Dengue fever
| Dengue virus | |
|---|---|
| |
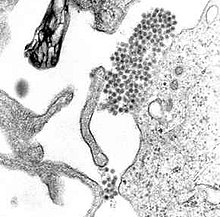
| A TEM micrograph showing Dengue virus virions (the cluster of dark dots near the center). | |
| Virus classification | |
| Group: | Group IV ((+)ssRNA)
|
| Family: | |
| Genus: | |
| Species: | Dengue virus
|
| Dengue fever | |
|---|---|
| Specialty | Infectious diseases |
Dengue fever (Template:Pron-en (BrE), Template:IPAlink-en (AmE)) and dengue hemorrhagic fever (DHF) are acute febrile diseases, found in the tropics and Africa, and caused by four closely related virus serotypes of the genus Flavivirus, family Flaviviridae.[1] It is also known as breakbone fever. The geographical spread is similar to malaria, including northern Australia, Singapore, Malaysia, Taiwan, Thailand, Vietnam, Indonesia, Honduras, Philippines, Pakistan, India, Bangladesh, Puerto Rico, Bolivia[2], Brazil, Guyana, Venezuela, Trinidad and now Samoa[3]. Unlike malaria, dengue is just as prevalent in the urban districts of its range as in rural areas. Each serotype is sufficiently different that there is no cross-protection and epidemics caused by multiple serotypes (hyperendemicity) can occur. Dengue is transmitted to humans by the Aedes aegypti or more rarely the Aedes albopictus mosquito, which feed during the day.[4]
The WHO says some 2.5 billion people, two fifths of the world's population, are now at risk from dengue and estimates that there may be 50 million cases of dengue infection worldwide every year. The disease is now endemic in more than 100 countries.[5]
This is manifested by a sudden onset of severe headache, muscle and joint pains (myalgias and arthralgias—severe pain gives it the name break-bone fever or bonecrusher disease), fever, and rash.[6] The dengue rash is characteristically bright red petechiae and usually appears first on the lower limbs and the chest; in some patients, it spreads to cover most of the body. There may also be gastritis with some combination of associated abdominal pain, nausea, vomiting, or diarrhea.
Some cases develop much milder symptoms which can be misdiagnosed as influenza or other viral infection when no rash is present. Thus travelers from tropical areas may pass on dengue in their home countries inadvertently, having not been properly diagnosed at the height of their illness. Patients with dengue can pass on the infection only through mosquitoes or blood products and only while they are still febrile.
The classic dengue fever lasts about six to seven days, with a smaller peak of fever at the trailing end of the disease (the so-called biphasic pattern). Clinically, the platelet count will drop until the patient's temperature is normal.
Cases of DHF also show higher fever, variable haemorrhagic phenomena, thrombocytopenia, and haemoconcentration. A small proportion of cases lead to dengue shock syndrome (DSS) which has a high mortality rate.
DHF combined with a cirrhotic liver has been suspected in rapid development of Hepatocellular Carcinoma . Given the DEN virus is related to the Hepatitis C virus this is an avenue for further research as HCC is the top 5 leading Cancer cause of death outside of Europe and North America . Normally HCC does not normally occur in a cirrhotic liver for 10+ years after the cessation of the poisioning agent. DHF patients can develop HCC within one year of cessation of abuse.
Diagnosis
The diagnosis of dengue is usually made clinically. The classic picture is high fever with no localising source of infection, a petechial rash with thrombocytopenia and relative leukopenia - low platelet and white blood cell count. Care has to be taken as diagnosis of DHF can mask end stage liver disease and vice versa.
- Fever, bladder problem, constant headaches, severe dizziness and loss of appetite.
- Hemorrhagic tendency (positive tourniquet test, spontaneous bruising, bleeding from mucosa, gingiva, injection sites, etc.; vomiting blood, or bloody diarrhea)
- Thrombocytopenia (<100,000 platelets per mm³ or estimated as less than 3 platelets per high power field)
- Evidence of plasma leakage (hematocrit more than 20% higher than expected, or drop in haematocrit of 20% or more from baseline following IV fluid, pleural effusion, ascites, hypoproteinemia)
- Encephalitic occurrences.
