Ayurveda

| This article is part of a series on |
| Alternative medicine |
|---|
 |
| Part of a series on |
| Hinduism |
|---|
 |
Ayurveda (/ˌɑːjʊərˈveɪdə, -ˈviː-/; IAST: ayurveda)[1] is an alternative medicine system with historical roots in the Indian subcontinent.[2] It is heavily practiced in India and Nepal, where around 80% of the population report using ayurveda.[3][4][5] The theory and practice of ayurveda is pseudoscientific.[6][7][8]
Ayurveda therapies have varied and evolved over more than two millennia.[2] Therapies include herbal medicines, special diets, meditation, yoga, massage, laxatives, enemas, and medical oils.[9][10] Ayurvedic preparations are typically based on complex herbal compounds, minerals, and metal substances (perhaps under the influence of early Indian alchemy or rasashastra). Ancient ayurveda texts also taught surgical techniques, including rhinoplasty, kidney stone extractions, sutures, and the extraction of foreign objects.[11][12]
The main classical ayurveda texts begin with accounts of the transmission of medical knowledge from the gods to sages, and then to human physicians.[13] Printed editions of the Sushruta Samhita (Sushruta's Compendium), frame the work as the teachings of Dhanvantari, Hindu god of ayurveda, incarnated as King Divodāsa of Varanasi, to a group of physicians, including Sushruta.[14][15] The oldest manuscripts of the work, however, omit this frame, ascribing the work directly to King Divodāsa.[16] Through well-understood processes of modernization and globalization, ayurveda has been adapted for Western consumption, notably by Baba Hari Dass in the 1970s and Maharishi ayurveda in the 1980s.[17] Historical evidence for ayurvedic texts, terminology and concepts appears from the middle of the first millennium BCE onwards.[18]
In ayurveda texts, dosha balance is emphasized, and suppressing natural urges is considered unhealthy and claimed to lead to illness.[19] Ayurveda treatises describe three elemental doshas: vāta, pitta and kapha, and state that balance (Skt. sāmyatva) of the doshas results in health, while imbalance (viṣamatva) results in disease. Ayurveda treatises divide medicine into eight canonical components. Ayurveda practitioners had developed various medicinal preparations and surgical procedures from at least the beginning of the common era.[20]
There is no good evidence that ayurveda is effective to treat or cure cancer.[10] Some ayurvedic preparations have been found to contain lead, mercury, and arsenic,[9][21] substances known to be harmful to humans. A 2008 study found the three substances in close to 21% of U.S. and Indian-manufactured patent ayurvedic medicines sold through the Internet.[22] The public health implications of such metallic contaminants in India are unknown.[22]
Etymology
The term āyurveda (Sanskrit: आयुर्वेद) is composed of two words, āyus, आयुस्, "life" or "longevity", and veda, वेद, "knowledge", translated as "knowledge of longevity"[23][24] or "knowledge of life and longevity".[25]
Eight components

The earliest classical Sanskrit works on ayurveda describe medicine as being divided into eight components (Skt. aṅga).[27][28] This characterization of the physician's art, "the medicine that has eight components" (Sanskrit: चिकित्सायामष्टाङ्गायाम्, romanized: cikitsāyām aṣṭāṅgāyāṃ), is first found in the Sanskrit epic the Mahābhārata, c. 4th century BCE.[29] The components are:[30][25][31]
- Kāyachikitsā: general medicine, medicine of the body
- Kaumāra-bhṛtya (Pediatrics): Discussions about prenatal and postnatal care of baby and mother; methods of conception; choosing the child's sex, intelligence, and constitution; childhood diseases; and midwifery[32]
- Śalyatantra: surgical techniques and the extraction of foreign objects
- Śhālākyatantra: treatment of ailments affecting openings or cavities in the upper body: ears, eyes, nose, mouth, etc.
- Bhūtavidyā: pacification of possessing spirits, and the people whose minds are affected by such possession
- Agadatantra/Vishagara-vairodh Tantra (Toxicology): includes epidemics; toxins in animals, vegetables and minerals; and keys for recognizing those anomalies and their antidotes
- Rasāyantantra: rejuvenation and tonics for increasing lifespan, intellect and strength
- Vājīkaraṇatantra: aphrodisiacs; treatments for increasing the volume and viability of semen and sexual pleasure; infertility problems; and spiritual development (transmutation of sexual energy into spiritual energy)
Principles and terminology
The central theoretical ideas of ayurveda show parallels with Samkhya and Vaisheshika philosophies, as well as with Buddhism and Jainism.[33][34] Balance is emphasized, and suppressing natural urges is considered unhealthy and claimed to lead to illness.[19] For example, to suppress sneezing is said to potentially give rise to shoulder pain.[35] However, people are also cautioned to stay within the limits of reasonable balance and measure when following nature's urges.[19] For example, emphasis is placed on moderation of food intake,[36] sleep, and sexual intercourse.[19]
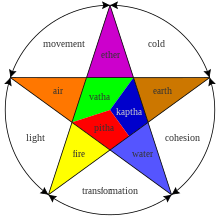
According to ayurveda, the human body is composed of tissues (dhatus), waste (malas), and humeral biomaterials (doshas).[37] The seven dhatus are chyle (rasa), blood (rakta), muscles (māmsa), fat (meda), bone (asthi), marrow (majja), and semen (shukra). Like the medicine of classical antiquity, the classic treatises of ayurveda divided bodily substances into five classical elements (panchamahabhuta) viz. earth, water, fire, air and ether.[38] There are also twenty gunas (qualities or characteristics) which are considered to be inherent in all matter. These are organized in ten pairs: heavy/light, cold/hot, unctuous/dry, dull/sharp, stable/mobile, soft/hard, non-slimy/slimy, smooth/coarse, minute/gross, and viscous/liquid.[39]
The three postulated elemental bodily humours, the doshas or tridosha, are vata (air, which some modern authors equate with the nervous system), pitta (bile, fire, equated by some with enzymes), and kapha (phlegm, or earth and water, equated by some with mucus). Contemporary critics assert that doshas are not real, but are a fictional concept.[40] The humours (doshas) may also affect mental health. Each dosha has particular attributes and roles within the body and mind; the natural predominance of one or more doshas thus explains a person's physical constitution (prakriti) and personality.[37][41][42] Ayurvedic tradition holds that imbalance among the bodily and mental doshas is a major etiologic component of disease. One ayurvedic view is that the doshas are balanced when they are equal to each other, while another view is that each human possesses a unique combination of the doshas which define this person's temperament and characteristics. In either case, it says that each person should modulate their behavior or environment to increase or decrease the doshas and maintain their natural state. Practitioners of ayurveda must determine an individual's bodily and mental dosha makeup, as certain prakriti are said to predispose one to particular diseases.[43][37] For example, a person who is thin, shy, excitable, has a pronounced Adam's apple, and enjoys esoteric knowledge is likely vata prakriti and therefore more susceptible to conditions such as flatulence, stuttering, and rheumatism.[37][44] Deranged vata is also associated with certain mental disorders due to excited or excess vayu (gas), although the ayurvedic text Charaka Samhita also attributes "insanity" (unmada) to cold food and possession by the ghost of a sinful Brahman (brahmarakshasa).[37][43][45][46]
Ama (a Sanskrit word meaning "uncooked" or "undigested") is used to refer to the concept of anything that exists in a state of incomplete transformation. With regards to oral hygiene, it is claimed to be a toxic byproduct generated by improper or incomplete digestion.[47][48][49] The concept has no equivalent in standard medicine.
In medieval taxonomies of the Sanskrit knowledge systems, ayurveda is assigned a place as a subsidiary Veda (upaveda).[50] Some medicinal plant names from the Atharvaveda and other Vedas can be found in subsequent ayurveda literature.[51] Some other school of thoughts considers 'ayurveda' as the 'Fifth Veda'.[52] The earliest recorded theoretical statements about the canonical models of disease in ayurveda occur in the earliest Buddhist Canon.[53]
Practice

Ayurvedic practitioners regard physical existence, mental existence, and personality as three separate elements of a whole person with each element being able to influence the others.[54] This holistic approach used during diagnosis and healing is a fundamental aspect of ayurveda. Another part of ayurvedic treatment says that there are channels (srotas) which transport fluids, and that the channels can be opened up by massage treatment using oils and Swedana (fomentation). Unhealthy, or blocked, channels are thought to cause disease.[55]
Diagnosis

Ayurveda has eight ways to diagnose illness, called nadi (pulse), mootra (urine), mala (stool), jihva (tongue), shabda (speech), sparsha (touch), druk (vision), and aakruti (appearance).[56] Ayurvedic practitioners approach diagnosis by using the five senses.[57] For example, hearing is used to observe the condition of breathing and speech.[38] The study of the lethal points or marman marma is of special importance.[39]

Treatment and prevention
Two of the eight branches of classical ayurveda deal with surgery (Śalya-cikitsā and Śālākya-tantra), but contemporary ayurveda tends to stress attaining vitality by building a healthy metabolic system and maintaining good digestion and excretion.[39] Ayurveda also focuses on exercise, yoga, and meditation.[58] One type of prescription is a Sattvic diet.
Ayurveda follows the concept of Dinacharya, which says that natural cycles (waking, sleeping, working, meditation etc.) are important for health. Hygiene, including regular bathing, cleaning of teeth, oil pulling, tongue scraping, skin care, and eye washing, is also a central practice.[38]
Substances used

The vast majority (90%) of ayurvedic remedies are plant based.[59] Plant-based treatments in ayurveda may be derived from roots, leaves, fruits, bark, or seeds; some examples of plant-based substances include cardamom and cinnamon. In the 19th century, William Dymock and co-authors summarized hundreds of plant-derived medicines along with the uses, microscopic structure, chemical composition, toxicology, prevalent myths and stories, and relation to commerce in British India.[60] Triphala, an herbal formulation of three fruits, Amalaki, Bibhitaki, and Haritaki, is one of the most commonly used[61] Ayurvedic remedies.[62][63] The herbs Withania somnifera (Ashwagandha)[64] and Ocimum tenuiflorum (Tulsi)[59] are also routinely used in ayurveda.

