Cancer: Difference between revisions
m typo, period, sb in quotes |
unclear the heredity change is an improvement, not yet established this placement of phytochemical material follows due weight, discuss on talk first to develop consensus please |
||
| Line 19: | Line 19: | ||
<!--Cause --> |
<!--Cause --> |
||
Determining what causes cancer is complex. Many things are known to increase the risk of cancer, including [[tobacco]] use, certain [[infection]]s, [[radiation]], [[lack of physical activity]], [[obesity]], and environmental pollutants.<ref name=Enviro2008>{{cite journal | author = Anand P, Kunnumakkara AB, Kunnumakara AB, Sundaram C, Harikumar KB, Tharakan ST, Lai OS, Sung B, Aggarwal BB | title = Cancer is a preventable disease that requires major lifestyle changes | journal = Pharm. Res. | volume = 25 | issue = 9 | pages = 2097–116 | year = 2008 | month = September | pmid = 18626751 | pmc = 2515569 | doi = 10.1007/s11095-008-9661-9 }}</ref> These can directly damage genes or combine with existing genetic faults within cells to cause the disease.<ref name="Kinz">{{cite book | author = Kinzler, Kenneth W.; Vogelstein, Bert | title = The genetic basis of human cancer | edition = 2nd, illustrated, revised| publisher = McGraw-Hill, Medical Pub. Division | location = New York | year = 2002 | page = 5| isbn = 978-0-07-137050-9 | url = http://books.google.com/?id=pYG09OPbXp0C| chapter=Introduction |chapterurl=http://books.google.co.uk/books?id=pYG09OPbXp0C&pg=PA5}}</ref> |
Determining what causes cancer is complex. Many things are known to increase the risk of cancer, including [[tobacco]] use, certain [[infection]]s, [[radiation]], [[lack of physical activity]], [[obesity]], and environmental pollutants.<ref name=Enviro2008>{{cite journal | author = Anand P, Kunnumakkara AB, Kunnumakara AB, Sundaram C, Harikumar KB, Tharakan ST, Lai OS, Sung B, Aggarwal BB | title = Cancer is a preventable disease that requires major lifestyle changes | journal = Pharm. Res. | volume = 25 | issue = 9 | pages = 2097–116 | year = 2008 | month = September | pmid = 18626751 | pmc = 2515569 | doi = 10.1007/s11095-008-9661-9 }}</ref> These can directly damage genes or combine with existing genetic faults within cells to cause the disease.<ref name="Kinz">{{cite book | author = Kinzler, Kenneth W.; Vogelstein, Bert | title = The genetic basis of human cancer | edition = 2nd, illustrated, revised| publisher = McGraw-Hill, Medical Pub. Division | location = New York | year = 2002 | page = 5| isbn = 978-0-07-137050-9 | url = http://books.google.com/?id=pYG09OPbXp0C| chapter=Introduction |chapterurl=http://books.google.co.uk/books?id=pYG09OPbXp0C&pg=PA5}}</ref> Approximately five to ten percent of cancers are entirely hereditary.<ref name=Expert09/> |
||
<!--Diagnosis, Treatment, Epidemiology --> |
<!--Diagnosis, Treatment, Epidemiology --> |
||
Revision as of 00:00, 15 July 2013
| Cancer | |
|---|---|
| Specialty | Oncology |
Cancer /ˈkænsər/ , known medically as a malignant neoplasm, is a broad group of various diseases, all involving unregulated cell growth. In cancer, cells divide and grow uncontrollably, forming malignant tumors, and invade nearby parts of the body. The cancer may also spread to more distant parts of the body through the lymphatic system or bloodstream. Not all tumors are cancerous. Benign tumors do not grow uncontrollably, do not invade neighboring tissues, and do not spread throughout the body. There are over 200 different known cancers that afflict humans.[1]
Determining what causes cancer is complex. Many things are known to increase the risk of cancer, including tobacco use, certain infections, radiation, lack of physical activity, obesity, and environmental pollutants.[2] These can directly damage genes or combine with existing genetic faults within cells to cause the disease.[3] Approximately five to ten percent of cancers are entirely hereditary.[4]
Cancer can be detected in a number of ways, including the presence of certain signs and symptoms, screening tests, or medical imaging. Once a possible cancer is detected it is diagnosed by microscopic examination of a tissue sample. Cancer is usually treated with chemotherapy, radiation therapy and surgery. The chances of surviving the disease vary greatly by the type and location of the cancer and the extent of disease at the start of treatment. While cancer can affect people of all ages, and a few types of cancer are more common in children, the risk of developing cancer generally increases with age. In 2007, cancer caused about 13% of all human deaths worldwide (7.9 million). Rates are rising as more people live to an old age and as mass lifestyle changes occur in the developing world.[5]
Signs and symptoms

When cancer begins it invariably produces no symptoms with signs and symptoms only appearing as the mass continues to grow or ulcerates. The findings that result depends on the type and location of the cancer. Few symptoms are specific, with many of them also frequently occurring in individuals who have other conditions. Cancer is the new "great imitator". Thus it is not uncommon for people diagnosed with cancer to have been treated for other diseases to which it was assumed their symptoms were due.[6]
Local effects
Local symptoms may occur due to the mass of the tumor or its ulceration. For example, mass effects from lung cancer can cause blockage of the bronchus resulting in cough or pneumonia; esophageal cancer can cause narrowing of the esophagus, making it difficult or painful to swallow; and colorectal cancer may lead to narrowing or blockages in the bowel, resulting in changes in bowel habits. Masses of breast or testicles may be easily felt. Ulceration can cause bleeding which, if it occurs in the lung, will lead to coughing up blood, in the bowels to anemia or rectal bleeding, in the bladder to blood in the urine, and in the uterus to vaginal bleeding. Although localized pain may occur in advanced cancer, the initial swelling is usually painless. Some cancers can cause build up of fluid within the chest or abdomen.[6]
Systemic symptoms
General symptoms occur due to distant effects of the cancer that are not related to direct or metastatic spread. These may include: unintentional weight loss, fever, being excessively tired, and changes to the skin.[7] Hodgkin disease, leukemias, and cancers of the liver or kidney can cause a persistent fever of unknown origin.[6]
Specific constellations of systemic symptoms, termed paraneoplastic phenomena, may occur with some cancers. Examples include the appearance of myasthenia gravis in thymoma and clubbing in lung cancer.[6]
Metastasis
Symptoms of metastasis are due to the spread of cancer to other locations in the body. They can include enlarged lymph nodes (which can be felt or sometimes seen under the skin and are typically hard), hepatomegaly (enlarged liver) or splenomegaly (enlarged spleen) which can be felt in the abdomen, pain or fracture of affected bones, and neurological symptoms.[6]
Causes
Cancers are primarily an environmental disease with 90–95% of cases attributed to environmental factors and 5–10% due to genetics.[2] Environmental, as used by cancer researchers, means any cause that is not inherited genetically, not merely pollution.[8] Common environmental factors that contribute to cancer death include tobacco (25–30%), diet and obesity (30–35%), infections (15–20%), radiation (both ionizing and non-ionizing, up to 10%), stress, lack of physical activity, and environmental pollutants.[2]
It is nearly impossible to prove what caused a cancer in any individual, because most cancers have multiple possible causes. For example, if a person who uses tobacco heavily develops lung cancer, then it was probably caused by the tobacco use, but since everyone has a small chance of developing lung cancer as a result of air pollution or radiation, then there is a small chance that the cancer developed because of air pollution or radiation.
Chemicals

Cancer pathogenesis is traceable back to DNA mutations that impact cell growth and metastasis. Substances that cause DNA mutations are known as mutagens, and mutagens that cause cancers are known as carcinogens. Particular substances have been linked to specific types of cancer. Tobacco smoking is associated with many forms of cancer,[9] and causes 90% of lung cancer.[10]
Many mutagens are also carcinogens, but some carcinogens are not mutagens. Alcohol is an example of a chemical carcinogen that is not a mutagen.[11] In Western Europe 10% of cancers in males and 3% of cancers in females are attributed to alcohol.[12]
Decades of research has demonstrated the link between tobacco use and cancer in the lung, larynx, head, neck, stomach, bladder, kidney, esophagus and pancreas.[13] Tobacco smoke contains over fifty known carcinogens, including nitrosamines and polycyclic aromatic hydrocarbons.[14] Tobacco is responsible for about one in three of all cancer deaths in the developed world,[9] and about one in five worldwide.[14] Lung cancer death rates in the United States have mirrored smoking patterns, with increases in smoking followed by dramatic increases in lung cancer death rates and, more recently, decreases in smoking rates since the 1950s followed by decreases in lung cancer death rates in men since 1990.[15][16] However, the numbers of smokers worldwide is still rising, leading to what some organizations have described as the tobacco epidemic.[17]
Cancer related to one's occupation is believed to represent between 2–20% of all cases.[18] Every year, at least 200,000 people die worldwide from cancer related to their workplace.[19] Most cancer deaths caused by occupational risk factors occur in the developed world.[19] It is estimated that approximately 20,000 cancer deaths and 40,000 new cases of cancer each year in the U.S. are attributable to occupation.[20] Millions of workers run the risk of developing cancers such as lung cancer and mesothelioma from inhaling asbestos fibers and tobacco smoke, or leukemia from exposure to benzene at their workplaces.[19]
Diet and exercise
Diet, physical inactivity, and obesity are related to approximately 30–35% of cancer deaths.[2][21] In the United States excess body weight is associated with the development of many types of cancer and is a factor in 14–20% of all cancer deaths.[21] Physical inactivity is believed to contribute to cancer risk not only through its effect on body weight but also through negative effects on immune system and endocrine system.[21] More than half of the effect from diet is due to overnutrition rather than from eating too few healthful foods.
Diets that are very low in vegetables, fruits and whole grains, and high in processed or red meats are linked with a number of cancers.[21] A high-salt diet is linked to gastric cancer, aflatoxin B1, a frequent food contaminate, with liver cancer, and Betel nut chewing with oral cancer.[22] This may partly explain differences in cancer incidence in different countries. For example, gastric cancer is more common in Japan due to its high-salt diet[23] and colon cancer is more common in the United States. Immigrants develop the risk of their new country, often within one generation, suggesting a substantial link between diet and cancer.[24]
Infection
Worldwide approximately 18% of cancer deaths are related to infectious diseases.[2] This proportion varies in different regions of the world from a high of 25% in Africa to less than 10% in the developed world.[2] Viruses are the usual infectious agents that cause cancer but bacteria and parasites may also have an effect.
A virus that can cause cancer is called an oncovirus. These include human papillomavirus (cervical carcinoma), Epstein–Barr virus (B-cell lymphoproliferative disease and nasopharyngeal carcinoma), Kaposi's sarcoma herpesvirus (Kaposi's sarcoma and primary effusion lymphomas), hepatitis B and hepatitis C viruses (hepatocellular carcinoma), and Human T-cell leukemia virus-1 (T-cell leukemias). Bacterial infection may also increase the risk of cancer, as seen in Helicobacter pylori-induced gastric carcinoma.[25] Parasitic infections strongly associated with cancer include Schistosoma haematobium (squamous cell carcinoma of the bladder) and the liver flukes, Opisthorchis viverrini and Clonorchis sinensis (cholangiocarcinoma).[26]
Radiation
Up to 10% of invasive cancers are related to radiation exposure, including both ionizing radiation and non-ionizing ultraviolet radiation.[2] Additionally, the vast majority of non-invasive cancers are non-melanoma skin cancers caused by non-ionizing ultraviolet radiation.
