Wart
| Wart | |
|---|---|
| Other names | Verrucae,[1] papillomas[2] |
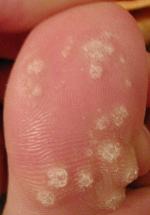 | |
| A large number of warts on the big toe | |
| Specialty | Dermatology |
| Symptoms | skin growth usually occurring on the hands, feet, or genitals[1][3] |
| Duration | Months to years[1] |
| Causes | Human papillomavirus[1] |
| Risk factors | Public showers and pools, eczema[3] |
| Differential diagnosis | Callus, seborrheic keratosis, squamous cell carcinoma[4] |
| Prevention | Avoiding skin contact with infected individual, not walking barefoot in public areas, having safe sex or sexual abstinence |
| Treatment | Salicylic acid, cryotherapy,[1] surgical removal |
| Frequency | Very common[2] |
Warts are non-cancerous viral growths usually occurring on the hands and feet but which can also affect other locations, such as the genitals or face.[1][3] One or many warts may appear.[3] They are distinguished from cancerous tumors as they are caused by a viral infection, such as a human papillomavirus, rather than a cancer growth.[3]
Factors that increase the risk include the use of public showers and pools, working with meat, eczema, and a weak immune system.[1][3] The virus is believed to infect the host through the entrance of a skin wound.[1] A number of types exist, including plantar warts, "filiform warts", and genital warts.[3] Genital warts are often sexually transmitted.[5]
Without treatment, most types of warts resolve in months to years.[1] A number of treatments may speed resolution, including salicylic acid applied to the skin and cryotherapy.[1] In those who are otherwise healthy, they do not typically result in significant problems.[1] Treatment of genital warts differs from that of other types.[3] Infection of a virus, such as HIV, can cause warts. This is prevented through careful handling of needles or sharp objects that could infect the individual through physical trauma of the skin, plus the practice of safe sex, and sexual abstinence. Viruses that are not sexually transmitted, or are not transmitted in the case of a wart, can be prevented through a number of behaviors, such as wearing shoes outdoors and avoiding unsanitized areas without proper shoes or clothing, such as public restrooms or locker rooms.
Warts are very common, with most people being infected at some point in their lives.[2] The estimated current rate of non-genital warts among the general population is 1–13%.[1] They are more common among young people.[1] Prior to widespread adoption of the HPV vaccine, the estimated rate of genital warts in sexually active women was 12%.[5] Warts have been described as far back as 400 BC by Hippocrates.[4]
Types
[edit]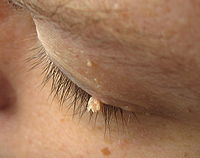
A range of types of wart have been identified, varying in shape and site affected, as well as the type of human papillomavirus involved.[6][7] These include:
- Common wart (verruca vulgaris),[8] a raised wart with a roughened surface, most common on hands, but can grow anywhere on the body. Sometimes known as a Palmer wart or Junior wart.
- Flat wart (verruca plana), a small, smooth flattened wart, flesh-coloured, which can occur in large numbers; most common on the face, neck, hands, wrists, and knees.
- Filiform or digitate wart, a thread- or finger-like wart, most common on the face, especially near the eyelids and lips.
- Genital wart (venereal wart, condyloma acuminatum, verruca acuminata), a wart that occurs on the genitalia.
- Periungual wart, a cauliflower-like cluster of warts that occurs around the nails.
- Plantar wart (verruca, verruca plantaris), a hard, sometimes painful lump, often with multiple black specks in the center; usually only found on pressure points on the soles of the feet.
- Mosaic wart, a group of tightly clustered plantar-type warts, commonly on the hands or soles of the feet.
Cause
[edit]Warts are caused by the human papillomavirus (HPV). There are about 130 known types of human papillomaviruses.[9] HPV infects the squamous epithelium, usually of the skin or genitals, but each HPV type is typically only able to infect a few specific areas of the body. Many HPV types can produce a benign growth, often called a "wart" or "papilloma", in the area they infect.[10] Many of the more common HPV and wart types are listed below.
