Hepatitis A: Difference between revisions
adjusted |
→Countries: added information about the latest HAV cases in Canada due to a Costco product |
||
| Line 199: | Line 199: | ||
| url = |
| url = |
||
}}</ref> In 1988, more than 300,000 people in [[Shanghai]], China, were infected with HAV after eating [[clam]]s (''Anadara subcrenata'') from a contaminated river.<ref name="Murray, P. r. 2005"/> |
}}</ref> In 1988, more than 300,000 people in [[Shanghai]], China, were infected with HAV after eating [[clam]]s (''Anadara subcrenata'') from a contaminated river.<ref name="Murray, P. r. 2005"/> |
||
In June 2013, frozen berries sold by US retailer Costco and purchased by around 240,000 people were the subject of a recall, after at least 158 people were infected with HAV, 69 of whom were hospitalized.<ref>{{cite news |first=Elizabeth |last=Weise |title=118 sickened in hepatitis A outbreak linked to berries |newspaper=USA Today |date=18 June 2013 |url=http://www.usatoday.com/story/news/nation/2013/06/18/hepatitis-a-frozen-berries-118-sick/2434267/}}</ref><ref>{{cite web |title=Outbreak Cases |date=28 October 2013 |work=Viral Hepatitis |publisher=Centers for Disease Control and Prevention |url=http://www.cdc.gov/hepatitis/Outbreaks/2013/A1b-03-31/index.html}}</ref> In Australia in February 2015, a recall of frozen berries was issued after at least 19 people contracted the illness following their consumption of the product.<ref>{{cite web |title=Frozen berries Heptitus A scare |date=17 February 2015 |newspaper=ABC News Australia |url=http://www.abc.net.au/news/2015-02-17/fourth-frozen-berry-product-recalled-in-hepatitis-a-scare/6126272}}</ref> |
In June 2013, frozen berries sold by US retailer Costco and purchased by around 240,000 people were the subject of a recall, after at least 158 people were infected with HAV, 69 of whom were hospitalized.<ref>{{cite news |first=Elizabeth |last=Weise |title=118 sickened in hepatitis A outbreak linked to berries |newspaper=USA Today |date=18 June 2013 |url=http://www.usatoday.com/story/news/nation/2013/06/18/hepatitis-a-frozen-berries-118-sick/2434267/}}</ref><ref>{{cite web |title=Outbreak Cases |date=28 October 2013 |work=Viral Hepatitis |publisher=Centers for Disease Control and Prevention |url=http://www.cdc.gov/hepatitis/Outbreaks/2013/A1b-03-31/index.html}}</ref> In April 2016, frozen berries sold by Costco were once again the subject of a recall, after at least 13 people in Canada were infected with HAV.<ref>{{cite news |title=Recalled Costco frozen berries linked to 13 cases of Hepatitis A |newspaper=The Canadian Press |date=19 April 2016 |url=http://www.thestar.com/news/canada/2016/04/19/recalled-costco-frozen-berries-linked-to-13-cases-of-hepatitis-a.html/}} In Australia in February 2015, a recall of frozen berries was issued after at least 19 people contracted the illness following their consumption of the product.<ref>{{cite web |title=Frozen berries Heptitus A scare |date=17 February 2015 |newspaper=ABC News Australia |url=http://www.abc.net.au/news/2015-02-17/fourth-frozen-berry-product-recalled-in-hepatitis-a-scare/6126272}}</ref> |
||
==References== |
==References== |
||
Revision as of 01:58, 21 April 2016
| Hepatitis A | |
|---|---|
| Specialty | Infectious diseases |
Hepatitis A (formerly known as infectious hepatitis) is an acute infectious disease of the liver caused by the hepatitis A virus (HAV).[1] Many cases have few or no symptoms, especially in the young.[2] The time between infection and symptoms, in those who develop them, is between two and six weeks.[3] When symptoms occur, they typically last eight weeks and may include nausea, vomiting, diarrhea, jaundice, fever, and abdominal pain.[2] Around 10–15% of people experience a recurrence of symptoms during the six months after the initial infection.[2] Acute liver failure may rarely occur with this being more common in the elderly.[2]
It is usually spread by eating or drinking food or water contaminated with infected feces.[2] Shellfish which have not been sufficiently cooked are a relatively common source.[4] It may also be spread through close contact with an infectious person.[2] While children often do not have symptoms when infected, they are still able to infect others.[2] After a single infection, a person is immune for the rest of his or her life.[5] Diagnosis requires blood testing, as the symptoms are similar to those of a number of other diseases.[2] It is one of five known hepatitis viruses: A, B, C, D, and E.