Sources of ionizing radiation include medical imaging, and radon gas. Radiation can cause cancer in most parts of the body, in all animals, and at any age, although radiation-induced solid tumors usually take 10–15 years, and can take up to 40 years, to become clinically manifest, and radiation-induced leukemias typically require 2–10 years to appear.[27] Some people, such as those with nevoid basal cell carcinoma syndrome or retinoblastoma, are more susceptible than average to developing cancer from radiation exposure.[27] Children and adolescents are twice as likely to develop radiation-induced leukemia as adults; radiation exposure before birth has ten times the effect.[27] Ionizing radiation is not a particularly strong mutagen.[27] Residential exposure to radon gas, for example, has similar cancer risks as passive smoking.[27] Low-dose exposures, such as living near a nuclear power plant, are generally believed to have no or very little effect on cancer development.[27] Radiation is a more potent source of cancer when it is combined with other cancer-causing agents, such as radon gas exposure plus smoking tobacco.[27]
Unlike chemical or physical triggers for cancer, ionizing radiation hits molecules within cells randomly. If it happens to strike a chromosome, it can break the chromosome, result in an abnormal number of chromosomes, inactivate one or more genes in the part of the chromosome that it hit, delete parts of the DNA sequence, cause chromosome translocations, or cause other types of chromosome abnormalities.[27] Major damage normally results in the cell dying, but smaller damage may leave a stable, partly functional cell that may be capable of proliferating and developing into cancer, especially if tumor suppressor genes were damaged by the radiation.[27] Three independent stages appear to be involved in the creation of cancer with ionizing radiation: morphological changes to the cell, acquiring cellular immortality (losing normal, life-limiting cell regulatory processes), and adaptations that favor formation of a tumor.[27] Even if the radiation particle does not strike the DNA directly, it triggers responses from cells that indirectly increase the likelihood of mutations.[27]
Medical use of ionizing radiation is a growing source of radiation-induced cancers. Ionizing radiation may be used to treat other cancers, but this may, in some cases, induce a second form of cancer.[27] It is also used in some kinds of medical imaging. One report estimates that approximately 29,000 future cancers could be related to the approximately 70 million CT scans performed in the US in 2007.[28] It is estimated that 0.4% of cancers in 2007 in the United States are due to CTs performed in the past and that this may increase to as high as 1.5–2% with rates of CT usage during this same time period.[29]
Prolonged exposure to ultraviolet radiation from the sun can lead to melanoma and other skin malignancies.[30] Clear evidence establishes ultraviolet radiation, especially the non-ionizing medium wave UVB, as the cause of most non-melanoma skin cancers, which are the most common forms of cancer in the world.[30]
Non-ionizing radio frequency radiation from mobile phones, electric power transmission, and other similar sources have been described as a possible carcinogen by the World Health Organization's International Agency for Research on Cancer.[31] However, studies have not found a consistent link between cell phone radiation and cancer risk.[32]
Heredity
The vast majority of cancers are non-hereditary ("sporadic cancers"). Hereditary cancers are primarily caused by an inherited genetic defect. Less than 0.3% of the population are carriers of a genetic mutation which has a large effect on cancer risk and these cause less than 3–10% of all cancer.[4] Some of these syndromes include: certain inherited mutations in the genes BRCA1 and BRCA2 with a more than 75% risk of breast cancer and ovarian cancer,[4] and hereditary nonpolyposis colorectal cancer (HNPCC or Lynch syndrome) which is present in about 3% of people with colorectal cancer,[33] among others.
Physical agents
Some substances cause cancer primarily through their physical, rather than chemical, effects on cells.[34]
A prominent example of this is prolonged exposure to asbestos, naturally occurring mineral fibers which are a major cause of mesothelioma, which is a cancer of the serous membrane, usually the serous membrane surrounding the lungs.[34] Other substances in this category, including both naturally occurring and synthetic asbestos-like fibers such as wollastonite, attapulgite, glass wool, and rock wool, are believed to have similar effects.[34]
Nonfibrous particulate materials that cause cancer include powdered metallic cobalt and nickel, and crystalline silica (quartz, cristobalite, and tridymite).[34]
Usually, physical carcinogens must get inside the body (such as through inhaling tiny pieces) and require years of exposure to develop cancer.[34]
Physical trauma resulting in cancer is relatively rare.[35] Claims that breaking bone resulted in bone cancer, for example, have never been proven.[35] Similarly, physical trauma is not accepted as a cause for cervical cancer, breast cancer, or brain cancer.[35]
One accepted source is frequent, long-term application of hot objects to the body. It is possible that repeated burns on the same part of the body, such as those produced by kanger and kairo heaters (charcoal hand warmers), may produce skin cancer, especially if carcinogenic chemicals are also present.[35] Frequently drinking scalding hot tea may produce esophageal cancer.[35]
Generally, it is believed that the cancer arises, or a pre-existing cancer is encouraged, during the process of repairing the trauma, rather than the cancer being caused directly by the trauma.[35] However, repeated injuries to the same tissues might promote excessive cell proliferation, which could then increase the odds of a cancerous mutation. There is no evidence that inflammation itself causes cancer.[35]
Hormones
Some hormones play a role in the development of cancer by promoting cell proliferation.[36] Insulin-like growth factors and their binding proteins play a key role in cancer cell proliferation, differentiation and apoptosis, suggesting possible involvement in carcinogenesis.[37]
Hormones are important agents in sex-related cancers such as cancer of the breast, endometrium, prostate, ovary, and testis, and also of thyroid cancer and bone cancer.[36] For example, the daughters of women who have breast cancer have significantly higher levels of estrogen and progesterone than the daughters of women without breast cancer. These higher hormone levels may explain why these women have higher risk of breast cancer, even in the absence of a breast-cancer gene.[36] Similarly, men of African ancestry have significantly higher levels of testosterone than men of European ancestry, and have a correspondingly much higher level of prostate cancer.[36] Men of Asian ancestry, with the lowest levels of testosterone-activating androstanediol glucuronide, have the lowest levels of prostate cancer.[36]
Other factors are also relevant: obese people have higher levels of some hormones associated with cancer and a higher rate of those cancers.[36] Women who take hormone replacement therapy have a higher risk of developing cancers associated with those hormones.[36] On the other hand, people who exercise far more than average have lower levels of these hormones, and lower risk of cancer.[36] Osteosarcoma may be promoted by growth hormones.[36] Some treatments and prevention approaches leverage this cause by artificially reducing hormone levels, and thus discouraging hormone-sensitive cancers.[36]
Other
Excepting the rare transmissions that occur with pregnancies and only a marginal few organ donors, cancer is generally not a transmissible disease. The main reason for this is tissue graft rejection caused by MHC incompatibility.[38] In humans and other vertebrates, the immune system uses MHC antigens to differentiate between "self" and "non-self" cells because these antigens are different from person to person. When non-self antigens are encountered, the immune system reacts against the appropriate cell. Such reactions may protect against tumour cell engraftment by eliminating implanted cells. In the United States, approximately 3,500 pregnant women have a malignancy annually, and transplacental transmission of acute leukemia, lymphoma, melanoma and carcinoma from mother to fetus has been observed.[38] The development of donor-derived tumors from organ transplants is exceedingly rare. The main cause of organ transplant associated tumors seems to be malignant melanoma, that was undetected at the time of organ harvest.[39] Job stress does not appear to be a significant factor at least in lung, colorectal, breast and prostate cancers.[40]
Pathophysiology
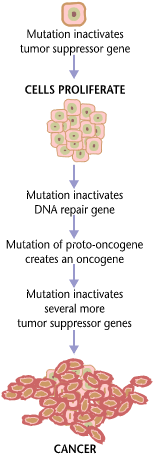
Genetic alterations
Cancer is fundamentally a disease of failure of regulation of tissue growth. In order for a normal cell to transform into a cancer cell, the genes which regulate cell growth and differentiation must be altered.[41]
The affected genes are divided into two broad categories. Oncogenes are genes which promote cell growth and reproduction. Tumor suppressor genes are genes which inhibit cell division and survival. Malignant transformation can occur through the formation of novel oncogenes, the inappropriate over-expression of normal oncogenes, or by the under-expression or disabling of tumor suppressor genes. Typically, changes in many genes are required to transform a normal cell into a cancer cell.[42]
Genetic changes can occur at different levels and by different mechanisms. The gain or loss of an entire chromosome can occur through errors in mitosis. More common are mutations, which are changes in the nucleotide sequence of genomic DNA.
Large-scale mutations involve the deletion or gain of a portion of a chromosome. Genomic amplification occurs when a cell gains many copies (often 20 or more) of a small chromosomal locus, usually containing one or more oncogenes and adjacent genetic material. Translocation occurs when two separate chromosomal regions become abnormally fused, often at a characteristic location. A well-known example of this is the Philadelphia chromosome, or translocation of chromosomes 9 and 22, which occurs in chronic myelogenous leukemia, and results in production of the BCR-abl fusion protein, an oncogenic tyrosine kinase.
Small-scale mutations include point mutations, deletions, and insertions, which may occur in the promoter region of a gene and affect its expression, or may occur in the gene's coding sequence and alter the function or stability of its protein product. Disruption of a single gene may also result from integration of genomic material from a DNA virus or retrovirus, and resulting in the expression of viral oncogenes in the affected cell and its descendants.
Replication of the enormous amount of data contained within the DNA of living cells will probabilistically result in some errors (mutations). Complex error correction and prevention is built into the process, and safeguards the cell against cancer. If significant error occurs, the damaged cell can "self-destruct" through programmed cell death, termed apoptosis. If the error control processes fail, then the mutations will survive and be passed along to daughter cells.
Some environments make errors more likely to arise and propagate. Such environments can include the presence of disruptive substances called carcinogens, repeated physical injury, heat, ionising radiation, or hypoxia[43]
The errors which cause cancer are self-amplifying and compounding, for example:
- A mutation in the error-correcting machinery of a cell might cause that cell and its children to accumulate errors more rapidly.
- A further mutation in an oncogene might cause the cell to reproduce more rapidly and more frequently than its normal counterparts.
- A further mutation may cause loss of a tumour suppressor gene, disrupting the apoptosis signalling pathway and resulting in the cell becoming immortal.
- A further mutation in signaling machinery of the cell might send error-causing signals to nearby cells.
The transformation of normal cell into cancer is akin to a chain reaction caused by initial errors, which compound into more severe errors, each progressively allowing the cell to escape the controls that limit normal tissue growth. This rebellion-like scenario becomes an undesirable survival of the fittest, where the driving forces of evolution work against the body's design and enforcement of order. Once cancer has begun to develop, this ongoing process, termed clonal evolution drives progression towards more invasive stages.[44]
Epigenetic alterations

Classically, cancer has been viewed as a set of diseases that are driven by progressive genetic abnormalities that include mutations in tumour-suppressor genes and oncogenes, and chromosomal abnormalities. However, it has become apparent that cancer is also driven by epigenetic alterations.[45]
Epigenetic alterations refer to functionally relevant modifications to the genome that do not involve a change in the nucleotide sequence. Examples of such modifications are changes in DNA methylation (hypermethylation and hypomethylation) and histone modification [46] and changes in chromosomal architecture (caused by inappropriate expression of proteins such as HMGA2 or HMGA1).[47] Each of these epigenetic alterations serves to regulate gene expression without altering the underlying DNA sequence. These changes may remain through cell divisions, last for multiple generations, and can be considered to be epimutations (equivalent to mutations).
Epigenetic alterations occur frequently in cancers. As an example, Schnekenburger and Diederich[48] listed protein coding genes that were frequently altered in their methylation in association with colon cancer. These included 147 hypermethylated and 27 hypomethylated genes. Of the hypermethylated genes, 10 were hypermethylated in 100% of colon cancers, and many others were hypermethylated in more than 50% of colon cancers.
