Rifapentine
 | |
| Clinical data | |
|---|---|
| Other names | 3{[(4-cyclopentyl-1-piperazinyl)imino]methyl}rifamycin |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a602026 |
| Pregnancy category |
|
| Routes of administration | by mouth |
| ATC code | |
| Pharmacokinetic data | |
| Bioavailability | increases when administered with food |
| Identifiers | |
| |
| CAS Number | |
| PubChem CID | |
| DrugBank | |
| ChemSpider | |
| UNII | |
| KEGG | |
| ChEBI | |
| ChEMBL | |
| NIAID ChemDB | |
| CompTox Dashboard (EPA) | |
| ECHA InfoCard | 100.057.021 |
| Chemical and physical data | |
| Formula | C47H64N4O12 |
| Molar mass | 877.031 g/mol g·mol−1 |
| 3D model (JSmol) | |
| Melting point | 179 to 180 °C (354 to 356 °F) |
| |
| |
| (verify) | |
Rifapentine (RPT), sold under the brand name Priftin, is an antibiotic used in the treatment of tuberculosis.[1] In active tuberculosis it is used together with other antituberculosis medications.[1] In latent tuberculosis it is typically used with isoniazid.[2] It is taken by mouth.[1]
Common side effects include low neutrophil counts in the blood, elevated liver enzymes, and white blood cells in the urine.[1] Serious side effects may include liver problems or Clostridium difficile associated diarrhea.[1] It is unclear if use during pregnancy is safe.[1] Rifapentine is in the rifamycin family of medication and works by blocking DNA-dependent RNA polymerase.[1]
Rifapentine was approved for medical use in the United States in 1998.[1] It is on the World Health Organization's List of Essential Medicines, the most effective and safe medicines needed in a health system.[3] In the United States it costs $100–200 per month.[4] In many areas of the world it is not easy to get as of 2015.[5]
Medical uses
A review of alternative regimens for prevention of active tuberculosis in HIV-negative individuals with latent TB found that a weekly, directly observed regimen of rifapentine with isoniazid for three months was as effective as a daily, self -administered regimen of isoniazid for nine months. But the rifapentine-isoniazid regimen had higher rates of treatment completion and lower rates of hepatotoxicity. However, the rate of treatment-limiting adverse events was higher in the rifapentine-isoniazid regimen. [6]
Pregnancy
Rifapentine has been assigned a Pregnancy Category C by the FDA. Rifapentine in pregnant women has not been studied, but animal reproduction studies have resulted in fetal harm and were teratogenic. If rifapentine and rifampin are used together in pregnancy, coagulation should be monitored due to a possible increased risk of maternal postpartum hemorrhage and infant bleeding.[7]
Adverse effects
Common side effects are hyperuricemia, pyuria, hematuria, urinary tract infection, proteinuria, neutropenia, anemia, and hypoglycemia.[7]
Contraindications
Rifapentine should be avoided in patients with an allergy to the rifamycin class of drugs.[7] This drug class includes rifampicin and rifabutin. [8]
Interactions
Rifapentine induces metabolism by CYP3A4, CYP2C8 and CYP2C9 enzymes. It may be necessary to adjust the dosage of drugs metabolized by these enzymes if they are taken with rifapentine. Examples of drugs that may be affected by rifapentine include warfarin, propranolol, digoxin, protease inhibitors and oral contraceptives.[7]
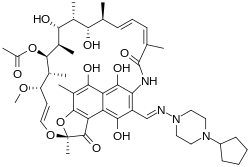
Chemical structure
The chemical structure of rifapentine is similar to that of rifamycin, with the notable substitution of a methyl group for a cyclopentane (C5H9) group.
History
Rifapentine was first synthesized in 1965 by the same company that produced rifampicin. The drug was approved by the Food and Drug Administration (FDA) in June 1998. It is synthesized in one step from rifampicin.
See also
References
- ^ a b c d e f g h "Rifapentine". The American Society of Health-System Pharmacists. Archived from the original on 20 December 2016. Retrieved 8 December 2016.
{{cite web}}: Unknown parameter|deadurl=ignored (|url-status=suggested) (help) - ^ The selection and use of essential medicines: Twentieth report of the WHO Expert Committee 2015 (including 19th WHO Model List of Essential Medicines and 5th WHO Model List of Essential Medicines for Children) (PDF). World Health Organization. 2015. p. 37. ISBN 9789240694941. Archived from the original (PDF) on 20 December 2016. Retrieved 10 December 2016.
{{cite book}}: Unknown parameter|deadurl=ignored (|url-status=suggested) (help) - ^ "WHO Model List of Essential Medicines (19th List)" (PDF). World Health Organization. April 2015. Archived from the original (PDF) on 13 December 2016. Retrieved 8 December 2016.
{{cite web}}: Unknown parameter|deadurl=ignored (|url-status=suggested) (help) - ^ Hamilton, Richart (2015). Tarascon Pocket Pharmacopoeia 2015 Deluxe Lab-Coat Edition. Jones & Bartlett Learning. p. 53. ISBN 9781284057560.
- ^ Nieburg, Phillip; Dubovi, Talia; Angelo, Sahil (2015). Tuberculosis—A Complex Health Threat: A Policy Primer of Global TB Challenges. Rowman & Littlefield. p. 15. ISBN 9781442240957. Archived from the original on 2016-12-20.
{{cite book}}: Unknown parameter|deadurl=ignored (|url-status=suggested) (help) - ^ Sharma SK; et al. (2013). "Rifamycins (rifampicin, rifabutin and rifapentine) compared to isoniazid for preventing tuberculosis in HIV-negative people at risk of active TB". Cochrane Database of Systematic Reviews. 7: CD007545. doi:10.1002/14651858.CD007545.pub2. PMID 23828580.
{{cite journal}}: Explicit use of et al. in:|author=(help) - ^ a b c d Sanofi-Aventis. (2010) Priftin (rifapentine): Highlights of Prescribing Information. Retrieved from "Archived copy" (PDF). Archived from the original (PDF) on 2017-06-23. Retrieved 2017-09-10.
{{cite web}}: Unknown parameter|deadurl=ignored (|url-status=suggested) (help)CS1 maint: archived copy as title (link). - ^ CDC. (2013) Core Curriculum on Tuberculosis: What the Clinician Should Know. Retrieved from "Archived copy". Archived from the original on 2017-07-11. Retrieved 2017-09-10.
{{cite web}}: Unknown parameter|deadurl=ignored (|url-status=suggested) (help)CS1 maint: archived copy as title (link).
