Barotrauma
This article may have too many section headers. (March 2023) |
| Barotrauma | |
|---|---|
| Other names | Squeeze, decompression illness, lung overpressure injury, volutrauma |
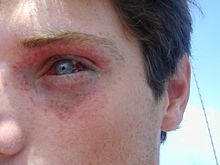 | |
| Mild barotrauma to a diver caused by mask squeeze. Eye and surrounding skin show petechiae and a subconjunctival haemmorhage. | |
| Symptoms | Dependent on location |
| Complications | Arterial gas embolism, pneumothorax, mediastinal emphysema |
| Causes | Pressure difference between the environment and a gas-filled space in or in contact with the affected tissues |
Barotrauma is physical damage to body tissues caused by a difference in pressure between a gas space inside, or in contact with, the body and the surrounding gas or liquid.[1][2] The initial damage is usually due to over-stretching the tissues in tension or shear, either directly by an expansion of the gas in the closed space or by pressure difference hydrostatically transmitted through the tissue. Tissue rupture may be complicated by the introduction of gas into the local tissue or circulation through the initial trauma site, which can cause blockage of circulation at distant sites or interfere with the normal function of an organ by its presence. The term is usually applied when the gas volume involved already exists prior to decompression. Barotrauma can occur during both compression and decompression events.[1][2]
Barotrauma generally manifests as sinus or middle ear effects, lung overpressure injuries and injuries resulting from external squeezes. Decompression sickness is indirectly caused by ambient pressure reduction, and tissue damage is caused directly and indirectly by gas bubbles. However, these bubbles form out of supersaturated solution from dissolved gases, and are not generally considered barotrauma. Decompression illness is a term that includes decompression sickness and arterial gas embolism caused by lung overexpansion barotrauma. It is also classified under the broader term of dysbarism, which covers all medical conditions resulting from changes in ambient pressure.[3]
Barotrauma typically occurs when the organism is exposed to a significant change in ambient pressure, such as when a scuba diver, a free-diver or an airplane passenger ascends or descends or during uncontrolled decompression of a pressure vessel such as a diving chamber or pressurized aircraft, but can also be caused by a shock wave. Ventilator-induced lung injury (VILI) is a condition caused by over-expansion of the lungs by mechanical ventilation used when the body is unable to breathe for itself and is associated with relatively large tidal volumes and relatively high peak pressures. Barotrauma due to overexpansion of an internal gas-filled space may also be termed volutrauma.
Presentation
[edit]Examples of organs or tissues easily damaged by barotrauma are:
- Middle ear and inner ear (barotitis or aerotitis)[1][2][4][5][6][7]
- Paranasal sinuses[1][2][5] (causing aerosinusitis)
- Lungs may be affected by both under-pressure or, more commonly, overpressure relative to the external pressure[1][2][8][9]
- Eyes[1][2] (the under-pressure air space is inside the diving mask or swimming goggles[10])
- Skin[1][2] (when wearing a diving suit which creates an air space)
- Brain and cranium (temporal lobe injury secondary to temporal bone rupture)[11]
- Teeth (causing barodontalgia, i.e., barometric pressure related dental pain,[12][13][14][15][16] or dental fractures[17][18][19])
- Genital squeeze and associated urinary complications of P-valve use[20]
- Intestinal barotrauma is caused by over-expansion of gas trapped in the intestines during ascent.
This section needs expansion with: Symptoms of each type. You can help by adding to it. (July 2022) |
Causes
[edit]When diving, the pressure differences which cause the barotrauma are changes in hydrostatic pressure. There are two components to the surrounding pressure acting on the diver: the atmospheric pressure and the water pressure. A descent of 10 metres (33 feet) in water increases the ambient pressure by an amount approximately equal to the pressure of the atmosphere at sea level. So, a descent from the surface to 10 metres (33 feet) underwater results in a doubling of the pressure on the diver. This pressure change will reduce the volume of a flexible gas-filled space by half. Boyle's law describes the relationship between the volume of the gas space and the pressure in the gas.[1][21]
Barotraumas of descent, also known as compression barotrauma, and squeezes, are caused by preventing the free change of volume of the gas in a closed space in contact with the diver, resulting in a pressure difference between the tissues and the gas space, and the unbalanced force due to this pressure difference causes deformation of the tissues resulting in cell rupture.[2] Barotraumas of ascent, also called decompression barotrauma, are also caused when the free change of volume of the gas in a closed space in contact with the diver is prevented. In this case the pressure difference causes a resultant tension in the surrounding tissues which exceeds their tensile strength.[2]
Patients undergoing hyperbaric oxygen therapy must equalize their ears to avoid barotrauma. High risk of otic barotrauma is associated with unconscious patients.[22] Explosive decompression of a hyperbaric environment can produce severe barotrauma, followed by severe decompression bubble formation and other related injury. The Byford Dolphin incident is an example. Rapid uncontrolled decompression from caissons, airlocks, pressurised aircraft, spacecraft, and pressure suits can have similar effects of decompression barotrauma.
Collapse of a pressure resistant structure such as a submarine, submersible, or atmospheric diving suit can cause rapid compression barotrauma. A rapid change of altitude can cause barotrauma when internal air spaces cannot be equalised. Excessively strenuous efforts to equalise the ears using the Valsalva manoeuvre can overpressurise the middle ear, and can cause middle ear and/or inner ear barotrauma. An explosive blast and explosive decompression create a pressure wave that can induce barotrauma. The difference in pressure between internal organs and the outer surface of the body causes injuries to internal organs that contain gas, such as the lungs, gastrointestinal tract, and ear.[23] Lung injuries can also occur during rapid decompression, although the risk of injury is lower than with explosive decompression.[24][25]
Mechanical ventilation can lead to barotrauma of the lungs. This can be due to either:[26]
- absolute pressures used in order to ventilate non-compliant lungs.
- shearing forces, particularly associated with rapid changes in gas velocity.
