Health economics
This article may need to be rewritten to comply with Wikipedia's quality standards. (May 2009) |
| Part of a series on |
| Economics |
|---|
 |
Health economics is a branch of economics concerned with issues related to efficiency, effectiveness, value and behavior in the production and consumption of health and healthcare. In broad terms, health economists study the functioning of healthcare systems and health-affecting behaviors such as smoking.
A seminal 1963 article by Kenneth Arrow, often credited with giving rise to health economics as a discipline, drew conceptual distinctions between health and other goods.[1] Factors that distinguish health economics from other areas include extensive government intervention, intractable uncertainty in several dimensions, asymmetric information, barriers to entry, externalities and the presence of a third-party agent.[2] In healthcare, the third-party agent is the physician, who makes purchasing decisions (e.g., whether to order a lab test, prescribe a medication, perform a surgery, etc.) while being insulated from the price of the product or service.
Health economists evaluate multiple types of financial information: costs, charges and expenditures.
Uncertainty is intrinsic to health, both in patient outcomes and financial concerns. The knowledge gap that exists between a physician and a patient creates a situation of distinct advantage for the physician, which is called asymmetric information.
Externalities arise frequently when considering health and health care, notably in the context of infectious disease. For example, making an effort to avoid catching the common cold affects people other than the decision maker.[3][4][5][6]
Scope
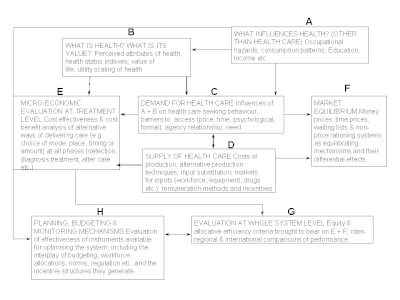
The scope of health economics is neatly encapsulated by Alan Williams' "plumbing diagram"[7] dividing the discipline into eight distinct topics:
- What influences health? (other than healthcare)
- What is health and what is its value?
- The demand for healthcare
- The supply of healthcare
- Micro-economic evaluation at treatment level
- Market equilibrium
- Evaluation at whole system level
- Planning, budgeting and monitoring mechanisms.
Healthcare demand
The demand for healthcare is a derived demand from the demand for health. Healthcare is demanded as a means for consumers to achieve a larger stock of "health capital." The demand for health is unlike most other goods because individuals allocate resources in order to both consume and produce health.
The above description gives three roles of persons in health economics. The World Health Report (p. 52) states that people take four roles in the healthcare:
- Contributors
- Citizens
- Provider
- Consumers
Michael Grossman's 1972 model of health production[8] has been extremely influential in this field of study and has several unique elements that make it notable. Grossman's model views each individual as both a producer and a consumer of health. Health is treated as a stock which degrades over time in the absence of "investments" in health, so that health is viewed as a sort of capital. The model acknowledges that health is both a consumption good that yields direct satisfaction and utility, and an investment good, which yields satisfaction to consumers indirectly through increased productivity, fewer sick days, and higher wages. Investment in health is costly as consumers must trade off time and resources devoted to health, such as exercising at a local gym, against other goals. These factors are used to determine the optimal level of health that an individual will demand. The model makes predictions over the effects of changes in prices of healthcare and other goods, labour market outcomes such as employment and wages, and technological changes. These predictions and other predictions from models extending Grossman's 1972 paper form the basis of much of the econometric research conducted by health economists.
In Grossman's model, the optimal level of investment in health occurs where the marginal cost of health capital is equal to the marginal benefit. With the passing of time, health depreciates at some rate δ. The interest rate faced by the consumer is denoted by r. The marginal cost of health capital can be found by adding these variables: . The marginal benefit of health capital is the rate of return from this capital in both market and non-market sectors. In this model, the optimal health stock can be impacted by factors like age, wages and education. As an example, increases with age, so it becomes more and more costly to attain the same level of health capital or health stock as one ages. Age also decreases the marginal benefit of health stock. The optimal health stock will therefore decrease as one ages.
Beyond issues of the fundamental, "real" demand for medical care derived from the desire to have good health (and thus influenced by the production function for health) is the important distinction between the "marginal benefit" of medical care (which is always associated with this "real demand" curve based on derived demand), and a separate "effective demand" curve, which summarizes the amount of medical care demanded at particular market prices. Because most medical care is not purchased from providers directly, but is rather obtained at subsidized prices due to insurance, the out-of-pocket prices faced by consumers are typically much lower than the market price. The consumer sets MB=MC out of pocket, and so the "effective demand" will have a separate relationship between price and quantity than will the "marginal benefit curve" or real demand relationship. This distinction is often described under the rubric of "ex-post moral hazard" (which is again distinct from ex-ante moral hazard, which is found in any type of market with insurance).