The hepatitis A vaccine is effective for prevention.[2][6] Some countries recommend it routinely for children and those at higher risk who have not previously been vaccinated.[2][7] It appears to be effective for life.[2] Other preventive measures include hand washing and properly cooking food.[2] No specific treatment is available, with rest and medications for nausea or diarrhea recommended on an as-needed basis.[2] Infections usually resolve completely and without ongoing liver disease.[2] Treatment of acute liver failure, if it occurs, is with liver transplantation.[2]
Globally, around 1.5 million symptomatic cases occur each year[2] and there were about 102 million cases in 2013.[8] It is more common in regions of the world with poor sanitation and not enough safe water.[7] In the developing world, about 90% of children have been infected by age 10, thus are immune by adulthood.[7] It often occurs in outbreaks in moderately developed countries where children are not exposed when young and vaccination is not widespread.[7] In 2010, acute hepatitis A resulted in 102,000 deaths.[9] World Hepatitis Day occurs each year on July 28 to bring awareness to viral hepatitis.[7]
Signs and symptoms
Early symptoms of hepatitis A infection can be mistaken for influenza, but some sufferers, especially children, exhibit no symptoms at all. Symptoms typically appear 2 to 6 weeks (the incubation period) after the initial infection.[10] 90% of children do not have symptoms. The time between infection and symptoms, in those who develop them, is between two and six weeks with an average of 28 days.[3]
The risk for symptomatic infection is directly related to age, with more than 80% of adults having symptoms compatible with acute viral hepatitis and the majority of children having either asymptomatic or unrecognized infections.[11]
Symptoms usually last less than 2 months, although some people can be ill for as long as 6 months:[12]
- Fatigue
- Fever
- Nausea
- Appetite loss
- Jaundice, a yellowing of the skin or whites of the eyes due to hyperbilirubinemia
- Bile is removed from blood stream and excreted in urine, giving it a dark amber colour
- Diarrhea
- Light, or clay-coloured faeces (acholic faeces)
- Abdominal discomfort[13]
- Dark colored urine
Virology
| Hepatitis A | |
|---|---|
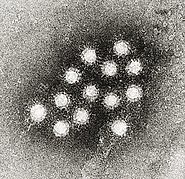
| |
| Electron micrograph of hepatitis A virions | |
| Virus classification | |
| Group: | Group IV ((+)ssRNA)
|
| Order: | |
| Family: | |
| Genus: | |
| Species: | Hepatovirus A
|
| Synonyms | |
| |
Taxonomy
Hepatovirus A is a species of virus in the order Picornavirales in the family Picornaviridae and is the type species of the genus Hepatovirus. Human and vertebrates serve as natural hosts.[14][15]
At least 13 additional species of the genus Hepatovirus have now been identified.[16] These species infect bats, rodents, hedgehogs and shrews. Phylogenetic analysis suggests a rodent origin for Hepatitis A.
A species of hepatovirus (Phopivirus) has been isolated from a seal.[17] This species shared a common ancestor with hepatitis A virus about 1800 years ago.
Another hepatovirus - Marmota Himalayana hepatovirus - has been isolated from the woodchuck Marmota himalayana.[18] This species appears to have had a common ancestor with the primate species ~1000 years ago.
Genotypes
One serotype and seven different genetic groups (four humans and three simian) have been described.[19] The human genotypes are numbered I-III. Six subtypes have been described (IA, IB, IIA, IIB, IIIA, IIIB). The simian genotypes have been numbered IV-VI. A single isolate of genotype VII isolated from a human has also been described.[20] Genotype III has been isolated from both humans and owl monkeys. Most human isolates are of genotype I.[21] Of the type I isolates subtype IA accounts for the majority.
