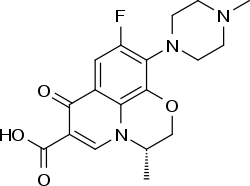
Levofloxacin
 | |
 | |
| Clinical data | |
|---|---|
| Trade names | Levaquin, Tavanic, Iquix, others |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a697040 |
| License data |
|
| Routes of administration | By mouth, IV, eye drops |
| ATC code | |
| Legal status | |
| Legal status | |
| Pharmacokinetic data | |
| Bioavailability | 99% |
| Protein binding | 24 to 38% |
| Metabolism | <5% desmethyl and N-oxide metabolites |
| Elimination half-life | 6 to 8 hours |
| Excretion | Urinary, mainly unchanged |
| Identifiers | |
| |
| CAS Number | |
| PubChem CID | |
| DrugBank | |
| ChemSpider | |
| UNII | |
| KEGG | |
| ChEMBL | |
| NIAID ChemDB | |
| CompTox Dashboard (EPA) | |
| ECHA InfoCard | 100.115.581 |
| Chemical and physical data | |
| Formula | C18H20FN3O4 |
| Molar mass | 361.368 g/mol g·mol−1 |
| 3D model (JSmol) | |
| |
| |
| | |
Levofloxacin, sold under the trade names Levaquin and Tavanic, among others is an antibiotic.[2] It is used to treat a number of bacterial infections including acute bacterial sinusitis, pneumonia, urinary tract infections, chronic prostatitis, and some types of gastroenteritis. Along with other antibiotics it may be used to treat tuberculosis, meningitis, or pelvic inflammatory disease. It is available by mouth or intravenously.[2]
Common side effects include nausea, diarrhea, and trouble sleeping. Serious side effects may include tendon rupture, tendon inflammation, seizures, psychosis, and potentially permanent peripheral nerve damage. Tendon damage may appear months after treatment is completed. People may also sunburn more easily. In people with myasthenia gravis muscle weakness and breathing problems may worsen.[2] The risk of use during pregnancy is low and it is probably okay during breastfeeding. Levofloxacin is a broad-spectrum antibiotic of the fluoroquinolone drug class.[3] It usually results in death of the bacteria.[2] It is the left sided isomer of the medication ofloxacin.[3]
Levofloxacin was approved for medical use in the United States in 1996.[2] It is on the World Health Organization's List of Essential Medicines, the most important medications needed in a basic health system.[4] It is available as a generic medication.[2] The wholesale cost is about 0.44 to 0.95 USD per week of treatment.[5] In the United States a week of treatment cost about 50 to 100 USD.[6]
Medical uses
Levofloxacin is used to treat infections including: respiratory tract infections, cellulitis, urinary tract infections, prostatitis, anthrax,[7] endocarditis, meningitis, pelvic inflammatory disease, traveler's diarrhea, tuberculosis and plague.[8]
Levofloxacin is used for the treatment of pneumonia, urinary tract infections, and abdominal infections. The Infectious Disease Society of America (IDSA) and the American Thoracic Society recommend levofloxacin and other respiratory fluoroquinolines as first line treatment for community acquired pneumonia when co-morbidities such as heart, lung, or liver disease are present or when in-patient treatment is required.[9] Levofloxacin also plays an important role in recommended treatment regimens for ventilator-associated and healthcare-associated pneumonia.[10]
It is recommended by the IDSA as a first-line treatment option for catheter-associated urinary tract infections in adults.[11] In combination with metronidazole it is recommended as one of several first-line treatment options for adult patients with community-acquired intra-abdominal infections of mild-to-moderate severity.[12] The IDSA also recommends it in combination with rifampicin as a first-line treatment for prosthetic joint infections.[13] The American Urological Association recommends levofloxacin as a first-line treatment for bacterial prostatitis.[14][15]
Levofloxacin and other fluoroquinolones have also been widely used for the treatment of uncomplicated community-acquired respiratory and urinary tract infections, indications for which major medical societies generally recommend the use of older, narrower spectrum drugs to avoid fluoroquinolone resistance development. Due to its widespread use, common pathogens such as Escherichia coli and Klebsiella pneumoniae have developed resistance. In many countries, resistance rates among healthcare-associated infections with these pathogens now exceeds 20%.[16][17][18]
Pregnancy
According to the FDA approved prescribing information, levofloxacin is pregnancy category C.[19] This designation indicates that animal reproduction studies have shown adverse effects on the fetus and there are no adequate and well-controlled studies in humans, but the potential benefit to the mother may in some cases outweigh the risk to the fetus. Other fluoroquinolones have also been reported as being present in the mother's milk and are passed on to the nursing child.[20][21]
Children
Levofloxacin is not approved in most countries for the treatment of children except in unique and life-threatening infections because it is associated with an elevated risk of musculoskeletal injury in this population, a property it shares with other fluoroquinolones.