Dengue shock syndrome is defined as dengue hemorrhagic fever plus:
- Weak rapid pulse,
- Narrow pulse pressure (less than 20 mm Hg)
- Cold, clammy skin and restlessness.
Serology and polymerase chain reaction (PCR) studies are available to confirm the diagnosis of dengue if clinically indicated.
Treatment
The mainstay of treatment is timely supportive therapy to tackle shock due to haemoconcentration and bleeding. Close monitoring of vital signs in critical period (between day 2 to day 7 of fever) is vital. Increased oral fluid intake is recommended to prevent dehydration. Supplementation with intravenous fluids may be necessary to prevent dehydration and significant concentration of the blood if the patient is unable to maintain oral intake. A platelet transfusion is indicated in rare cases if the platelet level drops significantly (below 20,000) or if there is significant bleeding. The presence of melena may indicate internal gastrointestinal bleeding requiring platelet and/or red blood cell transfusion.
Aspirin and non-steroidal anti-inflammatory drugs should be avoided as these drugs may worsen the bleeding tendency associated with some of these infections. Patients may receive paracetamol preparations to deal with these symptoms if dengue is suspected.[7]
Emerging treatments
Emerging evidence suggests that mycophenolic acid and ribavirin inhibit dengue replication. Initial experiments showed a fivefold increase in defective viral RNA production by cells treated with each drug.[8] In vivo studies, however, have not yet been done. Unlike HIV therapy, lack of adequate global interest and funding greatly hampers the development of treatment regime.
In Brazilian Traditional medicine, dengue is treated with cat's claw herb, which is for inflamation and DOES NOT prevent dengue.[9]
Epidemiology

Dengue is transmitted by Aedes mosquitoes, particularly A. aegypti and A. albopictus. Dengue may also be transmitted via infected blood products (blood transfusions, plasma, and platelets), but the scale of this problem is unknown.[10]

The first recognized Dengue epidemics occurred almost simultaneously in Asia, Africa, and North America in the 1780s, shortly after the identification and naming of the disease in 1779. A pandemic began in Southeast Asia in the 1950s, and by 1975 DHF had become a leading cause of death among children in the region. Epidemic dengue has become more common since the 1980s. By the late 1990s, dengue was the most important mosquito-borne disease affecting humans after malaria, with around 40 million cases of dengue fever and several hundred thousand cases of dengue hemorrhagic fever each year. Significant outbreaks of dengue fever tend to occur every five or six months. The cyclical rise and fall in numbers of dengue cases is thought to be the result of seasonal cycles interacting with a short-lived cross-immunity for all four strains in people who have had dengue. When the cross-immunity wears off the population is more susceptible to transmission whenever the next seasonal peak occurs. Thus over time there remain large numbers of susceptible people in affected populations despite previous outbreaks due to the four different serotypes of dengue virus and the presence of unexposed individuals from childbirth or immigration.
There is significant evidence, originally suggested by S.B. Halstead in the 1970s, that dengue hemorrhagic fever is more likely to occur in patients who have secondary infections by another one of dengue fever's four serotypes. One model to explain this process is known as antibody-dependent enhancement (ADE), which allows for increased uptake and virion replication during a secondary infection with a different strain. Through an immunological phenomenon, known as original antigenic sin, the immune system is not able to adequately respond to the stronger infection, and the secondary infection becomes far more serious.[11] This process is also known as superinfection.[12][13]
Reported cases of dengue are an under-representation of all cases when accounting for subclinical cases and cases where the patient did not present for medical treatment. With proper medical treatment the mortality rate for dengue can be brought down to less than 1 in 1000.[citation needed]
Country Specific Epidemics
There was a serious outbreak in Rio de Janeiro in February 2002 affecting around one million people and killing sixteen. On March 20, 2008, the secretary of health of the state of Rio de Janeiro, Sérgio Côrtes, announced that 23,555 cases of dengue, including 30 deaths, had been recorded in the state in less than three months. Côrtes said, "I am treating this as an epidemic because the number of cases is extremely high." Federal Minister of Health, José Gomes Temporão also announced that he was forming a panel to respond to the situation. Cesar Maia, mayor of the city of Rio de Janeiro, denied that there was serious cause for concern, saying that the incidence of cases was in fact declining from a peak at the beginning of February. [14] By April 3, 2008, the number of cases reported rose to 55,000 [15]
