Rectovaginal fistula
| Rectovestibular fistula | |
|---|---|
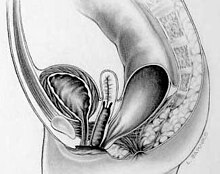 | |
| Rectovaginal fistula | |
| Specialty | Gynecology |
| Diagnostic method | • No anal opening
• A gloved finger or thermometer cannot be inserted into the infants rectum • No history of passage of meconium • Presence of abdominal distension • Presence of meconium in urine |
| Treatment | PSARP |
A rectovaginal fistula is a medical condition where there is a fistula or abnormal connection between the rectum and the vagina.[1]
Rectovaginal fistulae may be extremely debilitating. If the opening between the rectum and vagina is wide it will allow both flatulence and feces to escape through the vagina, leading to fecal incontinence. There is an association with recurrent urinary and vaginal infections. The fistula may also connect the rectum and urethra, which is called recto-urethral fistula. Either conditions can lead to labial fusion. This type of fistula can cause pediatricians to misdiagnose imperforate anus. The severity of the symptoms will depend on the size of fistula. Most often, it appears after about one week or so after childbirth.
Causes
[edit]Rectovaginal fistulas are often the result of trauma during childbirth (in which case it is known as obstetric fistula), with increased risk associated with significant lacerations or interventions are used such as episiotomy or operative (forceps/vacuum extraction) deliveries[2] or in situations where there is inadequate health care, such as in some developing countries. Rectovaginal fistula is said to be known as the leading cause in maternal death in developing countries.[3] Risk factors include prolonged labour, difficult instrumental delivery and paramedian episiotomy. Rates in Eritrea are estimated as high as 350 per 100,000 vaginal births. Fistulas can also develop as a result of physical trauma to either the vagina or anus, including from rape.[4] Women with rectovaginal fistulae are often stigmatized in developing countries, and become outcasts.[5]
Rectovaginal fistula can also be a symptom of various diseases, including infection by lymphogranuloma venereum,[6] or the unintended result of surgery, such as episiotomy or sex reassignment surgery. They may present as a complication of vaginal surgery, including vaginal hysterectomy. They are a recognized presentation of rectal carcinoma or rarely diverticular disease of the bowel or Crohn's disease. They are seen rarely after radiotherapy treatment for cervical cancer.[citation needed]
Treatment
[edit]After diagnosing rectovaginal fistula, it is best to wait for around three months to allow the inflammation to subside. For low fistulae, a vaginal approach is best, while an abdominal repair would be necessary for a high fistula at the posterior fornix.
A circular incision is made around the fistula and vagina is separated from the underlying rectum with a sharp circumferential dissection. The entire fistulous tract, along with a small rim of rectal mucosa is incised. The rectal wall is then closed extramucosally.[7]
Most rectovaginal fistulas will need surgery to fix. Medications such as antibiotics and Infliximab may be prescribed to help close the rectovaginal fistula or prepare for surgery.[8][9]
References
[edit]- ^ Kumaran SS, Palanivelu C, Kavalakat AJ, Parthasarathi R, Neelayathatchi M (2005). "Laparoscopic repair of high rectovaginal fistula: Is it technically feasible?". BMC Surg. 5: 20. doi:10.1186/1471-2482-5-20. PMC 1266383. PMID 16221302.
- ^ "Rectovaginal Fistula and Rectourethral Fistula | ASCRS". Archived from the original on 2015-04-11. Retrieved 2015-04-12.
- ^ Landry, 926
- ^ Nordland, Rod (12 November 2006). "Congo: More Vicious Than Rape". Newsweek. Retrieved 25 August 2019.
- ^ Nolen, Stephanie. "Not Women Anymore..." Ms. Magazine. Archived from the original on 24 October 2018. Retrieved 25 August 2019.
- ^ Lynch CM, Felder TL, Schwandt RA, Shashy RG (1999). "Lymphogranuloma venereum presenting as a rectovaginal fistula". Infect Dis Obstet Gynecol. 7 (4): 199–201. doi:10.1155/S1064744999000344. PMC 1784745. PMID 10449269.
- ^ "Rectovaginal fistula: Treatment and Management". Medscape. Retrieved 14 August 2012.
- ^ "Rectovaginal fistula Treatments and drugs - Mayo Clinic". www.mayoclinic.org. Retrieved 2015-12-14.
- ^ Sands, Bruce E.; Anderson, Frank H.; Bernstein, Charles N.; Chey, William Y.; Feagan, Brian G.; Fedorak, Richard N.; Kamm, Michael A.; Korzenik, Joshua R.; Lashner, Bret A. (2004-02-26). "Infliximab maintenance therapy for fistulizing Crohn's disease". The New England Journal of Medicine. 350 (9): 876–885. doi:10.1056/NEJMoa030815. ISSN 1533-4406. PMID 14985485.
External links
[edit]- Rectovaginal fistula at Curlie
 Media related to Rectovaginal fistula at Wikimedia Commons
Media related to Rectovaginal fistula at Wikimedia Commons