In the United States levofloxacin is approved for the treatment of anthrax and plague in children over six months of age.[22]
Levofloxacin is recommended by the Pediatric Infectious Disease Society and the Infectious Disease Society of America as a first-line treatment for pediatric pneumonia caused by penicillin-resistant Streptococcus pneumoniae, and as a second-line agent for the treatment of penicillin-sensitive cases.[23]
In one study,[24][25] 1534 juvenile patients (age 6 months to 16 years) treated with levofloxacin as part of three efficacy trials were followed up to assess all musculoskeletal events occurring up to 12 months post-treatment. At 12 months follow-up the cumulative incidence of musculoskeletal adverse events was 3.4%, compared to 1.8% among 893 patients treated with other antibiotics. In the levafloxacin-treated group, approximately two-thirds of these musculoskeletal adverse events occurred in the first 60 days, 86% were mild, 17% were moderate, and all resolved without long-term sequelae.
In a study comparing the safety and efficacy of levofloxacin to that of azithromycin or the ceftriaxone in 712 children with community-acquired pneumonia, adverse events were experienced by 6% of those treated with levofloxacin and 4% of those treated with comparator antibiotics. Most of these adverse events were thought to be unrelated or doubtfully related to the levofloxacin. Two deaths were observed in the levofloxacin group, neither of which was thought to be treatment-related. Spontaneous reports to the FDA Adverse Effects Reporting System at the time of the 20 September 2011 FDA Pediatric Drugs Advisory Committee include musculoskeletal events (39, including 5 cases of tendon rupture) and central nervous system events (19, including 5 cases of seizures) as the most common spontaneous reports between April 2005 and March 2008. An estimated 130,000 pediatric prescriptions for levofloxacin were filled on behalf of 112,000 pediatric patients during that period.[26]
Spectrum of activity
Levofloxacin and later generation fluoroquinolones are collectively referred to as "respiratory quinolones" to distinguish them from earlier fluoroquinolones which exhibited modest activity toward the important respiratory pathogen Streptococcus pneumoniae.[27]
The drug exhibits enhanced activity against the important respiratory pathogen Streptococcus pneumoniae relative to earlier fluoroquinolone derivatives like ciprofloxacin. For this reason, it is considered a "respiratory fluoroquinolone" along with more recently developed fluoroquinolones such as moxifloxacin and gemifloxacin. It is less active than ciprofloxacin against Gram-negative bacteria, especially Pseudomonas aeruginosa, and lacks the anti-methicillin-resistant Staphylococcus aureus (MRSA) activity of moxifloxacin and gemifloxacin.[28][29][30][31] Levofloxacin has shown moderate activity against anaerobes, and is about twice as potent as ofloxacin against Mycobacterium tuberculosis and other mycobacteria, including Mycobacterium avium complex.[32]
Its spectrum of activity includes most strains of bacterial pathogens responsible for respiratory, urinary tract, gastrointestinal, and abdominal infections, including Gram negative (Escherichia coli, Haemophilus influenzae, Klebsiella pneumoniae, Legionella pneumophila, Moraxella catarrhalis, Proteus mirabilis, and Pseudomonas aeruginosa), Gram positive (methicillin-sensitive but not methicillin-resistant Staphylococcus aureus, Streptococcus pneumoniae, Staphylococcus epidermidis, Enterococcus faecalis, and Streptococcus pyogenes), and atypical bacterial pathogens (Chlamydophila pneumoniae and Mycoplasma pneumoniae). Compared to earlier antibiotics of the fluoroquinoline class such as ciprofloxacin, levofloxacin exhibits greater activity towards Gram-positive bacteria[28] but lesser activity toward Gram-negative bacteria,[33] especially Pseudomonas aeruginosa.