In Singapore, there are 4,000–5,000 reported cases of dengue fever or dengue haemorrhagic fever every year. In the year 2003, there were six deaths from dengue shock syndrome.[citation needed]
Prevention
Vaccine development
There is no commercially available vaccine for the dengue flavivirus. However, one of the many ongoing vaccine development programs is the Pediatric Dengue Vaccine Initiative which was set up in 2003 with the aim of accelerating the development and introduction of dengue vaccine(s) that are affordable and accessible to poor children in endemic countries.[16] Thai researchers are testing a dengue fever vaccine on 3,000–5,000 human volunteers after having successfully conducted tests on animals and a small group of human volunteers.[17] A number of other vaccine candidates are entering phase I or II testing.[18]
Mosquito control

Primary prevention of dengue mainly resides in mosquito control. There are two primary methods: larval control and adult mosquito control. In urban areas, Aedes mosquitos breed on water collections in artificial containers such as plastic cups, used tires, broken bottles, flower pots, etc. Periodic draining or removal of artificial containers is the most effective way of reducing the breeding grounds for mosquitos. Larvicide treatment is another effective way to control the vector larvae but the larvicide chosen should be long-lasting and preferably have World Health Organization clearance for use in drinking water. There are some very effective insect growth regulators (IGRs) available which are both safe and long-lasting (e.g. pyriproxyfen). For reducing the adult mosquito load, fogging with insecticide is somewhat effective.
Prevention of mosquito bites is another way of preventing disease. This can be achieved by using insect repellent, mosquito traps or mosquito nets.
In 1998, scientists from the Queensland Institute of Research in Australia and Vietnam's Ministry of Health introduced a scheme that encouraged children to place a water bug, the crustacean Mesocyclops, in water tanks and discarded containers where the Aedes aegypti mosquito was known to thrive.[19] This method is viewed as being more cost-effective and more environmentally friendly than pesticides, though not as effective, and requires the ongoing participation of the community.[20]
In 2004, scientists from the Federal University of Minas Gerais, Brazil, discovered a fast way to find and count mosquito population inside urban areas. The technology, named Intelligent Monitoring of Dengue ( in Portuguese), uses traps with kairomones that capture Aedes gravid females, and upload insect counts with a combination of cell phone, GPS and internet technology. The result is a complete map of the mosquitoes in urban areas, updated in real time and accessible remotely, that can inform control methodologies.[21] The technology was recognized with a Tech Museum Award in 2006.[22]
In 2009, scientists from the School of Integrative Biology at The University of Queensland revealed that by infecting Aedes mosquitos with the bacterium Wolbachia, the adult lifespan was reduced by half. [23] In the study, super-fine needles were used to inject 10,000 mosquito embryos with the bacterium. Once an insect was infected, the bacterium would spread via its eggs to the next generation. A pilot release of infected mosquitoes could begin in Vietnam within three years. If no problems are discovered, a full-scale biological attack against the insects could be launched within five years. [24]
Potential antiviral approaches
Dengue virus belongs to the family Flaviviridae, which includes the hepatitis C virus, West Nile and Yellow fever viruses among others. Possible laboratory-based modification of the yellow fever vaccine YF-17D to target the dengue virus via chimeric replacement has been discussed extensively in scientific literature.[25] To date, however, no full scale studies have been conducted.[26]
In 2006, a group of Argentine scientists discovered the molecular replication mechanism of the virus, which could be specificaly attacked by disrupting the viral RMA polymerase.[27] In cell culture[28] and murine experiments,[29][30] morpholino antisense oligos have shown specific activity against Dengue virus.
In 2007 scientists' attenuated virus replication by interfering with activity of the dengue viral protease;[31] subsequently, a project to identify novel protease disruption mechanisms has been launched.