- Common warts – HPV types 2 and 4 (most common); also types 1, 3, 26, 29, and 57 and others.
- Cancers and genital dysplasia – "high-risk" HPV types are associated with cancers, notably cervical cancer, and can also cause some vulvar, vaginal,[11] penile, anal[12] and some oropharyngeal cancers. "Low-risk" types are associated with warts or other conditions.[13][14]
- High-risk: 16, 18 (cause the most cervical cancer); also 31, 33, 35, 39, 45, 52, 58, 59, and others.
- Plantar warts (verruca) – HPV type 1 (most common); also types 2, 3, 4, 27, 28, and 58[citation needed] and others.
- Anogenital warts (condylomata acuminata or venereal warts) – HPV types 6 and 11 (most common); also types 42, 44 and others.[15]
- Low-risk: 6, 11 (most common); also 13, 44, 40, 43, 42, 54, 61, 72, 81, 89, and others.
- Verruca plana (flat warts) – HPV types 3, 10, and 28.
- Butcher's warts – HPV type 7.
- Heck's disease (focal epithelial hyperplasia) – HPV types 13 and 32.
Pathophysiology
[edit]Common warts have a characteristic appearance under the microscope. They have thickening of the stratum corneum (hyperkeratosis), thickening of the stratum spinosum (acanthosis), thickening of the stratum granulosum, rete ridge elongation, and large blood vessels at the dermoepidermal junction.[citation needed]
Diagnosis
[edit]
On dermatoscopic examination, warts will commonly have fingerlike or knoblike extensions.[16]
Prevention
[edit]Gardasil 6 is an HPV vaccine aimed at preventing cervical cancers and genital warts. Gardasil is designed to prevent infection with HPV types 16, 18, 6, and 11. HPV types 16 and 18 currently cause about 70% of cervical cancer cases,[13][14] and also cause some vulvar, vaginal,[11] penile and anal cancers.[12] HPV types 6 and 11 are responsible for 90% of documented cases of genital warts.[17]
Gardasil 9 protects against HPV types 6, 11, 16, 18, 31, 33, 45, 52, and 58.[18]
HPV vaccines do not currently protect against the virus strains responsible for plantar warts (verrucae).[19]
Disinfection
[edit]The virus is relatively hardy and immune to many common disinfectants. Exposure to 90% ethanol for at least 1 minute, 2% glutaraldehyde,[citation needed] 30% Savlon, and/or 1% sodium hypochlorite can disinfect the pathogen.[20]
The virus is resistant to drying and heat, but killed by 100 °C (212 °F) temperature and ultraviolet radiation.[20]
Treatment
[edit]There are many treatments and procedures associated with wart removal.[21] A review of various skin wart treatments concluded that topical treatments containing salicylic acid were more effective than placebo.[22] Cryotherapy appears to be as effective as salicylic acid, but there have been fewer trials.[22]
Medication
[edit]- Salicylic acid can be prescribed by a dermatologist in a higher concentration than that found in over-the-counter products. Several over-the-counter products are readily available at pharmacies and supermarkets of roughly two types: adhesive pads treated with salicylic acid, and bottled concentrated salicylic acid and lactic acid solution.
- Fluorouracil — Fluorouracil cream, a chemotherapy agent sometimes used to treat skin cancer, can be used on particularly resistant warts, by blocking viral DNA and RNA production and repair.[23]
- Imiquimod is a topical cream that helps the body's immune system fight the wart virus by encouraging interferon production. It has been approved by the U.S. Food and Drug Administration (FDA) for genital warts.[24]
- Cantharidin, found naturally in the bodies of many members of the beetle family Meloidae, causes dermal blistering. It is used either by itself or compounded with podophyllin. Not FDA approved, but available through Canada or select US compounding pharmacies.