Availability
Levofloxacin is available in tablet form, injection, oral solution, as well as used in prescription eye and ear drops.[34]
Contraindications
Package inserts mention that levofloxacin is to be avoided in patients with a known hypersensitivity to levofloxacin or other quinolone drugs,[34] and that caution should be exercised in prescribing to patients with liver disease.[35][36]
Levofloxacin is also considered to be contraindicated in patients with epilepsy or other seizure disorders, and in patients who have a history of quinolone-associated tendon rupture.[35]
Adverse effects
Most adverse reactions are mild to moderate; however, sometimes serious adverse effects occur. There is some disagreement in the medical literature regarding whether and to what extent levofloxacin and other fluoroquinolones produce serious adverse effects more frequently than other broad spectrum antibacterial drugs.[37][38][39][40]
In pooled results from 7537 patients exposed to levofloxcacin in 29 clinical trials, 4.3% discontinued treatment due to adverse drug reactions. The most common adverse reactions leading to discontinuation were gastrointestinal, including nausea, vomiting, and constipation. Overall, 7% of patients experienced nausea, 6% headache, 5% diarrhea, 4% insomnia, along with other adverse reactions experienced at lower rates.[41]
Other less common but serious adverse effects have been observed both in clinical trials as well as in reviews of post-approval spontaneous adverse event reports. Prominent among these is the potential for tendon damage, including rupture of the Achilles tendon, which is the subject of a black box warning in the official prescribing informations for all fluoroquinolones in the United States. Injury, including tendon rupture, has been observed up to 6 months after cessation of treatment; the elderly, transplant patients, and those with a current or historical corticosteroid use are at elevated risk.[42] A population-based study in the Netherlands estimated that between 1 and 15 fluoroquinolone-attributable tendon ruptures resulted from 318,000 fluoroquinoline prescriptions in 1996. A detailed overview of risk factors for fluoroquinolone-associated tendon rupture has been published; advanced age, concurrent treatment with corticosteroids, and higher doses of fluoroquinolone appear to be the most important risk factors.[43] The U.S. label for levofloxacin also contains a black box warning for the exacerbation of the symptoms of the neurological disease myasthenia gravis.[44]
A wide variety of other uncommon but serious adverse events have been associated with fluoroquinolone use, with varying degrees of evidence supporting causation. These include irreversible peripheral neuropathy, anaphylaxis, hepatotoxicity, central nervous system effects including seizures and psychiatric effects, prolongation of the QT interval, blood glucose disturbances, and photosensitivity, among others.[41] Levofloxacin may produce fewer of these rare serious adverse effects than other fluoroquinolones.[45]
Administration of levofloxacin or other broad spectrum antibiotics is associated with Clostridium difficile associated diarrhea which may range in severity from mild diarrhea to fatal colitis. Fluoroquinoline administration may be associated with the acquisition and outgrowth of a particularly virulent Clostridium strain.[46]
The U.S. FDA requires a black box warning for levofloxacin, pertaining to peripheral nerve damage.[47]
Overdose
Overdosing experiments in animals showed central effects such as dizziness, confusion and seizures, as well as prolongation of the QT interval and gastrointestinal disorders.[35]
In the event of an acute overdosage, authorities recommend unspecific standard procedures such as emptying the stomach, observing the patient and maintaining appropriate hydration. Levofloxacin is not efficiently removed by hemodialysis or peritoneal dialysis.[34]
Interactions
Levofloxacin interacts with certain foods and several other drugs leading to undesirable increases or decreases in the serum levels or distribution of one or both drugs.
