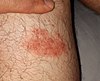
Erythema migrans
-
Erythema migrans ("redness migrating") and may have no definite pattern, as in this Lyme rash on a woman's neck.[4] Rashes from non-Lyme causes may look similar.[1][5]
Erythema migrans or erythema chronicum migrans is an expanding rash often seen in the early stage of Lyme disease, and can also (but less commonly) be caused by southern tick-associated rash illness (STARI).[6][7] It can appear anywhere from one day to one month after a tick bite. This rash does not represent an allergic reaction to the bite, but rather an actual skin infection of one of the Lyme bacteria species from the genus Borrelia. The rash's name comes from Neo-Latin for "Redness migrating."
Lyme disease[edit]
"Erythema migrans is the only manifestation of Lyme disease in the United States that is sufficiently distinctive to allow clinical diagnosis in the absence of laboratory confirmation."[8][9] Often, but not always, mentions of a target lesion (bull's-eye lesion) are talking about erythema migrans. However, the appearance of erythema migrans can vary considerably: while some look like a bull's eye, in the U.S. most are evenly red or bluish, without a central or ring-like clearing.[10][3][11] A minority of patients never have any rash. Because Lyme disease can within a few weeks cause long-term neurologic complications, persons with a rash and recent history of outdoor activities where Lyme is common should seek a doctor for diagnosis.[11]
Presentation[edit]
The initial sign of about 80% of Lyme infections is an erythema migrans (EM) rash at the site of a tick bite, often near skin folds, such as the armpit, groin, or back of knee, on the trunk, under clothing straps, or in children's hair, ear, or neck.[1][10] Most people who get infected do not remember seeing a tick or the bite. The EM rash appears typically one or two weeks (range 3–32 days) after the bite. The most distinctive features of the EM rash are the speed and extent to which it expands, respectively 2–3 cm per day and up to a diameter of 5–70 cm (50% attain more than 16 cm).[1][10][2] The rash is usually circular or oval, red or bluish, and may have an elevated or darker center.[10][3] In about 79% of cases in Europe but only 19% of cases in endemic areas of the U.S., the rash gradually clears from the center toward the edges, possibly forming a "bull's eye" pattern.[2][3] The rash may feel warm but usually is not itchy, is rarely tender or painful, and takes up to four weeks to resolve if untreated.[10][12][13]

The EM rash is often accompanied by symptoms of a viral-like illness, including fatigue, headache, body aches, fever, and chills, but usually not nausea or upper-respiratory problems. These symptoms may also appear without a rash, or linger after the rash disappears. Lyme can progress to later stages without these symptoms or a rash.[10]
A person with an asymptomatic EM rash can easily miss its significance. However, if the initial EM rash is not treated, the infection can disseminate through the lymphatic system or blood. Within days or weeks, additional EM rashes, usually smaller, can appear at other sites, or the infection can cause more serious complications in the nervous system, heart, or joints.[1][10]
Southern tick-associated rash illness[edit]
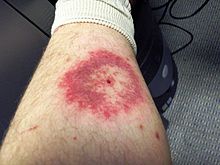
Southern tick-associated rash illness (STARI) produces a similar rash pattern although it develops more quickly and is smaller.[14] This erythema is also sometimes called erythema migrans[15] or EM. The associated infectious agent has not been determined. Antibiotic treatment resolves the illness quickly.[6][7]
Treatment[edit]
Both Lyme disease and STARI can be treated with antibiotics, particularly doxycycline.[1][16][17] Amoxicillin in children less than 8 years of age.
History[edit]
In a 1909 meeting of the Swedish Society of Dermatology, Arvid Afzelius first presented research about an expanding, ring-like lesion he had observed. Afzelius published his work 12 years later and speculated the rash came from the bite of an Ixodes tick, meningitic symptoms and signs in a number of cases and that both sexes were affected. This rash was known as erythema chronicum migrans, the skin rash found in early-stage Lyme disease.[18]
In the 1920s, French physicians Garin and Bujadoux described a patient with meningoencephalitis, painful sensory radiculitis, and erythema migrans following a tick bite, and they postulated the symptoms were due to a spirochetal infection. In the 1940s, German neurologist Alfred Bannwarth described several cases of chronic lymphocytic meningitis and polyradiculoneuritis, some of which were accompanied by erythematous skin lesions.[citation needed]
References[edit]
- ^ a b c d e f Wright WF, Riedel DJ, Talwani R, Gilliam BL (June 2012). "Diagnosis and management of Lyme disease". Am Fam Physician. 85 (11): 1086–93. PMID 22962880. Archived from the original on 27 September 2013.
- ^ a b c Tibbles CD, Edlow JA (20 June 2007). "Does This Patient Have Erithema Migrans?". JAMA. 297 (23): 2617–27. doi:10.1001/jama.297.23.2617. PMID 17579230.