- Bleomycin — A more potent chemotherapy drug, can be injected into deep warts, destroying the viral DNA or RNA. Bleomycin is notably not US FDA approved for this purpose. Possible side effects include necrosis of the digits, nail loss and Raynaud syndrome. The usual treatment is one or two injections.[25][26]
- Dinitrochlorobenzene (DNCB), like salicylic acid, is applied directly to the wart. Studies show this method is effective with a cure rate of 80%.[medical citation needed] But DNCB must be used much more cautiously than salicylic acid; the chemical is known to cause genetic mutations, so it must be administered by a physician. This drug induces an allergic immune response, resulting in inflammation that wards off the wart-causing virus.[27]
- Cidofovir is an antiviral drug which is injected into HPV lesions within the larynx (laryngeal papillomatosis) as an experimental treatment.[28]
- Verrutop verruca treatment is a topical solution made from a combination of organic acids, inorganic acids, and metal ions. This solution causes the production of nitrites, which act to denature viral proteins and mummify the wart tissue. The difference between Verrutop and other acid treatments is that it does not damage the surrounding skin.
- Another product available over-the-counter that can aid in wart removal is silver nitrate in the form of a caustic pencil, which is also available at drug stores. In a placebo-controlled study of 70 patients, silver nitrate given over nine days resulted in clearance of all warts in 43% and improvement in warts in 26% one month after treatment compared to 11% and 14%, respectively, in the placebo group.[29] The instructions must be followed to minimize staining of skin and clothing. Occasionally, pigmented scars may develop.
- Trichloroacetic acid can be used to treat warts if salicylic acid or cryotherapy fail or are not available. It requires repeat treatments every week or so. Side effects are burning and stinging.[30]
-
Two viral warts on a middle finger, being treated with a mixture of acids (like salicylic acid) to remove them. A white precipitate forms on the area where the product was applied.
-
Throat warts before and after carbon dioxide laser treatment.
Procedures
[edit]
- Keratolysis, of dead surface skin cells usually using salicylic acid, blistering agents, immune system modifiers ("immunomodulators"), or formaldehyde, often with mechanical paring of the wart with a pumice stone, blade etc.[31]
- Electrodesiccation[32]
- Microwave Treatment[33][34][35][36][37][38]
- Cryosurgery or cryotherapy, which involves freezing the wart (generally with liquid nitrogen),[39] creating a blister between the wart and epidermal layer after which the wart and the surrounding dead skin fall off. An average of three to four treatments are required for warts on thin skin. Warts on calloused skin like plantar warts might take dozens or more treatments.[40]
- Surgical curettage of the wart
- Laser treatment – often with a pulse dye laser or carbon dioxide (CO2) laser. Pulse dye lasers (wavelength 582 nm) work by selective absorption by blood cells (specifically hemoglobin). CO2 lasers work by selective absorption by water molecules. Pulse dye lasers are less destructive and more likely to heal without scarring. CO2 laser works by vaporizing and destroying tissue and skin. Laser treatments can be painful, expensive (though covered by many insurance plans), and not extensively scarring when used appropriately. CO2 lasers will require local anaesthetic. Pulse dye laser treatment does not need conscious sedation or local anesthetic. It takes 2 to 4 treatments but can be many more for extreme cases. Typically, 10–14 days are required between treatments. Preventive measures are important.[40]
- Infrared coagulator – an intense source of infrared light in a small beam like a laser. This works essentially on the same principle as laser treatment. It is less expensive. Like the laser, it can cause blistering, pain and scarring.[41]
- Intralesional immunotherapy with purified candida, MMR, and tuberculin (PPD) protein appears safe and effective.[42][43]
- Duct tape occlusion therapy involves placing a piece of duct tape over the wart. The mechanism of action of this technique still remains unknown. Despite several trials, evidence for the efficacy of duct tape therapy is inconclusive.[44][45] Despite the mixed evidence for efficacy, the simplicity of the method and its limited side-effects leads some researchers to be reluctant to dismiss it.[46]
- No intervention. Spontaneous resolution within a few years can be recommended.[47]

Alternative medicine
[edit]
Daily application of the latex of Chelidonium majus is a traditional treatment.[48]
The acrid yellow sap of Greater Celandine is used as a traditional wart remedy.[49]
According to English folk belief, touching toads causes warts; according to a German belief, touching a toad under a full moon cures warts.[50] The most common Northern Hemisphere toads have glands that protrude from their skin that superficially resemble warts. Warts are caused by a virus, and toads do not harbor it.[51] A variety of traditional folk remedies and rituals claim to be able to remove warts.
