Vitamin B12
 | |
 | |
| Clinical data | |
|---|---|
| Routes of administration | oral, iv |
| ATC code | |
| Legal status | |
| Legal status |
|
| Pharmacokinetic data | |
| Bioavailability | readily absorbed in lower half ileum |
| Protein binding | Very high to specific transcobalamins plasma proteins Binding of hydroxocobalamin is slightly higher than cyanocobalamin. |
| Metabolism | hepatic |
| Elimination half-life | Approximately 6 days (400 days in the liver) |
| Excretion | renal |
| Identifiers | |
| |
| CAS Number | |
| PubChem CID | |
| DrugBank | |
| Chemical and physical data | |
| Formula | C63H88CoN14O14P |
| Molar mass | 1355.37 g/mol g·mol−1 |
Cyanocobalamin is a compound that is metabolized to a vitamin in the B complex commonly known as vitamin B12 (or B12 for short).
Terminology
The name vitamin B12 is used in two different ways.
- In a broad sense it refers to a group of cobalt-containing compounds known as cobalamins - cyanocobalamin (an artifact formed as a result of the use of cyanide in the purification procedures), hydroxocobalamin and the two coenzyme forms of B12, methylcobalamin (MeB12) and 5-deoxyadenosylcobalamin (adenosylcobalamin - AdoB12).
- In a more specific way, the term B12 is used to refer to only one of these forms, cyanocobalamin, which is the principal B12 form used for foods and in nutritional supplements.
Pseudo-B12 refers to B12-like substances which are found in certain organisms; however, these substances do not have B12 biological activity for humans.
Structure
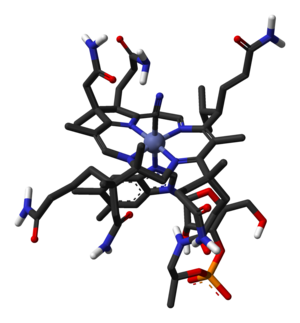
B12 is the most chemically complex of all the vitamins. The structure of B12 is based on a corrin ring, which is similar to the porphyrin ring found in heme, chlorophyll, and cytochrome. The central metal ion is Co (cobalt). Four of the six coordination sites are provided by the corrin ring, and a fifth by a dimethylbenzimidazole group. The sixth coordination site, the center of reactivity, is variable, being a cyano group (-CN), a hydroxyl group (-OH), a methyl group (-CH3) or a 5'-deoxyadenosyl group (here the C5' atom of the deoxyribose forms the covalent bond with Co), respectively, to yield the four B12 forms mentioned above. The covalent C-Co bond is one of first examples of carbon-metal bonds in biology. The hydrogenases and, by necessity, enzymes associated with CO utilization, involve metal-carbon bonds.[1]
Synthesis
B12 cannot be made by plants or animals[2], as the only type of organisms that have the enzymes required for the synthesis of B12 are bacteria and archaea. The total synthesis of B12 was reported by Robert Burns Woodward[3] [4] and Albert Eschenmoser[5], and remains one of the classic feats of total synthesis.
Functions
Coenzyme B12's reactive C-Co bond participates in two types of enzyme-catalyzed reactions. [6]
- Rearrangements in which a hydrogen atom is directly transferred between two adjacent atoms with concomitant exchange of the second substituent, X, which may be a carbon atom with substituents, an oxygen atom of an alcohol, or an amine.
- Methyl (-CH3) group transfers between two molecules.
In humans there are only two coenzyme B12-dependent enzymes:
- MUT which uses the AdoB12 form and reaction type 1 to catalyze a carbon skeleton rearrangement (the X group is -COSCoA). MUT's reaction converts MMl-CoA to Su-CoA, an important step in the extraction of energy from proteins and fats (for more see MUT's reaction mechanism). This functionality is lost in vitamin B12 deficiency, and can be measured clinically as an increased methylmalonic acid level in vitro
- MTR, a methyl transfer enzyme, which uses the MeB12 and reaction type 2 to catalyzes the conversion of the amino acid Hcy into Met (for more see MTR's reaction mechanism). This functionality is lost in vitamin B12 deficiency, and can be measured clinically as an increased homocysteine level in vitro. Increased homocysteine can also be diagnostic of a folic acid deficiency.