When levofloxacin is taken with anti-acids containing magnesium hydroxide or aluminum hydroxide, the two combine to form insoluble salts that are difficult to absorb from the intestines. Peak serum concentrations of levofloxacin may be reduced by 90% or more, which can prevent the levofloxacin from working. Similar results have been reported when levofloxacin is taken with iron supplements and multi-vitamins containing zinc.[48][49]
Unlike ciprofloxacin, levofloxacin does not appear to deactivate the drug metabolizing enzyme CYP1A2. Therefore, drugs that use that enzyme, like theophylline, do not interact with levofloxacin. It is a weak inhibitor of CYP2C9,[50] suggesting potential to block the breakdown of warfarin and phenprocoumon. This can result in more action of drugs like warfarin, leading to more potential side effects, such as bleeding.[51]
The use of non-steroidal anti-inflammatory drugs (NSAIDs) in combination with high dose fluoroquinolone therapy may lead to seizures.[52]
Mechanism of action
Levofloxacin is a broad-spectrum antibiotic that is active against both Gram-positive and Gram-negative bacteria. Like all quinolones, it functions by inhibiting the two type II topoisomerase enzymes, namely DNA gyrase and topoisomerase IV.[53] Topoisomerase IV is necessary to separate DNA that has been replicated (doubled) prior to bacterial cell division. With the DNA not being separated, the process is stopped, and the bacterium cannot divide. DNA gyrase, on the other hand, is responsible for supercoiling the DNA, so that it will fit in the newly formed cells. Both mechanisms amount to killing the bacterium, that is, levofloxacin acts as a bactericide.[54]
Chemical properties
Levofloxacin is the levo isomer of the racemate ofloxacin, another quinolone antimicrobial agent. In layman terms, this means that levofloxacin is the 50% of ofloxacin that have been found to be effective against bacteria, while the other 50% have been removed. In chemical terms, levofloxacin, a chiral fluorinated carboxyquinolone, is the pure (−)-(S)-enantiomer of the racemic ofloxacin.[55][56]
The substance is used as the hemihydrate, which has the empirical formula C18H20FN3O4 · ½ H2O and a molecular mass of 370.38 g/mol. Levofloxacin is a light-yellowish-white to yellow-white crystal or crystalline powder.[34]
Pharmacokinetics
Levofloxacin is rapidly and essentially completely absorbed after oral administration, with a plasma concentration profile over time that is essentially identical to that obtained from intravenous administration of the same amount over 60 minutes. As such, the intravenous and oral formulations of levofloxacin are considered interchangeable.[41]
The drug undergoes widespread distribution into body tissues. Peak levels in skin are achieved 3 hours after administration and exceed those in plasma by a factor of 2. Similarly, lung tissue concentrations range from two-fold to five-fold higher than plasma concentrations in the 24 hours after a single dose.
The mean terminal plasma elimination half-life of levofloxacin ranges from approximately 6 to 8 hours following single or multiple doses of levofloxacin given orally or intravenously. Elimination occurs mainly via excretion of unmetabolized drug in the urine. Following oral administration, 87% of an administered dose was recovered in the urine as unchanged drug within 2 days. Less than 5% was recovered in the urine as the desmethyl and N-oxide metabolites, the only metabolites identified in humans.
History
Levofloxacin contains the same main active ingredient as ofloxacin. Within the New Drug Application (NDA) for levofloxacin it was stated that:
- “...pre- NDA discussions with the applicant suggested quite strongly that levofloxacin is conceptually identical to ofloxacin. For ofloxacin, the dominant active drug substance is its 1- isomer, which is levofloxacin. Conceptually, this premise should lead to microbiological labeling essentially identical to ofloxacin... the applicant provided various basic studies in support of levofloxacin that had been actually performed using ofloxacin instead of levofloxacin. Particularly, some of the studies on mechanisms of action and the related resistance mechanisms were recapitulated from ofloxacin data rather than being generated anew for levofloxacin...."[57]
Levofloxacin is marketed by Sanofi-Aventis under the trade name "Tavanic" in Europe, Africa, the Middle East and South America, and by the Ortho-McNeil Pharmaceuticals subsidiary of Johnson and Johnson in the United States.[58][59]
Levofloxacin was first patented in 1987 (Levofloxacin European patent by Daiichi Pharmaceutical Co., Ltd.) and was approved by the United States Food and Drug Administration on 20 December 1996 for use in the United States to treat bacterial sinusitus, bacterial exacerbations of bronchitis, community-acquired pneumonia, uncomplicated skin infections, complicated urinary tract infections, and acute pyelonephritis.[60]