In The Adventures of Tom Sawyer, Mark Twain has his characters discuss a variety of such remedies. Tom Sawyer proposes "spunk-water" (or "stump-water", the water collecting in the hollow of a tree stump) as a remedy for warts on the hand. You put your hand into the water at midnight and say:
Barley-corn, barley-corn, injun-meal shorts,
Spunk-water, spunk-water, swaller these warts
You then "walk away quick, eleven steps, with your eyes shut, and then turn around three times and walk home without speaking to anybody. Because if you speak the charm's busted." This is given as an example of Huckleberry Finn's planned remedy, which involves throwing a dead cat into a graveyard as a devil or devils comes to collect a recently buried wicked person. Another remedy involved splitting a bean, drawing blood from the wart and putting it on one of the halves, and burying that half at a crossroads at midnight. The theory of operation is that the blood on the buried bean will draw away the wart.[52] Twain is recognized as an early collector and recorder of genuine American folklore.[53]
Similar practices are recorded elsewhere. In Louisiana, one remedy for warts involves rubbing the wart with a potato, which is then buried; when the "buried potato dries up, the wart will be cured".[54] Another remedy similar to Twain's is reported from Northern Ireland, where water from a specific well on Rathlin Island is credited with the power to cure warts.[55]
History
[edit]
Surviving ancient medical texts show that warts were a documented disease since at least the time of Hippocrates, who lived c. 460 – c. 370 BC. In the book De Medecia by the Roman physician Aulus Cornelius Celsus, who lived c. 25 BC – c. 50 AD, different types of warts were described. Celsus described Myrmecia, today recognized as plantar wart, and categorized acrochordon (a skin tag) as a wart. In the 13th century, warts were described in books published by the surgeons William of Saliceto and Lanfranc of Milan. The word verruca to describe a wart was introduced by the physician Daniel Sennert, who described warts in his 1636 book Hypomnemata physicae.[56]
The cause of warts was initially disputed in the medical profession. In the early 18th century the physician Daniel Turner, who published the first book on dermatology, suggested that warts were caused by damaged nerves close to the skin. In the mid-18th century, the surgeon John Hunter popularized the belief that warts were caused by a bacterial syphilis infection. The surgeon Benjamin Bell documented that warts were caused by a disease entirely unrelated to syphilis, and established a causal link between warts and cancer. In the 19th century, the chief physician of Verona Hospital established a link between warts and cervical cancer. But in 1874 it was noted by the dermatologist Ferdinand Ritter von Hebra that while various theories were advanced by the medical profession, the "influences causing warts are still very obscure".[56]
In 1907 the physician Giuseppe Ciuffo was the first to demonstrate that warts were caused by a virus infection. In 1976 the virologist Harald zur Hausen was the first to discover that warts were caused by the human papillomavirus (HPV). His continuous research established the evidence necessary to develop a HPV vaccine, which first became available in 2006.[56]
Other animals
[edit]References
[edit]- ^ a b c d e f g h i j k l m Loo SK, Tang WY (12 June 2014). "Warts (non-genital)". BMJ Clinical Evidence. 2014. PMC 4054795. PMID 24921240.
- ^ a b c "Papillomas (Warts) – National Library of Medicine". PubMed Health. Archived from the original on 10 September 2017. Retrieved 6 November 2016.
- ^ a b c d e f g h "Warts: Overview". U.S. National Library of Medicine. 30 July 2014. Archived from the original on 10 September 2017.
- ^ a b Bope ET, Kellerman RD (2012). Conn's Current Therapy 2012. Elsevier Health Sciences. p. 275. ISBN 978-1-4557-3305-7. Archived from the original on 7 November 2016.
- ^ a b W Buck H (13 August 2010). "Warts (genital)". BMJ Clinical Evidence. 2010. PMC 3217761. PMID 21418685.