Human digestion
The human physiology of vitamin B12 is complex, and therefore is prone to mishaps leading to vitamin B12 deficiency. The vitamin enters the digestive tract bound to proteins, known as salivary R-binders. Stomach proteolysis of these proteins requires an acid pH, and also requires proper pancreatic release of proteolytic enzymes. The vitamin B12 then attaches to gastric intrinsic factor, which is generated by the gastric parietal cells. The conjugated vitamin B12-intrinsic factor complex can then be absorbed by the terminal ileum of the small bowel. Absorption of vitamin B12 therefore requires an intact and functioning stomach, exocrine pancreas, intrinsic factor, and small bowel. Problems with any one of these organs makes a vitamin B12 deficiency possible.
History as a treatment for anemia
B12 deficiency is the cause of several forms of anemia. The treatment for this disease was first devised by William Murphy who devised experiments on anemia in dogs due to blood loss and then fed them various substances to see what (if anything) would make them healthy again. He discovered that ingesting large amounts of liver seemed to cure the disease. George Minot and George Whipple then set about to chemically isolate the curative substance and ultimately were able to isolate vitamin B12 from the liver. For this, all three shared the 1934 Nobel Prize in Medicine.
The chemical structure of the molecule was determined by Dorothy Crowfoot Hodgkin and her team in 1956, based on crystallographic data.
Other medical uses
Hydroxycobalamin, also known as Vitamin B12a, is used in Europe both for vitamin B12 deficiency and as a treatment for cyanide poisoning, sometimes with a large amount (5-10 g) given intravenously, and sometimes in combination with sodium thiosulfate[7]. The mechanism of action is straightforward, the hydroxycobalamin hydroxide ligand is displaced by the toxic cyanide ion, and the resulting harmless B12 complex is excreted in urine. In the United States, the FDA has approved in 2006 the use of hydroxocobalamin for acute treatment of cyanide poisoning.
Deficiency
The usual daily intake in the Western diet is 5-7 µg (Food and Drug Administration (FDA) Daily Value [8]); the daily requirement is 1-2 µg. B12 is mostly absorbed in the terminal ileum. The production of intrinsic factor in the parietal cells of the stomach is vital to absorption of this vitamin in terminal ileum. Megaloblastic anemia can result from inadequate intake of B12, inadequate production of intrinsic factor (pernicious anemia), disorders of the terminal ileum resulting in malabsorption, or by competition for available B12 (such as fish tapeworms or bacteria present in blind loop syndrome).
The diabetes medication, metformin, can be associated with vitamin B12 deficiency, according to a retrospective study. The mechanism may include inhibition of calcium-dependent ileal absorption of the B12-intrinsic factor complex. [9]. Primary care health professionals should consider vitamin B12 deficiency in the differential diagnosis of diabetic patients with neuropathic symptoms while taking metformin.
B12 deficiency is manifested primarily by anemia and macrocytosis; other cell lines such as white blood cells and platelets are often also low. Bone marrow examination may show megaloblastic hemopoiesis. Serum homocysteine and methylmalonic acid levels are also high in B12 deficiency and can be helpful if the diagnosis is unclear.
Neurological signs of B12 deficiency, which can occur without accompanying hematologic abnormalities, include demyelination and irreversible nerve cell death. Symptoms include numbness or tingling of the extremities and an ataxic gait, a syndrome known as subacute combined degeneration of the cord.
The American Psychiatric Association's American Journal of Psychiatry has published studies showing a relationship between depression levels and deficient B12 blood levels in elderly people in 2000 [10] and 2002 [11].
Diagnosis of B12 deficiency
Serum B12 levels are often low in B12 deficiency, but there does not exist a robust assay, and if other features of B12 deficiency are present then the diagnosis must not be discounted. One possible explanation for normal B12 levels in B12 deficiency is antibody interference in people with high titres of intrinsic factor antibody.[12] Bone marrow aspiration, serum homocysteine and methylmalonic acid levels can also be helpful.[13]
Treatment of B12 deficiency
Traditionally, treatment for B12 deficiency was through intramuscular injections of cyanocobalamin. However, it has been appreciated since the 1960s that deficiency can sometimes be treated with oral B12 supplements when given in sufficient doses. When given in oral doses ranging from 0.1–2 mg daily, B12 can be absorbed in a pathway that does not require an intact ileum or intrinsic factor. [14][15] Oral absorption is limited so regular intramuscular injections of cyanocobalamin or hydroxocobalamin are necessary to restore systemic stores to physiological levels. The Schilling test can determine whether symptoms of B12 deficiency are caused by lack of intrinsic factor, though this is being performed less often due to the lack of availability of reagent for the test.
