Human betaherpesvirus 5
| Human cytomegalovirus | |
|---|---|
| Specialty | Infectious disease |
| Causes | Human betaherpesvirus 5 |
| Human betaherpesvirus 5 | |
|---|---|
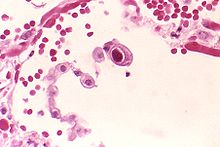
| |
| CMV infection of a human lung pneumocyte | |
| Virus classification | |
| (unranked): | Virus |
| Realm: | Duplodnaviria |
| Kingdom: | Heunggongvirae |
| Phylum: | Peploviricota |
| Class: | Herviviricetes |
| Order: | Herpesvirales |
| Family: | Orthoherpesviridae |
| Genus: | Cytomegalovirus |
| Species: | Human betaherpesvirus 5
|
| Synonyms[1] | |
| |
Human betaherpesvirus 5, also called human cytomegalovirus (HCMV,HHV-5),[2] is a species of virus in the genus Cytomegalovirus, which in turn is a member of the viral family known as Herpesviridae or herpesviruses. It is also commonly called CMV.[3] Within Herpesviridae, HCMV belongs to the Betaherpesvirinae subfamily, which also includes cytomegaloviruses from other mammals.[4] CMV is a double-stranded DNA virus.[5]
Although they may be found throughout the body, HCMV infections are frequently associated with the salivary glands.[4] HCMV infection is typically unnoticed in healthy people, but can be life-threatening for the immunocompromised, such as HIV-infected persons, organ transplant recipients, or newborn infants.[3] Congenital cytomegalovirus infection can lead to significant morbidity and even death. After infection, HCMV remains latent within the body throughout life and can be reactivated at any time. Eventually, it may cause mucoepidermoid carcinoma and possibly other malignancies[6] such as prostate cancer,[7][8] breast cancer,[9] ovarian cancer[10] and glioblastoma.[11][12]
HCMV is found in all geographic locations and all socioeconomic groups, and infects between 60% and 70% of adults in the first world and almost 100% in the third world.[13] Of all herpes viruses, HCMV harbors the most genes dedicated to altering (evading) innate and adaptive host immunity and represents a lifelong burden of antigenic T cell surveillance and immune dysfunction.[14] Commonly it is indicated by the presence of antibodies in the general population.[3] Seroprevalence is age-dependent: 58.9% of individuals aged 6 and older are infected with CMV while 90.8% of individuals aged 80 and older are positive for HCMV.[15] HCMV is also the virus most frequently transmitted to a developing fetus.[16] HCMV infection is more widespread in developing countries and in communities with lower socioeconomic status and represents the most significant viral cause of birth defects in industrialized countries. Congenital HCMV is the leading infectious cause of deafness, learning disabilities, and intellectual disability in children.[17] CMV also "seems to have a large impact on immune parameters in later life and may contribute to increased morbidity and eventual mortality."[18]
Signs and symptoms
[edit]Human betaherpesvirus 5 infection has a classic triad of symptoms: fever, peaking in the late afternoon or early evening; pharyngitis, usually exudative; and symmetrical adenopathy.[19][20][21]
Virology
[edit]Transmission
[edit]The mode of HCMV transmission from person to person is unknown, but is presumed to occur through bodily fluids, including saliva, urine, blood, and tears.[22] Cytomegalovirus is most commonly transmitted through kissing and sexual intercourse. It can also be transferred from an infected mother to her unborn child.[4] Infection requires close, intimate contact with a person secreting the virus in their saliva, urine, or other bodily fluids. CMV can be transmitted sexually and via breast milk, and also occurs through receiving transplanted organs or blood transfusions.[23] Although HCMV is not highly contagious, it has been shown to spread in households and among young children in day care centers.[3]
Replication
[edit]HCMV replicates within infected endothelial cells[24] at a slow rate, taking about five days in cell culture.[25] It also infects fibroblasts, which requires expression of only a trimeric viral receptor complex, rather than the full pentameric complex that is required for infection of endothelial and epithelial cells.[26] Like other herpesviruses, HCMV expresses genes in a temporally controlled manner.[27][28] Immediate early genes (expressed 0–4 hours after infection) are involved in the regulation of transcription, followed by early genes (expressed 4–48 hours after infection) which are involved in viral DNA replication and further transcriptional regulation.[27] Late genes are expressed during the remainder of infection up to viral egress and typically code for structural proteins. While HCMV encodes for its own functional DNA polymerase, the virus makes use of the host RNA polymerase for the transcription of all of its genes.[29]
In disseminated cytomegalovirus infections, as may be seen in the context of an immunosuppressed host, the virus is readily transmitted between polymorphonuclear leukocytes (PM-NLs) and endothelial cells. Infected endothelial cells produce cytokines that attract PM-NLs, which then adhere to the endothelium by interactions between their CD18-containing cell surface integrins and the endothelial-expressed ICAM-1. Microfusions between the cells then take place in a manner dependent on expression of the viral gene locus UL128L.[26]
Synthesis of the viral double-stranded DNA genome occurs at the host cell nucleus within specialized viral replication compartments.[30]
Nearly 75% of the genes encoded by HCMV strain AD169 can be deleted and still result in the production of infectious virus.[31] This suggests that the virus focuses on avoiding the host immune system for a timely entrance into latency.[32]
At-risk populations
[edit]CMV infections are most significant in the perinatal period and in people who are immunocompromised.
