Mpox
| Mpox | |
|---|---|
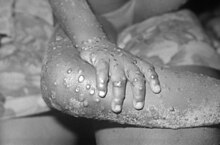 | |
| The rash of monkeypox | |
| Specialty | Infectious disease |
| Symptoms | Fever, headache, muscle pains, blistering rash, swollen lymph nodes[1] |
| Usual onset | 5-21 days post exposure[1] |
| Duration | 2 to 5 weeks[1] |
| Causes | Monkeypox virus[2] |
| Diagnostic method | Testing for viral DNA[3] |
| Differential diagnosis | Chickenpox, smallpox[4] |
| Prevention | Smallpox vaccine[3] |
| Medication | Cidofovir[4] |
| Frequency | Rare[2] |
| Deaths | Up to 10%[1] |
Monkeypox is an infectious disease caused by the monkeypox virus.[2] Symptoms begin with fever, headache, muscle pains, swollen lymph nodes, and feeling tired.[1] This is then followed by a rash that forms blisters and scabs over.[1] The time from exposure to onset of symptoms is around 10 days.[1] The duration of symptoms is typically 2 to 5 weeks.[1]
Monkeypox may be spread from handling bush meat, an animal bite or scratch, body fluids, contaminated objects, or close contact with an infected person.[5] The virus is believed to normally circulate among certain rodents in Africa.[5] Diagnosis can be confirmed by testing a lesion for the viruses DNA.[3] The disease can appear similar to chickenpox.[4]
The smallpox vaccine is believed to prevent infection.[3] Cidofovir may be useful as treatment.[4] The risk of death in those infected is up to 10%.[1]
The disease mostly occurs in Central and West Africa.[6] It was first identified in 1958 among laboratory monkeys.[6] The first cases in humans were found in 1970 in the Democratic Republic of the Congo.[6] An outbreak that occurred in the United States in 2003 was traced to a pet store where imported Gambian rodents were sold.[3]
Signs and symptoms

Monkeypox is similar to smallpox, although it is often milder.
Limited person-to-person spread of infection has been reported in disease-endemic areas in Africa. Case-fatality ratios in Africa have ranged from 1% to 10%.[7]
Cause
Monkeypox virus
| Monkeypox virus | |
|---|---|
| File:Monkeypox.gif | |
| Virus classification | |
| Group: | Group I (dsDNA)
|
| Order: | Unassigned
|
| Family: | |
| Subfamily: | |
| Genus: | |
| Type species | |
| Vaccinia virus | |
| Species | |
|
Monkeypox virus | |
Monkeypox virus causes the disease in both humans and animals. It was first identified in 1958 as a pathogen of crab-eating macaque monkeys (Macaca fascicularis) being used as laboratory animals. The crab-eating macaque is often used for neurological experiments. Monkeypox virus is an Orthopoxvirus, a genus of the family Poxviridae that contains other viral species that target mammals. The virus is found mainly in tropical rainforest regions of central and West Africa.
The virus was first discovered in monkeys (hence the name) in 1958, and in humans in 1970. Between 1970 and 1986, over 400 cases in humans were reported. Small viral outbreaks with a death rate in the range of 10% and a secondary human to human infection rate of about the same amount occur routinely in equatorial Central and West Africa.[8] The primary route of infection is thought to be contact with the infected animals or their bodily fluids.[8] The first reported outbreak in the United States occurred in 2003 in the midwestern states of Illinois, Indiana, and Wisconsin, with one occurrence in New Jersey. The outbreak was traced to a prairie dogs infected from an imported Gambian pouch rat. No deaths occurred.
The virus can spread both from animal to human and from human to human. Infection from animal to human can occur via an animal bite or by direct contact with an infected animal’s bodily fluids. The virus can spread from human to human by both respiratory (airborne) contact and contact with infected person's bodily fluids. Risk factors for transmission include sharing a bed, room, or using the same utensils as an infected patient. Increased transmission risk associated with factors involving introduction of virus to the oral mucosa.[9] Incubation period is 10–14 days. Prodromal symptoms include swelling of lymph nodes, muscle pain, headache, fever, prior to the emergence of the rash.The rash is usually only present on the trunk but has the capacity to spread to the palms and soles of the feet, occurring in a centrifugal distribution. The initial macular lesions exhibit a papular, then vesicular and pustular appearance.[9]
Reservoir
In addition to monkeys, reservoirs for the virus are found in Gambian pouched rats (Cricetomys gambianus), dormice (Graphiurus sp.) and African squirrels (Heliosciurus, and Funisciurus). The use of these animals as food may be an important source of transmission to humans.[citation needed]
Prevention
Vaccination against smallpox is assumed to provide protection against human monkeypox infection considering they are closely related viruses and the vaccine protects animals from experimental lethal monkeypox challenge.[10] This has not been conclusively demonstrated in humans because routine smallpox vaccination was discontinued following the apparent eradication of smallpox and due to safety concerns with the vaccine.
Smallpox vaccine has been reported to reduce the risk of monkeypox among previously vaccinated persons in Africa. The decrease in immunity to poxviruses in exposed populations is a factor in the prevalence of monkeypox. It is attributed both to waning cross-protective immunity among those vaccinated before 1980 when mass smallpox vaccinations were discontinued, and to the gradually increasing proportion of unvaccinated individuals.[9] The United States Centers for Disease Control and Prevention (CDC) recommends that persons investigating monkeypox outbreaks and involved in caring for infected individuals or animals should receive a smallpox vaccination to protect against monkeypox. Persons who have had close or intimate contact with individuals or animals confirmed to have monkeypox should also be vaccinated.
CDC does not recommend preexposure vaccination for unexposed veterinarians, veterinary staff, or animal control officers, unless such persons are involved in field investigations.