While large numbers of epigenetic alterations are found in cancers, the epigenetic alterations in DNA repair genes, causing reduced expression of DNA repair proteins, may be of particular importance. Such alterations are thought to occur early in progression to cancer and to be a likely cause of the genetic instability characteristic of cancers.[49][50][51][52]
Reduced expression of DNA repair genes causes deficient DNA repair. This is shown in the figure at the 4th level from the top. (In the figure, red wording indicates the central role of DNA damage and defects in DNA repair in progression to cancer.) When DNA repair is deficient DNA damages remain in cells at a higher than usual level (5th level from the top in figure), and these excess damages cause increased frequencies of mutation and/or epimutation (6th level from top of figure). Mutation rates increase substantially in cells defective in DNA mismatch repair[53][54] or in homologous recombinational repair (HRR).[55] Chromosomal rearrangements and aneuploidy also increase in HRR defective cells.[56]
Higher levels of DNA damage not only cause increased mutation (right side of figure), but also cause increased epimutation. During repair of DNA double strand breaks, or repair of other DNA damages, incompletely cleared sites of repair can cause epigenetic gene silencing.[57][58]
Deficient expression of DNA repair proteins due to an inherited mutation can cause increased risk of cancer. Individuals with an inherited impairment in any of 34 DNA repair genes (see article DNA repair-deficiency disorder) have an increased risk of cancer, with some defects causing up to a 100% lifetime chance of cancer (e.g. p53 mutations).[59] Germ line DNA repair mutations are noted in a box on the left side of the figure, with an arrow indicating their contribution to DNA repair deficiency. However, such germline mutations (which cause highly penetrant cancer syndromes) are the cause of only about 1 percent of cancers.[60]
In sporadic cancers, deficiencies in DNA repair are occasionally caused by a mutation in a DNA repair gene, but are much more frequently caused by epigenetic alterations that reduce or silence expression of DNA repair genes. This is indicated in the figure at the 3rd level from the top. For example, when 113 colorectal cancers were examined in sequence, only four had a missense mutation in the DNA repair gene MGMT, while the majority had reduced MGMT expression due to methylation of the MGMT promoter region (an epigenetic alteration).[61] Five different studies found that between 40% and 90% of colorectal cancers have reduced MGMT expression due to methylation of the MGMT promoter region.[62][63][64][65][66]
Similarly, out of 119 cases of mismatch repair-deficient colorectal cancers that lacked DNA repair gene PMS2 expression, PMS2 was deficient in 6 due to mutations in the PMS2 gene, while in 103 cases PMS2 expression was deficient because its pairing partner MLH1 was repressed due to promoter methylation (PMS2 protein is unstable in the absence of MLH1).[67] In the other 10 cases, loss of PMS2 expression was likely due to epigenetic overexpression of the microRNA, miR-155, which down-regulates MLH1.[68]
In further examples, tabulated in the article Epigenetics, epigenetic defects were found at frequencies of between 13%-100% for the DNA repair genes BRCA1, WRN, FANCB, FANCF, MGMT, MLH1, MSH2, MSH4, ERCC1, XPF, NEIL1 and ATM in cancers including those in breast, ovarian, colorectal, and head and neck. In particular, two or more epigenetic deficiencies in expression of ERCC1, XPF and/or PMS2 occurred simultaneously in the majority of the 49 colon cancers evaluated by Facista et al.[69]
Many studies of heavy metal-induced carcinogenesis show that such heavy metals cause reduction in expression of DNA repair enzymes, some through epigenetic mechanisms. In some cases, DNA repair inhibition is proposed to be a predominant mechanism in heavy metal-induced carcinogenicity. For example, one group of studies shows that arsenic inhibits the DNA repair genes PARP, XRCC1, Ligase III, Ligase IV, DNA POLB, XRCC4, DNA PKCS, TOPO2B, OGG1, ERCC1, XPF, XPB, XPC, XPE and P53.[70][71][72][73][74][75] Another group of studies shows that cadmium inhibits the DNA repair genes MSH2, ERCC1, XRCC1, OGG1, MSH6, DNA-PK, XPD and XPC.[76][77][78][79][80]
Cancers usually arise from an assemblage of mutations and epimutations that confer a selective advantage leading to clonal expansion (see Field defects in progression to cancer). Mutations, however, may not be as frequent in cancers as epigenetic alterations. An average cancer of the breast or colon can have about 60 to 70 protein-altering mutations, of which about 3 or 4 may be “driver” mutations, and the remaining ones may be “passenger” mutations.[81] Colon cancers were also found to have an average of 17 duplicated segments of chromosomes, 28 deleted segments of chromosomes and up to 10 translocations.[82] However, by comparison, epigenetic alterations appear to be more frequent in colon cancers. There are large numbers of hypermethylated genes in colon cancer, as discussed above.[48]
In addition, there are frequent epigenetic alterations of the DNA sequences coding for small RNAs called microRNAs (or miRNAs). MiRNAs do not code for proteins, but can “target” protein-coding genes and reduce their expression. For instance, epigenetic increase in CpG island methylation of the DNA sequence encoding miR-137 reduces its expression and is a frequent early epigenetic event in colorectal carcinogenesis, occurring in 81% of colon cancers and in 14% of the normal appearing colonic mucosa adjacent to the cancers. Silencing of miR-137 can affect expression of over 400 genes, the targets of this miRNA.[83] Changes in the level of miR-137 expression cause altered mRNA expression of the target genes by 2 to 20-fold and corresponding, though often smaller, changes in expression of the protein products of the genes. Other microRNAs, with likely comparable numbers of target genes, are even more frequently epigenetically altered in colonic field defects and in the colon cancers that arise from them. These include miR-124a, miR-34b/c and miR-342 which are silenced by CpG island methylation of their encoding DNA sequences in primary tumors at rates of 99%, 93% and 86%, respectively, and in the adjacent normal appearing mucosa at rates of 59%, 26% and 56%, respectively.[84][85] Thus, epigenetic alterations are a major source of changes in gene expression, important in cancer.
As pointed out above under genetic alterations, cancer is caused by failure to regulate tissue growth, when the genes which regulate cell growth and differentiation are altered. It has become clear that these alterations are caused by both DNA sequence mutation in oncogenes and tumor suppressor genes as well as by epigenetic alterations. The epigenetic deficiencies in expression of DNA repair genes, in particular, likely cause an increased frequency of mutations, some of which then occur in oncogenes and tumor suppressor genes.
Diagnosis

Most cancers are initially recognized either because of the appearance of signs or symptoms or through screening. Neither of these lead to a definitive diagnosis, which requires the examination of a tissue sample by a pathologist. People with suspected cancer are investigated with medical tests. These commonly include blood tests, X-rays, CT scans and endoscopy.
Classification
Cancers are classified by the type of cell that the tumor cells resemble and is therefore presumed to be the origin of the tumor. These types include:
- Carcinoma: Cancers derived from epithelial cells. This group includes many of the most common cancers, particularly in the aged, and include nearly all those developing in the breast, prostate, lung, pancreas, and colon.
- Sarcoma: Cancers arising from connective tissue (i.e. bone, cartilage, fat, nerve), each of which develop from cells originating in mesenchymal cells outside the bone marrow.
- Lymphoma and leukemia: These two classes of cancer arise from hematopoietic (blood-forming) cells that leave the marrow and tend to mature in the lymph nodes and blood, respectively. Leukemia is the most common type of cancer in children accounting for about 30%.[86]
- Germ cell tumor: Cancers derived from pluripotent cells, most often presenting in the testicle or the ovary (seminoma and dysgerminoma, respectively).
- Blastoma: Cancers derived from immature "precursor" cells or embryonic tissue. Blastomas are more common in children than in older adults.
Cancers are usually named using -carcinoma, -sarcoma or -blastoma as a suffix, with the Latin or Greek word for the organ or tissue of origin as the root. For example, cancers of the liver parenchyma arising from malignant epithelial cells is called hepatocarcinoma, while a malignancy arising from primitive liver precursor cells is called a hepatoblastoma, and a cancer arising from fat cells is called a liposarcoma. For some common cancers, the English organ name is used. For example, the most common type of breast cancer is called ductal carcinoma of the breast. Here, the adjective ductal refers to the appearance of the cancer under the microscope, which suggests that it has originated in the milk ducts.
Benign tumors (which are not cancers) are named using -oma as a suffix with the organ name as the root. For example, a benign tumor of smooth muscle cells is called a leiomyoma (the common name of this frequently occurring benign tumor in the uterus is fibroid). Confusingly, some types of cancer use the -noma suffix, examples including melanoma and seminoma.
Some types of cancer are named for the size and shape of the cells under a microscope, such as giant cell carcinoma, spindle cell carcinoma, and small-cell carcinoma.
Pathology
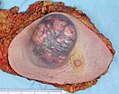
The tissue diagnosis given by the pathologist indicates the type of cell that is proliferating, its histological grade, genetic abnormalities, and other features of the tumor. Together, this information is useful to evaluate the prognosis of the patient and to choose the best treatment. Cytogenetics and immunohistochemistry are other types of testing that the pathologist may perform on the tissue specimen. These tests may provide information about the molecular changes (such as mutations, fusion genes, and numerical chromosome changes) that has happened in the cancer cells, and may thus also indicate the future behavior of the cancer (prognosis) and best treatment.
-
An invasive ductal carcinoma of the breast (pale area at the center) surrounded by spikes of whitish scar tissue and yellow fatty tissue.
-
An invasive colorectal carcinoma (top center) in a colectomy specimen.
-
A squamous-cell carcinoma (the whitish tumor) near the bronchi in a lung specimen.
-
A large invasive ductal carcinoma in a mastectomy specimen.
Prevention
Cancer prevention is defined as active measures to decrease the risk of cancer.[87] The vast majority of cancer cases are due to environmental risk factors, and many, but not all, of these environmental factors are controllable lifestyle choices. Thus, cancer is considered a largely preventable disease.[88] Greater than 30% of cancer deaths could be prevented by avoiding risk factors including: tobacco, overweight / obesity, an insufficient diet, physical inactivity, alcohol, sexually transmitted infections, and air pollution.[89] Not all environmental causes are controllable, such as naturally occurring background radiation, and other cases of cancer are caused through hereditary genetic disorders, and thus it is not possible to prevent all cases of cancer.
Dietary
While many dietary recommendations have been proposed to reduce the risk of cancer, few have significant supporting scientific evidence.[90] The primary dietary factors that increase risk are obesity and alcohol consumption; with a diet low in fruits and vegetables and high in red meat being implicated but not confirmed.[91][92] Consumption of coffee is associated with a reduced risk of liver cancer.[93] Studies have linked consumption of red or processed meat to an increased risk of breast cancer, colon cancer, and pancreatic cancer, a phenomenon which could be due to the presence of carcinogens in meats cooked at high temperatures.[94][95] Dietary recommendations for cancer prevention typically include an emphasis on vegetables, fruit, whole grains, and fish, and an avoidance of red meat, animal fats and refined carbohydrates. However, these recommendations are based on relatively limited evidence.[90]
Medication
The concept that medications can be used to prevent cancer is attractive, and evidence supports their use in a few defined circumstances.[96] In the general population NSAIDs reduce the risk of colorectal cancer however due to the cardiovascular and gastrointestinal side effects they cause overall harm when used for prevention.[97] Aspirin has been found to reduce the risk of death from cancer by about 7%.[98] COX-2 inhibitor may decrease the rate of polyp formation in people with familial adenomatous polyposis however are associated with the same adverse effects as NSAIDs.[99] Daily use of tamoxifen or raloxifene has been demonstrated to reduce the risk of developing breast cancer in high-risk women.[100] The benefit verses harm for 5-alpha-reductase inhibitor such as finasteride is not clear.[101]
Vitamins have not been found to be effective at preventing cancer,[102] although low blood levels of vitamin D are correlated with increased cancer risk.[103][104] Whether this relationship is causal and vitamin D supplementation is protective is not determined.[105] Beta-Carotene supplementation has been found to increase lung cancer rates in those who are high risk.[106] Folic acid supplementation has not been found effective in preventing colon cancer and may increase colon polyps.[107]
Vaccination
Vaccines have been developed that prevent some infection by some viruses.[108] Human papillomavirus vaccine (Gardasil and Cervarix) decreases the risk of developing cervical cancer.[108] The hepatitis B vaccine prevents infection with hepatitis B virus and thus decreases the risk of liver cancer.[108]
Screening
Unlike diagnosis efforts prompted by symptoms and medical signs, cancer screening involves efforts to detect cancer after it has formed, but before any noticeable symptoms appear.[109] This may involve physical examination, blood or urine tests, or medical imaging.[109]
Cancer screening is currently not possible for many types of cancers, and even when tests are available, they may not be recommended for everyone. Universal screening or mass screening involves screening everyone.[110] Selective screening identifies people who are known to be at higher risk of developing cancer, such as people with a family history of cancer.[110] Several factors are considered to determine whether the benefits of screening outweigh the risks and the costs of screening.[109] These factors include:
- Possible harms from the screening test: for example, X-ray images involve exposure to potentially harmful ionizing radiation.
- The likelihood of the test correctly identifying cancer.
- The likelihood of cancer being present: Screening is not normally useful for rare cancers.
- Possible harms from follow-up procedures.
- Whether suitable treatment is available.
- Whether early detection improves treatment outcomes.
- Whether the cancer will ever need treatment.
- Whether the test is acceptable to the people: If a screening test is too burdensome (for example, being extremely painful), then people will refuse to participate.[110]
- Cost of the test.