The resultant alveolar rupture can lead to pneumothorax, pulmonary interstitial emphysema (PIE) and pneumomediastinum.[27]
Barotrauma is a recognised complication of mechanical ventilation that can occur in any patient receiving mechanical ventilation, but is most commonly associated with acute respiratory distress syndrome. It used to be the most common complication of mechanical ventilation but can usually be avoided by limiting tidal volume and plateau pressure to less than 30 to 50 cm water column (30 to 50 mb). As an indicator of transalveolar pressure, which predicts alveolar distention, plateau pressure or peak airway pressure (PAP) may be the most effective predictor of risk, but there is no generally accepted safe pressure at which there is no risk.[27][28] Risk also appears to be increased by aspiration of stomach contents and pre-existing disease such as necrotising pneumonia and chronic lung disease. Status asthmaticus is a particular problem as it requires relatively high pressures to overcome bronchial obstruction.[28]
When lung tissues are damaged by alveolar over-distension, the injury may be termed volutrauma, but volume and transpulmonary pressure are closely related. Ventilator induced lung injury is often associated with high tidal volumes (Vt).[29]
Other injuries with similar causes are decompression sickness and ebullism.[30]
Pathophysiology
[edit]Lung overpressure injury
[edit]A free-diver can dive and safely ascend without exhaling, because the gas in the lungs had been inhaled at atmospheric pressure, is compressed during the descent, and expands back to the original volume during ascent. A scuba or surface-supplied diver breathing gas at depth from underwater breathing apparatus fills their lungs with gas at an ambient pressure greater than atmospheric pressure. At 10 metres the lungs contain twice the amount of gas that they would contain at atmospheric pressure, and if they ascend without exhaling the gas will expand to match the decreasing pressure until the lungs reach their elastic limit, and begin to tear, and is very likely to sustain life-threatening lung damage.[2][21] Besides tissue rupture, the overpressure may cause ingress of gases into the tissues through the ruptures, and further afield through the circulatory system.[2] Pulmonary barotrauma (PBt) of ascent is also known as pulmonary over-inflation syndrome (POIS), lung over-pressure injury (LOP) and burst lung.[21] Consequent injuries may include arterial gas embolism, pneumothorax, mediastinal, interstitial and subcutaneous emphysemas, depending on where the gas ends up, not usually all at the same time.
POIS may also be caused by mechanical ventilation.
Arterial gas embolism
[edit]Gas in the arterial system can be carried to the blood vessels of the brain and other vital organs. It typically causes transient embolism similar to thromboembolism but of shorter duration. Where damage occurs to the endothelium inflammation develops and symptoms resembling stroke may follow. The bubbles are generally distributed and of various sizes, and usually affect several areas, resulting in an unpredictable variety of neurological deficits. Unconsciousness or other major changes to the state of consciousness within about 10 minutes of surfacing are generally assumed to be gas embolism until proven otherwise. The belief that the gas bubbles themselves formed static emboli which remain in place until recompression has been superseded by the knowledge that the gas emboli are normally transient, and the damage is due to inflammation following endothelial damage and secondary injury from inflammatory mediator upregulation.[31]
Hyperbaric oxygen can cause downregulation of the inflammatory response and resolution of oedema by causing hyperoxic arterial vasoconstriction of the supply to capillary beds. High concentration normobaric oxygen is appropriate as first aid but is not considered definitive treatment even when the symptoms appear to resolve. Relapses are common after discontinuing oxygen without recompression.[31]
Pneumothorax
[edit]A pneumothorax is an abnormal collection of air in the pleural space between the lung and the chest wall.[32] Symptoms typically include sudden onset of sharp, one-sided chest pain and shortness of breath.[33] In a minority of cases, a one-way valve is formed by an area of damaged tissue, and the amount of air in the space between chest wall and lungs increases; this is called a tension pneumothorax.[32] This can cause a steadily worsening oxygen shortage and low blood pressure. This leads to a type of shock called obstructive shock, which can be fatal unless reversed.[32] Very rarely, both lungs may be affected by a pneumothorax.[34] It is often called a "collapsed lung", although that term may also refer to atelectasis.[35]
Divers who breathe from an underwater apparatus are supplied with breathing gas at ambient pressure, which results in their lungs containing gas at higher than atmospheric pressure. Divers breathing compressed air (such as when scuba diving) may develop a pneumothorax as a result of barotrauma from ascending just 1 metre (3 ft) while breath-holding with their lungs fully inflated.[36] An additional problem in these cases is that those with other features of decompression sickness are typically treated in a diving chamber with hyperbaric therapy; this can lead to a small pneumothorax rapidly enlarging and causing features of tension.[36]
Diagnosis of a pneumothorax by physical examination alone can be difficult (particularly in smaller pneumothoraces).[37] A chest X-ray, computed tomography (CT) scan, or ultrasound is usually used to confirm its presence.[38] Other conditions that can result in similar symptoms include a hemothorax (buildup of blood in the pleural space), pulmonary embolism, and heart attack.[33][39] A large bulla may look similar on a chest X-ray.[32]
Pneumomediastinum
[edit]Also known as mediastinal emphysema to divers, pneumomediastinum is a volume of gas inside the mediastinum, the central cavity in the chest between the lungs and surrounding the heart and central blood vessels, usually formed by gas escaping from the lungs as a result of lung rupture.[40]
Gas bubbles escaping from a ruptured lung can travel along the outside of bronchioles and blood vessels until they reach the mediastinal cavity round the heart, major blood vessels, oesophagus and trachea. Gas trapped in the mediastinum expands as the diver continues to rise. The pressure of the trapped gas may cause intense pain inside the rib cage and in the shoulders, and the gas may compress the respiratory passageways, making breathing difficult, and collapse blood vessels. Symptoms range from pain under the sternum, shock, shallow breathing, unconsciousness, respiratory failure, and associated cyanosis. The gas will usually be absorbed by the body over time, and when the symptoms are mild, no treatment may be necessary. Otherwise it may be vented through a hypodermic needle inserted into the mediastinum.[40] Recompression is not usually indicated.
Diagnosis
[edit]
Diagnosis of barotrauma generally involves a history of exposure to a source of pressure which could cause the injury suggested by the symptoms. This can vary from the immediately obvious if exposed to explosive blast, or mask squeeze, to rather complex discrimination between possibilities of inner ear decompression sickness and inner ear barotrauma, which may have nearly identical symptoms but different causative mechanism and mutually incompatible treatments. The detailed dive history may be necessary in these cases.[41]
In terms of barotrauma the diagnostic workup for the affected individual could include the following:
Laboratory:[42]
- Creatine kinase (CPK) level: Increases in CPK levels indicate tissue damage associated with decompression sickness.
- Complete blood count (CBC)
- Arterial blood gas (ABG) determination
Imaging:[42]
- Chest radiography can show pneumothorax, and is indicated if there is chest discomfort or breathing difficulty
- Computed tomography (CT) scans and magnetic resonance imaging (MRI) may be indicated when there is severe headache or severe back pain after diving.
- CT is the most sensitive method to evaluate for pneumothorax. It can be used where barotrauma-related pneumothorax is suspected and chest radiograph findings are negative.
- Echocardiography can be used to detect the number and size of gas bubbles in the right side of the heart.
Ear barotrauma
[edit]Barotrauma can affect the external, middle, or inner ear. Middle ear barotrauma (MEBT) is the most common diving injury,[43] being experienced by between 10% and 30% of divers and is due to insufficient equilibration of the middle ear. External ear barotrauma may occur if air is trapped in the external auditory canal. Diagnosis of middle and external ear barotrauma is relatively simple, as the damage is usually visible if severe enough to require intervention.
