Venlafaxine
 | |
 | |
| Clinical data | |
|---|---|
| Pronunciation | /ˌvɛnləˈfæksiːn/ VEN-lə-FAK-seen |
| Trade names | Effexor, others[1] |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a694020 |
| License data |
|
| Pregnancy category |
|
| Routes of administration | Oral |
| Drug class | Serotonin–norepinephrine reuptake inhibitor |
| ATC code | |
| Legal status | |
| Legal status | |
| Pharmacokinetic data | |
| Bioavailability | 42±15%[2] |
| Protein binding | 27±2% (parent compound), 30±12% (active metabolite, desvenlafaxine)[6] |
| Metabolism | Extensively metabolised by the liver,[2][6] primarily via CYP2D6[8] |
| Metabolites | O-desmethylvenlafaxine (ODV), see desvenlafaxine |
| Elimination half-life | 5±2 h (parent compound for immediate release preparations), 15±6 h (parent compound for extended release preparations), 11±2 h (active metabolite)[2][6] |
| Excretion | Kidney (87%; 5% as unchanged drug; 29% as desvenlafaxine and 53% as other metabolites)[2][6] |
| Identifiers | |
| |
| CAS Number |
|
| PubChem CID | |
| DrugBank |
|
| ChemSpider | |
| UNII |
|
| KEGG | |
| ChEBI |
|
| ChEMBL |
|
| CompTox Dashboard (EPA) | |
| ECHA InfoCard | 100.122.418 |
| Chemical and physical data | |
| Formula | C17H27NO2 |
| Molar mass | 277.408 g·mol−1 |
| 3D model (JSmol) | |
| Chirality | Racemic mixture |
| |
| |
| (verify) | |
Venlafaxine, sold under the brand name Effexor among others, is an antidepressant medication of the serotonin–norepinephrine reuptake inhibitor (SNRI) class.[6][9] It is used to treat major depressive disorder, generalized anxiety disorder, panic disorder, and social anxiety disorder.[9] Studies have shown that venlafaxine improves post-traumatic stress disorder (PTSD).[10] It may also be used for chronic neuropathic pain.[11] It is taken orally (swallowed by mouth).[9] It is also available as the salt venlafaxine besylate (venlafaxine benzenesulfonate monohydrate) in an extended-release formulation (Venbysi XR).[7]
Common side effects include loss of appetite, constipation, dry mouth, dizziness, sweating, insomnia, drowsiness and sexual problems.[9] Severe side effects include an increased risk of suicide, mania, and serotonin syndrome.[9] Antidepressant withdrawal syndrome may occur if stopped.[9] There are concerns that use during the later part of pregnancy can harm the baby.[9] How it works is not entirely clear, but it seems to be related to the potentiation of the activity of some neurotransmitters in the brain.[9]
Venlafaxine was approved for medical use in the United States in 1993.[9] It is available as a generic medication.[9] In 2022, it was the 44th most commonly prescribed medication in the United States, with more than 13 million prescriptions.[12][13]
Medical uses
[edit]Venlafaxine is used primarily for the treatment of depression, general anxiety disorder, social phobia, panic disorder, and vasomotor symptoms.[14]
Venlafaxine has been used off label for the treatment of diabetic neuropathy[15] and migraine prevention.[16] It may work on pain via effects on the opioid receptor.[17] It has also been found to reduce the severity of 'hot flashes' in menopausal women and men on hormonal therapy for the treatment of prostate cancer.[18][19]
Due to its action on both the serotoninergic and adrenergic systems, venlafaxine is also used as a treatment to reduce episodes of cataplexy, a form of muscle weakness, in patients with the sleep disorder narcolepsy.[20] Some open-label and three double-blind studies have suggested the efficacy of venlafaxine in the treatment of attention deficit-hyperactivity disorder (ADHD).[21] Clinical trials have found possible efficacy in those with post-traumatic stress disorder (PTSD).[22] Case reports, open trials and blinded comparisons with established medications have suggested the efficacy of venlafaxine in the treatment of obsessive–compulsive disorder.[23]
Depression
[edit]A comparative meta-analysis of 21 major antidepressants found that venlafaxine, agomelatine, amitriptyline, escitalopram, mirtazapine, paroxetine, and vortioxetine were more effective than other antidepressants, although the quality of many comparisons was assessed as low or very low.[24][25]
Venlafaxine was similar in efficacy to the atypical antidepressant bupropion; however, the remission rate was lower for venlafaxine.[26] In a double-blind study, patients who did not respond to an SSRI were switched to either venlafaxine or another SSRI (citalopram); similar improvement was observed in both groups.[27]
Studies have not established its efficacy for use by children.[28] In children and adolescents with depression, venlafaxine increases the risk of suicidal thoughts or attempts.[29][30][31][32][33][34]
Higher doses (e.g. 225 mg and 375 mg per day) of venlafaxine are more effective than lower doses (e.g. 75 mg per day), but also cause more side effects.[35]
Studies have shown that the extended release is superior to the immediate release form of venlafaxine.[36]
A meta-analysis has shown that efficacy of venlafaxine is not correlated with baseline severity of depression.[36] In other words, regardless of how severe a person's depression is initially, the efficacy of venlafaxine remains consistent and is not influenced by the severity of depression at the start of treatment.