Recommendations
The U.S. Preventive Services Task Force (USPSTF) strongly recommends cervical cancer screening in women who are sexually active and have a cervix at least until the age of 65.[111] They recommend that Americans be screened for colorectal cancer via fecal occult blood testing, sigmoidoscopy, or colonoscopy starting at age 50 until age 75.[112] There is insufficient evidence to recommend for or against screening for skin cancer,[113] oral cancer,[114] lung cancer,[115] or prostate cancer in men under 75.[116] Routine screening is not recommended for bladder cancer,[117] testicular cancer,[118] ovarian cancer,[119] pancreatic cancer,[120] or prostate cancer.[121]
The USPSTF recommends mammography for breast cancer screening every two years for those 50–74 years old; however, they do not recommend either breast self-examination or clinical breast examination.[122] A 2011 Cochrane review came to slightly different conclusions with respect to breast cancer screening stating that routine mammography may do more harm than good.[123]
Japan screens for gastric cancer using photofluorography due to the high incidence there.[5]
Genetic testing
| Gene | Cancer types |
|---|---|
| BRCA1, BRCA2 | Breast, ovarian, pancreatic |
| HNPCC, MLH1, MSH2, MSH6, PMS1, PMS2 | Colon, uterine, small bowel, stomach, urinary tract |
Genetic testing for individuals at high-risk of certain cancers is recommended.[124] Carriers of these mutations may then undergo enhanced surveillance, chemoprevention, or preventative surgery to reduce their subsequent risk.[124]
Management
Many management options for cancer exist with the primary ones including surgery, chemotherapy, radiation therapy, and palliative care. Which treatments are used depends upon the type, location and grade of the cancer as well as the person's health and wishes.
Palliative care
Palliative care refers to treatment which attempts to make the patient feel better and may or may not be combined with an attempt to attack the cancer. Palliative care includes action to reduce the physical, emotional, spiritual, and psycho-social distress experienced by people with cancer. Unlike treatment that is aimed at directly killing cancer cells, the primary goal of palliative care is to improve the patient's quality of life.
Patients at all stages of cancer treatment need some kind of palliative care to comfort them. In some cases, medical specialty professional organizations recommend that patients and physicians respond to cancer only with palliative care and not with cancer-directed therapy.[125] Those cases have the following characteristics:[126]
- patient has low performance status, corresponding with limited ability to care for oneself[125]
- patient received no benefit from prior evidence-based treatments[125]
- patient is ineligible to participate in any appropriate clinical trial[125]
- the physician sees no strong evidence that treatment would be effective[125]
Palliative care is often confused with hospice and therefore only involved when people approach end of life. Like hospice care, palliative care attempts to help the person cope with the immediate needs and to increase the person's comfort. Unlike hospice care, palliative care does not require people to stop treatment aimed at prolonging their lives or curing the cancer.
Multiple national medical guidelines recommend early palliative care for people whose cancer has produced distressing symptoms (pain, shortness of breath, fatigue, nausea) or who need help coping with their illness. In people who have metastatic disease when first diagnosed, oncologists should consider a palliative care consult immediately. Additionally, an oncologist should consider a palliative care consult in any patient they feel has a prognosis of less than 12 months even if continuing aggressive treatment.[127][128][129]
Surgery
Surgery is the primary method of treatment of most isolated solid cancers and may play a role in palliation and prolongation of survival. It is typically an important part of making the definitive diagnosis and staging the tumor as biopsies are usually required. In localized cancer surgery typically attempts to remove the entire mass along with, in certain cases, the lymph nodes in the area. For some types of cancer this is all that is needed to eliminate the cancer.[130]
Chemotherapy
Chemotherapy in addition to surgery has proven useful in a number of different cancer types including: breast cancer, colorectal cancer, pancreatic cancer, osteogenic sarcoma, testicular cancer, ovarian cancer, and certain lung cancers.[130] The effectiveness of chemotherapy is often limited by toxicity to other tissues in the body.
Radiation
Radiation therapy involves the use of ionizing radiation in an attempt to either cure or improve the symptoms of cancer. It is used in about half of all cases and the radiation can be from either internal sources in the form of brachytherapy or external sources. Radiation is typically used in addition to surgery and or chemotherapy but for certain types of cancer such as early head and neck cancer may be used alone. For painful bone metastasis it has been found to be effective in about 70% of people.[131]
Alternative treatments
Complementary and alternative cancer treatments are a diverse group of health care systems, practices, and products that are not part of conventional medicine.[132] "Complementary medicine" refers to methods and substances used along with conventional medicine, while "alternative medicine" refers to compounds used instead of conventional medicine.[133] Most complementary and alternative medicines for cancer have not been rigorously studied or tested. Some alternative treatments have been investigated and shown to be ineffective but still continue to be marketed and promoted.[134]
Prognosis
Cancer has a reputation as a deadly disease. Taken as a whole, about half of people receiving treatment for invasive cancer (excluding carcinoma in situ and non-melanoma skin cancers) die from cancer or its treatment.[5] Survival is worse in the developing world.[5] However, the survival rates vary dramatically by type of cancer, with the range running from basically all people surviving to almost no one surviving.
Those who survive cancer are at increased risk of developing a second primary cancer at about twice the rate of those never diagnosed with cancer.[135] The increased risk is believed to be primarily due to the same risk factors that produced the first cancer, partly due to the treatment for the first cancer, and potentially related to better compliance with screening.[135]
Predicting either short-term or long-term survival is difficult and depends on many factors. The most important factors are the particular kind of cancer and the patient's age and overall health. People who are frail with many other health problems have lower survival rates than otherwise healthy people. A centenarian is unlikely to survive for five years even if the treatment is successful. People who report a higher quality of life tend to survive longer.[136] People with lower quality of life may be affected by major depressive disorder and other complications from cancer treatment and/or disease progression that both impairs their quality of life and reduces their quantity of life. Additionally, patients with worse prognoses may be depressed or report a lower quality of life directly because they correctly perceive that their condition is likely to be fatal.
Epidemiology

In 2008 approximately 12.7 million cancers were diagnosed (excluding non-melanoma skin cancers and other non-invasive cancers) and 7.6 million people died of cancer worldwide.[5] Cancers as a group account for approximately 13% of all deaths each year with the most common being: lung cancer (1.4 million deaths), stomach cancer (740,000 deaths), liver cancer (700,000 deaths), colorectal cancer (610,000 deaths), and breast cancer (460,000 deaths).[138] This makes invasive cancer the leading cause of death in the developed world and the second leading cause of death in the developing world.[5] Over half of cases occur in the developing world.[5]
Global cancer rates have been increasing primarily due to an aging population and lifestyle changes in the developing world.[5] The most significant risk factor for developing cancer is old age.[139] Although it is possible for cancer to strike at any age, most people who are diagnosed with invasive cancer are over the age of 65.[139] According to cancer researcher Robert A. Weinberg, "If we lived long enough, sooner or later we all would get cancer."[140] Some of the association between aging and cancer is attributed to immunosenescence,[141] errors accumulated in DNA over a lifetime,[142] and age-related changes in the endocrine system.[143]
Some slow-growing cancers are particularly common. Autopsy studies in Europe and Asia have shown that up to 36% of people have undiagnosed and apparently harmless thyroid cancer at the time of their deaths, and that 80% of men develop prostate cancer by age 80.[144][145] As these cancers did not cause the person's death, identifying them would have represented overdiagnosis rather than useful medical care.
The three most common childhood cancers are leukemia (34%), brain tumors (23%), and lymphomas (12%).[146] Rates of childhood cancer have increased by 0.6% per year between 1975 to 2002 in the United States[147] and by 1.1% per year between 1978 and 1997 in Europe.[146]
History

The earliest written record regarding cancer is from 3000 BC in the Egyptian Edwin Smith Papyrus and describes cancer of the breast.[148] Cancer however has existed for all of human history.[148] Hippocrates (ca. 460 BC – ca. 370 BC) described several kinds of cancer, referring to them with the Greek word καρκίνος karkinos (crab or crayfish).[148] This name comes from the appearance of the cut surface of a solid malignant tumour, with "the veins stretched on all sides as the animal the crab has its feet, whence it derives its name".[149] Celsus (ca. 25 BC – 50 AD) translated karkinos into the Latin cancer, also meaning crab and recommended surgery as treatment.[148] Galen (2nd century AD) disagreed with the use of surgery and recommended purgatives instead.[148] These recommendations largely stood for 1000 years.[148]
In the 15th, 16th and 17th centuries, it became more acceptable for doctors to dissect bodies to discover the cause of death.[150] The German professor Wilhelm Fabry believed that breast cancer was caused by a milk clot in a mammary duct. The Dutch professor Francois de la Boe Sylvius, a follower of Descartes, believed that all disease was the outcome of chemical processes, and that acidic lymph fluid was the cause of cancer. His contemporary Nicolaes Tulp believed that cancer was a poison that slowly spreads, and concluded that it was contagious.[151]
The physician John Hill described tobacco snuff as the cause of nose cancer in 1761.[150] This was followed by the report in 1775 by British surgeon Percivall Pott that cancer of the scrotum was a common disease among chimney sweeps.[152] With the widespread use of the microscope in the 18th century, it was discovered that the 'cancer poison' spread from the primary tumor through the lymph nodes to other sites ("metastasis"). This view of the disease was first formulated by the English surgeon Campbell De Morgan between 1871 and 1874.[153]
Society and culture
Though many diseases (such as heart failure) may have a worse prognosis than most cases of cancer, cancer is the subject of widespread fear and taboos. The euphemism, "after a long illness" is still commonly used (2012), reflecting an apparent stigma.[154] This deep belief that cancer is necessarily a difficult and usually deadly disease is reflected in the systems chosen by society to compile cancer statistics: the most common form of cancer—non-melanoma skin cancers, accounting for about one-third of all cancer cases worldwide, but very few deaths[155][156]—are excluded from cancer statistics specifically because they are easily treated and almost always cured, often in a single, short, outpatient procedure.[157]
Cancer is regarded as a disease that must be "fought" to end the "civil insurrection"; a War on Cancer has been declared. Military metaphors are particularly common in descriptions of cancer's human effects, and they emphasize both the parlous state of the affected individual's health and the need for the individual to take immediate, decisive actions himself, rather than to delay, to ignore, or to rely entirely on others caring for him. The military metaphors also help rationalize radical, destructive treatments.[158][159]
In the 1970s, a relatively popular alternative cancer treatment was a specialized form of talk therapy, based on the idea that cancer was caused by a bad attitude.[160] People with a "cancer personality"—depressed, repressed, self-loathing, and afraid to express their emotions—were believed to have manifested cancer through subconscious desire. Some psychotherapists said that treatment to change the patient's outlook on life would cure the cancer.[160] Among other effects, this belief allows society to blame the victim for having caused the cancer (by "wanting" it) or having prevented its cure (by not becoming a sufficiently happy, fearless, and loving person).[161] It also increases patients' anxiety, as they incorrectly believe that natural emotions of sadness, anger or fear shorten their lives.[161] The idea was excoriated by the notoriously outspoken Susan Sontag, who published Illness as Metaphor while recovering from treatment for breast cancer in 1978.[160] Although the original idea is now generally regarded as nonsense, the idea partly persists in a reduced form with a widespread, but incorrect, belief that deliberately cultivating a habit of positive thinking will increase survival.[161] This notion is particularly strong in breast cancer culture.[161]
In 2007, the overall costs of cancer in the U.S. — including treatment and indirect mortality expenses (such as lost productivity in the workplace) — was estimated to be $226.8 billion. In 2009, 32% of Hispanics and 10% of children 17 years old or younger lacked health insurance; "uninsured patients and those from ethnic minorities are substantially more likely to be diagnosed with cancer at a later stage, when treatment can be more extensive and more costly."[162]
Research
Because cancer is a class of diseases,[163][164] it is unlikely that there will ever be a single "cure for cancer" any more than there will be a single treatment for all infectious diseases.[165] Angiogenesis inhibitors were once thought to have potential as a "silver bullet" treatment applicable to many types of cancer, but this has not been the case in practice.[166]
Experimental cancer treatments are treatments that are being studied to see whether they work. Typically, these are studied in clinical trials to compare the proposed treatment to the best existing treatment. They may be entirely new treatments, or they may be treatments that have been used successfully in one type of cancer, and are now being tested to see whether they are effective in another type.[167] More and more, such treatments are being developed alongside companion diagnostic tests to target the right drugs to the right patients, based on their individual biology.[168]
Cancer research is the intense scientific effort to understand disease processes and discover possible therapies.
Research about cancer causes focuses on the following issues:
- Agents (e.g. viruses) and events (e.g. mutations) which cause or facilitate genetic changes in cells destined to become cancer.
- The precise nature of the genetic damage, and the genes which are affected by it.