External auditory canal
[edit]Barotrauma can occur in the external auditory canal if it is blocked by cerumen, exostoses, a tight-fitting diving suit hood or earplugs, which create an airtight, air-filled space between the eardrum and the blockage. On descent, a pressure differential develops between the ambient water and the interior of this space, and this can cause swelling and haemorrhagic blistering of the canal. Treatment is usually analgesics and topical steroid eardrops. Complications may include local infection. This form of barotrauma is usually easily avoided.[43]
Middle ear
[edit]Middle ear barotrauma (MEBT) is an injury caused by a difference in pressure between the external ear canal and the middle ear. It is common in underwater divers and usually occurs when the diver does not equalise sufficiently during descent or, less commonly, on ascent. Failure to equalise may be due to inexperience or eustachian tube dysfunction, which can have many possible causes.[43] Unequalised ambient pressure increase during descent causes a pressure imbalance between the middle ear air space and the external auiditory canal over the eardrum, referred to by divers as ear squeeze, causing inward stretching, serous effusion and haemorrhage, and eventual rupture. During ascent internal over-pressure is normally passively released through the eustachian tube, but if this does not happen the volume expansion of middle ear gas will cause outward bulging, stretching and eventual rupture of the eardrum known to divers as reverse ear squeeze. This damage causes local pain and hearing loss. Tympanic rupture during a dive can allow water into the middle ear, which can cause severe vertigo from caloric stimulation. This may cause nausea and vomiting underwater, which has a high risk of aspiration of vomit or water, with possible fatal consequences.[43]
This section needs expansion with: Other causes - altitude changes, shock waves, blows to the side of the head. You can help by adding to it. (August 2022) |
Inner ear
[edit]Inner ear barotrauma (IEBt), though much less common than MEBT, shares a similar external cause. Mechanical trauma to the inner ear can lead to varying degrees of conductive and sensorineural hearing loss as well as vertigo. It is also common for conditions affecting the inner ear to result in auditory hypersensitivity.[44] Two possible mechanisms are associated with forced Valsalva manoeuvre. In the one, the Eustachian tube opens in response to the pressure, and a sudden rush of high pressure air into the middle ear causes stapes footplate dislocation and inward rupture of the oval or round window. In the other, the tube remains closed and increased cerebrospinal fluid pressure is transmitted through the cochlea and causes outward rupture of the round window.[43]
Inner ear barotrauma can be difficult to distinguish from Inner ear decompression sickness. Both conditions manifest as cochleovestibular symptoms. The similarity of symptoms makes differential diagnosis difficult, which can delay appropriate treatment or lead to inappropriate treatment.[41]
Nitrogen narcosis, oxygen toxicity, hypercarbia, and hypoxia can cause disturbances in balance or vertigo, but these appear to be central nervous system effects, not directly related to effects on the vestibular organs. High-pressure nervous syndrome during heliox compression is also a central nervous system dysfunction. Inner ear injuries with lasting effects are usually due to round window ruptures, often associated with Valsalva maneuver or inadequate middle ear equalisation.[45] Inner ear barotrauma is often concurrent with middle ear barotrauma as the external causes are generally the same. A variety of injuries may be present, which may include inner ear haemorrhage, intralabyrinthine membrane tear, perilymph fistula, and other pathologies.[46]
Divers who develop cochlear and/or vestibular symptoms during descent to any depth, or during shallow diving in which decompression sickness is unlikely, should be treated with bed rest with head elevation, and should avoid any activity which could cause raised cerebrospinal fluid and intralabyrinthine pressure.[clarification needed] If there is no improvement in symptoms after 48 hours, exploratory tympanotomy may be considered to investigate possible repair of a labyrinthine window fistula. Recompression therapy is contraindicated in these cases, but is the definitive treatment for inner ear decompression sickness, making an early and accurate differential diagnosis important for deciding on appropriate treatment. IEBt in divers may be difficult to distinguish from inner ear decompression sickness (IEDCS), and as a dive profile alone cannot always eliminate either of the possibilities, the detailed dive history may be necessary to diagnose the more likely injury.[41][46] It is also possible for both to occur at the same time, and IEDCS is more likely to affect the semicircular canals, causing severe vertigo, while IEBt is more likely to affect the cochlea, causing hearing loss, but these are just statistical probabilities, and in reality it can go either way or both.[47] It is accepted practice to assume that if any symptom typical of DCS is present, that the diver has DCS and will be treated accordingly with recompression.[47] Limited case data suggest that recompression does not usually cause harm if the differential diagnosis between IEBt vs IEDCS is doubtful.[46]
| Barotrauma | Decompression sickness |
|---|---|
| Conductive or mixed hearing loss | Sensorineural hearing loss |
| Occurs during descent or ascent | Onset during ascent or after surfacing |
| Cochlear symptoms (i.e. hearing loss) predominate | Vestibular symptoms (vertigo) predominant; right sided |
| History of difficult ear clearing or forced Valsalva manoeuvre | No history of eustachian tube dysfunction |
| Low-risk dive profile | Depth >15 m, helium mixtures, helium to nitrogen gas switches, repetitive dives |
| Isolated inner ear symptoms, or inner and middle ear on the same sides | Other neurological or dermatological symptoms suggestive of DCS |
Barosinusitis
[edit]The sinuses, like other air-filled cavities, are susceptible to barotrauma if their openings become obstructed. This can result in pain as well as epistaxis (nosebleed). Diagnosis is usually simple provided the history of pressure exposure is mentioned.[48] Barosinusitis, is also called aerosinusitis, sinus squeeze or sinus barotrauma. Sinus barotrauma can be caused by external or internal overpressure. External over-pressure is called sinus squeeze by divers, while internal over-pressure is usually referred to as reverse block or reverse squeeze.
Mask squeeze
[edit]If a diver's mask is not equalized during descent the relative negative internal pressure can produce petechial hemorrhages in the area covered by the mask along with subconjunctival hemorrhages.[48]
Helmet squeeze
[edit]A problem mostly of historical interest, but still relevant to surface supplied divers who dive with the helmet sealed to the dry suit. If the air supply hose is ruptured near or above the surface, the pressure difference between the water around the diver and the air in the hose can be several bar. The non-return valve at the connection to the helmet will prevent backflow if it is working correctly, but if absent, as in the early days of helmet diving, or if it fails, the pressure difference will tend to squeeze the diver into the rigid helmet, which can result in severe trauma. The same effect can result from a large and rapid increase in depth if the air supply is insufficient to keep up with the increase in ambient pressure.[49] On a helmet with a neck dam, the neck dam will allow water to flood the helmet before serious barotrauma can occur. This can happen with helium reclaim helmets if the reclaim regulator system fails, so there is a manual bypass valve, which allows the helmet to be purged so breathing can continue on open circuit.