Contraindications
[edit]Venlafaxine is not recommended in patients hypersensitive to it, nor should it be taken by anyone who is allergic to the inactive ingredients, which include gelatin, cellulose, ethylcellulose, iron oxide, titanium dioxide and hypromellose. It should not be used in conjunction with a monoamine oxidase inhibitor (MAOI), as it can cause potentially fatal serotonin syndrome.[2][6][37] Venlafaxine might interact with tramadol or other opioids, as well as trazodone, so caution is needed while mixing multiple serotonergic agents together.[38]
Adverse effects
[edit]Venlafaxine can increase eye pressure, so those with glaucoma may require more frequent eye checks.[6]
A 2017 meta-analysis estimated venlafaxine discontinuation rate due to adverse effects to be 9.4%.[36]
Suicide
[edit]The US Food and Drug Administration (FDA) requires all antidepressants, including venlafaxine, to carry a black box warning with a generic warning about a possible suicide risk.[citation needed]
A 2014 meta analysis of 21 clinical trials of venlafaxine for the treatment of depression in adults found that compared to placebo, venlafaxine reduced the risk of suicidal thoughts and behavior.[39]
A study conducted in Finland followed more than 15,000 patients for 3.4 years. Venlafaxine increased suicide risk by 60% (statistically significant), as compared to no treatment. At the same time, fluoxetine (Prozac) halved the suicide risk.[40]
In a study sponsored by Wyeth, which produces and markets venlafaxine, the data on more than 200,000 cases were obtained from the UK general practice research database. At baseline, patients prescribed venlafaxine had a greater number of risk factors for suicide (such as prior suicide attempts) than patients treated with other anti-depressants. The patients taking venlafaxine had significantly higher risk of suicide than the ones on fluoxetine or citalopram (Celexa). After adjusting for known risk factors, venlafaxine was associated with an increased risk of suicide relative to fluoxetine and dothiepin that was not statistically significant. A statistically significant greater risk for attempted suicide remained after adjustment, but the authors concluded that it could be due to residual confounding.[41]
An analysis of clinical trials by the FDA statisticians showed the incidence of suicidal behaviour among the adults on venlafaxine to be not significantly different from fluoxetine or placebo.[42]
Venlafaxine is contraindicated in children, adolescents and young adults. In children and adolescents with depression, venlafaxine increases the risk of suicidal thoughts or attempts.[29][30][31][32][33][34]
Serotonin syndrome
[edit]The development of a potentially life-threatening serotonin syndrome (also classified as "serotonin toxicity")[43] may occur with venlafaxine treatment, particularly with concomitant use of serotonergic drugs, including but not limited to SSRIs and SNRIs, many hallucinogens such as tryptamines and phenethylamines (e.g., LSD/LSA, DMT, MDMA, mescaline), dextromethorphan (DXM), tramadol, tapentadol, pethidine (meperidine) and triptans and with drugs that impair metabolism of serotonin (including MAOIs).[citation needed] Serotonin syndrome symptoms may include mental status changes (e.g. agitation, hallucinations, coma), autonomic instability (e.g. tachycardia, labile blood pressure, hyperthermia), neuromuscular aberrations (e.g. hyperreflexia, incoordination), or gastrointestinal symptoms (e.g. nausea, vomiting, diarrhea). Venlafaxine-induced serotonin syndrome has also been reported when venlafaxine has been taken in isolation in overdose.[44] An abortive serotonin syndrome state, in which some but not all of the symptoms of the full serotonin syndrome are present, has been reported with venlafaxine at mid-range dosages (150 mg per day).[45] A case of a patient with serotonin syndrome induced by low-dose venlafaxine (37.5 mg per day) has also been reported.[46]
Pregnancy
[edit]There are few well-controlled studies of venlafaxine in pregnant women. A study released in May 2010 by the Canadian Medical Association Journal suggests use of venlafaxine doubles the risk of miscarriage.[47][48] Consequently, venlafaxine should only be used during pregnancy if clearly needed.[6] A large case-control study done as part of the National Birth Defects Prevention Study and published in 2012 found a significant association of venlafaxine use during pregnancy and several birth defects including anencephaly, cleft palate, septal heart defects and coarctation of the aorta.[49] Prospective studies have not shown any statistically significant congenital malformations.[50] There have, however, been some reports of self-limiting effects on newborn infants.[51] As with other serotonin reuptake inhibitors (SRIs), these effects are generally short-lived, lasting only 3 to 5 days,[52] and rarely resulting in severe complications.[53]
Bipolar disorder
[edit]According to the ISBD Task Force report on antidepressant use in bipolar disorder,[54] during the course of treatment for depression with those suffering from bipolar I and II, venlafaxine "appears to carry a particularly high risk of inducing pathologically elevated states of mood and behavior." Because venlafaxine appears to be more likely than SSRIs and bupropion to induce mania and mixed episodes in these patients, provider discretion is advised through "carefully evaluating individual clinical cases and circumstances."