Treatment
Currently, there is no proven, safe treatment for monkeypox. The people who have been infected can be vaccinated up to 14 days after exposure.
Epidemiology
Monkeypox as a disease in humans was first associated with an illness in the Democratic Republic of the Congo (formerly Zaire), in the town of Basankusu, Équateur Province, in 1970.[11] A second outbreak of human illness was identified in DRC/Zaire in 1996–1997. In 2003, a small outbreak of human monkeypox in the United States occurred among owners of pet prairie dogs.[12] The outbreak originated from Villa Park, Illinois, outside of Chicago, when an exotic animal dealer kept young prairie dogs in close proximity to an infected Gambian pouched rat (Cricetomys gambianus) recently imported from Accra, Ghana. Seventy-one people were reportedly infected, of which there were no fatalities.
A second African focus of infection has been discovered in Sudan. No infected patients died.[13]
2003 U.S. outbreak
In May, 2003, a young child became ill with fever and rash after being bitten by a prairie dog purchased at a local swap meet near Milwaukee, Wisconsin.[14] In total, 71 cases of monkeypox were reported through June 20, 2003. All cases were traced to Gambian rats imported by a Texas exotic animal distributor, from Accra, Ghana in April, 2003. No deaths resulted.[15] Electron microscopy and serologic studies were used to confirm that the disease was human monkeypox.
Patients typically experienced prodromal symptoms of fever, headaches, muscle aches, chills, and drenching sweats. Roughly one-third of patients had nonproductive coughs. This prodromal phase was followed 1–10 days later by the development of a papular rash that typically progressed through stages of vesiculation, pustulation, umbilication, and crusting. In some patients, early lesions had become ulcerated. Rash distribution and lesions occurred on head, trunk, and extremities; many of the patients had initial and satellite lesions on palms, soles, and extremities. Rashes were generalized in some patients. After onset of the rash, patients generally manifested rash lesions in different stages. All patients reported direct or close contact with prairie dogs, later found to be infected with the monkeypox virus.[16]
2017 Nigeria outbreak
Monkey pox has been reportedly spread around south east and south south Nigeria. Some states and the federal government of Nigeria are currently seeking for a way to contain it as well as find a cure for the infected ones. it has spread to Lagos and federal capital territory .
References
- ^ a b c d e f g h i "Signs and Symptoms Monkeypox". CDC. 11 May 2015. Retrieved 15 October 2017.
- ^ a b c "About Monkeypox". CDC. 11 May 2015. Retrieved 15 October 2017.
- ^ a b c d e "2003 U.S. Outbreak Monkeypox". CDC. 11 May 2015. Retrieved 15 October 2017.
- ^ a b c d McCollum, AM; Damon, IK (January 2014). "Human monkeypox". Clinical infectious diseases : an official publication of the Infectious Diseases Society of America. 58 (2): 260–7. doi:10.1093/cid/cit703. PMID 24158414.
- ^ a b "Transmission} Monkeypox". CDC. 11 May 2015. Retrieved 15 October 2017.
- ^ a b c "Monkeypox". CDC. 11 May 2015. Retrieved 15 October 2017.
- ^ Hutin YJ, Williams RJ, Malfait P, et al. (2001). "Outbreak of human monkeypox, Democratic Republic of Congo, 1996 to 1997". Emerging Infect. Dis. 7 (3): 434–8. doi:10.3201/eid0703.010311. PMC 2631782. PMID 11384521.
- ^ a b Meyer, H.; Mathilde Perrichot; Markus Stemmler; Petra Emmerich; Herbert Schmitz; Francis Varaine; Robert Shungu; Florimond Tshioko; Pierre Formenty (2002). "Outbreaks of Disease Suspected of Being Due to Human Monkeypox Virus Infection in the Democratic Republic of Congo in 2001". Journal of Clinical Microbiology. 40 (8). American Society for Microbiology: 2919–2921. doi:10.1128/JCM.40.8.2919-2921.2002. PMC 120683. PMID 12149352.
{{cite journal}}:|access-date=requires|url=(help) - ^ a b c Kantele A, Chickering K, Vapalahti O, Rimoin AW (2016). "Emerging diseases—the monkeypox epidemic in the Democratic Republic of the Congo". Clinical Microbiology and Infection. 22 (8): 658–659.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Marriott KA, Parkinson CV, Morefield SI, Davenport R, Nichols R, Monath TP (2008). "Clonal vaccinia virus grown in cell culture fully protects monkeys from lethal monkeypox challenge". Vaccine. 26 (4): 581–8. doi:10.1016/j.vaccine.2007.10.063. PMID 18077063.
- ^ Ladnyj ID, Ziegler P, Kima E. "A human infection caused by monkeypox virus in Basankusu Territory, Democratic Republic of the Congo". Bull World Health Organ. 46: 593–7. PMC 2480792. PMID 4340218.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ "What You Should Know About Monkeypox" (PDF). Fact Sheet. Centers for disease control and prevention. 2003-06-12. Retrieved 2008-03-21.
- ^ Damon IK, Roth CE, Chowdhary V (2006). "Discovery of monkeypox in Sudan". N. Engl. J. Med. 355 (9): 962–3. doi:10.1056/NEJMc060792. PMID 16943415.
- ^ Anderson MG, Frenkel LD, Homann S, and Guffey J. (2003), "A case of severe monkeypox virus disease in an American child: emerging infections and changing professional values"; Pediatr Infect Dis J;22(12): 1093–1096; discussion 1096–1098.
- ^ "Medscape Monkeypox Review". Bcbsma.medscape.com. Retrieved 2013-03-22.
- ^ Centers for Disease Control (CDC), Morbidity and Mortality Weekly Report. Atlanta, Georgia. (MMWR) July 11, 2003. (52) 27; 642-646.