Economic evaluation in Germany and in the United Kingdom
A large focus of health economics, is the microeconomic evaluation of the value of individual treatments. The states in Europe appraise certain new and existing pharmaceuticals and devices using economic evaluations by health technology assessments by different national institutions. In Europe's largest health market Germany the Institute for Quality and Economy in Health Services (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen — IQWiG) is responsible,[9] while it is the National Institute for Health and Care Excellence NICE in the United Kingdom.
Economic evaluation is the comparison of two or more alternative courses of action in terms of both their costs and consequences (Drummond et al.). Economists usually distinguish several types of economic evaluation, differing in how consequences are measured:
- Cost-minimization analysis
- Cost–benefit analysis
- Cost-effectiveness analysis
- Cost–utility analysis
- Cost consequence analysis
In cost minimization analysis (CMA), the effectiveness of the comparators in question must be proven to be equivalent. The 'cost-effective' comparator is simply the one which costs less (as it achieves the same outcome). In cost–benefit analysis (CBA), costs and benefits are both valued in cash terms. Cost effectiveness analysis (CEA) measures outcomes in 'natural units', such as mmHg, symptom free days, life years gained. Finally cost–utility analysis (CUA) measures outcomes in a composite metric of both length and quality of life, the Quality-adjusted life year (QALY). (Note there is some international variation in the precise definitions of each type of analysis).
A final approach which is sometimes classed an economic evaluation is a cost of illness study. This is not a true economic evaluation as it does not compare the costs and outcomes of alternative courses of action. Instead, it attempts to measure all the costs associated with a particular disease or condition. These will include direct costs (where money actually changes hands, e.g. health service use, patient co-payments and out of pocket expenses), indirect costs (the value of lost productivity from time off work due to illness), and intangible costs (the 'disvalue' to an individual of pain and suffering). (Note specific definitions in health economics may vary slightly from other branches of economics.)
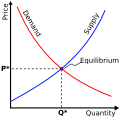
Market equilibrium
Healthcare markets
The five health markets typically analyzed are:
- Healthcare financing market
- Physician and nurses services market
- Institutional services market
- Input factors markets
- Professional education market
Although assumptions of textbook models of economic markets apply reasonably well to healthcare markets, there are important deviations. Many states have created risk pools in which relatively healthy enrollees subsidise the care of the rest. Insurers must cope with adverse selection which occurs when they are unable to fully predict the medical expenses of enrollees; adverse selection can destroy the risk pool. Features of insurance market risk pools, such as group purchases, preferential selection ("cherry-picking"), and preexisting condition exclusions are meant to cope with adverse selection.
Insured patients are naturally less concerned about healthcare costs than they would if they paid the full price of care. The resulting moral hazard drives up costs, as shown by the famous RAND Health Insurance Experiment. Insurers use several techniques to limit the costs of moral hazard, including imposing copayments on patients and limiting physician incentives to provide costly care. Insurers often compete by their choice of service offerings, cost sharing requirements, and limitations on physicians.
Consumers in healthcare markets often suffer from a lack of adequate information about what services they need to buy and which providers offer the best value proposition. Health economists have documented a problem with supplier induced demand, whereby providers base treatment recommendations on economic, rather than medical criteria. Researchers have also documented substantial "practice variations", whereby the treatment aols on service availability to rein in inducement and practice variations.
The U.S. healthcare market has relied extensively on competition to control costs and improve quality. Critics question whether problems with adverse selection, moral hazard, information asymmetries, demand inducement, and practice variations can be addressed by private markets.[citation needed] Competition has fostered reductions in prices, but consolidation by providers and, to a lesser extent, insurers, has tempered this effect.