Liver injury
[edit]A rare but serious side effect of venlafaxine is liver injury. It appears to affect both male and female patients with a median age of 44. Cessation of venlafaxine is one of the appropriate measures of management. While the mechanism of venlafaxine-related liver injury remains unclear, findings suggest that it may be related to a CYP2D6 polymorphism.[55]
Overdose
[edit]Most patients overdosing with venlafaxine develop only mild symptoms. Plasma venlafaxine concentrations in overdose survivors have ranged from 6 to 24 mg/L, while postmortem blood levels in fatalities are often in the 10–90 mg/L range.[56] Published retrospective studies report that venlafaxine overdosage may be associated with an increased risk of fatal outcome compared to that observed with SSRI antidepressant products, but lower than that for tricyclic antidepressants. Healthcare professionals are advised to prescribe Effexor and Effexor XR in the smallest quantity of capsules consistent with good patient management to reduce the risk of overdose.[57] It is usually reserved as a second-line treatment for depression due to a combination of its superior efficacy to the first-line treatments like fluoxetine, paroxetine and citalopram and greater frequency of side effects like nausea, headache, insomnia, drowsiness, dry mouth, constipation, sexual dysfunction, sweating and nervousness.[24][58]
There is no specific antidote for venlafaxine, and management is generally supportive, providing treatment for the immediate symptoms. Administration of activated charcoal can prevent absorption of the drug. Monitoring of cardiac rhythm and vital signs is indicated. Seizures are managed with benzodiazepines or other anticonvulsants. Forced diuresis, hemodialysis, exchange transfusion, or hemoperfusion are unlikely to be of benefit in hastening the removal of venlafaxine, due to the drug's high volume of distribution.[59]
Withdrawal syndrome
[edit]People stopping venlafaxine commonly experience SSRI withdrawal symptoms such as dysphoria, headaches, nausea, irritability, emotional lability, sensation of electric shocks (commonly called "brain zaps"[60][61]), and sleep disturbance.[62] Venlafaxine has a higher rate of moderate to severe withdrawal symptoms relative to other antidepressants (similar to the SSRI paroxetine).[63]
The higher risk and increased severity of withdrawal symptoms relative to other antidepressants may be related to the short half-life of venlafaxine and its active metabolite.[64] After stopping venlafaxine, the levels of both serotonin and norepinephrine decrease, leading to the hypothesis that the withdrawal symptoms could result from an overly rapid reduction of neurotransmitter levels.[65]
Other
[edit]In rare cases, drug-induced akathisia can occur after use in some people.[66]
Venlafaxine should be used with caution in hypertensive patients. Venlafaxine must be discontinued if significant hypertension persists.[67][68][69] It can also have undesirable cardiovascular effects.[70]
Pharmacology
[edit]| Transporter | Ki [nM][71] | IC50 [nM][72] |
|---|---|---|
| SERT | 82 | 27 |
| NET | 2480 | 535 |
| DAT | 7647 | ND |
| Receptor | Ki [nM] [71][73] | Species |
|---|---|---|
| 5-HT2A | 2230 | Human |
| 5-HT2C | 2004 | Human |
| 5-HT6 | 2792 | Human |
| α1A | >1000 | Human |
Pharmacodynamics
[edit]Venlafaxine is usually categorized as a serotonin-norepinephrine reuptake inhibitor (SNRI), but it has also been referred to as a serotonin-norepinephrine-dopamine reuptake inhibitor (SNDRI).[74][75] It is described as 'synthetic phenethylamine bicyclic derivative with antidepressant activity'.[76][77] It works by blocking the transporter "reuptake" proteins for key neurotransmitters affecting mood, thereby leaving more active neurotransmitters in the synapse. The neurotransmitters affected are serotonin and norepinephrine. Additionally, in high doses it weakly inhibits the reuptake of dopamine.[78] The frontal cortex largely lacks dopamine transporters; therefore venlafaxine can increase dopamine neurotransmission in this part of the brain.[79][80]
Venlafaxine selectively inhibits the serotonin transporter at lower doses, but at a dose of 225 mg per day it additionally blocks the norepinephrine transporter (NET), as measured by the intravenous tyramine pressor test.[81]
Venlafaxine indirectly affects opioid receptors as well as the α2-adrenergic receptor, and was shown to increase pain threshold in mice. These benefits with respect to pain were reversed with naloxone, an opioid antagonist, thus supporting an opioid mechanism.[82][17]
Pharmacokinetics
[edit]Venlafaxine is well absorbed, with at least 92% of an oral dose being absorbed into systemic circulation. It is extensively metabolized in the liver via the CYP2D6 isoenzyme to desvenlafaxine (O-desmethylvenlafaxine, now marketed as a separate medication named Pristiq[83]), which is just as potent an SNRI as the parent compound, meaning that the differences in metabolism between extensive and poor metabolisers are not clinically important in terms of efficacy. Side effects, however, are reported to be more severe in CYP2D6 poor metabolisers.[84][85] Steady-state concentrations of venlafaxine and its metabolite are attained in the blood within 3 days. Therapeutic effects are usually achieved within 3 to 4 weeks. No accumulation of venlafaxine has been observed during chronic administration in healthy subjects. The primary route of excretion of venlafaxine and its metabolites is via the kidneys.[6] The half-life of venlafaxine is relatively short, so patients are directed to adhere to a strict medication routine, avoiding missing a dose. Even a single missed dose can result in withdrawal symptoms.[86]
Venlafaxine is a substrate of P-glycoprotein (P-gp), which pumps it out of the brain. The gene encoding P-gp, ABCB1, has the SNP rs2032583, with alleles C and T. The majority of people (about 70% of Europeans and 90% of East Asians) have the TT variant.[87][unreliable source?] A 2007 study[88] found that carriers of at least one C allele (variant CC or CT) are 7.72 times more likely than non-carriers to achieve remission after 4 weeks of treatment with amitriptyline, citalopram, paroxetine or venlafaxine (all P-gp substrates). The study included patients with mood disorders other than major depression, such as bipolar II; the ratio is 9.4 if these other disorders are excluded. At the 6-week mark, 75% of C-carriers had remitted, compared to only 38% of non-carriers.[citation needed]
Chemistry
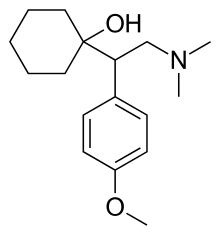
[edit]The IUPAC name of venlafaxine is 1-[2-(dimethylamino)-1-(4 methoxyphenyl)ethyl]cyclohexanol, though it is sometimes referred to as (±)-1-[a-[a-(dimethylamino)methyl]-p-methoxybenzyl]cyclohexanol. It consists of two enantiomers present in equal quantities (termed a racemic mixture), both of which have the empirical formula of C17H27NO2. It is usually sold as a mixture of the respective hydrochloride salts, (R/S)-1-[2-(dimethylamino)-1-(4 methoxyphenyl)ethyl]cyclohexanol hydrochloride, C17H28ClNO2, which is a white to off-white crystalline solid. Venlafaxine is structurally and pharmacologically related to the atypical opioid analgesic tramadol, and more distantly to the newly released opioid tapentadol, but not to any of the conventional antidepressant drugs, including tricyclic antidepressants, SSRIs, MAOIs, or RIMAs.[89]
Venlafaxine extended release is chemically the same as normal venlafaxine. The extended release (controlled release) version distributes the release of the drug into the gastrointestinal tract over a longer period than normal venlafaxine. This results in a lower peak plasma concentration. Studies have shown that the extended release formula has a lower incidence of nausea as a side effect, resulting in better compliance.[90]
Interactions
[edit]Venlafaxine should be taken with caution when using St John's wort.[91] Venlafaxine may lower the seizure threshold, and coadministration with other drugs that lower the seizure threshold such as bupropion and tramadol should be done with caution and at low doses.[92]
Society and culture
[edit]Recreational use
[edit]Venlafaxine can be abused as a recreational drug, with damages that can manifest within a month.[93]
Brand names
[edit]

Venlafaxine was originally marketed as Effexor in most of the world; generic venlafaxine has been available since around 2008 and extended release venlafaxine has been available since around 2010.[94]
Venlafaxine is sold under many brand names worldwide.[1] In some countries, Effexor is marketed by Viatris after Upjohn was spun off from Pfizer.[95][96]
Veterinary uses
[edit]Veterinary overdose in dogs is very well treated by Cyproheptadine HCl.[97]: 1371
Venlafaxine is highly toxic to Bacillariophyta and Chlorophyta phytoplankton.[98] Cats are drawn to the smell of venlafaxine and tend to ingest the pills, which is highly toxic to them.[99]
References
[edit]- ^ a b "Venlafaxine (International)". Drugs.com. January 2020. Archived from the original on 6 September 2020. Retrieved 24 January 2020.