- ^ a b c d "Lyme disease rashes and look-alikes". Lyme Disease. Centers for Disease Control and Prevention. 2018-12-21. Retrieved April 18, 2019.
- ^ Boyce, RM; Pretsch, P; Tyrlik, K; Schulz, A; Giandomenico, DA; Barbarin, AM; Williams, C (March 2024). "Delayed Diagnosis of Locally Acquired Lyme Disease, Central North Carolina, USA". Emerging Infectious Diseases. 30 (3): 564–567. doi:10.3201/eid3003.231302. PMC 10902532. PMID 38407256.
- ^ Trayes, KP; Savage, K; Studdiford, JS (1 September 2018). "Annular Lesions: Diagnosis and Treatment". American Family Physician. 98 (5): 283–291. PMID 30216021.
- ^ a b "Lone star tick a concern, but not for Lyme disease". U.S. Centers for Disease Control and Prevention (CDC). Retrieved 2017-10-06. Page last reviewed: October 22, 2015
- ^ a b Naktin, Jaan Peter (2017). "Diagnostic Utility of Erythema Migrans". Clinical Infectious Diseases. 65 (12): 2156–2157. doi:10.1093/cid/cix544. ISSN 1058-4838. PMID 28605419.
- ^ Wormser GP, Dattwyler RJ, Shapiro ED, et al. (November 2006). "The clinical assessment, treatment, and prevention of Lyme disease, Human Granulocytic Anaplasmosis, and Babesiosis: Clinical Practice Guidelines by the Infectious Diseases Society of America". Clin. Infect. Dis. 43 (9): 1089–134. doi:10.1086/508667. PMID 17029130.
"pp. 1101–2 Background and Diagnosis of Erythema Migrans
- ^ Ogden NH, Lindsay LR, Morshed M, Sockett PN, Artsob H (January 2008). "The rising challenge of Lyme borreliosis in Canada". Can. Commun. Dis. Rep. 34 (1): 1–19. PMID 18290267.
- ^ a b c d e f g Shapiro ED (May 2014). "Clinical practice. Lyme disease" (PDF). The New England Journal of Medicine. 370 (18): 1724–1731. doi:10.1056/NEJMcp1314325. PMC 4487875. PMID 24785207. Archived from the original (PDF) on 19 October 2016.
- ^ a b Juckett, G (2014), "In reply: Comment on 'Identifying erythema migrans rash in patients with Lyme disease'", Am Fam Physician, 89 (6): 424, PMID 24818260.
- ^ Smith RP, Schoen RT, Rahn DW, Sikand VK, Nowakowski J, Parenti DL, Holman MS, Persing DH, Steere AC (2002). "Clinical characteristics and treatment outcome of early Lyme disease in patients with microbiologically confirmed erythema migrans". Ann Intern Med. 136 (6): 421–8. doi:10.7326/0003-4819-136-6-200203190-00005. PMID 11900494.
- ^ Edlow JA (2002). "Erythema migrans". Med Clin North Am. 86 (2): 239–60. doi:10.1016/S0025-7125(03)00085-3. PMID 11982300.
- ^ Goddard J (2017) Not all erythema migrans lesions are Lyme disease. The American journal of medicine, 130(2), 231-233.
- ^ Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology. St. Louis: Mosby. ISBN 978-1-4160-2999-1.
- ^ James AM, Liveris D, Wormser GP, Schwartz I, Montecalvo MA, Johnson BJ (June 2001). "Borrelia lonestari infection after a bite by an Amblyomma americanum tick". J. Infect. Dis. 183 (12): 1810–4. doi:10.1086/320721. PMID 11372036.
- ^ Blanton L, Keith B, Brzezinski W (June 2008). "Southern Tick-Associated Rash Illness: Erythema Migrans Is Not Always Lyme Disease". South. Med. J. 101 (7): 759–760. doi:10.1097/SMJ.0b013e31817a8b3f. PMID 18580719.
- ^ Lipschütz, B. (1931). "Zur Kenntnis der "Erythema chronicum migrans"". Acta Dermato-Venereologica. 12. Stockholm: 100–2.

![In Europe, 80% of Lyme rashes look like a "bull's eye," but in only 20% of cases in the United States. (20 percent of Lyme infections show no rash.)[1][2][3]](http://upload.wikimedia.org/wikipedia/commons/thumb/8/8e/Bullseye_Lyme_Disease_Rash.jpg/180px-Bullseye_Lyme_Disease_Rash.jpg)
![Erythema migrans ("redness migrating") and may have no definite pattern, as in this Lyme rash on a woman's neck.[4] Rashes from non-Lyme causes may look similar.[1][5]](http://upload.wikimedia.org/wikipedia/commons/thumb/0/03/Solid_erythema_migrans_rash_on_the_neck_of_a_woman_with_Lyme_disease.jpg/180px-Solid_erythema_migrans_rash_on_the_neck_of_a_woman_with_Lyme_disease.jpg)