Though the market for healthcare in the U.S. is primarily coordinated by competition, there is an abundance of regulations that inhibit market efficiency. A classic example is medical licenses. Some economists argue that requiring doctors to have a medical license constrains inputs, inhibits innovation, and increases cost to consumers while largely only benefiting the doctors themselves.[10]
Competitive equilibrium in the five health markets
While the nature of healthcare as a private good is preserved in the last three markets, market failures occur in the financing and delivery markets due to two reasons: (1) Perfect information about price products is not a viable assumption (2) Various barriers of entry exist in the financing markets (i.e. monopoly formations in the insurance industry)
Ideological bias in the debate about the financing and delivery health markets
The healthcare debate in public policy is often informed by ideology and not sound economic theory. Often, politicians subscribe to a moral order system or belief about the role of governments in public life that guides biases towards provision of health care as well. The ideological spectrum spans: individual savings accounts and catastrophic coverage, tax credit or voucher programs combined with group purchasing arrangements, and expansions of public-sector health insurance. These approaches are advocated by healthcare conservatives, moderates and liberals, respectively.[citation needed]
Other issues
Medical economics
Often used synonymously with health economics, medical economics, according to Culyer,[11] is the branch of economics concerned with the application of economic theory to phenomena and problems associated typically with the second and third health market outlined above. Typically, however, it pertains to cost–benefit analysis of pharmaceutical products and cost-effectiveness of various medical treatments. Medical economics often uses mathematical models to synthesise data from biostatistics and epidemiology for support of medical decision-making, both for individuals and for wider health policy.
Behavioral economics
Peter Orszag has suggested that behavioral economics is an important factor for improving the healthcare system, but that relatively little progress has been made when compared to retirement policy.[12]
Mental health economics
Mental health economics incorporates a vast array of subject matters, ranging from pharmacoeconomics to labor economics and welfare economics. Mental health can be directly related to economics by the potential of affected individuals to contribute as human capital. In 2009 Currie and Stabile published "Mental Health in Childhood and Human Capital" in which they assessed how common childhood mental health problems may alter the human capital accumulation of affected children.[13] Externalities may include the influence that affected individuals have on surrounding human capital, such as at the workplace or in the home.[14] In turn, the economy also affects the individual, particularly in light of globalization. For example, studies in India, where there is an increasingly high occurrence of western outsourcing, have demonstrated a growing hybrid identity in young professionals who face very different sociocultural expectations at the workplace and in at home.[15]
Mental health economics presents a unique set of challenges to researchers. Individuals with cognitive disabilities may not be able to communicate preferences. These factors represent challenges in terms of placing value on the mental health status of an individual, especially in relation to the individual's potential as human capital. Further, employment statistics are often used in mental health economic studies as a means of evaluating individual productivity; however, these statistics do not capture "presenteeism", when an individual is at work with a lowered productivity level, quantify the loss of non-paid working time, or capture externalities such as having an affected family member. Also, considering the variation in global wage rates or in societal values, statistics used may be contextually, geographically confined, and study results may not be internationally applicable.[14]
Though studies have demonstrated mental healthcare to reduce overall healthcare costs, demonstrate efficacy, and reduce employee absenteeism while improving employee functioning, the availability of comprehensive mental health services is in decline. Petrasek and Rapin (2002) cite the three main reasons for this decline as (1) stigma and privacy concerns, (2) the difficulty of quantifying medical savings and (3) physician incentive to medicate without specialist referral.[16] Evers et al. (2009) have suggested that improvements could be made by promoting more active dissemination of mental health economic analysis, building partnerships through policy-makers and researchers, and employing greater use of knowledge brokers.[14]
See also
|
|
References
- ^ Arrow 1963
- ^ Phelps, Charles E. (2003), Health Economics (3rd ed.), Boston: Addison Wesley, ISBN 0-321-06898-X Description and 2nd ed. preview.
- ^ Fuchs, Victor R. (1987). "health economics" The New Palgrave: A Dictionary of Economics, v. 2, pp. 614–19.
- ^ Fuchs, Victor R. (1996). "Economics, Values, and Health Care Reform," American Economic Review, 86(1), pp. 1–24 (press +).
- ^ Fuchs, Victor R. ([1974] 1998). Who Shall Live? Health, Economics, and Social Choice, Expanded edition. Chapter-preview links, pp. vii–xi.
- ^ Wolfe, Barbara (2008). "health economics." The New Palgrave Dictionary of Economics', 2nd Edition. Abstract & TOC.