Pregnancy and congenital infection
[edit]HCMV is one of the vertically transmitted infections that lead to congenital abnormalities. (Others are: toxoplasmosis, rubella and herpes simplex.) Congenital HCMV infection occurs when the mother has a primary infection during pregnancy.[33][34][35]
Up to 5 of every 1,000 live births are infected. Five percent develop multiple handicaps, and develop cytomegalic inclusion disease with nonspecific signs that resemble rubella. Another five percent later develop cerebral calcification (decreasing IQ levels dramatically and causing sensorineural deafness and psychomotor retardation).[citation needed]
However, infants born preterm and infected with HCMV after birth may experience cognitive and motor impairments later in life.[36]
Immunocompromised adults
[edit]CMV infection or reactivation in people whose immune systems are compromised—for example people who have received transplants or are significantly burned—causes illness and increases the risk of death.[37][38]
CMV reactivation is commonly seen in people with severe colitis.[39]
Specific disease entities recognized in those people are
- CMV hepatitis, which may cause fulminant liver failure
- cytomegalovirus retinitis (inflammation of the retina, characterised by a "pizza pie appearance" on ophthalmoscopy)
- cytomegalovirus colitis (inflammation of the large bowel)
- CMV pneumonitis
- CMV esophagitis[40]
- polyradiculopathy, transverse myelitis, and subacute encephalitis
People without CMV infection who are given organ transplants from CMV-infected donors require prophylactic treatment with valganciclovir (ideally) or ganciclovir, and regular serological monitoring to detect a rising CMV titre; if treated early establishment of a potentially life-threatening infection can be prevented.[41]
Immunocompetent adults
[edit]CMV infections can still be of clinical significance in adult immunocompetent populations.[42]
- CMV mononucleosis (some sources reserve "mononucleosis" for Epstein–Barr virus only). However, the mononucleosis syndrome associated with CMV typically lacks signs of enlarged cervical lymph nodes and splenomegaly.[43][22]
- CMV has also been associated with Guillain–Barré syndrome,[44] type 1 diabetes,[45] and type 2 diabetes.[46]
The question of whether latent CMV infection has any negative effects on people who are otherwise healthy has been debated; as of 2016 the answer was not clear, but discussions had focused on whether latent CMV might increase the risk of some cardiovascular diseases and cancers.[37]
Pathogenesis
[edit]
Most healthy people who are infected by HCMV after birth have no symptoms.[3] Some develop a syndrome similar to infectious mononucleosis or glandular fever,[47] with prolonged fever, and a mild hepatitis. A sore throat is common. After infection, the virus remains latent in lymphocytes in the body for the rest of the person's life. Overt disease rarely occurs unless immunity is suppressed either by drugs, infection or old age. Initial HCMV infection, which often is asymptomatic, is followed by a prolonged, inapparent infection during which the virus resides in mononuclear cells without causing detectable damage or clinical illness.[48]
Infectious CMV may be shed in the bodily fluids of any infected person, and can be found in urine, saliva, blood, tears, semen, and breast milk. The shedding of virus can occur intermittently, without any detectable signs or symptoms.
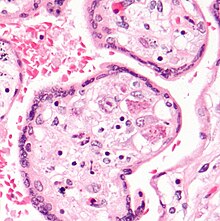
CMV infection can be demonstrated microscopically by the detection of intranuclear inclusion bodies. On H&E staining, the inclusion bodies stain dark pink and are called "owl's eye" inclusion bodies.[49]
HCMV infection is important to certain high-risk groups.[50] Major areas of risk of infection include pre-natal or postnatal infants and immunocompromised individuals, such as organ transplant recipients, persons with leukemia, or those infected with human immunodeficiency virus (HIV). In HIV infected persons, HCMV is considered an AIDS-defining infection, indicating that the T-cell count has dropped to low levels.
Lytically replicating viruses disrupt the cytoskeleton, causing massive cell enlargement, which is the source of the virus' name.
A study published in 2009 links infection with CMV to high blood pressure in mice, and suggests that the result of CMV infection of blood vessel endothelium in humans is a major cause of atherosclerosis.[51] Researchers also found that when the cells were infected with CMV, they created renin, a protein known to contribute to high blood pressure.
Human CMV causes cellular senescence, which could contribute to chronic inflammation (inflammaging).[52] Human CMV is also linked to age-associated T cell dysfunction, contributing to immunosenescence.[52] In persons infected with CMV about 10% of memory T cells are CMV-specific, but these may expand to as much as 30% in the elderly,[53] 50% or more of CD8+ memory T-cells.[54] COVID-19 symptom severity is associated with CMV, although the exact mechanism has not been elucidated.[55]
CMV encodes a protein, UL16, which is involved in the immune evasion of NK cell responses. It binds to ligands ULBP1, ULBP2 and MICB of NK cell activating receptor NKG2D, which prevents their surface expression. These ligands are normally upregulated in times of cellular stress, such as in viral infection, and by preventing their upregulation, CMV can prevent its host cell from dying due to NK cells[56]
A substantial portion of the immune system is involved in continuously controlling CMV, which drains the resources of the immune system.[57][58] Death rates from infectious disease accelerate with age,[59] and CMV infection correlates with reduced effectiveness of vaccination.[60] Persons with the highest levels of CMV antibodies have a much higher risk of death from all causes compared with persons having few or no antibodies.[61][62]
Diagnosis
[edit]
Most infections with CMV go undiagnosed, as the virus usually produces few, if any, symptoms and tends to reactivate intermittently without symptoms. Persons who have been infected with CMV develop antibodies to the virus, which persist in the body for the lifetime of that individual. A number of laboratory tests that detect these antibodies to CMV have been developed to determine if infection has occurred and are widely available from commercial laboratories. In addition, the virus can be cultured from specimens obtained from urine, throat swabs, bronchial lavages and tissue samples to detect active infection. Both qualitative and quantitative polymerase chain reaction (PCR) testing for CMV are available as well, allowing physicians to monitor the viral load of people infected with CMV.
The CMV pp65 antigenemia test is an immunofluorescence-based assay which utilizes an indirect immunofluorescence technique for identifying the pp65 protein of cytomegalovirus in peripheral blood leukocytes.[63] The CMV pp65 assay is widely used for monitoring CMV infection and its response to antiviral treatment in people who are under immunosuppressive therapy and have had renal transplantation surgery, as the antigenemia results are obtained about 5 days before the onset of symptomatic CMV disease. The advantage of this assay is the rapidity in providing results in a few hours and that the pp65 antigen determination represents a useful criterion for the physician to initiate antiviral therapy. The major disadvantage of the pp65 assay is that only a limited number of samples can be processed per test batch.