- The consequences of those genetic changes on the biology of the cell, both in generating the defining properties of a cancer cell, and in facilitating additional genetic events which lead to further progression of the cancer.
The improved understanding of molecular biology and cellular biology due to cancer research has led to a number of new treatments for cancer since U.S. President Nixon declared the "War on Cancer" in 1971. Since then, the U.S. has spent over $200 billion on cancer research, including resources from the public and private sectors and foundations.[169] During that time, the country has seen a five percent decrease in the cancer death rate (adjusting for size and age of the population) between 1950 and 2005.[170] Phytochemicals from dietary plants and spices have been shown to prevent cancer initiation, promotion, and progression by exerting anti-inflammatory and anti-oxidative stress effects, and have been shown to induce apoptosis in cancer cells and suppress tumor growth in vivo.[171]
Pregnancy
Because cancer is largely a disease of older adults, it is not common in pregnant women. Cancer affects approximately 1 in 1,000 pregnant women.[172] The most common cancers found during pregnancy are the same as the most common cancers found in non-pregnant women during childbearing ages: breast cancer, cervical cancer, leukemia, lymphoma, melanoma, ovarian cancer, and colorectal cancer.[172]
Diagnosing a new cancer in a pregnant woman is difficult, in part because any symptoms are commonly assumed to be a normal discomfort associated with pregnancy.[172] As a result, cancer is typically discovered at a somewhat later stage than average in many pregnant or recently pregnant women. Some imaging procedures, such as MRIs (magnetic resonance imaging), CT scans, ultrasounds, and mammograms with fetal shielding are considered safe during pregnancy; some others, such as PET scans are not.[172]
Treatment is generally the same as for non-pregnant women.[172] However, radiation and radioactive drugs are normally avoided during pregnancy, especially if the fetal dose might exceed 100 cGy. In some cases, some or all treatments are postponed until after birth if the cancer is diagnosed late in the pregnancy. Early deliveries to speed the start of treatment are not uncommon. Surgery is generally safe, but pelvic surgeries during the first trimester may cause miscarriage. Some treatments, especially certain chemotherapy drugs given during the first trimester, increase the risk of birth defects and pregnancy loss (spontaneous abortions and stillbirths).[172]
Elective abortions are not required and, for the most common forms and stages of cancer, do not improve the likelihood of the mother surviving or being cured.[172] In a few instances, such as advanced uterine cancer, the pregnancy cannot be continued, and in others, such as an acute leukemia discovered early in pregnancy, the pregnant woman may choose to have abortion so that she can begin aggressive chemotherapy without worrying about birth defects.[172]
Some treatments may interfere with the mother's ability to give birth vaginally or to breastfeed her baby.[172] Cervical cancer may require birth by Caesarean section. Radiation to the breast reduces the ability of that breast to produce milk and increases the risk of mastitis. Also, when chemotherapy is being given after birth, many of the drugs pass through breast milk to the baby, which could harm the baby.[172]
Other animals
In non-humans, a few types of transmissible cancer have been described, wherein the cancer spreads between animals by transmission of the tumor cells themselves. This phenomenon is seen in dogs with Sticker's sarcoma, also known as canine transmissible venereal tumor,[173] as well as devil facial tumour disease in Tasmanian devils.
Notes
- ^ "How many different types of cancer are there? : Cancer Research UK : CancerHelp UK". Retrieved 11 May 2012.
- ^ a b c d e f g Anand P, Kunnumakkara AB, Kunnumakara AB, Sundaram C, Harikumar KB, Tharakan ST, Lai OS, Sung B, Aggarwal BB (2008). "Cancer is a preventable disease that requires major lifestyle changes". Pharm. Res. 25 (9): 2097–116. doi:10.1007/s11095-008-9661-9. PMC 2515569. PMID 18626751.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Kinzler, Kenneth W.; Vogelstein, Bert (2002). "Introduction". The genetic basis of human cancer (2nd, illustrated, revised ed.). New York: McGraw-Hill, Medical Pub. Division. p. 5. ISBN 978-0-07-137050-9.
{{cite book}}: External link in|chapterurl=|chapterurl=ignored (|chapter-url=suggested) (help)CS1 maint: multiple names: authors list (link) - ^ a b c Roukos DH (2009). "Genome-wide association studies: how predictable is a person's cancer risk?". Expert Rev Anticancer Ther. 9 (4): 389–92. doi:10.1586/era.09.12. PMID 19374592.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ a b c d e f g h Jemal A, Bray, F, Center, MM, Ferlay, J, Ward, E, Forman, D (2011). "Global cancer statistics". CA: a cancer journal for clinicians. 61 (2): 69–90. doi:10.3322/caac.20107. PMID 21296855.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b c d e Holland Chp. 1
- ^ O'Dell, edited by Michael D. Stubblefield, Michael W. (2009). Cancer rehabilitation principles and practice. New York: Demos Medical. p. 983. ISBN 978-1-933864-33-4.
{{cite book}}:|first=has generic name (help)CS1 maint: multiple names: authors list (link) - ^ Kravchenko J, Akushevich I, Manton, KG (2009). Cancer mortality and morbidity patterns in the U. S. population: an interdisciplinary approach. Berlin: Springer. ISBN 0-387-78192-7.
The term environment refers not only to air, water, and soil but also to substances and conditions at home and at the workplace, including diet, smoking, alcohol, drugs, exposure to chemicals, sunlight, ionizing radiation, electromagnetic fields, infectious agents, etc. Lifestyle, economic and behavioral factors are all aspects of our environment.
{{cite book}}: CS1 maint: multiple names: authors list (link) - ^ a b Sasco AJ, Secretan MB, Straif K (2004). "Tobacco smoking and cancer: a brief review of recent epidemiological evidence". Lung Cancer. 45 Suppl 2: S3–9. doi:10.1016/j.lungcan.2004.07.998. PMID 15552776.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Biesalski HK, Bueno de Mesquita B, Chesson A, Chytil F, Grimble R, Hermus RJ, Köhrle J, Lotan R, Norpoth K, Pastorino U, Thurnham D (1998). "European Consensus Statement on Lung Cancer: risk factors and prevention. Lung Cancer Panel". CA Cancer J Clin. 48 (3): 167–76, discussion 164–6. doi:10.3322/canjclin.48.3.167. PMID 9594919.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Seitz HK, Pöschl G, Simanowski UA (1998). "Alcohol and cancer". Recent Dev Alcohol. 14: 67–95. PMID 9751943.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Schütze M, Boeing H, Pischon T, Rehm J, Kehoe T, Gmel G, Olsen A, Tjønneland AM, Dahm CC, Overvad K, Clavel-Chapelon F, Boutron-Ruault MC, Trichopoulou A, Benetou V, Zylis D, Kaaks R, Rohrmann S, Palli D, Berrino F, Tumino R, Vineis P, Rodríguez L, Agudo A, Sánchez MJ, Dorronsoro M, Chirlaque MD, Barricarte A, Peeters PH, van Gils CH, Khaw KT, Wareham N, Allen NE, Key TJ, Boffetta P, Slimani N, Jenab M, Romaguera D, Wark PA, Riboli E, Bergmann MM (2011). "Alcohol attributable burden of incidence of cancer in eight European countries based on results from prospective cohort study". BMJ. 342: d1584. doi:10.1136/bmj.d1584. PMC 3072472. PMID 21474525.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Kuper H, Boffetta P, Adami HO (2002). "Tobacco use and cancer causation: association by tumour type". J. Intern. Med. 252 (3): 206–24. doi:10.1046/j.1365-2796.2002.01022.x. PMID 12270001.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b Kuper H, Adami HO, Boffetta P (2002). "Tobacco use, cancer causation and public health impact". J. Intern. Med. 251 (6): 455–66. doi:10.1046/j.1365-2796.2002.00993.x. PMID 12028500.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Thun MJ, Jemal A (2006). "How much of the decrease in cancer death rates in the United States is attributable to reductions in tobacco smoking?". Tob Control. 15 (5): 345–7. doi:10.1136/tc.2006.017749. PMC 2563648. PMID 16998161.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Dubey S, Powell CA (2008). "Update in lung cancer 2007". Am. J. Respir. Crit. Care Med. 177 (9): 941–6. doi:10.1164/rccm.200801-107UP. PMC 2720127. PMID 18434333.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Proctor RN (2004). "The global smoking epidemic: a history and status report". Clin Lung Cancer. 5 (6): 371–6. doi:10.3816/CLC.2004.n.016. PMID 15217537.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Irigaray P, Newby JA, Clapp R, Hardell L, Howard V, Montagnier L, Epstein S, Belpomme D (2007). "Lifestyle-related factors and environmental agents causing cancer: an overview". Biomed. Pharmacother. 61 (10): 640–58. doi:10.1016/j.biopha.2007.10.006. PMID 18055160.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b c "WHO calls for prevention of cancer through healthy workplaces" (Press release). World Health Organization. 27 April 2007. Retrieved 13 October 2007.
- ^ "National Institute for Occupational Safety and Health- Occupational Cancer". United States National Institute for Occupational Safety and Health. Retrieved 13 October 2007.
- ^ a b c d Kushi LH, Byers T, Doyle C, Bandera EV, McCullough M, McTiernan A, Gansler T, Andrews KS, Thun MJ (2006). "American Cancer Society Guidelines on Nutrition and Physical Activity for cancer prevention: reducing the risk of cancer with healthy food choices and physical activity". CA Cancer J Clin. 56 (5): 254–81, quiz 313–4. doi:10.3322/canjclin.56.5.254. PMID 17005596.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Park S, Bae J, Nam BH, Yoo KY (2008). "Aetiology of cancer in Asia" (PDF). Asian Pac. J. Cancer Prev. 9 (3): 371–80. PMID 18990005.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Brenner H, Rothenbacher D, Arndt V (2009). "Epidemiology of stomach cancer". Methods Mol. Biol. 472: 467–77. doi:10.1007/978-1-60327-492-0_23. PMID 19107449.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Buell P, Dunn JE (1965). "Cancer mortality among Japanese Issei and Nisei of California". Cancer. 18 (5): 656–64. doi:10.1002/1097-0142(196505)18:5<656::AID-CNCR2820180515>3.0.CO;2-3. PMID 14278899.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Pagano JS, Blaser M, Buendia MA, Damania B, Khalili K, Raab-Traub N, Roizman B (2004). "Infectious agents and cancer: criteria for a causal relation". Semin. Cancer Biol. 14 (6): 453–71. doi:10.1016/j.semcancer.2004.06.009. PMID 15489139.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Samaras V, Rafailidis PI, Mourtzoukou EG, Peppas G, Falagas ME (2010). "Chronic bacterial and parasitic infections and cancer: a review" (PDF). J Infect Dev Ctries. 4 (5): 267–81. PMID 20539059.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b c d e f g h i j k l Little JB (2000). "Chapter 14: Ionizing Radiation". In Kufe DW, Pollock RE, Weichselbaum RR, Bast RC Jr, Gansler TS, Holland JF, Frei E III (ed.). Cancer medicine (6th ed.). Hamilton, Ont: B.C. Decker. ISBN 1-55009-113-1.
{{cite book}}: CS1 maint: multiple names: editors list (link) - ^ Berrington de González A, Mahesh M, Kim KP, Bhargavan M, Lewis R, Mettler F, Land C (2009). "Projected cancer risks from computed tomographic scans performed in the United States in 2007". Arch. Intern. Med. 169 (22): 2071–7. doi:10.1001/archinternmed.2009.440. PMID 20008689.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Brenner DJ, Hall EJ (2007). "Computed tomography—an increasing source of radiation exposure". N. Engl. J. Med. 357 (22): 2277–84. doi:10.1056/NEJMra072149. PMID 18046031.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ a b Cleaver JE, Mitchell DL (2000). "15. Ultraviolet Radiation Carcinogenesis". In Bast RC, Kufe DW, Pollock RE; et al. (eds.). Holland-Frei Cancer Medicine (5th ed.). Hamilton, Ontario: B.C. Decker. ISBN 1-55009-113-1. Retrieved 31 January 2011.
{{cite book}}: Explicit use of et al. in:|editor=(help)CS1 maint: multiple names: editors list (link) - ^ "IARC classifies radiofrequency electromagnetic fields as possibly carcinogenic to humans" (PDF). World Health Organization.