- ^ Williams, A. (1987), "Health economics: the cheerful face of a dismal science", in Williams, A. (ed.), Health and Economics, London: Macmillan
- ^ Grossman, Michael (1972), "On the Concept of Health Capital and the Demand for Health", Journal of Political Economy, 80 (2): 223–255, doi:10.1086/259880
- ^ Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen → de:IQWiG
- ^ Svorny, Shirley (2004), "Licensing Doctors: Do Economists Agree?", Econ Journal Watch, 1 (2): 279–305
- ^ A.J. Culyer (1989) "A Glossary of the more common terms encountered in health economics" in MS Hersh-Cochran and KP Cochran (Eds.) Compendium of English Language Course Syllabi and Textbooks in Health Economics, Copenhagen, WHO, 215–34
- ^ Peter Orszag, "Behavioral Economics: Lessons from Retirement Research for Health Care and Beyond," Presentation to the Retirement Research Consortium, August 7, 2008
- ^ Currie, Janet and Mark Stabile. "Mental Health in Childhood and Human Capital". The Problems of Disadvantaged Youth: An Economic Perspective ed. J. Gruber. Chicago: University of Chicago Press, 2009.
- ^ a b c Evers, S.; Salvador–Carulla, L.; Halsteinli, V.; McDaid, D.; MHEEN Group (April 2007), "Implementing mental health economic evaluation evidence: Building a Bridge between theory and practice", Journal of Mental Health, 16 (2): 223–241, doi:10.1080/09638230701279881
{{citation}}: CS1 maint: year (link) - ^ Bhavsar, V.; Bhugra, D. (December 2008), "Globalization: Mental health and social economic factors", Global Social Policy, 8 (3): 378–396, doi:10.1177/1468018108095634
- ^ Petrasek M, Rapin L; Rapin (2002), "The mental health paradox", Benefits Q, 18 (2): 73–7, PMID 12004583
Further reading
- Alastair M. Gray, Philip M. Clarke, Jane Wolstenholme, Sarah Wordsworth (2010) Applied Methods of Cost-effectiveness Analysis in Healthcare, Oxford University Press. Preview ISBN 0-19-922728-4
- Arrow, K. (December 1963), "Uncertainty and the welfare economics of medical care" (PDF), American Economic Review, 53 (5): 941–973
{{citation}}: Invalid|ref=harv(help) - Drummond, Michael F. (2005) Methods for the Economic Evaluation of Health Care Programmes, Oxford University Press. Preview. ISBN 0-19-852945-7
- Fuchs, Victor R. (1998) Who Shall Live? Health, Economics, and Social Choice, Wspc.
- Mahar, Maggie, Money-Driven Medicine: The Real Reason Health Care Costs So Much, Harper/Collins, 2006. ISBN 978-0-06-076533-0
- Morrisey, Michael A. (2008), "Health Care", in David R. Henderson (ed.) (ed.), Concise Encyclopedia of Economics (2nd ed.), Indianapolis: Library of Economics and Liberty, ISBN 978-0865976658, OCLC 237794267
{{citation}}:|editor=has generic name (help) - Siegel, Joanna E.; Russell, Louise B.; Weinstein, Milton C.; Gold, Marthe R. (1996), Cost-effectiveness in health and medicine, New York [u.a.]: Oxford Univ. Press, ISBN 978-0-19-510824-8
- Starr, Paul, The Social Transformation of American Medicine, Basic Books, 1982. ISBN 0-465-07934-2
- Wennberg J, Gittelsohn; Gittelsohn, A. (December 1973), "Small area variations in health care delivery", Science, 182 (4117): 1102–8, doi:10.1126/science.182.4117.1102, PMID 4750608
- Whittington, Ruth (2008). Introduction to Health Economics: A Beginners Guide Preview. ISBN 978-0-9545494-5-9.
- Wise, David A. (2009), Developments in the Economics of Aging, University of Chicago Press, ISBN 978-0-226-90335-4
- A.J. Culyer and J.P. Newhouse, ed. (2000). Handbook of Health Economics, Elsevier. 1A. Description. Elsevier.
- _____ (2000). Handbook of Health Economics, 1B. Description. Elsevier.
Journals
- Health Economics. Aims & scope and links back-issue titles and abstracts.
- Journal of Health Economics Aims & scope and links to back-issue titles and abstracts.
- Review of Economics of the Household
External links
This article's use of external links may not follow Wikipedia's policies or guidelines. (November 2012) |
Associations
- International Health Economics Association
- Health Economics education (HEe) – UK-based site for teachers of Health Economics
- International Society for Pharmacoeconomics and Outcomes Research
Links/Terminology/Discussion
- Health Economics Online Glossary of Terms – maintained by the University of Groningen, The Netherlands
- HealthEconomics.Com