The mutation rate in the genome has been estimated to be 1.73–9.76 x 10−4 nucleotide substitution per site per year.[22][23] The human strains appear to have diverged from the simian about 3600 years ago.[23] The mean age of genotypes III and IIIA strains has been estimated to be 592 and 202 years, respectively.[23]
Structure
Hepatovirus A is a picornavirus; it is nonenveloped and contains a single-stranded RNA packaged in a protein shell.[19] There is only one serotype of the virus, but multiple genotypes exist.[24] Codon use within the genome is biased and unusually distinct from its host. It also has a poor internal ribosome entry site.[25] In the region that codes for the HAV capsid, highly conserved clusters of rare codons restrict antigenic variability.[14][26]
| Genus | Structure | Symmetry | Capsid | Genomic arrangement | Genomic segmentation |
|---|---|---|---|---|---|
| Hepatovirus | Icosahedral | Pseudo T=3 | Nonenveloped | Linear | Monopartite |
Life cycle
Humans and vertebrates serve as the natural hosts. Transmission routes are fecal-oral and blood.[14]
Following ingestion, HAV enters the bloodstream through the epithelium of the oropharynx or intestine.[27] The blood carries the virus to its target, the liver, where it multiplies within hepatocytes and Kupffer cells (liver macrophages). Viral replication is cytoplasmic. Entry into the host cell is achieved by attachment of the virus to host receptors, which mediates endocytosis. Replication follows the positive-stranded RNA virus replication model. Positive-stranded RNA virus transcription is the method of transcription. Translation takes place by viral initiation. The virus exits the host cell by lysis, and viroporins. Virions are secreted into the bile and released in stool. HAV is excreted in large quantities about 11 days prior to appearance of symptoms or anti-HAV IgM antibodies in the blood. The incubation period is 15–50 days and mortality is less than 0.5%.
Within the liver hepatocytes, the RNA genome is released from the protein coat and is translated by the cell's own ribosomes. Unlike other picornaviruses, this virus requires an intact eukaryote initiating factor 4G (eIF4G) for the initiation of translation.[28] The requirement for this factor results in an inability to shut down host protein synthesis, unlike other picornaviruses. The virus must then inefficiently compete for the cellular translational machinery which may explain its poor growth in cell culture. Presumably for this reason, the virus has strategically adopted a naturally highly deoptimized codon usage with respect to that of its cellular host. Precisely how this strategy works is not quite clear yet.
No apparent virus-mediated cytotoxicity occurs, presumably because of the virus' own requirement for an intact eIF4G and liver pathology is likely immune-mediated.
| Genus | Host details | Tissue tropism | Entry details | Release details | Replication site | Assembly site | Transmission |
|---|---|---|---|---|---|---|---|
| Hepatovirus | Humans; vertebrates | Liver | Cell receptor endocytosis | Lysis | Cytoplasm | Cytoplasm | Oral-fecal; blood |
Transmission
The virus spreads by the fecal–oral route, and infections often occur in conditions of poor sanitation and overcrowding. Hepatitis A can be transmitted by the parenteral route, but very rarely by blood and blood products. Food-borne outbreaks are not uncommon,[29] and ingestion of shellfish cultivated in polluted water is associated with a high risk of infection.[30] About 40% of all acute viral hepatitis is caused by HAV.[27] Infected individuals are infectious prior to onset of symptoms, roughly 10 days following infection. The virus is resistant to detergent, acid (pH 1), solvents (e.g., ether, chloroform), drying, and temperatures up to 60 °C. It can survive for months in fresh and salt water. Common-source (e.g., water, restaurant) outbreaks are typical. Infection is common in children in developing countries, reaching 100% incidence, but following infection, lifelong immunity results. HAV can be inactivated by chlorine treatment (drinking water), formalin (0.35%, 37 °C, 72 hours), peracetic acid (2%, 4 hours), beta-propiolactone (0.25%, 1 hour), and UV radiation (2 μW/cm2/min).