Animal products used in ayurveda include milk, bones, and gallstones.[65] In addition, fats are prescribed both for consumption and for external use. Consumption of minerals, including sulphur, arsenic, lead, copper sulfate and gold, are also prescribed.[38] The addition of minerals to herbal medicine is called rasashastra.
Ayurveda uses alcoholic beverages called Madya,[66] which are said to adjust the doshas by increasing pitta and reducing vatta and kapha.[66] Madya are classified by the raw material and fermentation process, and the categories include: sugar-based, fruit-based, cereal-based, cereal-based with herbs, fermentated with vinegar, and tonic wines. The intended outcomes can include causing purgation, improving digestion or taste, creating dryness, or loosening joints. Ayurvedic texts describe Madya as non-viscid and fast-acting, and say that it enters and cleans minute pores in the body.[66]
Purified opium[67] is used in eight ayurvedic preparations[68] and is said to balance the vata and kapha doshas and increase the pitta dosha.[67] It is prescribed for diarrhea and dysentery, for increasing the sexual and muscular ability, and for affecting the brain. The sedative and pain-relieving properties of opium are considered in ayurveda. The use of opium is found in the ancient ayurvedic texts, and is first mentioned in the Sarngadhara Samhita (1300–1400 CE), a book on pharmacy used in Rajasthan in Western India, as an ingredient of an aphrodisiac to delay male ejaculation.[69] It is possible that opium was brought to India along with or before Muslim conquests.[68][70] The book Yoga Ratnakara (1700–1800 CE, unknown author), which is popular in Maharashtra, uses opium in a herbal-mineral composition prescribed for diarrhea.[69] In the Bhaisajya Ratnavali, opium and camphor are used for acute gastroenteritis. In this drug, the respiratory depressant action of opium is counteracted by the respiratory stimulant property of camphor.[69] Later books have included the narcotic property for use as analgesic pain reliever.[69]
Cannabis indica is also mentioned in the ancient ayurveda books, and is first mentioned in the Sarngadhara Samhita as a treatment for diarrhea.[69] In the Bhaisajya Ratnavali it is named as an ingredient in an aphrodisiac.[69]
Ayurveda says that both oil and tar can be used to stop bleeding,[38] and that traumatic bleeding can be stopped by four different methods: ligation of the blood vessel, cauterisation by heat, use of preparations to facilitate clotting, and use of preparations to constrict the blood vessels.

Massage with oil is commonly prescribed by ayurvedic practitioners.[71] Oils are used in a number of ways, including regular consumption, anointing, smearing, head massage, application to affected areas,[72][failed verification] and oil pulling. Liquids may also be poured on the patient's forehead, a technique called shirodhara.[73]
Panchakarma
According to ayurveda, panchakarma are techniques to eliminate toxic elements from the body.[74] Panchakarma refers to five actions, which are meant to be performed in a designated sequence with the stated aim of restoring balance in the body through a process of purgation.[75]
Current status
Ayurveda is widely practiced in India, Bangladesh, Sri Lanka, and Nepal[76] where public institutions offer formal study in the form of a Bachelor of Ayurvedic Medicine and Surgery (BAMS) degree. In certain parts of the world, the legal standing of practitioners is equivalent to that of conventional medicine.[76] Several scholars have described the contemporary Indian application of ayurvedic practice as being "biomedicalized" relative to the more "spiritualized" emphasis to practice found in variants in the West.[77][75]
Exposure to European developments in medicine from the nineteenth century onwards, through European colonization of India and the subsequent institutionalized support for European forms of medicine amongst European heritage settlers in India[78] were challenging to ayurveda, with the entire epistemology called into question. From the twentieth century, ayurveda became politically, conceptually, and commercially dominated by modern biomedicine, resulting in "modern ayurveda" and "global ayurveda".[23] Modern ayurveda is geographically located in the Indian subcontinent and tends towards secularization through minimization of the magic and mythic aspects of ayurveda.[23][24] Global ayurveda encompasses multiple forms of practice that developed through dispersal to a wide geographical area outside of India.[23] Smith and Wujastyk further delineate that global ayurveda includes those primarily interested in the ayurveda pharmacopeia, and also the practitioners of New Age ayurveda (which may link ayurveda to yoga and Indian spirituality and/or emphasize preventative practice, mind body medicine, or Maharishi ayurveda).[24]
Since the 1980s, ayurveda has also become the subject of interdisciplinary studies in ethnomedicine which seeks to integrate the biomedical sciences and humanities to improve the pharmacopeia of ayurveda.[24] According to industry research, the global ayurveda market was worth US$4.5 billion in 2017.[79]
The Indian subcontinent

India
It was reported in 2008[3] and again in 2018[80] that 80 percent of people in India used ayurveda exclusively or combined with conventional Western medicine.[3][80] A 2014 national health survey found that, in general, forms of the Indian system of medicine or AYUSH (ayurveda, yoga and naturopathy, unani, siddha, and homeopathy) were used by about 3.5% of patients who were seeking outpatient care over a two-week reference period.[81]
In 1970, the Parliament of India passed the Indian Medical Central Council Act which aimed to standardise qualifications for ayurveda practitioners and provide accredited institutions for its study and research.[82] In 1971, the Central Council of Indian Medicine (CCIM) was established under the Department of Ayurveda, Yoga and Naturopathy, Unani, Siddha medicine and Homoeopathy (AYUSH), Ministry of Health and Family Welfare, to monitor higher education in ayurveda in India.[83] The Indian government supports research and teaching in ayurveda through many channels at both the national and state levels, and helps institutionalise traditional medicine so that it can be studied in major towns and cities.[84] The state-sponsored Central Council for Research in Ayurvedic Sciences (CCRAS) is designed to do research on ayurveda.[85] Many clinics in urban and rural areas are run by professionals who qualify from these institutes.[82] As of 2013[update], India had over 180 training centers that offered degrees in traditional ayurvedic medicine.[58]
To fight biopiracy and unethical patents, the government of India set up the Traditional Knowledge Digital Library in 2001 to serve as a repository for formulations from systems of Indian medicine, such as ayurveda, unani and siddha medicine.[86][87] The formulations come from over 100 traditional ayurveda books.[88] An Indian Academy of Sciences document quoting a 2003–04 report states that India had 432,625 registered medical practitioners, 13,925 dispensaries, 2,253 hospitals and a bed strength of 43,803. 209 undergraduate teaching institutions and 16 postgraduate institutions.[89] In 2012, it was reported that insurance companies covered expenses for ayurvedic treatments in case of conditions such as spinal cord disorders, bone disorder, arthritis and cancer. Such claims constituted 5–10 percent of the country's health insurance claims.[90]
Maharashtra Andhashraddha Nirmoolan Samiti, an organisation dedicated to fighting superstition in India, considers ayurveda to be pseudoscience.[8]
On 9 November 2014, India formed the Ministry of AYUSH.[91][92] National Ayurveda Day is also observed in India on the birth of Dhanvantari that is Dhanteras.[93]
In 2016, the World Health Organization (WHO) published a report titled "The Health Workforce in India" which found that 31 percent of those who claimed to be doctors in India in 2001 were educated only up to the secondary school level and 57 percent went without any medical qualification.[94] The WHO study found that the situation was worse in rural India with only 18.8 percent of doctors holding a medical qualification.[94] Overall, the study revealed that nationally the density of all doctors (mainstream, ayurvedic, homeopathic and unani) was 8 doctors per 10,000 people compared to 13 per 10,000 people in China.[94][95]
Nepal
About 75% to 80% of the population of Nepal use ayurveda.[4][5] As of 2009, ayurveda was considered to be the most common and popular form of medicine in Nepal.[96]
Sri Lanka

The Sri Lankan tradition of ayurveda is similar to the Indian tradition. Practitioners of ayurveda in Sri Lanka refer to Sanskrit texts which are common to both countries. However, they do differ in some aspects, particularly in the herbs used.