Sources
Vitamin B12 is naturally found in foods that harbor B12 bacteria including meat (especially liver and shellfish), eggs, and milk products. Fortified breakfast cereals are a particularly valuable source of vitamin B12 for vegetarians and vegans. Table 1 lists a variety of food sources of vitamin B12.
B12 can be supplemented in healthy subjects by oral pill; sublingual pill, liquid, or strip; or by injection. B12 is available singly or in combination with other supplements. B12 supplements are available in forms including cyanocobalamin, hydroxocobalamin, methylcobalamin, and adenosylcobalamin (sometimes called cobamamide or dibencozide).
Cyanocobalamin is converted to its active forms, first hydroxocobalamin and then methylcobalamin and adenosylcobalamin in the liver. A 2003 study found no significant difference in absorption for serum levels from oral vs sublingual delivery of 500 micrograms of cobalamin [16]. Injection is useful and usually necessary in cases where digestive absorption is impaired. Oral absorption is complex and requires specific intestinal transport proteins (intrinsic factor) produced in the stomach. In any case the absorption is saturated and is rate limited.
While lacto-ovo vegetarians usually get enough B12 through dairy products or eggs, it may be found lacking in those practicing vegan diets who do not use multivitamin supplements or eat B12 fortified foods, such as fortified breakfast cereals, fortified soy-based products, and fortified energy bars. Claimed sources of B12 that have been shown through direct studies[17] of vegans to be inadequate or unreliable include, nori (a seaweed), barley grass, and human gut bacteria. However B12 deficiencies in vegans are so uncommon that the medical press still record cases. [18] People on a vegan raw food diet are also susceptible to B12 deficiency if no supplementation is used[19].
A natural vegan source of B12 is the Chinese herb Dang Gui (Angelica sinensis) [20]. The herb is used in Traditional Chinese medicine for treating anemia.[1] Other potential sources of B12 for vegans include Indonesian tempeh [2], ontjom, and other fermented food products. Spirulina, an algae that has recently gained popularity as a dietary supplement, may also contain some B12. Another source of B12 is yeast spreads, such as Marmite and Vegemite, which are suitable for vegetarians and vegans.
Interestingly, certain insects such as termites have been found to contain B12. [21]
Cyanocobalamin may also found in many energy drinks.
Allergies
Vitamin B12 supplements should be avoided in people sensitive or allergic to cobalamin, cobalt or any other product ingredients.
Side effects, contraindications, and warnings
- Cardiovascular: Caution should be used in patients undergoing angioplasty since an intravenous loading dose of folic acid, vitamin B6 and vitamin B12 followed by oral administration of folic acid 1.2mg plus vitamin B6 48mg and vitamin B12 60mcg taken daily after coronary stenting might actually increase restenosis rates. Due to the potential for harm this combination of vitamins should not be recommended for patients receiving coronary stents.
- Dermatologic: Itching, rash, transitory exanthema, and urticaria have been reported. Vitamin B12 (20 micrograms/day) and pyridoxine (80mg/day) has been associated with cases of rosacea fulminans, characterized by intense erythema with nodules, papules, and pustules. Symptoms may persist for up to 4 months after the supplement is stopped, and may require treatment with systemic corticosteroids and topical therapy.
- Gastrointestinal: Diarrhea has been reported.
- Hematologic: Peripheral vascular thrombosis has been reported. Treatment of vitamin B12 deficiency can unmask polycythemia vera, which is characterized by an increase in blood volume and the number of red blood cells. The correction of megaloblastic anemia with vitamin B12 can result in fatal hypokalemia and gout in susceptible individuals, and it can obscure folate deficiency in megaloblastic anemia. Caution is warranted.
- Leber's disease: Vitamin B12 in the form of cyanocobalamin is contraindicated in early Leber's disease, which is hereditary optic nerve atrophy. Vitamin B12 can cause severe and swift optic atrophy.
Pregnancy and breastfeeding
Vitamin B12 is likely safe when used orally in amounts that do not exceed the recommended dietary allowance (RDA). The RDA for vitamin B12 in pregnant women is 2.6mcg per day and 2.8mcg during lactation periods.
There is insufficient reliable information available about the safety of consuming greater amounts of Vitamin B12 during pregnancy.
Interactions
Interactions with drugs
- Alcohol (ethanol): Excessive alcohol intake lasting longer than two weeks can decrease vitamin B12 absorption from the gastrointestinal tract.