CMV should be suspected if a person has symptoms of infectious mononucleosis but has negative test results for mononucleosis and Epstein–Barr virus, or if they show signs of hepatitis, but have negative test results for hepatitis A, B, and C.
For best diagnostic results, laboratory tests for CMV antibody should be performed by using paired serum samples. One blood sample should be taken upon suspicion of CMV, and another one taken within 2 weeks. A virus culture can be performed any time the person is symptomatic. Laboratory testing for antibodies to CMV can be performed to determine if a woman has already had CMV infection. However, routine testing of all pregnant women is costly and the need for testing should therefore be evaluated on a case-by-case basis.
Serologic testing
[edit]The enzyme-linked immunosorbent assay (or ELISA) is the most commonly available serologic test for measuring antibody to CMV. The result can be used to determine if acute infection, prior infection, or passively acquired maternal antibody in an infant is present. Other tests include various fluorescence assays, indirect hemagglutination, (PCR) and latex agglutination.[64][65]
An ELISA technique for CMV-specific IgM is available, but may give false-positive results unless steps are taken to remove rheumatoid factor or most of the IgG antibody before the serum sample is tested. Because CMV-specific IgM may be produced in low levels in reactivated CMV infection, its presence is not always indicative of primary infection. Only virus recovered from a target organ, such as the lung, provides unequivocal evidence that the current illness is caused by acquired CMV infection. If serologic tests detect a positive or high titer of IgG, this result should not automatically be interpreted to mean that active CMV infection is present. Active CMV infection is considered to be present if antibody tests of paired serum samples show a fourfold rise in IgG antibody and a significant level of IgM antibody (equal to at least 30% of the IgG value), or if virus is cultured from a urine or throat specimen.[citation needed]
Relevance to blood donors
[edit]Although the risks discussed above are generally low, CMV assays are part of the standard screening for non-directed blood donation (donations not specified for a particular person) in the U.S., the UK and many other countries. CMV-negative donations are then earmarked for transfusion to infants or people who are immunocompromised. Some blood donation centers maintain lists of donors whose blood is CMV negative due to special demands.[66]
Relevance to bone marrow donors
[edit]During allogeneic hematopoietic stem cell transplant, it is generally advised to match the serostatus of donor and recipient. If the recipient is seronegative, a seropositive donor carries a risk of de novo infection. Conversely, a seropositive recipient is at risk of viral reactivation if they receive a transplant from a seronegative donor, losing their innate defenses in the process. In general, the risk is highest for CMV seropositive recipients, in which viral reactivation is a cause of significant morbidity. For these reasons, CMV serologic testing is routine for both bone marrow donors and recipients.[67][68]
Prevention
[edit]Vaccination
[edit]A phase 2 study of a CMV-vaccine published in 2009 indicated an efficacy of 50%—the protection provided was limited, and a number of subjects contracted CMV infection despite vaccination. In one case also congenital CMV was encountered.[69]
In 2013, Astellas Pharma started on individuals who received a hematopoietic stem cell transplant a phase 3 trial with its CMV deoxyribonucleic acid DNA cytomegalovirus vaccine ASP0113.[70]
In 2015, Astellas Pharma commenced on healthy volunteers a phase 1 trial with its cytomegalovirus vaccine ASP0113.[71]
Further cytomegalovirus vaccines candidates are the CMV-MVA Triplex vaccine and the CMVpp65-A*0201 peptide vaccine. Both vaccine candidates are sponsored by the City of Hope National Medical Center. As of 2016, the development is in clinical phase 2 trial stage.[72][73]
Hygiene
[edit]The Centers for Disease Control and Prevention (CDC) recommend regular hand washing,[74] especially after changing diapers.[75] Hand washing is also recommended after feeding a child, wiping a child's nose or mouth, or handling children's toys.[76]
Treatment
[edit]Hyperimmune globulin enriched for CMV (CMV-IGIV) is an immunoglobulin G (IgG) containing a standardized number of antibodies to cytomegalovirus. It may be used for the prophylaxis of cytomegalovirus disease associated with transplantation of kidney, lung, liver, pancreas, and heart. Alone or in combination with an antiviral agent, it has been shown to:
- Reduce the risk of CMV-related disease and death in some of the highest-risk transplant recipients
- Provide a measurable long-term survival benefit
- Produce minimal treatment-related side effects and adverse events.[77]
Ganciclovir (Cytovene) treatment is used for people with depressed immunity who have either sight-related or life-threatening illnesses. Valganciclovir (Valcyte) is an antiviral drug that is also effective and is given orally: it is a pro-drug that gets converted into ganciclovir in the body, but is much better absorbed orally than the latter. The therapeutic effectiveness is frequently compromised by the emergence of drug-resistant virus isolates. A variety of amino acid changes in the UL97 protein kinase and the viral DNA polymerase have been reported to cause drug resistance. Foscarnet or cidofovir are only given to people with CMV resistant to ganciclovir, because foscarnet has notable nephrotoxicity, resulting in increased or decreased Ca2+ or PO43−, and decreased Mg2+ levels.[78][79]
Letermovir has been approved by the European Medicines Agency[80] and the FDA[81] for treatment and prophylaxis of HCMV infection.