In 1980, the Sri Lankan government established a Ministry of Indigenous Medicine to revive and regulate ayurveda.[97] The Institute of Indigenous Medicine (affiliated to the University of Colombo) offers undergraduate, postgraduate, and MD degrees in ayurveda medicine and surgery, and similar degrees in unani medicine.[98] In 2010, the public system had 62 ayurvedic hospitals and 208 central dispensaries, which served about 3 million people (about 11% of Sri Lanka's population). There are an estimated 20,000 registered practitioners of ayurveda in Sri Lanka.[99][100]
According to the Mahavamsa, an ancient chronicle of Sinhalese royalty from the sixth century CE, King Pandukabhaya (reigned 437 BCE to 367 BCE) had lying-in-homes and ayurvedic hospitals (Sivikasotthi-Sala) built in various parts of the country. This is the earliest documented evidence available of institutions dedicated specifically to the care of the sick anywhere in the world.[101][102] The hospital at Mihintale is the oldest in the world.[103]
Outside the Indian subcontinent

Ayurveda is a system of traditional medicine developed during antiquity and the medieval period, and as such is comparable to pre-modern Chinese and European systems of medicine. In the 1960s, ayurveda began to be advertised as alternative medicine in the Western world. Due to different laws and medical regulations around the globe, the expanding practice and commercialisation of ayurveda raised ethical and legal issues.[104] Ayurveda was adapted for Western consumption, particularly by Baba Hari Dass in the 1970s and by Maharishi Ayurveda in the 1980s.[17] In some cases, this involved active fraud on the part of proponents of ayurveda in an attempt to falsely represent the system as equal to the standards of modern medical research.[104][105][106]
United States
Baba Hari Dass was an early proponent who helped bring ayurveda to the United States in the early 1970s. His teachings led to the establishment of the Mount Madonna Institute.[107] He invited several notable ayurvedic teachers, including Vasant Lad, Sarita Shrestha, and Ram Harsh Singh. The ayurvedic practitioner Michael Tierra wrote that the "history of Ayurveda in North America will always owe a debt to the selfless contributions of Baba Hari Dass".[108]
In the United States, the practice of ayurveda is not licensed or regulated by any state. The National Center for Complementary and Integrative Health (NCCIH) stated that "Few well-designed clinical trials and systematic research reviews suggest that Ayurvedic approaches are effective". The NCCIH warned against the issue of heavy metal poisoning, and emphasised the use of conventional health providers first.[109] As of 2018, the NCCIH reported that 240,000 Americans were using ayurvedic medicine.[109]
Europe
The first ayurvedic clinic in Switzerland was opened in 1987 by Maharishi Mahesh Yogi.[110] In 2015, the government of Switzerland introduced a federally recognized diploma in ayurveda.[111]
Classification and efficacy
Ayurvedic medicine is considered pseudoscientific because its premises are not based on science.[7][6] Both the lack of scientific soundness in the theoretical foundations of ayurveda and the quality of research have been criticized.[7][112][113][114]
Although laboratory experiments suggest that some herbs and substances in ayurveda might be developed into effective treatments, there is no evidence that any are effective in themselves.[115][116] There is no good evidence that ayurvedic medicine is effective to treat or cure cancer in people.[10] Although ayurveda may help "improve quality of life" and Cancer Research UK also acknowledges that "researchers have found that some Ayurvedic treatments can help relieve cancer symptoms", the organization warns that some ayurvedic drugs contain toxic substances or may interact with legitimate cancer drugs in a harmful way.[10]
Ethnologist Johannes Quack writes that although the rationalist movement Maharashtra Andhashraddha Nirmoolan Samiti officially labels ayurveda a pseudoscience akin to astrology, these practices are in fact embraced by many of the movement's members.[8]
A review of the use of ayurveda for cardiovascular disease concluded that the evidence is not convincing for the use of any ayurvedic herbal treatment for heart disease or hypertension, but that many herbs used by ayurvedic practitioners could be appropriate for further research.[117]
Research
In India, research in ayurveda is undertaken by the Ministry of AYUSH through a national network of research institutes.[118]
In Nepal, the National Ayurvedic Training and Research Centre (NATRC) researches medicinal herbs in the country.[119]
In Sri Lanka, the Ministry of Health, Nutrition and Indigenous Medicine looks after the research in ayurveda through various national research institutes.[120]
Use of toxic metals
Rasashastra, the practice of adding metals, minerals or gems to herbal preparations, may include toxic heavy metals such as lead, mercury and arsenic.[22] The public health implications of metals in rasashastra in India is unknown.[22] Adverse reactions to herbs are described in traditional ayurvedic texts, but practitioners are reluctant to admit that herbs could be toxic and that reliable information on herbal toxicity is not readily available. There is a communication gap between practitioners of medicine and ayurveda.[121]
Some traditional Indian herbal medicinal products contain harmful levels of heavy metals, including lead.[122] For example, ghasard, a product commonly given to infants for digestive issues, has been found to have up to 1.6% lead concentration by weight, leading to lead encephalopathy.[123] A 1990 study on ayurvedic medicines in India found that 41% of the products tested contained arsenic, and that 64% contained lead and mercury.[3] A 2004 study found toxic levels of heavy metals in 20% of ayurvedic preparations made in South Asia and sold in the Boston area, and concluded that ayurvedic products posed serious health risks and should be tested for heavy-metal contamination.[124] A 2008 study of more than 230 products found that approximately 20% of remedies (and 40% of rasashastra medicines) purchased over the Internet from U.S. and Indian suppliers contained lead, mercury or arsenic.[22][125][126] A 2015 study of users in the United States found elevated blood lead levels in 40% of those tested, leading physician and former U.S. Air Force flight surgeon Harriet Hall to say that "Ayurveda is basically superstition mixed with a soupçon of practical health advice. And it can be dangerous."[127][128] A 2022 study found that ayurvedic preparations purchased over-the-counter in Chandigarh, India, had levels of zinc, mercury, arsenic and lead over the limits set by the Food and Agriculture Organisation / World Health Organisation. 83% exceeded the limit for zinc, 69% for mercury, 14% for arsenic and 5% for lead.[21]
Heavy metals are thought of as active ingredients by advocates of Indian herbal medicinal products.[122] According to ancient ayurvedic texts, certain physico-chemical purification processes such as samskaras or shodhanas (for metals) 'detoxify' the heavy metals in it.[129][130] These are similar to the Chinese pao zhi, although the ayurvedic techniques are more complex and may involve physical pharmacy techniques as well as mantras. However, these products have nonetheless caused severe lead poisoning and other toxic effects.[125] Between 1978 and 2008, "more than 80 cases of lead poisoning associated with Ayurvedic medicine use [were] reported worldwide".[131] In 2012, the U.S. Centers for Disease Control and Prevention (CDC) linked ayurvedic drugs to lead poisoning, based on cases where toxic materials were found in the blood of pregnant women who had taken ayurvedic drugs.[132]
Ayurvedic practitioners argue that the toxicity of bhasmas (ash products) comes from improper manufacturing processes, contaminants, improper use of ayurvedic medicine, quality of raw materials and that the end products and improper procedures are used by charlatans.[130]
In India, the government ruled that ayurvedic products must be labelled with their metallic content.[133] However, in Current Science, a publication of the Indian Academy of Sciences, M. S. Valiathan said that "the absence of post-market surveillance and the paucity of test laboratory facilities [in India] make the quality control of Ayurvedic medicines exceedingly difficult at this time".[133] In the United States, most ayurvedic products are marketed without having been reviewed or approved by the FDA. Since 2007, the FDA has placed an import alert on some ayurvedic products in order to prevent them from entering the United States.[134] A 2012 toxicological review of mercury-based traditional herbo-metallic preparations concluded that the long-term pharmacotherapeutic and in-depth toxicity studies of these preparations are lacking.[135]
History
This section may rely excessively on sources too closely associated with the subject, potentially preventing the article from being verifiable and neutral. (April 2018) |
Some scholars assert that the concepts of traditional ayurvedic medicine have existed since the times of the Indus Valley civilisation but since the Indus script has not been deciphered, such assertions are moot.[23]: 535–536 The Atharvaveda contains hymns and prayers aimed at curing disease. There are various legendary accounts of the origin of ayurveda, such as that it was received by Dhanvantari (or Divodasa) from Brahma.[15][38] Tradition also holds that the writings of ayurveda were influenced by a lost text by the sage Agnivesha.[136]
Ayurveda is one of the few systems of medicine developed in ancient times that is still widely practised in modern times.[24] As such, it is open to the criticism that its conceptual basis is obsolete and that its contemporary practitioners have not taken account of the developments in medicine.[137][138] Responses to this situation led to an impassioned debate in India during the early decades of the twentieth century, between proponents of unchanging tradition (śuddha "pure" ayurveda) and those who thought ayurveda should modernize and syncretize (aśuddha "impure, tainted" ayurveda).[139][140][141] The political debate about the place of ayurveda in contemporary India has continued to the present, both in the public arena and in government.[142] Debate about the place of ayurvedic medicine in the contemporary internationalized world also continues today.[143][144]
Main texts
Many ancient works on ayurvedic medicine are lost to posterity,[145] but manuscripts of three principal early texts on ayurveda have survived to the present day. These works are the Charaka Samhita, the Sushruta Samhita and the Bhela Samhita. The dating of these works is historically complicated since they each internally present themselves as composite works compiled by several editors. All past scholarship on their dating has been evaluated by Meulenbeld in volumes IA and IB of his History of Indian Medical Literature.[2] After considering the evidence and arguments concerning the Suśrutasaṃhitā, Meulenbeld stated (IA, 348),
The Suśrutasaṃhitā is most probably the work of an unknown author who drew much of the material he incorporated in his treatise from a multiplicity of earlier sources from various periods. This may explain that many scholars yield to the temptation to recognize a number of distinct layers and, consequently, try to identify elements belonging to them. As we have seen, the identification of features thought to belong to a particular stratum is in many cases determined by preconceived ideas on the age of the strata and their supposed authors.