Pulmonary barotrauma
[edit]Lung over-pressure injury in ambient pressure divers using underwater breathing apparatus is usually caused by breath-holding on ascent. The compressed gas in the lungs expands as the ambient pressure decreases causing the lungs to over-expand and rupture unless the diver allows the gas to escape by maintaining an open airway, as in normal breathing. The lungs do not sense pain when over-expanded giving the diver little warning to prevent the injury. This does not affect breath-hold divers as they bring a lungful of air with them from the surface, which merely re-expands safely to near its original volume on ascent.[2] The problem only arises if a breath of ambient pressure gas is taken at depth, which may then expand on ascent to more than the lung volume. Pulmonary barotrauma may also be caused by explosive decompression of a pressurised aircraft,[50] as occurred on 1 February 2003 to the crew in the Space Shuttle Columbia disaster.
Prevention
[edit]Diving
[edit]Barotrauma may be caused when diving, either from being crushed, or squeezed, on descent or by stretching and bursting on ascent; both can be avoided by equalising the pressures. A negative, unbalanced pressure is known as a squeeze, crushing eardrums, dry suit, lungs or mask inwards and can be equalised by putting air into the squeezed space. A positive unbalanced pressure expands internal spaces rupturing tissue and can be equalised by letting air out, for example by exhaling. Both may cause barotrauma. There are a variety of techniques depending on the affected area and whether the pressure inequality is a squeeze or an expansion:
- Ears and sinuses: There is a risk of stretched or burst eardrums, usually crushed inwards during descent but sometimes stretched outwards on ascent. The diver can use a variety of methods to let air into or out of the middle ears via the Eustachian tubes. Sometimes swallowing will open the Eustachian tubes and equalise the ears.[51]
- Lungs: There is a risk of pneumothorax, arterial gas embolism, and mediastinal and subcutaneous emphysema during ascent, which are commonly called burst lung or lung overpressure injury by divers. To equalise the lungs, all that is necessary is not to hold the breath during ascent. This risk does not occur when breath-hold diving from the surface, unless the diver breathes from an ambient pressure gas source underwater; breath-hold divers do suffer squeezed lungs on descent, crushing in the chest cavity, but, while uncomfortable, this rarely causes lung injury and returns to normal at the surface. Some people have pathology of the lung which prevent rapid flow of excess air through the passages, which can lead to lung barotrauma even if the breath is not held during rapid depressurisation. These people should not dive as the risk is unacceptably high. Most commercial or military diving medical examinations will look specifically for signs of this pathology.[52]
- Diving mask squeeze enclosing the eyes and nose: The main risk is rupture of the capillaries of the eyes and facial skin because of the negative pressure difference between the gas space and blood pressure,[10] or orbital emphysema from higher pressures.[53][clarification needed] This can be avoided by breathing air into the mask through the nose. Goggles covering only the eyes are not suitable for deep diving as they cannot be equalised.
- Dry suit squeeze. The main risk is skin getting pinched and bruised by folds of the dry suit when squeezed on descent. Most dry suits can be equalised against squeeze via a manually operated valve fed from a low pressure gas supply. Air must be manually injected during the descent to avoid squeeze and is manually or automatically vented on the ascent to maintain buoyancy control.[54]
- Diving helmet squeeze: Helmet squeeze will occur if the gas supply hose is severed above the diver and the non-return valve at the helmet gas inlet fails or is not fitted. Severity will depend on the hydrostatic pressure difference.[55] A very rapid descent, usually by accident, may exceed the rate at which the breathing gas supply can equalise the pressure causing a temporary squeeze. The introduction of the non-return valve and high maximum gas supply flow rates have all but eliminated both these risks. In helmets fitted with a neck dam, the dam will admit water into the helmet if the internal pressure gets too low; this is less of a problem than helmet squeeze but the diver may drown if the gas supply is not reinstated quickly.[49]: 90 This form of barotrauma is avoidable by controlled descent rate, which is standard practice for commercial divers, who will use shotlines, diving stages and wet bells to control descent and ascent rates.
Medical screening
[edit]Professional divers are screened for risk factors during initial and periodical medical examination for fitness to dive.[56] In most cases recreational divers are not medically screened, but are required to provide a medical statement before acceptance for training in which the most common and easy to identify risk factors must be declared. If these factors are declared, the diver may be required to be examined by a medical practitioner, and may be disqualified from diving if the conditions indicate.[57]
Asthma, Marfan syndrome, and COPD pose a very high risk of pneumothorax.[clarification needed] In some countries these may be considered absolute contraindications, while in others the severity may be taken into consideration. Asthmatics with a mild and well controlled condition may be permitted to dive under restricted circumstances.[58]
Training
[edit]A significant part of entry level diver training is focused on understanding the risks and procedural avoidance of barotrauma.[59] Professional divers and recreational divers with rescue training are trained in the basic skills of recognizing and first aid management of diving barotrauma.[60][61]
Mechanical ventilation
[edit]Isolated mechanical forces may not adequately explain ventilator induced lung injury (VILI). The damage is affected by the interaction of these forces and the pre-existing state of the lung tissues, and dynamic changes in alveolar structure may be involved. Factors such as plateau pressure and positive end-expiratory pressure (PEEP) alone do not adequately predict injury. Cyclic deformation of lung tissue may play a large part in the cause of VILI, and contributory factors probably include tidal volume, positive end-expiratory pressure and respiratory rate. There is no protocol guaranteed to avoid all risk in all applications.[29]
Aviation and spaceflight
[edit]Barotrauma caused during airplane journeys is also referred to as airplane ear.[62] The environmental pressure must be prevented from changing rapidly by large amounts.[30] One should include multiple redundant levels of protection against rapid decompression, and systems allowing non-catastrophic failure with sufficient time to allow comfortable equalization of relevant air spaces, particularly the inner ear. A low internal pressure reduces decompression rate and severity in a catastrophic decompression reduces the risk of barotrauma but can increase the risk of decompression sickness and hypoxia in normal operating conditions.
Some measures for protection against rapid decompression specific to airplanes include:[62]
- Yawn and swallow during ascent and descent
- Use the Valsalva maneuver during ascent and descent
- Avoid sleeping during takeoffs and landings
- Use an over the counter nasal spray
- Using filtered earplugs which slowly equalize the pressure against your eardrum during ascents and descents
Outside of a pressurized cabin environment at very high altitudes, a pressure suit is the usual protective measure and is the definitive protection in decompression and exposure to vacuum, but they are expensive, heavy, bulky, restrict mobility, cause thermal regulatory problems, and reduce comfort.[63] To prevent injury from unavoidable pressure changes, similar equalization techniques and relatively slow pressure changes are required, which in turn require patent Eustachian tubes and sinuses.
