List of benzodiazepines: Difference between revisions
| Line 4: | Line 4: | ||
==Benzodiazepine half life and equivalent dose table== |
==Benzodiazepine half life and equivalent dose table== |
||
{{See also|Benzodiazepine drug misuse#Risk factors for misuse}} |
{{See also|Benzodiazepine drug misuse#Risk factors for misuse}} |
||
It is important to note that the [[elimination half life]] of diazepam and chlordiazepoxide as well as other long half-life benzodiazepines is twice as long in the elderly compared to younger individuals. Many doctors make the mistake of not adjusting benzodiazepine dosage according to age in elderly patients. Thus the equivalent doses below may need to be adjusted accordingly in individuals on short acting |
It is important to note that the [[elimination half life]] of diazepam and chlordiazepoxide as well as other long half-life benzodiazepines is twice as long in the elderly compared to younger individuals. Individuals with an impaired liver also metabolise benzodiazepines more slowly. Many doctors make the mistake of not adjusting benzodiazepine dosage according to age in elderly patients. Thus the equivalent doses below may need to be adjusted accordingly in individuals on short acting benzodiazepines who metabolise long-acting benzodiazepines more slowly and vice versa. The changes are most notable with long acting benzodiazepines as these are prone to significant accumulation in such individuals.<ref>{{cite book |last1=Salzman |first1=Carl |title=Clinical geriatric psychopharmacology |url=http://books.google.co.uk/books?id=RXvpjJ1Un2gC |edition=4th |date=15 May 2004 |publisher=Lippincott Williams & Wilkins |location=USA |isbn=978-0781743808 |pages=450-453}}</ref><ref>{{cite journal |author=Delcò F, Tchambaz L, Schlienger R, Drewe J, Krähenbühl S |title=Dose adjustment in patients with liver disease |journal=Drug Saf |volume=28 |issue=6 |pages=529–45 |year=2005 |pmid=15924505 |doi= |url=}}</ref> |
||
{| class="wikitable sortable" style="float:center; margin-left:3px;text-size:100%; text-align:right" |
{| class="wikitable sortable" style="float:center; margin-left:3px;text-size:100%; text-align:right" |
||
Revision as of 14:06, 18 July 2009
| Benzodiazepines |
|---|
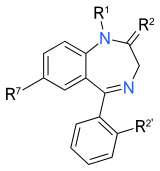 |
The below tables contain a list of benzodiazepines that are commonly prescribed, with their basic pharmacological characteristics such as half-life and equivalent doses to other benzodiazepines also listed. Most of the more commonly used benzodiazepines and their respective trade names, half-lives, primary uses and benzodiazepine equivalent doses are listed in the below table. The elimination half life is how long it takes for half of the drug to be eliminated by the body. "Time to peak" refers to when maximum levels of the drug in the blood occur after a given dose. Benzodiazepines generally share the same pharmacological properties, such as anxiolytic, sedative, hypnotic, skeletal muscle relaxant, amnesic and anticonvulsant, but some variation in potency of certain effects may exist among individual benzodiazepines. Some benzodiazepines produce active metabolites. Active metabolites are produced when a person's body metabolizes the drug into compounds that share a similar pharmacological profile to the parent compound and thus are relevant when calculating how long the pharmacological effects of a drug will last. Long-acting benzodiazepines with long-acting active metabolites such as diazepam and chlordiazepoxide are often utilized for benzodiazepine or alcohol withdrawal or for the treatment of anxiety where constant dose levels are required throughout the day. Shorter-acting benzodiazepines are often preferred for insomnia due to a reduced hangover effect.[1][2][3][4][5]