A better understanding of how HCMV supports viral latency and reactivation should allow for the development of new therapies that target the latent reservoir.[82]
Drug resistance
[edit]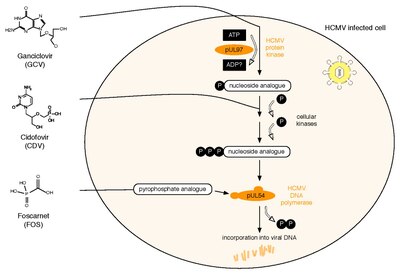
All three currently licensed anti-HCMV drugs target the viral DNA polymerase, pUL54. Ganciclovir (GCV) acts as nucleoside analogue. Its antiviral activity requires phosphorylation by the HCMV protein kinase, pUL97.[83] The second drug, Cidofovir (CDV), is a nucleotide analogue, which is already phosphorylated and thus active. Finally, Foscarnet (FOS) has a different mode of action. It directly inhibits polymerase function by blocking the pyrophosphate binding site of pUL54 (note: investigational drug letermovir acts through a mechanism that involves viral terminase).[84] Two HCMV proteins are implicated in antiviral resistance against these three drugs: pUL97 and pUL54. Specific mutations in pUL97 can cause reduced phosphorylation activity of this viral protein kinase. Thus, fewer monophosphorylated – and thus active – GCV can be synthesized,[85] leading to antiviral resistance against GCV. About 90% of all GCV resistances are caused by such mutations in UL97.[86] Mutations in pUL54 may have different effects leading to antiviral drug resistance: A. They can lead to decreased affinity to antiviral compounds. This resistance mechanism concerns GCV, CDV and FOS and may lead to multidrug resistance.[87] B. Some mutations in pUL54 can increase the polymerase's exonuclease activity. This causes enhanced recognition of incorporated GCV and CDV. As a result, these dNTP analogues are excised more efficiently. Major risk factors for HCMV drug resistance are the residual capacity of the host's immune system to control viral replication and the overall amount and duration of viral replication.[88] HCMV antiviral drug resistance can be detected by phenotypic or by genotypic drug resistance testing. Phenotypic resistance testing involves cultivation of the virus in cell culture and testing its susceptibility using different antiviral drug concentrations in order to determine EC50 values. In contrast, genotypic resistance testing means the detection of resistance associated mutations in UL97 and UL54 by sequencing. Genotypic resistance testing is becoming the method of choice because it is faster, but requires previous phenotypic characterisation of each newly found mutation. This can be performed via a web-based search tool Archived 9 January 2016 at the Wayback Machine that links a person's HCMV sequence to a database containing all published UL97 and UL54 mutations and corresponding antiviral drug susceptibility phenotypes.[89]
Epidemiology
[edit]In the United States, CMV infection rises with age from about 60% of people infected by 6 years of age[38] leveling off at about 85–90% of the population by ages 75–80.[90]
References
[edit]- ^ Davison, Andrew (27 January 2016). "Rename species in the family Herpesviridae to incorporate a subfamily designation" (PDF). International Committee on Taxonomy of Viruses (ICTV). Retrieved 13 March 2019.
- ^ taxonomy. "Taxonomy browser (Human betaherpesvirus 5)". www.ncbi.nlm.nih.gov. Retrieved 25 July 2020.
- ^ a b c d e Ryan KJ, Ray CG, eds. (2004). Sherris Medical Microbiology (4th ed.). McGraw Hill. pp. 556, 566–9. ISBN 978-0-8385-8529-0.
- ^ a b c Koichi Yamanishi; Arvin, Ann M.; Gabriella Campadelli-Fiume; Edward Mocarski; Moore, Patrick; Roizman, Bernard; Whitley, Richard (2007). Human herpesviruses: biology, therapy, and immunoprophylaxis. Cambridge, UK: Cambridge University Press. ISBN 978-0-521-82714-0.
- ^ Zanella M, Cordey S, Kaiser L (2020). "Beyond Cytomegalovirus and Epstein-Barr Virus: a Review of Viruses Composing the Blood Virome of Solid Organ Transplant and Hematopoietic Stem Cell Transplant Recipients". Clinical Microbiology Reviews. 33 (4): e00027-20. doi:10.1128/CMR.00027-20. PMC 7462738. PMID 32847820.
- ^ Melnick M, Sedghizadeh PP, Allen CM, Jaskoll T (10 November 2011). "Human cytomegalovirus and mucoepidermoid carcinoma of salivary glands: cell-specific localization of active viral and oncogenic signaling proteins is confirmatory of a causal relationship". Experimental and Molecular Pathology. 92 (1): 118–25. doi:10.1016/j.yexmp.2011.10.011. PMID 22101257. S2CID 41446671.
- ^ Geder L, Sanford EJ, Rohner TJ, Rapp F (1977). "Cytomegalovirus and cancer of the prostate: in vitro transformation of human cells". Cancer Treat Rep. 61 (2): 139–46. PMID 68820.
- ^ Bouezzedine, Fidaa; El Baba, Ranim; Haidar Ahmad, Sandy; Herbein, Georges (January 2023). "Polyploid Giant Cancer Cells Generated from Human Cytomegalovirus-Infected Prostate Epithelial Cells". Cancers. 15 (20): 4994. doi:10.3390/cancers15204994. ISSN 2072-6694. PMC 10604969. PMID 37894361.
- ^ Kumar, Amit; Tripathy, Manoj Kumar; Pasquereau, Sébastien; Al Moussawi, Fatima; Abbas, Wasim; Coquard, Laurie; Khan, Kashif Aziz; Russo, Laetitia; Algros, Marie-Paule; Valmary-Degano, Séverine; Adotevi, Olivier (April 2018). "The Human Cytomegalovirus Strain DB Activates Oncogenic Pathways in Mammary Epithelial Cells". eBioMedicine. 30: 167–183. doi:10.1016/j.ebiom.2018.03.015. ISSN 2352-3964. PMC 5952350. PMID 29628341.
- ^ El Baba, Ranim; Haidar Ahmad, Sandy; Monnien, Franck; Mansar, Racha; Bibeau, Frédéric; Herbein, Georges (October 2023). "Polyploidy, EZH2 upregulation, and transformation in cytomegalovirus-infected human ovarian epithelial cells". Oncogene. 42 (41): 3047–3061. doi:10.1038/s41388-023-02813-4. ISSN 1476-5594. PMC 10555822. PMID 37634008.
- ^ Guyon, Joris; Haidar Ahmad, Sandy; El Baba, Ranim; Le Quang, Mégane; Bikfalvi, Andreas; Daubon, Thomas; Herbein, Georges (July 2024). "Generation of glioblastoma in mice engrafted with human cytomegalovirus-infected astrocytes". Cancer Gene Therapy. 31 (7): 1070–1080. doi:10.1038/s41417-024-00767-7. ISSN 1476-5500. PMC 11257955.
