence or absence of purulence,[8] although the best treatment choice is unclear.[15] If an abscess is also present, surgical drainage is usually indicated, with antibiotics often prescribed for co-existent cellulitis, especially if extensive.[9] Pain relief is also often prescribed, but excessive pain should always be investigated, as it is a symptom of necrotizing fasciitis. Elevation of the affected area is often recommended.[citation needed]
Steroids may speed recovery in those on antibiotics.[1]
Antibiotics
Antibiotics choices depend on regional availability, but a penicillinase-resistant semisynthetic penicillin or a first-generation cephalosporin is currently recommended for cellulitis without abscess.[8] A course of antibiotics is not effective in between 6 and 37% of cases.[16]
Epidemiology
Cellulitis in 2013 resulted in about 30,000 deaths worldwide, up from 27,000 in 1990.[17]
Other animals
Horses may acquire cellulitis, usually secondarily to a wound (which can be extremely small and superficial) or to a deep-tissue infection, such as an abscess or infected bone, tendon sheath, or joint.[18][19] Cellulitis from a superficial wound usually creates less lameness (grade 1–2 of 5) than that caused by septic arthritis (grade 4–5). The horse exhibits inflammatory edema, which is hot, painful swelling. This swelling differs from stocking up in that the horse does not display symmetrical swelling in two or four legs, but in only one leg. This swelling begins near the source of infection, but eventually continues down the leg. In some cases, the swelling also travels distally. Treatment includes cleaning the wound and caring for it properly, the administration of NSAIDs, such as phenylbutazone, cold hosing, applying a sweat wrap or a poultice, and mild exercise. Veterinarians may also prescribe antibiotics. Cellulitis is also seen in staphylococcal and corynebacterial mixed infections in bulls.[20]
See also
References
- ^ a b c d e f g h i j k l m n o Vary, JC; O'Connor, KM (May 2014). "Common Dermatologic Conditions". The Medical clinics of North America. 98 (3): 445–85. doi:10.1016/j.mcna.2014.01.005. PMID 24758956.
- ^ a b c d e Mistry, RD (Oct 2013). "Skin and soft tissue infections". Pediatric clinics of North America. 60 (5): 1063–82. doi:10.1016/j.pcl.2013.06.011. PMID 24093896.
- ^ a b c d e Tintinalli, Judith E. (2010). Emergency Medicine: A Comprehensive Study Guide (Emergency Medicine (Tintinalli)) (7th ed.). New York: McGraw-Hill Companies. p. 1016. ISBN 0-07-148480-9.
- ^ a b c d e f Phoenix, G; Das, S; Joshi, M (Aug 7, 2012). "Diagnosis and management of cellulitis". BMJ (Clinical research ed.). 345: e4955. doi:10.1136/bmj.e4955. PMID 22872711.
- ^ a b GBD 2015 Disease and Injury Incidence and Prevalence, Collaborators. (8 October 2016). "Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990-2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet. 388 (10053): 1545–1602. doi:10.1016/S0140-6736(16)31678-6. PMC 5055577. PMID 27733282.
{{cite journal}}:|first1=has generic name (help)CS1 maint: numeric names: authors list (link) - ^ a b GBD 2015 Mortality and Causes of Death, Collaborators. (8 October 2016). "Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980-2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet. 388 (10053): 1459–1544. doi:10.1016/S0140-6736(16)31012-1. PMC 5388903. PMID 27733281.
{{cite journal}}:|first1=has generic name (help)CS1 maint: numeric names: authors list (link) - ^ Dhingra, PL; Dhingra, Shruti (2010) [1992]. Nasim, Shabina (ed.). Diseases of Ear, Nose and Throat. Dhingra, Deeksha (5th ed.). New Delhi: Elsevier. pp. 277–78. ISBN 978-81-312-2364-2.
- ^ a b c d e Stevens, Dennis L.; Bisno, Alan L.; Chambers, Henry F.; Dellinger, E. Patchen; Goldstein, Ellie J. C.; Gorbach, Sherwood L.; Hirschmann, Jan V.; Kaplan, Sheldon L.; Montoya, Jose G. (2014-06-18). "Practice Guidelines for the Diagnosis and Management of Skin and Soft Tissue Infections: 2014 Update by the Infectious Diseases Society of America". Clinical Infectious Diseases. 59 (2): 147–59. doi:10.1093/cid/ciu296. ISSN 1058-4838. PMID 24947530. Archived from the original on 2015-01-31.
{{cite journal}}: Unknown parameter|deadurl=ignored (|url-status=suggested) (help) - ^ a b Singer, Adam J.; Talan, David A. (2014-03-13). "Management of Skin Abscesses in the Era of Methicillin-Resistant Staphylococcus aureus". New England Journal of Medicine. 370 (11): 1039–1047. doi:10.1056/NEJMra1212788. ISSN 0028-4793. PMID 24620867.