Treatment
[edit]Treatment of diving barotrauma depends on the symptoms, which depend on the affected tissues. Lung over-pressure injury may require a chest drain to remove air from the pleura or mediastinum. Recompression with hyperbaric oxygen therapy is the definitive treatment for arterial gas embolism, as the raised pressure reduces bubble size, the reduced blood inert gas concentration may accelerate inert gas solution, and high oxygen partial pressure helps oxygenate tissues compromised by the emboli. Care must be taken when recompressing to avoid a tension pneumothorax.[64] Barotraumas that do not involve gas in the tissues are generally treated according to severity and symptoms for similar trauma from other causes.
This section needs expansion with: Treatment for VILI. You can help by adding to it. (July 2022) |
First aid
[edit]Pre-hospital care for lung barotrauma includes basic life support of maintaining adequate oxygenation and perfusion, assessment of airway, breathing and circulation, neurological assessment, and managing any immediate life-threatening conditions. High-flow oxygen up to 100% is considered appropriate for diving accidents. Large-bore venous access with isotonic fluid infusion is recommended to maintain blood pressure and pulse.[65]
Emergency treatment
[edit]Pulmonary barotrauma:[66]
- Endotracheal intubation may be required if the airway is unstable or hypoxia persists when breathing 100% oxygen.
- Needle decompression or tube thoracostomy may be necessary to drain a pneumothorax or haemothorax
- Foley catheterization may be necessary for spinal cord AGE if the person is unable to urinate.
- Intravenous hydration may be required to maintain adequate blood pressure.
- Therapeutic recompression is indicated for severe AGE. The diving medical practitioner will need to know the vital signs and relevant symptoms, along with the recent pressure exposure and breathing gas history of the patient. Air transport should be below 1,000 feet (300 m) if possible, or in a pressurized aircraft which should be pressurised to as low an altitude as reasonably possible.
Sinus squeeze and middle ear squeeze are generally treated with decongestants to reduce the pressure differential, with anti-inflammatory medications to treat the pain. For severe pain, narcotic analgesics may be appropriate.[66]
Suit, helmet and mask squeeze are treated as trauma according to symptoms and severity.
Medication
[edit]The primary medications for lung barotrauma are hyperbaric and normobaric oxygen, hyperbaric heliox or nitrox, isotonic fluids, anti-inflammatory medications, decongestants, and analgesics.[67]
This section needs expansion with: medication used to treat ear barotrauma. You can help by adding to it. (July 2022) |
Outcomes
[edit]Following barotrauma of the ears or lungs from diving the diver should not dive again until cleared by a diving doctor. After ear injury examination will include a hearing test and a demonstration that the middle ear can be autoinflated. Recovery can take weeks to months.[68]
Epidemiology
[edit]An estimate of in the order of 1000 dive injuries per year occur in the United States and Canada. Many of these involve barotrauma, with nearly 50% of reported injuries involving middle ear barotrauma. Diving injuries tend to correlate with trait anxiety and a tendency to panic, lack of experience, advancing age and reduction in fitness, alcohol usage, obesity, asthma, chronic sinusitis and otitis.[69]
This section needs expansion with: Epidemiology of VILI. COPD?. You can help by adding to it. (July 2022) |
Barotrauma in other animals
[edit]Whales and dolphins develop severely disabling barotrauma when exposed to excessive pressure changes induced by navy sonar, oil industry airguns, explosives, undersea earthquakes and volcanic eruptions.[citation needed] Injury and mortality of fish, marine mammals, including sea otters, seals, dolphins and whales, and birds by underwater explosions has been recorded in several studies.[70]
It has been claimed that bats can suffer fatal barotrauma in the low pressure zones behind the blades of wind turbines due to their more fragile mammalian lung structure in comparison with the more robust avian lungs, which are less affected by pressure change.[71][72] The claims that have been made that bats can be killed by lung barotrauma when flying in low-pressure regions close to operating wind-turbine blades, have been supported by reports of measurements of the pressures around the turbine blades.[73] The diagnosis and contribution of barotrauma to bat deaths near wind turbine blades have been disputed by other research comparing dead bats found near wind turbines with bats killed by impact with buildings in areas with no turbines.[74]
Swim bladder overexpansion
[edit]

Fish with isolated swim bladders are susceptible to barotrauma of ascent when brought to the surface by fishing. The swim bladder is an organ of buoyancy control which is filled with gas extracted from solution in the blood, and which is normally removed by the reverse process. If the fish is brought upwards in the water column faster than the gas can be resorbed, the gas will expand until the bladder is stretched to its elastic limit, and may rupture. Barotrauma can be directly fatal or disable the fish rendering it vulnerable to predation, but rockfish are able to recover if they are returned to depths similar to those they were pulled up from, shortly after surfacing. Scientists at NOAA developed the Seaqualizer to quickly return rockfish to depth.[75] The device could increase survival in caught-and-released rockfish.
See also
[edit]- Alternobaric vertigo – Dizziness resulting from unequal pressures in the middle ears
- Atelectotrauma – Damage caused to the lung by mechanical ventilation
- Barodontalgia – Tooth pain caused by ambient pressure change
- Diving hazards and precautions – Hazards associated with underwater diving
- Dysbarism – Medical conditions resulting from changes in ambient pressure
- Decompression sickness – Disorder caused by dissolved gases forming bubbles in tissues
- Inner ear decompression sickness – Medical condition caused by inert gas bubbles forming out of solution
- Modes of mechanical ventilation – Methods of inspiratory support
- Rheotrauma – Harm caused to a patient's lungs by high gas flows as delivered by mechanical ventilation
- Weather pains, also known as Meteoropathy – Claims of pain associated with changes in barometric pressure, humidity or other weather phenomena
- Uncontrolled decompression – Unplanned drop in the pressure of a sealed system
References
[edit]- ^ a b c d e f g h US Navy Diving Manual, 6th revision. United States: US Naval Sea Systems Command. 2006. Archived from the original on 2 May 2008. Retrieved 26 May 2008.
- ^ a b c d e f g h i j k l Brubakk, A.O.; Neuman, T.S. (2003). Bennett and Elliott's physiology and medicine of diving (5th Rev. ed.). United States: Saunders Ltd. p. 800. ISBN 978-0-7020-2571-6.
- ^ James, P.B. (October 1993). "Dysbarism: the medical problems from high and low atmospheric pressure". Journal of the Royal College of Physicians of London. 27 (4): 367–74. PMC 5396710. PMID 8289154.
- ^ Reinhart, Richard O. (1996). Basic Flight Physiology. McGraw-Hill Professional. ISBN 978-0-07-052223-7.
- ^ a b Fitzpatrick, D.T.; Franck, B.A.; Mason, K.T.; Shannon, S.G. (1999). "Risk factors for symptomatic otic and sinus barotrauma in a multiplace hyperbaric chamber". Undersea and Hyperbaric Medicine. 26 (4): 243–7. PMID 10642071. Archived from the original on 11 August 2011. Retrieved 26 May 2008.