The dating of this work to 600 BCE was first proposed by Hoernle over a century ago,[146] but has long since been overturned by subsequent historical research. The current consensus amongst medical historians of South Asia is that the Suśrutasaṃhitā was compiled over a period of time starting with a kernel of medical ideas from the century or two BCE and then being revised by several hands into its present form by about 500 CE.[2][20] The view that the text was updated by the Buddhist scholar Nagarjuna in the 2nd century CE[147] has been disproved, although the last chapter of the work, the Uttaratantra, was added by an unknown later author before 500 CE.[2] Similar arguments apply to the Charaka Samhita, written by Charaka, and the Bhela Samhita, attributed to Atreya Punarvasu, that are also dated to the 6th century BCE by non-specialist scholars[148][149][150] but are in fact, in their present form, datable to a period between the second and fifth centuries CE.[2][20][11] The Charaka Samhita was also updated by Dridhabala during the early centuries of the Common Era.[151]

The Bower Manuscript (dated to the early 6th century CE[152]) includes of excerpts from the Bheda Samhita[153] and its description of concepts in Central Asian Buddhism. In 1987, A. F. R. Hoernle identified the scribe of the medical portions of the manuscript to be a native of India using a northern variant of the Gupta script, who had migrated and become a Buddhist monk in a monastery in Kucha. The Chinese pilgrim Fa Hsien (c. 337–422 CE) wrote about the healthcare system of the Gupta empire (320–550) and described the institutional approach of Indian medicine. This is also visible in the works of Charaka, who describes hospitals and how they should be equipped.[154]
Some dictionaries of materia medica include Astanga nighantu (8th century) by Vagbhata, Paryaya ratnamala (9th century) by Madhava, Siddhasara nighantu (9th century) by Ravi Gupta, Dravyavali (10th century), and Dravyaguna sangraha (11th century) by Chakrapani Datta, among others.[155][156]
Illnesses portrayed

Underwood and Rhodes state that the early forms of traditional Indian medicine identified fever, cough, consumption, diarrhea, dropsy, abscesses, seizures, tumours, and leprosy,[38] and that treatments included plastic surgery, lithotomy, tonsillectomy,[158] couching (a form of cataract surgery), puncturing to release fluids in the abdomen, extraction of foreign bodies, treatment of anal fistulas, treating fractures, amputations, cesarean sections,[Vagbhata 1][158][disputed ] and stitching of wounds.[38] The use of herbs and surgical instruments became widespread.[38] During this period, treatments were also prescribed for complex ailments, including angina pectoris, diabetes, hypertension, and stones.[160][161]
Further development and spread
Ayurveda flourished throughout the Indian Middle Ages. Dalhana (fl. 1200), Sarngadhara (fl. 1300) and Bhavamisra (fl. 1500) compiled works on Indian medicine.[162] The medical works of both Sushruta and Charaka were also translated into the Chinese language in the 5th century,[163] and during the 8th century, they were translated into the Arabic and Persian language.[164] The 9th-century Persian physician Muhammad ibn Zakariya al-Razi was familiar with the text.[165][166] The Arabic works derived from the ayurvedic texts eventually also reached Europe by the 12th century.[167][168] In Renaissance Italy, the Branca family of Sicily and Gaspare Tagliacozzi (Bologna) were influenced by the Arabic reception of the Sushruta's surgical techniques.[168]
British physicians traveled to India to observe rhinoplasty being performed using Indian methods, and reports on their rhinoplasty methods were published in the Gentleman's Magazine in 1794.[169] Instruments described in the Sushruta Samhita were further modified in Europe.[170] Joseph Constantine Carpue studied plastic surgery methods in India for 20 years and, in 1815, was able to perform the first major rhinoplasty surgery in the western world, using the "Indian" method of nose reconstruction.[171] In 1840 Brett published an article about this technique.[172]
The British had shown some interest in understanding local medicinal practices in the early nineteenth century. A Native Medical Institution was setup in 1822 where both indigenous and European medicine were taught. After the English Education Act 1835, their policy changed to champion European medicine and disparage local practices.[173] After Indian independence, there was more focus on ayurveda and other traditional medical systems. Ayurveda became a part of the Indian National healthcare system, with state hospitals for ayurveda established across the country. However, the treatments of traditional medicines were not always integrated with others.[76]
See also
Footnotes
- ^ Vāgbhaṭa's Aṣṭāṅgahṛdayasaṃhitā describes a procedure for the removal of a dead foetus from the womb of a living mother, and of a living child from the womb of a mother who has died (शारीरस्थान २, गर्भव्यापद्, २.२६-२७, २.५३).[159] Both these descriptions speak of removal of the fetus through the uterine passage, rather than from the front lower abdomen as with the caesarian section procedure. The earlier description of the Suśrutasaṃhitā (चिकित्सास्थान १५ "मूढगर्भ") is similar. A dead fetus is removed through the uterine passage and vagina. Although Suśruta does not describe removing a living child from a dead mother.
References
- ^ "Ayurveda". Oxford University Press. Archived from the original on 10 December 2016.
- ^ a b c d e f Meulenbeld, Gerrit Jan (1999). "Introduction". A History of Indian Medical Literature. Groningen: Egbert Forsten. ISBN 978-90-6980-124-7.
- ^ a b c d Dargan, Paul I.; Gawarammana, Indika B.; Archer, John R.H.; House, Ivan M.; Shaw, Debbie; Wood, David M. (2008). "Heavy metal poisoning from Ayurvedic traditional medicines: An emerging problem?". International Journal of Environment and Health. 2 (3/4): 463. CiteSeerX 10.1.1.561.9726. doi:10.1504/IJENVH.2008.020936.
- ^ a b "Weeklong programme to observe Health Day". The Himalayan Times. 28 October 2013. Archived from the original on 23 March 2017. Retrieved 7 January 2015.
In Nepal, 80 per cent of the population receives Ayurvedic medicine as first aid treatment.
- ^ a b Alam, Zulfeequar (2008). Herbal Medicines. New Delhi, India: A.P.H. Publishing. pp. 8–13, 122. ISBN 978-81-313-0358-0. Archived from the original on 7 September 2023. Retrieved 15 February 2022.
- ^ a b Beall, Jeffrey (2018). "Scientific soundness and the problem of predatory journals". In Kaufman, Allison B.; Kaufman, James C. (eds.). Pseudoscience: The Conspiracy Against Science. MIT Press. p. 293. ISBN 978-0-262-03742-6. Archived from the original on 7 September 2023. Retrieved 11 September 2020.
Ayurveda, a traditional Indian medicine, is the subject of more than a dozen, with some of these 'scholarly' journals devoted to Ayurveda alone ..., others to Ayurveda and some other pseudoscience. ... Most current Ayurveda research can be classified as 'tooth fairy science,' research that accepts as its premise something not scientifically known to exist. ... Ayurveda is a long-standing system of beliefs and traditions, but its claimed effects have not been scientifically proven. Most Ayurveda researchers might as well be studying the tooth fairy. The German publisher Wolters Kluwer bought the Indian open-access publisher Medknow in 2011....It acquired its entire fleet of journals, including those devoted to pseudoscience topics such as An International Quarterly Journal of Research in Ayurveda.
- ^ a b c Semple D, Smyth R (2019). "Chapter 1: Thinking about psychiatry". Oxford Handbook of Psychiatry (4th ed.). Oxford University Press. p. 24. doi:10.1093/med/9780198795551.003.0001. ISBN 978-0-19-879555-1. Archived from the original on 7 September 2023. Retrieved 3 July 2020.
These pseudoscientific theories may ... confuse metaphysical with empirical claims (e.g. ... Ayurvedic medicine)
(subscription required) - ^ a b c Quack, Johannes (2011). Disenchanting India: Organized Rationalism and Criticism of Religion in India. Oxford University Press. pp. 213, 3. ISBN 978-0-19-981260-8. Archived from the original on 7 September 2023. Retrieved 6 February 2022.
ordinary members told me how they practice some of these pseudosciences, either privately or as certified doctors themselves, most often Ayurveda.
- ^ a b Miller, Kelli (20 March 2021). "What Is Ayurveda?". WebMD. Medically Reviewed by Melinda Ratini. Archived from the original on 4 July 2020. Retrieved 16 August 2020.
- ^ a b c d "Ayurvedic medicine". Cancer Research UK. Archived from the original on 24 November 2020. Retrieved 18 April 2022.
There is no scientific evidence to prove that Ayurvedic medicine can treat or cure cancer. Researchers have found that some Ayurvedic treatments can help relieve cancer symptoms. It can also improve quality of life.
- ^ a b Wujastyk 2003a.
- ^ Mukhopadhyaya, Girindranath (1913). The Surgical Instruments of the Hindus, with a Comparative Study of the Surgical Instruments of the Greek, Roman, Arab, and the Modern European Surgeons. Calcutta: Calcutta University. Retrieved 16 October 2015.
- ^ Zysk, Kenneth G. (1999). "Mythology and the Brāhmaṇization of Indian medicine: Transforming Heterodoxy into Orthodoxy". In Josephson, Folke (ed.). Categorisation and Interpretation. Meijerbergs institut för svensk etymologisk forskning, Göteborgs universitet. pp. 125–145. ISBN 978-91-630-7978-8.
- ^ Bhishagratna, Kaviraj Kunjalal (1907). An English Translation of the Sushruta Samhita Based on Original Sanskrit text. Calcutta: K. K. Bhishagratna. p. 1. Retrieved 16 October 2015.
- ^ a b "Dhanvantari. (2010). In Encyclopædia Britannica. Retrieved 4 August 2010, from Encyclopædia Britannica Online". Archived from the original on 27 April 2015. Retrieved 2 June 2022.
- ^ Birch, Jason; Wujastyk, Dominik; Klebanov, Andrey; Parameswaran, Madhu; Rimal, Madhusudan; Chakraborty, Deepro; Bhatt, Harshal; Shenoy, Devyani; Lele, Vandana (2021). "Further Insight into the Role of Dhanvantari, the physician to the gods, in the Suśrutasaṃhitā". Academia Letters. doi:10.20935/al2992. S2CID 238681626. Archived from the original on 15 April 2023. Retrieved 2 May 2022.
- ^ a b Wujastyk, Dagmar; Smith, Frederick M. (9 September 2013). Modern and Global Ayurveda: Pluralism and Paradigms. SUNY Press. ISBN 978-0-7914-7816-5. Archived from the original on 7 September 2023. Retrieved 10 March 2022.
- ^ Meulenbeld, G. Jan (1999–2000). A history of Indian medical literature. Groningen: Egbert Forsten; Brill. pp. passim. ISBN 90-6980-124-8. OCLC 42207455.
- ^ a b c d Wujastyk 2003a, p. xviii
- ^ a b c Sharma, Priya Vrat (1992). History of Medicine in India. New Delhi: Indian National Science Academy.
- ^ a b Bhalla, A; Pannu, A K (15 January 2022). "Are Ayurvedic medications store house of heavy metals?" (PDF). Toxicology Research. 11 (1). Oxford University Press (published February 2022): 179–183. PMID 35237422.
- ^ a b c d e Saper RB; Phillips RS; et al. (2008). "Lead, mercury, and arsenic in US- and Indian-manufactured medicines sold via the internet". JAMA. 300 (8): 915–923. doi:10.1001/jama.300.8.915. PMC 2755247. PMID 18728265.