- ^ a b c d e f g "Efexor-XR (venlafaxine hydrochloride)" (PDF). TGA eBS. Archived from the original on 12 May 2021. Retrieved 11 May 2021.
- ^ "FDA-sourced list of all drugs with black box warnings (Use Download Full Results and View Query links.)". nctr-crs.fda.gov. FDA. Retrieved 22 October 2023.
- ^ Anvisa (31 March 2023). "RDC Nº 784 - Listas de Substâncias Entorpecentes, Psicotrópicas, Precursoras e Outras sob Controle Especial" [Collegiate Board Resolution No. 784 - Lists of Narcotic, Psychotropic, Precursor, and Other Substances under Special Control] (in Brazilian Portuguese). Diário Oficial da União (published 4 April 2023). Archived from the original on 3 August 2023. Retrieved 16 August 2023.
- ^ "Efexor XL 75 mg hard prolonged release capsules - Summary of Product Characteristics (SmPC)". (emc). 16 March 2020. Archived from the original on 7 October 2020. Retrieved 15 April 2020.
- ^ a b c d e f g h i j "Effexor XR- venlafaxine hydrochloride capsule, extended release". DailyMed. Archived from the original on 12 May 2021. Retrieved 11 May 2021.
- ^ a b "Venlafaxine tablet, extended release". DailyMed. 30 June 2022. Retrieved 7 January 2023.
- ^ Dean L (2015). Pratt VM, Scott SA, Pirmohamed M, Esquivel B, Kane MS, Kattman BL, Malheiro AJ (eds.). Venlafaxine Therapy and CYP2D6 Genotype. National Center for Biotechnology Information (US). PMID 28520361. Archived from the original on 29 November 2017. Retrieved 28 December 2018.
- ^ a b c d e f g h i j "Venlafaxine Hydrochloride Monograph for Professionals". Drugs.com. AHFS. Archived from the original on 27 November 2020. Retrieved 24 December 2018.
- ^ Forman-Hoffman V, Middleton JC, Feltner C, Gaynes BN, Weber RP, Bann C, et al. (17 May 2018). Psychological and Pharmacological Treatments for Adults With Posttraumatic Stress Disorder: A Systematic Review Update (Report). Agency for Healthcare Research and Quality (AHRQ). doi:10.23970/ahrqepccer207. PMID 30204376. Archived from the original on 10 July 2018. Retrieved 29 July 2023.
- ^ "Antidepressants: Another weapon against chronic pain". Mayo Clinic. Archived from the original on 26 October 2021. Retrieved 25 January 2020.
- ^ "The Top 300 of 2022". ClinCalc. Archived from the original on 30 August 2024. Retrieved 30 August 2024.
- ^ "Venlafaxine Drug Usage Statistics, United States, 2013 - 2022". ClinCalc. Retrieved 30 August 2024.
- ^ "venlafaxine-hydrochloride". The American Society of Health-System Pharmacists. Archived from the original on 27 November 2020. Retrieved 3 April 2011.
- ^ Grothe DR, Scheckner B, Albano D (May 2004). "Treatment of pain syndromes with venlafaxine". Pharmacotherapy. 24 (5): 621–629. doi:10.1592/phco.24.6.621.34748. PMID 15162896. S2CID 28187627.
- ^ Singh D, Saadabadi A (2022). "Venlafaxine". StatPearls. Treasure Island (FL): StatPearls Publishing. PMID 30570984.
- ^ a b The Opioid System as the Interface between the Brain's Cognitive and Motivational Systems. Academic Press. 2018. p. 73. ISBN 978-0-444-64168-7. Archived from the original on 27 August 2021. Retrieved 9 May 2020.
- ^ Mayo Clinic staff (2005). "Beyond hormone therapy: Other medicines may help". Hot flashes: Ease the discomfort of menopause. Mayo Clinic. Archived from the original on 25 February 2005. Retrieved 19 August 2005.
- ^ Schober CE, Ansani NT (November 2003). "Venlafaxine hydrochloride for the treatment of hot flashes". The Annals of Pharmacotherapy. 37 (11): 1703–1707. doi:10.1345/aph.1C483. PMID 14565812. S2CID 45334784.
- ^ "Medications". Stanford University School of Medicine, Center for Narcolepsy. 7 February 2003. Archived from the original on 21 August 2007. Retrieved 3 September 2007.
- ^ Ghanizadeh A, Freeman RD, Berk M (March 2013). "Efficacy and adverse effects of venlafaxine in children and adolescents with ADHD: a systematic review of non-controlled and controlled trials". Reviews on Recent Clinical Trials. 8 (1): 2–8. doi:10.2174/1574887111308010002. PMID 23157376.