{{cite journal}}: CS1 maint: unfit URL (link) - ^ Fiesseler, F.W.; Silverman, M.E.; Riggs, R.L.; Szucs, P.A. (2006). "Indication for hyperbaric oxygen treatment as a predictor of tympanostomy tube placement". Undersea and Hyperbaric Medicine. 33 (4): 231–5. PMID 17004409. Archived from the original on 3 February 2011. Retrieved 26 May 2008.
{{cite journal}}: CS1 maint: unfit URL (link) - ^ Klokker, M.; Vesterhauge, S.; Jansen, E.C. (November 2005). "Pressure-equalizing earplugs do not prevent barotrauma on descent from 8000 ft cabin altitude". Aviation, Space, and Environmental Medicine. 76 (11): 1079–82. PMID 16313146. Archived from the original on 3 February 2019. Retrieved 5 June 2008.
- ^ Broome, J.R.; Smith, D.J. (November 1992). "Pneumothorax as a complication of recompression therapy for cerebral arterial gas embolism". Undersea Biomedical Research. 19 (6): 447–55. PMID 1304671. Archived from the original on 3 February 2011. Retrieved 26 May 2008.
{{cite journal}}: CS1 maint: unfit URL (link) - ^ Nicol, E.; Davies, G.; Jayakumar, P.; Green, N.D. (April 2007). "Pneumopericardium and pneumomediastinum in a passenger on a commercial flight". Aviation, Space, and Environmental Medicine. 78 (4): 435–9. PMID 17484349. Archived from the original on 3 February 2019. Retrieved 5 June 2008.
- ^ a b Butler, F.K.; Gurney, N. (2001). "Orbital hemorrhage following face-mask barotrauma". Undersea and Hyperbaric Medicine. 28 (1): 31–4. PMID 11732882. Archived from the original on 11 August 2011. Retrieved 7 July 2008.
{{cite journal}}: CS1 maint: unfit URL (link) - ^ Cortes, Maria D.P.; Longridge, Neil S.; Lepawsky, Michael; Nugent, Robert A. (May 2005). "Barotrauma Presenting as Temporal Lobe Injury Secondary to Temporal Bone Rupture" (PDF). American Journal of Neuroradiology. 26 (5): 1218–1219. PMC 8158631. PMID 15891187. Archived (PDF) from the original on 27 September 2011. Retrieved 30 May 2008.
- ^ Robichaud, R.; McNally, M.E. (January 2005). "Barodontalgia as a differential diagnosis: symptoms and findings". Journal of the Canadian Dental Association. 71 (1): 39–42. PMID 15649340. Archived from the original on 29 August 2017. Retrieved 19 July 2008.
- ^ Rauch, J.W. (1985). "Barodontalgia—dental pain related to ambient pressure change". Gen Dent. 33 (4): 313–5. PMID 2863194.
- ^ Zadik, Y. (August 2006). "Barodontalgia due to odontogenic inflammation in the jawbone". Aviation, Space, and Environmental Medicine. 77 (8): 864–6. PMID 16909883. Archived from the original on 20 December 2019. Retrieved 16 July 2008.
- ^ Zadik, Y.; Chapnik, L.; Goldstein, L. (June 2007). "In-flight barodontalgia: analysis of 29 cases in military aircrew". Aviation, Space, and Environmental Medicine. 78 (6): 593–6. PMID 17571660. Archived from the original on 20 December 2019. Retrieved 16 July 2008.
- ^ Zadik, Yehuda (April 2009). "Barodontalgia". Journal of Endodontics. 35 (4): 481–5. doi:10.1016/j.joen.2008.12.004. PMID 19345791.
- ^ Zadik, Y.; Einy, S.; Pokroy, R.; Bar Dayan, Y.; Goldstein, L. (June 2006). "Dental Fractures on Acute Exposure to High Altitude". Aviation, Space, and Environmental Medicine. 77 (6): 654–7. PMID 16780246. Archived from the original on 27 March 2020. Retrieved 17 July 2008.
- ^ Zadik, Yehuda (January 2009). "Aviation dentistry: current concepts and practice" (PDF). British Dental Journal. 206 (1): 11–6. doi:10.1038/sj.bdj.2008.1121. PMID 19132029. S2CID 25000523. Archived (PDF) from the original on 25 October 2012. Retrieved 2 June 2009.
- ^ Zadik, Yehuda; Drucker, Scott (September 2011). "Diving dentistry: a review of the dental implications of scuba diving". Australian Dental Journal. 56 (3): 265–71. doi:10.1111/j.1834-7819.2011.01340.x. PMID 21884141.
- ^ Harris, Richard (December 2009). "Genitourinary infection and barotrauma as complications of 'P-valve' use in drysuit divers". Diving and Hyperbaric Medicine. 39 (4): 210–2. PMID 22752741. Archived from the original on 26 May 2013. Retrieved 5 April 2013.
{{cite journal}}: CS1 maint: unfit URL (link) - ^ a b c "Mechanism of Injury for Pulmonary Over-Inflation Syndrome". DAN Medical Frequently Asked Questions. Diver's Alert Network. Archived from the original on 18 November 2018. Retrieved 17 January 2017.
- ^ Lehm, Jan P.; Bennett, Michael H. (2003). "Predictors of middle ear barotrauma associated with hyperbaric oxygen therapy". South Pacific Underwater Medicine Society Journal. 33: 127–133. Archived from the original on 22 July 2009.
{{cite journal}}: CS1 maint: unfit URL (link) - ^ Torkki, Markus; Koljonen, Virve; Sillanpää1, Kirsi; Tukiainen, Erkki; Pyörälä, Sari; Kemppainen, Esko; Kalske, Juha; Arajärvi, Eero; Keränen, Ulla; Hirvensalo, Eero (August 2006). "Triage in a Bomb Disaster with 166 Casualties". European Journal of Trauma. 32 (4): 374–80. doi:10.1007/s00068-006-6039-8. S2CID 32968659.
{{cite journal}}: CS1 maint: numeric names: authors list (link) - ^ Williams, Kenneth Gabriel (1959). The New Frontier: Man's Survival in the Sky. Thomas.
- ^ Bason, R.; Yacavone, D.W. (May 1992). "Loss of cabin pressurization in U.S. Naval aircraft: 1969–90". Aviation, Space, and Environmental Medicine. 63 (5): 341–5. PMID 1599378.
- ^ Parker, J.C.; Hernandez, L.A.; Peevy, K.J. (1993). "Mechanisms of ventilator-induced lung injury". Crit Care Med. 21 (1): 131–43. doi:10.1097/00003246-199301000-00024. PMID 8420720. S2CID 23200644.