The term of the levofloxacin United States patent was extended by the U.S. Patent and Trademark Office under the provisions of the Hatch Waxman Amendment. Under the terms of Hatch-Waxman, the patent terms of pharmaceutical products that contain a novel active ingredient are extended by up to five years to compensate the developer for the patent life lost while performing clinical trials and other activities required to fulfill regulatory requirements. This extension was challenged by generic drug manufacturer Lupin Pharmaceuticals who argued that since levofloxacin is a single isomer of the previously approved antibacterial ofloxacin, it is not a "novel active ingredient" and thus ineligible for patent term extension. The federal patent court ruled in favor of Ortho McNeil, and generic versions of levofloxacin did not enter the U.S. market until 2009.[61]
Usage
The U.S. Food and Drug Administration (FDA) estimates that over 23 million outpatient prescriptions for fluoroquinolones were filled in the United States in 2011.[62]
Litigation
Class action
As of 2012, Johnson and Johnson was facing around 3400 state and federal lawsuits filed by people who claimed tendon damage from levofloxacin; about 1900 pending in a class action at the United States District Court in Minnesota[63] and about 1500 pending at a district court in New Jersey.[64][65]
In October 2012, J&J settled 845 cases in the Minnesota action, after Johnson and Johnson prevailed in three of the first four cases to go to trial. By May 2014, all but 363 cases had been settled or adjudicated.[65][66][67]
Research
Levofloxacin can be used effectively as a positive control in thorough QT/QTc studies in healthy volunteers. It can fulfill the criteria for a positive comparator, meaning in studies that require the target to have a long QT interval, it can be given to create such an interval in normally healthy individuals. The ICH E14 guidelines recommend a threshold of around 5 ms for a positive QT/QTc study. Studies have shown that levofloxacin causes a QT lengthening that is above this threshold, indicating its potential use in QT/QTc studies.[68]
References
- ^ "FDA-sourced list of all drugs with black box warnings (Use Download Full Results and View Query links.)". nctr-crs.fda.gov. FDA. Retrieved 22 October 2023.
- ^ a b c d e f "Levofloxacin". The American Society of Health-System Pharmacists. Retrieved Jan 2016.
{{cite web}}: Check date values in:|accessdate=(help) - ^ a b Yaffe, Gerald G. Briggs, Roger K. Freeman, Sumner J. (2011). Drugs in pregnancy and lactation : a reference guide to fetal and neonatal risk (9th ed.). Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins. p. 828. ISBN 9781608317080.
{{cite book}}: CS1 maint: multiple names: authors list (link) - ^ "WHO Model List of EssentialMedicines" (PDF). World Health Organization. October 2013. Retrieved 22 April 2014.
- ^ "Levofloxacin". International Drug Price Indicator Guide. Retrieved January 2016.
{{cite web}}: Check date values in:|accessdate=(help) - ^ Hamilton, Richart (2015). Tarascon Pocket Pharmacopoeia 2015 Deluxe Lab-Coat Edition. Jones & Bartlett Learning. p. 102. ISBN 9781284057560.
- ^ Renata Albrecht (24 November 2004). "NDA 20-634/S-035, NDA 20-635/S-035, NDA 21-721/S-003" (PDF). U.S. Food and Drug Administration (FDA).
- ^ "Levofloxacin". The American Society of Health-System Pharmacists. Retrieved 3 April 2011.
- ^ Mandell LA, Wunderink RG, Anzueto A, et al. (March 2007). "Infectious Diseases Society of America/American Thoracic Society consensus guidelines on the management of community-acquired pneumonia in adults". Clin. Infect. Dis. 44 Suppl 2: S27–72. doi:10.1086/511159. PMID 17278083.
- ^ File TM (August 2010). "Recommendations for treatment of hospital-acquired and ventilator-associated pneumonia: review of recent international guidelines". Clin. Infect. Dis. 51 Suppl 1: S42–7. doi:10.1086/653048. PMID 20597671.
- ^ Hooton TM, Bradley SF, Cardenas DD, et al. (March 2010). "Diagnosis, prevention, and treatment of catheter-associated urinary tract infection in adults: 2009 International Clinical Practice Guidelines from the Infectious Diseases Society of America". Clin. Infect. Dis. 50 (5): 625–63. doi:10.1086/650482. PMID 20175247.
- ^ Solomkin JS, Mazuski JE, Bradley JS, et al. (January 2010). "Diagnosis and management of complicated intra-abdominal infection in adults and children: guidelines by the Surgical Infection Society and the Infectious Diseases Society of America". Clin. Infect. Dis. 50 (2): 133–64. doi:10.1086/649554. PMID 20034345.