- ^ Pae CU, Lim HK, Ajwani N, Lee C, Patkar AA (June 2007). "Extended-release formulation of venlafaxine in the treatment of post-traumatic stress disorder". Expert Review of Neurotherapeutics. 7 (6): 603–615. doi:10.1586/14737175.7.6.603. PMID 17563244. S2CID 25215502.
- ^ Phelps NJ, Cates ME (January 2005). "The role of venlafaxine in the treatment of obsessive-compulsive disorder". The Annals of Pharmacotherapy. 39 (1): 136–140. doi:10.1345/aph.1E362. PMID 15585743. S2CID 30973410.
- ^ a b Cipriani A, Furukawa TA, Salanti G, Geddes JR, Higgins JP, Churchill R, et al. (February 2009). "Comparative efficacy and acceptability of 12 new-generation antidepressants: a multiple-treatments meta-analysis". Lancet. 373 (9665): 746–758. doi:10.1016/S0140-6736(09)60046-5. PMID 19185342. S2CID 35858125.
- ^ Cipriani A, Furukawa TA, Salanti G, Chaimani A, Atkinson LZ, Ogawa Y, et al. (April 2018). "Comparative efficacy and acceptability of 21 antidepressant drugs for the acute treatment of adults with major depressive disorder: a systematic review and network meta-analysis". Lancet. 391 (10128): 1357–1366. doi:10.1016/S0140-6736(17)32802-7. PMC 5889788. PMID 29477251.
- ^ Thase ME, Clayton AH, Haight BR, Thompson AH, Modell JG, Johnston JA (October 2006). "A double-blind comparison between bupropion XL and venlafaxine XR: sexual functioning, antidepressant efficacy, and tolerability". Journal of Clinical Psychopharmacology. 26 (5): 482–488. doi:10.1097/01.jcp.0000239790.83707.ab. PMID 16974189. S2CID 276619.
- ^ Lenox-Smith AJ, Jiang Q (May 2008). "Venlafaxine extended release versus citalopram in patients with depression unresponsive to a selective serotonin reuptake inhibitor". International Clinical Psychopharmacology. 23 (3): 113–119. doi:10.1097/YIC.0b013e3282f424c2. PMID 18408525. S2CID 34986490.
- ^ Courtney DB (August 2004). "Selective serotonin reuptake inhibitor and venlafaxine use in children and adolescents with major depressive disorder: a systematic review of published randomized controlled trials". Canadian Journal of Psychiatry. 49 (8): 557–563. doi:10.1177/070674370404900807. PMID 15453105.
- ^ a b "Antidepressants for children and teenagers: what works for anxiety and depression?". NIHR Evidence (Plain English summary). National Institute for Health and Care Research. 3 November 2022. doi:10.3310/nihrevidence_53342. S2CID 253347210.
- ^ a b Zhou X, Teng T, Zhang Y, Del Giovane C, Furukawa TA, Weisz JR, et al. (July 2020). "Comparative efficacy and acceptability of antidepressants, psychotherapies, and their combination for acute treatment of children and adolescents with depressive disorder: a systematic review and network meta-analysis". The Lancet. Psychiatry. 7 (7): 581–601. doi:10.1016/S2215-0366(20)30137-1. PMC 7303954. PMID 32563306.
- ^ a b Hetrick SE, McKenzie JE, Bailey AP, Sharma V, Moller CI, Badcock PB, et al. (Cochrane Common Mental Disorders Group) (May 2021). "New generation antidepressants for depression in children and adolescents: a network meta-analysis". The Cochrane Database of Systematic Reviews. 2021 (5): CD013674. doi:10.1002/14651858.CD013674.pub2. PMC 8143444. PMID 34029378.
- ^ a b Solmi M, Fornaro M, Ostinelli EG, Zangani C, Croatto G, Monaco F, et al. (June 2020). "Safety of 80 antidepressants, antipsychotics, anti-attention-deficit/hyperactivity medications and mood stabilizers in children and adolescents with psychiatric disorders: a large scale systematic meta-review of 78 adverse effects". World Psychiatry. 19 (2): 214–232. doi:10.1002/wps.20765. PMC 7215080. PMID 32394557.
- ^ a b Boaden K, Tomlinson A, Cortese S, Cipriani A (2 September 2020). "Antidepressants in Children and Adolescents: Meta-Review of Efficacy, Tolerability and Suicidality in Acute Treatment". Frontiers in Psychiatry. 11: 717. doi:10.3389/fpsyt.2020.00717. PMC 7493620. PMID 32982805.
- ^ a b Correll CU, Cortese S, Croatto G, Monaco F, Krinitski D, Arrondo G, et al. (June 2021). "Efficacy and acceptability of pharmacological, psychosocial, and brain stimulation interventions in children and adolescents with mental disorders: an umbrella review". World Psychiatry. 20 (2): 244–275. doi:10.1002/wps.20881. PMC 8129843. PMID 34002501.
- ^ Rudolph RL, Fabre LF, Feighner JP, Rickels K, Entsuah R, Derivan AT (March 1998). "A randomized, placebo-controlled, dose-response trial of venlafaxine hydrochloride in the treatment of major depression". The Journal of Clinical Psychiatry. 59 (3): 116–122. doi:10.4088/jcp.v59n0305. PMID 9541154.
- ^ a b c Thase M, Asami Y, Wajsbrot D, Dorries K, Boucher M, Pappadopulos E (February 2017). "A meta-analysis of the efficacy of venlafaxine extended release 75-225 mg/day for the treatment of major depressive disorder". Current Medical Research and Opinion. 33 (2). Informa UK Limited: 317–326. doi:10.1080/03007995.2016.1255185. PMID 27794623. S2CID 4394404.
- ^ Taylor D, Paton C, Kapur S, eds. (2012). The Maudsley Prescribing Guidelines in Psychiatry (illustrated ed.). John Wiley & Sons. ISBN 978-0-470-97948-8.