- ^ El Baba, Ranim; Pasquereau, Sébastien; Haidar Ahmad, Sandy; Monnien, Franck; Abad, Marine; Bibeau, Frédéric; Herbein, Georges (June 2023). "EZH2-Myc driven glioblastoma elicited by cytomegalovirus infection of human astrocytes". Oncogene. 42 (24): 2031–2045. doi:10.1038/s41388-023-02709-3. ISSN 1476-5594. PMC 10256614. PMID 37147437.
- ^ T. Fülöp; A. Larbi & G. Pawelec (September 2013). "Human T cell aging and the impact of persistent viral infections". Frontiers in Immunology. 4: 271. doi:10.3389/fimmu.2013.00271. PMC 3772506. PMID 24062739. article: 271.
- ^ S. Varani & M. P. Landini (2011). "Cytomegalovirus-induced immunopathology and its clinical consequences". Herpesviridae. 2 (6): 6. doi:10.1186/2042-4280-2-6. PMC 3082217. PMID 21473750.
- ^ Staras SA, Dollard SC, Radford KW, Flanders WD, Pass RF, Cannon MJ (November 2006). "Seroprevalence of cytomegalovirus infection in the United States, 1988–1994". Clin. Infect. Dis. 43 (9): 1143–51. doi:10.1086/508173. PMID 17029132.
- ^ Britt, William J. (1 August 2017). "Congenital Human Cytomegalovirus Infection and the Enigma of Maternal Immunity". Journal of Virology. 91 (15): e02392–16. doi:10.1128/JVI.02392-16. ISSN 0022-538X. PMC 5512250. PMID 28490582.
- ^ Elizabeth G. Damato; Caitlin W. Winnen (2006). "Cytomegalovirus infection: perinatal implications". J Obstet Gynecol Neonatal Nurs. 31 (1): 86–92. doi:10.1111/j.1552-6909.2002.tb00026.x. PMID 11843023.
- ^ Caruso C, et al. (2009). "Mechanisms of immunosenescence". Immun Ageing. 6: 10. doi:10.1186/1742-4933-6-10. PMC 2723084. PMID 19624841.
- ^ "Human Herpesvirus 5 - an overview | ScienceDirect Topics".
- ^ Sarma, Shohinee; Little, Derek; Ali, Tooba; Jones, Emily; Haider, Shariq (27 August 2018). "Cytomegalovirus Primary Infection in an Immunocompetent Female with Mononucleosis Features: A Review of Mononucleosis-Like Syndromes". Canadian Journal of General Internal Medicine. 13 (3): 39–43. doi:10.22374/cjgim.v13i3.258 (inactive 18 August 2024). S2CID 80706263.
{{cite journal}}: CS1 maint: DOI inactive as of August 2024 (link) - ^ Whitley, R. J.; Baron, S. (1996). "Herpesviruses". Medical Microbiology. University of Texas Medical Branch at Galveston. ISBN 9780963117212. PMID 21413307.
- ^ a b Larsen, Laura. Sexually Transmitted Diseases Sourcebook. Health Reference Series Detroit: Omnigraphics, Inc., 2009. Online.
- ^ Taylor GH (February 2003). "Cytomegalovirus". Am Fam Physician. 67 (3): 519–24. PMID 12588074.
- ^ Kahl, M.; Siegel-Axel, D.; Stenglein, S. (1 August 2000). "Efficient Lytic Infection of Human Arterial Endothelial Cells by Human Cytomegalovirus Strains". Journal of Virology. 74 (16): 7628–7635. doi:10.1128/jvi.74.16.7628-7635.2000. ISSN 0022-538X. PMC 112284. PMID 10906217.
- ^ Emery, Vincent C.; Cope, Alethea V.; Bowen, E. Frances; Gor, Dehila; Griffiths, Paul D. (19 July 1999). "The Dynamics of Human Cytomegalovirus Replication in Vivo". The Journal of Experimental Medicine. 190 (2): 177–182. doi:10.1084/jem.190.2.177. ISSN 0022-1007. PMC 2195570. PMID 10432281.
- ^ a b Gerna, Giuseppe; Kabanova, Anna; Lilleri, Daniele (2019). "Human Cytomegalovirus Cell Tropism and Host Cell Receptors". Vaccines. 7 (3): 70. doi:10.3390/vaccines7030070. PMC 6789482. PMID 31336680. 70.
- ^ a b Wathen, M. W.; Stinski, M. F. (1 February 1982). "Temporal patterns of human cytomegalovirus transcription: mapping the viral RNAs synthesized at immediate early, early, and late times after infection". Journal of Virology. 41 (2): 462–477. doi:10.1128/JVI.41.2.462-477.1982. ISSN 0022-538X. PMC 256775. PMID 6281461.
- ^ Stern-Ginossar, Noam; Weisburd, Ben; Michalski, Annette; Le, Vu Thuy Khanh; Hein, Marco Y.; Huang, Sheng-Xiong; Ma, Ming; Shen, Ben; Qian, Shu-Bing (23 November 2012). "Decoding Human Cytomegalovirus". Science. 338 (6110): 1088–1093. Bibcode:2012Sci...338.1088S. doi:10.1126/science.1227919. ISSN 0036-8075. PMC 3817102. PMID 23180859.
- ^ Snaar, S. P.; Vincent, M.; Dirks, R. W. (1 February 1999). "RNA polymerase II localizes at sites of human cytomegalovirus immediate-early RNA synthesis and processing". Journal of Histochemistry and Cytochemistry. 47 (2): 245–254. doi:10.1177/002215549904700213. ISSN 0022-1554. PMID 9889260.
- ^ Penfold, M. E.; Mocarski, E. S. (8 December 1997). "Formation of cytomegalovirus DNA replication compartments defined by localization of viral proteins and DNA synthesis". Virology. 239 (1): 46–61. doi:10.1006/viro.1997.8848. ISSN 0042-6822. PMID 9426445.