- ^ a b Soo Hoo, Guy W. (31 December 2015). Mosenifar, Zab (ed.). "Barotrauma and Mechanical Ventilation". Drugs and Diseases – Clinical Procedures. Medscape. Archived from the original on 10 July 2019. Retrieved 16 January 2017.
- ^ a b Haake, Ronald; Schlichtig, Robert; Ulstad, David R.; Henschen, Ross R. (April 1987). "Barotrauma: Pathophysiology, Risk Factors, and Prevention". Chest. 91 (4): 608–613. doi:10.1378/chest.91.4.608. PMID 3549176.
- ^ a b Albaiceta, G.M.; Blanch, L (2011). "Beyond volutrauma in ARDS: the critical role of lung tissue deformation". Crit Care. 15 (2): 304. doi:10.1186/cc10052. PMC 3219320. PMID 21489320.
- ^ a b Norfleet, W.T. (2008). "Decompression-Related Disorders: Decompression Sickness, Arterial Gas Embolism, and Ebullism Syndrome". In Barratt, M.R.; Pool, S.L. (eds.). Principles of Clinical Medicine for Space Flight. Springer, New York, NY. pp. 223–246. doi:10.1007/978-0-387-68164-1_11. ISBN 978-0-387-98842-9.
- ^ a b Walker, J. R. III; Murphy-Lavoie, Heather M. (20 December 2019). "Diving Gas Embolism". www.ncbi.nlm.nih.gov. StatPearls. PMID 29493946. Archived from the original on 17 March 2021. Retrieved 29 March 2020.
- ^ a b c d Bintcliffe, O; Maskell, N. (May 2014). "Spontaneous pneumothorax". BMJ. 348: g2928. doi:10.1136/bmj.g2928. PMID 24812003. S2CID 32575512.
- ^ a b "What Are the Signs and Symptoms of Pleurisy and Other Pleural Disorders". www.nhlbi.nih.gov. 21 September 2011. Archived from the original on 8 October 2016. Retrieved 31 October 2016.
- ^ Morjaria, J.B.; Lakshminarayana, U.B.; Liu-Shiu-Cheong, P.; Kastelik, J.A. (November 2014). "Pneumothorax: a tale of pain or spontaneity". Therapeutic Advances in Chronic Disease. 5 (6): 269–273. doi:10.1177/2040622314551549. PMC 4205574. PMID 25364493.
- ^ Orenstein, D.M. (2004). Cystic Fibrosis: A Guide for Patient and Family. Lippincott Williams & Wilkins. p. 62. ISBN 9780781741521. Archived from the original on 31 October 2016.
- ^ a b Neuman TS (2003). "Arterial gas embolism and pulmonary barotrauma". In Brubakk AO, Neuman TS (eds.). Bennett and Elliott's physiology and medicine of diving (5th Rev ed.). United States: Saunders. pp. 558–61. ISBN 978-0-7020-2571-6.
- ^ Yarmus, L.; Feller-Kopman, D. (April 2012). "Pneumothorax in the critically ill patient". Chest. 141 (4): 1098–1105. doi:10.1378/chest.11-1691. PMID 22474153. S2CID 207386345.
- ^ Chen, L.; Zhang, Z. (August 2015). "Bedside ultrasonography for diagnosis of pneumothorax". Quantitative Imaging in Medicine and Surgery. 5 (4): 618–623. doi:10.3978/j.issn.2223-4292.2015.05.04. PMC 4559988. PMID 26435925.
- ^ Peters, J.R.; Egan, D.; Mick, N.W. (2006). Nadel, E.S. (ed.). Blueprints Emergency Medicine. Lippincott Williams & Wilkins. p. 44. ISBN 9781405104616. Archived from the original on 1 November 2016.
- ^ a b "Mediastinal emphysema". www.britannica.com. Encyclopedia Britannica. Retrieved 28 September 2022.
- ^ a b c Lindfors, O.H.; Räisänen-Sokolowski, A.K.; Hirvonen, T.P.; Sinkkonen, S.T. (20 December 2021). "Inner ear barotrauma and inner ear decompression sickness: a systematic review on differential diagnostics". Diving and Hyperbaric Medicine. 51 (4): 328–337. doi:10.28920/dhm51.4.328-337. PMC 8923696. PMID 34897597.
- ^ a b Kaplan, Joseph. Alcock, Joe (ed.). "Barotrauma Workup: Laboratory Studies, Imaging Studies, Other Tests". emedicine.medscape.com. Archived from the original on 23 August 2017. Retrieved 15 January 2017.
- ^ a b c d e f Nofz, Lyndon; Porrett, Jemma; Yii, Nathan; De Alwis, Nadine. "Diving related otological injuries". www1.racgp.org.au. Archived from the original on 1 December 2021. Retrieved 25 July 2022. Reprinted from AJGP vol 49, no 8, August 2020 The Royal Australian College of General Practitioners 2020
- ^ Marx, John (2010). Rosen's emergency medicine: concepts and clinical practice (7th ed.). Philadelphia, PA: Mosby/Elsevier. p. 1906. ISBN 978-0-323-05472-0.
- ^ Farmer, J.C. Jr. (January–February 1977). "Diving injuries to the inner ear". Ann Otol Rhinol Laryngol Suppl. 86 (1 Pt 3 Suppl 36): 1–20. doi:10.1177/00034894770861s201. PMID 402882. S2CID 29563783.
- ^ a b c Elliott, E.J.; Smart, D.R. (December 2014). "The assessment and management of inner ear barotrauma in divers and recommendations for returning to diving". Diving Hyperb Med. 44 (4): 208–22. PMID 25596834.
- ^ a b Meier, Matthew (5 November 2021). "Inner-Ear Barotrauma vs. DCS". xray-mag.com. X-Ray Magazine. Archived from the original on 26 July 2022. Retrieved 26 July 2022.
- ^ a b Marx, John (2010). Rosen's emergency medicine: concepts and clinical practice 7th edition. Philadelphia, PA: Mosby/Elsevier. p. 1907. ISBN 978-0-323-05472-0.
- ^ a b Barsky, Steven; Neuman, Tom (2003). Investigating Recreational and Commercial Diving Accidents. Santa Barbara, California: Hammerhead Press. pp. 61, 90. ISBN 978-0-9674305-3-9.
- ^ Staff (29 March 2013). "Aircraft Operations at Altitudes Above 25,000 Feet Mean Sea Level or Mach Numbers Greater Than .75" (PDF). Advisory Circular 61-107B. U.S. Department of Transportation Federal Aviation Administration. p. 36. Archived (PDF) from the original on 28 January 2017. Retrieved 13 January 2017.
- ^ Kay, E. (2000). "Prevention of middle ear barotrauma". Doc's Diving Medicine. staff.washington.edu. Archived from the original on 16 January 2017. Retrieved 13 January 2017.