- ^ a b c d e Maas, Philipp A. (2018). "27. Indian Medicine and Ayurveda". In Jones, Alexander; Taub, Liba (eds.). The Cambridge History of Science: Volume 1, Ancient Science. Cambridge University Press. pp. 532–550. doi:10.1017/9780511980145.029. ISBN 978-1-108-68262-6. S2CID 209267391. Archived from the original on 7 September 2023. Retrieved 24 April 2022.
- ^ a b c d e Smith, Frederick M.; Wujastyk, Dagmar (2008). "Introduction". In Smith, Frederick M.; Wujastyk, Dagmar (eds.). Modern and Global Ayurveda: Pluralism and Paradigms. New York: SUNY Press. pp. 1–28. ISBN 978-0-7914-7816-5. OCLC 244771011. Archived from the original on 7 September 2023. Retrieved 10 March 2022.
- ^ a b Fields, Gregory P. (2001). Religious Therapeutics: Body and Health in Yoga, Ayurveda, and Tantra. SUNY Press. p. 36. ISBN 978-0-7914-4915-8. Archived from the original on 7 September 2023. Retrieved 10 March 2022.
- ^ Clifford, Terry; Chandra, Lokesh (2017). Tibetan Buddhist Medicine and Psychiatry. Archived 8 May 2023 at the Wayback Machine 42. Motilal Banarsidass Publications. ISBN 978-8120812055.
- ^ Ācārya, Yādava Trivikramātmaja, ed. (1945). "Sūtrasthāna 1.7–9". Suśrutasaṃhitā. Bombay: Nirṇayasāgara Press. pp. 2–3.
- ^ Ācārya, Yādava Trivikramātmaja, ed. (1941). "Sūtrasthāna 30.28". The Carakasaṃhitā of Caraka, with the commentary by Cakrapāṇidatta, edited by Yadavaśarman Trivikarama Ācārya. Bombay: Nirṇayasāgara Press. p. 189.
- ^ Wujastyk, Dominik (2003b). "Indian Medicine". In Flood, Gavin (ed.). The Blackwell Companion to Hinduism. Oxford: Blackwell. p. 394. ISBN 978-1-4051-3251-0.
- ^ Sharma, Priya Vrat (1999). Suśruta-Samhitā With English Translation of text…. Vol. 1. Varanasi: Chaukhambha Visvabharati. pp. 7–11.[need quotation to verify]
- ^ Bhishagratna, Kaviraj Kunja Lal (1907). An English Translation of the Sushruta Samhita Based on Original Sanskrit Text. Vol. 1. Calcutta: The Author. pp. 2–6.
- ^ Swami Sadashiva Tirtha (1998). The Ãyurveda Encyclopedia: Natural Secrets to Healing, Prevention & Longevity. Ayurveda Holistic Center Press. ISBN 0-9658042-2-4.
- ^ Comba, Antonella (2001). "Carakasaṃhitā, Śārīrasthāna~I and Vaiśeṣika Philosophy". In Meulenbeld, Gerrit Jan; Wujastyk, Dominik (eds.). Studies on Indian Medical History. Delhi: Motilal Banarsidass. pp. 39–55. ISBN 978-8120817685. Archived from the original on 7 September 2023. Retrieved 9 April 2022.
- ^ Basham, A. L. (1976). "The Practice of Medicine in Ancient and Medieval India". In Leslie, Charles (ed.). Asian Medical Systems. Berkeley: University of California Press. pp. 18–43. doi:10.1525/9780520322295-005. ISBN 978-0-520-32229-5. Archived from the original on 1 March 2022. Retrieved 1 March 2022.
- ^ Pathak, Namyata; Raut, Ashwinikumar; Vaidya, Ashok (1 October 2008). "Acute cervical pain syndrome resulting from suppressed sneezing". The Journal of the Association of Physicians of India. 56: 728–9.
- ^ Chopra 2003, p. 75
- ^ a b c d e Mishra, Lakshmi-chandra; Singh, Betsy B.; Dagenais, Simon (March 2001). "Ayurveda: a historical perspective and principles of the traditional healthcare system in India". Alternative Therapies in Health and Medicine. 42 (2): 36–42. PMID 11253415.
- ^ a b c d e f g h i Underwood & Rhodes (2008)
- ^ a b c Chopra 2003, p. 76, citing Sushrutasamhita 25.36.
- ^ Novella S (21 November 2019). "Ayurvedic practitioners push for licensing in Colorado". Science-Based Medicine. Archived from the original on 27 March 2022. Retrieved 27 March 2022.
- ^ Payyappallimana, Unnikrishnan; Venkatasubramanian, Padma (31 March 2016). "Exploring Ayurvedic Knowledge on Food and Health for Providing Innovative Solutions to Contemporary Healthcare". Frontiers in Public Health. 4 (57): 57. doi:10.3389/fpubh.2016.00057. PMC 4815005. PMID 27066472.
- ^ Shilpa, S; Venkatesha Murthy, C.G. (January 2011). "Understanding personality from Ayurvedic perspective for psychological assessment: A case". AYU. 32 (1). Institute for Post Graduate Teaching & Research in Ayurveda: 12–19. doi:10.4103/0974-8520.85716. PMC 3215408. PMID 22131752.
- ^ a b Ramu, M.G.; Venkataram, B.S. (January 1985). "Manovikara (mental disorders) in Ayurveda". Ancient Science of Life. 4 (3). Wolters Kluwer Medknow Publications: 165–73. PMC 3331508. PMID 22557473.
- ^ Bhagwan Dash, Vaidya (1995). Fundamentals of Ayurvedic Medicine. Lotus Press. ISBN 978-81-220-0117-4.
- ^ "Ayurvedic & Western approaches to the treatment of Schizophrenia". ayurvedacollege.com. 21 September 2009. Archived from the original on 8 July 2020. Retrieved 6 July 2020.
- ^ Acharya, YT (1941). Charaka samhita. Commentary of Chakrapani. Bombay: Nirnayasagar Press.
- ^ Kacera, Walter (2007). "Ama and Disease". Ayurvedic Tongue Diagnosis. Lotus Press. pp. 159–176. ISBN 978-0-940985-77-3.
- ^ Amruthesh, Sunita (1 January 2008). "Dentistry and Ayurveda – IV: Classification and management of common oral diseases". Indian Journal of Dental Research. 19 (1): 52–61. doi:10.4103/0970-9290.38933. PMID 18245925.
- ^ Amruthesh, Sunita (2007). "Dentistry and Ayurveda-III (basics – ama, immunity, ojas, rasas, etiopathogenesis and prevention)". Indian Journal of Dental Research. 18 (3): 112–9. doi:10.4103/0970-9290.33786. PMID 17687173.
- ^ Madhusūdanasarasvatī (1912). प्रस्थानभेदः श्रीमधुसूदनसरस्वत्या विरचितः (in Sanskrit). श्रीरङ्गम्: श्रीवाणिविलासमुद्रायन्त्रालय. p. 14. Retrieved 16 October 2015.
- ^ Zysk, Kenneth G. (2010). Medicine in the Veda: Religious Healing in the Veda with Translations and Annotations of Medical Hymns from the Rgveda and the Atharvaveda and Renderings from the Corresponding Ritual Texts. New Delhi: Motilal Banarsidass. ISBN 978-81-208-1401-1.
- ^ Sengupta, Pradip Kumar (2012). History of Science and Philosophy of Science: A Philosophical Perspective of the Logic of Ideas in Science. Longman. p. 486. ISBN 978-81-317-1931-2. Archived from the original on 7 September 2023. Retrieved 25 October 2021.
Sometimes Ayurveda is also considered as the fifth Veda or Pañcama Veda.
- ^ Zysk, Kenneth G. (1998). Asceticism and Healing in Ancient India: Medicine in the Buddhist Monastery. Indian Medical Tradition. Vol. 2. Delhi: Motilal Banarsidass Publishers. ISBN 978-81-208-1507-0. Archived from the original on 7 September 2023. Retrieved 28 February 2022.
- ^ Cornelissen, R. M. Matthijs; Misra, Girishwar; Varma, Suneet, eds. (2013). "The blending of healing and pedagogy in Āyurveda". Foundations and Applications of Indian Psychology (2nd ed.). New Delhi: Pearson Education India. ISBN 9789-332537460. OCLC 987023188.
Central to Āyurvedic healing is the notion of the human persona as a three-dimensional composite of body, mind and self. Āyurveda aims to empower the body to invigorate the mind and, consequently, to use the invigorated mind to generate self-awareness.
- ^ Wujastyk 2003a, pp. xix–xx
- ^ Mishra, Lakshmi-chandra; Singh, Betsy B.; Dagenais, Simon (2001). "Healthcare and disease management in Ayurveda". Alternative Therapies in Health and Medicine. 7 (2): 44–50. PMID 11253416.
- ^ Chopra 2003, p. 79
- ^ a b "Ayurveda". Encarta. Redmond, WA: Microsoft. 2008. Archived from the original on 28 October 2009.
- ^ a b Kumar, Syal; Dobos, Gustav J.; Rampp, Thomas (July 2017). "The Significance of Ayurvedic Medicinal Plants". Journal of Evidence-Based Complementary & Alternative Medicine. 22 (3): 494–501. doi:10.1177/2156587216671392. ISSN 2156-5872. PMC 5871155. PMID 27707902.
- ^ Pharmacographia Indica Archived 5 July 2017 at the Wayback Machine, A history of principal drugs of vegetable origin in British India – Volume 1, William Dymock et al. (1890), London
- ^ O'mathuna, Donal (12 April 2011). "Does it work? Can triphala act as an antimicrobial?". The Irish Times. Archived from the original on 7 July 2022. Retrieved 1 March 2022.