In developing countries, and in regions with poor hygiene standards, the rates of infection with this virus are high[31] and the illness is usually contracted in early childhood. As incomes rise and access to clean water increases, the incidence of HAV decreases.[32] In developed countries, though, the infection is contracted primarily by susceptible young adults, most of whom are infected with the virus during trips to countries with a high incidence of the disease[3] or through contact with infectious persons.
Diagnosis

Although HAV is excreted in the feces towards the end of the incubation period, specific diagnosis is made by the detection of HAV-specific IgM antibodies in the blood.[33] IgM antibody is only present in the blood following an acute hepatitis A infection. It is detectable from one to two weeks after the initial infection and persists for up to 14 weeks. The presence of IgG antibodies in the blood means the acute stage of the illness is past and the person is immune to further infection. IgG antibodies to HAV are also found in the blood following vaccination, and tests for immunity to the virus are based on the detection of this antibody.[33]
During the acute stage of the infection, the liver enzyme alanine transferase (ALT) is present in the blood at levels much higher than is normal. The enzyme comes from the liver cells damaged by the virus.[34]
Hepatovirus A is present in the blood (viremia) and feces of infected people up to two weeks before clinical illness develops.[34]
Prevention
Hepatitis A can be prevented by vaccination, good hygiene, and sanitation.[1][35]
The two types of vaccines are one containing inactivated hepatitis A virus, and another containing a live but attenuated virus.[36] Both provide active immunity against a future infection. The vaccine protects against HAV in more than 95% of cases for longer than 25 years.[37] In the US, the vaccine was first used in 1996 for children in high-risk areas, and in 1999 it was spread to areas with elevating levels of infection.[38]
The vaccine is given by injection. An initial dose provides protection starting two to four weeks after vaccination; the second booster dose, given six to 12 months later, provides protection for over 20 years.[38]
Vaccination programmes
The vaccine was introduced in 1992 and was initially recommended for persons at high risk. Since then, Bahrain and Israel have embarked on eradication programmes.[39] Australia, China, Belarus, Italy, Spain, and the United States have started similar programmes. The incidence of hepatitis A where widespread vaccination has been practised has decreased dramatically. In China and the United States, the incidence of hepatitis A has decreased by 90% since 1990.[40][41]
In the United States, vaccination of children is recommended at 1 and 2 years of age.[2] It is also recommended in those who have not been previously immunized and who have been exposed or are likely to be exposed due to travel.[2]
Treatment
There is no specific treatment for hepatitis A. Recovery from symptoms following infection may be slow and may take several weeks or months. Therapy is aimed at maintaining comfort and adequate nutritional balance, including replacement of fluids that are lost from vomiting and diarrhoea. [42]
Prognosis
In the United States in 1991, the mortality rate for hepatitis A was four deaths per 1000 cases for the general population, but a higher at 17.5 per 1000 in those aged 50 and over. The risk of death from acute liver failure following HAV infection increases with age and when the person has underlying chronic liver disease.
Young children who are infected with hepatitis A typically have a milder form of the disease, usually lasting from 1–3 weeks, whereas adults tend to experience a much more severe form of the disease.[29]
Epidemiology

Globally, symptomatic HAV infections are believed to occur in around 1.4 million people a year.[2] About 102 million cases occurred all together in 2013.[8] In 2010, acute hepatitis A resulted in 102,000 deaths, which is slightly up from 99,000 in 1990.[9] Developed countries have low circulating levels of hepatovirus A while developing countries have higher levels of circulation.[43] Most adolescents and adults in developing countries have already had the disease, thus are immune.[43] Adults in midlevel countries may be at risk of disease with the potential of being exposed.[43]
Countries
Over 30,000 cases of hepatitis A were reported to the CDC in the US in 1997, but the number has since dropped to less than 2,000 cases reported per year.[44]
The most widespread hepatitis A outbreak in the 2003 United States hepatitis outbreak afflicted at least 640 people (killing four) in northeastern Ohio and southwestern Pennsylvania in late 2003. The outbreak was blamed on tainted green onions at a restaurant in Monaca, Pennsylvania.[45][46] In 1988, more than 300,000 people in Shanghai, China, were infected with HAV after eating clams (Anadara subcrenata) from a contaminated river.[27]
In June 2013, frozen berries sold by US retailer Costco and purchased by around 240,000 people were the subject of a recall, after at least 158 people were infected with HAV, 69 of whom were hospitalized.[47][48] In April 2016, frozen berries sold by Costco were once again the subject of a recall, after at least 13 people in Canada were infected with HAV.Cite error: A <ref> tag is missing the closing </ref> (see the help page).