- ^ http://www.cancer.gov/cancertopics/factsheet/Risk/cellphones Cell Phones and Cancer Risk
- ^ Cunningham D, Atkin W, Lenz HJ, Lynch HT, Minsky B, Nordlinger B, Starling N (2010). "Colorectal cancer". Lancet. 375 (9719): 1030–47. doi:10.1016/S0140-6736(10)60353-4. PMID 20304247.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b c d e Maltoni CFM, Holland JF (2000). "Chapter 16: Physical Carcinogens". In Bast RC, Kufe DW, Pollock RE; et al. (eds.). Holland-Frei Cancer Medicine (5th ed.). Hamilton, Ontario: B.C. Decker. ISBN 1-55009-113-1. Retrieved 31 January 2011.
{{cite book}}: Explicit use of et al. in:|editor=(help)CS1 maint: multiple names: editors list (link) - ^ a b c d e f g Gaeta, John F (2000). "Chapter 17: Trauma and Inflammation". In Bast RC, Kufe DW, Pollock RE; et al. (eds.). Holland-Frei Cancer Medicine (5th ed.). Hamilton, Ontario: B.C. Decker. ISBN 1-55009-113-1. Retrieved 27 January 2011.
{{cite book}}: Explicit use of et al. in:|editor=(help)CS1 maint: multiple names: editors list (link) - ^ a b c d e f g h i j Henderson BE, Bernstein L, Ross
RK (2000). "Chapter 13: Hormones and the Etiology of Cancer". In Bast RC, Kufe DW, Pollock RE; et al. (eds.). Holland-Frei Cancer Medicine (5th ed.). Hamilton, Ontario: B.C. Decker. ISBN 1-55009-113-1. Retrieved 27 January 2011.
{{cite book}}: Explicit use of et al. in:|editor=(help); line feed character in|author=at position 32 (help)CS1 maint: multiple names: authors list (link) - ^ Rowlands MA (15 May 2009). "Circulating insulin-like growth factor peptides and prostate cancer risk: a systematic review and meta-analysis". Int J Cancer.: 2416–29. doi:10.1002/ijc.24202. PMID 19142965.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ a b Tolar J, Neglia JP (2003). "Transplacental and other routes of cancer transmission between individuals". J. Pediatr. Hematol. Oncol. 25 (6): 430–4. doi:10.1097/00043426-200306000-00002. PMID 12794519.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Dingli D, Nowak MA (2006). "Cancer biology: infectious tumour cells". Nature. 443 (7107): 35–6. Bibcode:2006Natur.443...35D. doi:10.1038/443035a. PMC 2711443. PMID 16957717.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Heikkilä, K (2013 Feb 7). "Work stress and risk of cancer: meta-analysis of 5700 incident cancer events in 116 000 European men and women". BMJ (Clinical research ed.). 346: f165. PMID 23393080.
{{cite journal}}: Check date values in:|date=(help); Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Croce CM (2008). "Oncogenes and cancer". N. Engl. J. Med. 358 (5): 502–11. doi:10.1056/NEJMra072367. PMID 18234754.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Knudson AG (2001). "Two genetic hits (more or less) to cancer". Nat. Rev. Cancer. 1 (2): 157–62. doi:10.1038/35101031. PMID 11905807.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Nelson DA, Tan TT, Rabson AB, Anderson D, Degenhardt K, White E (2004). "Hypoxia and defective apoptosis drive genomic instability and tumorigenesis". Genes & Development. 18 (17): 2095–107. doi:10.1101/gad.1204904. PMC 515288. PMID 15314031.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Merlo LM, Pepper JW, Reid BJ, Maley CC (2006). "Cancer as an evolutionary and ecological process". Nat. Rev. Cancer. 6 (12): 924–35. doi:10.1038/nrc2013. PMID 17109012.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Baylin SB, Ohm JE (2006). "Epigenetic gene silencing in cancer - a mechanism for early oncogenic pathway addiction?". Nat. Rev. Cancer. 6 (2): 107–16. doi:10.1038/nrc1799. PMID 16491070.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Kanwal R, Gupta S. (2012). Epigenetic modifications in cancer. Clin Genet 81:303-311. PMID 22082348 doi: 10.1111/j.1399-0004.2011.01809.x. http://www.ncbi.nlm.nih.gov/pubmed/22082348
- ^ Baldassarre G, Battista S, Belletti B, Thakur S, Pentimalli F, Trapasso F, Fedele M, Pierantoni G, Croce CM, Fusco A. (2003). Negative regulation of BRCA1 gene expression by HMGA1 proteins accounts for the reduced BRCA1 protein levels in sporadic breast carcinoma. Mol Cell Biol. 2003;23:2225-2238. PMID 12640109 http://www.ncbi.nlm.nih.gov/pmc/articles/PMC150734/
- ^ a b Schnekenburger M, Diederich M. Epigenetics Offer New Horizons for Colorectal Cancer Prevention. Curr Colorectal Cancer Rep 2012;8(1) 66-81. PMID 22389639 http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3277709/
- ^ Jacinto FV, Esteller M (2007). "Mutator pathways unleashed by epigenetic silencing in human cancer". Mutagenesis. 22 (4): 247–53. doi:10.1093/mutage/gem009. PMID 17412712.
{{cite journal}}: Unknown parameter|month=ignored (help) http://mutage.oxfordjournals.org/content/22/4/247.long - ^ Lahtz C, Pfeifer GP (2011). "Epigenetic changes of DNA repair genes in cancer". J Mol Cell Biol. 3 (1): 51–8. doi:10.1093/jmcb/mjq053. PMC 3030973. PMID 21278452.
{{cite journal}}: Unknown parameter|month=ignored (help) http://jmcb.oxfordjournals.org/content/3/1/51.long - ^ Bernstein C, Nfonsam V, Prasad AR, Bernstein H (2013). "Epigenetic field defects in progression to cancer". World J Gastrointest Oncol. 5 (3): 43–9. doi:10.4251/wjgo.v5.i3.43. PMC 3648662. PMID 23671730.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) CS1 maint: unflagged free DOI (link) http://www.wjgnet.com/1948-5204/full/v5/i3/43.htm - ^ Bernstein C, Prasad AR, Nfonsam V, Bernstein H. (2013). DNA Damage, DNA Repair and Cancer, New Research Directions in DNA Repair, Prof. Clark Chen (Ed.), ISBN 978-953-51-1114-6, InTech, http://www.intechopen.com/books/new-research-directions-in-dna-repair/dna-damage-dna-repair-and-cancer
- ^ Narayanan L, Fritzell JA, Baker SM, Liskay RM, Glazer PM. (1997). Elevated levels of mutation in multiple tissues of mice deficient in the DNA mismatch repair gene Pms2. Proc Natl Acad Sci U S A 94(7) 3122-3127. PMID 9096356
- ^ Hegan DC, Narayanan L, Jirik FR, Edelmann W, Liskay RM, Glazer PM. (2006). Differing patterns of genetic instability in mice deficient in the mismatch repair genes Pms2, Mlh1, Msh2, Msh3 and Msh6. Carcinogenesis 27(12) 2402-2408. PMID 16728433
- ^ Tutt AN, van Oostrom CT, Ross GM, van Steeg H, Ashworth A. (2002). Disruption of Brca2 increases the spontaneous mutation rate in vivo: synergism with ionizing radiation. EMBO Rep 3(3) 255-260. PMID 11850397
- ^ German J. (1969). Bloom's syndrome. I. Genetical and clinical observations in the first twenty-seven patients. Am J Hum Genet 21(2) 196-227. PMID 5770175
- ^ O'Hagan HM, Mohammad HP, Baylin SB. (2008) Double strand breaks can initiate gene silencing and SIRT1-dependent onset of DNA methylation in an exogenous promoter CpG island. PLoS Genet. 4(8):e1000155. PMID 18704159
- ^ Cuozzo C, Porcellini A, Angrisano T, Morano A, Lee B, Di Pardo A, Messina S, Iuliano R, Fusco A, Santillo MR, Muller MT, Chiariotti L, Gottesman ME, Avvedimento EV (2007). DNA damage, homology-directed repair, and DNA methylation. PLoS Genet 3(7):e110. PMID 17616978
- ^ Malkin D. (2011). Li-fraumeni syndrome. Genes Cancer 2(4) 475-484. PMID 21779515
- ^ Fearon ER. (1997). Human cancer syndromes: clues to the origin and nature of cancer. Science 278(5340):1043-1050. PMID 9353177
- ^ Halford S, Rowan A, Sawyer E, Talbot I, Tomlinson I (2005). "O(6)-methylguanine methyltransferase in colorectal cancers: detection of mutations, loss of expression, and weak association with G:C>A:T transitions". Gut. 54 (6): 797–802. doi:10.1136/gut.2004.059535. PMC 1774551. PMID 15888787.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) http://www.ncbi.nlm.nih.gov/pubmed - ^ Shen L, Kondo Y, Rosner GL, Xiao L, Hernandez NS, Vilaythong J, Houlihan PS, Krouse RS, Prasad AR, Einspahr JG, Buckmeier J, Alberts DS, Hamilton SR, Issa JP (2005). MGMT promoter methylation and field defect in sporadic colorectal cancer. J Natl Cancer Inst 97(18) 1330-1338. PMID 16174854
- ^ Psofaki V, Kalogera C, Tzambouras N, Stephanou D, Tsianos E, Seferiadis K, Kolios G (2010). Promoter methylation status of hMLH1, MGMT, and CDKN2A/p16 in colorectal adenomas. World J Gastroenterol 16(28) 3553-3560. PMID 20653064 PMCID: PMC2909555
- ^ Lee KH, Lee JS, Nam JH, Choi C, Lee MC, Park CS, Juhng SW, Lee JH (2011). Promoter methylation status of hMLH1, hMSH2, and MGMT genes in colorectal cancer associated with adenoma-carcinoma sequence. Langenbecks Arch Surg 396(7) 1017-1026. PMID 21706233
- ^ Amatu A, Sartore-Bianchi A, Moutinho C, Belotti A, Bencardino K, Chirico G, Cassingena A, Rusconi F, Esposito A, Nichelatti M, Esteller M, Siena S (2013). Promoter CpG Island Hypermethylation of the DNA Repair Enzyme MGMT Predicts Clinical Response to Dacarbazine in a Phase II Study for Metastatic Colorectal Cancer. Clin Cancer Res [Epub ahead of print] PMID 23422094
- ^ Mokarram P, Zamani M, Kavousipour S, Naghibalhossaini F, Irajie C, Moradi Sarabi M, Hosseini SV (2013). Different patterns of DNA methylation of the two distinct O6-methylguanine-DNA methyltransferase (O(6)-MGMT) promoter regions in colorectal cancer. Mol Biol Rep 40(5):3851-3857. doi: 10.1007/s11033-012-2465-3. PMID 23271133
- ^ Truninger K, Menigatti M, Luz J, Russell A, Haider R, Gebbers JO, Bannwart F, Yurtsever H, Neuweiler J, Riehle HM, Cattaruzza MS, Heinimann K, Schär P, Jiricny J, Marra G. (2005). Immunohistochemical analysis reveals high frequency of PMS2 defects in colorectal cancer. Gastroenterology 128:1160-1171. PMID 15887099
- ^ Valeri N, Gasparini P, Fabbri M, Braconi C, Veronese A, Lovat F, Adair B, Vannini I, Fanini F, Bottoni A, Costinean S, Sandhu SK, Nuovo GJ, Alder H, Gafa R, Calore F, Ferracin M, Lanza G, Volinia S, Negrini M, Mcllhatton MA, Amadori D, Fishel R, Croce CM: Modulation of mismatch repair and genomic stability by miR-155. Proc Natl Acad Sci USA 2010, 107:6982-6987. PMID 20351277
- ^ Facista A, Nguyen H, Lewis C, Prasad AR, Ramsey L, Zaitlin B, Nfonsam V, Krouse RS, Bernstein H, Payne CM, Stern S, Oatman N, Banerjee B, Bernstein C. (2012). Deficient expression of DNA repair enzymes in early progression to sporadic colon cancer. Genome Integr. 3(1):3. doi: 10.1186/2041-9414-3-3. PMID 22494821 http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3351028/
- ^ Roy M, Sinha D, Mukherjee S, Biswas J. (2011). Curcumin prevents DNA damage and enhances the repair potential in a chronically arsenic-exposed human population in West Bengal, India. Eur J Cancer Prev 20(2) 123-131. PMID 21332098
- ^ Qin XJ, Liu W, Li YN, Sun X, Hai CX, Hudson LG, Liu KJ. (2012). Poly(ADP-ribose) polymerase-1 inhibition by arsenite promotes the survival of cells with unrepaired DNA lesions induced by UV exposure. Toxicol Sci 127(1) 120-129. PMID 22387748 PMCID: PMC3327874
- ^ Ebert F, Weiss A, Bültemeyer M, Hamann I, Hartwig A, Schwerdtle T. (2011). Arsenicals affect base excision repair by several mechanisms. Mutat Res 2011;715(1-2) 32-41. PMID 21782832
- ^ Andrew AS, Karagas MR, Hamilton JW. (2003). Decreased DNA repair gene expression among individuals exposed to arsenic in United States drinking water. Int J Cancer 104(3) 263-268. PMID 12569548
- ^ Nollen M, Ebert F, Moser J, Mullenders LH, Hartwig A, Schwerdtle T. (2009). Impact of arsenic on nucleotide excision repair: XPC function, protein level, and gene expression. Mol Nutr Food Res 53(5) 572-582. PMID 19382146
- ^ Shen S, Lee J, Weinfeld M, Le XC. (2008). Attenuation of DNA damage-induced p53 expression by arsenic: a possible mechanism for arsenic co-carcinogenesis. Mol Carcinog 47(7) 508-518. PMID 18085531
- ^ Zhou ZH, Lei YX, Wang CX. (2012). Analysis of aberrant methylation in DNA repair genes during malignant transformation of human bronchial epithelial cells induced by cadmium. Toxicol Sci 125(2) 412-417. PMID 22112500
- ^ Wieland M, Levin MK, Hingorani KS, Biro FN, Hingorani MM. (2009). Mechanism of cadmium-mediated inhibition of Msh2-Msh6 function in DNA mismatch repair. Biochemistry 2009;48(40) 9492-9502. PMID 19320425
- ^ Bravard A, Vacher M, Gouget B, Coutant A, de Boisferon FH, Marsin S, Chevillard S, Radicella JP. Redox regulation of human OGG1 activity in response to cellular oxidative stress. Mol Cell Biol 2006;26(20) 7430-7436. PMID 16923968 PMCID: PMC1636869
- ^ Viau M, Gastaldo J, Bencokova Z, Joubert A, Foray N. (2008). Cadmium inhibits non-homologous end-joining and over-activates the MRE11-dependent repair pathway. Mutat Res 654(1) 13-21. PMID 18539077
- ^ Schwerdtle T, Ebert F, Thuy C, Richter C, Mullenders LH, Hartwig A. Genotoxicity of soluble and particulate cadmium compounds: impact on oxidative DNA damage and nucleotide excision repair. Chem Res Toxicol 2010;23(2) 432-442. PMID 20092276
- ^ Vogelstein B, Papadopoulos N, Velculescu VE, Zhou S, Diaz LA Jr, Kinzler KW. (2013). Cancer genome landscapes. Science 339(6127):1546-58. doi: 10.1126/science.1235122. Review. PMID 23539594
- ^ Cancer Genome Atlas Network. Comprehensive molecular characterization of human colon and rectal cancer. Nature 2012;487(7407) 330-337. doi: 10.1038/nature11252.