Etymology
The origins of the word dengue are not clear, but one theory is that it is derived from the Swahili phrase "Ka-dinga pepo", which describes the disease as being caused by an evil spirit.[32] The Swahili word "dinga" may possibly have its origin in the Spanish word "dengue" meaning fastidious or careful, which would describe the gait of a person suffering the bone pain of dengue fever.[33] Alternatively, the use of the Spanish word may derive from the similar-sounding Swahili.[34]
Also known as "Dandy Fever", slaves in the West Indies who contracted dengue were said to have the posture and gait of a dandy. [35]
History
The first recorded potential case of dengue fever comes from a Chinese medical encyclopedia from the Jin Dynasty (265–420 AD). The Chinese referred to a “water poison” associated with flying insects. [34] The first definitive case report dates from 1789 and is attributed to Benjamin Rush, who coined the term "breakbone fever" because of the symptoms of myalgia and arthralgia.[36] The viral etiology and the transmission by mosquitoes were deciphered only in the 20th century. Population movements during World War II spread the disease globally.
Use as a biological weapon
Dengue fever was one of more than a dozen agents that the United States researched as potential biological weapons before the nation suspended its biological weapons program.[37]
See also
- Discovering Dengue Drugs – Together, a distributed computing project attempting to identify drug leads with broad spectrum activity against dengue.[38]
External links
References
- ^ "Chapter 4, Prevention of Specific Infectious Diseases". CDC Traveler's Health: Yellow Book. Retrieved 2007-05-20.
- ^ "Dengue fever outbreak in Bolivia". BBC. 2009-02-03. Retrieved 2009-02-26.
- ^ http://www.samoalivenews.com/Health/Dengue-Fever-Outbreak-Confirmed-In-Samoa.html
- ^ Dengue Fever – Information Sheet. World Health Organization, October 9 2006. Retrieved on 2007-11-30.
- ^ Dengue epidemic threatens India's capital
- ^ Ryan KJ, Ray CG (editors) (2004). Sherris Medical Microbiology (4th ed. ed.). McGraw Hill. p. 592. ISBN 0838585299.
{{cite book}}:|author=has generic name (help);|edition=has extra text (help) - ^ "Dengue & DHF: Information for Health Care Practitioners". Dengue Fever. CDC Division of Vector-Borne Infectious Diseases (DVBID). 2007-10-22. Retrieved 2008-10-05.
- ^ Takhampunya R, Ubol S, Houng HS, Cameron CE, Padmanabhan R (2006). "Inhibition of dengue virus replication by mycophenolic acid and ribavirin". J. Gen. Virol. 87 (Pt 7): 1947–52. doi:10.1099/vir.0.81655-0. PMID 16760396.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Brazil Scientists Discover "Cat's Claw" Combats Dengue Fever
- ^ Wilder-Smith A, Chen LH, Massad E, Wilson ME (2009). "Threat of dengue to blood safety in dengue-endemic countries". Emerg Infect Dis. 15 (1): 8–11. PMID 19116042.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Rothman AL (2004). "Dengue: defining protective versus pathologic immunity". J. Clin. Invest. 113 (7): 946–51. doi:10.1172/JCI200421512. PMC 379334. PMID 15057297.
- ^ Nowak MA, May RM (1994). "Superinfection and the evolution of parasite virulence". Proceedings. Biological sciences / the Royal Society. 255 (1342): 81–9. doi:10.1098/rspb.1994.0012. PMID 8153140.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Levin SA, Pimentel D (1981). "Selection of intermediate rates of increase in parasite-host systems". American Naturalist. 117: 308–15.
- ^ Fernanda Pontes (20 March 2008), "Secretário estadual de Saúde Sérgio Côrtes admite que estado vive epidemia de dengue", O Globo Online (in Portuguese)
{{citation}}: CS1 maint: date and year (link). - ^ CNN (3 April 2008), "Thousands hit by Brazil outbreak of dengue", CNN
{{citation}}:|author=has generic name (help)CS1 maint: date and year (link). - ^ "Pediatric Dengue Vaccine Initiative". 2008. Retrieved 2008-10-05.
- ^ "Thailand to test Mahidol-developed dengue vaccine prototype". People's Daily Online. 2005-09-05. Retrieved 2006-10-08.
- ^ Edelman R (2007). "Dengue vaccines approach the finish line". Clinical infectious diseases : an official publication of the Infectious Diseases Society of America. 45 Suppl 1: S56–60. doi:10.1086/518148. PMID 17582571.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ Vu SN, Nguyen TY, Kay BH, Marten GG, Reid JW (1998). "Eradication of Aedes aegypti from a village in Vietnam, using copepods and community participation". Am J Trop Med Hyg. 59 (4): 657–60. PMID 9790448.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ "Water bug aids dengue fever fight". BBC News. 2005-02-11. Retrieved 2008-10-05.