- ^ Vorosmarti, J.; Linaweaver, P.G., eds. (1987). "Fitness to Dive. 34th Undersea and Hyperbaric Medical Society Workshop". UHMS Publication Number 70(WS-WD)5-1-87. Bethesda, Maryland: Undersea and Hyperbaric Medical Society. Archived from the original on 20 August 2008. Retrieved 13 January 2017.
{{cite web}}: CS1 maint: unfit URL (link) - ^ Bolognini, A.; Delehaye, E.; Cau, M.; Cosso, L. (2008). "Barotraumatic orbital emphysema of rhinogenic origin in a breath-hold diver: a case report". Undersea and Hyperbaric Medicine. 35 (3): 163–7. PMID 18619111. Archived from the original on 15 April 2013.
{{cite journal}}: CS1 maint: unfit URL (link) - ^ Barsky, Steven M.; Long, Dick; Stinton, Bob (2006). Dry Suit Diving: A Guide to Diving Dry. Ventura, Calif.: Hammerhead Press. ISBN 978-0-9674305-6-0.
- ^ Staff. "Incidents list". Incidents database. The Divers Association. p. 22. Retrieved 18 May 2017.[permanent dead link]
- ^ Joint Medical Subcommittee of ECHM and EDTC (24 June 2003). Wendling, Jürg; Elliott, David; Nome, Tor (eds.). Fitness to Dive Standards – Guidelines for Medical Assessment of Working Divers (PDF). pftdstandards edtc rev6.doc (Report). European Diving Technology Committee. Archived from the original (PDF) on 26 August 2016. Retrieved 18 May 2017.
- ^ Richardson, Drew. "The RSTC Medical statement and candidate screening model". South Pacific Underwater Medicine Society (SPUMS) Journal Volume 30 No.4 December 2000. South Pacific Underwater Medicine Society. pp. 210–213. Archived from the original on 5 July 2013.
{{cite web}}: CS1 maint: unfit URL (link) - ^ Adir, Yochai; Bove, Alfred A. (2016). "Can asthmatic subjects dive?" (PDF). European Respiratory Review. 25 (140): 214–220. doi:10.1183/16000617.0006-2016. PMC 9487249. PMID 27246598. S2CID 35971130. Archived (PDF) from the original on 23 June 2016. Retrieved 10 June 2016.
- ^ "Minimum course standard for Open Water Diver training" (PDF). World Recreational Scuba Training Council. 1 October 2004. pp. 8–9. Archived (PDF) from the original on 17 October 2016. Retrieved 16 January 2017.
- ^ "Diving Regulations 2009". Occupational Health and Safety Act 85 of 1993 – Regulations and Notices – Government Notice R41. Pretoria: Government Printer. Archived from the original on 4 November 2016. Retrieved 3 November 2016 – via Southern African Legal Information Institute.
- ^ "International Diver Training Certification: Diver Training Standards, Revision 4" (PDF). Diver Training Standards. Malestroit, Brittany: International Diving Schools Association. 29 October 2009. Archived from the original (PDF) on 3 March 2016. Retrieved 6 November 2016.
- ^ a b "Airplane ear-Airplane ear - Symptoms & causes". Mayo Clinic. Retrieved 24 September 2024.
- ^ Murray, Daniel H.; Pilmanis, Andrew A.; Blue, Rebecca S.; Pattarini, James M; Law, Jennifer; Bayne, C Gresham; Turney, Matthew W.; Clark, Jonathan B (2013). "Pathophysiology, prevention, and treatment of ebullism". Aviation, Space, and Environmental Medicine. 84 (2): 89–96. doi:10.3357/ASEM.3468.2013. PMID 23447845.
- ^ Stephenson, Jeffrey. "Pathophysiology, treatment and aeromedical retrieval of SCUBA – related DCI". Journal of Military and Veterans' Health. 17 (3). ISSN 1835-1271. Archived from the original on 23 December 2017. Retrieved 13 January 2017.
- ^ Kaplan, Joseph. Alcock, Joe (ed.). "Barotrauma Treatment & Management". emedicine.medscape.com. Archived from the original on 18 January 2017. Retrieved 15 January 2017.
- ^ a b Kaplan, Joseph. Alcock, Joe (ed.). "Barotrauma Treatment & Management: Emergency Department Care". emedicine.medscape.com. Archived from the original on 18 January 2017. Retrieved 15 January 2017.
- ^ Kaplan, Joseph. Alcock, Joe (ed.). "Barotrauma Medication". emedicine.medscape.com. Archived from the original on 11 January 2017. Retrieved 15 January 2017.
- ^ Bentz, Brandon G.; Hughes, C. Anthony (October 2012). "Barotrauma". Hearing and balance disorders. American Hearing Research Foundation. Archived from the original on 17 January 2017. Retrieved 16 January 2017.
- ^ Battisti, Amanda S.; Haftel, Anthony; Murphy-Lavoie, Heather M. (27 June 2022). "Barotrauma". www.ncbi.nlm.nih.gov. StatPearls Publishing LLC. PMID 29493973. Archived from the original on 18 December 2022. Retrieved 30 July 2022.
- ^ Danil, K.; St.Leger, J.A. (2011). "Seabird and Dolphin Mortality Associated with Underwater Detonation Exercises" (PDF). Marine Technology Society Journal. 45 (6): 89–95. doi:10.4031/mtsj.45.6.5. Archived (PDF) from the original on 27 December 2016. Retrieved 17 December 2013.
- ^ "Wind farms cause thousands of bats to die from trauma". The Times. 26 August 2008.
- ^ staff (26 August 2008). "Why Wind Turbines Can Mean Death For Bats". Science news. Science Daily. Archived from the original on 26 July 2024. Retrieved 13 January 2017.
- ^ Baerwald, Erin F.; D'Amours, Genevieve H.; Klug, Brandon J.; Barclay, Robert M. R. (26 August 2008). "Barotrauma is a significant cause of bat fatalities at wind turbines". Current Biology. 18 (16): R695–R696. Bibcode:2008CBio...18.R695B. doi:10.1016/j.cub.2008.06.029. OCLC 252616082. PMID 18727900. S2CID 17019562. Lay source includes audio podcast of interview with author.
- ^ Rollins, K.E.; Meyerholz, D.; Johnson, D.; Capparella, A.; Loew, S. (January 2012). "A Forensic Investigation Into the Etiology of Bat Mortality at a Wind Farm: Barotrauma or Traumatic Injury?". Veterinary Pathology. 49 (2): 362–371. doi:10.1177/0300985812436745. PMID 22291071. S2CID 11189743.
- ^ Tripp, Emily (5 November 2012). "Saving Rockfish Stocks One Recompression at a Time". Marine Science Today. Archived from the original on 15 November 2015. Retrieved 29 August 2015.
External links
[edit]