- ^ Osmon DR, Berbari EF, Berendt AR, et al. (January 2013). "Executive summary: diagnosis and management of prosthetic joint infection: clinical practice guidelines by the Infectious Diseases Society of America". Clin. Infect. Dis. 56 (1): 1–10. doi:10.1093/cid/cis966. PMID 23230301.
- ^ "www.uroweb.org" (PDF).
- ^ Schaeffer AJ (September 2004). "NIDDK-sponsored chronic prostatitis collaborative research network (CPCRN) 5-year data and treatment guidelines for bacterial prostatitis". Int. J. Antimicrob. Agents. 24 Suppl 1: S49–52. doi:10.1016/j.ijantimicag.2004.02.009. PMID 15364307.
- ^ "Antimicrobial resistance interactive database (EARS-Net)".
- ^ "www.ecdc.europa.eu" (PDF).
- ^ "www.cdc.gov" (PDF).
- ^ http://www.fda.gov/downloads/Drugs/EmergencyPreparedness/BioterrorismandDrugPreparedness/UCM133684.pdf
- ^ Shin HC, Kim JC, Chung MK (September 2003). "Fetal and maternal tissue distribution of the new fluoroquinolone DW-116 in pregnant rats". Comp. Biochem. Physiol. C Toxicol. Pharmacol. 136 (1): 95–102. doi:10.1016/j.cca.2003.08.004. PMID 14522602.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Dan M, Weidekamm E, Sagiv R, Portmann R, Zakut H (February 1993). "Penetration of fleroxacin into breast milk and pharmacokinetics in lactating women". Antimicrob. Agents Chemother. 37 (2): 293–6. doi:10.1128/AAC.37.2.293. PMC 187655. PMID 8452360.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Renata Albrecht (5 May 2008). "NDA 20-634/S-047, NDA 20-635/S-051, NDA 21-721/S-015" (PDF). U.S. Food and Drug Administration (FDA).
- ^ Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL, Mace SE, McCracken GH, Moore MR, St Peter SD, Stockwell JA, Swanson JT (2011). "The management of community-acquired pneumonia in infants and children older than 3 months of age: clinical practice guidelines by the Pediatric Infectious Diseases Society and the Infectious Diseases Society of America". Clin. Infect. Dis. 53 (7): e25–76. doi:10.1093/cid/cir531. PMID 21880587.
- ^ "www.accessdata.fda.gov" (PDF).
- ^ Noel GJ, Bradley JS, Kauffman RE (October 2007). "Comparative safety profile of levofloxacin in 2523 children with a focus on four specific musculoskeletal disorders". Pediatr. Infect. Dis. J. 26 (10): 879–91. doi:10.1097/INF.0b013e3180cbd382. PMID 17901792.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ "www.fda.gov" (PDF).
- ^ Wispelwey B, Schafer KR (November 2010). "Fluoroquinolones in the management of community-acquired pneumonia in primary care". Expert Rev Anti Infect Ther. 8 (11): 1259–71. doi:10.1586/eri.10.110. PMID 21073291.
- ^ a b Lafredo SC, Foleno BD, Fu KP (1993). "Induction of resistance of Streptococcus pneumoniae to quinolones in vitro". Chemotherapy. 39 (1): 36–9. doi:10.1159/000238971. PMID 8383031.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Fu KP, Lafredo SC, Foleno B, et al. (April 1992). "In vitro and in vivo antibacterial activities of levofloxacin (l-ofloxacin), an optically active ofloxacin". Antimicrob. Agents Chemother. 36 (4): 860–6. doi:10.1128/aac.36.4.860. PMC 189464. PMID 1503449.
- ^ Blondeau JM (May 1999). "A review of the comparative in-vitro activities of 12 antimicrobial agents, with a focus on five new respiratory quinolones'". J. Antimicrob. Chemother. 43 Suppl B (90002): 1–11. doi:10.1093/jac/43.suppl_2.1. PMID 10382869.
- ^ Cormican MG, Jones RN (January 1997). "Antimicrobial activity and spectrum of LB20304, a novel fluoronaphthyridone". Antimicrob. Agents Chemother. 41 (1): 204–11. PMC 163688. PMID 8980783.
- ^ John A. Bosso (1998). "New and Emerging Quinolone Antibiotics". Journal of Infectious Disease Pharmacotherapy. 2 (4): 61–76. doi:10.1300/J100v02n04_06. ISSN 1068-7777.