References
- ^ a b Ryan KJ, Ray CG (editors) (2004). Sherris Medical Microbiology (4th ed.). McGraw Hill. pp. 541–4. ISBN 0-8385-8529-9.
{{cite book}}:|author=has generic name (help) - ^ a b c d e f g h i j k l m n o p q r s Matheny, SC; Kingery, JE (1 December 2012). "Hepatitis A." Am Fam Physician. 86 (11): 1027–34, quiz 1010–2. PMID 23198670.
- ^ a b c Connor BA (2005). "Hepatitis A vaccine in the last-minute traveler". Am. J. Med. 118 (Suppl 10A): 58S–62S. doi:10.1016/j.amjmed.2005.07.018. PMID 16271543.
- ^ Bellou, M.; Kokkinos, P.; Vantarakis, A. (March 2013). "Shellfish-borne viral outbreaks: a systematic review". Food Environ Virol. 5 (1): 13–23. doi:10.1007/s12560-012-9097-6. PMID 23412719.
- ^ The Encyclopedia of Hepatitis and Other Liver Diseases. Infobase. 2006. p. 105. ISBN 9780816069903.
- ^ Irving, GJ.; Holden, J.; Yang, R.; Pope, D. (2012). "Hepatitis A immunisation in persons not previously exposed to hepatitis A.". Cochrane Database Syst Rev. 7: CD009051. doi:10.1002/14651858.CD009051.pub2. PMID 22786522.
- ^ a b c d e "Hepatitis A Fact sheet N°328". World Health Organization. July 2013. Retrieved 20 February 2014.
- ^ a b Global Burden of Disease Study 2013, Collaborators (22 August 2015). "Global, regional, and national incidence, prevalence, and years lived with disability for 301 acute and chronic diseases and injuries in 188 countries, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013". Lancet (London, England). 386 (9995): 743–800. PMID 26063472.
{{cite journal}}:|first1=has generic name (help)CS1 maint: numeric names: authors list (link) - ^ a b Lozano, R (Dec 15, 2012). "Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: a systematic analysis for the Global Burden of Disease Study 2010". Lancet. 380 (9859): 2095–128. doi:10.1016/S0140-6736(12)61728-0. PMID 23245604.
- ^ "Hepatitis A Symptoms". eMedicineHealth. 2007-05-17. Retrieved 2007-05-18.
- ^ Ciocca M. (2000). "Clinical course and consequences of hepatitis A infection". Vaccine. 18: 71–4. doi:10.1016/S0264-410X(99)00470-3. PMID 10683554.
- ^ "Hepatitis A Information for the Public". Center for Disease Control. 2009-09-17. Retrieved 2011-01-08.
- ^ http://www.who.int/mediacentre/factsheets/fs328/en/
- ^ a b c "Viral Zone". ExPASy. Retrieved 15 June 2015.
- ^ ICTV. "Virus Taxonomy: 2014 Release". Retrieved 15 June 2015.