- ^ Ripple MG, Pestaner JP, Levine BS, Smialek JE (December 2000). "Lethal combination of tramadol and multiple drugs affecting serotonin". The American Journal of Forensic Medicine and Pathology. 21 (4): 370–374. doi:10.1097/00000433-200012000-00015. PMID 11111800. Archived from the original on 6 April 2022. Retrieved 6 April 2022.
- ^ Gibbons RD, Brown CH, Hur K, Davis J, Mann JJ (June 2012). "Suicidal thoughts and behavior with antidepressant treatment: reanalysis of the randomized placebo-controlled studies of fluoxetine and venlafaxine". Archives of General Psychiatry. 69 (6): 580–587. doi:10.1001/archgenpsychiatry.2011.2048. PMC 3367101. PMID 22309973.
- ^ Tiihonen J, Lönnqvist J, Wahlbeck K, Klaukka T, Tanskanen A, Haukka J (December 2006). "Antidepressants and the risk of suicide, attempted suicide, and overall mortality in a nationwide cohort". Archives of General Psychiatry. 63 (12): 1358–1367. doi:10.1001/archpsyc.63.12.1358. PMID 17146010.
- ^ Rubino A, Roskell N, Tennis P, Mines D, Weich S, Andrews E (February 2007). "Risk of suicide during treatment with venlafaxine, citalopram, fluoxetine, and dothiepin: retrospective cohort study". BMJ. 334 (7587): 242. doi:10.1136/bmj.39041.445104.BE. PMC 1790752. PMID 17164297.
- ^ "Overview for December 13 Meeting of Psychopharmacologic Drugs Advisory Committee" (PDF). Food and Drug Administration: Center for Drug Evaluation and Research. 16 November 2006. Archived (PDF) from the original on 16 March 2007. Retrieved 20 June 2007.
- ^ Dunkley EJ, Isbister GK, Sibbritt D, Dawson AH, Whyte IM (September 2003). "The Hunter Serotonin Toxicity Criteria: simple and accurate diagnostic decision rules for serotonin toxicity". QJM. 96 (9): 635–642. doi:10.1093/qjmed/hcg109. PMID 12925718.
- ^ Kolecki P (July–August 1997). "Isolated venlafaxine-induced serotonin syndrome". The Journal of Emergency Medicine. 15 (4): 491–493. doi:10.1016/S0736-4679(97)00078-4. PMID 9279702.
- ^ Ebert D, et al. "Hallucinations as a side effect of venlafaxine treatment". Psychiatry On-line. Archived from the original on 21 May 2008. Retrieved 17 June 2008.
- ^ Pan JJ, Shen WW (February 2003). "Serotonin syndrome induced by low-dose venlafaxine". The Annals of Pharmacotherapy. 37 (2): 209–211. doi:10.1345/aph.1C021. PMID 12549949.
- ^ Broy P, Bérard A (January 2010). "Gestational exposure to antidepressants and the risk of spontaneous abortion: a review". Current Drug Delivery. 7 (1): 76–92. doi:10.2174/156720110790396508. PMID 19863482. S2CID 28153571.
- ^ Nakhai-Pour HR, Broy P, Bérard A (July 2010). "Use of antidepressants during pregnancy and the risk of spontaneous abortion". CMAJ. 182 (10): 1031–1037. doi:10.1503/cmaj.091208. PMC 2900326. PMID 20513781.
- ^ Polen KN, Rasmussen SA, Riehle-Colarusso T, Reefhuis J (January 2013). "Association between reported venlafaxine use in early pregnancy and birth defects, national birth defects prevention study, 1997-2007". Birth Defects Research. Part A, Clinical and Molecular Teratology. 97 (1): 28–35. doi:10.1002/bdra.23096. PMC 4484721. PMID 23281074.
- ^ Gentile S (2005). "The safety of newer antidepressants in pregnancy and breastfeeding". Drug Safety. 28 (2): 137–152. doi:10.2165/00002018-200528020-00005. PMID 15691224. S2CID 24798891.
- ^ de Moor RA, Mourad L, ter Haar J, Egberts AC (July 2003). "[Withdrawal symptoms in a neonate following exposure to venlafaxine during pregnancy]". Nederlands Tijdschrift voor Geneeskunde. 147 (28): 1370–1372. PMID 12892015.
- ^ Ferreira E, Carceller AM, Agogué C, Martin BZ, St-André M, Francoeur D, et al. (January 2007). "Effects of selective serotonin reuptake inhibitors and venlafaxine during pregnancy in term and preterm neonates". Pediatrics. 119 (1): 52–59. doi:10.1542/peds.2006-2133. PMID 17200271. S2CID 27443298.
- ^ Moses-Kolko EL, Bogen D, Perel J, Bregar A, Uhl K, Levin B, et al. (May 2005). "Neonatal signs after late in utero exposure to serotonin reuptake inhibitors: literature review and implications for clinical applications". JAMA. 293 (19): 2372–2383. doi:10.1001/jama.293.19.2372. PMID 15900008. S2CID 30284439.
- ^ Pacchiarotti I, Bond DJ, Baldessarini RJ, Nolen WA, Grunze H, Licht RW, et al. (November 2013). "The International Society for Bipolar Disorders (ISBD) task force report on antidepressant use in bipolar disorders". The American Journal of Psychiatry. 170 (11): 1249–1262. doi:10.1176/appi.ajp.2013.13020185. PMC 4091043. PMID 24030475.
- ^ Stadlmann S, Portmann S, Tschopp S, Terracciano LM (November 2012). "Venlafaxine-induced cholestatic hepatitis: case report and review of literature". The American Journal of Surgical Pathology. 36 (11). Ovid Technologies (Wolters Kluwer Health): 1724–1728. doi:10.1097/pas.0b013e31826af296. PMID 23073329.
- ^ Baselt R (2008). Disposition of Toxic Drugs and Chemicals in Man (8th ed.). Foster City, CA: Biomedical Publications. pp. 1634–1637. ISBN 978-0-9626523-7-0.