- ^ Bornemann, Paul; Rao, Victor; Hoppmann, Richard (2015-05-04). "Ambulatory Ultrasound". In Mayeaux, E.J. (ed.). The Essential Guide to Primary Care Procedures. Lippincott Williams & Wilkins. ISBN 9781496318718. Archived from the original on 2016-05-06.
{{cite book}}: Unknown parameter|deadurl=ignored (|url-status=suggested) (help) - ^ Weng, Qing Yu; Raff, Adam B.; Cohen, Jeffrey M.; Gunasekera, Nicole; Okhovat, Jean-Phillip; Vedak, Priyanka; Joyce, Cara; Kroshinsky, Daniela; Mostaghimi, Arash (2017). "Costs and Consequences Associated With Misdiagnosed Lower Extremity Cellulitis". JAMA Dermatology. 153 (2): 141. doi:10.1001/jamadermatol.2016.3816. Archived from the original on 2016-11-04.
{{cite journal}}: Unknown parameter|deadurl=ignored (|url-status=suggested) (help) - ^ Scheinfeld NS (February 2003). "A case of dissecting cellulitis and a review of the literature". Dermatol. Online J. 9 (1): 8. PMID 12639466. Archived from the original on 2012-04-14.
{{cite journal}}: Unknown parameter|deadurl=ignored (|url-status=suggested) (help) - ^ Nowakowski J, McKenna D, Nadelman RB (June 2000). "Failure of treatment with cephalexin for Lyme disease". Arch Fam Med. 9 (6): 563–7. doi:10.1001/archfami.9.6.563. PMID 10862221.
{{cite journal}}: Unknown parameter|displayauthors=ignored (|display-authors=suggested) (help) - ^ Oh, CC; Ko, HC; Lee, HY; Safdar, N; Maki, DG; Chlebicki, MP (Feb 24, 2014). "Antibiotic prophylaxis for preventing recurrent cellulitis: A systematic review and meta-analysis". The Journal of infection. 69 (1): 26–34. doi:10.1016/j.jinf.2014.02.011. PMID 24576824.
- ^ Kilburn, SA; Featherstone, P; Higgins, B; Brindle, R (16 June 2010). "Interventions for cellulitis and erysipelas". The Cochrane database of systematic reviews (6): CD004299. doi:10.1002/14651858.CD004299.pub2. PMID 20556757.
- ^ Obaitan, Itegbemie; Dwyer, Richard; Lipworth, Adam D.; Kupper, Thomas S.; Camargo, Carlos A.; Hooper, David C.; Murphy, George F.; Pallin, Daniel J. (May 2016). "Failure of antibiotics in cellulitis trials: a systematic review and meta-analysis". The American Journal of Emergency Medicine. 34 (8): 1645–52. doi:10.1016/j.ajem.2016.05.064. PMID 27344098.
- ^ GBD 2013 Mortality and Causes of Death, Collaborators (17 December 2014). "Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990–2013: a systematic analysis for the Global Burden of Disease Study 2013". Lancet. 385 (9963): 117–71. doi:10.1016/S0140-6736(14)61682-2. PMC 4340604. PMID 25530442.
{{cite journal}}:|first1=has generic name (help)CS1 maint: numeric names: authors list (link) - ^ Adam EN, Southwood LL (August 2006). "Surgical and traumatic wound infections, cellulitis, and myositis in horses". Vet. Clin. North Am. Equine Pract. 22 (2): 335–61, viii. doi:10.1016/j.cveq.2006.04.003. PMID 16882479.
- ^ Fjordbakk CT, Arroyo LG, Hewson J (February 2008). "Retrospective study of the clinical features of limb cellulitis in 63 horses". Vet. Rec. 162 (8): 233–36. doi:10.1136/vr.162.8.233. PMID 18296664.
- ^ Pathan MM, Khan MA, Bhonsle AV, Bhikane AU, Moregaonkar SD, Kulkarni MB (2012). "Cellulitis in a Red Kandhari Bull : A Case Report". Vetworld. 5 (3): 183–84. doi:10.5455/vetworld.2012.183-184. Archived from the original on 2013-03-16.
{{cite journal}}: Unknown parameter|deadurl=ignored (|url-status=suggested) (help)
Further reading
- Stevens, DL; Bisno, AL; Chambers, HF; Dellinger, EP; Goldstein, EJ; Gorbach, SL; Hirschmann, JV; Kaplan, SL; Montoya, JG; Wade, JC (15 July 2014). "Practice guidelines for the diagnosis and management of skin and soft tissue infections: 2014 update by the infectious diseases society of America". Clinical Infectious Diseases. 59 (2): 147–59. doi:10.1093/cid/ciu296. PMID 24947530.