Benzodiazepine half life and equivalent dose table
It is important to note that the elimination half life of diazepam and chlordiazepoxide as well as other long half-life benzodiazepines is twice as long in the elderly compared to younger individuals. Individuals with an impaired liver also metabolise benzodiazepines more slowly. Many doctors make the mistake of not adjusting benzodiazepine dosage according to age in elderly patients. Thus the equivalent doses below may need to be adjusted accordingly in individuals on short acting benzodiazepines who metabolise long-acting benzodiazepines more slowly and vice versa. The changes are most notable with long acting benzodiazepines as these are prone to significant accumulation in such individuals.[6][7]
| Drug Name | Common Brand Names* | Time to Peak (Onset of action in hours) | Elimination Half-Life (h)** [active metabolite] | Therapeutic use | Approximate Equivalent Dose*** |
| Alprazolam | Xanax, Xanor, Tafil, Alprox, Frontal (Brazil) | 1-2 | 6-12 hours | anxiolytic | 0.5 mg |
| Bromazepam | Lexotanil, Lexotan, Lexomil, Somalium, Bromam | 1-3 | 10-20 hours | anxiolytic | 5-6 mg |
| Chlordiazepoxide | Librium, Tropium, Risolid, Klopoxid | 1.5-4 | 5-30 hours [36-200 hours] | anxiolytic | 25 mg |
| Cinolazepam | Gerodorm | .5-2 | 9 h | hypnotic | 40 mg |
| Clonazepam | Klonopin, Klonapin, Rivotril, Iktorivil | 1-4 | 18-50 hours | anxiolytic, anticonvulsant | 0.5 mg |
| Cloxazolam | Olcadil (Brazil) | 2-5 (?) | 18-50 hours | anxiolytic, anticonvulsant | 1 mg |
| Clorazepate | Tranxene | Variable | [36-100 hours] | anxiolytic, anticonvulsant | 15 mg |
| Diazepam | Valium, Apzepam, Stesolid, Vival, Apozepam, Hexalid, Valaxona | 1-2 | 20-100 hours [36-200] | anxiolytic, anticonvulsant, muscle relaxant | 10 mg |
| Estazolam | ProSom | 0.5-5 | 10-24 h | hypnotic | 1-2 mg |
| Flunitrazepam | Rohypnol, Fluscand, Flunipam, Ronal, Rohydorm (Brazil) | 0.5-3 | 18-26 hours [36-200 hours] | hypnotic | 1 mg |
| Flurazepam | Dalmadorm, Dalmane | 1-1.5 | [40-250 hours] | hypnotic | 15-30 mg |
| Flutoprazepam | Restas | 0.5-9 | 60-90 hours | hypnotic | 2-3 mg |
| Halazepam | Paxipam | 1-3 | [30-100 hours] | anxiolytic | 20-40 mg |
| Ketazolam | Anxon | 2.5-3 | 30-100 hours [36-200] | anxiolytic | 15-30 mg |
| Loprazolam | Dormonoct | 0.5-4 | 6-12 hours | hypnotic | 1-2 mg |
| Lorazepam | Ativan, Temesta, Lorabenz | 2-4 | 10-20 hours | anxiolytic,anticonvulsant | 1 mg |
| Lormetazepam | Loramet, Noctamid, Pronoctan | 0.5-2 | 10-12 hours | hypnotic | 1-2 mg |
| Medazepam | Nobrium | ? | 36-200 hours | anxiolytic | 10 mg |
| Midazolam | Dormicum, Versed, Hypnovel, Dormonid (Brazil) | 0.5-1 | 3 hours (1.8-6 hours) | hypnotic | 5 mg |
| Nimetazepam | Erimin | 0.5-3 | 14-30 hours | hypnotic | 5 mg |
| Nitrazepam | Mogadon, Alodorm, Pacisyn, Dumolid | 0.5-7 | 15-38 hours | hypnotic, anticonvulsant | 10 mg |
| Nordazepam | Madar, Stilny | ? | 50-120 hours | anxiolytic | 10 mg |
| Oxazepam | Seresta, Serax, Serenid, Serepax, Sobril, Oxascand, Alopam, Oxabenz, Oxapax | 3-4 | 4-15 hours | anxiolytic | 30 mg |
| Phenazepam | феназепам | 1.5-4 | 60 hours | anxiolytic, anticonvulsant | 1 mg |
| Pinazepam | Domar | ? | 40-100 hours | anxiolytic | 20 mg |
| Prazepam | Lysanxia, Centrax | 2-6 | 36-200 hours | anxiolytic | 10-20 mg |
| Premazepam | 1 | 2-6 | 10-13 hours | anxiolytic | 3.75 mg |
| Quazepam | Doral | 1-5 | 39-120 hours | hypnotic | 20 mg |