- ^ "Wyeth Letter to Health Care Providers". Wyeth Pharmaceuticals Inc. 2006. Archived from the original on 27 August 2009. Retrieved 6 August 2009.
- ^ Taylor D, Lenox-Smith A, Bradley A (June 2013). "A review of the suitability of duloxetine and venlafaxine for use in patients with depression in primary care with a focus on cardiovascular safety, suicide and mortality due to antidepressant overdose". Therapeutic Advances in Psychopharmacology. 3 (3): 151–161. doi:10.1177/2045125312472890. PMC 3805457. PMID 24167687.
- ^ Hanekamp BB, Zijlstra JG, Tulleken JE, Ligtenberg JJ, van der Werf TS, Hofstra LS (September 2005). "Serotonin syndrome and rhabdomyolysis in venlafaxine poisoning: a case report" (PDF). The Netherlands Journal of Medicine. 63 (8): 316–318. PMID 16186642. Archived from the original on 4 March 2016. Retrieved 6 November 2013.
- ^ Papp A, Onton JA (December 2018). "Brain Zaps: An Underappreciated Symptom of Antidepressant Discontinuation". The Primary Care Companion for CNS Disorders. 20 (6): 18m02311. doi:10.4088/PCC.18m02311. PMID 30605268. S2CID 58577252.
- ^ Rizkalla M, Kowalkowski B, Prozialeck WC (February 2020). "Antidepressant Discontinuation Syndrome: A Common but Underappreciated Clinical Problem". The Journal of the American Osteopathic Association. 120 (3): 174–178. doi:10.7556/jaoa.2020.030. PMID 32077900.
- ^ Petit J, Sansone RA (2011). "A case of interdose discontinuation symptoms with venlafaxine extended release". The Primary Care Companion for CNS Disorders. 13 (5). doi:10.4088/PCC.11l01140. PMC 3267502. PMID 22295261.
- ^ Hosenbocus S, Chahal R (February 2011). "SSRIs and SNRIs: A review of the Discontinuation Syndrome in Children and Adolescents". Journal of the Canadian Academy of Child and Adolescent Psychiatry. 20 (1): 60–67. PMC 3024727. PMID 21286371.
- ^ Haddad PM (March 2001). "Antidepressant discontinuation syndromes". Drug Safety. 24 (3): 183–197. doi:10.2165/00002018-200124030-00003. PMID 11347722. S2CID 26897797.
- ^ Campagne DM (July 2005). "Venlafaxine and serious withdrawal symptoms: warning to drivers". MedGenMed. 7 (3): 22. PMC 1681629. PMID 16369248.
- ^ "Venlafaxine Side Effects in Detail". Archived from the original on 3 October 2020. Retrieved 3 January 2018.
- ^ Khurana RN, Baudendistel TE (December 2003). "Hypertensive crisis associated with venlafaxine". The American Journal of Medicine. 115 (8): 676–677. doi:10.1016/S0002-9343(03)00472-8. PMID 14656626.
- ^ Thase ME (October 1998). "Effects of venlafaxine on blood pressure: a meta-analysis of original data from 3744 depressed patients". The Journal of Clinical Psychiatry. 59 (10): 502–508. doi:10.4088/JCP.v59n1002. PMID 9818630.
- ^ Edvardsson B (26 February 2015). "Venlafaxine as single therapy associated with hypertensive encephalopathy". SpringerPlus. 4 (1): 97. doi:10.1186/s40064-015-0883-0. PMC 4348355. PMID 25763307.
- ^ Johnson EM, Whyte E, Mulsant BH, Pollock BG, Weber E, Begley AE, et al. (September 2006). "Cardiovascular changes associated with venlafaxine in the treatment of late-life depression". The American Journal of Geriatric Psychiatry. 14 (9): 796–802. doi:10.1097/01.JGP.0000204328.50105.b3. PMID 16943176.
- ^ a b Bymaster FP, Dreshfield-Ahmad LJ, Threlkeld PG, Shaw JL, Thompson L, Nelson DL, et al. (December 2001). "Comparative affinity of duloxetine and venlafaxine for serotonin and norepinephrine transporters in vitro and in vivo, human serotonin receptor subtypes, and other neuronal receptors". Neuropsychopharmacology. 25 (6): 871–880. doi:10.1016/S0893-133X(01)00298-6. PMID 11750180.
- ^ Sabatucci JP, Mahaney PE, Leiter J, Johnston G, Burroughs K, Cosmi S, et al. (May 2010). "Heterocyclic cycloalkanol ethylamines as norepinephrine reuptake inhibitors". Bioorganic & Medicinal Chemistry Letters. 20 (9): 2809–2812. doi:10.1016/j.bmcl.2010.03.059. PMID 20378347.
- ^ Roth BL, Kroeze WK (2006). "Screening the receptorome yields validated molecular targets for drug discovery". Current Pharmaceutical Design. 12 (14): 1785–1795. doi:10.2174/138161206776873680. PMID 16712488.
- ^ Clinical trial number NCT00001483 for "Acute Effectiveness of Additional Drugs to the Standard Treatment of Depression" at ClinicalTrials.gov
- ^ Goeringer KE, McIntyre IM, Drummer OH (September 2001). "Postmortem tissue concentrations of venlafaxine". Forensic Science International. 121 (1–2): 70–75. doi:10.1016/S0379-0738(01)00455-8. PMID 11516890.
- ^ "venlafaxine". National Cancer Institute. Archived from the original on 24 January 2022.
- ^ Singh D, Saadabadi A (2022). "Venlafaxine". StatPearls. StatPearls. PMID 30570984. Archived from the original on 30 June 2022. Retrieved 24 January 2022.
- ^ Wellington K, Perry CM (2001). "Venlafaxine extended-release: a review of its use in the management of major depression". CNS Drugs. 15 (8): 643–669. doi:10.2165/00023210-200115080-00007. PMID 11524036. S2CID 26795121.
- ^ "Stahl's Essential Psychopharmacology – Cambridge University Press". Stahlonline.cambridge.org. Archived from the original on 27 February 2012. Retrieved 21 November 2013.