- Aminosalicylic acid (para-aminosalicylic acid, PAS, Paser): Aminosalicylic acid can reduce oral vitamin B12 absorption, possibly by as much as 55%, as part of a general malabsorption syndrome. Megaloblastic changes, and occasional cases of symptomatic anemia have occurred, usually after doses of 8 to 12 grams/day for several months. Vitamin B12 levels should be monitored in people taking aminosalicylic acid for more than one month.
- Antibiotics: An increased bacterial load can bind significant amounts of vitamin B12 in the gut, preventing its absorption. In people with bacterial overgrowth of the small bowel, antibiotics such as metronidazole (Flagyl®) can actually improve vitamin B12 status. The effects of most antibiotics on gastrointestinal bacteria are unlikely to have clinically significant effects on vitamin B12 levels.
- Birth control pills: The data regarding the effects of oral contraceptives on vitamin B12 serum levels are conflicting. Some studies have found reduced serum levels in oral contraceptive users, but others have found no effect despite use of oral contraceptives for up to 6 months. When oral contraceptive use is stopped, normalization of vitamin B12 levels usually occurs. Lower vitamin B12 serum levels seen with oral contraceptives probably are not clinically significant.
- Chloramphenicol (Chloromycetin®): Limited case reports suggest that chloramphenicol can delay or interrupt the reticulocyte response to supplemental vitamin B12 in some patients. Blood counts should be monitored closely if this combination cannot be avoided.
- Cobalt irradiation: Cobalt irradiation of the small bowel can decrease gastrointestinal (GI) absorption of vitamin B12.
- Colchicine: Colchicine in doses of 1.9 to 3.9mg/day can disrupt normal intestinal mucosal function, leading to malabsorption of several nutrients, including vitamin B12. Lower doses do not seem to have a significant effect on vitamin B12 absorption after 3 years of colchicine therapy. The significance of this interaction is unclear. Vitamin B12 levels should be monitored in people taking large doses of colchicine for prolonged periods.
- Colestipol (Colestid®), Cholestyramine (Questran®): These resins used for sequestering bile acids in order to decrease cholesterol, can decrease gastrointestinal (GI) absorption of vitamin B12. It is unlikely that this interaction will deplete body stores of vitamin B12 unless there are other factors contributing to deficiency. In a group of children treated with cholestyramine for up to 2.5 years there was not any change in serum vitamin B12 levels. Routine supplements are not necessary.
- H2-receptor antagonists: include cimetidine (Tagamet®), famotidine (Pepcid®), nizatidine (Axid®), and ranitidine (Zantac®). Reduced secretion of gastric acid and pepsin produced by H2 blockers can reduce absorption of protein-bound (dietary) vitamin B12, but not of supplemental vitamin B12. Gastric acid is needed to release vitamin B12 from protein for absorption. Clinically significant vitamin B12 deficiency and megaloblastic anemia are unlikely, unless H2 blocker therapy is prolonged (2 years or more), or the person's diet is poor. It is also more likely if the person is rendered achlorhydric (with complete absence of gastric acid secretion), which occurs more frequently with proton pump inhibitors than H2 blockers. Vitamin B12 levels should be monitored in people taking high doses of H2 blockers for prolonged periods.
- Metformin (Glucophage®): Metformin may reduce serum folic acid and vitamin B12 levels. These changes can lead to hyperhomocysteinemia, adding to the risk of cardiovascular disease in people with diabetes.[citation needed] There are also rare reports of megaloblastic anemia in people who have taken metformin for 5 years or more. Reduced serum levels of vitamin B12 occur in up to 30% of people taking metformin chronically.[22][23] However, clinically significant deficiency is not likely to develop if dietary intake of vitamin B12 is adequate. Deficiency can be corrected with vitamin B12 supplements even if metformin is continued. The metformin-induced malabsorption of vitamin B12 is reversible by oral calcium supplementation.[24] The general clinical significance of metformin upon B12 levels is as yet unknown.[25]
- Neomycin: Absorption of vitamin B12 can be reduced by neomycin, but prolonged use of large doses is needed to induce pernicious anemia. Supplements are not usually needed with normal doses.
- Nicotine: Nicotine can reduce serum vitamin B12 levels. The need for vitamin B12 supplementation has not been adequately studied.