- ^ Anderson, Keith, Keith, Jeff, Novak, Patricia D., Elliot, Michelle A. (2005). Mosby's Medical, Nursing & Allied Health Dictionary (5th ed.). C.V. Mosby. ISBN 978-0-323-03736-5. Archived from the original on 7 January 2017.
- ^ "MedlinePlus: Warts". 2010. Archived from the original on 16 May 2013.
- ^ Adigun CG. "Verruca Vulgaris". Merck Manual. Retrieved 16 December 2022.
- ^ De Villiers EM, Fauquet C, Broker TR, Bernard HU, Zur Hausen H (June 2004). "Classification of papillomaviruses". Virology. 324 (1): 17–27. doi:10.1016/j.virol.2004.03.033. PMID 15183049.
- ^ Syrjänen S (1 August 2003). "Human papillomavirus infections and oral tumors". Medical Microbiology and Immunology. 192 (3): 123–128. doi:10.1007/s00430-002-0173-7. ISSN 1432-1831. PMID 12920585. S2CID 2768273.
- ^ a b "FDA Approves Expanded Uses for Gardasil to Include Preventing Certain Vulvar and Vaginal Cancers". FDA. 12 September 2008. Archived from the original on 6 March 2010.
- ^ a b Cortez, Michelle Fay, Pettypiece, Shannon (13 November 2008). "Merck Cancer Shot Cuts Genital Warts, Lesions in Men". Bloomberg News. Retrieved 17 May 2013.
- ^ a b Lowy DR, Schiller JT (2006). "Prophylactic human papillomavirus vaccines". J. Clin. Invest. 116 (5): 1167–73. doi:10.1172/JCI28607. PMC 1451224. PMID 16670757.
- ^ a b Muñoz N, Bosch FX, Castellsagué X, Díaz M, de Sanjose S, Hammouda D, Shah KV, Meijer CJ (20 August 2004). "Against which human papillomavirus types shall we vaccinate and screen? The international perspective". Int J Cancer. 111 (2): 278–85. doi:10.1002/ijc.20244. PMID 15197783. S2CID 20679802.
- ^ Kumar, Vinay, Abbas, Abul K., Fausto, Nelson, Mitchell, Richard (2007). "Chapter 19 The Female Genital System and Breast". Robbins Basic Pathology (8 ed.). Philadelphia: Saunders. ISBN 978-1-4160-2973-1.
- ^ Dong H (2011). "Dermatoscopy of genital warts". Journal of the American Academy of Dermatology. 64 (5): 859–864. doi:10.1016/j.jaad.2010.03.028. PMID 21429619. S2CID 33381261 – via Elsevier Science Direct.
- ^ Steinbrook R (2006). "The Potential of Human Papillomavirus Vaccines". New England Journal of Medicine. 354 (11): 1109–12. doi:10.1056/NEJMp058305. PMID 16540608.
- ^ "Prescribing information Gardasil 9" (PDF). Food and Drug Administration. 2015. Archived (PDF) from the original on 10 October 2016.
- ^ Bossart S, Imstepf V, Hunger RE, Seyed Jafari SM (2020). "Nonavalent Human Papillomavirus Vaccination as a Treatment for Skin Warts in Immunosuppressed Adults: A Case Series". Acta Dermato Venereologica. 100 (6): adv00078-2. doi:10.2340/00015555-3437. PMC 9128913. PMID 32115668.
- ^ a b Human Papillomavirus Archived 23 August 2015 at the Wayback Machine. Public Health Agency of Canada
- ^ Lipke MM (2006). "An armamentarium of wart treatments". Clin Med Res. 4 (4): 273–93. doi:10.3121/cmr.4.4.273. PMC 1764803. PMID 17210977.
- ^ a b Kwok CS, Gibbs S, Bennett C, Holland R, Abbott R (12 September 2012). Gibbs S (ed.). "Topical treatments for cutaneous warts". The Cochrane Database of Systematic Reviews. 9 (9): CD001781. doi:10.1002/14651858.CD001781.pub3. PMC 8101088. PMID 22972052. Archived from the original on 4 July 2013.