- ^ Yamane N, Jones RN, Frei R, Hoban DJ, Pignatari AC, Marco F (April 1994). "Levofloxacin in vitro activity: results from an international comparative study with ofloxacin and ciprofloxacin". J Chemother. 6 (2): 83–91. PMID 8077990.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ a b c d Janssen Pharmaceutica (September 2008). "Highlights of Prescribing Information" (PDF). U.S. Food and Drug Administration (FDA).
- ^ a b c Jasek, W, ed. (2007). Austria-Codex (in German) (62nd ed.). Vienna: Österreichischer Apothekerverlag. pp. 7961–7. ISBN 978-3-85200-181-4.
- ^ Coban S, Ceydilek B, Ekiz F, Erden E, Soykan I (October 2005). "Levofloxacin-induced acute fulminant hepatic failure in a patient with chronic hepatitis B infection". Ann Pharmacother. 39 (10): 1737–40. doi:10.1345/aph.1G111. PMID 16105873.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Liu HH (May 2010). "Safety profile of the fluoroquinolones: focus on levofloxacin". Drug Saf. 33 (5): 353–69. doi:10.2165/11536360-000000000-00000. PMID 20397737.
- ^ Karageorgopoulos DE, Giannopoulou KP, Grammatikos AP, Dimopoulos G, Falagas ME (March 2008). "Fluoroquinolones compared with beta-lactam antibiotics for the treatment of acute bacterial sinusitis: a meta-analysis of randomized controlled trials". CMAJ. 178 (7): 845–54. doi:10.1503/cmaj.071157. PMC 2267830. PMID 18362380.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Lipsky BA, Baker CA (February 1999). "Fluoroquinolone toxicity profiles: a review focusing on newer agents". Clin. Infect. Dis. 28 (2): 352–64. doi:10.1086/515104. PMID 10064255.
- ^ Stahlmann R, Lode HM (July 2013). "Risks associated with the therapeutic use of fluoroquinolones". Expert Opin Drug Saf. 12 (4): 497–505. doi:10.1517/14740338.2013.796362. PMID 23651367.
- ^ a b c "www.accessdata.fda.gov" (PDF).
- ^ Khaliq Y, Zhanel GG (June 2003). "Fluoroquinolone-associated tendinopathy: a critical review of the literature". Clin. Infect. Dis. 36 (11): 1404–10. doi:10.1086/375078. PMID 12766835.
- ^ Kim GK (April 2010). "The Risk of Fluoroquinolone-induced Tendinopathy and Tendon Rupture: What Does The Clinician Need To Know?". J Clin Aesthet Dermatol. 3 (4): 49–54. PMC 2921747. PMID 20725547.
- ^ Jones SC, Sorbello A, Boucher RM (October 2011). "Fluoroquinolone-associated myasthenia gravis exacerbation: evaluation of postmarketing reports from the US FDA adverse event reporting system and a literature review". Drug Saf. 34 (10): 839–47. doi:10.2165/11593110-000000000-00000. PMID 21879778.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Carbon C (2001). "Comparison of side effects of levofloxacin versus other fluoroquinolones". Chemotherapy. 47 Suppl 3: 9–14, discussion 44–8. doi:10.1159/000057839. PMID 11549784.
- ^ Vardakas KZ, Konstantelias AA, Loizidis G, Rafailidis PI, Falagas ME (November 2012). "Risk factors for development of Clostridium difficile infection due to BI/NAP1/027 strain: a meta-analysis". Int. J. Infect. Dis. 16 (11): e768–73. doi:10.1016/j.ijid.2012.07.010. PMID 22921930.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ http://www.fda.gov/Drugs/DrugSafety/ucm365050.htm
- ^ Rodvold KA, Piscitelli SC (August 1993). "New oral macrolide and fluoroquinolone antibiotics: an overview of pharmacokinetics, interactions, and safety". Clin. Infect. Dis. 17 Suppl 1: S192–9. doi:10.1093/clinids/17.supplement_1.s192. PMID 8399914.
- ^ Tanaka M, Kurata T, Fujisawa C, et al. (October 1993). "Mechanistic study of inhibition of levofloxacin absorption by aluminum hydroxide". Antimicrob. Agents Chemother. 37 (10): 2173–8. doi:10.1128/aac.37.10.2173. PMC 192246. PMID 8257141.