- Nitrous oxide: Nitrous oxide inactivates the cobalamin form of vitamin B12 by oxidation. Symptoms of vitamin B12 deficiency, including sensory neuropathy, myelopathy, and encephalopathy, can occur within days or weeks of exposure to nitrous oxide anesthesia in people with subclinical vitamin B12 deficiency. Symptoms are treated with high doses of vitamin B12, but recovery can be slow and incomplete. People with normal vitamin B12 levels have sufficient vitamin B12 stores to make the effects of nitrous oxide insignificant, unless exposure is repeated and prolonged (such as recreational use). Vitamin B12 levels should be checked in people with risk factors for vitamin B12 deficiency prior to using nitrous oxide anesthesia.
- Phenytoin (Dilantin®), phenobarbital, primidone (Mysoline®): These anticonvulsants have been associated with reduced vitamin B12 absorption, and reduced serum and cerebrospinal fluid levels in some patients. This may contribute to the megaloblastic anemia, primarily caused by folate deficiency, associated with these drugs. It's also suggested that reduced vitamin B12 levels may contribute to the neuropsychiatric side effects of these drugs. Patients should be encouraged to maintain adequate dietary vitamin B12 intake. Folate and vitamin B12 status should be checked if symptoms of anemia develop.
- Proton pump inhibitors (PPIs): The PPIs include omeprazole (Prilosec®, Losec®), lansoprazole (Prevacid®), rabeprazole (Aciphex®), pantoprazole (Protonix®, Pantoloc®), and esomeprazole (Nexium®). The reduced secretion of gastric acid and pepsin produced by PPIs can reduce absorption of protein-bound (dietary) vitamin B12, but not supplemental vitamin B12. Gastric acid is needed to release vitamin B12 from protein for absorption. Reduced vitamin B12 levels may be more common with PPIs than with H2-blockers, because they are more likely to produce achlorhydria (complete absence of gastric acid secretion). However, clinically significant vitamin B12 deficiency is unlikely, unless PPI therapy is prolonged (2 years or more) or dietary vitamin intake is low. Vitamin B12 levels should be monitored in people taking high doses of PPIs for prolonged periods.
- Zidovudine (AZT, Combivir®, Retrovir®): Reduced serum vitamin B12 levels may occur when zidovudine therapy is started. This adds to other factors that cause low vitamin B12 levels in people with HIV, and might contribute to the hematological toxicity associated with zidovudine. However, data suggests vitamin B12 supplements are not helpful for people taking zidovudine.
Interactions with herbs and dietary supplements
- Folic acid: Folic acid, particularly in large doses, can mask vitamin B12 deficiency. In vitamin B12 deficiency, folic acid can produce hematologic improvement in megaloblastic anemia, while allowing potentially irreversible neurological damage to progress. Vitamin B12 status should be determined before folic acid is given as monotherapy.
- Potassium: Potassium supplements can reduce absorption of vitamin B12 in some people. This effect has been reported with potassium chloride and, to a lesser extent, with potassium citrate. Potassium might contribute to vitamin B12 deficiency in some people with other risk factors, but routine supplements are not necessary.
Footnotes
- ^ Bioorganometallics: Biomolecules, Labeling, Medicine; Jaouen, G., Ed. Wiley-VCH: Weinheim, 2006.3-527-30990-X.
- ^ G. Loeffler (2005). Basiswissen Biochemie. p. 606.
{{cite book}}: Unknown parameter|isdn=ignored (help) - ^ Woodward,RB (1973). "The Total Synthesis of Vitamin B12". Pure Appl Chem. 33(1): 145–77.
- ^ Khan,AG and Easwaran,SV (2003). "Woodward's Synthesis of Vitamin B12". Resonance. 8: 8–16.
{{cite journal}}: Cite has empty unknown parameter:|1=(help)CS1 maint: multiple names: authors list (link) - ^ Riether, D. and Mulzer, J. (2003). "Total Synthesis of Cobyric Acid: Historical Development and Recent Synthetic Innovations". Eur. J. Org. Chem. (1): 30–45.
{{cite journal}}: Cite has empty unknown parameter:|1=(help)CS1 maint: multiple names: authors list (link) - ^ Donald and Judith Voet (1995). Biochemistry (2nd ed.). John Wiley & Sons Ltd. p. 675. ISBN 0-471-58651-X.
- ^ Hall AH, Rumack BH. Hydroxycobalamin/sodium thiosulfate as a cyanide antidote. J Emerg Med. 1987;5(2):115-21. PMID 3295013.