Kay B, Vu SN (2005). "New strategy against Aedes aegypti in Vietnam". Lancet. 365 (9459): 613–7. doi:10.1016/S0140-6736(05)17913-6. PMID 15708107. - ^ "Dengue fever GPS mapping". CNN.com Technology. 2007-07-09. Retrieved 2009-01-07.
- ^ "Health Awards Benefiting Humanity Laureates". Tech Museum of Innovation. 2006. Retrieved 2009-01-07.
- ^ McMeniman CJ, Lane RV, Cass BN; et al. (2009). "Stable Introduction of a Life-Shortening Wolbachia Infection into the Mosquito Aedes aegypti". Science. 323 (5910): 141–4. doi:10.1126/science.1165326. PMID 19119237.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ "Dengue fever breakthrough". Sydney Morning Herald. 2009-01-02. Retrieved 2009-01-02.
- ^ Lai CJ, Monath TP (2003). "Chimeric flaviviruses: novel vaccines against dengue fever, tick-borne encephalitis, and Japanese encephalitis". Advances in virus research. 61: 469–509. PMID 14714441.
- ^ Querec T, Bennouna Sex is a good thing plesure multiple dendritic cell subsets via TLR2, 7, 8, and 9 to stimulate polyvalent immunity (2006). J. Exp. Med. 203 (2): 413–24. doi:10.1084/jem.20051720. PMID 16461338.
{{cite journal}}: Missing or empty|title=(help)CS1 maint: multiple names: authors list (link) CS1 maint: numeric names: authors list (link) - ^ Filomatori CV, Lodeiro MF, Alvarez DE, Samsa MM, Pietrasanta L, Gamarnik AV (2006). "A 5' RNA element promotes dengue virus RNA synthesis on a circular genome". Genes Dev. 20 (16): 2238–49. doi:10.1101/gad.1444206. PMID 16882970.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Kinney RM, Huang CY, Rose BC; et al. (2005). "Inhibition of dengue virus serotypes 1 to 4 in vero cell cultures with morpholino oligomers". Journal of virology. 79 (8): 5116–28. doi:10.1128/JVI.79.8.5116-5128.2005. PMC 1069583. PMID 15795296.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Burrer R, Neuman BW, Ting JP; et al. (2007). "Antiviral effects of antisense morpholino oligomers in murine coronavirus infection models". Journal of virology. 81 (11): 5637–48. doi:10.1128/JVI.02360-06. PMC 1900280. PMID 17344287.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Stein DA, Huang CY, Silengo S; et al. (2008). "Treatment of AG129 mice with antisense morpholino oligomers increases survival time following challenge with dengue 2 virus". The Journal of antimicrobial chemotherapy. 62 (3): 555–65. doi:10.1093/jac/dkn221. PMID 18567576.
{{cite journal}}: Explicit use of et al. in:|author=(help); Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ "Project Summary". Discovering Dengue Drug-Together. University of Texas, Medical Branch. 2007. Retrieved 2008-10-05.
- ^ "Dengue fever: essential data". 1999. Retrieved 2008-10-05.
- ^ Harper D (2001). "Etymology: dengue". Online Etymology Dictionary. Retrieved 2008-10-05.
- ^ a b "etymologia: dengue" (PDF). Emerging Infectious Diseases. 12 (6): 893. 2006.
- ^ url=http://www.medterms.com/script/main/art.asp?articlekey=6620
- ^ Gubler DJ (1998). "Dengue and dengue hemorrhagic fever". Clinical microbiology reviews. 11 (3): 480–96. PMC 88892. PMID 9665979.
{{cite journal}}: Unknown parameter|month=ignored (help) - ^ "Chemical and Biological Weapons: Possession and Programs Past and Present", James Martin Center for Nonproliferation Studies, Middlebury College, April 9, 2002, accessed November 14, 2008.
- ^ "Discovering Dengue Drugs – Together". University of Texas Medical Branch. 2009-01-04. Retrieved 2009-01-04.
External links
- Template:DMOZ
- Dengue Virus Genomes database search results from the Dengue Virus Database at the Viral Bioinformatics Resource Center
- Virtual Exhibition about Dengue Fever
- [1]