- ^ Drexler JF, Corman VM, Lukashev AN, van den Brand JM, Gmyl AP, Brünink S, Rasche A, Seggewiβ N, Feng H, Leijten LM, Vallo P, Kuiken T, Dotzauer A, Ulrich RG, Lemon SM, Drosten C; Hepatovirus Ecology Consortium. Evolutionary origins of hepatitis A virus in small mammals. Proc Natl Acad Sci U S A112(49):15190-15195. doi: 10.1073/pnas.1516992112
- ^ Anthony SJ, St Leger JA, Liang E, Hicks AL, Sanchez-Leon MD, Jain K, Lefkowitch JH, Navarrete-Macias I, Knowles N, Goldstein T, Pugliares K, Ip HS, Rowles T, Lipkin WI (2015) Discovery of a novel hepatovirus (Phopivirus of seals) related to human hepatitis A virus. MBio 6(4). pii: e01180-15. doi: 10.1128/mBio.01180-15
- ^ Yu JM, Li LL, Zhang CY, Lu S, Ao YY, Gao HC, Xie ZP, Xie GC, Sun XM, Pang LL, Xu JG, Lipkin WI, Duan ZJ (2016) A novel hepatovirus identified in wild woodchuck Marmota himalayana .Sci Rep 6:22361. doi: 10.1038/srep22361
- ^ a b Cristina J, Costa-Mattioli M (August 2007). "Genetic variability and molecular evolution of hepatitis A virus". Virus Res. 127 (2): 151–7. doi:10.1016/j.virusres.2007.01.005. PMID 17328982.
- ^ Ching KZ, Nakano T, Chapman LE, Demby A, Robertson BH (January 2002). "Genetic characterization of wild-type genotype VII hepatitis A virus". J. Gen. Virol. 83 (Pt 1): 53–60. PMID 11752700.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ de Paula VS, Baptista ML, Lampe E, Niel C, Gaspar AM (January 2002). "Characterization of hepatitis A virus isolates from subgenotypes IA and IB in Rio de Janeiro, Brazil". J. Med. Virol. 66 (1): 22–7. doi:10.1002/jmv.2106. PMID 11748654.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Moratorio G, Costa-Mattioli M, Piovani R, Romero H, Musto H, Cristina J (November 2007). "Bayesian coalescent inference of hepatitis A virus populations: evolutionary rates and patterns". J. Gen. Virol. 88 (Pt 11): 3039–42. doi:10.1099/vir.0.83038-0. PMID 17947528.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ a b c Kulkarni MA, Walimbe AM, Cherian S, Arankalle VA (December 2009). "Full length genomes of genotype IIIA Hepatitis A Virus strains (1995–2008) from India and estimates of the evolutionary rates and ages". Infect. Genet. Evol. 9 (6): 1287–94. doi:10.1016/j.meegid.2009.08.009. PMID 19723592.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Costa-Mattioli M, Di Napoli A, Ferré V, Billaudel S, Perez-Bercoff R, Cristina J (December 2003). "Genetic variability of hepatitis A virus". J. Gen. Virol. 84 (Pt 12): 3191–201. doi:10.1099/vir.0.19532-0. PMID 14645901.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Whetter LE, Day SP, Elroy-Stein O, Brown EA, Lemon SM (August 1994). "Low efficiency of the 5' nontranslated region of hepatitis A virus RNA in directing cap-independent translation in permissive monkey kidney cells". J. Virol. 68 (8): 5253–63. PMC 236470. PMID 8035522.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Aragonès L, Bosch A, Pintó RM (February 2008). "Hepatitis A virus mutant spectra under the selective pressure of monoclonal antibodies: codon usage constraints limit capsid variability". J. Virol. 82 (4): 1688–700. doi:10.1128/JVI.01842-07. PMC 2258700. PMID 18057242.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ a b c Murray, P.R., Rosenthal, K.S. & Pfaller, M.A. (2005). Medical Microbiology 5th ed., Elsevier Mosby.
- ^ Aragonès L, Guix S, Ribes E, Bosch A, Pintó RM (March 2010). Andino, Raul (ed.). "Fine-tuning translation kinetics selection as the driving force of codon usage bias in the hepatitis A virus capsid". PLoS Pathog. 6 (3): e1000797. doi:10.1371/journal.ppat.1000797. PMC 2832697. PMID 20221432.
{{cite journal}}: CS1 maint: multiple names: authors list (link) CS1 maint: unflagged free DOI (link) - ^ a b Brundage SC, Fitzpatrick AN (2006). "Hepatitis A". Am Fam Physician. 73 (12): 2162–8. PMID 16848078.
- ^ Lees D (2000). "Viruses and bivalve shellfish". Int. J. Food Microbiol. 59 (1–2): 81–116. doi:10.1016/S0168-1605(00)00248-8. PMID 10946842.