- ^ Salk RS, Grogan KA, Chang TJ (May 2006). "Topical 5% 5-fluorouracil cream in the treatment of plantar warts: a prospective, randomized, and controlled clinical study". Journal of Drugs in Dermatology. 5 (5): 418–24. PMID 16703777.
- ^ Barclay L (4 June 2011). "Short-Acting Imiquimod Cream Approved for Genital Warts". Medscape. Archived from the original on 18 August 2011. Retrieved 10 August 2011.
- ^ Soni P, Khandelwal K, Aara N, Ghiya BC, Mehta RD, Bumb RA (2011). "Efficacy of Intralesional Bleomycin in Palmo-plantar and Periungual Warts". Journal of Cutaneous and Aesthetic Surgery. 4 (3): 188–191. doi:10.4103/0974-2077.91250. PMC 3263129. PMID 22279384.
- ^ Champion, R. H., et al. (1998). Rook's Textbook of Dermatology. Blackwell Science, p. 1044, ISBN 0-632-06429-3
- ^ "Treating Warts". British Medical Journal. 31 August 2002. Archived from the original on 3 November 2010. Retrieved 17 May 2013.
- ^ Soma MA, Albert DM (2008). "Cidofovir: to use or not to use?". Current Opinion in Otolaryngology & Head and Neck Surgery. 16 (1): 86–90. doi:10.1097/MOO.0b013e3282f43408. PMID 18197029. S2CID 22895067.
- ^ Sterling JC, Handfield-Jones S, Hudson PM (2001). "Guidelines for the management of cutaneous warts" (PDF). British Journal of Dermatology. 144 (1): 4–11. doi:10.1046/j.1365-2133.2001.04066.x. PMID 11167676. S2CID 20179474. Archived from the original (PDF) on 3 March 2012.
- ^ "Common warts - Diagnosis and treatment - Mayo Clinic". www.mayoclinic.org. Retrieved 6 November 2022.
- ^ Warts Archived 17 May 2008 at the Wayback Machine at About.com
- ^ Stone KM, Becker TM, Hadgu A, Kraus SJ (1990). "Treatment of external genital warts: A randomized clinical trial comparing podophyllin, cryotherapy, and electrodesiccation". Genitourinary Medicine. 66 (1): 16–19. doi:10.1136/sti.66.1.16. PMC 1194434. PMID 2179111.
- ^ Solomon K, Yip V (December 2023). "The novel treatment of children with viral warts using microwave technology". Skin Health and Disease. 3 (6): e291. doi:10.1002/ski2.291. ISSN 2690-442X. PMC 10690651. PMID 38047251.
- ^ Hagon W, Hagon J, Noble G, Brenton-Rule A, Stewart S, Bristow I (January 2023). "Microwave therapy for the treatment of plantar warts". Journal of Foot and Ankle Research. 16 (1): 37. doi:10.1186/s13047-023-00638-8. ISSN 1757-1146. PMC 10268531. PMID 37322512.
- ^ Bristow IR, Webb C, Ardern-Jones MR (27 July 2017). "The Successful Use of a Novel Microwave Device in the Treatment of a Plantar Wart". Case Reports in Dermatology. 9 (2): 102–107. doi:10.1159/000477377. ISSN 1662-6567. PMC 5624246. PMID 29033812.
- ^ Gupta AK, Wang T, Cooper EA, Conenello RM, Bristow IR (October 2023). "The treatment of plantar warts using microwave—A review of 85 consecutive cases in the United States". Journal of Cosmetic Dermatology. 22 (10): 2729–2736. doi:10.1111/jocd.15802. ISSN 1473-2130. PMID 37340590.
- ^ Dhinsa A, Philip G, Daknish F, Amin S, Vlahovic T (September 2023). "42057 Microwave Therapy for Plantar Warts: A Chart Review". Journal of the American Academy of Dermatology. 89 (3): AB64. doi:10.1016/j.jaad.2023.07.259. ISSN 0190-9622.
- ^ "The Royal College of Podiatry". College of Podiatry. Retrieved 22 March 2024.