- ^ Berry, Jennifer (3 October 2019). "What are the benefits of triphala? Uses, evidence, and risks". Medical News Today. Medically reviewed by Zara Risoldi Cochrane. Archived from the original on 1 March 2022. Retrieved 1 March 2022.
- ^ Peterson, Christine Tara; Denniston, Kate; Chopra, Deepak (1 August 2017). "Therapeutic Uses of Triphala in Ayurvedic Medicine". Journal of Alternative and Complementary Medicine. 23 (8): 607–614. doi:10.1089/acm.2017.0083. ISSN 1075-5535. PMC 5567597. PMID 28696777.
- ^ Goldman, Rena (29 September 2020). "What are the benefits of ashwagandha?". Medical News Today. Medically reviewed by Debra Rose Wilson. Archived from the original on 15 March 2022. Retrieved 15 March 2022.
- ^ Ng, P.K.L.; Corlett, R.; Tan, H.T.W.; Raffles Museum of Biodiversity Research (2011). Singapore Biodiversity: An Encyclopedia of the Natural Environment and Sustainable Development. Editions Didier Millet. p. 164. ISBN 978-981-4260-08-4.
- ^ a b c Sekar, S. (2007). "Traditional alcoholic beverages from Ayurveda and their role on human health". Indian Journal of Traditional Knowledge. 6 (1): 144–149. Archived from the original on 18 December 2014.
- ^ a b Mani, Dayanandan; Dhawan, Sunita S. (2011). "Scientific basis of therapeutic uses of opium poppy (Papaver somniferum) in Ayurveda". Acta Horticulturae (International Symposium on Papaver) (1036): 175–180. Archived from the original on 12 January 2015. Retrieved 7 December 2014.
- ^ a b Ram Nath Chopra; I. C. Chopra (1 January 1955). "UNODC – Bulletin on Narcotics – 1955 Issue 3 – 001". Archived from the original on 5 January 2016. Retrieved 27 December 2015.
- ^ a b c d e f Chaturvedi, G. N.; Tiwari, S. K.; Rai, N. P. (May 1981). "Medicinal Use of Opium and Cannabis in Medieval India" (PDF). Indian Journal of History of Science. 16 (1): 31–35. Archived from the original (PDF) on 28 October 2014. Retrieved 28 October 2014.
- ^ Chopra 2003, p. 80
- ^ Satake, Alison; McDaniel, Andi. "Frontline World India: A Second Opinion: Ayurveda 101". PBS. Archived from the original on 26 October 2021. Retrieved 24 April 2022.
- ^ Wujastyk 2003a, p. 20
- ^ Cacho, V.; Lum, E. (2021). Integrative Sleep Medicine. Weil Integrative Medicine Library. Oxford University Press. p. 296. ISBN 978-0-19-088542-7. Archived from the original on 10 July 2023. Retrieved 10 July 2023.
Shirodhara massage is an Ayurvedic oil- dripping treatment that is often used to treat sleep problems. It consists of pouring a gentle stream of warm oil (sesame or herbal oil) over the forehead
- ^ Ajanal, M; Nayak, S; Prasad, BS; Kadam, A (December 2013). "Adverse drug reaction and concepts of drug safety in Ayurveda: An overview". Journal of Young Pharmacists. 5 (4): 116–120. doi:10.1016/j.jyp.2013.10.001. PMC 3930110. PMID 24563588.
- ^ a b Sujatha, V. (January 2020). "The Universal and the Global: Contextualising European Ayurvedic Practices". Society and Culture in South Asia. 6 (1): 52–73. doi:10.1177/2393861719883067. ISSN 2393-8617. S2CID 213828818. Archived from the original on 15 April 2023. Retrieved 25 March 2022 – via Sage.
- ^ a b c Xiaorui Zhang (2001). "Legal Status of Traditional Medicine and Complementary/Alternative Medicine: A Worldwide Review". World Health Organization (WHO). Archived from the original on 31 August 2009. Retrieved 24 June 2014.
- ^ Warrier, Maya (January 2009). "Seekership, Spirituality and Self-Discovery: Ayurveda Trainees in Britain". Asian Medicine. 4 (2): 423–451. doi:10.1163/157342009X12526658783691. ISSN 1573-420X. PMC 2898496. PMID 20617123.
- ^ Sriram, Veena; Keshri, Vikash R.; Kumbhar, Kiran (18 August 2021). "The impact of colonial-era policies on health workforce regulation in India: lessons for contemporary reform". Human Resources for Health. 19 (1): 100. doi:10.1186/s12960-021-00640-w. ISSN 1478-4491. PMC 8371885. PMID 34407831.
Traditional practitioners of medicine were at the mercy of the 'newly' imposed system of modern medicine that arrived with colonialism. Despite some early efforts to understand the value of traditional medicine and some efforts at exchange between the systems, "British criticisms of indigenous medicine became increasingly strident and intolerant".
- ^ "Global Ayurvedic Market". Industry Research. 8 April 2019. Archived from the original on 15 April 2023. Retrieved 27 March 2022.
- ^ a b Bhowmick, Nilanjana (2 June 2021). "Indian doctors protest herbal treatments being touted for COVID-19". National Geographic. Archived from the original on 21 March 2022. Retrieved 21 March 2022.
- ^ Rudra, Shalini; Kalra, Aakshi; Kumar, Abhishek; Joe, William (2017). "Utilization of alternative systems of medicine as health care services in India: Evidence on AYUSH care from NSS 2014". PLOS ONE. 12 (5): e0176916. Bibcode:2017PLoSO..1276916R. doi:10.1371/journal.pone.0176916. PMC 5417584. PMID 28472197.
- ^ a b Wujastyk 2003a, p. XXII
- ^ "Introduction to Central Council of Indian Medicine". Central Council of Indian Medicine (CCIM). Archived from the original on 18 December 2014.
- ^ Wujastyk 2003a, p. XVI
- ^ "Welcome to Central Council for Research in Ayurveda and Siddha (India)". Ccras.nic.in. Archived from the original on 28 July 2011. Retrieved 21 June 2012.
- ^ "About TKDL". Traditional Knowledge Digital Library. Archived from the original on 4 July 2014.
- ^ "Know Instances of Patenting on the UES of Medicinal Plants in India". PIB, Ministry of Environment and Forests. 6 May 2010. Archived from the original on 10 May 2010. Retrieved 22 May 2010.
- ^ "Source of Information". Traditional Knowledge Digital Library (Government of India). Archived from the original on 13 June 2010. Retrieved 25 May 2010.
- ^ Valiathan, M. S. "Towards Ayurvedic Biology" (PDF). Indian Academy of Sciences. Archived from the original (PDF) on 13 May 2015. Retrieved 13 June 2015.
- ^ Roy, Shobha (28 March 2012). "Insurers stepping up cover for ayurveda treatment". The Hindu. Archived from the original on 11 December 2013. Retrieved 13 June 2015.
- ^ "Prime Minister's Yoga Awards on International Day of Yoga 2021". The Statesman. 1 April 2021. Archived from the original on 13 February 2022. Retrieved 12 February 2022.
- ^ "Modi allocates 'AYUSH' department to MoS". India TV News. 10 November 2014. Archived from the original on 13 February 2022. Retrieved 13 February 2022.
- ^ "National Ayurveda Day – Vikaspedia". vikaspedia.in. Archived from the original on 20 December 2018. Retrieved 20 December 2018.
- ^ a b c Bansal, Samarth (18 July 2016). "WHO report sounds alarm on 'doctors' in India". The Hindu. ISSN 0971-751X. Archived from the original on 6 February 2022. Retrieved 6 February 2022.
- ^ Anand, Sudhir; Fan, Victoria (2016). "The Health Workforce in India" (PDF). World Health Organization. Archived (PDF) from the original on 28 March 2022. Retrieved 13 February 2022.
- ^ Guneratne, Arjun (2009). Culture and the Environment in the Himalaya. Routledge contemporary South Asia series, #24. New York: Routledge. pp. 84–85. ISBN 978-0-415-77883-1. Archived from the original on 7 September 2023. Retrieved 23 March 2022.
- ^ "Ministry of Indigenous Medicine". Archived from the original on 14 December 2012. Retrieved 2 December 2012.
- ^ "Institute of indigenous Medicine". Iim.cmb.ac.lk. Archived from the original on 16 June 2012. Retrieved 21 June 2012.
- ^ "Statistics Report" (PDF). Sri Lanka Institute of Indigenous Medicine. November 2011. Archived from the original (PDF) on 24 April 2012.
- ^ "About Us". The Ministry of Indigenous Medicine (Sri Lanka). 14 February 1980. Archived from the original on 8 November 2011. Retrieved 11 December 2011.
- ^ Aluvihare, Arjuna (November 1993). "Rohal Kramaya Lovata Dhayadha Kale Sri Lankikayo". Vidhusara Science Magazine.
- ^ Rannan-Eliya, Ravi P.; De Mel, Nishan (February 1997). "Resource Mobilization in Sri Lanka's Health Sector" (PDF). Harvard School of Public Health & Health Policy Programme, Institute of Policy Studies. p. 19. Archived (PDF) from the original on 7 July 2017. Retrieved 17 December 2014.
- ^ Müller-Dietz, Heinz E. (1975). "Die Krankenhaus-ruinen in Mihintale (Ceylon)". Historia Hospitalium. 10: 65–71. PMID 11627253.
- ^ a b Skolnick, Andrew A. (1991). "The Maharishi Caper: Or How to Hoodwink Top Medical Journals". ScienceWriters: The Newsletter of the National Association of Science Writers (Fall). Archived from the original (print) on 16 July 2008. Retrieved 23 January 2016.
From time to time, even the most prestigious science journals publish erroneous or fraudulent data, unjustified conclusions, and sometimes balderdash. Balderdash was the right word when The Journal of the American Medical Association (JAMA) published the article, 'Maharishi Ayur-Veda: Modern Insights Into Ancient Medicine,' in its 22/29 May issue. Discovering that they had been deceived by the article's authors, the editors published a correction in the 14 August issue, which was followed on 2 October by a six-page exposé on the people who had hoodwinked them.