- ^ Balaguer F, Link A, Lozano JJ; et al. (2010). "Epigenetic silencing of miR-137 is an early event in colorectal carcinogenesis". Cancer Res. 70 (16): 6609–18. doi:10.1158/0008-5472.CAN-10-0622. PMC 2922409. PMID 20682795.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link)http://www.ncbi.nlm.nih.gov/pubmed/20682795 - ^ Deng G, Kakar S, Kim YS. (2011). MicroRNA-124a and microRNA-34b/c are frequently methylated in all histological types of colorectal cancer and polyps, and in the adjacent normal mucosa. Oncol Lett. 2:175-180. PMID 22870149
- ^ Grady WM, Parkin RK, Mitchell PS, Lee JH, Kim YH, Tsuchiya KD, Washington MK, Paraskeva C, Willson JK, Kaz AM. (2008). Epigenetic silencing of the intronic microRNA hsa-miR-342 and its host gene EVL in colorectal cancer. Oncogene 27:3880-3888. PMID 18264139 doi: 10.1038/onc.2008.10.
- ^ Varricchio, Claudette G. (2004). A cancer source book for nurses. Boston: Jones and Bartlett Publishers. p. 229. ISBN 0-7637-3276-1.
- ^ "Cancer prevention: 7 steps to reduce your risk". Mayo Clinic. 27 September 2008. Retrieved 30 January 2010.
- ^ Danaei G, Vander Hoorn S, Lopez AD, Murray CJ, Ezzati M (2005). "Causes of cancer in the world: comparative risk assessment of nine behavioural and environmental risk factors". Lancet. 366 (9499): 1784–93. doi:10.1016/S0140-6736(05)67725-2. PMID 16298215.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ "Cancer". World Health Organization. Retrieved 9 January 2011.
- ^ a b Wicki A, Hagmann, J (2011). "Diet and cancer". Swiss medical weekly. 141: w13250. doi:10.4414/smw.2011.13250. PMID 21904992.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Cappellani A, Di Vita M, Zanghi A, Cavallaro A, Piccolo G, Veroux M, Berretta M, Malaguarnera M, Canzonieri V, Lo Menzo E (2012). "Diet, obesity and breast cancer: an update". Front Biosci (Schol Ed). 4: 90–108. PMID 22202045.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Key TJ (2011). "Fruit and vegetables and cancer risk". Br. J. Cancer. 104 (1): 6–11. doi:10.1038/sj.bjc.6606032. PMC 3039795. PMID 21119663.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Larsson SC, Wolk A (2007). "Coffee consumption and risk of liver cancer: a meta-analysis". Gastroenterology. 132 (5): 1740–5. doi:10.1053/j.gastro.2007.03.044. PMID 17484871.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Zheng W, Lee SA (2009). "Well-done meat intake, heterocyclic amine exposure, and cancer risk". Nutr Cancer. 61 (4): 437–46. doi:10.1080/01635580802710741. PMC 2769029. PMID 19838915.
- ^ Ferguson LR (2010). "Meat and cancer". Meat Sci. 84 (2): 308–13. doi:10.1016/j.meatsci.2009.06.032. PMID 20374790.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Holland Chp.33
- ^ Rostom A, Dubé C, Lewin G, Tsertsvadze A, Barrowman N, Code C, Sampson M, Moher D (2007). "Nonsteroidal anti-inflammatory drugs and cyclooxygenase-2 inhibitors for primary prevention of colorectal cancer: a systematic review prepared for the U.S. Preventive Services Task Force". Ann. Intern. Med. 146 (5): 376–89. PMID 17339623.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Rothwell PM, Fowkes FG, Belch JF, Ogawa H, Warlow CP, Meade TW (2011). "Effect of daily aspirin on long-term risk of death due to cancer: analysis of individual patient data from randomised trials". Lancet. 377 (9759): 31–41. doi:10.1016/S0140-6736(10)62110-1. PMID 21144578.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Cooper K, Squires H, Carroll C, Papaioannou D, Booth A, Logan RF, Maguire C, Hind D, Tappenden P (2010). "Chemoprevention of colorectal cancer: systematic review and economic evaluation". Health Technol Assess. 14 (32): 1–206. doi:10.3310/hta14320. PMID 20594533.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Thomsen A, Kolesar JM (2008). "Chemoprevention of breast cancer". Am J Health Syst Pharm. 65 (23): 2221–8. doi:10.2146/ajhp070663. PMID 19020189.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Wilt TJ, MacDonald R, Hagerty K, Schellhammer P, Kramer BS (2008). "Five-alpha-reductase Inhibitors for prostate cancer prevention". Cochrane Database Syst Rev (2): CD007091. doi:10.1002/14651858.CD007091. PMID 18425978.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ "Vitamins and minerals: not for cancer or cardiovascular prevention". Prescrire Int. 19 (108): 182. 2010. PMID 20939459.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Giovannucci E, Liu Y, Rimm EB, Hollis BW, Fuchs CS, Stampfer MJ, Willett WC (2006). "Prospective study of predictors of vitamin D status and cancer incidence and mortality in men". J. Natl. Cancer Inst. 98 (7): 451–9. doi:10.1093/jnci/djj101. PMID 16595781.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ "Vitamin D Has Role in Colon Cancer Prevention". Archived from the original on 4 December 2006. Retrieved 27 July 2007.
- ^ Schwartz GG, Blot WJ (2006). "Vitamin D status and cancer incidence and mortality: something new under the sun". J. Natl. Cancer Inst. 98 (7): 428–30. doi:10.1093/jnci/djj127. PMID 16595770.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Fritz H, Kennedy D, Fergusson D, Fernandes R, Doucette S, Cooley K, Seely A, Sagar S, Wong R, Seely D (2011). "Vitamin A and retinoid derivatives for lung cancer: a systematic review and meta analysis". PLoS ONE. 6 (6): e21107. Bibcode:2011PLoSO...6E1107F. doi:10.1371/journal.pone.0021107. PMC 3124481. PMID 21738614.
{{cite journal}}: CS1 maint: multiple names: authors list (link) CS1 maint: unflagged free DOI (link) - ^ Cole BF, Baron JA, Sandler RS, Haile RW, Ahnen DJ, Bresalier RS, McKeown-Eyssen G, Summers RW, Rothstein RI, Burke CA, Snover DC, Church TR, Allen JI, Robertson DJ, Beck GJ, Bond JH, Byers T, Mandel JS, Mott LA, Pearson LH, Barry EL, Rees JR, Marcon N, Saibil F, Ueland PM, Greenberg ER (2007). "Folic acid for the prevention of colorectal adenomas: a randomized clinical trial". JAMA. 297 (21): 2351–9. doi:10.1001/jama.297.21.2351. PMID 17551129.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b c "Cancer Vaccine Fact Sheet". NCI. 8 June 2006. Retrieved 15 November 2008.
- ^ a b c "What Is Cancer Screening?". National Cancer Institute.
- ^ a b c Wilson JMG, Jungner G. (1968) Principles and practice of screening for disease. Geneva:World Health Organization. Public Health Papers, #34.
- ^ "Screening for Cervical Cancer". U.S. Preventive Services Task Force. 2003.
- ^ "Screening for Colorectal Cancer". U.S. Preventive Services Task Force. 2008.
- ^ "Screening for Skin Cancer". U.S. Preventive Services Task Force. 2009.
- ^ "Screening for Oral Cancer". U.S. Preventive Services Task Force. 2004.
- ^ "Lung Cancer Screening". U.S. Preventive Services Task Force. 2004.
- ^ "Screening for Prostate Cancer". U.S. Preventive Services Task Force. 2008.
- ^ "Screening for Bladder Cancer". U.S. Preventive Services Task Force. 2004.
- ^ "Screening for Testicular Cancer". U.S. Preventive Services Task Force. 2004.
- ^ "Screening for Ovarian Cancer". U.S. Preventive Services Task Force. 2004.
- ^ "Screening for Pancreatic Cancer". U.S. Preventive Services Task Force. 2004.
- ^ Chou, Roger; Croswell, Jennifer M.; Dana, Tracy; Bougatous, Christina; Blazina, Ian; Fu, Rongwei; Gleitsmann, Ken; Koenig, Helen C.; Lam, Clarence; Maltz, Ashley; Rugge, J. Bruin; Lin, Kenneth (7 October 2011). "Screening for Prostate Cancer: A Review of the Evidence for the U.S. Preventive Services Task Force". United States Preventive Services Task Force. Retrieved 8 October 2011.
- ^ "Screening for Breast Cancer". U.S. Preventive Services Task Force. 2009.
- ^ Gøtzsche PC, Nielsen M (2011). "Screening for breast cancer with mammography". Cochrane Database Syst Rev (1): CD001877. doi:10.1002/14651858.CD001877.pub4. PMID 21249649.