- ^ Dunn, Walter; Chou, Cassie; Li, Hong; Hai, Rong; Patterson, David; Stolc, Viktor; Zhu, Hua; Liu, Fenyong (25 November 2003). "Functional profiling of a human cytomegalovirus genome". Proceedings of the National Academy of Sciences. 100 (24): 14223–14228. Bibcode:2003PNAS..10014223D. doi:10.1073/pnas.2334032100. ISSN 0027-8424. PMC 283573. PMID 14623981.
- ^ "Human Cytomegalovirus (HCMV) | British Society for Immunology".
- ^ "Congenital CMV Infection | CDC". 3 December 2021.
- ^ Carlson, A.; Norwitz, E. R.; Stiller, R. J. (2010). "Cytomegalovirus Infection in Pregnancy: Should All Women be Screened?". Reviews in Obstetrics & Gynecology. 3 (4): 172–179. PMC 3046747. PMID 21364849.
- ^ Britt, W. J. (2018). "Maternal Immunity and the Natural History of Congenital Human Cytomegalovirus Infection". Viruses. 10 (8): 405. doi:10.3390/v10080405. PMC 6116058. PMID 30081449.
- ^ Brecht, Katharina F.; Goelz, Rangmar; Bevot, Andrea; Krägeloh-Mann, Ingeborg; Wilke, Marko; Lidzba, Karen (1 April 2015). "Postnatal Human Cytomegalovirus Infection in Preterm Infants Has Long-Term Neuropsychological Sequelae". The Journal of Pediatrics. 166 (4): 834–839.e1. doi:10.1016/j.jpeds.2014.11.002. ISSN 0022-3476. PMID 25466679.
- ^ a b Cook CH (2007). "Cytomegalovirus reactivation in "immunocompetent" patients: a call for scientific prophylaxis". The Journal of Infectious Diseases. 196 (9): 1273–1275. doi:10.1086/522433. PMID 17922387.
- ^ Sager K, Alam S, Bond A, Chinnappan L, Probert CS (2015). "Review article: cytomegalovirus and inflammatory bowel disease". Alimentary Pharmacology & Therapeutics. 41 (8): 725–733. doi:10.1111/apt.13124. PMID 25684400. S2CID 5969716.
- ^ Meinhard Classen; Guido N. J. Tytgat; M.D. PhD; Charles J. Lightdale (2010). Gastroenterological Endoscopy. Thieme. pp. 490–. ISBN 978-3-13-125852-6. Retrieved 26 June 2010.
- ^ Albekairy, Abdulkareem M.; Shawaqfeh, Mohammad S.; Alharbi, Shroug H.; Almuqbil, Faisal; Alghamdi, Mesfer A.; Albekairy, Nataleen A.; Muflih, Suhaib M.; Alkatheri, Abdulmalik (2022). "Prophylaxis of Cytomegalovirus Infection in Solid Organ Transplantation, Retrospective Evaluation". Transplant Research and Risk Management. 14: 35–45. doi:10.2147/TRRM.S366213. S2CID 249441439.
- ^ Rafailidis, PI; Mourtzoukou, EG; Varbobitis, IC; Falagas, ME (27 March 2008). "Severe cytomegalovirus infection in apparently immunocompetent patients: a systematic review". Virology Journal. 5: 47. doi:10.1186/1743-422X-5-47. PMC 2289809. PMID 18371229.
- ^ Klemola E, Von Essen R, Henle G, Henle W (June 1970). "Infectious-mononucleosis-like disease with negative heterophil agglutination test. Clinical features in relation to Epstein–Barr virus and cytomegalovirus antibodies". J. Infect. Dis. 121 (6): 608–14. doi:10.1093/infdis/121.6.608. PMID 4316146.
- ^ Lunn, M.; Hughes, R. (1 April 2011). "The Relationship between Cytomegalovirus Infection and Guillain-Barre Syndrome". Clinical Infectious Diseases. 52 (7): 845–847. doi:10.1093/cid/cir082. ISSN 1058-4838. PMID 21427391.
- ^ Pak, Chiny; McArthur, Robertg; Eun, Hyone-Myong; Yoon, Ji-Won (1988). "Association of Cytomegalovirus Infection with Autoimmune Type 1 Diabetes". The Lancet. 332 (8601): 1–4. doi:10.1016/S0140-6736(88)92941-8. PMID 2898620. S2CID 42852009.
- ^ Lohr, J.M; Oldstone, M.B.A (1990). "Detection of cytomegalovirus nucleic acid sequences in pancreas in type 2 diabetes". The Lancet. 336 (8716): 644–648. doi:10.1016/0140-6736(90)92145-8. PMID 1975850. S2CID 9783330.
- ^ Bottieau E, Clerinx J, Van den Enden E, et al. (2006). "Infectious mononucleosis-like syndromes in febrile travelers returning from the tropics". Journal of Travel Medicine. 13 (4): 191–7. doi:10.1111/j.1708-8305.2006.00049.x. PMID 16884400.
- ^ "Human Cytomegalovirus - an overview | ScienceDirect Topics".
- ^ Mattes FM, McLaughlin JE, Emery VC, Clark DA, Griffiths PD (August 2000). "Histopathological detection of owl's eye inclusions is still specific for cytomegalovirus in the era of human herpesviruses 6 and 7". J. Clin. Pathol. 53 (8): 612–4. doi:10.1136/jcp.53.8.612. PMC 1762915. PMID 11002765.
- ^ Bennekov T, Spector D, Langhoff E (March 2004). "Induction of immunity against human cytomegalovirus". Mt. Sinai J. Med. 71 (2): 86–93. PMID 15029400.
- ^ Cheng J, Ke Q, Jin Z, et al. (May 2009). Früh K (ed.). "Cytomegalovirus infection causes an increase of arterial blood pressure". PLOS Pathog. 5 (5): e1000427. doi:10.1371/journal.ppat.1000427. PMC 2673691. PMID 19436702.