- ^ Skolnick, Andrew A. (1991). "Maharishi Ayur-Veda: Guru's marketing scheme promises the world eternal 'perfect health'". JAMA. 266 (13): 1741–2, 1744–5, 1749–50. doi:10.1001/jama.1991.03470130017003. PMID 1817475.
- ^ "National Policy on Traditional Medicine and Regulation of Herbal Medicines" (PDF). World Health Organization. May 2005. Archived from the original (PDF) on 27 September 2009.
- ^ Jones, Constance; Ryan, James D. (2006). Melton, J. Gordon (ed.). Encyclopedia of Hinduism. Encyclopedia of World Religions. Infobase Publishing. p. 179. ISBN 978-0-8160-7564-5. Archived from the original on 7 September 2023. Retrieved 23 March 2022.
- ^ Khalsa, Karta Purkh Singh; Tierra, Michael (2008). The Way of Ayurvedic Herbs: The Most Complete Guide to Natural Healing and Health with Traditional Ayurvedic Herbalism. Lotus Press. pp. x. ISBN 978-0-940985-98-8. Archived from the original on 7 September 2023. Retrieved 23 March 2022.
Independently, we both first learned Ayurvedic medicine from our respective spiritual mentors – myself with Baba Hari Dass and K.P., with Yogi Bhajan.
- ^ a b "Ayurvedic Medicine: In Depth". National Center for Complementary and Integrative Health. December 2018. Archived from the original on 13 August 2020. Retrieved 23 August 2020.
- ^ Wujastyk, Dagmar; Smith, Frederick M. (9 September 2013). Modern and Global Ayurveda: Pluralism and Paradigms. SUNY Press. p. 285. ISBN 978-0-7914-7816-5. Archived from the original on 7 September 2023. Retrieved 10 March 2022.
- ^ Chandrasekhar, Anand (4 June 2017). "Ayurveda seeks respectability through Swiss diploma". SWI. Archived from the original on 16 March 2022. Retrieved 16 March 2022.
- ^ Sujatha, V (July 2011). "What could 'integrative' medicine mean? Social science perspectives on contemporary Ayurveda". Journal of Ayurveda and Integrative Medicine. 2 (3): 115–23. doi:10.4103/0975-9476.85549. PMC 3193682. PMID 22022153.
- ^ Manohar, PR (April 2013). "Uniform standards and quality control of research publications in the field of Ayurveda". Ancient Science of Life. 32 (4): 185–6. doi:10.4103/0257-7941.131968. PMC 4078466. PMID 24991064.
- ^ Bausell, R. Barker (2007). Snake Oil Science: The Truth About Complementary and Alternative Medicine. Oxford University Press. p. 259. ISBN 978-0-19-538342-3.
- ^ "Ayurveda". American Cancer Society. 26 August 2011. Archived from the original on 22 February 2014. Retrieved 7 January 2015.
The effectiveness of Ayurveda has not been proven in scientific studies, but early research suggests that certain herbs may offer potential therapeutic value ... Although Ayurveda has been largely untested by Western researchers, there is a growing interest in integrating some parts of the system into medical practice. In fact, a few of the herbs and substances have been purified into drugs that are used (along with other medicines) to treat cancer. Early studies suggest that other parts of Ayurveda may have potential therapeutic value.
- ^ Patwardhan, Bhushan (1 November 2014). "Bridging Ayurveda with evidence-based scientific approaches in medicine". The EPMA Journal. 5 (1): 19. doi:10.1186/1878-5085-5-19. ISSN 1878-5077. PMC 4230501. PMID 25395997.
- ^ Mamtani, R.; Mamtani, R. (2005). "Ayurveda and Yoga in Cardiovascular Diseases". Cardiology in Review. 13 (3): 155–162. doi:10.1097/01.crd.0000128730.31658.36. PMID 15834238. S2CID 27195105.
- ^ "Research in Ayurveda – About CCRAS". Central Council for Research in Ayurveda and Siddha. Department of AYUSH, Ministry of Health and Family Welfare. Archived from the original on 30 May 2014.
- ^ "China hands over Ayurveda research centre to govt". Kantipur Publications. The Kathmandu Post. Archived from the original on 21 January 2015. Retrieved 7 January 2015.
The centre will play a positive role in promotion and utilisation of Ayurveda in the country, by conducting research on medicinal herbs available here.
- ^ "Part I: Section (I) — General Government Notifications The Constitution of the Democratic Socialist Republic of Sri Lanka Notification" (PDF). The Gazette of the Democratic Socialist Republic of Sri Lanka Extraordinary. 1933/13. Colombo, Sri Lanka. 21 September 2015. Archived (PDF) from the original on 19 January 2022. Retrieved 25 March 2022.
- ^ Urmila, T.; Supriya, B. (2008). "Pharmacovigilance of ayurvedic medicines in India". Indian Journal of Pharmacology. 40 (S1): 10–12. Archived from the original on 30 March 2009. Retrieved 15 January 2009.
- ^ a b Ernst, Edzard (2002). "Heavy metals in traditional Indian remedies". European Journal of Clinical Pharmacology. 57 (12): 891–896. doi:10.1007/s00228-001-0400-y. ISSN 0031-6970. PMID 11936709. S2CID 1698767.
- ^ Karri, Surya K.; Saper, Robert B.; Kales, Stefanos N. (January 2008). "Lead Encephalopathy Due to Traditional Medicines". Current Drug Safety. 3 (1): 54–59. doi:10.2174/157488608783333907. ISSN 1574-8863. PMC 2538609. PMID 18690981.
- ^ Saper, R. B.; Kales SN; Paquin, J; et al. (2004). "Heavy metal content of ayurveda herbal medicine products". Journal of the American Medical Association. 292 (23): 2868–73. doi:10.1001/jama.292.23.2868. PMID 15598918. S2CID 9914911.
- ^ a b Ellin, Abby (17 September 2008). "Skin deep: ancient, but how safe?". The New York Times. Archived from the original on 30 April 2011. Retrieved 19 September 2008.
A report in the August 27 [2008] issue of The Journal of the American Medical Association found that nearly 21 percent of 193 ayurvedic herbal supplements bought online, produced in both India and the United States, contained lead, mercury or arsenic.
- ^ Szabo, Liz (26 August 2008). "Study finds toxins in some herbal medicines". USA Today. Archived from the original on 8 October 2012.
- ^ Hall, Harriet (14 December 2017). "Ayurveda: Ancient Superstition, Not Ancient Wisdom". Skeptical Inquirer. Archived from the original on 14 December 2017. Retrieved 1 February 2018.
- ^ Breeher L, Mikulski MA, Czeczok T, Leinenkugel K, Fuortes LJ (6 April 2015). "A cluster of lead poisoning among consumers of Ayurvedic medicine". International Journal of Occupational and Environmental Health. 21 (4): 303–307. doi:10.1179/2049396715Y.0000000009. PMC 4727589. PMID 25843124.
- ^ CCRAS. "Guidelines for toxicity / safety profile evaluation of Ayurveda & Siddha plant drugs". CCRAS Guidelines. Archived from the original on 11 March 2013.
- ^ a b Katiyar, C. K. (2006). "Safety Aspects of Ayurveda" (PDF). Ranbaxy Research Laboratories. Archived (PDF) from the original on 2 February 2017. Retrieved 25 January 2017.
- ^ Saper RB; Phillips RS; Sehgal A (August 2008). "Lead, mercury, and arsenic in US- and Indian-manufactured ayurvedic medicines sold via the internet". JAMA. 300 (8): 915–923. doi:10.1001/jama.300.8.915. PMC 2755247. PMID 18728265.
- ^ "Ayurveda linked to lead poisoning in US women". The Financial Express (Washington ed.). 24 August 2012. Archived from the original on 9 December 2014.
- ^ a b Valiathan, MS (2006). "Ayurveda: putting the house in order" (PDF). Current Science. 90 (1): 5–6. Archived (PDF) from the original on 9 October 2022. Retrieved 27 October 2013.
- ^ "Use caution with Ayurvedic products". US FDA. Archived from the original on 23 April 2019. Retrieved 17 December 2014.
- ^ Kamath, Sushant U.; Pemiah, Brindha; Sekar, Rajan K.; Krishnaswamy, Sridharan; Sethuraman, Swaminathan; Krishnan, Uma Maheswari (1 June 2012). "Mercury-based traditional herbo-metallic preparations: a toxicological perspective". Archives of Toxicology. 86 (6): 831–838. doi:10.1007/s00204-012-0826-2. ISSN 1432-0738. PMID 22441626. S2CID 13947298.
- ^ Ṭhākara, Vināyaka Jayānanda (1989). Methodology of Research in Ayurveda. Jamnagar, India: Gujarat Ayurved University Press. p. 7.
- ^ Leslie, Charles, ed. (1976). Asian Medical Systems. Berkeley: University of California Press. pp. passim. ISBN 978-0-520-03511-9. Archived from the original on 7 September 2023. Retrieved 10 March 2022.
- ^ Taylor, Carl (1977). "The Place of Indigenous Medical Practitioners in the Modernization of Health Services". In Leslie, Charles (ed.). Asian Medical Systems. University of California Press. pp. 285–292. ISBN 978-0-520-03511-9. Archived from the original on 7 September 2023. Retrieved 1 March 2022.
- ^ Leslie, Charles (1976). "The Ambiguities of Medical Revivalism in Modern India". The Ambiguites of Medical Revivalism in Modern India. University of California Press. pp. 356–367. doi:10.1525/9780520322295-022. ISBN 978-0-520-32229-5. Archived from the original on 7 September 2023. Retrieved 1 March 2022.