- ^ Delgado PL, Moreno FA (2000). "Role of norepinephrine in depression". The Journal of Clinical Psychiatry. 61 (Suppl 1): 5–12. PMID 10703757.[full citation needed]
- ^ Aldosary F, Norris S, Tremblay P, James JS, Ritchie JC, Blier P (April 2022). "Differential Potency of Venlafaxine, Paroxetine, and Atomoxetine to Inhibit Serotonin and Norepinephrine Reuptake in Patients With Major Depressive Disorder". The International Journal of Neuropsychopharmacology. 25 (4): 283–292. doi:10.1093/ijnp/pyab086. PMC 9017767. PMID 34958348.
- ^ Stern TA, Fava M, Wilens TE, Rosenbaum JF (2015). Massachusetts General Hospital Comprehensive Clinical Psychiatry. Elsevier Health Sciences. p. 860. ISBN 978-0-323-29507-9. Archived from the original on 27 August 2021. Retrieved 9 May 2020.
- ^ Pae CU (December 2011). "Desvenlafaxine in the treatment of major depressive disorder". Expert Opinion on Pharmacotherapy. 12 (18): 2923–2928. doi:10.1517/14656566.2011.636033. PMID 22098230. S2CID 33558428.
- ^ Shams ME, Arneth B, Hiemke C, Dragicevic A, Müller MJ, Kaiser R, et al. (October 2006). "CYP2D6 polymorphism and clinical effect of the antidepressant venlafaxine". Journal of Clinical Pharmacy and Therapeutics. 31 (5): 493–502. doi:10.1111/j.1365-2710.2006.00763.x. PMID 16958828. S2CID 22236102.
- ^ Dean L (2015). "Venlafaxine Therapy and CYP2D6 Genotype". In Pratt VM, McLeod HL, Rubinstein WS, et al. (eds.). Medical Genetics Summaries. National Center for Biotechnology Information (NCBI). PMID 28520361. Bookshelf ID: NBK305561. Archived from the original on 26 October 2020. Retrieved 7 February 2020.
- ^ Parker G, Blennerhassett J (April 1998). "Withdrawal reactions associated with venlafaxine". The Australian and New Zealand Journal of Psychiatry. 32 (2): 291–294. doi:10.3109/00048679809062742. PMID 9588310. S2CID 34824025.
- ^ "Rs2032583 -SNPedia". Snpedia.com. Archived from the original on 11 December 2013. Retrieved 21 November 2013.
- ^ Uhr M, Tontsch A, Namendorf C, Ripke S, Lucae S, Ising M, et al. (January 2008). "Polymorphisms in the drug transporter gene ABCB1 predict antidepressant treatment response in depression". Neuron. 57 (2): 203–209. doi:10.1016/j.neuron.2007.11.017. PMID 18215618. S2CID 6772775.
- ^ Whyte IM, Dawson AH, Buckley NA (May 2003). "Relative toxicity of venlafaxine and selective serotonin reuptake inhibitors in overdose compared to tricyclic antidepressants". QJM. 96 (5): 369–374. doi:10.1093/qjmed/hcg062. PMID 12702786.
- ^ DeVane CL (2003). "Immediate-release versus controlled-release formulations: pharmacokinetics of newer antidepressants in relation to nausea". The Journal of Clinical Psychiatry. 64 (Suppl 18): 14–19. PMID 14700450.
- ^ Karch A (2006). 2006 Lippincott's Nursing Drug Guide. Philadelphia, Baltimore, New York, London, Buenos Aires, Hong Kong, Sydney, Tokyo: Lippincott Williams & Wilkins. ISBN 978-1-58255-436-5.
- ^ Thundiyil JG, Kearney TE, Olson KR (March 2007). "Evolving epidemiology of drug-induced seizures reported to a Poison Control Center System". Journal of Medical Toxicology. 3 (1): 15–19. doi:10.1007/BF03161033. PMC 3550124. PMID 18072153.
- ^ Iliou T, Casta P, Lequeux J, Pochard L, Frauger E, Spadari M, et al. (2019). "Venlafaxine Abuse in a Patient With a History of Methylphenidate Abuse: A Case Report". Journal of Clinical Psychopharmacology. 39 (2): 172–174. doi:10.1097/JCP.0000000000001011. PMID 30811375. S2CID 73496502.
- ^ Staton T (13 June 2012). "Drugstores accuse Pfizer, Teva of blocking Effexor generics". FiercePharma. Archived from the original on 26 November 2020. Retrieved 22 June 2017.
- ^ "Pfizer Completes Transaction to Combine Its Upjohn Business with Mylan" (Press release). Pfizer. 16 November 2020. Retrieved 17 June 2024 – via Business Wire.
- ^ "Brands". Viatris. 16 November 2020. Retrieved 17 June 2024.
- ^ Gupta RC, ed. (2012). Veterinary Toxicology : Basic and Clinical Principles (2 ed.). Amsterdam Boston: Academic Press. pp. xii+1438. ISBN 978-0-12-385926-6. OCLC 794491298.
- ^ Chia MA, Lorenzi AS, Ameh I, Dauda S, Cordeiro-Araújo MK, Agee JT, et al. (May 2021). "Susceptibility of phytoplankton to the increasing presence of active pharmaceutical ingredients (APIs) in the aquatic environment: A review". Aquatic Toxicology. 234. Elsevier: 105809. Bibcode:2021AqTox.23405809C. doi:10.1016/j.aquatox.2021.105809. PMID 33780670. S2CID 232419482.
- ^ "The Top 5 Cat Toxins". Pet Health Network. Retrieved 3 May 2023.
Further reading
[edit]- Dean L (July 2015). "Venlafaxine Therapy and CYP2D6 Genotype". In Pratt VM, McLeod HL, Rubinstein WS, et al. (eds.). Medical Genetics Summaries. National Center for Biotechnology Information (NCBI). PMID 28520361.