- ^ "Cryotherapy for Warts". WebMD. Archived from the original on 9 July 2016.
- ^ a b Bacelieri R, Johnson SM (2005). "Cutaneous warts: An evidence-based approach to therapy". American Family Physician. 72 (4): 647–52. PMID 16127954. Archived from the original on 21 April 2014.
- ^ Halasz CL (1994). "Treatment of common warts using the infrared coagulator". The Journal of Dermatologic Surgery and Oncology. 20 (4): 252–56. doi:10.1111/j.1524-4725.1994.tb01620.x. PMID 8163746.
- ^ Aldahan AS, Mlacker S, Shah VV, Kamath P, Alsaidan M, Samarkandy S, Nouri K (May 2016). "Efficacy of intralesional immunotherapy for the treatment of warts: A review of the literature". Dermatologic Therapy. 29 (3): 197–207. doi:10.1111/dth.12352. PMID 26991521. S2CID 40536366.
- ^ Salman S (2019). "Intralesional Immunotherapy for the Treatment of Warts: A Network Meta-analysis". Journal of the American Academy of Dermatology. 80 (4): 922–930.e4. doi:10.1016/j.jaad.2018.07.003. PMID 30003983. S2CID 51617793 – via Elsevier Science Direct.
- ^ Loo SK, Tang WY (12 June 2014). "Warts (non-genital)". BMJ Clinical Evidence. 2014. PMC 4054795. PMID 24921240.
- ^ Kwok CS, Gibbs S, Bennett C, Holland R, Abbott R (12 September 2012). "Topical treatments for cutaneous warts". Cochrane Database Syst Rev. 9 (9): CD001781. doi:10.1002/14651858.CD001781.pub3. PMC 8101088. PMID 22972052.
- ^ Stubbings A, Wacogne I (September 2011). "Question 3. What is the efficacy of duct tape as a treatment for verruca vulgaris?". Archives of Disease in Childhood. 96 (9): 897–99. doi:10.1136/archdischild-2011-300533. PMID 21836182. S2CID 206853952.
- ^ Goldman RD (May 2019). "Duct tape for warts in children: Should nature take its course?". Canadian Family Physician. 65 (5): 337–338. ISSN 1715-5258. PMC 6516695. PMID 31088871.
- ^ Gilca, Marilena, et al. Chelidonium majus–an integrative review: traditional knowledge versus modern findings Archived 5 December 2020 at the Wayback Machine Forschende Komplementärmedizin/Research in Complementary Medicine2010; 17(5): 241–248.
- ^ Greater Celandine For Warts Archived 17 July 2014 at the Wayback Machine. botanical-online.com
- ^ Ley W (December 1963). "The Names of the Constellations". For Your Information. Galaxy Science Fiction. pp. 90–99.
- ^ Clark, Josh (2 March 2009). "Do toads cause warts?". science.howstuffworks.com. p. 2. Archived from the original on 16 October 2012. Retrieved 20 October 2012.
- ^ Mark Twain, The Adventures of Tom Sawyer, ch. 6
- ^ LeMaster, J. R. (1993) The Mark Twain Encyclopedia (Taylor and Francis, pp. 293–94 Archived 7 January 2017 at the Wayback Machine, ISBN 0-8240-7212-X.
- ^ Webb, Julie Yvonne (1971). "Louisiana Voodoo and Superstitions Relating to Health". HSMHA Health Reports. 86 (4): 291, 296–97. doi:10.2307/4594154. JSTOR 4594154. PMC 1937133. PMID 4324337.
- ^ Ballard LM (2009). "An approach to traditional cures in Ulster". The Ulster Medical Journal. 78 (1): 26–33. PMC 2629017. PMID 19252727.
- ^ a b c Karamanou M, Agapitos E, Kousoulis A, Androutsos G (17 August 2010). "From the humble wart to HPV: a fascinating story throughout centuries". Oncology Reviews. 4 (3): 133–135. doi:10.1007/s12156-010-0060-1. S2CID 72238300.
External links
[edit]- Wart photo library. Archived 12 October 2007 at the Wayback Machine. Dermnet.com.