- ^ Zhang L, Wei MJ, Zhao CY, Qi HM (December 2008). "Determination of the inhibitory potential of 6 fluoroquinolones on CYP1A2 and CYP2C9 in human liver microsomes". Acta Pharmacol. Sin. 29 (12): 1507–14. doi:10.1111/j.1745-7254.2008.00908.x. PMID 19026171.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Schelleman H, Bilker WB, Brensinger CM, Han X, Kimmel SE, Hennessy S (November 2008). "Warfarin with fluoroquinolones, sulfonamides, or azole antifungals: interactions and the risk of hospitalization for gastrointestinal bleeding". Clin. Pharmacol. Ther. 84 (5): 581–8. doi:10.1038/clpt.2008.150. PMC 2574587. PMID 18685566.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Domagala JM (April 1994). "Structure-activity and structure-side-effect relationships for the quinolone antibacterials". J. Antimicrob. Chemother. 33 (4): 685–706. doi:10.1093/jac/33.4.685. PMID 8056688.
- ^ Drlica K, Zhao X (1 September 1997). "DNA gyrase, topoisomerase IV, and the 4-quinolones". Microbiol Mol Biol Rev. 61 (3): 377–92. PMC 232616. PMID 9293187.
- ^ Mutschler, Ernst; Schäfer-Korting, Monika (2001). Arzneimittelwirkungen (in German) (8 ed.). Stuttgart: Wissenschaftliche Verlagsgesellschaft. p. 814f. ISBN 3-8047-1763-2.
- ^ Morrissey, I.; Hoshino, K.; Sato, K.; Yoshida, A.; Hayakawa, I.; Bures, MG.; Shen, LL. (August 1996). "Mechanism of differential activities of ofloxacin enantiomers" (PDF). Antimicrob Agents Chemother. 40 (8): 1775–84. PMC 163416. PMID 8843280.
- ^ Kannappan, Valliappan; Mannemala, Sai Sandeep (7 June 2014). "Multiple Response Optimization of a HPLC Method for the Determination of Enantiomeric Purity of S-Ofloxacin". Chromatographia. 77 (17–18): 1203–1211. doi:10.1007/s10337-014-2699-4.
- ^ "STATISTICAL REVIEW AND EVALUATION" (PDF). USA: FDA. 21 November 1996.
- ^ University of Maryland Medical Center. "Levofloxacin". USA: University of Maryland. Archived from the original on 10 December 2008.
{{cite web}}: Unknown parameter|deadurl=ignored (|url-status=suggested) (help) - ^ Takashi Shoda (23 October 2008). "UK Levofloxacin SPC and Underlying Patent Upheld by High Court Patent Court". USA: Daiichi Sankyo, Limited. Archived from the original on 27 August 2009.
{{cite web}}: Unknown parameter|deadurl=ignored (|url-status=suggested) (help) - ^ "www.accessdata.fda.gov" (PDF).
- ^ "GenericsWeb - The Search is Over".
- ^ "FDA Drug Safety Communication: FDA requires label changes to warn of risk for possibly permanent nerve damage from antibacterial fluoroquinolone drugs taken by mouth or by injection".
- ^ Judge John R. Tunheim. "Levaquin MDL". USA: US Courts. Retrieved 7 September 2009.
- ^ Charles Toutant (6 July 2009). "Litigation Over Johnson & Johnson Antibiotic Levaquin Designated N.J. Mass Tort". New Jersey Law Journal.
- ^ a b Margaret Cronin Fisk and Beth Hawkins for Bloomberg News. Nov 1, 2012 Johnson & Johnson Settles 845 Levaquin Lawsuits
- ^ "Johnson & Johnson Settles 845 Levaquin Lawsuits - Businessweek".
- ^ "Levaquin MDL | United States District Court - District of Minnesota, United States District Court - District of Minnesota".
- ^ Taubel J, Naseem A, Harada T, Wang D, Arezina R, Lorch U, Camm AJ (November 2009). "Levofloxacin can be used effectively as a positive control in thorough QT/QTc studies in healthy volunteers" (PDF). British Journal of Clinical Pharmacology. 69 (4): 391–400. doi:10.1111/j.1365-2125.2009.03595.x. PMC 2848412. PMID 20406223.