- ^ a b Gulati AP, Domchek, SM (2008). "The clinical management of BRCA1 and BRCA2 mutation carriers". Current oncology reports. 10 (1): 47–53. doi:10.1007/s11912-008-0008-9. PMID 18366960.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b c d e American Society of Clinical Oncology, "Five Things Physicians and Patients Should Question" (PDF), Choosing Wisely: an initiative of the ABIM Foundation, American Society of Clinical Oncology, retrieved 14 August 2012
- ^
- The American Society of Clinical Oncology made this recommendation based on various cancers. See American Society of Clinical Oncology, "Five Things Physicians and Patients Should Question" (PDF), Choosing Wisely: an initiative of the ABIM Foundation, American Society of Clinical Oncology, retrieved 14 August 2012
- for lung cancer, see Template:Cite PMID and Template:Cite PMID
- for breast cancer, see Template:Cite PMID
- for colon cancer, see Template:Cite PMID
- for other general statements see Attention: This template ({{cite doi}}) is deprecated. To cite the publication identified by doi:10.1056/NEJMsb1013826, please use {{cite journal}} (if it was published in a bona fide academic journal, otherwise {{cite report}} with
|doi=10.1056/NEJMsb1013826instead. and Attention: This template ({{cite doi}}) is deprecated. To cite the publication identified by doi:10.1200/JCO.2010.33.1744, please use {{cite journal}} (if it was published in a bona fide academic journal, otherwise {{cite report}} with|doi=10.1200/JCO.2010.33.1744instead.
- ^ "NCCN Guidelines".
- ^ "Clinical Practice Guidelines for Quality Palliative Care" (PDF). The National Consensus Project for Quality Palliative Care (NCP).
- ^ Levy MH, Back, A, Bazargan, S, Benedetti, C, Billings, JA, Block, S, Bruera, E, Carducci, MA, Dy, S, Eberle, C, Foley, KM, Harris, JD, Knight, SJ, Milch, R, Rhiner, M, Slatkin, NE, Spiegel, D, Sutton, L, Urba, S, Von Roenn, JH, Weinstein, SM, National Comprehensive Cancer Network (2006). "Palliative care. Clinical practice guidelines in oncology". Journal of the National Comprehensive Cancer Network: JNCCN. 4 (8): 776–818. PMID 16948956.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b Holland Chp. 40
- ^ Holland Chp. 41
- ^ Cassileth BR, Deng G (2004). "Complementary and alternative therapies for cancer". Oncologist. 9 (1): 80–9. doi:10.1634/theoncologist.9-1-80. PMID 14755017.
- ^ What Is CAM? National Center for Complementary and Alternative Medicine. retrieved 3 February 2008.
- ^ Vickers A (2004). "Alternative cancer cures: 'unproven' or 'disproven'?". CA Cancer J Clin. 54 (2): 110–8. doi:10.3322/canjclin.54.2.110. PMID 15061600.
- ^ a b Rheingold, Susan; Neugut, Alfred; Meadows, Anna (2003). "156: Secondary Cancers: Incidence, Risk Factors, and Management". In Frei, Emil; Kufe, Donald W.; Holland, James F. (ed.). Holland-Frei Cancer Medicine (6th ed.). Hamilton, Ont: BC Decker. p. 2399. ISBN 1-55009-213-8.
{{cite book}}:|access-date=requires|url=(help); External link in|chapterurl=|chapterurl=ignored (|chapter-url=suggested) (help)CS1 maint: multiple names: authors list (link) - ^ Montazeri A (2009). "Quality of life data as prognostic indicators of survival in cancer patients: an overview of the literature from 1982 to 2008". Health Qual Life Outcomes. 7. doi:10.1186/1477-7525-7-102. PMC 2805623. PMID 20030832.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: unflagged free DOI (link) - ^ "WHO Disease and injury country estimates". World Health Organization. 2009. Retrieved 11 November 2009.
- ^ WHO (2010). "Cancer". World Health Organization. Retrieved 5 January 2011.
{{cite web}}: Unknown parameter|month=ignored (help) - ^ a b Coleman, William B. and Rubinas, Tara C. (2009). "4". In Tsongalis, Gregory J. and Coleman, William L. (ed.). Molecular Pathology: The Molecular Basis of Human Disease. Amsterdam: Elsevier Academic Press. p. 66. ISBN 0-12-374419-9.
{{cite book}}: CS1 maint: multiple names: authors list (link) - ^ Johnson, George (28 December 2010). "Unearthing Prehistoric Tumors, and Debate". The New York Times.
- ^ Pawelec G, Derhovanessian, E, Larbi, A (2010). "Immunosenescence and cancer". Critical reviews in oncology/hematology. 75 (2): 165–72. doi:10.1016/j.critrevonc.2010.06.012. PMID 20656212.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Alberts, B, Johnson A, Lewis J; et al. (2002). "The Preventable Causes of Cancer". Molecular biology of the cell (4th ed.). New York: Garland Science. ISBN 0-8153-4072-9.
A certain irreducible background incidence of cancer is to be expected regardless of circumstances: mutations can never be absolutely avoided, because they are an inescapable consequence of fundamental limitations on the accuracy of DNA replication, as discussed in Chapter 5. If a human could live long enough, it is inevitable that at least one of his or her cells would eventually accumulate a set of mutations sufficient for cancer to develop.
{{cite book}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Anisimov VN, Sikora, E, Pawelec, G (2009). "Relationships between cancer and aging: a multilevel approach". Biogerontology. 10 (4): 323–38. doi:10.1007/s10522-008-9209-8. PMID 19156531.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Fraumeni, Joseph F.; Schottenfeld, David; Marshall, James M. (2006). Cancer epidemiology and prevention. Oxford [Oxfordshire]: Oxford University Press. p. 977. ISBN 0-19-514961-0.
{{cite book}}: CS1 maint: multiple names: authors list (link) - ^ Bostwick, David G.; Eble, John N. (2007). Urological Surgical Pathology. St. Louis: Mosby. p. 468. ISBN 0-323-01970-6.
{{cite book}}: CS1 maint: multiple names: authors list (link) - ^ a b Kaatsch P, Sikora, E, Pawelec, G (2010). "Epidemiology of childhood cancer". Cancer treatment reviews. 36 (4): 277–85. doi:10.1016/j.ctrv.2010.02.003. PMID 20231056.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Ward EM, Thun, MJ, Hannan, LM, Jemal, A (2006). "Interpreting cancer trends". Annals of the New York Academy of Sciences. 1076: 29–53. Bibcode:2006NYASA1076...29W. doi:10.1196/annals.1371.048. PMID 17119192.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ a b c d e f Hajdu SI, Thun, MJ, Hannan, LM, Jemal, A (2011). "A note from history: landmarks in history of cancer, part 1". Cancer. 117 (5): 1097–102. doi:10.1002/cncr.25553. PMID 20960499.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Paul of Aegina, 7th Century AD, quoted in Moss, Ralph W. (2004). "Galen on Cancer". CancerDecisions. Archived from the original on 16 July 2011. Referenced from Michael Shimkin, Contrary to Nature, Washington, D.C.: Superintendent of Document, DHEW Publication No. (NIH) 79-720, p. 35.
- ^ a b Hajdu SI, Thun, MJ, Hannan, LM, Jemal, A (2011). "A note from history: landmarks in history of cancer, part 2". Cancer. 117 (12): 2811–20. doi:10.1002/cncr.25825. PMID 21656759.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Yalom, Marilyn (1998). A history of the breast (1st Ballantine Books ed. ed.). New York: Ballantine Books. ISBN 0-679-43459-3.
{{cite book}}:|edition=has extra text (help) - ^ Hajdu SI, Thun, MJ, Hannan, LM, Jemal, A (2011). "A note from history: Landmarks in history of cancer, part 3". Cancer. 118 (4): 1155–68. doi:10.1002/cncr.26320. PMID 21751192.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Grange JM, Stanford JL, Stanford CA (2002). "Campbell De Morgan's 'Observations on cancer', and their relevance today". Journal of the Royal Society of Medicine. 95 (6): 296–9. doi:10.1258/jrsm.95.6.296. PMC 1279913. PMID 12042378.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Ehrenreich, Barbara (November 2001). "Welcome to Cancerland". Harper's Magazine. ISSN 0017-789X.
- ^ Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. ISBN 1-4160-2999-0.
{{cite book}}: CS1 maint: multiple names: authors list (link) - ^ "Skin cancers". World Health Organization. Retrieved 19 January 2011.
- ^ McCulley, Michelle; Greenwell, Pamela (2007). Molecular therapeutics: 21st-century medicine. London: J. Wiley. p. 207. ISBN 0-470-01916-6.
{{cite book}}: CS1 maint: multiple names: authors list (link) - ^ Gwyn, Richard (1999). "10". In Cameron, Lynne; Low, Graham (ed.). Researching and applying metaphor. Cambridge, UK: Cambridge University Press. ISBN 0-521-64964-1.
{{cite book}}: CS1 maint: multiple names: editors list (link) - ^ Sulik, Gayle (2010). Pink Ribbon Blues: How Breast Cancer Culture Undermines Women's Health. New York: Oxford University Press. pp. 78–89. ISBN 0-19-974045-3. OCLC 535493589.
- ^ a b c Olson, James Stuart (2002). Bathsheba's Breast: Women, Cancer and History. Baltimore: The Johns Hopkins University Press. pp. 145–170. ISBN 0-8018-6936-6. OCLC 186453370.
- ^ a b c d Ehrenreich, Barbara (2009). Bright-sided: How the Relentless Promotion of Positive Thinking Has Undermined America. New York: Metropolitan Books. pp. 15–44. ISBN 0-8050-8749-4.
- ^ "Cancer Facts and Figures 2012". Journalist's Resource.org.
- ^ "What Is Cancer?". National Cancer Institute. Retrieved 17 August 2009.
- ^ "Cancer Fact Sheet". Agency for Toxic Substances & Disease Registry. 30 August 2002. Retrieved 17 August 2009.
- ^ Wanjek, Christopher (16 September 2006). "Exciting New Cancer Treatments Emerge Amid Persistent Myths". Retrieved 17 August 2009.
- ^ Hayden EC, Thun, MJ, Hannan, LM, Jemal, A (2009). "Cutting off cancer's supply lines". Nature. 458 (7239): 686–687. doi:10.1038/458686b. PMID 19360048.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Sleigh SH, Barton CL (2010). "Repurposing Strategies for Therapeutics". Pharm Med. 24 (3): 151–159. doi:10.2165/11536770-000000000-00000.
- ^ Winther H, Jorgensen JT (2010). "Drug-Diagnostic Co-Development in Cancer". Pharm Med. 24 (6): 363–375. doi:10.2165/11586320-000000000-00000.
- ^ Sharon Begley (16 September 2008). "Rethinking the War on Cancer". Newsweek. Retrieved 8 September 2008.
- ^ Kolata, Gina (23 April 2009). "Advances Elusive in the Drive to Cure Cancer". The New York Times. Retrieved 5 May 2009.
- ^ Shu, L (2010). "Phytochemicals: cancer chemoprevention and suppression of tumor onset and metastasis". Cancer Metastasis Rev.: 483–502. doi:10.1007/s10555-010-9239-y. PMID 20798979. Retrieved 14 July 2013.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ a b c d e f g h i j Connie Henke Yarbro, Debra Wujcik, Barbara Holmes Gobel, ed. (2011). Cancer nursing: principles and practice (7 ed.). Jones & Bartlett Publishers. pp. 901–905. ISBN 978-1-4496-1829-2.
{{cite book}}: CS1 maint: multiple names: editors list (link) - ^ Murgia C, Pritchard JK, Kim SY, Fassati A, Weiss RA (2006). "Clonal origin and evolution of a transmissible cancer". Cell. 126 (3): 477–87. doi:10.1016/j.cell.2006.05.051. PMC 2593932. PMID 16901782.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link)
- References
- Holland, James F. (2009). Holland-Frei cancer medicine (8th ed. ed.). New York: McGraw-Hill Medical. ISBN 978-1-60795-014-1.
{{cite book}}:|edition=has extra text (help)
Further reading
- Kleinsmith, Lewis J. (2006). Principles of cancer biology. Pearson Benjamin Cummings. ISBN 978-0-8053-4003-7.
- Mukherjee, Siddhartha (16 November 2010). The Emperor of All Maladies: A Biography of Cancer. Simon and Schuster. ISBN 978-1-4391-0795-9.
{{cite book}}:|access-date=requires|url=(help) - Pazdur, Richard; et al. (May 2009). Cancer Management: A Multidisciplinary Approach. Cmp United Business Media. ISBN 978-1-891483-62-2.
{{cite book}}: Explicit use of et al. in:|author2=(help) (online at cancernetwork.com) - Tannock, Ian (2005). The basic science of oncology. McGraw-Hill Professional. ISBN 978-0-07-138774-3.
- Manfred Schwab (2008). Encyclopedia of Cancer (4 Volume Set). Berlin: Springer. ISBN 3-540-36847-7.