| Temazepam | Restoril, Normison, Euhypnos, Tenox | 0.5-3 | 8-22 hours | hypnotic | 20 mg |
| Tetrazepam | Mylostan | 1-3 | 3-26 hours | Skeletal muscle relaxant | 50mg |
| Triazolam | Halcion, Rilamir | 0.5-2 | 2 hours | hypnotic | 0.25 mg |
Atypical benzodiazepine receptor ligands
| Drug Name | Common Brand Names* | Elimination Half-Life (h)** [active metabolite] | Primary Effects | Approximate Equivalent Dose*** |
| Clobazam | Frisium, Urbanol | 8-60 hours | anxiolytic, anticonvulsant | 20 mg |
| DMCM | ? | ? | anxiogenic, convulsant | N/A, not used therapeutically |
| Flumazenil | Anexate, Lanexat, Mazicon, Romazicon | 1 hour | antidote | N/A, typical dose 0.2 - 0.6 mg |
| Eszopiclone**** | Lunesta | 6 hours | hypnotic | 3 mg |
| Zaleplon**** | Sonata, Starnoc | 1 hours | hypnotic | 20 mg |
| Zolpidem**** | Ambien, Nytamel, Stilnoct, Stilnox, Zoldem, Zolnod | 2.6 hours | hypnotic | 20 mg |
| Zopiclone**** | Imovane, Rhovane, Zileze; Zimoclone; Zimovane; Zopitan; Zorclone, | 4-6 hours | hypnotic | 15 mg |
*Not all trade names are listed. Click on drug name to see a more comprehensive list.
**The duration of apparent action is usually considerably less than the half-life. With most benzodiazepines, noticeable effects usually wear off within a few hours. Nevertheless, as long as the drug is present it will exert subtle effects within the body. These effects may become apparent during continued use or may appear as withdrawal symptoms when dosage is reduced or the drug is stopped.
***Equivalent doses are based on clinical experience but may vary between individuals.[1]
****The molecular structure of these drugs differs from the benzodiazepine molecule but they work on benzodiazepine receptors with the same or similar effects and are cross tolerant drugs.
See also
References
- ^ Golombok S, Lader M (1984). "The psychopharmacological effects of premazepam, diazepam and placebo in healthy human subjects" (PDF). Br J Clin Pharmacol. 18 (2): 127–33. PMC 1463527. PMID 6148956.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ de Visser SJ, van der Post JP, de Waal PP, Cornet F, Cohen AF, van Gerven JM (2003). "Biomarkers for the effects of benzodiazepines in healthy volunteers" (PDF). Br J Clin Pharmacol. 55 (1): 39–50. PMC 1884188. PMID 12534639.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ "Benzodiazepine Names". non-benzodiazepines.org.uk. Retrieved 2009-04-05.
- ^ C. Heather Ashton (2007). "Benzodiazepine Equivalence Table". benzo.org.uk. Retrieved 2009-04-05.
{{cite web}}: Unknown parameter|month=ignored (help) - ^ Bob, Dr (1995). "Benzodiazepine Equivalence Charts". dr-bob.org. Retrieved 2009-04-05.
{{cite web}}: Unknown parameter|month=ignored (help) - ^ Salzman, Carl (15 May 2004). Clinical geriatric psychopharmacology (4th ed.). USA: Lippincott Williams & Wilkins. pp. 450–453. ISBN 978-0781743808.
- ^ Delcò F, Tchambaz L, Schlienger R, Drewe J, Krähenbühl S (2005). "Dose adjustment in patients with liver disease". Drug Saf. 28 (6): 529–45. PMID 15924505.
{{cite journal}}: CS1 maint: multiple names: authors list (link)
Further reading
- Gitlow, Stuart (1st October 2006). Substance Use Disorders: A Practical Guide (2nd ed.). USA: Lippincott Williams and Wilkins. p. 110. ISBN 978-0781769983.
{{cite book}}: Check date values in:|date=(help) - Galanter, Marc; Kleber, Herbert D. (1 July 2008). The American Psychiatric Publishing Textbook of Substance Abuse Treatment (4th ed.). United States of America: American Psychiatric Publishing Inc. p. 216. ISBN 978-1585622764.
{{cite book}}: Cite has empty unknown parameter:|chapterurl=(help)