- ^ a b Wei W, Ji S (2018). "Cellular senescence: Molecular mechanisms and pathogenicity". Journal of Cellular Physiology. 233 (12): 9121–9135. doi:10.1002/jcp.26956. PMID 30078211. S2CID 51924586.
- ^ Goodrum F (2016). "Human Cytomegalovirus Latency: Approaching the Gordian Knot". Annual Review of Virology. 3 (1): 333–357. doi:10.1146/annurev-virology-110615-042422. PMC 5514425. PMID 27501258.
- ^ Nikolich-Zugich J (2008). "Ageing and life-long maintenance of T-cell subsets in the face of latent persistent infections". Nature Reviews Immunology. 8 (7): 512–522. doi:10.1038/nri2318. PMC 5573867. PMID 18469829.
- ^ Bartleson JM, Radenkovic D, Verdin E (2021). "SARS-CoV-2, COVID-19 and the Ageing Immune System". Nature Aging. 1 (9): 769–782. doi:10.1038/s43587-021-00114-7. PMC 8570568. PMID 34746804.
- ^ Welte, Stefan A.; Sinzger, Christian; Lutz, Stefan Z.; Singh-Jasuja, Harpreet; Sampaio, Kerstin Laib; Eknigk, Ute; Rammensee, Hans-Georg; Steinle, Alexander (2003). "Selective intracellular retention of virally induced NKG2D ligands by the human cytomegalovirus UL16 glycoprotein". European Journal of Immunology. 33 (1): 194–203. doi:10.1002/immu.200390022. PMID 12594848. S2CID 20718868.
- ^ Hadrup SR, Strindhall J, Køllgaard T, Seremet T, Johansson B, Pawelec G, thor Straten P, Wikby A (2006). "Longitudinal studies of clonally expanded CD8 T cells reveal a repertoire shrinkage predicting mortality and an increased number of dysfunctional cytomegalovirus-specific T cells in the very elderly". Journal of Immunology. 176 (4): 2645–2653. doi:10.4049/jimmunol.176.4.2645. PMID 16456027.
- ^ Derhovanessian E, Maier AB, Hähnel K, Beck R, de Craen AJ, Slagboom EP, Westendorp RG, Pawelec G (2011). "Infection with cytomegalovirus but not herpes simplex virus induces the accumulation of late-differentiated CD4+ and CD8+ T-cells in humans". Journal of General Virology. 92 (Pt 12): 2746–2756. doi:10.1099/vir.0.036004-0. PMID 21813708.
- ^ Pawelec G, Koch S, Franceschi C, Wikby A (2006). "Human immunosenescence: does it have an infectious component?". Annals of the New York Academy of Sciences. 1067 (1): 56–65. Bibcode:2006NYASA1067...56P. doi:10.1196/annals.1354.009. PMID 16803971. S2CID 45806175.
- ^ Derhovanessian E, Theeten H, Hähnel K, Van Damme P, Cools N, Pawelec G (2013). "Cytomegalovirus-associated accumulation of late-differentiated CD4 T-cells correlates with poor humoral response to influenza vaccination" (PDF). Vaccine. 31 (4): 685–690. doi:10.1016/j.vaccine.2012.11.041. PMID 23196209. S2CID 10483363. Archived from the original (PDF) on 19 April 2018.
- ^ Roberts ET, Haan MN, Dowd JB, Aiello AE (2010). "Cytomegalovirus antibody levels, inflammation, and mortality among elderly Latinos over 9 years of follow-up". American Journal of Epidemiology. 172 (4): 363–371. doi:10.1093/aje/kwq177. PMC 2950794. PMID 20660122. S2CID 14983626.
- ^ Simanek AM, Dowd JB, Pawelec G, Melzer D, Dutta A, Aiello AE (2011). "Seropositivity to cytomegalovirus, inflammation, all-cause and cardiovascular disease-related mortality in the United States". PLOS One. 6 (2): e16103. Bibcode:2011PLoSO...616103S. doi:10.1371/journal.pone.0016103. PMC 3040745. PMID 21379581.
- ^ Ross, S.A.; Novak, Z.; Pati, S.; Boppana, S.B. (October 2011). "Diagnosis of Cytomegalovirus Infections". Infectious Disorders Drug Targets. 11 (5): 466–474. doi:10.2174/187152611797636703. ISSN 1871-5265. PMC 3730495. PMID 21827433.
- ^ "CMV Infection Laboratory Testing | CDC". 3 December 2021.
- ^ Revello, M. G.; Gerna, G. (2002). "Diagnosis and Management of Human Cytomegalovirus Infection in the Mother, Fetus, and Newborn Infant". Clinical Microbiology Reviews. 15 (4): 680–715. doi:10.1128/CMR.15.4.680-715.2002. PMC 126858. PMID 12364375.
- ^ "United Blood Services FAQs". Archived from the original on 19 May 2007. Retrieved 23 May 2007.
- ^ Ljungman, Per (15 August 2014). "Donor cytomegalovirus status influences the outcome of allogeneic stem cell transplant: a study by the European group for blood and marrow transplantation". Clin Infect Dis. 59 (4): 473–81. doi:10.1093/cid/ciu364. PMID 24850801. Retrieved 3 September 2020.
- ^ Ljungman, Per; Hakki, Morgan; Boeckh, Michael (February 2011). "Cytomegalovirus in Hematopoietic Stem Cell Transplant Recipients". Hematology/Oncology Clinics of North America. 25 (1): 151–169. doi:10.1016/j.hoc.2010.11.011. PMC 3340426. PMID 21236396.
- ^ Pass RF, Zhang C, Evans A, et al. (March 2009). "Vaccine prevention of maternal cytomegalovirus infection". N. Engl. J. Med. 360 (12): 1191–9. doi:10.1056/NEJMoa0804749. PMC 2753425. PMID 19297572.
- ^ "A Study to Evaluate a Therapeutic Vaccine, ASP0113, in Cytomegalovirus (CMV)-Seropositive Recipients Undergoing Allogeneic, Hematopoietic Cell Transplant (HCT) (HELIOS)". ClinicalTrials.gov. 12 June 2013. Retrieved 26 October 2015.