- ^ "Dietary Supplement Fact Sheet: Vitamin B12". National Institutes of Health: Office of Dietary Supplements. Retrieved 2006-06-06.
- ^ Ting R, Szeto C, Chan M, Ma K, Chow K (2006). "Risk factors of vitamin B(12) deficiency in patients receiving metformin". Arch Intern Med. 166 (18): 1975–9. PMID 17030830.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Brenda W. J. H. Penninx; et al. (2000). "Vitamin B12 Deficiency and Depression in Physically Disabled Older Women: Epidemiologic Evidence From the Women's Health and Aging Study". Am. J. Psychiatry. 157: 715–721. PMID 10784463.
{{cite journal}}: Explicit use of et al. in:|author=(help) - ^ Henning Tiemeier; et al. (2002). "Vitamin B12, Folate, and Homocysteine in Depression: The Rotterdam Study". Am. J. Psychiatry. 159: 2099–2101. PMID 12450964.
{{cite journal}}: Explicit use of et al. in:|author=(help) - ^ Hamilton MS, Blackmore S, Lee A. (2006). "Possible cause of flase normal B-12 assays (letter)". Brit Med J. 333 (7569): 654–5.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Devalia V (2006). "Diagnosing vitamin B-12 deficiency on the basis of serum B-12 assay". Brit J Med. 333 (7564): 385–6. PMID 16916826.
- ^ Antoinette M. Kuzminski; et al. (1998). "Effective Treatment of Cobalamin Deficiency With Oral Cobalamin". Blood. 92 (4): 1191–1198. PMID 9694707.
{{cite journal}}: Explicit use of et al. in:|author=(help) - ^ Butler CC, Vidal-Alaball J, Cannings-John R; et al. (2006). "Oral vitamin B12 versus intramuscular vitamin B12 for vitamin B12 deficiency: a systematic review of randomized controlled trials". Fam Pract. 23 (3): 279–85. PMID 16585128.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Sharabi A, Cohen E, Sulkes J, Garty M. Replacement therapy for vitamin B12 deficiency: comparison between the sublingual and oral route. Br J Clin Pharmacol. 2003 Dec;56(6):635-8. PMID 14616423.
- ^ Norris, Jack, RD. "B12 in Tempeh, Seaweeds, Organic Produce, and Other Plant Foods". VeganHealth.org. Retrieved 2006-09-10.
{{cite web}}: CS1 maint: multiple names: authors list (link) - ^ Gerras, Charles. The Complete Book of Vitamins. Emmaus, PA: Rodale Press, 1977.
- ^ Donaldson MS. Metabolic vitamin B12 status on a mostly raw vegan diet with follow-up using tablets, nutritional yeast, or probiotic supplements. Ann Nutr Metab. 2000;44(5-6):229-34. PMID 11146329.
- ^ Huang KC. The Pharmacology of Chinese Herbs. 2nd ed. Boca Raton, FL: CRC Press; 1999. ISBN 0849316650.
- ^ Wakayama EJ, Dillwith JW, Howard RW, Blomquist GJ (1984). "Vitamin B-12 levels in selected insects". Insect Biochemistry. 14: 175–179.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Andrès E, Noel E, Goichot B (2002). "Metformin-associated vitamin B12 deficiency". Arch Intern Med. 162 (19): 2251–2. PMID 12390080.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Gilligan M (2002). "Metformin and vitamin B12 deficiency". Arch Intern Med. 162 (4): 484–5. PMID 11863489.
- ^ Bauman WA, Shaw S, Jayatilleke E, Spungen AM, Herbert V. Increased intake of calcium reverses vitamin B12 malabsorption induced by metformin. Diabetes Care. 2000 Sep;23(9):1227-31. PMID 10977010.
- ^ Samantha Copp (2005-12-01). "What effect does metformin have on vitamin B12 levels?". UK Medicines Information, NHS. - Full report (DOC)
External links
- [http://www.vitab12.com
- Jane Higdon, "Vitamin B12", Micronutrient Information Center, Linus Pauling Institute, Oregon State University
- NIH fact sheet
- Vitamin B12. Medline Plus (National Library of Medicine). Part of it was used for this article (US Government public domain), specially for drug and other interactions.
- Vitamin B12 deficiency article in American Family Physician journal
- Vitamin B12: Vital Nutrient for Good Health at the Weston A. Price Foundation
- Cyanocobalamin at the U.S. National Library of Medicine Medical Subject Headings (MeSH)