- ^ Steffen R (October 2005). "Changing travel-related global epidemiology of hepatitis A". Am. J. Med. 118 (Suppl 10A): 46S–49S. doi:10.1016/j.amjmed.2005.07.016. PMID 16271541.
- ^ Jacobsen KH, Koopman JS (2005). "The effects of socioeconomic development on worldwide hepatitis A virus seroprevalence patterns". Int J Epidemiol. 34 (3): 600–9. doi:10.1093/ije/dyi062. PMID 15831565.
- ^ a b Stapleton JT (1995). "Host immune response to hepatitis A virus". J. Infect. Dis. 171 (Suppl 1): S9–14. doi:10.1093/infdis/171.Supplement_1.S9. PMID 7876654.
- ^ a b Musana KA, Yale SH, Abdulkarim AS (2004). "Tests of Liver Injury". Clin Med Res. 2 (2): 129–31. doi:10.3121/cmr.2.2.129. PMC 1069083. PMID 15931347.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ "Hepatitis A — Prevention". NHS Choices. National Health Service (England). 21 March 2012.
- ^ Irving GJ, Holden J, Yang R, Pope D (2012). Irving, Greg J (ed.). "Hepatitis A immunisation in persons not previously exposed to hepatitis A". Cochrane Database Syst Rev. 7: CD009051. doi:10.1002/14651858.CD009051.pub2. PMID 22786522.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Nothdurft HD (July 2008). "Hepatitis A vaccines". Expert Rev Vaccines. 7 (5): 535–45. doi:10.1586/14760584.7.5.535. PMID 18564009.
- ^ a b "Hepatitis A Vaccine: What you need to know" (PDF). Vaccine Information Statement. CDC. 2006-03-21. Retrieved 2007-03-12.
- ^ André FE (2006). "Universal mass vaccination against hepatitis A". Curr Top Microbiol Immunol. 304: 95–114. PMID 16989266.
- ^ Cui F, Hadler SC, Zheng H, Wang F, Zhenhua W, Yuansheng H, Gong X, Chen Y, Liang X; et al. (2009). "Hepatitis A surveillance and vaccine use in China from 1990 through 2007". J Epidemiol. 19 (4): 189–195. doi:10.2188/jea.JE20080087. PMID 19561383.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Daniels D, Grytdal S, Wasley A (May 2009). "Surveillance for acute viral hepatitis — United States, 2007" (PDF). MMWR Surveill Summ. 58 (3): 1–27. PMID 19478727.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ http://www.who.int/mediacentre/factsheets/fs328/en/
- ^ a b c Jacobsen, KH; Wiersma, ST (24 September 2010). "Hepatitis A virus seroprevalence by age and world region, 1990 and 2005". Vaccine. 28 (41): 6653–7. doi:10.1016/j.vaccine.2010.08.037. PMID 20723630.
- ^ "Hepatitis A Information for Health Professionals — Statistics and Surveillance". Centers for Disease Control and Prevention. Retrieved 28 January 2014.
- ^ Centers for Disease Control and Prevention (CDC) (November 2003). "Hepatitis A outbreak associated with green onions at a restaurant—Monaca, Pennsylvania, 2003" (PDF). MMWR Morb. Mortal. Wkly. Rep. 52 (47): 1155–7. PMID 14647018.
- ^ Wheeler C, Vogt TM, Armstrong GL, et al. (September 2005). "An outbreak of hepatitis A associated with green onions". N. Engl. J. Med. 353 (9): 890–7. doi:10.1056/NEJMoa050855. PMID 16135833.
- ^ Weise, Elizabeth (18 June 2013). "118 sickened in hepatitis A outbreak linked to berries". USA Today.
- ^ "Outbreak Cases". Viral Hepatitis. Centers for Disease Control and Prevention. 28 October 2013.
External links
- Template:Dmoz
- CDC's hepatitis A links
- Virus Pathogen Database and Analysis Resource (ViPR): Picornaviridae
- "Human hepatitis A virus". NCBI Taxonomy Browser. 208726.