- ^ "An Evaluation of a Cytomegalovirus (CMV) Vaccine (ASP0113) in CMV-Seropositive and CMV-Seronegative Healthy Subjects and CMV-Seronegative Dialysis Patients". ClinicalTrials.gov. 8 July 2015. Retrieved 22 October 2015.
- ^ "Multi-antigen CMV-MVA Triplex Vaccine in Reducing CMV Complications in Patients Previously Infected With CMV and Undergoing Donor Hematopoietic Cell Transplant". ClinicalTrials.gov. 21 July 2015. Retrieved 23 January 2016.
- ^ "Vaccine Therapy in Reducing the Frequency of Cytomegalovirus Events in Patients With Hematologic Malignancies Undergoing Donor Stem Cell Transplant". ClinicalTrials.gov. 12 March 2015. Retrieved 23 January 2016.
- ^ "When & How to Wash Your Hands | Handwashing". CDC. 7 March 2016. Archived from the original on 13 September 2017. Retrieved 16 October 2017.
- ^ "CMV | Overview | Cytomegalovirus and Congenital CMV Infection". CDC. 17 June 2016. Archived from the original on 16 October 2017. Retrieved 16 October 2017.
- ^ "CMV Transmission". National CMV Foundation. Archived from the original on 16 October 2017. Retrieved 16 October 2017.
- ^ Cytogam Prescribing Info Archived 26 April 2012 at the Wayback Machine CSL Behring AG
- ^ Avery, R. K.; Arav-Boger, R.; Marr, K. A.; Kraus, E.; Shoham, S.; Lees, L.; Trollinger, B.; Shah, P.; Ambinder, R.; Neofytos, D.; Ostrander, D.; Forman, M.; Valsamakis, A. (2016). "Outcomes in Transplant Recipients Treated with Foscarnet for Ganciclovir-Resistant or Refractory Cytomegalovirus Infection". Transplantation. 100 (10): e74–e80. doi:10.1097/TP.0000000000001418. PMC 5030152. PMID 27495775.
- ^ Erice, A. (1999). "Resistance of Human Cytomegalovirus to Antiviral Drugs". Clinical Microbiology Reviews. 12 (2): 286–297. doi:10.1128/CMR.12.2.286. PMC 88918. PMID 10194460.
- ^ "Previmys EPAR summary for the public" (PDF). European Medicines Agency. Archived (PDF) from the original on 27 June 2018. Retrieved 27 June 2018.
- ^ "Approval Package for Letermovir" (PDF). FDA. Archived (PDF) from the original on 27 June 2018. Retrieved 27 June 2018.
- ^ Smith NA, Chan GC, O'Connor CM (2021). "Modulation of host cell signaling during cytomegalovirus latency and reactivation". Virology Journal. 18 (1): 207. doi:10.1186/s12985-021-01674-1. PMC 8524946. PMID 34663377.
- ^ Sullivan V, Talarico CL, Stanat SCC, Davis M, Coen DM, Biron KK (1992). "A protein kinase homologue controls phosphorylation of ganciclovir in human cytomegalovirus-infected cells". Nature. 358 (6382): 162–164. Bibcode:1992Natur.358..162S. doi:10.1038/358162a0. PMID 1319560. S2CID 4309307.
- ^ Chrisp P, Clissold SP (1991). "Foscarnet. A review of its antiviral activity, pharmacokinetic properties and therapeutic use in immunocompromised patients with cytomegalovirus retinitis". Drugs. 41 (1): 104–129. doi:10.2165/00003495-199141010-00009. PMID 1706982.
- ^ Biron KK, Fyfe JA, Stanat SC, Leslie LK, Sorrell JB, Lambe CU, Coen DM (1986). "A human cytomegalovirus mutant resistant to the nucleoside analog 9-([2-hydroxy-1-(hydroxymethyl)ethoxy]methyl)guanine (BW B759U) induces reduced levels of BW B759U triphosphate". Proc. Natl. Acad. Sci. U.S.A. 83 (22): 8769–8773. Bibcode:1986PNAS...83.8769B. doi:10.1073/pnas.83.22.8769. PMC 387013. PMID 3022304.
- ^ Chou S (1999). "Antiviral drug resistance in human cytomegalovirus". Transpl. Infect. Dis. 1 (2): 105–114. doi:10.1034/j.1399-3062.1999.010204.x. PMID 11428978. S2CID 23668301.
- ^ C. Gilbert & G. Boivin (2005). "Human cytomegalovirus resistance to antiviral drugs". Antimicrob. Agents Chemother. 49 (3): 873–883. doi:10.1128/AAC.49.3.873-883.2005. PMC 549271. PMID 15728878.
- ^ Drew WL (2000). "Ganciclovir resistance: a matter of time and titre". Lancet. 356 (9230): 609–610. doi:10.1016/S0140-6736(00)02597-6. PMID 10968428. S2CID 46533224.
- ^ Chevillotte M, von Einem J, Meier BM, Lin FM, Kestler HA, Mertens T (2010). "A new tool linking human cytomegalovirus drug resistance mutations to resistance phenotypes". Antiviral Research. 85 (2): 318–27. doi:10.1016/j.antiviral.2009.10.004. PMID 19853628.
- ^ Pawelec G, McElhaney JE, Aiello AE, Derhovanessian E (2012). "The impact of CMV infection on survival in older humans" (PDF). Current Opinion in Immunology. 24 (4): 507–511. doi:10.1016/j.coi.2012.04.002. PMID 22541724. S2CID 623760. Archived from the original (PDF) on 19 April 2018.
External links
[edit]- Human betaherpesvirus 5 at Curlie
- Cytomegalovirus (CMV) US Centers for Disease Control and Prevention (CDC). 22 May 2009
- HCMV drug resistance mutations tool Archived 9 January 2016 at the Wayback Machine
- "Human herpesvirus 5". NCBI Taxonomy Browser. 10359.