{{cite book}}:|work=ignored (help) - ^ Sharma, Shiv (1975). Ayurvedic Medicine: Past and Present. Calcutta: Dabur (S. K. Burman).
- ^ Berger, Rachel (2013). Ayurveda Made Modern: Political Histories of Indigenous Medicine in North India, 1900–1955. New York, NY: Palgrave Macmillan. doi:10.1057/9781137315908. ISBN 978-0-230-28455-5. Archived from the original on 1 March 2022. Retrieved 1 March 2022.
- ^ Wujastyk, Dominik (2008). "The Evolution of Indian Government Policy on Ayurveda in the Twentieth Century". Modern and Global Ayurveda: Pluralism and Paradigms. SUNY Press. pp. 43–76. doi:10.7939/r3-xjj8-cg73. ISBN 978-0-7914-7490-7. Archived from the original on 7 September 2023. Retrieved 1 March 2022.
- ^ Wujastyk, Dominik (2005). "Policy Formation and Debate Concerning the Government Regulation of Ayurveda in Great Britain in the 21st Century" (PDF). Asian Medicine. 1: 162–184. doi:10.1163/157342105777996719. S2CID 71229532. Archived (PDF) from the original on 22 September 2017. Retrieved 28 January 2019.
- ^ Redy, Sita (2002). "Asian Medicine in America: The Ayurvedic Case". Annals of the American Academy of Political and Social Science. 583: 97–121. doi:10.1177/000271620258300107. JSTOR 1049691. S2CID 145626093.
- ^ Meulenbeld, G. Jan (1999–2000). A history of Indian medical literature. Vol. IA. Groningen. pp. 689–699. ISBN 90-6980-124-8. OCLC 42207455.
{{cite book}}: CS1 maint: location missing publisher (link) - ^ Hoernle, A. F. Rudolf (1907). Osteology or the bones of the human body. Oxford: Clarendon P. OCLC 28563136.
- ^ J. N. Roy; Braja Bihārī Kumāra. India and Central Asia: Classical to Contemporary Periods. Concept Publishing Company. p. 103.
- ^ Leonore Loeb Adler; B. Runi Mukherji. Spirit Versus Scalpel: Traditional Healing and Modern Psychotherapy. Greenwood. p. 76.
- ^ Saxena, Praveen K. Development of Plant-Based Medicines: Conservation, Efficacy and Safety. Springer. p. 48.
- ^ Mohammad Ali Jazayery; Winter, Werner (1988). Languages and Cultures: Studies in Honor of Edgar C. Polomé. Walter de Gruyter. p. 116. ISBN 978-3-11-010204-8.
- ^ Glucklich, Ariel (2008). The Strides of Vishnu: Hindu Culture in Historical Perspective. Oxford, England: Oxford University Press. p. 141. ISBN 978-0-19-531405-2.
- ^ Sander, Lore (1987). "Origin and Date of the {Bower Manuscript}, a New Approach" in Investigating Indian Art: Proceedings of a Symposium on the Development of Early Buddhist and Hindu Iconography Held at the Museum of Indian Art, Berlin, in May 1986. Berlin: Museum Fuer Indische Kunst. pp. 313–323.
- ^ Chattopadhyaya, Debiprasad (1991). History of Science and Technology in Ancient India: Formation of the theoretical fundamentals of natural science. p. 153.
- ^ Singh, Upinder (2008). A History of Ancient and Early Medieval India: From the Stone Age to the 12th Century. Pearson. ISBN 978-81-317-1120-0.
- ^ Vaidya Bhagwan Dash. Materia Medica of Ayurveda: Based on: Madanapala's Nighantu. B. Jain Publishers. p. 14.
- ^ AYUSH. "e-Nighantu". Archived from the original on 2 March 2022. Retrieved 2 May 2022.
- ^ Finger, p. 66
- ^ a b Magner, Lois N. (2002). A History of the Life Sciences, Revised and Expanded. CRC Press. p. 6. ISBN 978-0-8247-0824-5. Retrieved 26 December 2016.
- ^ Vāgbhaṭa (1939). Ashtanga Hridaya. Retrieved 2 January 2017 – via archive.org.
- ^ Dwivedi, Girish; Dwivedi, Shridhar (2007). "History of Medicine: Sushruta – the Clinician – Teacher par Excellence" (PDF). Indian Journal of Chest Diseases and Allied Sciences. 49: 243–244. Archived from the original (PDF) on 10 October 2008. (Republished by National Informatics Centre, Government of India.)
- ^ Lock et al., p. 836
- ^ Wujastyk 2003a, p. XXVI
- ^ Wujastyk, Dagmar (2002). Well-Mannered Medicine: Medical Ethics and Etiquette in Classical Ayurveda. Oxford University Press. ISBN 978-0-19-985627-5. Archived from the original on 7 September 2023. Retrieved 8 November 2020.
- ^ Encyclopaedia of the History of Science, Technology, and Medicine in Non-Western Cultures. Springer. 2008. Bibcode:2008ehst.book.....S. ISBN 978-1-4020-4559-2. Archived from the original on 7 September 2023. Retrieved 22 January 2015.
- ^ Rhyner, Hans H. (1994). Ayurveda: The Gentle Health System. Motilal Banarsidass. p. 15. ISBN 978-81-208-1500-1. Archived from the original on 7 September 2023. Retrieved 22 January 2015.
- ^ Ramachandra S.K. Rao, Encyclopaedia of Indian Medicine: historical perspective, Volume 1, 2005, 94–98[need quotation to verify]
- ^ K. Mangathayaru (2013). Pharmacognosy: An Indian perspective. Pearson education. p. 54. ISBN 978-93-325-2026-4. Archived from the original on 7 September 2023. Retrieved 22 January 2015.
- ^ a b Lock 2001, p. 607
- ^ Lock 2001, p. 651
- ^ Lock 2001, p. 652
- ^ Lock 2001, pp. 651–652
- ^ Brett, F. H. (1840). A practical essay on some of the principal surgical diseases of India. Calcutta, India: W. Thacker & Company. p. 458. Retrieved 6 January 2015.
- ^ Hardiman, David (2009). "Indian Medical Indigeneity: From Nationalist Assertion to the Global Market". Social History. 34 (3): 263–283. doi:10.1080/03071020902975131. ISSN 0307-1022. JSTOR 25594366. S2CID 144288544. Archived from the original on 7 May 2022. Retrieved 7 May 2022.
On the whole, such courses provided a back door into a career of improvised and only half-understood biomedical practice. Indeed, for biomedical practitioners, such self-titled 'doctors' are no more than quacks.
Cited references
- Chopra, Ananda S. (2003). "Āyurveda". In Selin, Helaine (ed.). Medicine across cultures: history and practice of medicine in non-western cultures. Kluwer Academic. pp. 75–83. ISBN 978-1-4020-1166-5. Archived from the original on 7 September 2023. Retrieved 15 November 2015.
- Dwivedi, Girish; Dwivedi, Shridhar (2007). "History of Medicine: Sushruta – the Clinician – Teacher par Excellence" (PDF). Indian Journal of Chest Diseases and Allied Sciences. 49: 243–244. Archived from the original (PDF) on 10 October 2008. (Republished by National Informatics Centre, Government of India.)
- Finger, Stanley (2001). Origins of Neuroscience: A History of Explorations into Brain Function. Oxford University Press. ISBN 978-0-19-514694-3.
- Kutumbian, P. (1999). Ancient Indian Medicine. Andhra Pradesh: Orient Longman. ISBN 978-81-250-1521-5.
- Lock, Stephen (2001). The Oxford Illustrated Companion to Medicine. Oxford University Press. ISBN 978-0-19-262950-0.
- Underwood, E. Ashworth; Rhodes, P. (2008). "History of Medicine". Encyclopædia Britannica (2008 ed.).
- Wujastyk, D. (2003a). The Roots of Ayurveda: Selections from Sanskrit Medical Writings. Penguin Books. ISBN 978-0-14-044824-5. Archived from the original on 7 September 2023. Retrieved 8 November 2020.
Further reading
- Drury, Heber (1873). The Useful plants of India. William H Allen & Co., London. ISBN 978-1-4460-2372-3.
- Dymock, William; et al. (1890). Pharmacographia Indica A history of principal drugs of vegetable origin in British India. Vol. 1. London, Bombat, Calcutta: Kegan Paul, Trench, Trübner & Co, Education Society Press, Byculla, Thacker, Spink and Co.
- Hoernle, Rudolf August Friedrich (1907). Studies in the Medicine of Ancient India: Part I: Osteology. Clarendon Press, Oxford.
- Pattathu, Anthony George (2018). Ayurveda and Discursive Formations between Religion, Medicine and Embodiment: A Case Study from Germany. In: Lüddeckens, D., & Schrimpf, M. (2018). Medicine – religion – spirituality: Global perspectives on traditional, complementary, and alternative healing. Bielefeld: transcript Verlag. ISBN 978-3-8376-4582-8, pp. 133–166.
- Patwardhan, Kishore (2008). Pabitra Kumar Roy (ed.). Concepts of Human Physiology in Ayurveda (PDF). Samyak Vak Series-14. Sarnath, Varanasi: Central Institute of Higher Tibetan Studies. pp. 53–73. ISBN 978-81-87127-76-5.
{{cite book}}:|work=ignored (help) - Wise, Thomas T. (1845). Commentary on the Hindu System of Medicine. Calcutta: Thacker & Co.
- Wujastyk, Dominik (2011). "Indian Medicine". Oxford Bibliographies. Oxford University Press. doi:10.1093/obo/9780195399318-0035.. A bibliographical survey of the history of Indian medicine.
- WHO guidelines on safety monitoring of herbal medicines in pharmacovigilance systems
- Use Caution With Ayurvedic Products – US Food and Drug Administration.
External links
- WHO benchmarks for the training of ayurveda World Health Organization (WHO), Geneva, 2022.

